Tongue Cancer at 37: Brittany’s Misdiagnosis, Major Surgery, and Finding Her Voice Again
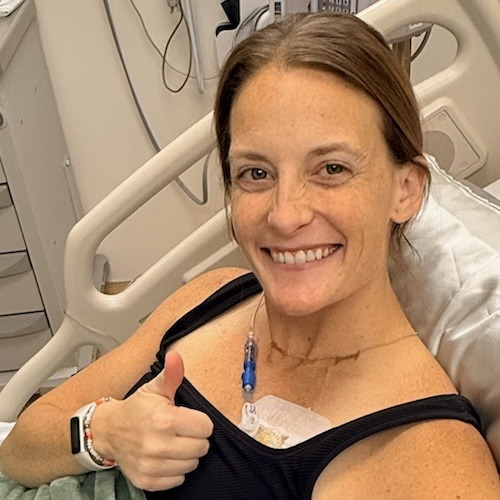
Brittany’s tongue cancer experience began with a simple moment at the bathroom sink and turned into a fight for her own diagnosis, survival, and identity. She was 37, newly married, and thriving as a project manager, actor, and burlesque performer when she noticed a red patch on the side of her tongue and severe ear pain that felt like an infection. Over the next five months, she was misdiagnosed multiple times, dismissed as being “too young for cancer,” and even accused of seeking pain medication, all while the pain intensified and a hidden tumor under her tongue made eating nearly impossible. She lost 35 pounds and watched her body change dramatically before an ENT finally took her seriously, ordered imaging, and confirmed squamous cell carcinoma of the tongue (tongue cancer).
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
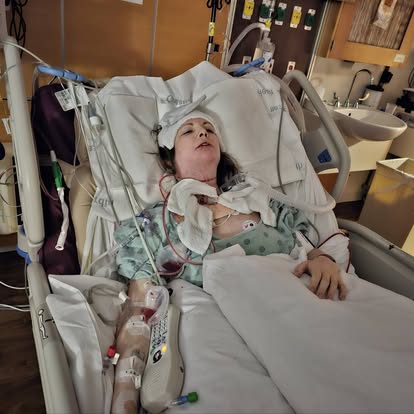
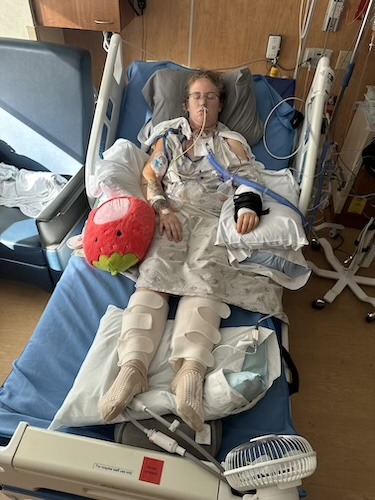
By the time Brittany reached Dr. Michael Moore at Indiana University, the tongue cancer had spread to her lymph nodes. Her team moved quickly. She underwent a 12-hour surgery that removed 70% of her tongue and 22 lymph nodes. Surgeons reconstructed her tongue using tissue from her back, installed a percutaneous endoscopic gastronomy or PEG feeding tube, and performed a tracheostomy so she could breathe while she healed. Later, she went through 33 rounds of radiation with a tight immobilizing mask and six weeks of weekly chemotherapy. Complications like a neck fistula, profound weight loss, and persistent side effects layered onto the already intense treatment.

Recovery meant beginning again with basic functions. Brittany now works closely with a speech therapist twice a week to relearn how to speak, swallow, and manage food safely. She uses tools to stretch her jaw, practices step-by-step swallowing techniques to reduce the risk of aspiration, and celebrates small but meaningful wins, like the first time she managed to eat Oreos dunked in milk. Socially, she navigates the emotional impact of not being able to eat like others, living with scars, a feeding tube, and a voice that sounds different than before.
