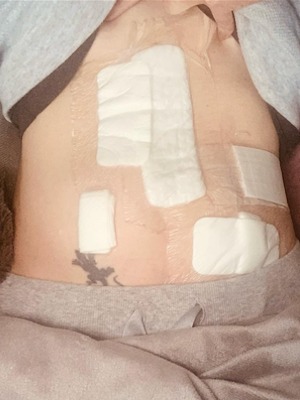
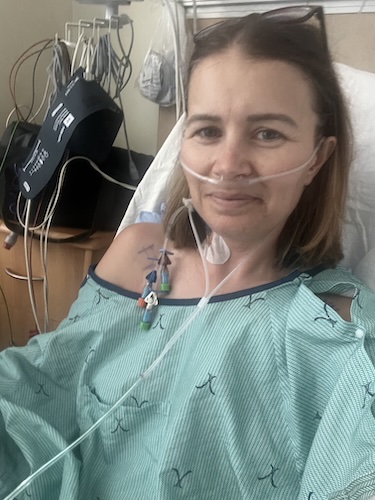
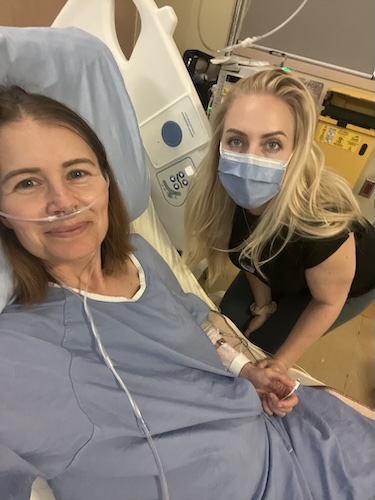
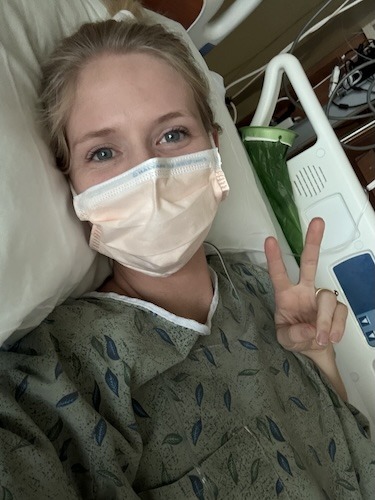
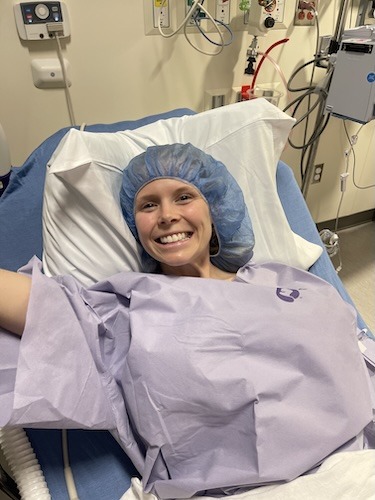
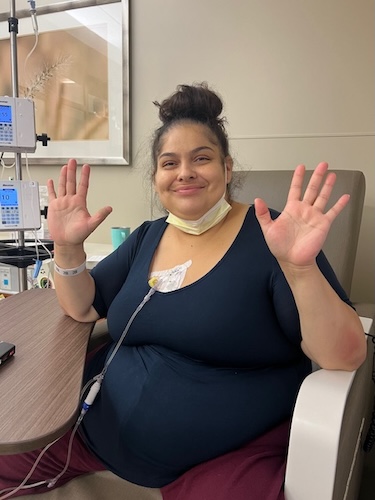
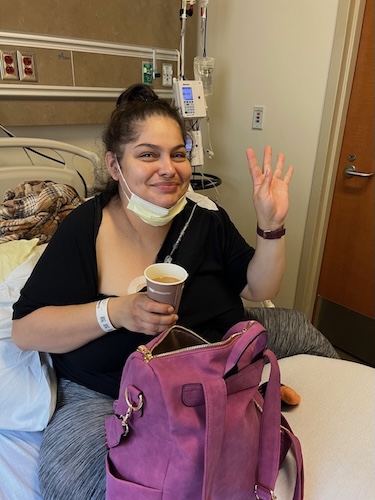
“Never Give Up, Never Surrender”: How Cora Finds Hope After Six Colorectal Cancer Relapses
Cora was a therapist who supported kids and families. During graduate school, she started feeling fatigued. She initially assumed it was burnout from years in trauma-heavy environments. In 2018, after blood and mucus appeared in her stool, a colonoscopy revealed colorectal cancer.
