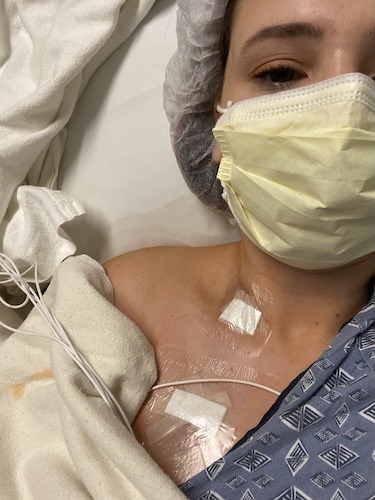
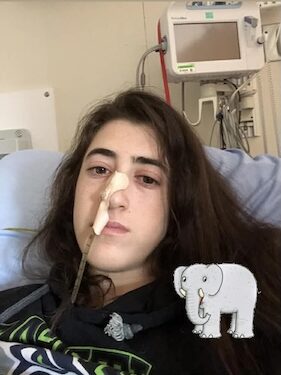
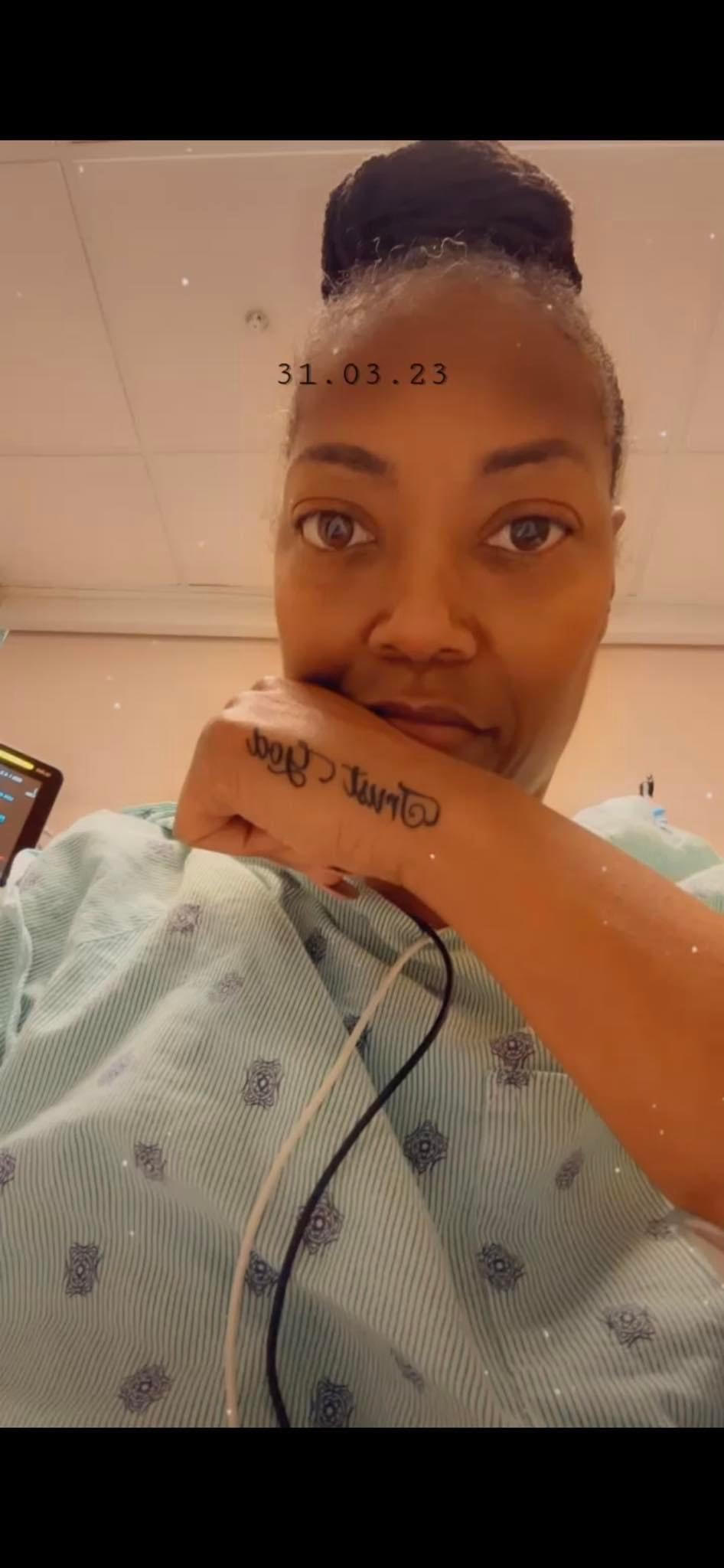Self-Advocacy Saved Sydney’s Life: Diagnosed with Stage 4 Colon Cancer
Stage 4 colon cancer is a diagnosis that carries immense weight, especially when it comes at age 27. For Sydney, the path to discovering this reality began long before a doctor confirmed it. After years of dismissing chronic bloating and constipation as travel issues or normal digestive quirks, her symptoms escalated. Despite severe pain and an intuitive sense that something was wrong, she faced a barrier familiar to many young patients: being told she was too young for serious illness.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
The turning point came when Sydney, desperate for answers and unable to get a referral, made a bold decision to advocate for herself by fabricating a specific symptom — blood in her stool — to secure an appointment. This critical move led to a colonoscopy that revealed a massive blockage, resulting in an immediate colon cancer diagnosis. What followed was a whirlwind of emergency surgery, an unexpected ileostomy, and a move to a new city, all while processing the shock of a life-altering disease during the height of the pandemic.

