Rebuilding Her Identity: Alicia’s Pancreatic Neuroendocrine Cancer (pNET) Experience
Stage 4 pancreatic neuroendocrine cancer (pNET) reshaped Alicia’s life in ways she never anticipated. She describes herself as someone who “was always… a healthy person,” a full-time mom, professional makeup artist, and former salon owner who poured her energy into her children, her clients, and her 22‑acre farm. Looking back, she now sees how long she sidelined her own needs. She pushed through escalating symptoms while telling herself it was just stress from a difficult home environment and an emotionally taxing divorce.
Interviewed by: Carly Knowlton
Edited by: Chris Sanchez
The early signs of pancreatic neuroendocrine cancer, a type of pancreatic cancer, were subtle and easy to dismiss. In Alicia’s case, they included hormonal changes, intense acne despite her expertise in skincare, flushing she did not yet have language for, stomach pain, and nausea so reminiscent of pregnancy that she kept taking pregnancy tests. As her divorce progressed and her health insurance fell away, financial barriers compounded the problem. Even as her stomach pain worsened and her legs became so swollen she could not bend them, she hesitated to go to the hospital.

Everything shifted when loved ones physically helped her into the car and drove her to the emergency room. A cascade of scans, GI referrals, and ultimately blood work led to the call that changed everything: she had an urgent appointment with an oncologist that same day. The diagnosis, stage 4, grade 3 pancreatic neuroendocrine cancer, meant starting with oral chemotherapy and monthly hormone therapy injections. She then had surgery to remove part of her pancreas and her spleen, followed by liver-directed treatments. Later, she had chemotherapy infusions with a take-home pump.
Alongside the side effects of nausea, fatigue, pain, night sweats, and the reality of lifelong treatment, came deep emotional work. Alicia speaks candidly about feeling crushed by the timing of her diagnosis, the impact of a toxic relationship, and the heartache of stepping back from the makeup work that once fueled her sense of purpose. Over time, she rebuilt a new identity centered on integrative care: yoga, meditation, journaling, putting on her own makeup, and intentionally celebrating every victory, no matter how small. Now, she is channeling her experience into videos and advocacy so that others with pancreatic neuroendocrine cancer might recognize symptoms earlier and learn to prioritize themselves sooner than she did.
Watch Alicia’s video and read through the edited transcript of her interview. You’ll find out more about her story:
- Listening to persistent hormonal and digestive changes, like flushing, severe stomach pain, and unexplained nausea, can be critical in catching pancreatic neuroendocrine cancer earlier, even when life stress makes symptoms easy to dismiss.
- Financial barriers and lack of insurance delayed Alicia’s workup, underscoring how structural issues can slow diagnosis even when someone knows in their gut that something is wrong.
- Treatment for stage 4 pancreatic neuroendocrine cancer can include multiple treatments. It is the disease and its response to these treatments, not the patient, that dictate outcomes.
- A universal truth Alicia highlights for patients: you know your body best. When something feels off, it is important to keep advocating, even if you have been brushed off before or are used to putting yourself last.
- Alicia’s transformation centers on learning to ask for help and to rebuild her identity beyond work and caregiving. It also includes embracing daily practices, like yoga, meditation, journaling, and doing her own makeup, that make room for joy and small victories alongside lifelong cancer treatment.
- Name: Alicia S.