Through all of this, Brittany’s transformation is not about becoming someone new but recognizing who she has always been. She describes herself as a “chatterbox” who loves people and connection, and she’s leaned into that strength. Today, she does speaking engagements on side effects, self-image, and self-advocacy, participates in support groups at Indiana University, and hopes to speak at future head and neck cancer symposiums. She urges others to advocate for themselves, ask for help, and remember that “no one can navigate cancer alone.” Brittany has also started blogging about her experience, hearing from readers who feel less alone because of her honesty. She emphasizes that life can even be better after cancer, and encourages patients to seek out community, patient advocates, and peers who truly understand what they’re going through.
Watch Brittany’s video and read the edited transcript of her interview below.
- Self-advocacy can be life-saving; she was misdiagnosed for nearly five months and believes that insisting on more opinions is the reason she’s still here.
- Tongue cancer and head and neck cancer treatments affect every part of life, including speech, eating, weight, appearance, work, and relationships; not just the tumor site.
- A universal truth for patients: no one can navigate cancer alone, and support from loved ones, peers, and professionals is essential for both physical and emotional healing.
- Brittany’s transformation is about reclaiming her voice and purpose. She’s moved from being a performer to a patient advocate, speaker, and blogger who helps others feel seen.
- Trauma from delayed diagnosis and aggressive treatment can coexist with hope; she reminds others that life can even be better after cancer and that small milestones (like eating a favorite cookie) matter.
- Name: Brittany Z.
- Age at Diagnosis:
- 37
- Diagnosis:
- Tongue Cancer (Squamous Cell Carcinoma of the Tongue and Lymph Nodes)
- Staging:
- Stage 4
- Symptoms:
- Painful tongue rash
- Loss of mobility
- Severe ear pain
- Treatments:
- Surgeries: partial glossectomy, lymphadenectomy, tonsillectomy, tracheostomy, feeding tube placement, tongue reconstruction
- Radiation therapy
- Chemotherapy: cisplatin
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Life before my tongue cancer diagnosis
- From being a performer to losing 70% of my tongue to tongue cancer
- My first tongue cancer symptoms and early red flags
- Five months of misdiagnosis and severe pain
- Trying to function while in debilitating pain
- An ENT finally believed me
- Partnering with doctors and speaking to other patients
- Hearing “You have tongue cancer” as a newlywed
- The devastation of delayed tongue cancer diagnosis
- The details of my 12-hour tongue cancer surgery
- Waking up after a tracheostomy and with no voice
- Relearning how to speak, eat, and swallow
- 33 rounds of radiation and weekly chemo
- Complications: Fistula, weight loss, and “If it’s not one thing, it’s another”
- Self-image and body image after tongue cancer
- What tongue cancer taught me about myself
- My biggest advice for tongue cancer and head and neck cancer patients
- Finding community, blogging, and patient advocacy
Life before my tongue cancer diagnosis
My husband and I met in 2022. His name is Mason, and we met in a murder mystery dinner theater. We were both on the house staff. I was divorced, and I was just like, “I’m going to do what I want to do,” so I joined the cast. And so I’ve been a project manager for years, and was with a company and lived in San Diego at the time.
I also had my own burlesque show in San Diego. So if I wasn’t in dance class, I was producing a show, making a costume, or something like that. So the majority of my time was working, acting, and burlesque. And then my husband and I met, and he rounded me off.
We are tiki bar enthusiasts and karaoke enthusiasts. So if we went out, we were at a bar and just having a great time. So that was pretty much life before this.
From being a performer to losing 70% of my tongue to tongue cancer
I actually started doing speaking engagements now, and what I focus on a lot is side effects and self-image. Cancer affects everyone. In my support group, there are a lot of older people, but that’s not all it is. It’s young people as well. I’m 38, and I was diagnosed at 37.