Sydney’s experience has been defined not just by her diagnosis but by her resilience in navigating the medical system. After initially feeling written off by providers who offered no long-term hope, she sought multiple opinions and transferred her care to Siteman Cancer Center. There, she found a team that championed her quality of life, offering advanced procedures such as biomarker testing and various therapies. Today, Sydney balances ongoing treatment with her passions as a foodie and animal lover, finding strength in community and proving that a stage 4 colon cancer diagnosis does not mean the end of living fully.
Watch Sydney’s video and browse her edited transcript below to learn more.
- Trust your intuition: When medical professionals dismissed her pain due to her age, she trusted her body’s signals enough to push for a screening, even when it required bending the rules to get in the door
- The power of second opinions: Transitioning from a care team that told Sydney “we don’t know how to help you” to specialists at a research center opened new doors for treatment and renewed her hope
- Quality over quantity: Her current care team prioritizes her ability to live a full life — traveling, eating well, and resting — rather than just focusing on aggressive treatment schedules at all costs
- Community is vital: Finding specific patient groups, such as COLONTOWN and Fight Colorectal Cancer (Fight CRC), transformed Sydney’s experience from one of isolation to one of empowerment, connecting her with others who are walking the same path
- Rest is productive: One universal truth she learned is that resting is not laziness; it is an active and essential part of the healing process that allows the body to recover from the trauma of treatment
- Name: Sydney S.
- Diagnosis:
- Colon Cancer
- Age at Diagnosis:
- 27
- Staging:
- Stage 4
- Symptoms:
- Constant stomachaches that only went away after bowel movements
- Pain after eating
- Changes in bowel shape and size
- Treatments:
- Surgeries: colectomy, temporary ileostomy, ileostomy reversal
- Chemotherapy: FOLFOX, FOLFIRI, trifluridine and tipiracil
- Monoclonal antibody: bevacizumab
- Radiation therapy
- Hormone therapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My name is Sydney
- My early symptoms
- My path to diagnosis: advocating for care
- Receiving the colon cancer diagnosis and emergency surgery
- Coping with the initial shock and chaos
- Finding the right care team and second opinions
- A look at my treatment
- Managing my colon cancer treatments and side effects
- Maintaining quality of life during colon cancer treatment
- How to support someone with cancer
- The importance of hope and doctor-patient communication
- My final advice: finding community and moments of joy
My name is Sydney
I am 32 now. I was diagnosed when I was 27, on September 28th of 2020, with stage 4 colorectal cancer. I’m from St. Louis. Well, actually, I’m originally from Arkansas, but right now I live in St. Louis.
I work in a cat cafe on my off weeks. I absolutely love animals and helping them. We get the cats adopted. I have two cats and a pit bull of my own right now. I love anything creative. Before I was diagnosed, I did a lot of professional theater work. I really like acting on stage, but I haven’t done that in a while.
I love Disney. I did the Disney College program in 2013, and so the obsession grew from that. I love food. My husband and I are really big foodies, so it’s really cool that we live in St. Louis because it has really great restaurants.
My early symptoms
I would always get what I thought was travel constipation because anytime we would travel, I could never go. Who knows when the cancer or a polyp started forming, but I remember always having trouble with constipation and bloating. Growing up, I never thought that there was an issue. It was just a normal thing because it would always work itself out.
Then, around the time my husband and I got married in 2018, things started getting worse. I was in pain more often. I thought I had IBS, and the doctors would just tell me, “No, you’re fine. All your labs look good. You’re too young for anything.”
