Michelle’s Accidental EGFR+ Non-Small Cell Lung Cancer Diagnosis
EGFR-positive non-small cell lung cancer doesn’t wait for warning signs – and Michelle’s diagnosis arrived without any. A longtime staff member in the University of Cincinnati athletic department, Michelle was busy supporting student‑athletes, traveling, and playing weekly volleyball when a fall down the stairs set off years of confusing pain. What started as jaw, neck, and shoulder issues sent her through rounds of physical therapy and imaging, all without anyone suspecting lung cancer.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
When a neurologist finally ordered MRIs for possible trigeminal neuralgia or multiple sclerosis, Michelle did what many patients do: she refreshed her patient portal constantly and even pasted her radiology reports into an AI tool for translation. A CT and PET scan, followed by a bronchoscopy, revealed the words she never expected to hear in her mid‑30s as a nonsmoker: it was lung cancer, specifically stage 1 non‑small cell lung cancer. A thoracic surgeon recommended surgery to remove her right lower lobe, with the hope that surgery alone would be enough.

Recovery from surgery was intense: five days in the hospital, chest tubes, and the shock of discovering that walking 200 feet with a walker could feel like a marathon. Michelle was also the youngest patient on the floor by decades, an experience that underscored how often lung cancer is still misperceived as an “old person’s” disease. Help from her community poured in around her: her mom, friends, coworkers, and students filled her room, sent gifts, and showed up repeatedly, helping her feel less alone.
Pathology results later upgraded Michelle’s diagnosis to stage 2B after cancer was found in three of 18 lymph nodes, making chemotherapy and a long‑term targeted therapy pill part of the plan due to her EGFR biomarker. At the same time, her team raised critical questions about fertility, leading to an emotionally overwhelming but ultimately successful egg retrieval. 34 eggs were successfully collected, of which 28 were frozen.
Through surgical complications, chemo‑induced nausea, insomnia, and fears of recurrence, Michelle keeps naming both truths at once: this experience “still effing sucks” and she is “hopeful that I am going to kick this thing’s a**.” She leans on her care team, her “pods” of community, and her love of movement, trusting that she’ll get back to volleyball, a full caseload at work, and the future she’s still building.
Watch Michelle’s video and read the edited transcript of her interview. You’ll learn more about her story, including how:
- A “healthy” lifestyle and being a nonsmoker do not eliminate the risk of EGFR‑positive lung cancer, especially when concerning symptoms like persistent pain are dismissed or misrouted in the healthcare system.
- Biomarker testing that revealed Michelle’s EGFR‑positive lung cancer opened the door to a targeted therapy pill after chemotherapy, highlighting how critical comprehensive testing is in non‑small cell lung cancer today.
- Fertility conversations before chemotherapy can be emotionally overwhelming and time‑sensitive; Michelle’s decision to freeze eggs, despite costs and chaos, gave her meaningful hope for a future family.
- Community is not “extra”; from coworkers to former teammates and her mom, the consistent support around Michelle transformed long hospital days and difficult recoveries into something more bearable.
- A universal truth: it is possible to hold both gratitude and anger at the same time, acknowledging that “things could be worse” while still recognizing that treatment, side effects, and fear of recurrence are profoundly hard.
- Michelle’s transformation is not about becoming “perfectly positive,” but about allowing herself to share more openly, claim her story as the “1%,” and still see herself returning to volleyball courts, Opening Day games, and the house she dreams of.
- Name: Michelle W.
- Age at Diagnosis:
- 34
- Diagnosis:
- Non-Small Cell Lung Cancer (NSCLC)
- Staging:
- Stage 2B
- Biomarker:
- EGFR exon 19 deletion
- Symptoms:
- None; discovered by chance during a check-up for persistent head and neck pain
- Treatments:
- Surgery: lung resection
- Chemotherapy (upcoming)
- Targeted therapy (upcoming)
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions. The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Pre‑diagnosis life, career, and mindset
- The accidental path to my non-small cell lung cancer diagnosis
- My first lung surgery and hospital experience
- Processing a non-small cell lung cancer diagnosis as a young, active nonsmoker
- What happened after my surgery
- Port placement complication and egg retrieval
- Starting chemotherapy and the side effects
- EGFR biomarker and targeted therapy, plus integrative care
- Being the 1% and owning my story
Pre‑diagnosis life, career, and mindset
I work at the University of Cincinnati in the athletic department. Last year, I hit ten years there. Things were good. I was kind of more focused on whether I was going to stay at UC, what I was going to do, and then traveling a lot. I do a lot of traveling, play a lot of volleyball, and was looking to build a house and do some major life things. And then obviously this came on and shifted everything.
