Ellis’ Stage 3A Melanoma Story
Ellis shares her stage 3A melanoma story, a subtype of skin cancer, and undergoing treatment from surgery, immunotherapy, and targeted therapy.
In her story, Ellis also highlights navigating important quality of life issues, from managing hair loss, dating as a cancer patient, what support helped the most, and parenting with cancer.
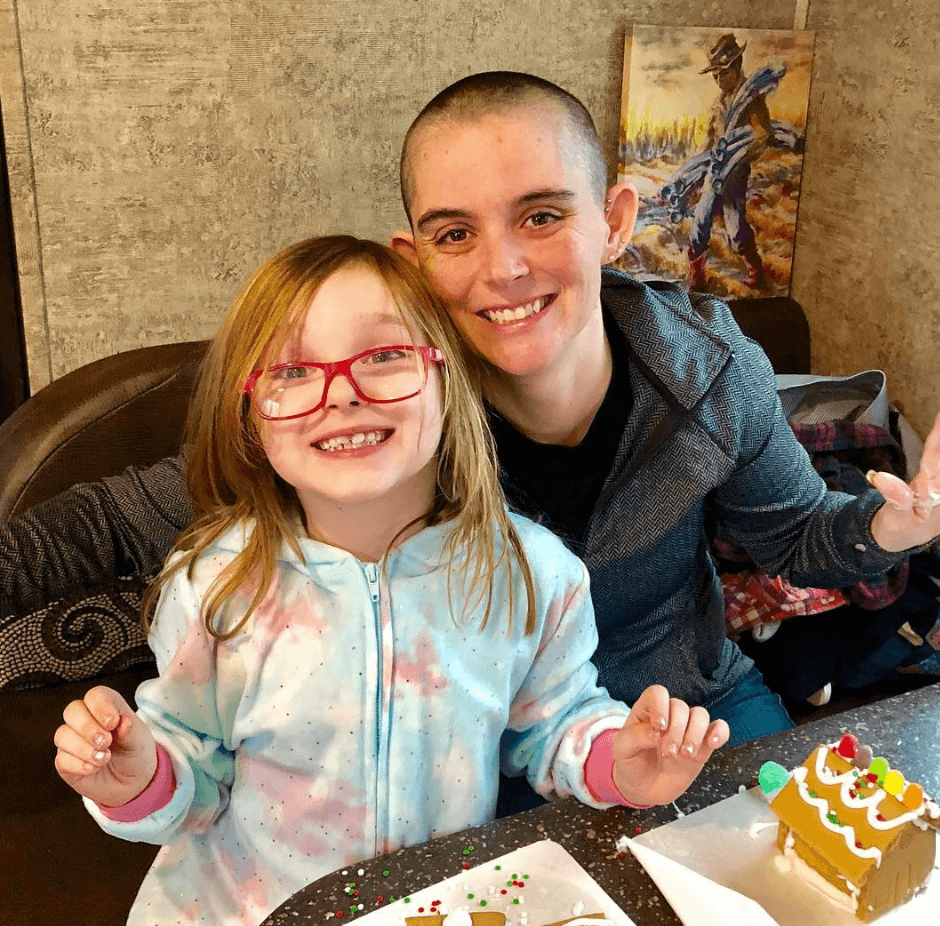
- Name: Ellis E.
- Diagnosis:
- Melanoma
- Type of skin cancer
- Staging: 3A
- 1st Symptoms: Changing mole on arm
- Treatment:
- Surgery
- Surgical biopsy
- Complete lymph node resection
- Immunotherapy
- Opdivo
- Infusions once every two weeks; only made it through 9 treatments
- More stories with immunotherapy
- Opdivo
- Targeted Therapy
- BRAF Inhibitor
- Taken orally daily for a year
- BRAF Inhibitor
- Surgery
- Hospital:
- Medical City Dallas
- Diagnosis
- Surgery, Immunotherapy, Targeted Therapy
- Reflections
- Did you lose your hair?
- Can you talk about the mental and emotional side of cancer?
- Can you talk about your support system?
- What’s your advice for friends and family members of cancer patients who want to show their support?
- What’s your advice on self-advocacy?
- How did cancer change your perspective on life?
- What was dating with cancer like?
- How did cancer affect your relationship with your boyfriend?
- Was there a talk about fertility?
- What’s it like to be a parent with cancer?