In 2019, we went on a first anniversary trip to Riviera Maya. It was so bad. I was trying to read all these drug labels, and I was like, “I don’t know what this means, but I need something to help me get this out.” I think that maybe when the blockage started growing. I tried elimination diets, gluten-free, dairy-free, just to see if maybe it was the diet, because I used to do CrossFit four times a week. I would do spin classes. I love a sweet treat and a good burger, but I was eating pretty healthy. Every doctor would just be like, “You’re too young.” So I just never thought cancer would ever be the thing.
My path to diagnosis: advocating for care
Mid-summer in 2020, I was bent over at work in so much pain. I would only be relieved if I tried to go to the restroom, but after I ate, I was just always in so much pain. I finally called a gastroenterologist in Arkansas because I was still living there, and they wouldn’t see me just from the symptoms that I was telling them. They were like, “Well, you don’t have a referral.”
Then this thought came into my head. People always say, if there’s blood in your stool, they’ll see you hopefully. So I was like, “Oh, there’s blood in my stool,” even though I had never seen any. I lied, and she was like, “Okay, we can get you in.” I went in for my colonoscopy and endoscopy. I woke up in the middle of my colonoscopy because I heard them say “cancer.” They could not even get a foot inside my colon. Then they sent me straight for scans and surgery and everything from there.
I was just like, “I can’t be the one to figure out what’s wrong with me, right?” I have no experience in the health field, and people just continuously told me, “You’re too young, you’re fine.” I’m like, “I know something’s wrong inside my body.” For a little bit, you almost feel kind of crazy, or you just have these breakdowns of, “Is anyone going to believe me?” Thank God for that gastroenterologist for being like, “Okay, we can take you.” Even though I did have to lie because I was only 27 and didn’t have a referral, because my doctor at the time was like, “You’re too young.”
Receiving the colon cancer diagnosis and emergency surgery
It was 2020, the peak of the pandemic, so my husband was not allowed to come in with me. But I knew because, waking up after the colonoscopy, I didn’t remember them saying “cancer” at that moment. I just knew something was up whenever the doctor was like, “Okay, your husband’s going to come sit down in this room with us.” I was like, “Okay, well, that’s not a good sign.”
He was just like, “I’m 99.9% sure you have colon cancer… whether it’s cancer or not, you either way have a huge blockage that needs to be removed.” He said, “You cannot eat. You have to have smoothies and drink until your surgery because the blockage is so bad.”
On that weekend, I had a colonoscopy, and they scheduled surgery, but we had already scheduled to move to St. Louis. 2020 was a crazy year. So we move over that weekend, and I have to be back that Monday for surgery. But we had moved so much that I was like, “I need to eat, I have to eat something.” So I ate a little bit and was in pain. Then the prep for the surgery did not work. Nothing came out. On the way to the hospital, I’m crying because I’m like, “They’re not going to do the surgery because nothing came out.” But then I’m also trying not to throw up.
They did the surgery, and I woke up with an ileostomy that I did not know I was going to get because the prep did not work. They had to let my bowels rest. But I got it reversed after a little over a year.
Coping with the initial shock and chaos
I don’t really know how to describe it other than I was just like, “Okay, that’s what they told me to do. So that’s what’s going to happen.” I know nothing of this world. I had only known family members or friends who had cancer. I’ve never experienced it myself. I was like, “Well, these are the professionals, so I’ll just listen to what they do.”
Sticking to the matter-of-fact things was the only way that I was able to grasp what was going on. Even five years into it now, people still give you all of this advice, “You should try this,” or “Have you looked into this?” Or people would always ask, “Do you have an update?” or “What did your doctor say?” It’s just all the constant questions. For the first two years, I was just telling anyone, “If you have advice for me or if you have a question, please don’t, because I do not have the capacity to deal with that when I’m dealing with all these new things that have been thrown at me.”
I just pretty much stayed like, “This is what’s happening, and this is what I have to do. So this is what I’m going to do 100%.”
When we were sitting in that room, not when it was confirmed, but in the room after the colonoscopy with the doctor saying, “I’m 99% sure,” I was also still a little bit high from the anesthesia. I was just sitting there, and my husband was trying to comfort me, but he’s freaking out. He’s like, “How is she not freaking out?” I think I just froze. I just remember he was rubbing my back so hard. I was like, “Okay, that’s enough.” He was like, “I’m sorry, I’m just — how are you not freaking out right now?” I was like, “I think I’m just literally in shock. I’m a little frozen right now.”
When I woke up after surgery with the ileostomy, the doctor told me it was only stage 3B at that point. But then, when I got to St. Louis, and we did scans again, it was stage IV. I have never had a doctor give me a timeline or anything or tell me that I’m incurable. So that was very helpful. But I have had doctors tell me, “We don’t know how to help you anymore.” So that can be discouraging. To be told, “Hey, we don’t know how to help you anymore, you need to go elsewherer” was like, “No, what do I do now?”