The biggest thing I’ve always told myself, which may seem morbid, is that I lost my dad. It was ten years ago, actually, and a couple of days after my first major surgery. He had such a good outlook on life, even when he was diagnosed with cancer, and then three weeks later, he passed away. I always told myself if something were to happen to me — God forbid I were to get cancer, and here we are — that I wouldn’t just dwell on it, sit in bed, and kind of go, “Woe is me.” I think it was a good way to take on this, but I think it kind of kicked me in the butt in a way when we talk about mental health and taking care of myself, because I don’t want people to feel bad for me.
I do a lot for myself. I’m trying to be independent, and that’s been really hard throughout this whole thing. I really don’t like asking for help or wanting people to help me. I usually am the one to reach out or help other people, so that’s been really hard. This kind of hit me out of nowhere, obviously, as they found it accidentally. I try to stay as positive as possible, even when they were like, “It probably is cancer,” and especially when it lit up on all the scans and things like that. I thought the first surgery was going to be all I needed — no chemo or anything like that. So my world, everything, is on pause. I think pretty much everyone can agree with that; life shifted quickly, especially when I finally felt in a spot where I thought, “I can make some really good changes and make myself really happy and do the things that I’ve dreamed of.” I still can, but I wouldn’t actually enjoy that whole process, like building a house and all that stuff. It’s just not possible to do that with everything going on right now.
So I work in athletics, but I work in the academics unit, actually. I basically — I don’t want to say I do school all day with student-athletes — but essentially I do. I do have a small caseload. I went to Mount St. Joe, which is now Mount St. Joseph University. I played volleyball there. It’s pretty close, about 30 minutes from me. That’s where a lot of my pictures are from; the girls that are in there were my teammates in college, and that was the best experience ever. People knock on D3, blah, blah, blah, small school, but it was hands down the best decision I’ve ever made. My mom is still best friends with some of my teammates’ parents. It was a cool experience. We still play volleyball weekly, so it’s been a really cool thing.
There, I studied sports management, and I wanted to be an athletic director. As I got in a little bit, I realized I quickly did not want to do that because it would be a lot of talking to people and fundraising, and that’s not me. I never thought I would be in the position that I am. I ended up going to Xavier University for my master’s. One of my professors is actually a colleague of mine now; her name is Maggie McKinley.
I went to her, and I was like, “I don’t know what I want to do.” I was coaching volleyball at the time, kind of always wanted to coach, but I knew that I was not going to be able to pay the bills and stuff like that. She was like, “Well, you could be an academic coach.” She hooked me up with somebody who is a coworker of mine now, Carrie, and I ended up getting on as a volunteer and worked my way up. When my dad was sick, actually, I got offered the intern job, and then I think it was like a year after that that I got hired full-time. They made a position for me.
There was one other learning specialist, and there are still only two of us, which is a grind. Our job is interesting. It’s kind of hard to explain because people are like, “You’re a tutor,” and we’re like, “No, not at all.” We do all subjects. We have a small caseload, but it’s intense. I’ve been at UC, like I said, for ten years. Year-round, every single day in the summer, we teach a class to incoming freshmen in men’s basketball, women’s basketball, and football incoming freshmen to get them acclimated. Then I have a small caseload and work with student-athletes all day, every day.
It is a grind, and especially now that we’re in the Big 12. They do a lot of traveling, and it’s just a lot. But I love my student-athletes, and I love who I work for and who I work with. That’s really what’s kept me in it. It’s actually been a blessing through all of this. I don’t want to say that corporate America doesn’t appreciate everybody, but working at a company that has a thousand employees and they don’t really know you is hard. Working where I work has been, I think, life-changing and keeps me from stressing about being off work and things like that. I thought I was going to be back January 5th, and they were like, “Yeah, you’re not going back until February,” and that was after the semester started. Work has just been amazing.
I obviously go to a lot of games. I love supporting student-athletes. My mom is the freaking biggest supporter of them all. The coolest thing is they respect her a lot, and they almost speak to her before they speak to me when they see us. It’s a really cool job. It is a grind, but there are some rewards here and there. There are highs and lows, as always, but it’s a unique job. It’s a cool job.
