-

Katrina Villareal
·
Living Longer With Lung Cancer: Jill’s Experience with Targeted Therapy
Jill Feldman, Non-Small Cell Lung Cancer (NSCLC), Stage 4 (Metastatic), EGFR+ Symptoms: None; nodule found during periodic scan Treatments: Surgery, targeted therapy, chemotherapy
-

Chris Sanchez
·
Michelle’s Accidental EGFR+ Non-Small Cell Lung Cancer Diagnosis
Michelle W., Non-Small Cell Lung Cancer, EGFR+, Stage 2B Symptoms: None; discovered by chance during a check-up for persistent head and neck pain Treatments: Surgery (lung resection), chemotherapy (upcoming), targeted therapy (upcoming)
-
Chris Sanchez
·
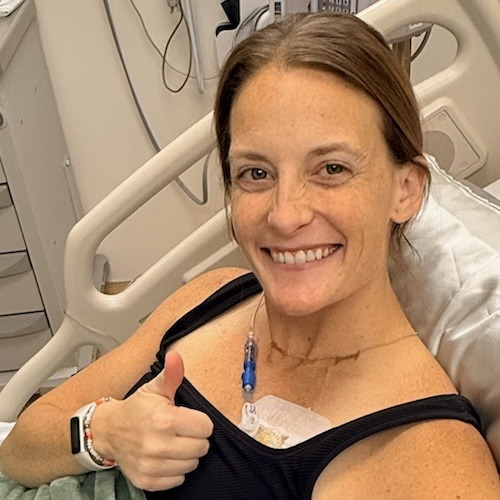
Kelsey’s Stage 4 EGFR+ and ALK+ Non-Small Cell Lung Cancer Story
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic) Symptoms: Severe back pain, falling due to collapsed spinal vertebrae Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
-

Jeff Forslund
·
Lung Cancer Comprehensive Biomarker Testing
The science is clear: knowing what is driving your specific lung cancer before you start treatment can change everything about the care you receive. This program will explain why comprehensive biomarker testing is the foundation of the right treatment plan.
-

Katrina Villareal
·
Roxanne’s Life as a Single Parent with Stage 3 EGFR+ Non-Small Cell Lung Cancer (NSCLC)
Roxanne C., Non-Small Cell Lung Cancer (NSCLC), Stage 3 Symptoms: None; incidental finding Treatments: Surgery (lobectomy), chemotherapy (cisplatin), radiation therapy, targeted therapy (tyrosine kinase inhibitor/TKI)
-

Katrina Villareal
·
Personalized Medicine: Biomarker Testing Guided Maggie in Her Stage 4 Lung Cancer
Maggie M., Non-Small Cell Lung Cancer, EGFR+, MET Amplification & Overexpression, Stage 4 (Metastatic) Symptoms: Ocular migraines (kaleidoscope vision), partial blood clot (DVT) in the leg, vision and balance problems, minor chest pain Treatments: Targeted therapy (tyrosine kinase inhibitors or TKIs), radiation therapy (stereotactic body radiotherapy or SBRT), clinical trials, chemotherapy (combined platinum-based regimen)
-

Chris Sanchez
·
“One Scan Saved My Life:” Shira’s Surprising Diagnosis With EGFR+ Lung Cancer
Shira B., Lung Cancer, EGFR+, Stage 1B Symptoms: None per se; discovered during a preventative full-body MRI Treatment: Surgery (thoracotomy)
-

Katrina Villareal
·
Emily Breaks Stigmas and Builds Awareness Around Stage 4 EGFR+ Lung Cancer
Emily N., Non-Small Cell Lung Cancer, EGFR+, Stage 4 (Metastatic) Symptoms: Chronic cough, persistent post-nasal drip, shortness of breath while doing simple activities, changes in voice, rib pain Treatments: Chemotherapy, targeted therapy (tyrosine kinase inhibitor), radiation therapy
-

Chris Sanchez
·
Jill Feldman’s EGFR+ Non-Small Cell Lung Cancer Story
Jill F., Lung Cancer, EGFR+, Stage 1A Symptom: Nodule found during periodic scan Treatments: Surgery, targeted therapy, radiation
-

Katrina Villareal
·
Filipe’s Stage 4 Lung Cancer with EGFR exon 19 Deletion Story
Filipe P., Non-Small Cell Lung Cancer with EGFR Exon 19 Deletion, Stage 4 (Metastatic) Symptom: Headache Treatments: Surgery (to remove brain metastasis), cryoablation (to remove kidney metastasis), targeted therapy, SBRT, bispecific antibody
Tag: EGFR
-

·
Lung Cancer Comprehensive Biomarker Testing
The science is clear: knowing what is driving your specific lung cancer before you start treatment can change everything about the care you receive. This program will explain why comprehensive biomarker testing is the foundation of the right treatment plan.