Finding the right care team and second opinions
When we first moved to St. Louis, it was a year after being kicked off my parents’ insurance. My husband and I were trying to find insurance and then find a hospital that would take it. I started treatment at St. Louis University (SLU), and I had my first oncologist for one year, but she moved back to Texas to be with her family.
I applied for disability because I couldn’t work through treatment, especially Folfox or Folfiri, the heavy treatment. My husband’s a barber, so basically self-employed. I applied for disability, and I got it. I didn’t know that after two years, you get put on Medicare if you’ve been on disability for two years. So when I was able to be put on Medicare — which there was a whole awfulness about because I was on Medicare for eight months without knowing it and still paying for regular insurance — I was able to move to Siteman Cancer Center.
Being at Siteman has rejuvenated my hope – 100%.
Now, just always kind of telling myself, “It may happen, but I’m not going to die from this.” I believe that I will reach no evidence of disease, and then I will see it for five years, and they will tell me that I’m cancer-free. That’s what I believe. Of course, there are hard days, but really, it’s just what I keep telling myself. My husband likes to say I’m a little witchy, but I do my little manifestations, write in my journal, and put it under my pillow.
A look at my treatment
Initially, I did 12 rounds of FOLFOX. We waited because I was clear after the 12 rounds of Folfox. We waited for scans for two to three months. While scans were clear, bloodwork wasn’t. My doctor at the time said, “Well, we need to be aggressive.” So I started on 12 rounds of FOLFIRI.
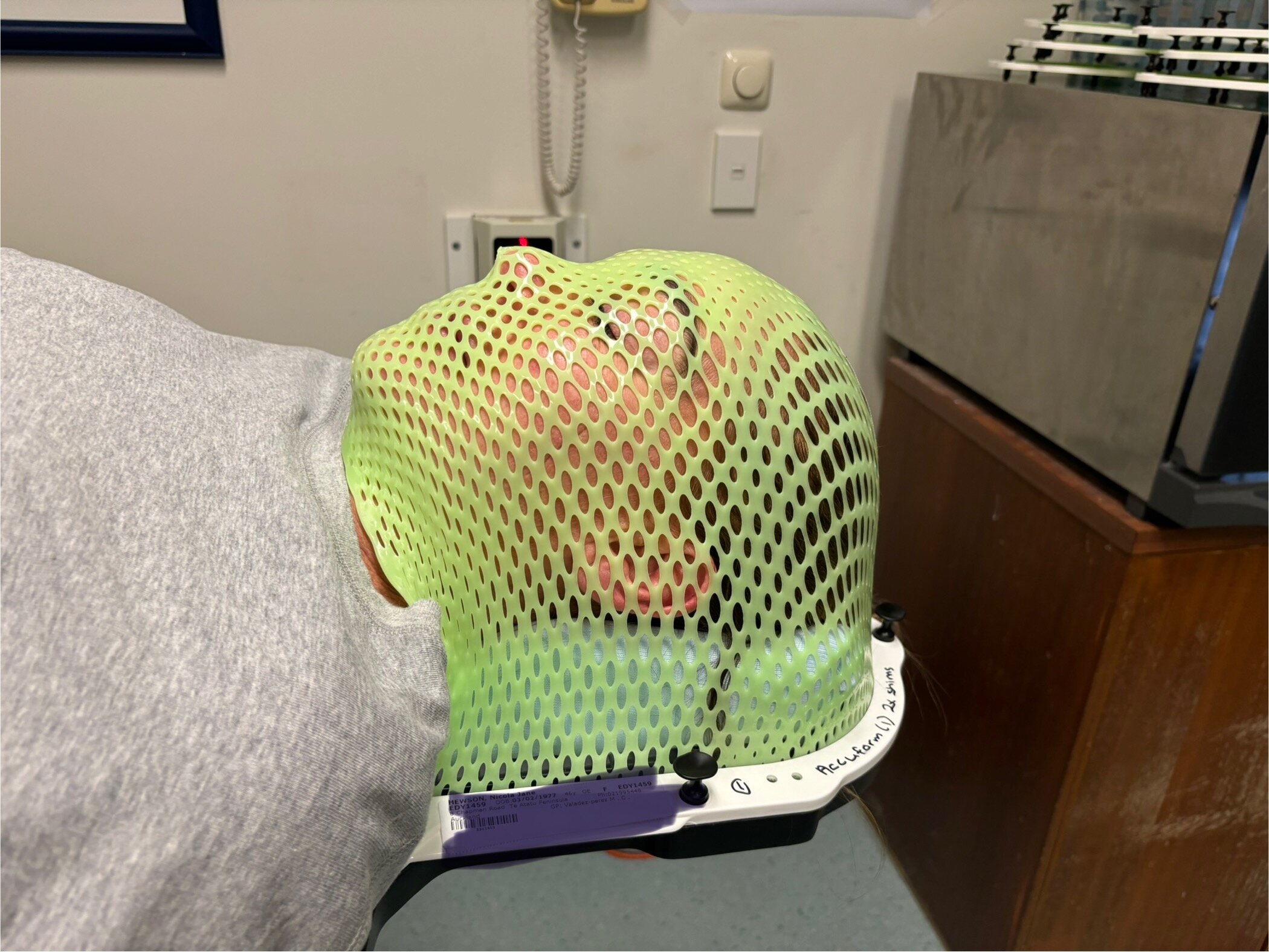
After my first 12 rounds of FOLFOX, I did six rounds of radiation, three on this side of my lungs and three on this side. Then the blood work came back bad, and so then I did the FOLFIRI for 12 rounds, and then they put me on capecitabine, which is a chemo pill. That’s when they told me, “We can’t help you anymore. I don’t know what to do.”