I am especially close with my mom, with my dad being gone. I have a brother, and it was like mom and son, and then dad and daughter. We were so, so close. My mom and I always hung out, but after that, we kind of did everything together. People invite her. My coworkers are like, “What’s Donna doing? Can she come?” Even people younger than me and my friends always include her. It’s really cool, actually.
The accidental path to my non-small cell lung cancer diagnosis
I think it stemmed from when I fell down the steps. It’s probably been three years now. I kind of messed up this whole area, my shoulder/neck/jaw, and it started — not bleeding — but the pain went up into my jaw and into my head. I don’t get headaches often, but it was giving me migraines. I couldn’t really stare at the computer screen and things like that.
Working in an athletic department, I was able to go down to the first floor and see some of our athletic trainers. They put me in a sling. I won’t go through every single thing because we’d be here for hours, but I saw all the doctors. I got MRIs and X-rays on almost everything here except my brain and, I believe, my neck. That kind of plays a part in the story. Someone did recommend getting that, but I was honestly tapped out after six months. They had put me in physical therapy. That wasn’t helping. Everything — muscle and everything — was getting so intense and causing so much discomfort. I can take a lot of pain, but it was getting really intense.
I finally was sick of everything, which is bad, and I just stopped and dealt with it all. About seven months later, I was out to eat with friends, and all of a sudden, I couldn’t chew or open my jaw. It felt TMJ-ish, like it locked. For about 30 minutes, it wouldn’t open, and then it kind of came out. I went to the dentist; they recommended another physical therapy place. They started looking more at my head and my neck and all of that.
I actually got denied by a neurologist. They said they wouldn’t see me and needed to send me to pain management. I was like, “I’ve been in pain management for two years. Can I please see a doctor?” I didn’t hear back for almost a month. So I went to St. Elizabeth and finally reached out to somebody. I got in with a neurologist there, and she was thinking it could have been trigeminal neuralgia, potential MS, and things like that. She ordered MRIs of my thoracic spine and my brain. That is how this all came about.
I had to wait a month, of course, to get all of those tests. I’m sitting here, and cancer never crossed my mind, to be honest. I was crossing off what she was mentioning. She said cluster headaches, but that didn’t go with all the symptoms I had. A month later, I went and got these exams. Naturally, I’m scrolling through MyChart obsessing over the results. When they came in, I put them into ChatGPT and asked it to translate them for me. I did.
It didn’t really say “lighting up” or anything like that. It just said there was a tumor and they wanted further imaging. I didn’t hear back from my neurologist on MyChart within a day or two, so I reached out to a friend who actually works for a doctor at St. Elizabeth. I don’t usually like reaching out and bothering people like that, but I was so on edge that I needed to. She got me in, and I think I left work that day at 9:45. She was like, “I have a 10:30,” and I was like, “Perfect, I’ll see you.” I texted a student and said, “We’ve got to reschedule.”
I saw the doctor, and he ordered a CT scan. He said the words, “I can see why you’re freaking out, because this could read that you do have cancer,” and I’m instantly spiraling. Being me, I went back to work and waited for the CT scan. I didn’t tell anybody. That was the biggest thing because I was remaining hopeful.
I was able to get a CT scan within a couple of days. My mom went with me. It was early. Those results came in ASAP. I did the same thing, ran them through AI to try to figure out everything I could. Those results recommended that I see a pulmonologist. That was the time things started happening so quickly, but also so slowly at the same time.
By October, mentally, I was not well at all. I was angry and hopeful at the same time, just trying to figure out what was going on. We went to the pulmonologist after I got my PET scan. He did tell me that it lit up, but he didn’t want to say 100% that it was cancer. He was hopeful that it could have been some type of infection we could knock out with medication. Here I am holding on to this hope of, “All right, it’s not cancer.” But I sometimes go to the worst-case scenario.
He wanted to get a biopsy. I saw him on October 14th. I got the bronchoscopy biopsy on the 23rd, and I found out immediately. I must have come to as he walked in, and he said, with my mom sitting there, “It is cancer.” I was heavily medicated, but I was so pissed, for so many reasons. More so, I don’t know, even for me, but that my mom has to go through another hard time. We’ve just lost a lot of people. It was something I never thought I would hear.