- Age at Diagnosis:
- 37
- Diagnosis:
- Pancreatic Neuroendocrine Tumor (pNET)
- Staging:
- Stage 4, Grade 3
- Symptoms:
- Abdominal pain
- Nausea
- Swelling
- Extreme fatigue
- Hormone-related changes
- Severe acne
- Flushing
- Treatments:
- Chemotherapy: CAPTEM and FOLFOX
- Surgeries: distal pancreatectomy, splenectomy
- Radiation therapy: Y-90 radioembolization
- Hormone therapy: lanreotide
- Bland embolization
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions. The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My stage 4 pancreatic neuroendocrine cancer diagnosis
- Passion for skincare, makeup, and family
- Life as a mom, business owner, and farmer before my diagnosis
- Early red flags and hormonal symptoms
- Reaching a breaking point and going to the ER
- Financial barriers, costly testing, and emotional toll in 2020
- Getting the call and meeting my oncologist
- Learning I had “the good pancreatic cancer”
- Rare neuroendocrine cancer and delayed diagnosis
- Feeling dismissed, yet knowing that something was wrong
- Paying out of pocket and cancer’s financial strain during chemo
- My initial treatment: Oral chemo and hormone therapy
- Surgery to remove part of my pancreas and spleen
- Liver-directed treatments: Chemoembolization, bland embolization, Y90
- Starting FOLFOX chemo, infusion pumps, and a changing oncology team
- Recovering from major surgery and rebuilding a routine
- Side effects from chemo and radiation
- My mental health struggles after diagnosis
- Parenting teen boys while in treatment
- The emotional challenge of asking for help
- Transitioning to FOLFOX maintenance and managing side effects
- Having to stop doing professional makeup
- Losing and rebuilding identity after cancer and divorce
- Prioritizing yourself, your energy, and a healthy environment
- My daily routine: Yoga, meditation, journaling, and makeup
- Celebrating my small victories and tracking my progress
- My long-term treatment plan, and living with chronic cancer
- Reaching a better mindset and helping others get there sooner
My stage 4 pancreatic neuroendocrine cancer diagnosis
Hi, my name is Alicia, and I was diagnosed in June of 2020 with stage 4, grade 3 pancreatic neuroendocrine cancer.
Passion for skincare, makeup, and family
I am incredibly passionate about skincare and makeup. It is something that I have always done, and I have been in the industry since I was about 15 or 16. I am incredibly passionate about that.
I love animals. I think I gravitate towards them more than people sometimes, and when I am not feeling good, I hug my babies. I also love spending as much time with my family and friends as possible. They are incredibly important to me. Family and friends are everything to me.
Life as a mom, business owner, and farmer before my diagnosis
Before being diagnosed, I was a professional makeup artist and owned a salon. I would go and do on-location bridal and event makeup, and I really loved what I did.
I have two boys, so I was a full-time mom and a full-time working business owner. I was homeschooling my children; I only did that for a year, but we did try it. About a year and a half before diagnosis, I had moved to a 22‑acre farm, so I had some animals out there. Every day life was, I thought, completely normal. I thought I was doing well. I was incredibly busy, taking care of my kids, taking care of a farm, and doing everything for our household.
Because of that, I pushed myself to the side. I was never a priority; everything else took priority. Daily life was normal, probably just like everybody else’s: working, taking care of my kids, taking care of my home, and just doing everything.
Early red flags and hormonal symptoms
I had been living in a very stressful environment, and a lot of the symptoms I was experiencing got pushed off because of the type of symptoms this cancer produces. There are a lot of hormonal symptoms, and they are very easy to brush off, especially when you are under so much stress and anxiety.
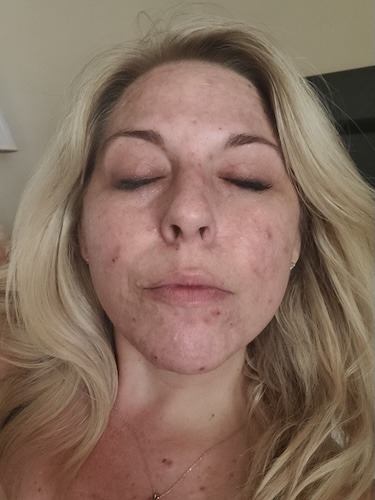
It started with emotional symptoms and feeling overwhelmed. My face was completely breaking out, and being a licensed esthetician and makeup artist for as long as I had been, I had always taken very good care of myself. When I could not get that under control, I blamed it on stress and anxiety.
A little over a year before I was diagnosed, I started having issues when I would eat, and my stomach would be in knots with stomach pains. Again, I thought I was under so much stress and anxiety, so everything was brushed off as that because of the type of symptoms this cancer produces. I was getting flushing, but at that point, I did not know what flushing was, just red splotchiness.
