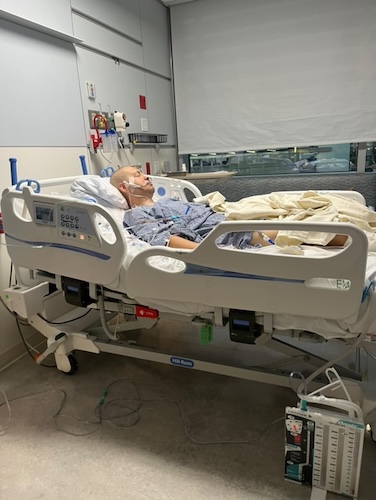
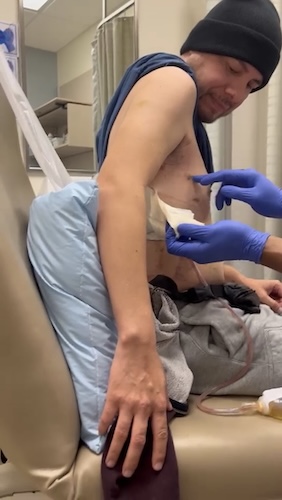
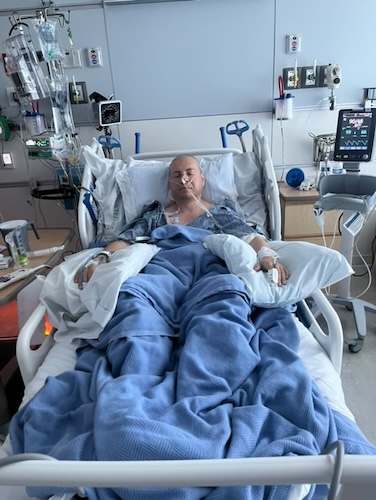
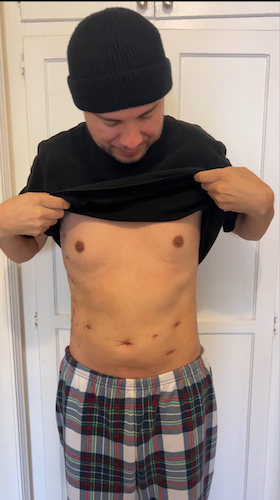
Life Without a Stomach? Graham’s Stomach Cancer Surgery Story
At 61, Graham found out that he had stomach cancer. He’d been vigilant for years due to his family’s history with Lynch syndrome, and so he started having annual screenings. These reassured him, but eventually also brought him the life-altering news about his health.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
Graham discovered he was positive for Lynch syndrome, a commonly inherited cancer syndrome that increases cancer risk, after his cousin was diagnosed with colon cancer and his family underwent genetic testing. Two decades followed, during which he had regular screenings. Nothing turned up suspicious, but everything changed in 2023. A routine endoscopy revealed something worrisome and, soon after, Graham was told he had stomach cancer, specifically early-stage diffuse gastric adenocarcinoma with signet ring cell features, poorly differentiated. (Editor’s Note: Signet ring adenocarcinoma is a rare and aggressive subtype of adenocarcinoma. Diffuse stomach cancer is a rare form of stomach cancer. Poorly differentiated adenocarcinomas spread faster than other carcinomas whose cells are better differentiated.)

Graham was devastated by his stomach cancer diagnosis. Thankfully, his wife, Christina, was with him when he had that fateful conversation with his doctor. She absorbed all the crucial information and helped him stay calm when his mind drifted due to shock, fear, and uncertainty.