For me, the biggest part came before. I was actually misdiagnosed four times for many months. So my tongue became very painful, and I couldn’t eat, and I dropped 35 pounds. People don’t realize how much your tongue helps you to eat. So I’m actually learning how to swallow. I still have a feeding tube as well, but that kind of abolished a burlesque career.
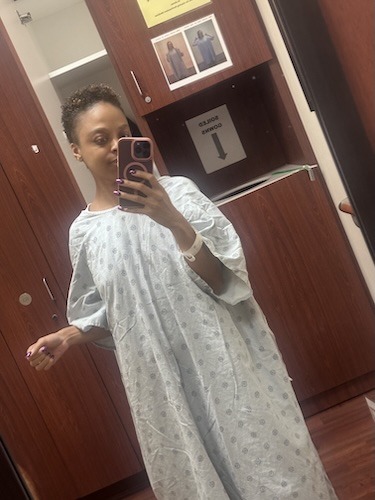
I have a tube in my stomach. My neck looks very different. I look very different. I’m 35 pounds lighter. My body is different. I say sometimes I feel like a stranger still when I look in the mirror. There are a lot of scars. For most tongue cancers, they will take tissue from other parts of your body to reconstruct. So for me, it was on my back. I actually tattooed over it, but I don’t look the same.
You don’t feel the same during treatment. So having the energy to do those things is just nonexistent. It’s a completely different life.
My first tongue cancer symptoms and early red flags
I was brushing my teeth. I was like, “Oh, my tongue hurts.” At first, I was like, “Did I bite my tongue?” I was looking at it, and I noticed I almost had a red patch on the side. It was exactly down the right side. I was like, “Oh, that’s bad. I should probably make a doctor’s appointment.” By the time I got to that doctor’s appointment, if I stuck my tongue out, it went to the side. I was like, “Oh, that can’t be good.” Everything for me was on the right side.
I started getting insane ear pain, like down inside my ear in here. I’ve heard that for a lot of people, that’s one of the first symptoms. It was like, “Do I have an ear infection?” That’s what it felt like.
So I went in. I actually went to urgent care, and they told me I had shingles, but they were inside my mouth. Oh, that makes sense. So they gave me medication. It didn’t get better; it got worse. So I went back. I went back twice. First, I was actually told I was just looking for pain meds, and they kicked me out essentially. I was like, “No, something is really wrong.”
I stuck out my tongue, and then finally the doctor was like, “You should see an infectious disease doctor because of the rash.” She wasn’t sure. She did some bloodwork. Nothing came back. And then finally I saw an ENT, and she poked the side of my tongue, and I literally got up out of the chair and was across the room in pain, this blinding pain. She said, “We are going down for an MRI.”
So they put me on the elevator, walked me downstairs, and moved everyone else out of the way. I had an MRI and a CT scan. She biopsied me the next week and confirmed that it was cancer.
Five months of misdiagnosis and severe pain
Awful. It was almost five months. And it got more and more and more painful. There was a tumor, tongue cancer, under my tongue. I couldn’t see it. Anytime I would try to put food in my mouth, the pain would literally radiate up my head, like through my forehead. I was like, “Something is not okay.” I felt very close to death.
When I finally got to surgery, they actually didn’t know if I would survive surgery, just because I had dropped so much weight so quickly, and I had no nutrients in my body. My eyes were actually sinking into my face, and even my friends tell me now they were very worried about me even making it through the surgery. They weren’t sure.
Trying to function while in debilitating pain
I was actually looking for jobs at the time, both remote, but we bought a house and immediately had some big house troubles. So I took on an extra job because I needed to pay to have those problems fixed. But I would sit here in my office and just cry because I couldn’t do anything else.
I went to the emergency room once because the pain was so bad. They gave me some pain meds and an IV and sent me home. They didn’t do anything. Everyone thinks that you’re trying to get pain meds. But I knew something was wrong with me. They were saying, “Oh, no, it can’t be something bad like cancer, you’re too young.”
