Cindy’s Stage 4 Diffuse Large B-Cell Lymphoma (DLBCL) Story
Interviewed by: Alexis Moberger
Edited by: Katrina Villareal

Cindy was diagnosed with stage 4 diffuse large B-cell lymphoma (DLBCL) in April 2021 and concurrently battled COVID.
About a month before getting diagnosed, the palms and soles of her feet started getting itchy. Later on, her skin started turning yellow and she was feeling sluggish. Since she never got sick, she didn’t think anything of it until her eyes turned yellow as well.
She took herself to the ER and there found out that her bile duct was completely blocked, in which they performed surgery to put a stent in.
Not long after, she tested positive for COVID and had double pneumonia and super pneumonia. To give her lungs a break, she had to be intubated, not realizing the severity of her condition.
Her oncologist was so relieved upon seeing her in his office since not all patients have the same outcome as her. Once she started treatment, the tumors started shrinking immediately.
She shares her journey going from being extremely healthy to getting diagnosed with cancer and getting COVID, how she had to relearn breathing, swallowing, walking, and talking, and her spiritual journey while she was in the ICU.
In addition to Cindy’s narrative, The Patient Story offers a diverse collection of diffuse large B-cell lymphoma (DLBCL) stories. These empowering stories provide real-life experiences, valuable insights, and perspectives on symptoms, diagnosis, and treatment options for cancer.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Name: Cindy M.
- Diagnosis:
- Diffuse Large B-cell Lymphoma (DLBCL)
- Staging:
- 4
- Initial Symptoms:
- Itchy skin on the palms and soles of feet
- Yellow skin and eyes
- Treatment:
- Chemotherapy: R-CHOP
- Neulasta
- Neupogen
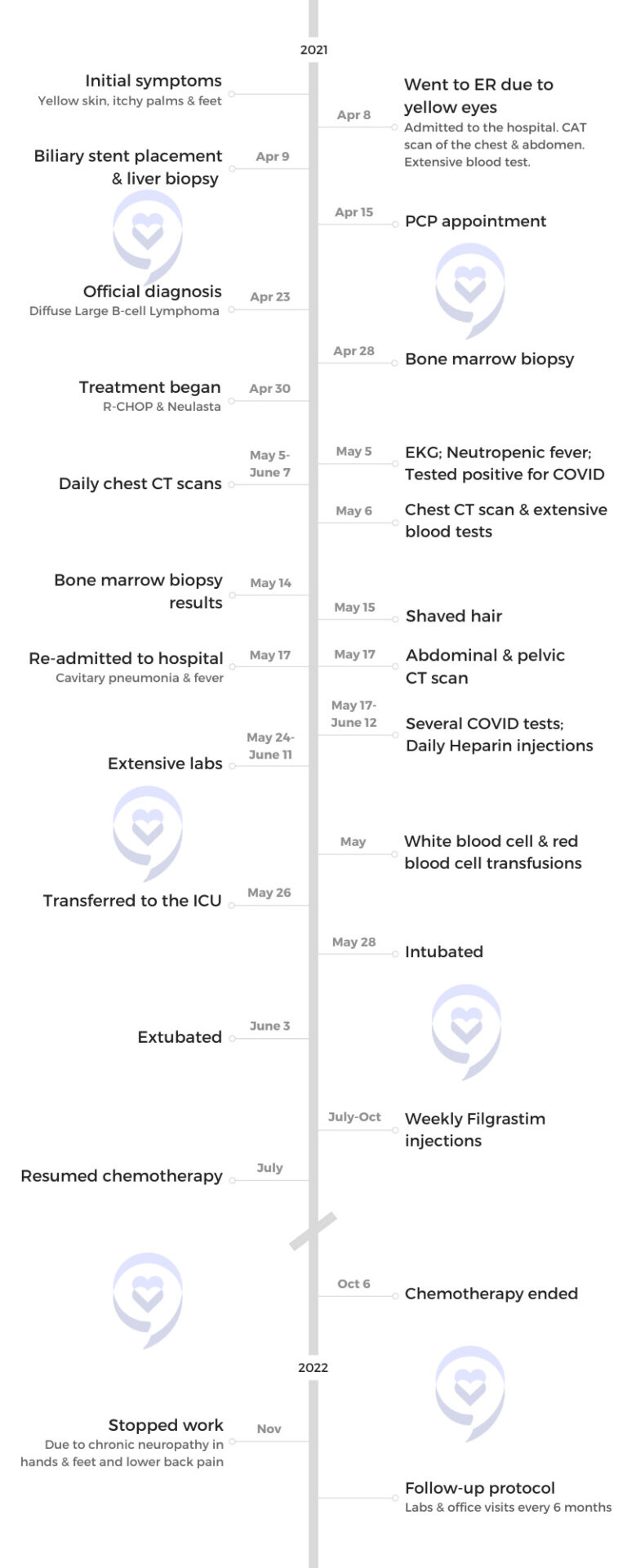
Introduction
I am retired so I’m no longer working. I have a couple of kids and six grandkids.