- How was the financial aspect of treatment?
- What advice do you have for someone who has just been diagnosed?
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Breathe first. Don’t Google too much. One thing I asked my doctor was where to find reputable information, and I went from there.
It’s easy to fall down a Google rabbit hole. Try not to.
Ellis E.
Diagnosis
What were the first symptoms
I’ve always been pretty careful about my skin health. I’ve got a pretty pale complexion, so I go to the dermatologist every year in the Spring. I had gone in March of 2017.
In October, I noticed this mole on my arm had changed. I took a picture of it and put it side by side with another picture and saw just how much it had changed.
I called my dermatologist at eight the next morning and made an appointment.
What happened at the first doctor’s appointment?
They did a biopsy of the mole. They cut off a portion of the area around the mole. They basically just scrape off part of your arm. They numb it first.
It wasn’t painful at all. It looks kind of like it would if you skinned your knee or something as it heals.
How long did the biopsy results take?
It was six days. I was super nervous. I had my birthday in between the biopsy and getting the results, so it was really hard to focus on birthday fun.
With melanoma, they measure the depth of the primary tumor. That indicates how likely it is to have spread.
The doctor called and told me mine was 1.45cm. Anything under 1 is considered pretty low.
Describe the surgical biopsy
On November 13th, I had surgery to take out a bigger portion of that area on my arm and then a biopsy of lymph nodes. I went under general anesthesia.
They did what they call a sentinel lymph node biopsy. That’s where they inject radioactive stuff in your arm and trace it to see where it goes. They removed the responsive lymph nodes to test them.
I wasn’t really nervous about the surgery itself. I’ve had a few other surgeries, so it wasn’t a big deal. I was definitely nervous about getting the results though.
I was up and walking around that same day. It was just a day procedure. There wasn’t really any recovery from that surgery. About two days later, my doctor called me. He said they found a small amount of one of the three lymph nodes they tested. He said they didn’t find it in the other two.
My work offers a retest program, and I got a second opinion. They found it in all three when they tested it. I didn’t have to go anywhere for the retest–that was actually done through Harvard.
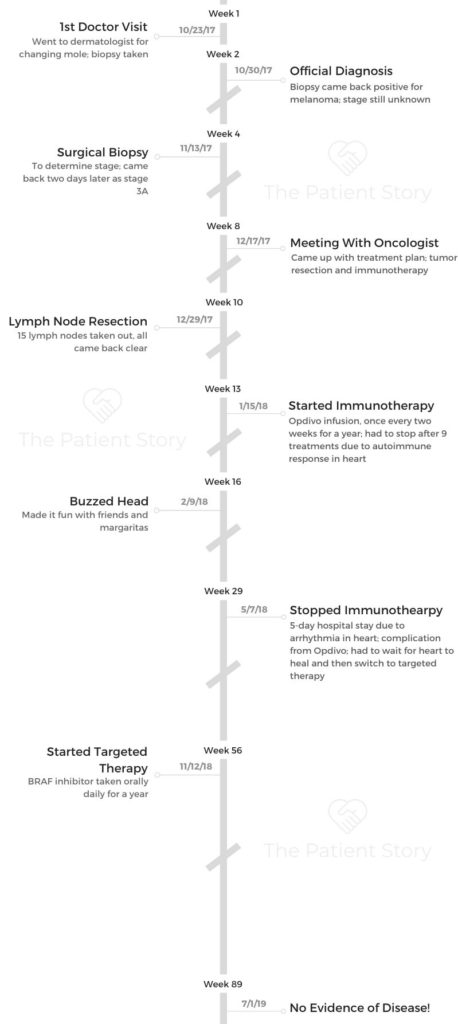
What was your treatment plan?
October 30th was the initial diagnosis. I knew I had melanoma on that day, but I got the staging results on November 15th, 2017.
On December 17th, I met with an oncologist, had a PET scan, and discussed next steps. The plan was another surgery and immunotherapy.
The next step was sort of up in the air. Some doctors want to do a full lymph node resection. I decided to go ahead and do it, so we did that on December 29th.
Surgery, Immunotherapy, Targeted Therapy
What was the complete lymph node resection like?
They took out 15 more lymph nodes, and luckily those were all clear. It was a much harder surgery than the initial biopsies. I had a drain for about a week after the surgery, and I definitely had a lot more limited mobility in my arm. I felt worse. I took a few days to recover.