So I went to Moffitt in Tampa to get a second opinion because they would take my insurance at the time. He was like, “No, I’d put you on trifluridine/tipiracil. You do have more options.” So we switched to that drug. I was on it for well over two years. It would be stable, then a little progression, and then go back down to stable.
Then I had a new spot show up in my liver, maybe in September or October of 2025. Now I’m on FOLFIRI again, but I’m at a low dosage, so it’s not as bad as the first time, but I am starting to experience a lot of the things — obviously, my hair is falling out again. My eyebrows are gone. Gotta draw them on. But that’s what makeup’s for.
I have two spots for sure on my liver, which significantly shrunk on scans after being on FOLFIRI. One almost went down a whole centimeter, or maybe it was cut in half. And then I have one that we’re not sure what it is on my liver. It’s not been confirmed. Then, on my lungs, I have numerous spots, too many for surgery.
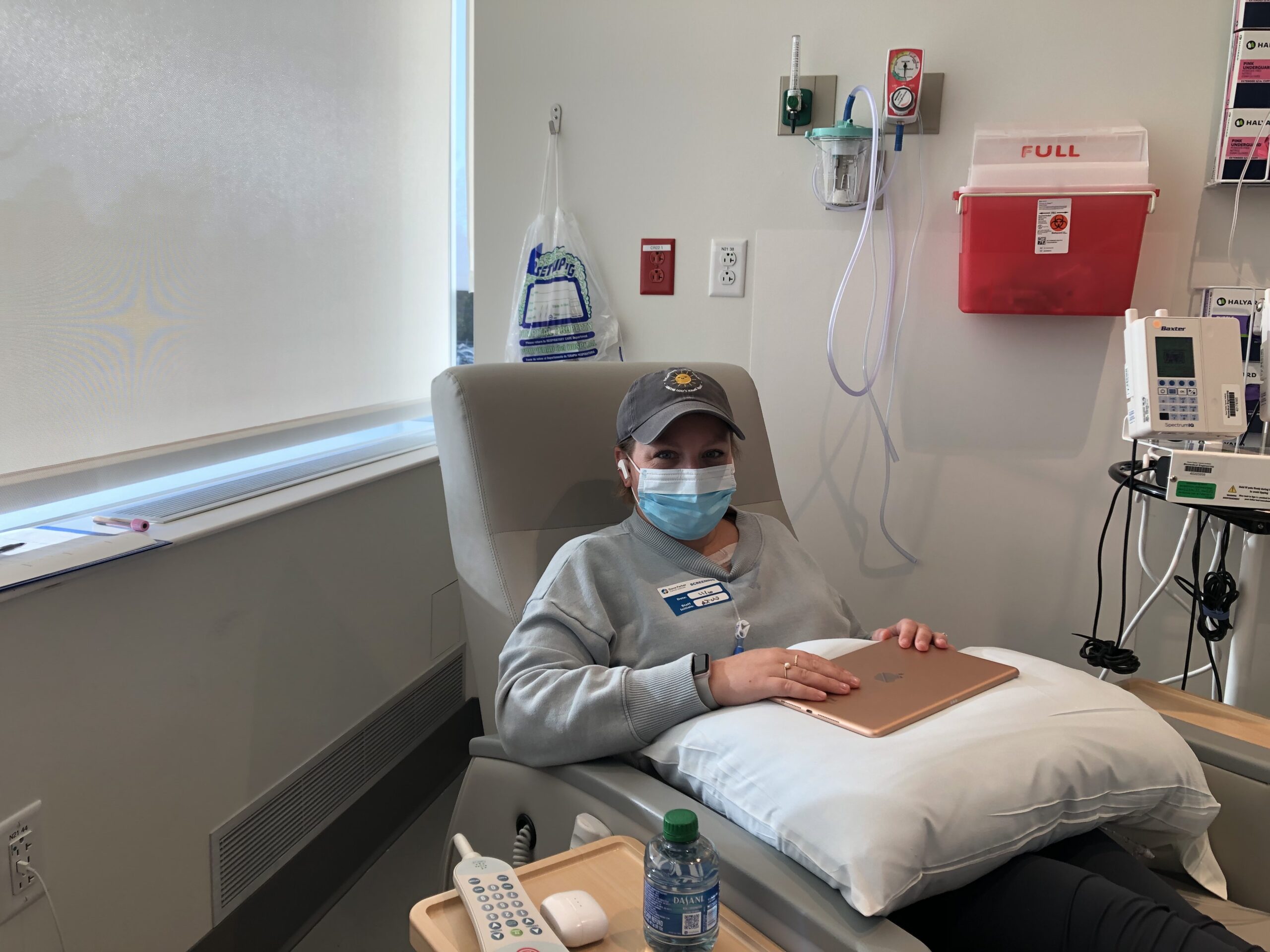
Managing my colon cancer treatments and side effects
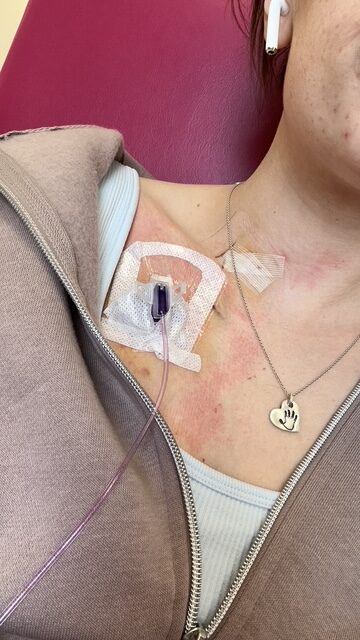
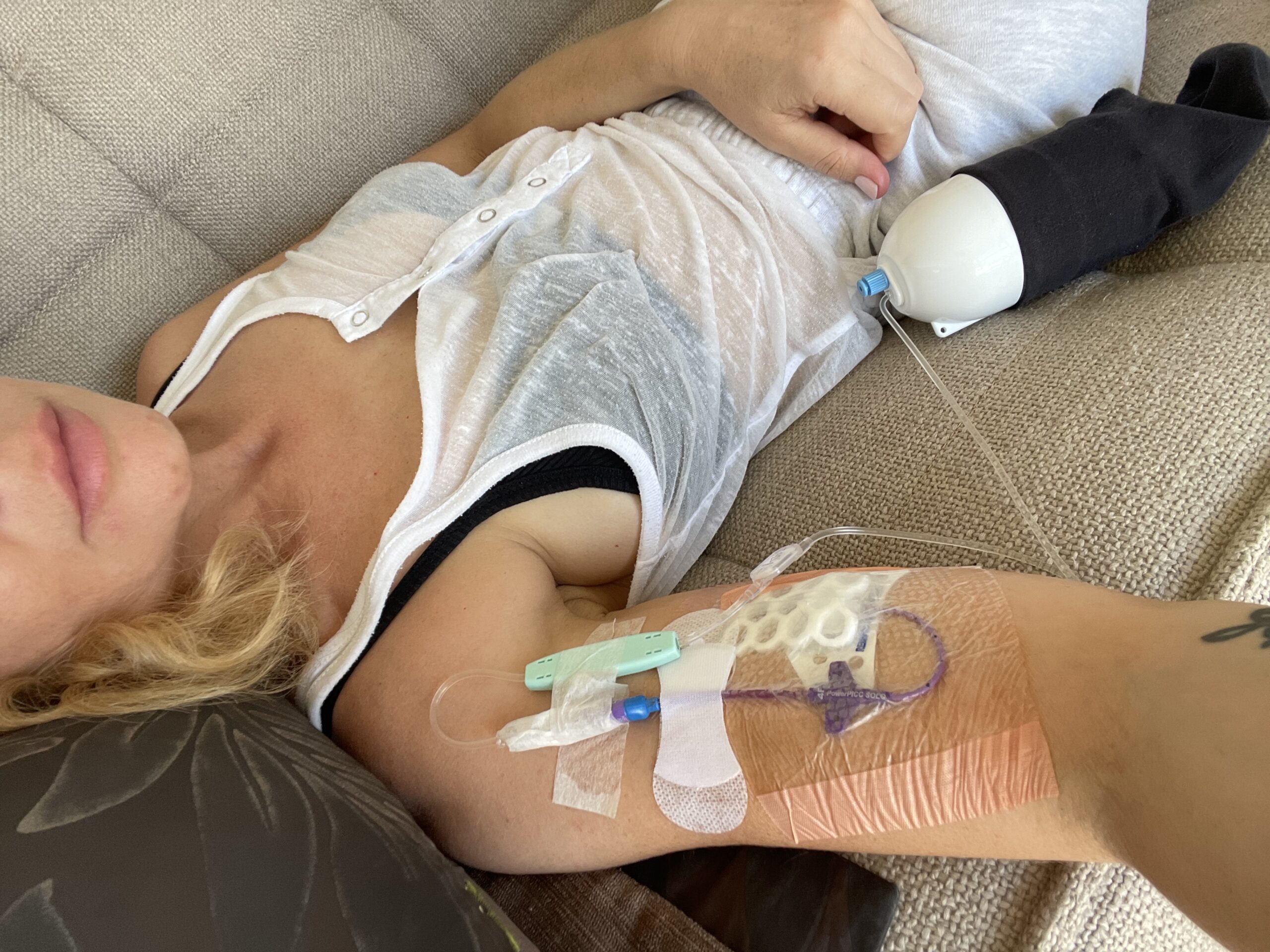
I have been on the schedule every other Tuesday for three years now. I’m on bevacizumab right now with FOLFIRI. So I go in, get labs drawn. They check my CEA every time. But I also have to do a urine sample to see if there’s protein in my urine from the bevacizumab. Unfortunately for me, I’ve been on bevacizumab for three years straight now, so my levels keep going up. I do have a kidney specialist who keeps track of it. We had to pause the bevacizumab on Tuesday because I had such high protein.