I have a couple of dogs that keep me as companions. I’m in remission now from the diffuse large B-cell cancer.




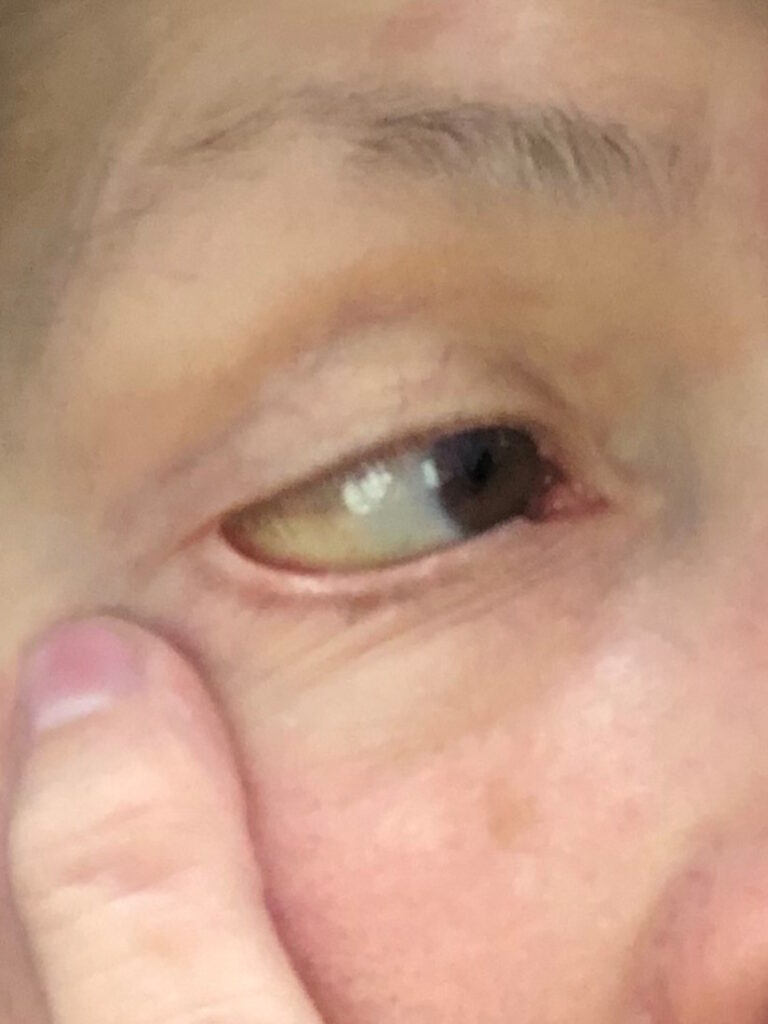
Pre-diagnosis
Initial Symptoms
I was diagnosed in April 2021. The skin on my palms and soles of my feet started to get itchy maybe a month before. I thought it was dry skin because it was still winter. I ignored it because I was in extremely good health. I never get sick.
My skin started turning yellow a couple of weeks later. I made an appointment with my primary care physician. I was a little sluggish and tired, but I wasn’t sure why. I thought I was working too hard so I ignored those. I told myself, “If my eyes turn yellow, I’ll go in.”
