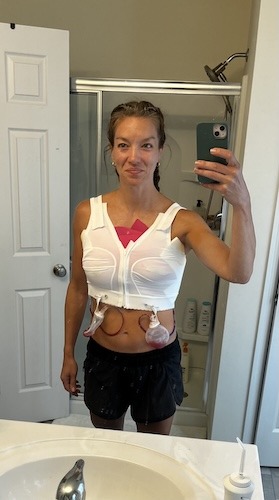
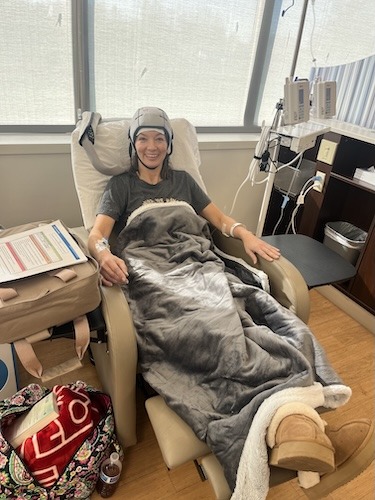
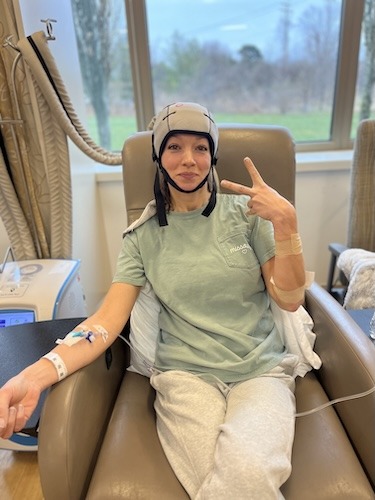
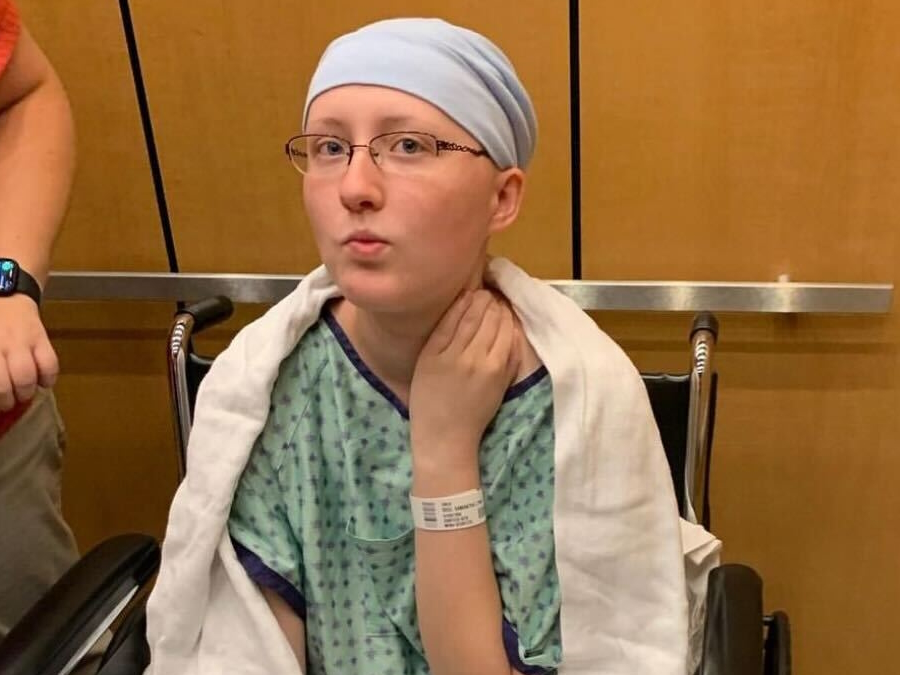
From Hip Pain to Metastatic Breast Cancer: How Mom and Teacher Erica Shows Up for ALL of Her Kids
Erica lives with metastatic breast cancer. She describes herself first as an elementary PE teacher and single mom to two active kids, and secondly as a patient. She was initially diagnosed with stage 1 hormone-positive, HER2-negative breast cancer in July 2024, and believed she was finally moving back into “normal life” after chemotherapy, a double mastectomy, and reconstruction. When new, relentless pain in her hip, ribs, spine, and shoulder blade led to an ER visit, scans and a biopsy confirmed metastatic breast cancer that had spread to her bones. The news, delivered abruptly in the middle of the night, felt devastating and unreal. She spent a long time in denial, trying to process what this diagnosis might mean for her future and her family.