Interviewed by: Ali Wolf
Edited by: Katrina Villareal
At first, Cora was told it was stage 2 colon cancer. She built a mental picture in which cancer would be just a blip in an otherwise thriving life and career. She completed chemotherapy, chemoradiation, and major surgery with a temporary ileostomy over the course of a year and rang the bell in celebration. She felt better than she had in years.

But later, imaging confirmed the disease had spread, and a stage 4 colorectal cancer diagnosis upended her plans. Once again, Cora stepped away from a career she loved and navigated multiple recurrences. She moved her care to MD Anderson for liver surgeries and ongoing treatment.
Cora’s background in mental health deeply colors how she copes with stage 4 colorectal cancer. She understands shock, delayed processing of trauma, and the way patients often cannot fully process what is happening while still in crisis. During her relapses, Cora focused on finding the best treatment plan and surviving each step. Isolation during the COVID pandemic while on second-line chemotherapy triggered some of Cora’s hardest mental health moments.
Cora’s cancer has come back six times, but she remains hopeful. She says her dogs have helped her get outside for sunlight and movement. Also, a group called the Project Athena Foundation opened her to a community of people who understood medical trauma, and even invited her back into marathon training after a devastating immunotherapy setback. She completed 10 miles while still sick and swollen from steroids, deciding that was “good enough” for someone living with cancer.
Cora says cancer slowed her down, but has helped her prioritize relationships and memories over career milestones. She’s guided by her mother’s mantra of “one foot in front of the other” and her late uncle’s advice of “never give up, never surrender.” She continues to move through uncertainty, but remains hopeful because of evolving treatments, such as ctDNA testing.
Watch Cora’s video or read the interview transcript below to know more about her story:
- Cora’s long-standing love for kids and work as a children’s therapist shaped how she understood mental health, trauma, and eventually her own cancer experience
- Early symptoms like fatigue and later blood and mucus in her stool were initially attributed to burnout or IBS
- Her perspective shifted from seeing cancer as a brief interruption to recognizing the reality of recurrent stage 4 disease and re-centering life around treatment, support, and presence
- Isolation during harsh second-line chemotherapy in the COVID pandemic underscored how essential meaningful support systems are, whether through family, pets, or communities like Project Athena
- Over time, Cora transformed from a career-focused professional into someone who actively prioritizes memories, relationships, and legacy, taking “one foot in front of the other” as a daily practice
- Patients often need time, tools, and community to process trauma; survival is not just physical but emotional, and no one should feel they have to carry it alone
- Name: Cora V.
- Age at Diagnosis:
- 37
- Diagnosis:
- Colorectal Cancer
- Staging:
- Stage 4
- Symptoms:
- Fatigue
- Unintentional weight loss
- Blood and mucus in stool
- Treatments:
- Chemotherapy
- Chemoradiation
- Surgeries: temporary ileostomy and reversal, liver surgeries and ablation
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Introduction and Identity as an Aunt and Therapist
- Family Mental Health History and Early Exposure
- Honoring Patients and Reframing the Therapist Role
- How Mental Health Training Prepared Her for Cancer
- Early Fatigue and First Symptoms in Grad School
- Ongoing Medical Workup and December 2018 Colonoscopy
- Shock of Initial Cancer Diagnosis
- Waiting for Staging and Facing Anxiety About Stage 4
- TikTok, Trauma Processing, and Protecting Her Mom
- From Stage 2 Mindset to Stage 4 Reality
- Missed Liver Spots and Transition to Stage 4
- First Treatment Plan: Chemo, Radiation, and Ileostomy
- Ringing the Bell and Brief Time Cancer-Free
- Facing Stage 4 Statistics and Focusing on Treatment
- Second-Line Chemo During COVID and Isolation
- Dogs as Emotional and Physical Support
- Multiple Recurrences and Care at MD Anderson
- ctDNA Testing and Invisible Tumors
- Six Years of Stage 4 and Hope from New Treatments
- Staying Focused on Forward Motion
- Building Support Systems and Project Athena
- Marathon Training, Immunotherapy Setback, and Ten Miles
- Shifts in Priorities, Memories, and Legacy
- “Never Give Up, Never Surrender” and Facing Mortality
Introduction and Identity as an Aunt and Therapist
My name is Cora, and I have stage 4 colorectal cancer, and I live in Oklahoma City, Oklahoma.
