Diagnosed with Stage 3C Low-Grade Serous Ovarian Cancer at 21: Julia’s Experience
Stage 3C ovarian cancer entered Julia’s life when she was just 21, in the middle of college, serving as sorority president, and working as a full-time nanny. What first showed up as unexplained weight loss, chronic acid reflux, and months of feeling unwell in 2020 was initially attributed to other causes, including an autoimmune condition, Behçet’s disease. By 2023, her symptoms escalated into rapid abdominal bloating, early fullness after a few bites of food, frequent urination with hip pain, and extreme fatigue. These are classic red flags of ovarian cancer that can be easy to miss in a young adult.
Interviewed by: Carly Knowlton
Edited by: Katrina Villareal

Concerned about sudden weight gain and ongoing pain she thought might be a urinary tract infection, Julia went to urgent care, where a clinician ordered abdominal and pelvic imaging. Ultrasounds revealed large ovarian cysts and a kidney nodule, leading to tumor marker tests, a CT scan, and a recommendation for surgery. Even with an elevated CA-125 level, she was reassured that it probably was not cancer. Eight days later, surgeons opened her abdomen and found tumors “like grains of salt or sand” across multiple organs, including a teratoma and widespread low-grade serous carcinoma.
After that first surgery, and an emotionally devastating moment reading the words “malignant metastatic” in her pathology report email, Julia underwent a full hysterectomy and debulking surgery that removed her reproductive organs, omentum, and affected peritoneal tissue. Pathology staged her as 3A after successful removal of visible disease, and she went on to receive six rounds of chemotherapy: “icing on the cake” measure for a cancer that is not fully chemo-responsive. Side effects included hair loss, severe mouth ulcers, joint and bone pain, neuropathy, weight gain, and intense chemo brain.
Today, on maintenance hormone therapy (exemestane), Julia lives with fatigue and ongoing emotional processing of young adulthood reshaped by cancer, infertility, and altered social life. At the same time, she embraces her scars, works in dermatology, and leans into survivorship by saying yes to new experiences, pursuing her goal of nursing school, and advocating through organizations like the Ovarian Cancer Research Alliance. For other young adults, she underscores the power of listening to your body, pushing for answers, and showing up for loved ones. She also says it’s helpful to acknowledge how much “this really, truly sucks.”
Watch Julia’s video or read the edited transcript of her interview below to find out more about her ovarian cancer experience:
- Listening to persistent symptoms like bloating, rapid weight changes, early fullness, and pelvic pain can be critical, even with other diagnoses
- Stage 3C low-grade serous ovarian cancer can be extensive at diagnosis, yet still managed with aggressive surgery, careful staging, and follow-up treatments such as chemotherapy and hormone therapy
- Many patients feel like a burden and hesitate to ask for help; having people who simply show up, acknowledge that the situation is not okay, and offer concrete support can make an enormous difference
- Julia’s experience shows a profound transformation from busy college leader and nanny to young adult cancer survivor who embraces her scars, reimagines fertility, and chooses to live life on her own timeline
- Support that honors a person’s full identity and not just their diagnosis helps maintain a sense of normalcy, especially for young people navigating cancer, fertility loss, and changing social lives
- Name: Julia T.
- Age at Diagnosis:
- 21
- Diagnoses:
- Low-Grade Serous Ovarian Carcinoma (Ovarian Cancer)
- Staging:
- Stage 3C (discharged as stage 3A after surgery and final pathology)
- Symptoms:
- Unexplained weight loss and then rapid weight gain
- Chronic acid reflux and heartburn
- Persistent bloating and abdominal distension
- Early satiety
- Frequent urination with hip pain
- Extreme abdominal pain and tenderness
- Treatments:
- Surgeries: abdominal surgery to remove large ovarian cysts, full hysterectomy, debulking surgery
- Chemotherapy
- Hormone therapy: exemestane
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Getting diagnosed with stage 3C low-grade serous ovarian carcinoma at 21
- What I’m passionate about and what I do for fun
- How my friends would describe me
- College, sorority life, and a very busy schedule before cancer
- First symptoms and changes I noticed
- What made me finally seek medical help
- Urgent care, ultrasounds, and first imaging results
- CT results, CA-125, and the first major surgery
- PET scan findings, spread of disease, and debulking surgery
- Recovering from the cystectomy and waiting for pathology
- Reading “malignant metastatic” in an email
- Chemo as ‘icing on the cake’ and what I went through
- Finishing chemo and celebrating at the infusion center
- Choosing to stay in Oregon while the family was in California
- The hardest parts of having cancer
- What helped and what to say (and not say)
- Living on hormone blockers and adjusting to a new normal
- Saying yes, following my own timeline, and advocating
- Being young, fertility loss, and wanting to be treated as ‘still me’
Getting diagnosed with stage 3C low-grade serous ovarian carcinoma at 21
My name is Julia. I live in Sacramento, California. In 2023, I was diagnosed with stage 3C low-grade serous ovarian carcinoma.