Interviewed by: Nikki Murphy
Edited by: Chris Sanchez
Today, Erica’s treatment for metastatic breast cancer includes a monthly hormone-suppressing injection and regular scans, along with integrative care, supplements, and a strict routine to support her health. She previously tried a combination of a targeted therapy and a hormone therapy drug, but the combination caused severe fatigue and low blood counts, so her oncology team adjusted the plan. Targeted radiation to a painful hip lesion around the femoral head gave her back the ability to walk without crutches, teach more comfortably, and be present in the gym again. She also manages hot flashes, tiredness, and brain fog, making daily choices to modify workouts and protect her bones while still staying as active as she safely can.

Erica’s experience with metastatic breast cancer has changed every part of her life: how she parents, shows up in her classroom, and thinks about the future. Her children know she has cancer and see her as a fighter, but she works hard to shield them from the hardest moments, often crying alone in the shower or car instead of in front of them. At school, students and families surround her with cards, T-shirts, fundraisers, and a deeply felt sense of community that has eased some of the financial burden of cancer treatment.
At the center of it all is a quiet, disciplined determination. Erica organizes her days around movement, nutrition, supplements, work, faith, and time with her kids. She talks openly about scanxiety and uncertainty, while also defining hope as being there to see her children graduate, get married, and have kids of their own. For her students, she keeps repeating one message she lives out herself: you can do hard things, even when life looks very different from what you expected.
Watch Erica’s video and read the edited transcript of her story to learn more.
- Staying connected to meaningful roles, like teaching and parenting, can help some patients with metastatic breast cancer feel more grounded and “normal” in the middle of constant medical appointments and scans.
- Adjusting treatment plans when side effects become overwhelming is not a personal failure; it reflects how a cancer responds to therapy and the need to find an approach that supports both effectiveness and quality of life.
- Community support from coworkers, students’ families, and strangers can ease the financial strain of metastatic breast cancer and remind patients that they do not have to navigate the experience alone.
- A universal truth in Erica’s story is that it is possible to feel deep fear and grief and still practice gratitude, faith, and hope in the same breath.
- She describes a powerful transformation from denial and shock after her metastatic breast cancer diagnosis to a disciplined, intentional way of living, where she structures her days around her health, her faith, and her children’s future.
- Name: Erica H.
- Age at Diagnosis:
- Stage 1: 39
- Stage 4: 41
- Diagnosis:
- Hormone-Positive, HER2-Negative Breast Cancer
- Staging:
- Stage 4 (Initially Stage 1)
- Symptoms:
- Stage 1: Appearance of lump in left breast
- Stage 4: Severe pain in hip, ribs, spine, and shoulder blade
- Treatments:
- Surgeries: double mastectomy, reconstruction
- Chemotherapy
- Cold caps
- Radiation therapy
- Hormone therapy: aromatase inhibitor (letrozole)
- Targeted therapy: CDK4/6 inhibitor (ribociclib)
- Integrative care
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My metastatic breast cancer diagnosis and teaching career
- A day in the life: Teaching with metastatic breast cancer
- Monthly hormone injections and bloodwork
- How my stage 4 diagnosis changed my daily life
- Why I continued teaching during treatment
- Working around germs during metastatic breast cancer treatment
- Walking into the gym each day with my students
- Community support, fundraisers, and the financial burden of metastatic breast cancer
- How teaching helps me feel normal
- The hidden discipline behind living with metastatic breast cancer
- Finding motivation in my children
- My first symptoms and path to my metastatic breast cancer diagnosis
- Hearing the official metastatic breast cancer diagnosis
- How far the cancer spread
- All my treatments, from my initial stage 1 breast cancer to now
- My treatment schedule around teaching and current side effects
- My thoughts on clinical trials and future treatment options
- Coping with hard days and mental health
- How metastatic breast cancer changed my roles as mom, teacher, daughter, and girlfriend
- Talking to my kids about cancer and protecting their childhood
- Scanxiety, stable breast cancer, and tumor shrinkage
- What hope means to me now
- Life lessons I want my children and students to learn
- How metastatic breast cancer changed my view of people
My metastatic breast cancer diagnosis and teaching career
My name is Erica. I was diagnosed the first time with stage 1 hormone-positive breast cancer, HER2-negative, in July of 2024. The second time I was diagnosed was on October 31st, 2025, with stage 4 metastatic breast cancer, same hormone-positive, HER2-negative.