I am, gosh, it is a hard thing to kind of start. I think first of all, I would identify myself as an auntie. That has been my role that I’ve loved the most in my life. I have been somebody whose primary focus in life has been my career and my family, but not starting my own family. So I didn’t get married and have my own kids. Rather, I worked with kids, and I have all of these siblings that I love.
I think that my love for kids has really directed my life a lot in a lot of ways, and that’s what keeps me going, even in this journey with cancer. I worked all kinds of different jobs, and I went through undergrad, and ultimately, I ended up working in a child support court doing mediation hearings. That led me on a path toward more social work and getting into being a therapist, and I was a children’s therapist. I’m still licensed as a therapist; I just have not been practicing for a couple of years because of my health issues and wanting to focus on that. So I think most of my life is directed towards helping kids and focusing on, I hope, building a little bit of a better future for kids.
Family Mental Health History and Early Exposure
Mental health was something that I hadn’t necessarily struggled with personally prior to my diagnosis, but I had seen my father struggle with it. He was diagnosed with PTSD while I was in grad school, and we were able to talk some about that and his experience with PTSD. I think, in general, seeing different people in my family struggle with mental health, but not necessarily get any resources or have that language as I was growing up, was impactful.
Honoring Patients and Reframing the Therapist Role
I think that one of the things about mental health and being in that field is that people often come to you thinking that you’re the one who’s going to give them the answers or that you are in some way doing them a favor. As a therapist, one of the things that I focused on was trying to bridge that into just a communal relationship and working together. Really, as a therapist, their sharing these kinds of things with me has been one of the greatest honors of my life.
Even going into my diagnosis, prior to that, I had worked with kids with chronic illness and some adults with chronic illness. You have this intellectual idea of what it looks like to have a chronic illness, or what it looks like to experience depression or anxiety, and then it’s very different when you’re in it. I think I’m so thankful for all of the different people who have exposed themselves to mental health, who have processed their lives and their griefs.
How Mental Health Training Prepared Her for Cancer
All of that study prepared me in some ways to be able to survive this diagnosis mentally and emotionally. I think that’s what I took from those kids as well. I worked with kids who had a lot of trauma for the most part, and you just see them survive, and there’s nothing better than that. Seeing them survive and make it through that kind of thing means that they’re a big part of that story for me now, even though I don’t work with them anymore.
Early Fatigue and First Symptoms in Grad School
It really started — and it ties in a little bit to the mental health stories — when I was in graduate school. I had always been somebody who worked more than 40 hours a week, had gone to school and worked, and suddenly I was so tired that I was coming home and not eating and going to sleep. I was losing weight unintentionally because of that, because I was just sleeping rather than eating. So my fatigue was really the first thing that I noticed. I thought it was probably burnout because I had been in this heavy trauma environment for years. As I switched to different jobs, that fatigue kept following me, and that’s what I noticed first.
Ongoing Medical Workup and December 2018 Colonoscopy
It was years, and I went through a process with my doctor of trying different things, even treatment for depression, even though I didn’t have any of the other symptoms besides fatigue. I had thyroid testing constantly, just different things, and everything came back normal. Then, in December of 2018, I had blood and mucus that I was passing, and that was a big worry immediately.
We all thought it was probably IBS (irritable bowel syndrome) or something like that. I ended up getting scheduled for a colonoscopy. When they woke me up from the colonoscopy, my mom was there with me, and the doctor walked in and said he was really surprised, but it looked like I had cancer. He gave us a picture of the tumor and said they couldn’t say 100% that it was cancer until the biopsy came back. That was a Thursday. By Monday, I was in for a different procedure to test staging, looking at things, talking to an oncologist, and the biopsy was back, confirming it was what we thought at that time was stage 2 colon cancer.