When I woke up from the first surgery, I had pain meds, they were attentive, and everything was great. I felt pretty good, ate some food, and went home.
For this surgery, I was begging for pain meds, and they were less attentive. Maybe that’s because it was the last Friday before the new year and no one wanted to be there. I don’t know. It was a much different experience though.
I was only in the hospital that day. The first biopsy had been an hour or so, and this one was about two hours.

What was immunotherapy like?
I started immunotherapy on the 15th of January in 2018. That was an infusion of Opdivo once every two weeks. I was originally supposed to do that for a year, but I wound up only doing that for about five months.
The infusion itself only took about an hour and a half, but it would always take all day long because they have to do your labs, order the drug, the pharmacist always took forever, and all that.
I ended up having an autoimmune response in my heart, and that caused arrhythmia. They initially thought it was my lungs having an issue, but they found out it was heart.
I’m a runner, so my resting heart rate is like 40 beats per minute (BPM). I would just be sitting there and it would jump to 140.
I got kicked off that treatment essentially after nine treatments because of that. I stayed in the hospital over Memorial Day weekend. It was so boring. I was the only one under 60 in the cardiac unit, and then I ended up back in oncology for a bit.
Did you have side effects from immunotherapy?
I had some fatigue. I also had some really bad rashes on my entire body. They weren’t on my face, but they were everywhere else. They itched a little. It wasn’t too bad, but when I got hot it would definitely itch.
They gave me a steroid cream for it, but it never got bad enough that it warranted taking anything.
»MORE: Read more patient experiences with immunotherapy
What was targeted therapy like?
I waited six months in between the heart complication and starting targeted therapy because they just wanted to make sure everything healed properly. They wanted my heart function to go back to normal first.
The targeted therapy I was on was a BRAF inhibitor. It was just a daily pill I took, and I did that for a year.
The first few months were the worst with the side effects. I had some nausea, fever, and chills.
I would get so cold, I’d be shivering. I had to crank the heater all the time and have a blanket with me just in case.

Were you getting scans during treatment?
I was getting PET scans every three months. I had blood work done every time I’d go in for appointments.
One thing the treatment can do is mess with your thyroid, so that was one thing they were often looking out for. My levels got a little low a few times, but they were never bad. I lucked out with that.
They found a hyper-metabolic spot on my left ovary that they found on a PET scan. They couldn’t determine if it was benign or not, so they opted to just go ahead and take it out. Oddly enough, that’s when I found out I’ve never actually had a right ovary. They took the spot out to test it, and it came back as benign.
That was another quick day surgery. It was only a couple of hours. I did take a couple of days off work to recover though. I was walking on the treadmill the next day. I was up and moving around pretty quickly.
When did you find out you were in remission?
I had a completely clear PET scan over the summer in 2019. I was happy about it, but I felt like there had been little bits of bad news every other time, so I was a little skeptical.
I was like, “This is fine, but in three months, what’s my next one going to look like?”
I never really experienced anxiety about my scans though. My first PET scan was a big deal, but I’ve been better able to handle scans and waiting for results as time has gone on.
I remember after my first scan wanting the results right away. Now, I’m able to wait days or weeks for results without being anxious.
»MORE: Dealing with scanxiety and waiting for resultss
Reflections
Did you lose your hair?
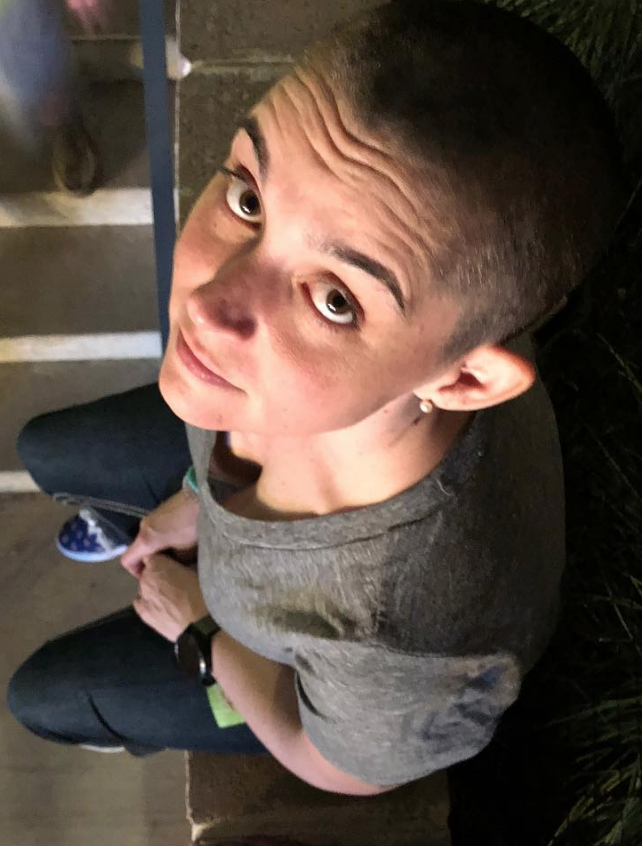
I didn’t completely lose my hair, but the texture did change and I had some bald spots, so I ended up just buzzing it.