I am an elementary PE teacher. I have been doing that for about 12 years now.
A day in the life: Teaching with metastatic breast cancer
A typical morning: I am feeling good enough right now that I like to go to the gym to work out, then come back and get my two kiddos ready for school. They get to go to school with me, so that’s perfect.
I go to my elementary school, and when I get there, I am in charge of setting up the gym for everyday activities. We do different things. Another PE teacher does the parent drop-off while I set up. We have some fifth graders who help us set up every day for PE.
We have ten total classes a day, and they are 30 minutes apiece. Everyone gets to have PE every day at our school, which is awesome. I love that.
After that, I coach basketball. That just ended, but I did coach my daughter and my son. That was my sport too, so I coached both of them. Now we are switching over into the spring sports, so now I am their taxi driver to all their different sports.
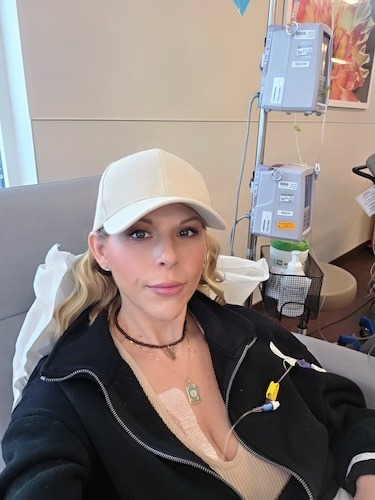
Throughout the day, I take different vitamins and supplements four times a day. I am taking a lot of different things. I have another medication, the hormone suppressant that I get injected with every month at my oncologist’s office.
Monthly hormone injections and bloodwork
Usually, when I go get my injections, they do blood work for me every single month, too. Before I get that injection, I get my blood work done to make sure that my levels are still good. Then I get my injection.
I try to do that before school because I’ve missed a lot of school, and I don’t want to miss it if I don’t have to. So I usually go straight to school from there.
This injection hasn’t been very bad. The injection itself isn’t bad. It is sore; they put something on, and they numb me before they do it, but I don’t really have side effects that hinder me from doing my job or anything like that.
Since it’s a hormone suppressant, I have hot flashes. That’s the biggest thing that’s bothering me right now. I haven’t had a ton of joint pain. When I was on ribociclib, I did notice my hair was thinning again and things like that. But I’m not on that anymore, and I’m not as tired. When I was on that, my white blood cell counts were very low, so I was really exhausted.
By just doing this hormone suppressant alone, I’m not having as bad a set of side effects as I was before. I’m lucky that I’m feeling as good as I feel right now. I feel so good.
How my stage 4 diagnosis changed my daily life
When I was first diagnosed, I was in a ton of pain. It was super scary, obviously. There were days when I was thinking, “How am I going to do this?” I was in so much pain.
I had a lesion on my right hip, right where the femoral head goes into the hip socket, and that was causing me a lot of pain. Some days I needed crutches. I couldn’t walk, and I was thinking that was going to be my new normal, and hoping that it wasn’t.
Luckily, I went and met with a radiologist, and they said they thought they could do four sessions and that would be able to help me. That was targeted therapy. Since I was in so much pain, I decided to do that.
My last session was on Christmas Eve. It actually made a difference really quickly. They said it could take weeks, but I was lucky that it did something quickly for me. I was able to walk, and I didn’t have that pain. I had been limping, and everybody was worried about me and asking my kids questions. It looked painful. It was painful. It was hard to walk.
I had to sit down a lot while I was teaching instead of being active like I usually am. Luckily, that has changed. I’m very thankful that that worked out for me.
Why I continued teaching during treatment
I’ve always been an active person, and I know that breast cancer slowed me down. My kids go to the school too. If I just sat at home by myself, that is when my brain starts running with different thoughts. I like to stay busy.
I love my job, and I love seeing my students every day. They have been awesome. They have sent me so many cards, and they are always checking on me. I don’t like them to worry about me either.
I’m in a hard position with the elementary kiddos because they know that I have it, and they’ve said some really silly things to me. They hate that I have it, but I do feel like I’ve been able to show up and still be a good PE teacher.