Shock of Initial Cancer Diagnosis
I think for the most part, it was just shock. I don’t even think I cried. My mom, I don’t think, cried right then. I think we were all in a lot of shock. My stepdad picked us up from the hospital, and when we got in the car, he asked how things went, and I said, “I have cancer.” He thought I was joking because we were very calm and in shock in that moment.
But then, when I got home, I cried for probably about 24 hours.
Waiting for Staging and Facing Anxiety About Stage 4
A couple of days later, the oncologist confirmed it was cancer. I had an ultrasound that day that confirmed it hadn’t broken through the colon wall yet, which is part of the staging. We were still waiting on CT scans to see if it had spread or not. I knew at that point that because of my age and that kind of thing, it was more likely I was going to be diagnosed as a stage 4 patient.
Typically, when you’re getting symptoms, a lot of times you’re already at that stage of having metastasized. I was just a mess of anxiety. I was supposed to start private practice the day after my diagnosis. I had left the hospital where I was working, and I had keys to my new office. I was going to start on Thursday, and on Friday, I was signing into my new office space. Instead, it was a morning of texting people. I couldn’t call anybody, and I feel bad about that. It’s hard to break that kind of news by text, but I couldn’t even say it for probably a long time afterwards.
TikTok, Trauma Processing, and Protecting Her Mom
Sometimes, the reason I started a TikTok channel was to analyze my own grief from that psychology perspective. I haven’t wanted to release that because it is painful for people like my family members. As you probably know, as a mom seeing your little kid go through it, my mom is the person I want to protect most in that. I started making these TikToks, analyzing some of that stuff.
That initial phase is the same kind of thing I talk to people about with trauma. We don’t go to somebody immediately and start processing trauma right when it’s happening or as it’s happening. We don’t send therapists into the battlefield to say, “You just saw your friend get shot. Is that hard?” We wait because it’s unsafe. Our bodies are unsafe. Our minds are unsafe. One of my aunts who had cancer told me it’s like you’re walking around with an octopus on your face all the time, and you have to peel back a leg every once in a while to peek out. You’re in that space of trauma psychologically, and it just takes time to move to a different step of processing that for most people.
From Stage 2 Mindset to Stage 4 Reality
No, actually, I got diagnosed initially as stage 2. My mindset then was like, this isn’t — I have a career I love. Cancer is going to be this little blip in my life. My whole goal was to put it behind me. It wasn’t until I got diagnosed with stage 4 cancer that I started posting on TikTok and recording some of my grief.
Really, that whole time I was stage 2, to a certain extent, people would say, “Well, it’s always cancer,” and I would say, “No.” I had a year-long treatment plan. That plan was supposed to be over, and I was supposed to have an 8% chance of recurrence or something. My mindset was on the future at that point. Later on, the diagnosis of stage 4 cancer changed that perspective.
Missed Liver Spots and Transition to Stage 4
It wasn’t that my cancer was clearly gone. In my first whole treatment cycle, that first year, we thought I was stage 2. There are always these little spots on people’s scans that are small, and radiologists sometimes note them, and sometimes they don’t. About halfway through my first treatment plan, a radiologist noted a spot on my liver for the first time, but my oncologist said it had been there before. None of those spots grew, and we really thought they were just incidental.
After I had been cleared of treatment and we thought I was good, we were monitoring me really closely because of those spots on my liver and lungs. I had started a new job at a treatment facility and was really excited. Within a couple of weeks, the oncologist was calling me saying, “Now these spots are growing,” and that they really had thought it wasn’t cancer — and it was.
First Treatment Plan: Chemo, Radiation, and Ileostomy
I had chemo and then radiation with an oral chemo pill for a month. Then I had a major open surgery with a temporary ileostomy. I had that for three months and then had it reversed. It was almost exactly a year from the time I was diagnosed, going through all of those steps, to the time that I had my ileostomy reversed.
Ringing the Bell and Brief Time Cancer-Free
I rang the bell, and we celebrated. I had no evidence of disease (NED). I really felt good again. I felt better than I had in years right about that summer. It was the summer that I finished everything.
By the end of summer and early fall, I was feeling bad again and fatigued again. It was about six months after we celebrated me being cancer-free and my ileostomy reversal and all that stuff before the stage 4 cancer came up.