I’ve had really short hair before, so it wasn’t the most drastic thing. The worst part was that because the balding started happening where my part had been, I couldn’t really cover it. That was when I decided to shave it.
»MORE: Dealing with hair loss during cancer treatment
My friends and I drank margaritas and buzzed my hair one night. It was actually really neat. They made it a fun experience.
I’ve never been particularly girly or feminine. My hair isn’t as big a part of how I express myself as it is for other people.
Can you talk about the mental and emotional side of cancer?
Looking back, right after my diagnosis was probably the hardest because I didn’t know what to expect. I got a little wine drunk and was really upset that first night.
Then I regrouped, and I started seeing a therapist pretty quickly. That helped a lot. I think especially since I was proactive about doing it and started early.
Overall, from a mental health perspective, I’ve been mostly okay. There’s some stressful moments, but I’ve been okay.
The hardest thing is those unnamed emotions where you’re not really sure why you feel what you feel.
Can you talk about your support system?
When I was going through treatment, I was dating someone else who was definitely not supportive at all.
It’s funny because I met Dave, my current boyfriend, early in my diagnosis. I met him through a cancer support group, and we were friends for about two years before we started dating.
I have a support community, but it didn’t come from the typical people who you’d expect it to come from, I guess.
What’s your advice for friends and family members of cancer patients who want to show their support?
I had a lot of people who I assume would genuinely say, “If you need anything, let me know.”
That was hard because I needed a lot of things. I wanted to know the general realm of what they were offering.
The things that were the best to me were when people would say things like, “Hey, I can come mow your grass this weekend. Does that work for you?” Or, “I can bring some food over tonight. Do you want me to do that?”
That way, I knew exactly what I could ask them for, and all I had to do was say yes or no and name the day and time.
»MORE: What kind of support cancer patients say helped the most

What’s your advice on self-advocacy?
The main thing I did was take advantage of the second opinion program at my job. That was huge because the first doctor missed those other lymph nodes.
I always tell people to get a second opinion until you feel comfortable, but there’s a line. When you get to be on your fourth or fifth opinion, are you really still looking or is it more so that it’s decision paralysis? At a certain point you have to make a choice and start treatment.
One thing I see and hear all the time is people asking, “Am I the only one?” No. The answer is no. I can guarantee that whatever it is, you’re not the only one, but people just need to talk about it.
People feel so alone, so I highly recommend talking about your story. The people who have been through what you’re going through are going to give the best advice. Seek them out.
»MORE: How to be a self-advocate as a patient
How did cancer change your perspective on life?
I sold my house, bought an RV, and I travel a ton. I’ve been to New Zealand, Amsterdam, Costa Rica, Iceland, Morocco, and so many places. I’m going to Italy in May 2020. I’ve just refocused how I want to spend my time and money.
It’s changed how I spend time with friends and family too. I’m more present when I spend time with people. I do better at balancing running and things I want to do and taking care of my daughter.
What was dating with cancer like?
It was okay. I didn’t have any negative experiences. I was always really upfront about it.
If you’re trying to date with cancer, just be open and honest with yourself about what you want. In my case, with people who were worth getting to know, it was never a big deal for them. If someone freaks out, that’s not your problem.

How did cancer affect your relationship with your boyfriend?
We met through a cancer app. We went out to CancerCon, and we just hung out, had coffee, and talked. The next year, we went out again, and we talked more.
That was how things started. We started dating in May of 2019. He doesn’t live in Texas, so he was flying back and forth some. Now he’s here pretty much all the time.