I do have a little bit of brain fog. If I’m trying to talk to classes about different things that we are doing that day, I’ll lose my train of thought more regularly than I used to. But I need to keep a routine. It keeps me more positive, and I just like being around them.
If I sat at home and did not work, I think that would cause me to spiral a little bit and just sit with what’s going on.
Working around germs during metastatic breast cancer treatment
My doctors, my oncologists, were really concerned about me being around germs. They said that I could wear a mask if I wanted to, to protect myself. I feel like sickness has been so wild lately.
Everybody has been sick. My daughter had flu A, and then a couple of weeks later, she got flu B. In between that, my son had strep. So not only do all the kids in the elementary school have germs, but my own kids do too. Somehow, I have been able to avoid that. I haven’t gotten the sickness, which I’m really surprised about.
They were really worried about that for me. I do think that some of the supplements that I’ve been taking have helped me stay healthy during this. I think that being in the sun and being outside and doing things like that helps keep my natural immune system up too.
Walking into the gym each day with my students
We get every class for 30 minutes a day, so it’s something new every 30 minutes. We are not with the same students all day, and every class is something different. We move on pretty quickly.
I’ve been doing this for so long that I don’t put too much thought into it. This is what I’ve done, so I go to work and do what I normally do. It hasn’t been too different. Now that the kiddos have seen me able to walk without limping, there haven’t been as many questions as there were in the beginning.
They tell me they hope that I feel better and say they are sorry that I have cancer. I had one student who told me that his grandma had what I had, but they had to put her down. He didn’t mean it like that; it was just coming from the mouths of babes. They all mean well.
When I go in, it’s just another day for me. I’m doing what I love to do, and I’m thankful that I have a job that I love. My coworkers are great, and the whole school system has really pulled together for me. They have supported me in different raffles and other ways. They’ve been amazing. I’m lucky with the school district I’m in and with all the students and their families.
Community support, fundraisers, and the financial burden of metastatic breast cancer
One of my coworkers is one of the high school football coaches, and I teach some of the sons of the football coaches. The head football coach and the team always have a breast cancer awareness game. They did fundraising for me that night.
They sold t-shirts that everyone in the district or anyone at all could buy. People bought a bunch of shirts, and they showed me support that way. Everyone in the school was wearing those shirts one day. It was pretty emotional to see that support.
That was the first time around. The second time around, they set up a GoFundMe page for me. It’s shocking to me, the amount that they raised for me, because treatment is so expensive. I never realized how expensive it can be. I’m a single mom and a teacher, so it was very helpful.
Strangers and everybody in the community have shown up. I don’t know how I would have done it without them. My integrative doctor has told me about getting out of fight-or-flight mode. I asked how I was supposed to get out of that when I am thinking about fighting incurable metastatic breast cancer.
I think taking that financial burden off of me has helped me a ton.
How teaching helps me feel normal
Teaching has absolutely helped me. It makes me feel normal. I get to do the things that I love, and I get to see my kids at school interacting and being normal. It makes me forget about cancer, especially when I feel good.
When I was limping, that was a constant reminder. Even just transitioning kids from one class to the next was really tough. Now that I’m feeling much better after radiation and everything, I’ve been able to live my normal life again.
The hidden discipline behind living with metastatic breast cancer
Right now, I have to be so disciplined. People always say, “You’re so strong,” and I do feel like I’m strong, but I don’t feel like I have a choice with my two kiddos.
I am on a special diet, and I take different supplements four times a day. I’m trying to move my body every day. I’m trying to get in the sunlight every single day. I’m trying to keep my house clean, do the normal chores, and take my kids to practices.
It’s very time-consuming to get all the things in to make myself as healthy as I can, so I can try to keep my cancer stable or even shrink the tumors. I have to be very disciplined. I am tired, and I don’t want to work out, but I know if I keep my body strong, I am giving myself a better chance.
I’m not drinking sugary drinks anymore. I’ve been on a keto diet, which is hard for me — no snacks or coffees like I used to have all the time. I have to be really disciplined, and it’s really, really tough.
Finding motivation in my children
My kids are my motivation. They are why I do all of this. I want to see them grow up, and I just want to be here for them. That is my motivation.
I have a ten-year-old girl and an eight-year-old boy. Their birthdays are both in April, so next month she will be 11, and my son will be 9.