He wasn’t able to tell me the aggressiveness or really anything. He said, “You probably will have to get some of your lung removed. You’ll never be able to run a marathon again.” I was like, “Eff marathons,” because I don’t run. I do a lot of working out, I play a lot of volleyball, but I don’t run. I had no symptoms. This came out of the blue from jaw pain and things like that, so it was a surprise.
I went home, and he recommended that I see a thoracic surgeon at the cancer center at St. Elizabeth. We have a good cancer center in Columbus — The James — but I didn’t really explore a lot of options. I just wanted to make decisions. When my dad was sick, he was at St. Elizabeth, but they didn’t have what the cancer center is now. I’d heard a lot of really great things about it and the doctors there. So I went to see Dr. Williams, and she confirmed that it was stage 1 lung cancer. Even though I knew it was still upsetting, and I started getting upset, she was trying to be hopeful: “We’re going to get this. We caught it early.” I was so thankful. I think I was writing it off a bit, like, we have it early, we’re going to get it, surgery is going to be all I need.
My first lung surgery and hospital experience
She told me the plan for my non-small cell lung cancer: she wanted to go in and take my right lower lobe. She had seen a little spot on my middle lobe. Thankfully, when she went in to do the surgery, it was nothing, but she was able to wedge that off. She said that surgery would then determine the next steps. That was kind of like, “What do you mean?” I was, again, in my mind just thinking, let’s get this out, and we are good. Golden. I’m back to work. I’m back to life.
She said if it spread, depending on what it was, I might have to get chemo or other treatments. That was mid‑November, and that day we scheduled surgery. Surgery was scheduled for December 1st. I didn’t want to do it that week because that was the tenth anniversary of my dad’s passing in the same hospital. Mentally, I didn’t think I could do this. I know I’m strong, but that is a lot. For insurance purposes, we couldn’t push it back, so we kept it on the first, which all worked out the way it should have.
I had surgery on December 1st, and that was a wild experience. Traumatic is probably not the right word, but life-changing. Even then, I was thinking my life wouldn’t change as much as it has. It’s still really great — my life is great — but life has changed. She took out my right lower lobe. Of course, we had to wait for all the results and fun things.
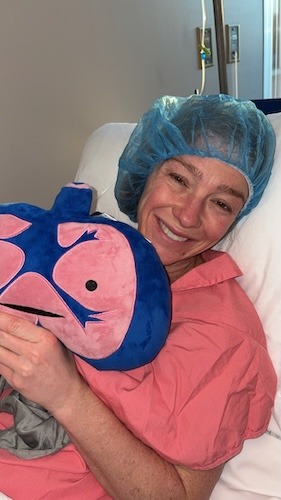
Being in the hospital for five days with tubes, some of my pictures and videos are from the next morning after surgery. My nurse’s name was Michelle, too, and she walked in at 4:45 a.m. and said, “All right, we’re going for a walk,” and I’m like, “What?” Down the hallway I went. Never in my life did I think walking 200 feet with a walker would be hard. I did well, but it was a lot, and I was in a lot of pain that week. I do not like medication, but the pain meds were great. They had to give me a shot in my stomach. That was not fun because the nurses kept telling me, “Oh, you’re so skinny,” and commenting on how small I was. That was a terrible experience, honestly.
People showed up for me. My mom was there the day of the surgery, obviously, but it was an all‑day thing. It took, I think, 6 to 8 hours or something like that. My best friends sat there literally all day long. My mom decided it was probably best that day for them not to see me because I was screaming our favorite word, “eff.” I asked the nurses the next day, “Was I mean?” I’ve never been knocked out that long or that hard, and I don’t remember that surgery day at all. They were like, “No, you just kept screaming ‘Eff,” and we just didn’t know what to do.” I was like, “I’m so sorry, I’m so sorry.” At least I wasn’t mean. My friends were there, and my mom didn’t want them to see me like that, so I appreciate that.
I was the youngest person on the floor. Through this whole process, every doctor has asked why I’m there: “What are you doing here?” I’m not a smoker. I’ve had no side effects at all. I’m healthy for the most part, I work out, things like that. Every time the doctors were asking me, I was like, “I’m trying to find out why I’m here.” I was probably the youngest on the floor by 30 or 40 years, and some of the people weren’t getting visitors, which made me sad. But I had people — it was like a revolving door. My room was full. When we were leaving the hospital, it took six trips because we had so much stuff. That’s been the best part — not the stuff, though that is nice — but the people. They’re not just showing up here and there; it’s consistent. Some of my friends, whether I’m asking or not, are still coming, checking on me, showing up at my house, texting my mom. The community support has been insane. I didn’t realize how many different pods I’m involved in, so it’s been really, really cool to see that all show up.