He was with me for the last half of my treatment and ending the targeted therapy. It was interesting because my ex didn’t understand the fatigue or stress or anything, and Dave has just always been so understanding and supportive.
Was there a talk about fertility?
There was a little talk about it, but not a big one. I can’t have any more kids. I have one. She’s seven, and she’s pretty fantastic. I feel okay about it.
My boyfriend had testicular cancer twice, so he can’t have any kids. I can’t have any more, so that’s something we tackle together.
What’s it like to be a parent with cancer?
It’s hard. She’s at a good age. She understands enough and is just a super sweet kid. She’ll crawl into bed with me and just cuddle.
I think she worries too though. She doesn’t know what’s happening or what’s going to happen.
When I first buzzed my hair, some kid at her daycare was like, “Why do you have no hair?” And she said, “My mommy has cancer!” I was like, “Okay, great, have a good day, everyone.”
She was 5 when I was diagnosed. She had just turned 5 too, so she probably didn’t understand as much as she would if I explained it all now that she’s 7. I just told her I was going to have some surgeries and maybe wouldn’t be feeling so great sometimes, and I just left it at that.
»MORE: Parents describe how they handled cancer with their kids
How was the financial aspect of treatment?
I’m running the Boston Marathon for a cancer-based non-profit that offers financial support for patients.
The cool thing is that the money isn’t just specifically for medical bills but for all the other expenses that don’t go away like mortgages, electric bills, food, and everything.
It’s something I care a lot about because I didn’t have to worry about it. I have incredible medical insurance, so my out of pocket was only a couple of thousand dollars a year. I lucked out.
There was very little financial stress for me in terms of this, but I know that I’m very fortunate, so that’s why it’s important for me.
What advice do you have for someone who has just been diagnosed?
Breathe first. Don’t Google too much. One thing I asked my doctor was where to find reputable information, and I went from there. It’s easy to fall down a Google rabbit hole. Try not to.
The thing to remember is that people on message boards are usually the people who are struggling with their diagnosis. You don’t see the people who are in remission and living their normal lives. Those message boards have good information sometimes, but you have to keep in mind that you’re getting a very singular focus.

Take charge of your own experience. Don’t be afraid to speak up and find a doctor that works for you. Don’t worry about offending someone.
I’m the same way, but don’t worry about being offensive by getting a second opinion or anything like that. This is ultimately your experience, so you’re allowed to own it.

Inspired by Ellis’s story?
Share your story, too!
Skin Cancer (Melanoma) Stories
Chris K., Melanoma, Stage 4 (Metastatic)
Symptom: Swollen lymph nodes in the neck
Treatments: Surgeries (lymphadenectomy, wide local excision, reconstruction), Immunotherapy (neoadjuvant immunotherapy – ipilimumab and nivolumab, PD-1/LAG-3 combination – nivolumab and relatlimab-rmbw through a clinical trial)
…
Jenn F., Melanoma, Stage 4
Symptoms: Initially asymptomatic, then a lump in the groin enlarged and changed color
Treatments: Surgery (lymphadenectomy), radiation therapy (Gamma Knife radiosurgery), immunotherapy (Opdivo/nivolumab and Yervoy/ipilimumab)
…
Tara S., Melanoma, Stage 1B
Symptom: Mole on back that became thicker and changed color
Treatments: Surgeries (wide local excision, sentinel lymph node biopsy)
…
Brittanny G., Melanoma, Stage 3A
Symptoms: Mole that enlarged, changed shape, and became dry, patchy, and flaky, fatigue
Treatments: Surgeries (wide local excision, lymphadenectomy), immunotherapy
…
Teresa B., Recurrent Breast Cancer (Hormone-Positive), Oral Cancer (Lip Cancer), and Skin Cancer (Melanoma)
Symptoms: Lip cancer: chapped lips & a pimple-like growth on lip, breast cancer: enlarged left breast with lump, melanoma: none
Treatments: Surgeries (bilateral mastectomy with reconstruction, lumpectomy, craniotomy, Mohs, surgery, wide local excision), hormone therapy, radiation therapy
…
Jennifer M., Melanoma, Stage 4 (Metastatic)
Symptom: Persistent cough, body and chest aches and pains, night sweats, fatigue
Treatments: Immunotherapy, surgeries (lung resection, pericardiectomy)
…









Leave a Reply