My first symptoms and path to my metastatic breast cancer diagnosis
I finished chemotherapy in February of 2025, and I had my exchange surgery because I had a double mastectomy. I had to wait a while to work out, maybe six weeks. After that, I was working out and started to get pain in my shoulder blade and in my hip.
I blew them off. I thought I had injured them somehow from working out. That went on and off for a couple of months. I couldn’t figure out why it wasn’t getting better or what I did to hurt it. Metastatic breast cancer never even crossed my mind.
The pain got pretty bad, and I was sick at a certain time, too. I wondered why I couldn’t get rid of this sickness. My body was aching so badly, and I could not figure out what was happening. The pain kept getting worse and would not go away. Even sitting hurt.
My boyfriend saw me crying because of the pain and said, “We’re going in. We’re going to at least get an X-ray or see what’s going on.” We went to the ER and sat there. We didn’t get checked out until probably 3 a.m. We went in around 11. I was so tired and delusional.
The doctor finally came in. He didn’t really have the best bedside manner and immediately said, “Yeah, it’s all over. We’re assuming it’s metastatic breast cancer.” I asked if he was sure and why he thought that. He said, “With your history.”
I was still not believing that was true. I thought there was no way. We were looking up other causes, like lesions, which could be something else. It wouldn’t have to be that. But they admitted me and did all the scans.
They did CT scans and MRIs with and without contrast. I was in so much pain during all that. They had me on all kinds of pain medications to try to keep me comfortable.
That’s how I found out. That’s what they said there. While I was admitted, they did a biopsy, and that confirmed it. It was very overwhelming and very hard to swallow that it was really happening. I never expected that. I feel like I’m one of the healthiest people I know. I never expected that, but here I am now.
Hearing the official metastatic breast cancer diagnosis
I was in denial. I didn’t believe it. It took me a long time to actually sit with that and cry about it and mourn that this is what is happening now.
I didn’t know what that meant. If you Google it, it’s very scary. When I first found out, it was bad. I was devastated. My whole family was devastated. We thought it was dire. I was thinking it was going to be a short period of time that I would be here. I didn’t know.
It was very scary. I feel like I just numbed out about it. It was really hard to accept.
How far the cancer spread
I had it on my shoulder blade. I had it on my femur. I had it in some places on my ribs. I had been having rib pain, too, and they found I had a broken rib from the lesions.
I had it on my ribs, my sternum, my spine, my femur, and my shoulder blade. My shoulder blade was causing me a ton of pain, too. Somehow, I didn’t have radiation on that one, but I haven’t felt that pain since I was in the hospital when I was first diagnosed. I don’t know why, but I’ll take it. I don’t feel that pain anymore.
All my treatments, from my initial stage 1 breast cancer to now
When I was first treated, I did four rounds of chemotherapy. I don’t know if that’s why I have these little pieces everywhere. I did a cold cap, so my hair’s still kind of wild, but I did cold capping during chemo.
They wanted to put me on a hormone suppressant, tamoxifen. I was on the fence about that and trying to decide. I ended up being diagnosed with metastatic breast cancer before I started taking that. That always makes me wonder if that’s what caused it, but some people have taken it and still had it come back.
There is no real right answer. I’m not going to blame myself for that because that would be even worse for me. I hadn’t started tamoxifen yet because I had heard about other people getting cancer from that as well. It’s a lot to take in and to know what to do. I had no idea, and I was trusting my doctors and trying to see what to do.
After that, when I went back, I had the same oncologist. My sister, right after I finished chemotherapy, was diagnosed with breast cancer as well. She had triple-negative breast cancer, so a different kind than mine, but we both have the same oncologist.
I went back in, and they put me on ribociclib and letrozole. I was not handling that combo well. It was making my numbers drop completely, so they took me off of that.
I am still getting the hormone suppressant injection every month. I have the option to either get my ovaries out or continue the shot. Right now, I’m doing the shot, and my oncologist is on board with continuing this since I’m stable. We’ll probably move on to something else if it shows progression.
Her goal for me is to put the cancer in the trunk. She says it’s always going to try to get back into the driver’s seat, and we just want to keep putting it back in the trunk. That’s our goal.
My treatment schedule around teaching and current side effects
Once a month, or every 28 days, I go get my injection and my blood work. I don’t have to miss school because I schedule that before school. My school doesn’t start until around 9:00, so I have time.