I was in the hospital for five days for that treatment. I have some battle wounds and scars. The tubes were painful. I don’t understand why they are so painful. They said it was because I didn’t have a bunch of room and I’m small, but I was like, “I could do without that.”
Processing a non-small cell lung cancer diagnosis as a young, active nonsmoker
It’s been really hard. It’s just been hard because I will say, no matter what, I never thought in my life that I would ever get non-small cell lung cancer, even with my dad having it. I never really thought about the genetic piece, which they said has nothing to do with this. When I found out, I was trying to stay so, so hopeful. Then I also was like, how do you tell people that you have cancer?
After all of this, I just went right back to work, going on with my normal life, usually just telling my mom what was going on and going back to work. Then I was a mess one of the days. I was in the stairwell, and one of my coworkers walked in on me. That’s how I was like, “Hey, yeah, so this is awkward,” but one of my other coworkers was in my office, and it was weird to say it again. I don’t know why it’s so weird for me and why I struggle, but I just tried to remain hopeful even through the really bad days in October.
The best thing was that in October, I had a bunch of random things planned. We had a girls’ trip planned. My mom and I had dinner planned and went and saw The Sound of Music. I love The Sound of Music. We always used to watch it growing up. We went and saw a play, and it was always an option, like, we didn’t have to go, but we did go, and I’m so glad that we went. I had a couple of different things planned, as I said, a girls’ trip. That one was hard, though, because not everybody on the trip knew. It was before my surgery and before the biopsy. I didn’t want to tell people and then have to “retract” and say, “Oh, just kidding, it’s not cancer,” which would have been great. Again, it’s just awkward. “How do you tell people that you have cancer?”
I honestly did not tell really anybody about it until maybe the end of October or November. I don’t want to say I regret it; that’s not the word. I probably could have handled it a lot differently, but it was such a personal thing for me. I don’t want people to feel bad for me. I didn’t know any answers to any questions. I knew I was getting surgery and that’s about it. People were like, “Are you going to get chemo?” I honestly was like, “I don’t know,” but in my mind, I had it that surgery was it and that’s all I was going to need.
I’m still staying positive. Some days it’s a really good thing, but I’m still not fully feeling my feelings all the time. When I get sad, I don’t want to be sad. I want to be happy. So sometimes I’m avoiding those feelings. That’s why I loved going through the pictures for this. Now I’m really happy that I’m doing this, so thank you. I just struggle because I want to be strong. I don’t want people to feel bad for me. I don’t like complaining. We’re all tired, we all have crap going on, things like that. But then I think about everything I’ve had to do since that December 1st surgery. Holy mackerel. It’s a different life. If you haven’t had it or gone through it, you really don’t know, even as a caregiver. The pain, the nausea, the medications, the appointments, trying to prioritize everything, the work‑life balance — things like that.
I didn’t share much, but I started sharing on social media, and I did feel like I had a weight lifted off my chest. It was a really cool thing. I like writing, so I’ve been trying to share a little bit more. I don’t know why I struggle so much with sharing. Some days I’m like, “Yeah, let me share,” and other days I’m like, “No.” Things like this are making me share a little bit more because everybody’s journey is different, but also somewhat similar in different ways. You meet new people, which I think is cool, especially when we know what we’re all going through. That’s been — I don’t want to say a nice thing — but it’s a feel‑good thing to have somebody who knows that.
I am missing the gym, though. That’s my big me‑time, me‑space. With all the surgeries and then starting chemo, it’s been hard, so I’m trying to get back moving and things like that.
What happened after my surgery
So on December 1st, I had my surgery. Next, I had my follow‑up mid‑December with the oncologist, where some of the results were back. The non-small cell lung cancer had spread to three of the 18 lymph nodes that she had taken, so it was upgraded to stage 2B. Again, she was trying to stay super hopeful, but that’s when she said, “You will need further treatment from here.” That was a dagger to the heart. We left the cancer center that day, and luckily, there was a cancellation for an oncologist, and we were able to get in that day. We met with an oncologist. What a blur. She said that I would need chemotherapy. I was adamant that I was not going to get it because I am not a fan of medication.