I had a lot of stomach pain. I was taking pregnancy tests because so many of the symptoms I was having, like nausea and not feeling well when I was eating, were very similar to pregnancy. Because of the hormonal issues, a lot of it felt like pregnancy, and I kept thinking, “How is this negative?“
Closer to diagnosis, I was going through a divorce, which amplified all the stress and anxiety. I was so encompassed with everything going on that there was so much I was not paying attention to. When you are taking care of your kids, your business, and going through a divorce, you get pushed to the very end of the list. I did not even make my own list of priorities, other than making sure I was put together so I could go to work and function.
Reaching a breaking point and going to the ER
I probably knew for sure by April of 2020 that there was something really wrong. I remember being at Easter dinner at my mom’s house and having to constantly get up and excuse myself to go to the bathroom because my stomach was in so much pain. That evening, I told her that something was not right, and I knew something was wrong.
Because I was going through a divorce, I did not have insurance, so I kept pushing it off. I did not financially have the means to go, and I did not have insurance, so I ignored it even though I knew something was wrong. Cancer was never on the radar. I always considered myself a healthy person. If I got sick, it was because my kids were sick, and I would go to a minute clinic and say, “My kids have strep; I have strep.” I did not even have a primary care physician and never prioritized my own health, just my kids’ health.
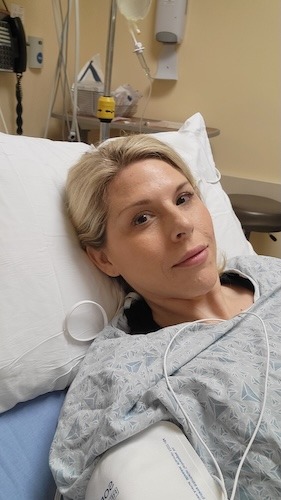
After April, the symptoms continued to worsen. My legs became so swollen that I could not bend them. People kept telling me I needed to go to the hospital, and I kept saying I was not going, that it would pass. Finally, I realized there was something really wrong, and I needed to go.
I could not move my legs, so they had to pick me up, put me in the car, and drive me to the emergency room. They did scans and blood work in the ER and then referred me to a gastrointestinal specialist. I was not told that there were any masses. The referral was to a doctor I would not be able to get in with for a couple of months, which was not an option with how I was feeling.
Fortunately, everything kind of fell into place. My parents had a doctor friend who referred me to a gastrointestinal specialist who could see me much quicker, and I went to see him.
Financial barriers, costly testing, and emotional toll in 2020
I did not have insurance, so I had to pay out of pocket for the appointment. At that point, it was obvious that something was wrong, so I had to find the funds to go.
I remember the doctor saying he thought it was hepatitis, and I wondered how that could even be possible. He sent me for blood work, and I had to pay for that out of pocket as well. It was incredibly expensive. During 2020, because of COVID, it was very difficult to get into places, and everything was very expensive.
I remember the nurse telling me she had never cried for a patient before, and she was bawling her eyes out when she had to charge me for my blood work. She looked through all the tests they wanted to run and knew there was nothing she could take off, and we both sat there crying. I felt like I did not have a choice any longer; we had to do the blood work.
I left still not thinking about cancer at all. Even going to the ER, seeing the GI specialist, and going for blood work, cancer never once popped into my head.
Getting the call and meeting my oncologist
The day after my blood work was done, I got a phone call first thing in the morning from the doctor’s personal phone, which is never good. He told me they already had my blood work back, he had already called and talked to an oncologist, and I had an appointment that day at 2:00. He told me I needed to go that day and meet with him.
I held it together until I ended the phone call, then I collapsed in my kitchen, bawling my eyes out and feeling completely crushed. I had been getting myself out of a bad situation, going through a divorce, and finally feeling like I was getting to a good place, and then I felt like I was crushed back down. I could not even make the phone call to my family because I was so emotional.