What I’m passionate about and what I do for fun
Since my diagnosis, I’ve become most passionate about awareness for ovarian cancer. Other than that, I’m passionate about skin care, makeup, and skin health. I like hanging out with my family and friends for fun. I have a dog, so I like playing with her.
I work at a dermatology office, which ties into my passion for skin and skin care.
How my friends would describe me
My friends might describe me as a little random, maybe sporadic at times. I think they would say I’m loving and thoughtful. My personality is pretty introverted overall, but with my close friends, I’m very loud and outgoing.
College, sorority life, and a very busy schedule before cancer
Before I was diagnosed, I had just turned 21. I was the president of my sorority and was about to be a senior in college. I was a full-time nanny for a baby who, at the time, was four months old, and I was watching her Monday through Friday.
I would come home, do all my sorority responsibilities, and prepare to start the school year. I had just gotten my phlebotomy license, so I was finishing schooling and had taken the test. Life was very busy. I was with my friends almost every day, or my boyfriend every day, plus work, school, and any other errands I had to do.
First symptoms and changes I noticed
Looking back now, I think my symptoms started in 2020. I got sick in June 2020, which lasted almost a full year. I had food poisoning that triggered a whole bunch of symptoms. I lost about 50 pounds without even trying.
My doctors kept telling me, “This is normal for you.” At that time, I wanted to lose weight, but I wasn’t trying to, and they were saying, “This is good. Keep the weight off and your symptoms will go away. You’re 18, but you have chronic acid reflux.” I remember thinking, “That’s not normal.” I even had a colonoscopy, but it was completely normal. There was nothing they were concerned about. I was very limited to a few foods. My very first symptom was unexplained weight loss.
In 2023, the majority of my symptoms became present. I had gained almost all of the weight back. I remember buying jeans in July, and by August, I didn’t fit into them anymore. That was a big sign that something was wrong. I was bloated 24/7. I would eat three bites of a meal and be completely full. No part of me wanted to eat anymore.
I had chronic acid reflux and heartburn. When I would go to the bar, I had to go to the bathroom all the time. I was still a nanny and kept thinking, “I can’t keep leaving her; this is stressing me out,” because I didn’t know why I was going so often. When I did go, I had shooting pain up my hips, which was weird. I thought I might have a UTI.
Another symptom was extreme abdominal pain. I was super bloated. I remember one night, while lying down, my boyfriend pressed on my stomach or something like that, and I jolted up because of a lot of pain. All of these symptoms that I consistently noticed happened within about two weeks. They had been happening for a while, but I wasn’t paying attention until they all came together at once in that window.
I also wasn’t paying attention to them because in 2021, I was diagnosed with an autoimmune disorder, Behçet’s disease, which has a lot of gastrointestinal (GI) problems. I thought it was my autoimmune disorder and not anything else.
What made me finally seek medical help
I originally went to the doctor because I was worried I was gaining too much weight too fast. That was odd to me. Then I went to urgent care after work one day because I thought I had a UTI that wasn’t resolving. I had been having that shooting pain in my hips for at least a week and thought, “This is weird,” so I went to urgent care for that. Everything started happening from there.
Urgent care, ultrasounds, and first imaging results
I went to urgent care and had an amazing doctor who felt my stomach and said, “It’s not normal, but it’s not so abnormal that I think something serious is wrong.” She sent me for an abdominal ultrasound and then a pelvic ultrasound. I was originally supposed to get that done a full week later.