Facing Stage 4 Statistics and Focusing on Treatment
With the stage 4 cancer, one of the situations I knew was that there were some bad statistics about stage 4 colorectal cancer out there. I didn’t want to hear any statistics. I just wanted to focus on the best treatment plan and do the best I could to survive that treatment plan.
It was a really dark time. It was a lot of crying. It was a lot of friends and family around, talking to my boss, having to say goodbye to all these kids at work again and leaving that. It was a time of grief. But still, at that point, my mind was set on living and this still being temporary. It was almost like that shock all over again — I’m shocked, and now I’m going to cry a lot, but my mind is going to be focused on the future and not the potential that I won’t recover from this.
Second-Line Chemo During COVID and Isolation
Second-line chemo was really difficult compared to the first line, and I got very, very sick from it. I don’t think I was nervous about doing chemo again. I did have a lot of weird side effects on my first round of chemo, but out of all the things I went through, it was the most manageable of the three-pronged treatment. I would rather have had the chemo again over the radiation or surgery from that first time.
I went into the chemo thinking, “Okay, I did this once before; it’s a different type of chemo. I’m going to be annoyed with having to keep this bag on me for a couple of days, but I’m going to survive it.” And I did, but it definitely took a much harder toll on me.
We were in the middle of COVID at that time, and I had to go to chemo by myself, which was not something I had ever done before. I always had a whole group of people around me. Then I had to come home and be by myself because everybody was scared of getting me sick, because I was so sick on that particular chemo. I think that’s where I started struggling with actual mental health.
We think we can build ourselves up and hold ourselves up through this kind of thing, especially if you’ve been independent your whole life and you’re in your mid-30s. You think, “I’m going to be fine,” and then all of a sudden, I was entirely isolated. I had people on the phone and different things, but it just wasn’t the same, and that second round of chemo was really difficult.
Dogs as Emotional and Physical Support
Yes, I actually had two dogs through all of my chemo and treatment. We lost one about a year ago. My dogs were always the ones who kept me going, not just emotionally, giving me some of what I needed, but also physically. I have to walk them every day. I have to go out and get sunshine every day. They keep me interested in the world. Even when I’m having a very bad physical day, I can force myself to do the things I need to be doing for myself because of them. I’ve really enjoyed having them, and during COVID, they were a very nice blessing to have.
Multiple Recurrences and Care at MD Anderson
I am on my fifth recurrence currently. This will be my sixth time having the tumor come back, having a recurrence, and asking, “What’s our treatment plan?” I switched over to MD Anderson when I became stage 4 to have surgery, instead of going to my local hospital for the liver surgeries. I’ve been treated there ever since.
I go there next week to find out what we’ll do next. Overall, I’ve made it through needing treatment five times, and now I’m at my sixth recurrence.
ctDNA Testing and Invisible Tumors
Some of the things that keep me hopeful are new discoveries. Most recently, I found out that they have ctDNA tests for colorectal cancer. I got a positive ctDNA test in October, but my CT scan was clear; they can’t find a tumor.
What the ctDNA does, from what I understand, is it looks for cells that match the genetic DNA of my original tumor. They can tell that a tumor is setting up somewhere in my body; they just can’t find it yet. Right now, I don’t know where it is. That’s the second time I’ve had a positive ctDNA test. The first time, it ended up showing up in my liver at my next CT scan — or maybe it was the third time; it’s hard to remember — but it ended up showing on my CT scan at my next appointment, and I had another liver surgery and ablation.
Six Years of Stage 4 and Hope from New Treatments
I think one of the things is that I’ve been lucky to have all of these ups and downs, but I’ve been lucky to have lived through six years of this. I had an ex and friend — the same person, somebody I had dated briefly — who also got diagnosed with stage 4 colorectal cancer about a year after I did. He ended up passing away from that cancer. I’ve been really lucky to have made it through six years of colon cancer.
Through those six years, many things have been developed in the medical field. The ctDNA test has been developed. When I was originally stage 4, the plan was for me to be on chemo for the rest of my life. I took a break from that because I didn’t know if I was going to make that choice to be on chemo for life. Just in that time period of taking a break, new data came out, new studies came out, and my oncologists changed their minds and said I didn’t need chemo for life. We could wait and do surgery sometimes or other types of treatment.