My now-fiancée was with me. He is the one who picked me up, put me in the car, and took me to the emergency room, telling me I did not have a choice. He really saved my life, because I probably would not have gone and would have continued to push it off. I had to give him the phone to call my family and tell them something had come back on my blood work and that I had an appointment with an oncologist.
Learning I had “the good pancreatic cancer”
I was told I had an appointment with the oncologist that day, and I am so blessed to have an amazing family and support system. My mom and stepdad live two hours away, and they met us at the doctor’s office.
My mom went in with me. During COVID, nobody could go into these appointments with you, but I was very fortunate that they allowed my mom to come in. I remember talking with the oncologist.
I am trying to remember whether they already knew at that point that it had something to do with my pancreas, or if I was sent for scans first and then had a biopsy. Either way, the oncologist said if we were lucky, it would be “the good one,” the good pancreatic cancer. There is no good cancer, and I do not think there is any good cancer, but fortunately for me, mine was the “good,” if you want to call it that, type of pancreatic cancer, because it is more slow‑growing.
The problem with a slower‑growing cancer is that most patients are not diagnosed until they are much further along because the symptoms are so easy to brush off. Another issue with neuroendocrine cancer is that it can appear in places other than the pancreas, and it is a rarer type of cancer. Because of that, most doctors do not immediately think of it, and a lot of patients get pushed off with explanations like “it is just this” or “it is just that,” when it is not.
Rare neuroendocrine cancer and delayed diagnosis
We put a lot of weight into our doctors’ words, especially if we have never prioritized ourselves or our health. Many patients just go with what they are told; if they do not push back, they keep getting brushed off, and time passes until they are diagnosed at later stages.
Before diagnosis, there was nothing that was a huge standout red flag to me, saying, “You need to go now.” There is no telling how long I had been living with this cancer without realizing it. I am stubborn and push myself through everything, so any symptom that popped up was pushed aside with that mindset.
Feeling dismissed, yet knowing that something was wrong
It can be very frustrating for patients because you know something is wrong, but when you tell a doctor how you feel, and they brush it off as something lesser, you think they know better than you do. In reality, we know our bodies, how we feel, what feels normal, and when something does not.
If you are not prioritizing yourself or you are not even on your own list of things to think about, you are not in tune with your body. That makes it even easier to ignore or minimize symptoms.
Paying out of pocket and cancer’s financial strain during chemo
Paying out of pocket was not an option I felt like I could avoid. If it meant maxing out a credit card, I still had to do it. During the divorce, I had closed my salon prior to 2020, so I did not have my salon income or anything coming in.
For me to come out of pocket was nearly impossible, but I still maxed out a credit card to get the blood work done because at that point, I knew I had to. Thank God I did.
My initial treatment: Oral chemo and hormone therapy
Once I met with the oncologist and the staging and pancreatic involvement were clear, I was told my primary tumor was in the tail of my pancreas and had spread to my liver. I was told the masses were too large for surgery, so that was not an option for me initially.
I was started on chemotherapy, specifically an oral chemo called CAPTEM. I was incredibly grateful for that because I was able to be at home in my own environment, where I felt comfortable, instead of being in a hospital. Being home meant I could have my support system around me, whereas others going through treatment at that time had to be alone in treatment rooms due to COVID.
I was mentally in a bad place before and after diagnosis, so it was a blessing to do oral chemo at home. I do not think I would have had such a positive response if I had not had my support system around me. We initially discussed 12 rounds of CAPTEM. It is two weeks on, two weeks off, in a repeating cycle. My body made it through 11 cycles and then said that was it; we could not do any more.
I have been on lanreotide injections monthly since the beginning, and that never stopped.
Surgery to remove part of my pancreas and spleen
After cycle 11, we did scans. Thankfully, my body responded very positively, and the primary mass at the tail of my pancreas had shrunk enough for me to be a candidate for surgery.
I had surgery to remove the tail of my pancreas, and they also removed my spleen. After that, I had to focus on recovery. Since the beginning, alongside all this, I continued my monthly lanreotide injections.