They turned yellow so I took myself to the ER, called my kids, and let them know. My daughter came to join me. They did blood tests and CAT scans. They came up with this horrible diagnosis that I was going to die from some rare type of cancer. They didn’t even know what it was.
I didn’t have time to process. I didn’t realize I was that sick.
They called a GI specialist who came in and did an endoscopy. That’s when they determined I needed to do surgery immediately because my bile duct was completely blocked.
They asked for a urine sample. The urine was red so it wouldn’t have been much longer and I would have been dead in the next couple of days.
Diagnosis
Reaction to the Diagnosis
I didn’t know anybody in my family who got diagnosed with what I exactly had. There was one tumor around the bile duct and one in the liver hiding.
It was surreal. I’d been extremely healthy. I didn’t get colds, flu, or anything. It was a shock.
I didn’t have time to process. I didn’t realize I was that sick. I went to the ER, got the surgery, got blood work, saw the oncologist, and started treatment the following week.
>>>MORE: Common Lymphoma Symptoms
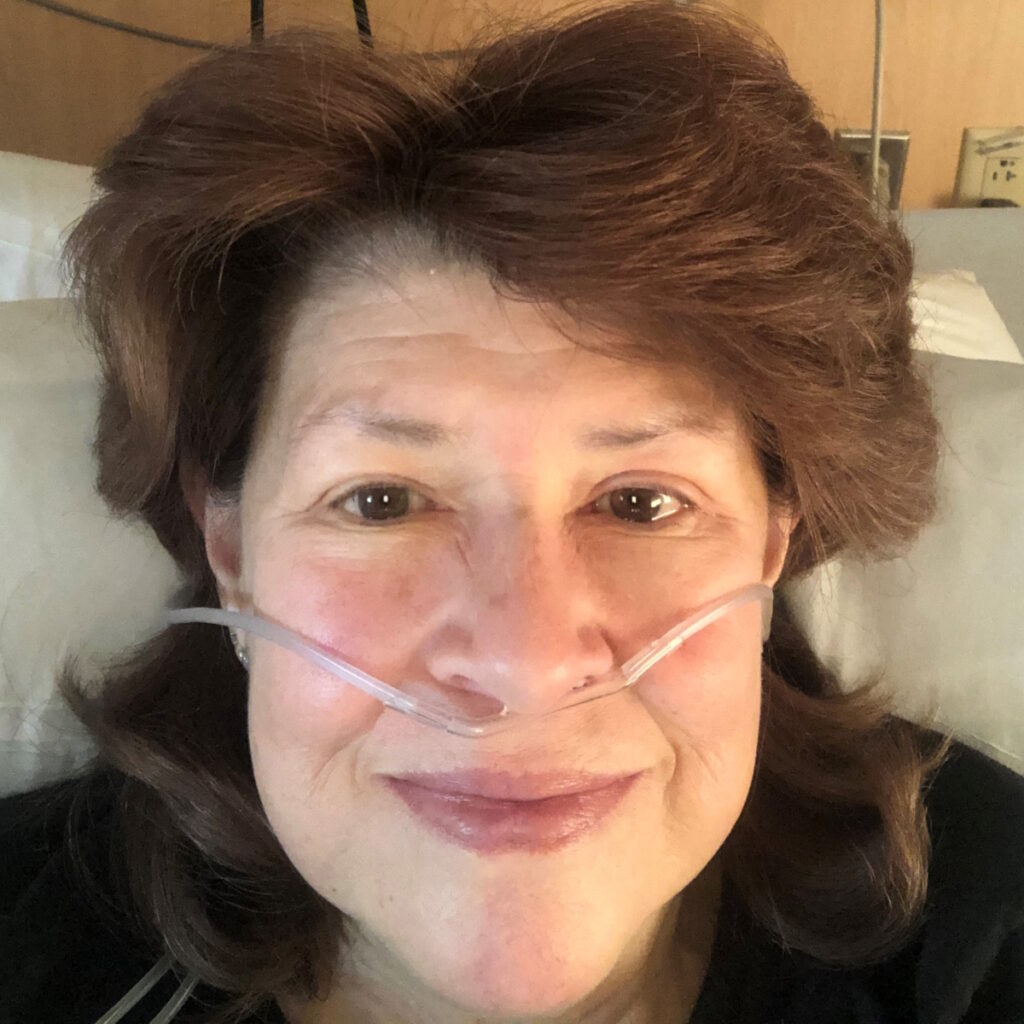
I didn’t know what to expect. I didn’t even know what this cancer was. I couldn’t sleep so I watched TV a lot at night. I saw an infomercial about the type of cancers that Roundup was causing and they said, “Call one of our lawyers.” They took my case like nothing.