She said, “We can stop talking,” and I was like, “No, keep going, say what you’ve got to say — inform me of everything.” She did not have the genetic results or any other results. When I met with her in January, she would know more about what type and what treatment plan I would need.
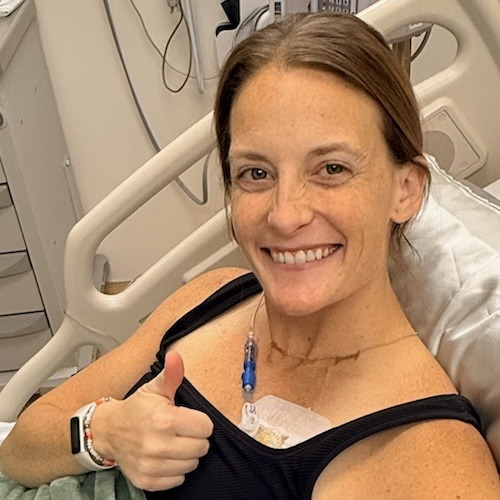
When I talked to my surgeon at the follow‑up, she recommended a port. I was like, “Wow, I have good veins, blah, blah, blah.” I’m so glad I got the port in some ways. She said, “We will talk about it now so you don’t have to come back, and you can just call and get it placed.” When I was at my oncologist appointment, thank God my mom was there because she brought up fertility. They referred me to the Institute of Reproductive Health. We were going out of town on a mom‑and‑daughter trip to the Hallmark experience for my mom’s birthday. I have to say that because my mom’s birthday is Christmas.
We did that, but I had a consultation with the reproductive health doctor the day after Christmas at 10:30 in the morning. I know nothing, and I will say I could have done some research, but that was the most overwhelming experience of my life. He wanted me to make a decision about what I wanted to do at that moment. I didn’t make a decision. I was sobbing my eyes out. He gave me the weekend. That Monday, I decided I was just going to freeze my eggs.
Everything got super chaotic because it’s like three different parties working together in a building, and they communicate through text message for everything. I could barely keep my life in order. I didn’t hop on that process ASAP because I was also getting my port placed. I think that was January 8th.
Port placement complication and egg retrieval
I got my port placed on January 8th. It was supposed to be super easy. My lung collapsed during the procedure because there was a hole poked in my lung. That was a great time. While I was in recovery, they realized that my other lung was collapsing. It was not great. My surgeon came out and told me that. I’m in a lot better spot now, thank God, because I’m not going to cry right now, but I will say that in that moment, I honestly thought I was going to die. Whenever I hear “lungs collapsing,” I thought, what do you mean? I’m sitting in a recovery room, like, shouldn’t I be somewhere else?
She basically said she was going to have to put a tube on the other side and keep me overnight. She turned, and an anesthesiologist was walking behind, and she asked, “How long are you here?” The anesthesiologist went and did a surgery, came to where I was, put a tube in, and then I stayed overnight. It was terrible because I was violently, violently ill. After that surgery, I felt like I took a step back, and then I had to deal with all the fertility appointments. Of course, as everybody knows, it’s time sensitive.
It wasn’t the right timing yet, so I had to wait until February. Within, I think, 13 days, I had like 27 injections. We did the trigger shot and the egg retrieval. I was so, so blessed that they were able to get 34 eggs and freeze 28 of them. I know. I’m not going to complain about that. The money is wild. It was never in my cards, to be honest. I don’t have anything on insurance that covers it. My future will never have a price on it, but I’m so thankful that I did it and that my mom thought about it, because that never really crossed my mind.
We did that around February 10th. They didn’t want me to start chemo until my next cycle came, and they thought everything was okay. During that time, with hormones and everything, my mental health was crap. I was just not myself. I said, “I need a few days before I start chemo.” I was going to call my oncologist.
The joke was on me because they called me and said, “We have to start chemo next Thursday.” I said, “Can we push it back, please, just a couple of days? I want to try to feel myself.” I love my oncologist and my nurse so much. They are amazing. But my nurse said, “Dr. Darnell says we need to start.” I didn’t ask why it’s time sensitive; I don’t want to know.
Starting chemotherapy and the side effects
That first round of chemo, on the 5th, put me down bad — really bad. I will take pain over any nausea any day of my life. The hardest part is not sleeping. People are like, “Yeah, I don’t sleep either,” and I’m like, “No, no, no, you don’t get it.” You get it — the sleeping and not sleeping, getting tired. It’s just hard.
