-

Chris Sanchez
·
Bile Duct Cancer at 27: Morgan’s Path to Answers, Care, and No Evidence of Disease
Morgan O., Bile Duct Cancer (Intrahepatic Cholangiocarcinoma) Symptoms: Fatigue, nausea, severe abdominal pain, dark urine, itching, clay-colored stool, significant weight loss, jaundice Treatments: Surgeries (liver resections), chemotherapy
-
Adrenalectomy, Axitinib, Belzutifan, Clear Cell Renal Cell Carcinoma, Hypoxia-inducible factor-2 alpha inhibitor, Immunotherapy, Keytruda (pembrolizumab), Kidney Cancer, Metastatic, Nephrectomy, Patient Stories, Radical nephrectomy, Renal Cell Carcinoma, Surgery, Targeted Therapy, Treatments, Tyrosine kinase inhibitor (TKI)
-

Chris Sanchez
·
Tongue Cancer at 37: Brittany’s Misdiagnosis, Major Surgery, and Finding Her Voice Again
Brittany Z., Tongue Cancer (Squamous Cell Carcinoma of the Tongue and Lymph Nodes), Stage 4 (Metastatic) Symptoms: Painful tongue rash, loss of mobility, severe ear pain Treatments: Surgeries (partial glossectomy, lymphadenectomy, tonsillectomy, tracheostomy, feeding tube placement, tongue reconstruction), radiation therapy, chemotherapy (cisplatin)
-
Chris Sanchez
·
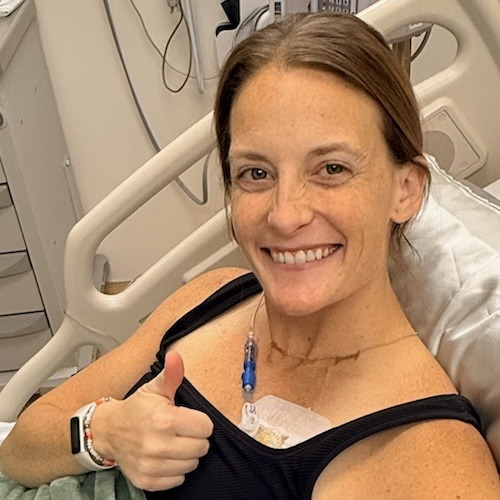
Kelsey’s Stage 4 EGFR+ and ALK+ Non-Small Cell Lung Cancer Story
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic) Symptoms: Severe back pain, falling due to collapsed spinal vertebrae Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
-

Chris Sanchez
·
Kalei’s Stage 4 Rectal Cancer Story: Has My Cancer Returned?
Kalei M., Rectal Cancer, Stage 4 (Metastatic) Symptoms: More frequent bowel movements, presence of mucus, tissue-like substance, and blood in stool, stomach cramping and sharp pains Treatments: Radiation therapy, chemotherapy (FOLFOX), surgeries (two lung resections)
-

Chris Sanchez
·
From Losing His Appetite to Stage 4 Colon Cancer: Joe’s Story
Joe C., Colon Cancer, Stage 4 (Metastatic) Symptoms: Loss of appetite, fatigue, malaise, severe pain in the abdominal/liver area, back and shoulder pain, lightheadedness Treatments: Surgery (colon resection), chemotherapy (FOLFOX, capecitabine, FOLFIRI), targeted therapy (panitumumab, a monoclonal antibody), radiation therapy, immunotherapy through a clinical trial
-

Chris Sanchez
·
From a Small Cut to Tongue Cancer: Katelynn’s Story
Katelynn R., Tongue Cancer (Squamous Cell Carcinoma of the Tongue), Stage 3 Symptoms: Ulcer on the side of the tongue, loss of appetite, extreme weight loss, fatigue, severe right ear pain and pressure Treatments: Surgeries (hemiglossectomy, radial forearm free flap, radical neck dissection, lymphadenectomy, tracheostomy, skin graft surgery), radiation therapy
-

Chris Sanchez
·
Hodgkin Lymphoma at 18: Kate’s Experience of Faith, Fertility Fears, and Finding Her Voice
Kate H., Hodgkin Lymphoma (Nodular Sclerosis), Stage 2 Symptoms: Severe persistent cold, shortness of breath during athletic activity, pale itchy skin, appearance of a lump in the neck Treatments: Chemotherapy (ABVD and ICE), autologous stem cell transplant