It’s been an interesting journey getting that sick. Honestly, even when I got out of the hospital, I never really thought I was that sick. It wasn’t until maybe six months later that it sunk in. Even when I had to learn how to walk, talk, and all that, I thought it was normal, but it’s not.
Those were challenges that I had to go through, but I stayed positive. I didn’t question anything and did what I was told. The way I looked at it, I’ll be okay by Christmas and be able to be with my family. That was my goal and that’s what I cared about. That’s what got me through everything.
I didn’t know what to expect. I didn’t even know what this cancer was.
Biliary Stent Placement
After they put the bile stent in, I started to get my color back.
Appointment with Oncologist
They scheduled me for an oncology appointment. When I saw the oncologist, he was very real. He said, “I can cure this hopefully in 6 to 8 treatments.”
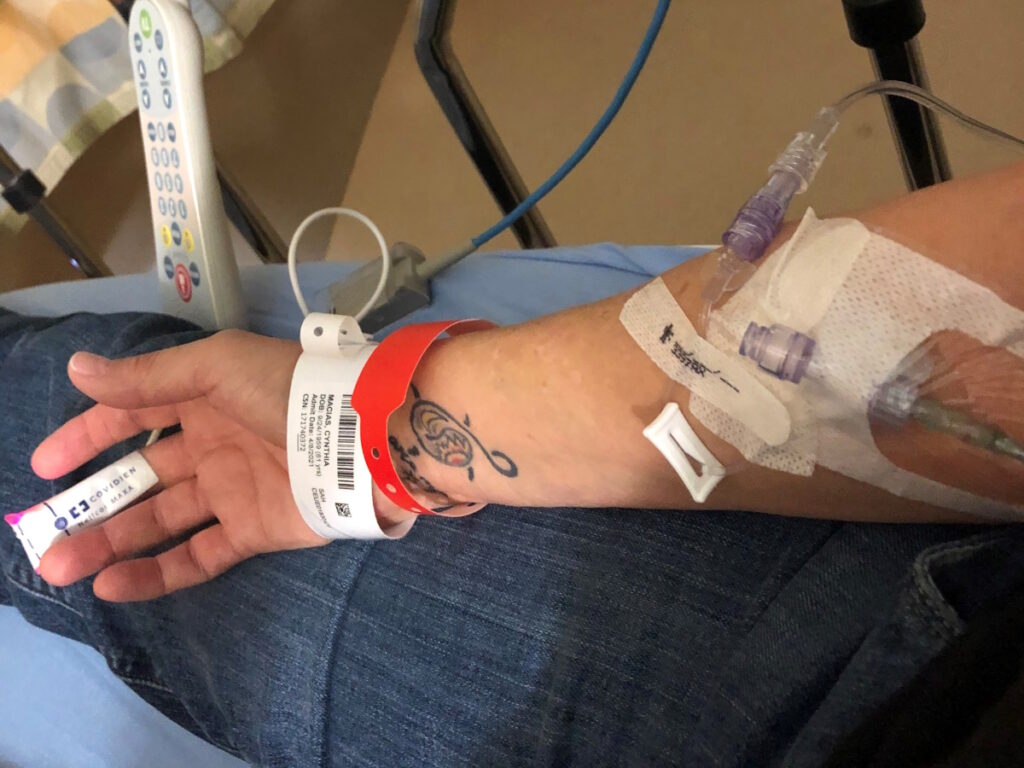
He asked if I had any questions. My daughter, poor thing, was crying her eyes out. I felt bad for her. What I heard was that I can be cured. What she heard was a death sentence because she heard chemo.
I asked if I was going to lose my hair. He said yes. She cried more. I said, “It’s just hair. It grows back. It’s not a big deal. Who cares?”