Liver-directed treatments: Chemoembolization, bland embolization, Y90
After surgery and a period of recovery, I had a break. About a year after surgery, follow‑up scans showed growth in the masses on my liver.
Because of that, it was decided that I needed to start treatment again. The treatments then included chemoembolization, bland embolizations, and Y90 radiation. I went through those and was able to have another break, which was really nice.
Starting FOLFOX chemo, infusion pumps, and a changing oncology team
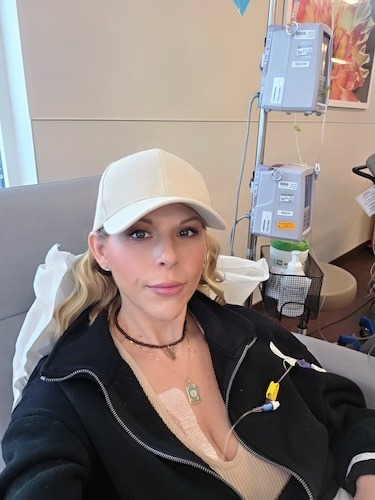
In October of 2024, my scans showed that I again needed to restart chemotherapy. I started on FOLFOX in December 2024, which required me to go into the treatment room for multiple hours.
After the infusion, I had to leave with a pump that continued to deliver chemotherapy for the next two days. Then I had to go back two days later to have the pump removed, and then I had a week before going back again. So, every other week, I was doing this.
It is very difficult to have a schedule like that because you cannot plan anything. First, with cancer in general, you never know how you are going to feel or how much energy you will have. On top of that, being connected to pumps, not feeling good, and not sleeping well made it even harder.
I have dogs, which is amazing, but because my port was connected to a pump, nobody could sleep in the bed with me because we did not want to risk anything getting pulled out.
In May of 2025, my original oncologist moved to Colorado. He referred me to another oncologist who is actually a neuroendocrine cancer specialist. My initial oncologist was not a specialist, but I was incredibly fortunate that he was someone who looked for rare things and was quick to diagnose me. During his care, every time I had a scan, he presented my case to a hospital board, so other oncologists weighed in.
The oncologist he transferred me to had always weighed in on my case when it was presented. That has been amazing. “
Recovering from major surgery and rebuilding a routine
Recovery from the big surgery was very difficult. I was in the hospital for about a week and then came home and spent a lot of time in bed.
I tried to do as much as I could to work myself back into a routine, because routine is incredibly important to me. It gives me something to look forward to and a “next thing” that I need to do. All of the things I needed to do were things I needed to put in place to support myself in healing and recovering.
Side effects from chemo and radiation
With the initial chemotherapy, I was incredibly sick. It was very hard on my body. I was already in pain before starting treatment, and that pain was amplified once chemotherapy began.
I was very sick and literally had to have a bucket next to me at all times. I was completely drained of energy and slept a lot. Fatigue was huge. I could not eat and had no appetite, whether it was because I was afraid of throwing up or because I could not really taste food.
I was hurting and uncomfortable, dealing with fatigue, stomach issues, and night sweats. Those are the side effects from that period that I remember the most.
My mental health struggles after diagnosis
To be completely honest, in the very beginning, when I was diagnosed, I was not in a good mental place. I felt like I had just started clawing my way out of a hole and had finally, after over a decade, found some happiness, and then I felt completely crushed.
On top of the cancer, I was going through a divorce in a toxic situation with a narcissist who was also an alcoholic. Even though I was sick and fighting, that did not stop him from adding to it and doing everything he could to make it worse.
It was very difficult to get to a good mental place because it was not just the cancer I was battling; there was so much more on my plate that I was trying to work through mentally. In the beginning, I was not in a good mental place at all, and my support system helped me the most because I could not do that for myself at that point.
Parenting teen boys while in treatment
Being a mom during all of this was really difficult. Luckily, my family is incredibly close, both emotionally and in proximity, so I had help when I needed it.