Every Thursday, I go to my integrative doctor and do different supplements and treatments with him. I get adjusted lightly because I have a risk of fractures due to my lesions. I go to him every week, every Thursday. I miss about an hour of school, but my co-teachers cover for me during that time. That’s kind of my plan period. I usually come in during the middle of my daughter’s class after that.
Every three months, I go for my scans. I do have to take off for that. I get different scans to make sure there isn’t progression or to see if there is progression.
Side effects right now, honestly, have not been that bad aside from the hot flashes and being tired. Then I think about how I’m not the same as I used to be. I can’t do the same things. I go to the same gym, but I have to modify a lot. I can’t do all the jumping because I could fracture something due to the lesions.
I’m tired, and the hot flashes make me not get as much sleep. The brain fog makes me feel like I’m not as sharp as I used to be, and that might be from all the medications and the chemo. But overall, I am feeling pretty good right now, and I feel blessed to feel this well.
My thoughts on clinical trials and future treatment options
The only clinical trial they’ve wanted to try with me so far was just a kind of testing. It wasn’t a new drug; it was a different way to test it. I opted out of taking that because I would have had to stay on the combination of ribociclib and letrozole, and I had gone off that anyway because it wasn’t working well for me.
I haven’t been in any trials yet. There is always that option, and I’m open to those things. I feel like even from when I was diagnosed to when my sister got diagnosed, there had already been advances. She was doing different things that I didn’t have the opportunity to do because they weren’t available yet. It’s wild that it’s progressing that fast.
There is always that option, but my oncologist hasn’t found one that fits me right now.
Coping with hard days and mental health
I do feel like I’m a positive person, but I am human. I definitely have rough days. It is hard. That’s why I try to keep myself busy. Being around all these little kiddos keeps me in a better mood.
I do have days where I break down, and it consumes me, but I try not to sit in that. I want to live for the day that I have and try to be grateful.
I’m 41 years old and was diagnosed with metastatic breast cancer at this age, thinking that I’m healthy, and especially thinking I was moving on from having the initial stage 1 breast cancer and that my life would finally go back to normal — and it didn’t. Now this is my new normal, and it’s tough and overwhelming a lot of the time.
I try my best not to sit in it. I believe in God, and that helps me a lot. My faith gives me hope, so that helps me.
How metastatic breast cancer changed my roles as mom, teacher, daughter, and girlfriend
This part makes me emotional. I used to be a high school basketball coach. I’ve been coaching my little ones, and my goal was to get back to coaching high school again. But I worry — am I going to be able to? Am I not going to be able to walk again? I don’t know what’s in the future, so I worry about that.
I am divorced, and about two weeks after I started dating my boyfriend, I was first diagnosed with breast cancer. He hung around, we got through it, and then we celebrated in Mexico. Then I found out I had metastatic breast cancer.
That is hard for me to process as a girlfriend because I want to possibly get married again. He has two young kids as well. I wonder if I even want to put them through that if I might not be here. Those thoughts go through my head.
My parents have been through so much because of this — my sister being diagnosed, me being diagnosed, and me being diagnosed again. That’s a lot of stress on them.
I hate that they’re worried about me. I want them to live their retired life and enjoy themselves, not worry about me. But I know I would worry about my kids, too, so I get it.
My kids, I don’t think they know how serious this is, and I don’t really want them to. They just know their mom as a fighter and think I’m going to beat it again. I want them to think that. This is nothing a little kid should have to think about.
A lot of things I want to do, I’m nervous about doing now. Even going on a field trip with my daughter — the fifth grade gets to go on a Smoky Mountain field trip to go hiking, and I’m going to be a chaperone. My principal said we might need to get somebody else just in case I’m not able to do it. That is hard.
I want to be able to do those things with my kids and have those memories with them. It has changed everything.
Talking to my kids about cancer and protecting their childhood
I bring my kids up in church, too, so I think they have that faith. We pray every night about things like that, and I think that gives them a little comfort. If something were to happen to me, they believe in heaven, so I think that helps them.
I think I’ve been able to hide the hardest parts from them. They haven’t seen me on really hard days. I try to keep that from them. I cry in the shower and in the car, but I don’t try to let them know.
They see me doing well right now. I feel great, so they’re not seeing a lot of the hard parts. I’m going to try to continue to do that for now.
Scanxiety, stable breast cancer, and tumor shrinkage
There has been no growth. I’m stable, and there has been some shrinkage, which makes me feel great. That’s a positive thing.