My other question that she couldn’t believe I asked was, “Can I still drink beer?” I like beer. He said, “Yeah, two a week.” He knows once you get on chemo, who wants a drink? You’re sicker than a dog.
They did blood work the week before I saw the oncologist and he explained what type of cancer it was and what type of chemo they were going to do. They have you watch videos, give you pamphlets, get the port put in, and start getting you hooked up.
My daughter asked, “If she doesn’t do chemo, how long will she last?” He said, “She’ll be dead by July.” It was that aggressive and I didn’t know. I was always against chemo, but when you’re in that position, you change your mind real quick. If that’s what’s going to save my life, so be it.



Testing Positive for COVID
I tested positive for COVID. My lungs were acting up, but they still sent me home only to come back three days later and be admitted for a month. I was intubated in between that time because the COVID was so bad.
If I never had chemo, I could have been okay with COVID. I never got sick. This is new to me so I didn’t know I was that sick.
I was rolling with the punches. I slept all the time. That was all I could do. I had no energy.
My lung capacity was going way down and I was on oxygen, but it didn’t concern me. I thought that I’d snap out of it sooner or later. Even when they said they needed to do a transfusion, it didn’t concern me.

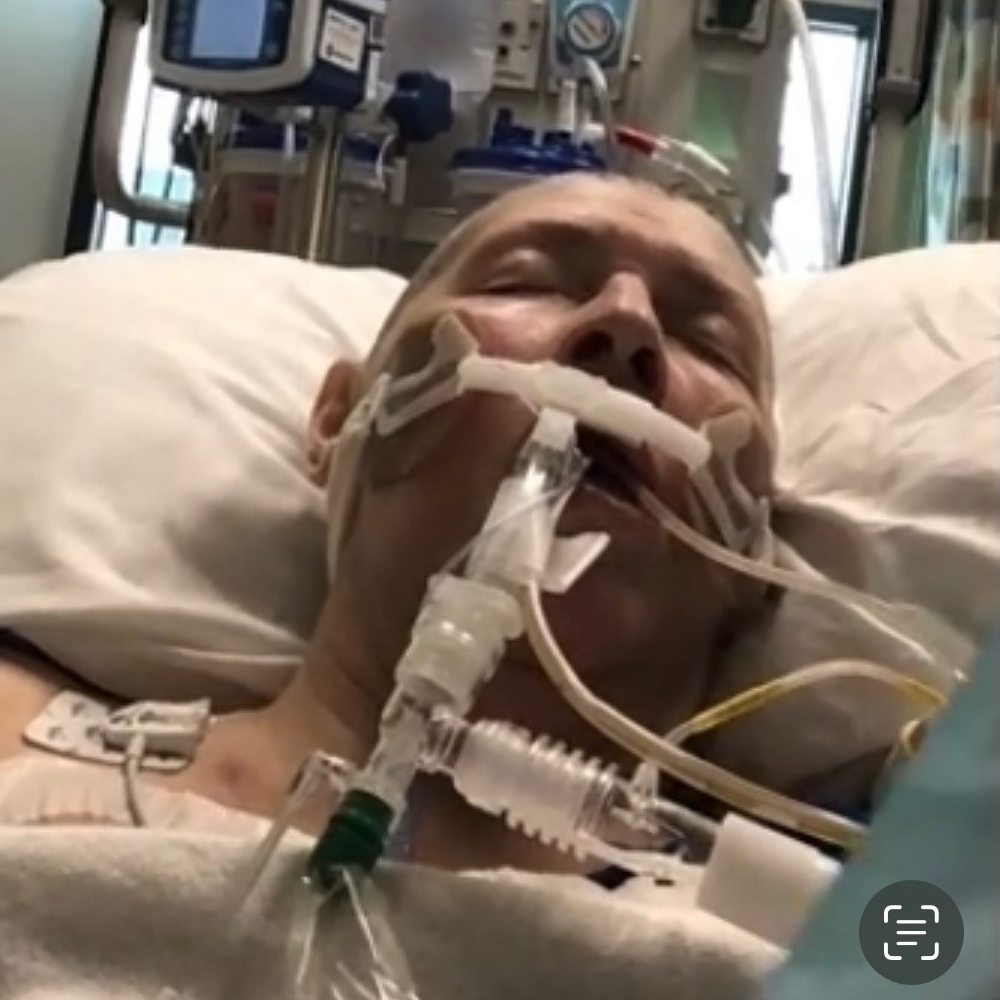
Getting Intubated
On my daughter’s 40th birthday, they woke me up and said, “We need to intubate you. We need to give your lungs a break.” As far as I was concerned, it had to sign the document and that’s all it has to be.