That’s just not true. Even now, it’s all ages, and it’s happening more and more in other people. Someone I know named Beth, who has cancer, is younger than I am. It happens with people in their 20s. Now I see it all the time from making connections and friends online. It doesn’t discriminate against your age.
An ENT finally believed me
Oh my gosh, it was such a relief. She did a scope on me as well, and she said, “I don’t like it. I don’t like the way that looks.” So we went immediately to the MRI, and then she set me up in just a few days with a biopsy.
I woke up from the biopsy, and everyone in the room was crying. So I was like, “Oh, this isn’t good.” My ENT said, “You have to get out of here and go to Indiana University. There’s an oncologist there, Dr. Moore, Dr. Michael Moore, and if I had cancer, he’s the person that I’d go to.”
I was like, “Oh my gosh, we have a plan now. Someone is taking it seriously.” She referred me to Dr. Moore, who saved my life, who is amazing, who got me in for surgery within two weeks, and said, “I’ll do everything I can.” If it weren’t for him, I would be dead, absolutely. I owe him. I tell him this all the time.
He’s just a great buffer, and he’s a great person. When we finally get into the hands of someone like that, it’s like there’s a glimmer of hope. “Finally, someone’s going to help me, and we can take a breath for the first time in all of it.”
Partnering with doctors and speaking to other patients
I really appreciate Dr. Hansen, too, the doctor who finally took me seriously. If it weren’t for those two, I wouldn’t be here. Both of them are wonderful about being like, “I’m the doctor, I can treat you, but I don’t have tongue cancer. So I will point you to places that support you because I’ve not been through it.”
I appreciate that too, because it’s like, “I can see you, I know how to treat you, but I don’t know how it feels.” Dr. Moore and I might actually pair up now, and I come in and speak to the pre-op patients because he’s like, “You’ve had it, you’ve done it.” I appreciate that he does that. Doctors throw a lot of information at you, and then it’s like, “Okay, are you ready?” And I’m like, “No, I’m not.” Talking to someone who’s been through it is just invaluable.
Hearing “You have tongue cancer” as a newlywed
I was absolutely overwhelmed. When you get a cancer diagnosis, I feel like your brain just shuts off to protect yourself in a way. I went through all of that to get here, and now that was just the start of something else. Everyone is different.
For me, the tongue cancer had already gotten to my lymph nodes as well. I had no idea, but I didn’t know if I was going to live. My husband and I had been married for two months when I got the news, and the only thing I could think of was that there hadn’t been enough time to love him properly. Is this the end of it with us here?
I felt that way for my friends and my family, too. That’s what I thought of first. It just hasn’t been enough time to tell all these people how I feel about them. A positive that came out of it is that I don’t wait anymore to tell people, “I care about you, I love you.” I tell people how I’m feeling. I just don’t wait anymore.
In my case, the tongue cancer was so advanced that I didn’t get to make decisions. Decisions were made for me. “We will come in on this day, and we will have the surgery, and then we will have radiation, and then we will have chemo, and we’ll just do our best, but we don’t know how things will go.”
I appreciate the honesty. I want honesty. But it’s hard to know I don’t get to choose. It’s been chosen for me and scheduled, and now I have to do it. It feels very out of control and overwhelming. So those are really the two main emotions that I went through, even through treatment, like I just have to keep going because this is what has to be done.
The devastation of delayed tongue cancer diagnosis
I think about that all the time because I probably wouldn’t have had to have as much of my tongue removed as I did. And then also from PET scan to surgery was two weeks, and it went from not being in the lymph nodes to being in two of them. That’s how quickly this spreads.
So with cancer, you’re just racing a clock. I’m not going to lie, I was mad when everything happened because I was like, “If we had caught this sooner, I wouldn’t have gone through as much suffering, and my husband wouldn’t have been left with so much.” With cancer, time is everything. Even in a matter of weeks, they don’t know how far it’s going to get. So that is the part that was very devastating for me. It was hard to deal with for a long time.