Since I came off ribociclib and letrozole, my oncologist wasn’t sure how my scans would look, but she was happy with them. She told me to keep going with this plan.
Scanxiety is real. I thought I was fine. We were driving to the hospital, and as soon as we got there, I just lost it. I didn’t realize I was keeping that in. I think I even hid it from myself.
Once we pulled up, it hit me: what do you do if it does progress? I don’t know yet. I know that happens for so many people. It is in the back of my mind, but I try to push that aside and live for the day.
What hope means to me now
Hope for me is seeing my kids graduate, seeing them get married, and seeing them have kids. That’s my hope.
I’m going to do everything I can to be able to do that. I know I don’t have the final say, but I’m definitely going to try. That is what I live for, and that is why I am so strict about everything that I do.
It’s hard, but it’s worth it. That is my hope.
Life lessons I want my children and students to learn
For my students, I always tell them they can do hard things, and I want them to believe that. Things are hard, but the reward of seeing your hard work pay off is worth it.
I want them to believe in themselves and know that they can do hard things. That is what I want to leave them with.
How metastatic breast cancer changed my view of people
I’m such an introvert, so it has surprised me how much people care and how many good people there are out there. I’ve been blown away.
It makes me not want to be as much of an introvert because there is so much good out there. I wish I could do for others what people have done for me. It’s been amazing. It’s wild to me.
I really love people now, even though I’m an introvert.

Inspired by Erica's story?
Share your story, too!
More Metastatic Breast Cancer Stories
Joelle E., Hormone Receptor-Positive Breast Cancer, Stage 4 (Metastatic)
Symptoms: None per se; attributed to pregnancy (severe pregnancy nausea, very low weight gain in pregnancy, lack of milk production in right breast, intermittent nipple inversion, profound fatigue and bone pain, severe right hip pain and difficulty walking)
Treatments: Targeted radiation therapy, hormone therapies (tamoxifen, leuprolide), targeted therapy (CDK4/6 inhibitor - abemaciclib)
Erica H., Breast Cancer, Stage 4 (Metastatic)
Symptoms: Stage 1: appearance of lump in left breast; Stage 4: severe pain in hip, ribs, spine, and shoulder blade
Treatments: Surgeries (double mastectomy, reconstruction), chemotherapy, cold caps, radiation therapy, hormone therapy (aromatase inhibitor, letrozole), targeted therapy (CDK4/6 inhibitor, ribociclib), integrative care
Christina W., Breast Cancer, Stage 4 (De Novo Metastatic), HER2+, ER-
Symptoms: Extreme fatigue, head and neck felt swollen, clogged lymph nodes, appearance of a lump on the breast
Treatments: Monoclonal antibodies (trastuzumab, pertuzumab), radiation therapy
Deb O., Breast Cancer (De Novo Triple Positive and ER+ HER-)
Symptoms: First instance: appearance of lump that later on increased in size, orange peel-like skin around inverted nipple, persistent ache under right arm; second instance: appearance of lump
Treatments: First instance: chemotherapy, targeted therapy, hormone therapy; second instance: surgery (mastectomy), chemotherapy, radiation therapy, CDK 4/6 inhibitor
Tammy U., Metastatic Breast Cancer, Stage 4
Symptoms: Severe back pain, right hip pain, left leg pain
Treatments: Surgeries (mastectomy, hip arthroplasty), chemotherapy, radiation therapy, hormone therapy, targeted therapies (CDK4/6 inhibitor, antibody-drug conjugate)
Nicole B., Triple-Negative Breast Cancer, Stage 4 (Metastatic)
Symptoms: Appearance of lumps in breast and liver, electric shock-like sensations in breast, fatigue
Treatments: Chemotherapy, surgeries (installation of chemotherapy port, mastectomy with flat aesthetic closure), targeted therapy (antibody-drug conjugate), hyperbaric oxygen therapy, lymphatic drainage
Dalitso N., IDC, Stage 4, HER+
Symptoms: Appearance of large tumor in left breast, severe back and body pain
Treatments: Surgery (hysterectomy), vertebroplasty, radiation therapy, hormone therapy, clinical trial
Marissa T., ILC, Stage 4, BRCA2+
Symptoms: Appearance of lump in right breast, significant fatigue, hot flashes at night, leg restlessness leading to sudden, unexpected leg muscle cramps
Treatments: Chemotherapy, hormone therapy, PARP inhibitor, integrative medicine