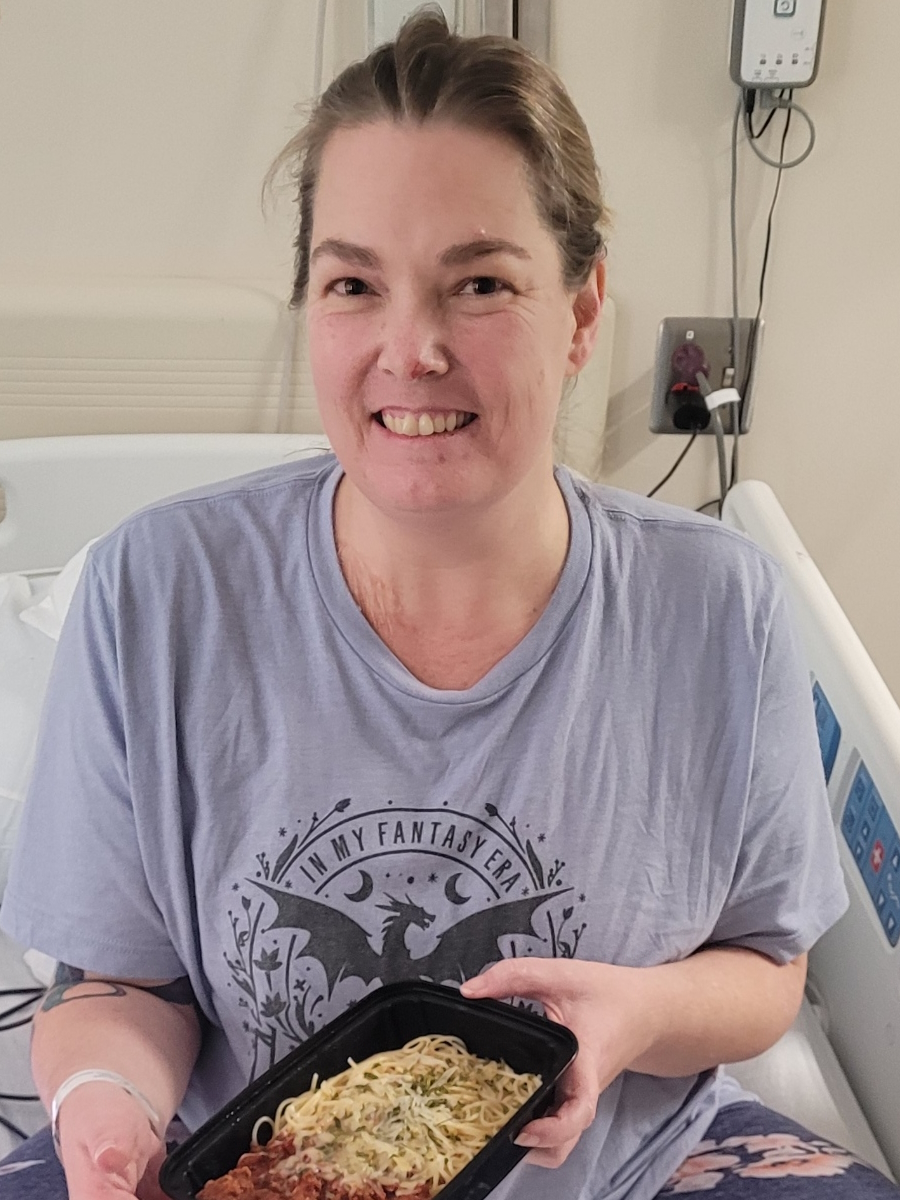
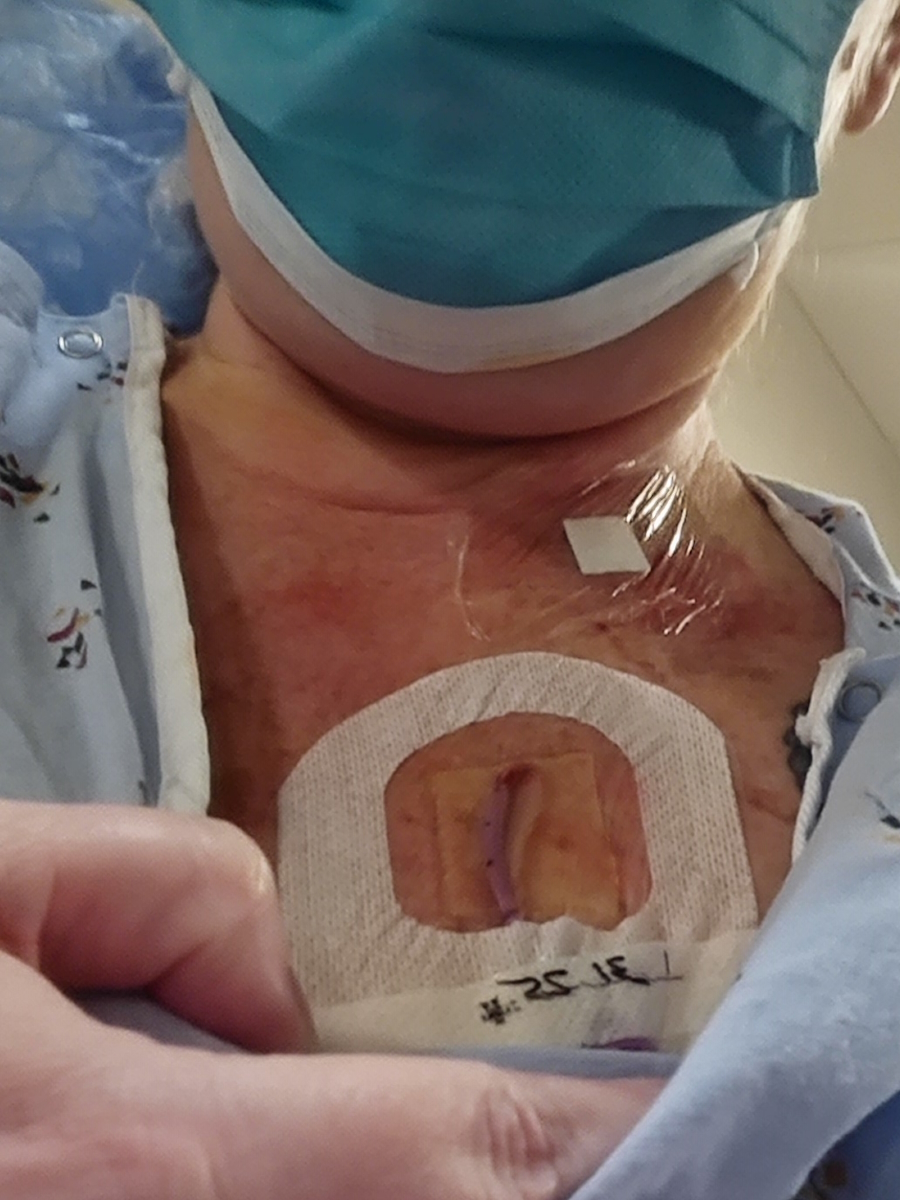
Dealing with everything after diagnosis involved coming to grips with stomach cancer and his treatment, which included adjusting both emotionally and physically. Graham underwent a total gastrectomy, which meant that he needed to learn to live without a stomach. Recovering from surgery wasn’t just about physical healing; it also involved redefining what was normal for him. Graham’s weight plummeted while he struggled to deal with the loss of his stomach. He also worked to find foods that his digestive system could manage, and he had to make do without the usual hunger cues.
Graham’s consultations with dietitians were crucial. Their guidance helped him learn to focus on nutrient-dense foods and supplements that could counter dietary deficiencies. He found that emotional support was also important. Graham found solace in counseling and an online support group where he connected with others, exchanged practical tips, and found mutual encouragement.
When Graham attempted to re-enter his social environment, he found new challenges. Because food is part and parcel of social gatherings, he faced “food anxiety” and thought twice about joining even friendly gatherings. Over time, though, he gradually became more confident as he found new ways to engage with his friends and family and became less pressured by eating norms.
Graham’s advice regarding stomach cancer is clear: talk to your doctor about screenings, regardless of your age. Early detection saved his life, and it may well save others’ lives, too.
Watch Graham’s video to learn more about:
- How does one live without a stomach? Graham’s story reveals the answer
- Graham’s candid reflections on life after stomach cancer
- The unexpected challenges of social life after a total gastrectomy
- The vital role of emotional support in Graham’s recovery from stomach cancer
- Why talking to your doctor about screenings could save your life: Graham’s heartfelt plea
- Name:
- Graham L.
- Age at Diagnosis:
- 59
- Diagnosis:
- Stomach Cancer (Diffuse Gastric Adenocarcinoma with Signet Ring Cell Features, Poorly Differentiated)
- Staging:
- Stage T1bN0
- Symptoms:
- None; a stomach polyp discovered during his annual screening tested positive for cancer
- Treatments:
- Surgeries: total gastrectomy, lymphadenectomy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.

Inspired by Graham's story?
Share your story, too!
More Stomach Cancer Stories
No post found