That’s why I tell everyone, please advocate for yourself. You know when something is wrong. If I had not pushed and gone back and seen five doctors, I would not be here. You know yourself the best, and you know when something is not right. So advocate for yourself until you find the answer.
The details of my 12-hour tongue cancer surgery
My tongue cancer surgery involved removing all of my lymph nodes on the right side of my neck. So they did a neck dissection, and they went up through that to remove the tumor. They removed 70% of my tongue on the right side.
Then they did a tonsillectomy just for precaution. The tongue cancer wasn’t there, but it shows up there a lot if it spreads, so they took my tonsils out. Then they took tissue from my back here and reconstructed my tongue for me. They put in a PEG tube in my stomach because I wasn’t able to eat.
So: neck dissection, 22 lymph nodes out, 70% of my tongue removed, reconstructed with tissue from my back, tonsillectomy, PEG tube, and a tracheostomy. That was temporary, just because there’s so much swelling after that surgery.
Waking up after a tracheostomy and with no voice
A big part that people don’t realize is that you can’t breathe on your own after that. So it’s not only all this to your head and neck, but when you wake up, you’re dependent on a machine to help you breathe. To me, that was also super scary on top of everything else. Even knowing that it’s temporary, you don’t know how you’re going to wake up. They don’t know. Something can change in surgery as well. They have a plan, but they don’t know until they get in there what is actually going to happen.
When I woke up, I couldn’t speak either. My husband and I were writing to each other, and I was like, “What actually happened?” That saved me — finding out this is what happened in surgery, this was the plan, and then this was reality. Knowing 70% of my tongue is gone, in the hospital, they’d be like, “Make a sound.” I was like, “I don’t know if I can.” For that first bit, it was just spit and no sound.
There’s a while there where I thought, “What will normal look like after this? What will happen today?” You’re just at the mercy of everyone else, and that’s a terrible feeling, especially for me. I’m someone who very much needs certainty. I’m kind of a control freak. I want to know what’s happening. I want to have a say.
I say this happened to me in life to be like, “No, you don’t always get to have control, and you have to learn to sit with it.” Sometimes I say that was my life lesson through all of this: you have to slow down and give up some of the control.
I don’t have a lot of patience either. Going through this takes a long time to heal. This month is a year since surgery, and I’ve come a long way, but there are days when it’s like, “When is it going to be better or be okay?” You just have to roll with it and do the best you can. It is what it is.
Relearning how to speak, eat, and swallow
I actually have an amazing speech therapist. I see her twice a week, and we focus on different things. A lot of people don’t realize that with tongue cancer and head and neck cancer, there are radiation aftereffects. I can’t open my mouth all the way. So putting food in my mouth or spitting requires so much other facial structure as well as the tongue and the jaw, and so to do all of that, I’ve had to just start from scratch.
I have a lot of tools that manually stretch my mouth. I do exercises so I can hopefully speak a little bit more clearly. You don’t realize how much you use your tongue to eat. If I put food in my mouth, my tongue doesn’t move it. So how do you put that down?
So I’m taking tiny passes and moving it through enough to chew. Then I have a step-by-step process to swallow food or liquid now, because I can’t swallow and breathe at the same time, or I’ll aspirate. I’ve done that a lot of times now, but it’s things that you do on autopilot, and that’s not how it goes anymore.
Working with therapists and other therapists there, it’s trying to figure out what works for you, what’s worked for other people. Some people have prostheses to help them. Everyone is different, and then you have to make adjustments. For me, I have to use my face a lot more to speak so people will understand me. So it’s things like that. They have to figure out what works for you and sit through it.
All the things that they said beforehand that are just automatic are not automatic anymore, and that’s the toughest part. Life revolves around food. Food is comfort. You feel left out. You feel like you don’t belong. Even social situations are based around food. I’m lucky. Everyone around me is very accommodating. All my friends don’t treat me differently, but I have to remind them that I can’t eat like I used to.