I could barely talk. My daughter planned a trip to Mexico and I kept trying to tell her, “Go on your trip. There is nothing you can do for me.” She was so emotional that I didn’t think she could hear what I was saying.
The next thing I know, I’m intubated. I remember waking up and being tied because I tried to pull it out, but I don’t remember that.
I remember waking up one time and biting it nervously. It’s an ordeal to be on a breathing tube. Nobody wipes your saliva so it goes down the back of your neck. Your nose runs and nobody cleans it. Your lips are severely chapped.
They do bathe you. Thank God for the port because that’s how they fed me.
My lung capacity was going way down and I was on oxygen, but it didn’t concern me. I thought that I’d snap out of it sooner or later.
Spiritual Journey
The things that I remember were crazy. During one of those times, I believed I was going to die because I saw my body float past the stars to the universe. I could see around the world.
I saw people from Saudi Arabia praying. I saw my friends and relatives who were Catholics praying with candles and my other cousins who were in two different congregations. My kids’ dad, who was Native American, was doing a ceremony in a teepee. All of these people were praying.
Seeing those woke me up to the things that I took for granted like breathing, walking, talking, and swallowing, which I all had to relearn.
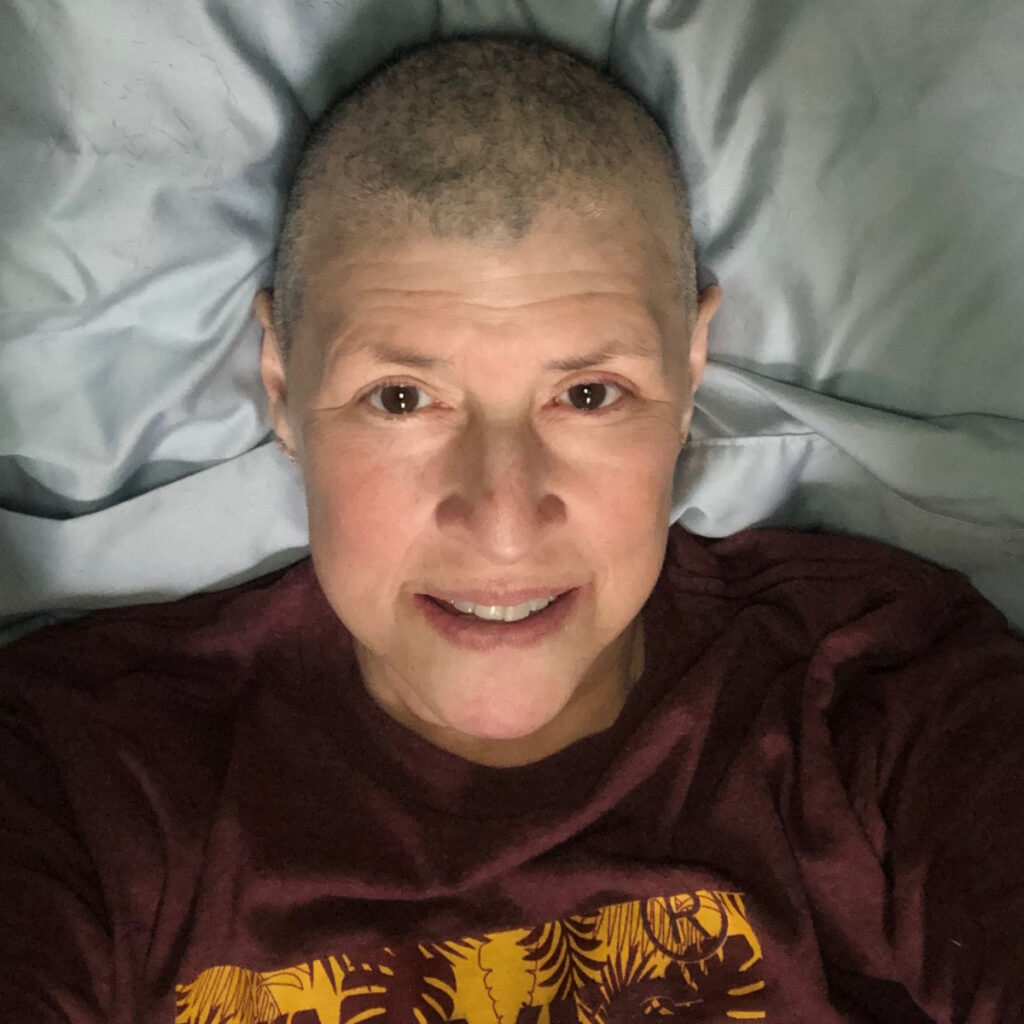
When I felt myself slipping, I prayed. All that came back to me. Am I religious? No, I’m more spiritual. But I was asking the universe, God, anybody, “Just let me live. I’ll figure it out from there.”