I went back to work, so finding a balance with that is extremely hard. I don’t have a full caseload. My coworker is taking on a ton of students, and that makes me feel so guilty. I know she doesn’t blame me; it’s not my fault. But it’s really hard. I don’t like being away from work, even though I’ve worked my butt off for the ten years that I’ve been there — and I still work my butt off — but it’s hard.
I’m supposed to get four rounds of chemo. After that, I will do a targeted pill for, research said, three years, so every day for three years.
EGFR biomarker and targeted therapy, plus integrative care
The question I asked was because I went through a lot of guilt: “What did I do to myself?” I thought I did this to myself. I want to give a shout‑out to my chiropractor, who is a chiropractor but also in the holistic medicine realm. He’s kind of a doctor in a sense. He actually had terminal brain cancer when he was young, and he beat it. He has been helping me also. My oncologist is totally open to it.
My oncologist said that my non-small cell lung cancer is not genetic. I asked, “Why? What happened?” She said, “It’s just a cell that wanted to mutate.” I kind of took that. My chiropractor is like, “There’s a deeper meaning, and we are going to find out.” We’re trying all different things to combat this, along with the chemo, and making different changes.
I did ask if I needed genetic testing and things like that. She seems pretty hopeful. I thought I was going to have to get immunotherapy, but then she said I would just get this targeted pill. I guess she was saying that it is — I don’t want to say a better thing — but I’m hoping that it’s helpful. I did ask if I would have to take the pill even if the cancer wasn’t there, and she said research says we just need to keep taking it. I’m like, “Okay.”
The targeted therapy is because of my EGFR biomarker. I didn’t ask a ton of other questions, except whether it was genetic and if I needed genetic testing.
How I look at the future, fear of recurrence, and holding on to hope
An emotion that hit me recently is the thought that it can always come back. I don’t know why — for some reason, I’m like, “Oh no, it’s gone, it’s going to be gone forever after one chemo treatment.” Some days, my thoughts are super hopeful and kind of out of this world. That’s going to be something I really have to work on: the fear of it coming back. That’s scary, especially when there are uncontrollable things, no matter what you try or what everybody tries.
That’s scary, especially with how women’s bodies are. I’m not saying men’s bodies aren’t affected, but I didn’t know that chemo could throw me into pre‑menopause at 35 or mess with my fertility. Thank God that I went through that process, because I can think about a family one day. No matter if it messes my insides up, I can still have a family, because that is something that I want. I love kids, so that is something I want.
I am hopeful that I am going to kick this non-small cell lung cancer’s a**. “Eff” is my favorite word. I have “Eff off” earrings, “Eff off” things; my friends get me funny things. Someone told me, “The way you’re handling it, laughing through all the challenges after you’re admitted to the hospital after a port placement — you have to do that or else you’re going to completely lose yourself.” I’m not saying it’s easy by any means, and some people may be like, “She’s having a great time, what the…” No, I’m not, but you have to. I try to make light of every situation. Usually in the doctor’s offices, I’m trying to laugh rather than cry.
My support squad is so crucial. My team of doctors is so crucial. That’s why I’m able to think of great things in the future. All the things we talked about — where my life was last year, doing girls’ trips, trips with everybody, family things, sports games, wanting to build a house, doing other things like that — that’s going to come, and I know it’s going to come. Don’t let things take the joy. The joy has to still be there. That’s what I’m trying to do: still live, still look into the future. My friends are like, “Where are we going when all this is over? We need a trip, what are we doing?” I’m like, “Okay.” It’s going to get back. My friends have not really let me lose sight of the fact that I’m going to be back playing volleyball here soon. I may not be diving and doing my normal crazy things, but I’m going to be back on the court with them and back at work with a caseload and things like that, back to normalcy.
Seriously, that’s what adds a lot to it — the extra appointments — because they’re worth it, but all of the other things are just a lot. Some people are like, “Don’t let it become your life,” and as you know, we don’t want it to, but it’s kind of hard when you’re supposed to be signing for your house, and you’re at the cancer center. We have Opening Day next week, and in Cincinnati, it is like Christmas. I don’t usually treat it like that, but I’d like to go out and enjoy. I’ll be watching. They’re like, “You can watch it from the small TV,” and I’m like, “Thanks, getting chemo, can’t wait — just kidding.” I always think, things really could be worse, but I need to remember it still effing sucks sometimes. We’re here. I just keep on keeping on, one day at a time.