I am sent home on a 46-hour pump with my port right here. It’s affecting my vocal cords; my voice always goes out on these three days of treatment. Obviously, I get digestive issues, appetite, and fatigue, all of the things. But once I get unplugged on Thursday, I’m usually slowly coming out of that chemo fog. By about Friday night, I’m okay again. I tell my husband, “I’m sorry I was so lazy today.” And he’s like, “You’re not being lazy. What are you talking about? You’re on chemo.”
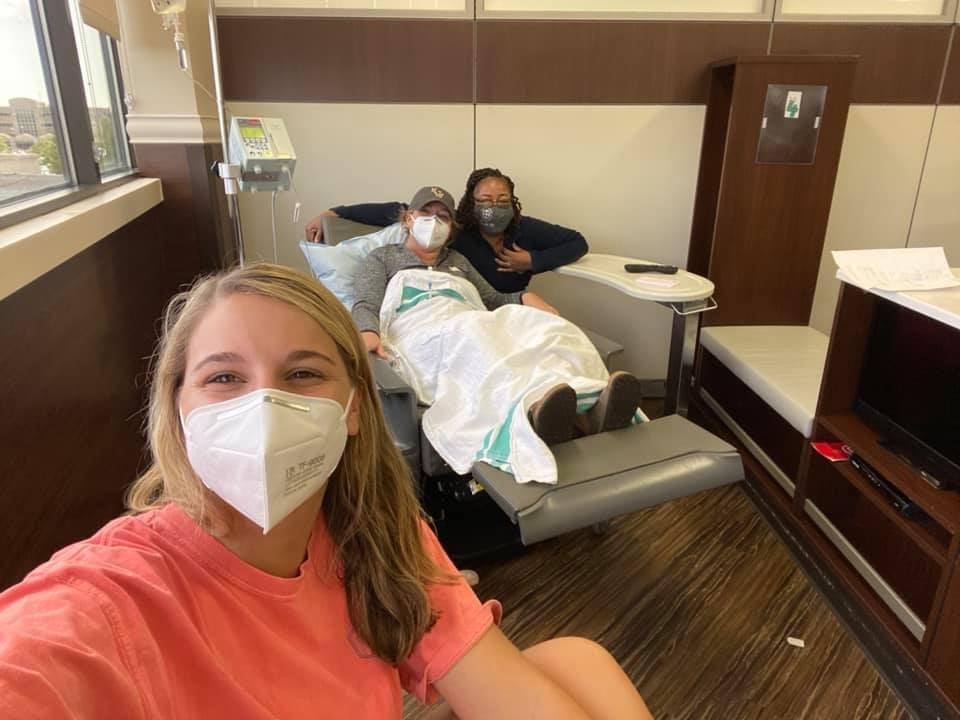
Maintaining quality of life during colon cancer treatment
My husband and I are both foodies, and so when I do have an appetite, I’m like, “Okay, we have to go find a good restaurant, or I need a good breakfast.” We also really love music. So we go to shows often, and we used to go to Music Fest all the time. We slowed down on the Music Fest, though, just because there are so many people and it’s a lot for a whole weekend. If the venue doesn’t have a chair, then I’m usually out.