I begged for my life that night. I woke up and the sun was out. I was so grateful. I wasn’t out of the woods.
When I could talk, the first thing I asked my daughter was, “Did your dad do a ceremony for me?” She said, “How did you know?” I said, “Because I saw it.” I asked my two cousins, “Were you guys praying for me? Each one of your congregations?” They said yes.
The one that stumped me was Saudi Arabia. I don’t know anybody there. I told my father about it and he said his wife’s daughter married Saudi Arabian. They live there and they told them so their whole congregation was praying. That’s what I saw.
When I felt myself slipping, I prayed. All that came back to me.
Getting Off the Ventilator
They tried to get me off the ventilator. I couldn’t talk, but they put me on a Zoom video call with my daughter. They put the phone on my chest and all I could hear was, “You breathe the same air that we breathe, Mom. They’re going to take you out tomorrow. Take deep breaths. You’re going to be fine.”
The next day, they said, “We’re going to take you off. Honestly, the worst thing is the stickers on your face that hold the breathing tube.” I didn’t feel the breathing tube coming out. They were too busy sticking their fingers in my mouth and checking that I didn’t crack my teeth.
The nurses loved my bald head. They’d come by and rub it all the time.
Recovering from COVID
It’s been an interesting journey being shut in because COVID was really bad. I had no immune system. I didn’t dare go to a store. I didn’t go anywhere out of the house except to the doctor’s visits or blood work. I was very cautious. I never want to be that sick again.
I had a double pneumonia and a super pneumonia from COVID so my lungs are scarred. Can I handle another pneumonia? I don’t know and I don’t want to find out.
My mother was very sick when I was a child. She had heart disease so she was intubated several times. We saw that and she came out of it every single time. To me, when he said they were going to intubate me, it didn’t scare me. I thought I’d be fine.”
My kids couldn’t understand that. You hear people dying from COVID, but in my mind, I’m going to come out of it. I’m going to be okay somehow.


Treatment
Getting back to the oncologist, I was determined to get off the walker and walk into the oncologist’s office with no cane and I did do that. He was so incredibly happy to see me. He kept saying, “So good to see you, my friend. So good to see you. I watch your chart every day hoping you weren’t going to die. When do you want to start chemo?” I looked at my daughter, “Why is he asking me that?” She said, “Do you not have anybody like my mom?” He said, “No, they all died.”
I want to get on with treatment as soon as possible because I want to get on with my life. His being concerned that the cancer was so aggressive scared me a little. I figured I had already gone through the worst. Plus I was trying to get my strength back.
I’m grateful to my children for being here, taking care of me, cooking my food, and helping me. You lose so much strength and muscle. Taking a shower is horrendous. It’s an energy sucker. I had to learn all these things a little at a time.

Side Effects of Treatment
Five days after treatment, I got neutropenia. I ended up in the hospital for a week.
I only had one chemo after coming out of the hospital so it did make me tired but not more tired than what I had already been through.