Being the 1% and owning my story
One of my friends said, “Just remember, you’ve always been the 1%.” Every time, they’re like, “You are the 1% of the 1%.” My doctor said I’m 1 in 100 of people whose lungs collapse with the port placement and things like that. I don’t want to — but that’s kind of how I laugh — I’m like, “Of course this would happen to me.” Stuff like that. “Every time they’re like, ‘You are the 1% of the 1%.”

Inspired by Erica’s story?
Share your story, too!
Related Cancer Stories
More Lung Cancer Stories
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
…
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
…
Natalie B., Non-Small Cell Lung Cancer, Stage 4 (Metastatic)
Symptoms: Extreme fatigue, severe cough
Treatments: Chemotherapy, immunotherapy, clinical trials, radiation therapy, surgery (double lung transplant)
…
Stephanie K., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent and intense cough, general feeling of sluggishness
Treatments: Chemotherapy, targeted therapy through a clinical trial, radiation therapy
…
Jennifer M., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptoms: None per se; discovered during physical checkup for what seemed to be a sinus infection
Treatments: Radiation therapy (stereotactic body radiation therapy or SBRT), targeted therapy
…
Laura R., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent cough, fatigue, bone pain
Treatments: Targeted therapies (tyrosine kinase inhibitors or TKIs, including through a clinical trial)
…
More Non-Small Cell Lung Cancer (NSCLC) Stories
Jill Feldman, Non-Small Cell Lung Cancer (NSCLC), Stage 4 (Metastatic), EGFR+
Symptoms: None; nodule found during periodic scan
Treatments: Surgery, targeted therapy, chemotherapy
Roy B., Non-Small Cell Lung Cancer (NSCLC) (Adenocarcinoma of the Lung with Mucinous Features), Stage 2B
Symptom: Nighttime chest rattle when lying prone
Treatments: Surgery (VATS lobectomy), chemotherapy (cisplain), immunotherapy
Jake L., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Severe, persistent migraines, throbbing headaches upon transitioning from horizontal to vertical (lasting 30-40 days before diagnosis, balance disruption
Treatments: Surgeries (multiple brain resections), radiation therapy (tradiational, Gamma Knife radiosurgery, proton therapy), chemotherapy, targeted therapy (ALK inhibitor), clinical trials
Michelle W., Non-Small Cell Lung Cancer, EGFR+, Stage 2B
Symptoms: None; discovered by chance during a check-up for persistent head and neck pain
Treatments: Surgery (lung resection), chemotherapy (upcoming), targeted therapy (upcoming)
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
More EGFR-Positive NSCLC Stories
Jennifer M., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptoms: None per se; discovered during physical checkup for what seemed to be a sinus infection
Treatments: Radiation therapy (stereotactic body radiation therapy or SBRT), targeted therapy
Samantha V., Lung Cancer, EGFR+, Stage 2, Grade 3
Symptoms: Breathlessness, hoarseness, sinus infections, fatigue, pain in left side
Treatments: Clinical trial (targeted therapy)
Natasha L., Lung Cancer, EGFR+, Stage 4
Symptoms: Hoarse voice, squeaky breathing, cough, weight loss, fatigue
Treatment: Targeted therapy
Jeff S., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptom: Slight cough
Treatments: Surgery, radiation, chemotherapy, targeted therapy
Jill F., Lung Cancer, EGFR+, Stage 1A
Symptom: Nodule found during periodic scan
Treatments: Surgery, targeted therapy, radiation

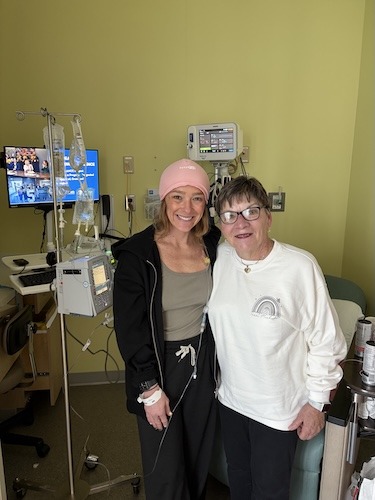


















Leave a Reply