It’s such a work in progress, and it’s a millimeter of progress. It feels slow, but if you look back on it, you’ve gone both sides without realizing.
33 rounds of radiation and weekly chemo
I did 33 rounds of radiation. That’s daily for six weeks. If you’re a head and neck cancer patient, you have to have this mask on, and that is a fresh hell that nobody prepares you for.
So they can pinpoint it, they put a mask on you and strap it down so they can be very precise. That was as bad as it sounds.
Then I had six rounds of chemotherapy. I was on cisplatin once a week for six weeks.
Complications: Fistula, weight loss, and “If it’s not one thing, it’s another”
I’m a small person. I’ve never been big. I’m 5’3″ and 100 pounds. I was like 130 pounds at my heaviest, so I don’t have a lot to work with. I had the surgery, and then they irradiated me, and then I had a fistula. So it opened up in my neck.
One day, they put me in the mask for radiation, and that had opened. They didn’t feel it, the fluid going down the back of my neck into the back of my shirt. Then they had to put a straw in it and drain it. It’s just, if it’s not one thing, it’s another. All that just compounds. Treatment compounds. That’s how it works.
Even when we’re done, it’s compounding. You still feel bad for a while. I just had every bad side effect you can have. I was like, I just have a bad case of the flu. I can’t do it. But it healed up. It was fine. But that day, I was like, “I don’t know what just happened, but something is wrong.” Then you have to take it from there and figure out what happened.
Self-image and body image after tongue cancer
I love our support group at IU. I spoke last month, and then I’m hopefully speaking at the Head and Neck Cancer Symposium this year.
A big part of it is the weight loss issues for anyone going through it, but for me, I have a PEG tube in my stomach, so I have that tacked onto myself all the time. I have a lot of scars on my neck and on my back as well, just from all the surgery. So it’s hard to see yourself so differently. I sometimes call this my second skin, because I feel like almost every part of me has changed.
Another thing people don’t realize is the way you speak. People take that as if you’re intelligent or not, or people think that I’m deaf, so they yell at me. Just having to explain yourself all the time — this is why I sound this way, this is why I have the scars, this is why all these other things. Sometimes it’s embarrassing or exhausting to be like, “Hey, this is why.”
I was a dancer before. I did burlesque. A big part of that was using my body to express myself. Now it’s not that I can’t do it; just for me, I’m not in a place to continue that at the moment. A lot of it is confidence. I’m not quite there.
I did a lot of acting before. I don’t sound the same. I don’t speak the same. Even getting a job is difficult. It touched every part of my life. It’s not just the self-image of surgery. It’s the self-image of how to express yourself, and now that’s so different. It’s not just the way it looks. It’s all of you.
You really have to figure out who you are at your core. What are the things about me that haven’t changed and won’t change? Navigating those things helps a lot — I’m still me under here, and the people who love you will still love you.
Being married, and being a newlywed, and now your body is completely different — my husband is amazing. He tells me I’m beautiful every day. But there was a time when he was like, “I’m afraid I’m going to hurt you or break you if I touch you.” That was very, very difficult. It’s not that he wasn’t attracted to me. He was legitimately worried about my body. He said, “I would never want to hurt you.”
People who hug me are like, “I’m trying not to hurt you.” You feel different, and people feel differently about you.
What tongue cancer taught me about myself
I love people. I’ve always been a chatterbox, and I said the universe tried to shut me up, and it just didn’t happen, so — sorry. I love knowing things about other people. The reason why I speak and do support groups and all of that now is that I want to know other people’s stories. I want to know how you persevere. I want to know what’s important to you.
I’ve always been that way. I just love getting to know people. I also will have a conversation with people anywhere, in a bar or out and about, because I want to know too. Everyone has been through things. It’s incredible.
That has not changed at all. Just wanting to help people, make people laugh, make people feel better, just having a connection — that’s always been part of me. Now I would say even more so, speaking to people. I look back on a lot of soul-sucking jobs, and now I’m like, “Maybe this was supposed to happen to me to be able to get away from that and do what I’m supposed to do.”