I tried to function as normally as I possibly could when my kids were there. I was still making their lunches and doing what I could, even if I was crawling up the stairs at the end of the night. I wanted to do everything I could to be the mom they knew, the person I knew, and the mom I did not want to go away. I did not want them to suffer because of what I was going through.
When I was diagnosed, my two boys, who are 14 months apart, were in eighth and ninth grade. I had just moved them from two hours away back to where we had lived before owning the farm, so at least we were in an area they were familiar with.
The emotional challenge of asking for help
One of the most difficult and emotional things for me in the beginning was coming to terms with the fact that I was going to have to ask for help. I was never one to ask for help and was always the one to do everything. I am very independent and have been that way my entire life.
I remember either just dropping off my boys with their dad or going to the store. I had to pull over and park my car, and I broke down in tears, realizing I could not do this alone. There was no way I could continue to function at the level I was functioning, do everything, and still try to help myself.
That was probably the point where I realized I had not been taking care of myself or prioritizing myself. Everyone else had come before me, and I needed to step back, ask others to step in and help with the things I was doing, and focus more on doing things for myself and my body and healing. I needed to do that so I could go back to being the mom I wanted to be and the person I wanted to be. Asking for something was probably the most difficult thing for me.
Transitioning to FOLFOX maintenance and managing side effects
I am still on chemotherapy, and I recently went back on treatment. With FOLFOX, I am currently in maintenance mode.
Now I am very fortunate that I do not leave with the pump. They tapered back some of what they were doing because I was having a plethora of side effects from the treatment. They wanted to see if backing off a bit would improve the side effects that were greatly impacting my life.
Having to stop doing professional makeup
I am not currently able to do hair and makeup on the side, even though I am so passionate about it and love it so much. My big thing was doing makeup for people because I could see their confidence grow while they were sitting in my chair.
I would have girls or women who, for whatever reason, had beaten themselves up emotionally, or life had just worn them down, and they did not feel good about themselves. As I did their makeup, I would see a boost in their confidence, and that made me so happy and was so fulfilling for me. I think that is why I was so passionate about it.
Unfortunately, because I never know how I am going to feel, I can no longer take on clients. You cannot cancel on a bride at the last minute, and I would never do that or put anyone in that position. With my body not being reliable, it is not something I can continue to do. That was very difficult because I got so much joy and fulfillment from providing that boost of confidence for people.
Losing and rebuilding identity after cancer and divorce
We talk a lot about losing our identity. My identity was a wife, a mother, and a business owner. I went through a divorce, my kids were no longer with me full‑time, and I was not able to do makeup, so everything I knew of myself was suddenly gone.
I had to pivot and figure out what I was going to do that would make me happy. It took a couple of years, and I had a very difficult time. I would say that within the past two to three years, I have really been able to make a mental shift, and that has made all the difference.
Most recently, because doing makeup and boosting other people’s confidence brought me so much joy and made me feel fulfilled, I decided to find a way to take that feeling and help others. Now I am making videos and trying to get the word out about this type of cancer, about prioritizing yourself, and about creating an environment where you can thrive and that is healthy for you.
When you are going through chemo, radiation, cancer, or any illness, creating a healthy environment for healing and thriving is so important. I am really excited that I have found that focus, because it has helped fill the void I have felt since no longer being able to do makeup, have the salon, and do all the things I was so passionate about.
Prioritizing yourself, your energy, and a healthy environment
I really hope that people will sit back and think about what they are spending their energy on, who they are spending their energy on, and where they are prioritizing themselves. We get so busy and focused on so many other things that we are not in tune with our bodies and are not prioritizing ourselves or putting ourselves in a position to thrive.
When we are able to make a mental shift to a more positive place, I really feel like our body listens to that. That is when you start to see more improvements, even if it is as simple as getting up and feeling excited to have something to look forward to instead of waking up and thinking, “I hurt, I do not want to get out of bed.”
There has to be a mental shift to positivity and things to look forward to, to keep you going and fighting. You have to make that mental decision that you are going to fight.
Even now, I still sometimes push myself too much because I am stubborn and was so used to doing everything and not asking for help. Sometimes I get myself in trouble and realize I am going to hurt later, and then not be able to do something fun.
