-
Chris Sanchez
·
Kelsey’s Stage 4 EGFR+ and ALK+ Non-Small Cell Lung Cancer Story
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic) Symptoms: Severe back pain, falling due to collapsed spinal vertebrae Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
-

Chris Sanchez
·
Living With Follicular Lymphoma: Tawanna and Barry on Watch & Wait, Marriage, and Faith
Tawanna T., Follicular Lymphoma, Stage 3 Symptoms: Incidental finding during pre-kidney donation scan Treatment: Watch and wait/active surveillance
-

Chris Sanchez
·
How an Athlete’s Mindset Guided Marina’s Triple-Negative Breast Cancer Experience – Twice
Marina B., Triple-Negative Breast Cancer, Stage 2, BRCA1+ Symptoms: Month-long twinge of pain in breast (first diagnosis), appearance of lump in armpit (second diagnosis) Treatments: Chemotherapy (AC and paclitaxel), surgery (mastectomy and reconstruction), radiation therapy
-

Chris Sanchez
·
Hope and Self‑Advocacy: Holly’s Stage 4 Endometrial Cancer Experience
Holly J., Endometrial Cancer, Stage 4 (Metastatic) Symptoms: Severe fatigue, depression, decreased appetite, feeling full quickly, abnormal bleeding, severe pelvic pain, persistent skin infection Treatments: Chemotherapy, surgery (hysterectomy)
-

Chris Sanchez
·
Colon Cancer at 24: Meagan’s Story of Listening to One Symptom
Meagan M., Colon Cancer, Stage 3C Symptom: Appearance of blood in stool Treatments: Surgery (partial colectomy), chemotherapy (FOLFOX)
-

Chris Sanchez
·
Metastatic Thyroid Cancer in College: Grace’s Story of Self‑Advocacy and Softball
Grace B., Thyroid Cancer (Papillary Thyroid Carcinoma), Metastatic Symptoms: Significant and unexplained weight gain, persistent fatigue, brain fog, bloating Treatments: Surgery (subtotal thyroidectomy with central neck dissection), watch and wait/active surveillance
-

Chris Sanchez
·
Kalei’s Stage 4 Rectal Cancer Story: Has My Cancer Returned?
Kalei M., Rectal Cancer, Stage 4 (Metastatic) Symptoms: More frequent bowel movements, presence of mucus, tissue-like substance, and blood in stool, stomach cramping and sharp pains Treatments: Radiation therapy, chemotherapy (FOLFOX), surgeries (two lung resections)
-

Chris Sanchez
·
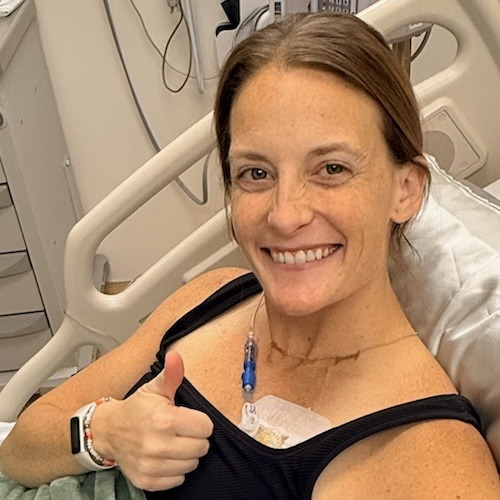
Living Every Breath: Megan’s Stage 4 ALK+ Lung Cancer Experience as a Young Mom
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic) Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain Treatment: Targeted therapy (lorlatinib)
-

Chris Sanchez
·
James Faced Recurrent Hodgkin Lymphoma While Becoming a Dad
James B., Relapsed Hodgkin Lymphoma Symptoms: Night sweats, itching, persistent lump in neck Treatments: Chemotherapy (ABVD, ICE, and BEAM), autologous stem cell transplant