I never got nauseated, which was a good thing. I did get neuropathy so now I have chronic neuropathy. I have chronic lower back pain. I don’t know what to contribute that to other than being in the hospital for so long and staying in the same positions plus the shortage of nurses to turn you when you’re in ICU.
The last chemo kicked my butt. That left me weak for weeks.
I want to get on with treatment as soon as possible because I want to get on with my life. His being concerned that the cancer was so aggressive scared me a little.
Follow-up Scans
The tumors were starting to shrink very fast. They were almost gone on the first treatment, but he wanted to do two more to make sure.
Right now, their only concern is a small lesion on my liver. They don’t know what it is. It’s staying steady, but it’s still there.
Some of my blood work for the liver is still high and we don’t know why. The liver could be damaged, probably from the chemo. I don’t know how long it takes to recover. The last scan I had still shows the lesion.
He may want to do a liver biopsy if it shows up again in six months. It might be scar tissue.


Life After Cancer
I hadn’t been out in so long that I didn’t even know what’s what anymore. There’s so much new development.
I went to play darts once and in the back of my mind, I got freaked out that I was around a lot of germs, but my counts were pretty good so I felt okay. It’s summertime and the doors are open.
In the fall, I’m not going anywhere. I do believe that my immune system is better. My granddaughter comes over and she’s been sick twice but I didn’t so I must be doing okay.
I don’t want COVID again. That put the fear of God in me. I don’t even know if I can handle the flu. It’s an interesting journey going from being extremely healthy to this crazy cancer because that never ran in my family.
They said I had to relearn to swallow; that’s part of having the breathing tube. I thought they were kidding me, but they didn’t lie because I tried to swallow Jell-O and it freaked me out. Even today, I have problems swallowing.
I have to chew my food in tiny little bites because I’ll choke. They can stretch it if they want to, but I don’t want to do that because I’ve had so many surgeries and procedures.


Staying Positive
Being positive is the key to anything, regardless of what you do in life. I never asked why me because why not? Why not me?
Words of Advice
Stay positive. It’s okay to get angry, but don’t dwell on it.


Try not to feel sorry for yourself because it’s not going to do any good. You’re going to give cancer the advantage. Go in with the attitude that you’re going to kick its butt. They give you all the tools to kick its butt.
Know that you’re not alone. It’s unfortunate, but you’ll get through it. There’s no reason not to.
I had a rare cancer. They told me I was going to die, but I thought to myself, No, I’m not because you don’t know me. I’m not going to die. I don’t care what kind of cancer you say I have. It’s not going to happen.
Be positive and know yourself. I’m pretty stubborn so that helps.
I’m alive and kicking. My grandkids and my dogs are happy. I get so excited to see a full moon or the leaves change. I appreciate life.


Inspired by Cindy’s story?
Share your story, too!
More DLBCL Stories
Anna M., Diffuse Large B-Cell Lymphoma (DLBCL), Stage 4
Symptom: a rRapidly growing, painless lump on the breast
Treatment: Chemotherapy
Ashley P., Diffuse Large B-Cell Lymphoma (DLBCL), Stage 4
Symptoms: Feeling like holding breath when bending down or picking up objects from the floor, waking abruptly at night feeling “off,” one episode of fainting (syncope), presence of a large mass in the breast
Treatments: Chemotherapy, bridge therapy of chemotherapy and radiation, CAR T-cell therapy
Melissa B., Relapsed Diffuse Large B-Cell Lymphoma (DLBCL)
Symptoms: Lump in the left breast, persistent rash (started near the belly button and spread), intense fatigue and energy loss
Treatments: Chemotherapy (R-EPOCH), Neulasta, radiation therapy, surgery (to remove scar tissue and necrosis), autologous stem cell transplant
Jen N., Diffuse Large B-Cell Lymphoma (DLBCL), Stage 4B
Symptoms: Blood-tinged phlegm, whole-body itching, shortness of breath, lump near collarbone, night sweats, upper body swelling, rapid weight loss
Treatments: Chemotherapy, immunotherapy, lumbar puncture, autologous stem cell transplant







Leave a Reply