I am very blessed to have people in my life who will step in and do the not‑so‑fun things, like laundry or grocery shopping, so I can reserve my energy for things I enjoy, like a date night with my fiancée.
My daily routine: Yoga, meditation, journaling, and makeup
When I talked about my routine and trying to put a routine in place for me, that looks like getting up and doing yoga in the morning and meditation. I journal, and I really try to make sure that every day I am putting myself together and putting my makeup on, even if I cannot do it for other people, doing it for me.
When I feel like I look good, I feel better. When you are put together, and you walk past a mirror, and you are not feeling good but still look like you, there is a huge difference between that and walking past a mirror looking sick and feeling sick. That can really impact how you feel mentally and how you fight.
When I can get up and do my yoga, my meditation, my journaling, and my makeup, that is a victory for me. Even if I cannot accomplish all of those things on a given day, because there are days when it is not going to happen, I will pick one or two of those things. Even accomplishing one of those things is a victory.
Celebrating my small victories and tracking my progress
We need to capitalize on every victory, no matter how small it is. That applies to everything in life.
When I look at my blood work and see that, even if it is not a huge difference, it is moving in the right direction, I choose to be happy and excited about that. If we do not recognize those smaller achievements and only focus on big milestones, we are probably not going to be as happy with our progress.
Recognizing little victories along the way, no matter how small, makes things more positive.
My long-term treatment plan, and living with chronic cancer
As far as my long‑term treatment plan, I have been told that for the rest of my life, I will have to be on some kind of treatment. That can be incredibly frustrating to hear.
I do not know if, at some point, the treatment will change from one thing to another. There are so many unknowns when you are going through cancer, especially when it is chronic, and you are going to be living with it for the rest of your life.
When the oncologist says you will have to be on treatment for the rest of your life until science catches up and comes up with a cure, that is where we are right now. I know what my current treatment plan is, but everything is up in the air, and you have to go with the flow.
I do not know at what point this treatment will no longer be as effective, and we will need to find something else. For me, incorporating yoga, journaling, doing things for myself, and making plans with friends for lunch dates and activities that bring me joy is just as important as chemotherapy and other treatments.
It has to be both; it cannot be just one or the other. It really has to be more of an integrative approach because one is not going to be as effective without the other. You need a very strong, motivated mindset to go along with your treatment to get the most out of it, in my opinion.
Reaching a better mindset and helping others get there sooner
I do have a really good mindset about it now, thank goodness. I am hoping that, by other people hearing this, they will be able to get to that point sooner than I did and see the benefits more quickly.
I wish I could put this message out on a big amplifier for everybody. If people can learn from my mistakes, then they do not have to go through the same things. If they can catch this sooner than I did, or even if it is not cancer‑related but about prioritizing yourself for your mental health, those things are very important.

Inspired by Alicia’s story?
Share your story, too!
Related Stories
Regina J., Lung Neuroendocrine Tumor
Symptoms: Wheezing, back pain, coughing that sometimes produced blood
Treatment: Surgery (partial lung resection)
…
Tabbie V., Pancreatic Neuroendocrine Tumor (pNET)
Symptoms: Abdominal pain, unusual organ “inflammation” feeling when walking, fatigue
Treatments: Chemotherapy (oral and IV), surgeries (Whipple procedure or pancreaticoduodenectomy, liver resection or partial hepatectomy)
…
Hayley O., Pancreatic Neuroendocrine Tumor (pNET)
Symptoms: Severe right-sided pelvic pain, nausea, diarrhea
Treatment: Surgery (pancreaticoduodenectomy or Whipple procedure)
…
Drea E., Gastric Neuroendocrine Tumor (gNET), Stage 3, Grade 1
Symptoms: Fainting spells, fatigue, dizziness, anemia, shortness of breath, absence of menstruation, unexplained weight loss, night sweats
Treatment: Surgery (total gastrectomy with a Roux-en-Y reconstruction)
…








Leave a Reply