Staying Focused on Forward Motion
I know there are people out there working toward this goal. They don’t necessarily have me individually in mind, but they’re doing so much good work. I keep myself focused on all of these things that people are doing and try to hold myself to that standard in my own life. My mom says “one foot in front of the other” a lot when we talk about my story, so I’m just going to keep putting the next step in front of me. I’m here, and I feel like that’s part of my obligation as a human and part of this community.
Building Support Systems and Project Athena
For me, one of my takeaways in mental health and dealing with really hard parts of life is that you have to reach out and find a support system. I was lucky enough to already have a really great support system, but I also had to keep looking for new resources as things progressed.
My family and loved ones have their own grief and denial and things that they process. As much as I would love to drag them through that, they have to go through it on their own. I can’t do it for them. Another really helpful thing I found was signing up for a group called the Project Athena Foundation. They do outdoor training for people who have survived medical trauma. There is this group of people — trainers and different people — who have been through all kinds of things. That’s who I turned to this summer.
I got kicked off an immunotherapy trial because my body couldn’t handle it. It was really devastating because we were hopeful it might give me some time cancer-free. The first person I texted was the coach of that group: “Can you just send me some crappy athletic story about going forward through loss? Even if it’s cheesy, even if it’s stupid, that’s what I need this morning, because I know you all have gone through that kind of thing.”
Marathon Training, Immunotherapy Setback, and Ten Miles
Rather than a cheesy line or poster, what they sent me was that I was going to be signed back up to rejoin them on the marathon I couldn’t join because of the immunotherapy trial. Instead, it was an invitation to California to go on the marathon I had been pulled from because of my medical condition. I thought, “Wait, I need a minute to process the possibility of that right now.” But it was still that mindset of, “Okay, you got kicked off that yesterday. Today, you can go back to marathon training.”
I had trained twice for this marathon, and both years, my cancer came back right at the end. I went to California super sick. I’m still swollen from steroids because my kidneys and liver kind of went into failure from the immunotherapy. I went with my team. I did 10 miles before I started vomiting everywhere, and they had to take me back to the hotel for a couple of hours. Then I was able to rejoin them at the finish line. Honestly, 10 miles is good enough for somebody dealing with cancer at that point.
Shifts in Priorities, Memories, and Legacy
I do notice a change in myself. One of the biggest changes is that the career-driven, forward-thinking mindset I had prior to my cancer diagnosis, as much as it was a good thing, might have shortchanged some of my relationships. Cancer has slowed me down in ways that have been helpful when it comes to making memories.
I have so many pictures. My friends and family now know that if they go somewhere with me, I’m going to make them do something really silly for a photo shoot. I do that for me, but also for them. I never thought about leaving them behind and them having to grieve me. Now I think about what I’m going to leave them, and that’s been impactful in a really wonderful way in my life.
“Never Give Up, Never Surrender” and Facing Mortality
I think one of the ways I deal with my own death sometimes is by thinking about fun questions I would ask my loved ones on the other side. I have this really weird, quirky uncle who gave me a book right before he passed away about us being aliens or something. It was this very quirky little book, out of nowhere. He would always say, “Never give up, never surrender.”
That quote sticks with me because of him and because of his giving me that book at a difficult time. I think that’s really the mindset you have to take with cancer. It’s a lot of different choices and different kinds of things, but you just can’t give up and you can’t surrender to it.

Inspired by Cora's story?
Share your story, too!
More Metastatic Colorectal Cancer Stories
Raquel A., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Frequent bowel movements, pin-thin stools, mild red blood in stool
Treatment: Chemotherapy
Steve S., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Blood in stool, changes in bowel habits, feeling gassy and bloated
Treatments: Surgery, chemotherapy, monoclonal antibody, liver transplant
Jessica T., Colon Cancer, BRAF+, Stage 4 (Metastatic)
Symptoms: Severe stomach cramps, diarrhea, vomiting, anemia (discovered later)
Treatments: Surgery (hemicolectomy), chemotherapy
Jennifer T., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Weight loss, coughing, vomiting, sciatica pain, fatigue
Treatments: Surgeries (colectomy, lung wedge resection on both lungs), chemotherapy, immunotherapy
Kasey S., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Extreme abdominal cramping, mucus in stool, rectal bleeding, black stool, fatigue, weight fluctuations, skin issues (guttate psoriasis)
Treatments: Surgeries (colectomy & salpingectomy), chemotherapy