So I started to think of it that way as well. Just being a good person and seeing people find me — that will never stop for me, and never will. It’s nice to know that it’s the thing that won’t change.
My biggest advice for tongue cancer and head and neck cancer patients
I’ve said it before, but you can’t say it enough: advocate for yourself through diagnosis and beyond. For me, I’m always fighting insurance companies and disability and the system and all these things.
I always had trouble asking for help. You will need help. Don’t be afraid to ask for help. The people around you want to help you. Let them do it. You will need it. No one can navigate cancer alone. Support is everything.
Having other people to talk to is super helpful. If you are going through cancer, reach out to a doctor or a nurse, somebody, and ask them, “Is there someone I can speak to who’s going through it?” Or a social worker and a therapist, because it touches every part of your life — not just physically, but in the head and in the heart. You think about things that you wouldn’t before, and having support to advise you will get you through.
The people who love you always will, and they want to help you. Don’t be afraid to ask for help. Ask for what you need.
For people going through tongue cancer or just anything in life, remember who you are and remember that we want to be here and want to live. Don’t be afraid to tell people how you feel. I don’t think we can say I love you enough. Be unapologetically yourself and tell others how you’re feeling all the time, no matter what.
Finding community, blogging, and patient advocacy
There’s such a great support system on the internet for people with head and neck and tongue cancer, either through social media or through certain organizations. They’re wonderful. It’s been super helpful for me. I have my own blog, so writing about it helps me, and it helps other people. I’ve had so many people reach out and be like, “Reading your blog really helps me, and now I’m writing about my experience. I love it. I’m always like, “Please do that.”
I feel like more places should have patient advocates like me and like Beth, the girl I know who has cancer, because doctors say they see you, but they don’t have cancer. I really wish somebody had been there for me who had been through it. It is on my mind a lot. People get very afraid. They said for me I might not have a great outcome, and that is like — they don’t know how this is going to go.
I’m flourishing, and I just had a PET scan. So don’t give up hope because you don’t know what’s going to happen. Life can even be better after cancer. Reach out to other people. They’re happy to tell their stories and help you through it because it’s a route that nobody wants to be on, but once you’re in it, everyone is there to have your back. We’re all here. Find us.

Inspired by Brittany's story?
Share your story, too!
More Head and Neck Cancer Stories
Vikki F., Head and Neck Cancer (Nasal Squamous Cell Carcinoma)
Symptoms: Nosebleeds that persisted for years, nose changed in shape, nasal pain, migraines
Treatments: Surgeries (subtotal rhinectomy, reconstruction surgery including radial forearm free flap, bone grafts, and cartilage), chemoradiation
...
Red S., Tongue Cancer (Squamous Cell Carcinoma of the Tongue), Stage 3
Symptom: Persistent tongue ulcer that increased in size
Treatments: Surgeries (partial glossectomy, flap surgery), radiation therapy
...
Alyssa N., Adenoid Cystic Carcinoma
Symptoms: Persistent jaw pain, lightning-like facial pain during the first bite of meals
Treatments: Surgery (tumor removal), radiation
...
Eva G., Oral Cancer, Stage 4
Symptoms: Sore on the tongue, which caused pain during eating and speaking; changes in the color and texture of the tissue where the sore was located
Treatments: Surgery (partial glossectomy, radical neck dissection, reconstruction), radiation
...
Teresa B., Recurrent Breast Cancer (Hormone-Positive), Oral Cancer (Lip Cancer), and Skin Cancer (Melanoma)
Symptoms: Lip cancer: chapped lips & a pimple-like growth on lip, breast cancer: enlarged left breast with lump, melanoma: none
Treatments: Surgeries (bilateral mastectomy with reconstruction, lumpectomy, craniotomy, Mohs, surgery, wide local excision), hormone therapy, radiation therapy
...