I spend time with my pets, working at the cat cafe, my friends, and my family. We travel home to Arkansas pretty often. Especially with being at Siteman now, they are very much into the quality over quantity. My doctor told me, “If you want to take a trip and you want to pause for a week, we can pause for a week.” He was like, “I would rather you go live your life than just constantly be on treatment and not doing anything fun.”
How to support someone with cancer
When I got diagnosed, people didn’t really know what to say. How do you tell someone, especially after you get a stage 4 diagnosis — people hear that, and they think “terminal.” No shade to my sister, but she didn’t know how to handle it. She told my young nephew when I was getting treatments that I was going to get my nails done. I was like, “I mean, I wish.”
People really don’t know what to say, what to do. It can be really isolating. But I would tell people that it is going to be okay. There’s going to be a lot of hard times. But you find that if you can find community, especially in your specific cancer — like I found Fight CRC, then Colon Town — and I’ve met so many people who are going through the same thing as me.
You just have to find someone to champion you. My husband and my parents have learned so much. It’s night and day from when I got diagnosed to how people support me now. I do think cancer patients also need to let people know how to maybe readjust the speech. Maybe don’t tell me, “My grandma died from cancer,” as soon as I tell you I have cancer. Maybe don’t say those things.
I found The Patient Story on Instagram. There’s a colorectal cancer patient right now who has been given only a certain amount of time to live. But she said, “You know, as long as I can tell my story, and it saves one person’s life…”
The importance of hope and doctor-patient communication
I am so grateful that no doctor has ever told me my prognosis. No one’s ever called it terminal for me. My first oncologist would let me break down in front of her, and she would just put her hand on my back, and she’d be like, “Sydney, you’re going to be okay. We have these treatments, and yes, they’re difficult, but we have so much proof behind the first treatment that I did that it can be successful for you.” She would always point that out to me.
Being at Siteman, they’ll sit down and explain everything to me. I got pushed into menopause from chemo, and they sent me to a woman specialist who’s in the hospital. If something else is wrong, they’ll send me to this specialist. They just really, really care. Having a doctor who, while they have so many patients, can be so personable and say, “We care about you as an individual and not just another number,” has really helped.
My final advice: finding community and moments of joy
I don’t want to be cliché and be like, “Don’t give up,” but don’t give up. You can do it. I know people speak about how they don’t want to be called a warrior. I’m tired of people telling me that I’m brave because what other option did I have? But I mean it. We are fighting.
Take the time to rest. Don’t think you are lazy for resting, because resting is how you’re going to heal. Do the things that make you happy. You have to find those moments of joy, even in the heartache of everything. Find a community 100%.
I have friends all over the world, and I’ve only maybe met them through social media or maybe once in DC, and I know that I can message them and be like, “Hey, I need to have a breakdown, and I don’t want to put that on my husband right now. Can I please break down to you?” Find community.
It’s hard, but you can do it. If you decide one day, “I’m tired of treatment,” that’s your decision. And I fully support that as well.

Inspired by Sydney's story?
Share your story, too!
More Metastatic Colon Cancer Stories
Raquel A., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Frequent bowel movements, pin-thin stools, mild red blood in stool
Treatment: Chemotherapy
Steve S., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Blood in stool, changes in bowel habits, feeling gassy and bloated
Treatments: Surgery, chemotherapy, monoclonal antibody, liver transplant
Jessica T., Colon Cancer, BRAF+, Stage 4 (Metastatic)
Symptoms: Severe stomach cramps, diarrhea, vomiting, anemia (discovered later)
Treatments: Surgery (hemicolectomy), chemotherapy
Jennifer T., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Weight loss, coughing, vomiting, sciatica pain, fatigue
Treatments: Surgeries (colectomy, lung wedge resection on both lungs), chemotherapy, immunotherapy
Kasey S., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Extreme abdominal cramping, mucus in stool, rectal bleeding, black stool, fatigue, weight fluctuations, skin issues (guttate psoriasis)
Treatments: Surgeries (colectomy & salpingectomy), chemotherapy