I had gone to urgent care on a Wednesday or Thursday. That Saturday, I was still having symptoms, so my boyfriend said, “We’re going to urgent care again, and you’re going to get imaging done today. You can’t wait.” I’m grateful he did that because I was able to get my abdominal ultrasound and pelvic/transvaginal ultrasound that same day.
I was told my results would be back in a week. My boyfriend played college football, so he had to go after one of the scans. I went to my friend’s house, and by the time I arrived, my results were already back. Immediately, I thought, “This is not good. They either found something bad or it’s nothing and they could just read it quickly.”
I looked at my results while walking into my friend’s house. At that time, they found an 8.5-centimeter cyst on my left ovary and a 6-centimeter cyst on my right ovary, or maybe it was 3 centimeters — it was large, and I was freaking out. My friends said, “It’s okay. Cysts happen all the time,” and started naming friends with ovarian cysts. I tried to reassure myself, but then I read that they also found a nodule on my kidney, and I started freaking out again. At the bottom, the report said, “Please refer to a gynecologist.”
I was able to get in to see a gynecologist the following Tuesday. The gynecologist said we would have to do a Cesarean-section–style removal of the cysts because they were large. He did a test for a few tumor markers, including a CA-125 test and two other ones, and sent me for a CT scan. Looking back, you can actually see my cysts when I’m standing to the side.
He said he didn’t think it was cancer but wanted to loop gynecologic oncology into my case because my cysts were so large. He wanted a surgeon present at the surgery so that if anything was cancerous, they could take over.
I remember being freaked out by that, but I was more concerned about missing the first week of school than the idea that it could be cancer. This all happened at the end of September, and where I went to school, our first week of classes was the first week of October.
CT results, CA-125, and the first major surgery
I got my CT scan done about two days after that appointment. The results arrived while I was at work. The doctor said, “Good news: it doesn’t look like cancer. We can’t see any other tumors or anything like that.” But my cyst on the left ovary was 13 centimeters, and the one on the right ovary was 8.5 centimeters, which were still causes for concern.
My CA 125 came back at 147; the normal range is 35 and below. They told me that was also concerning, but the CA 125 can be elevated for many reasons and doesn’t necessarily mean you have cancer. I remember going home thinking, “Okay, I probably don’t have cancer.”
I had surgery eight days after that appointment, the following Wednesday. At that time, I lived in Portland, Oregon, so my parents flew up to be with me. I went into surgery understanding that it could be cancer. When they opened me up, they found tumors everywhere.
My surgeon said my tumors looked like grains of salt or sand all over my organs, so she couldn’t easily tell what was abnormal. She biopsied a lot of areas, and everything she biopsied came back as cancer. Inside my right ovary, I had a 6-centimeter grade 1 germ cell teratoma, which is another type of ovarian cancer. I had two types of ovarian cancer at once, but my final diagnosis was low-grade serous carcinoma because that was the majority of the biopsies.
In that initial surgery, they were able to save my ovaries and successfully remove the cysts, which allowed me time to possibly freeze my eggs if I wanted to. My doctor was amazing. She said she knew what I wanted for my future and that saving my ovaries would be the best option for now, since we were going to have to go back in for a hysterectomy anyway. Saving them would give me the option to try to freeze my eggs.
PET scan findings, spread of disease, and debulking surgery
About two weeks after that first surgery, I had a PET scan and also attempted to freeze my eggs. Unfortunately, my ovaries were too damaged to successfully freeze eggs. I didn’t feel the cost of egg freezing was worth the likely outcome.
I didn’t want to put myself in a position where I might decide to have kids and be heartbroken if none of the eggs worked. If I didn’t freeze them, I might avoid being heartbroken in the future. That gave me a clearer mind going into my future and my next steps. My doctor totally understood.
The PET scan was incredible in the sense that it didn’t show any further spread beyond areas we already knew about. It didn’t show anything new that they were concerned about. The cancer involved my omentum, colon, bladder, entire reproductive system (including my uterus), the cul-de-sac (a tissue behind the uterus connecting to the colon), and my peritoneum. My peritoneal wall was covered in cancer as well, which put me at stage 3C.
Five weeks after my C-section–style cyst removal, I had a full hysterectomy. They cut me vertically instead of horizontally and removed my omentum, the lining of my colon, the lining of my bladder, my full reproductive system, some lymph nodes, and my peritoneum.
What was amazing was that there was no cancer in the lymph nodes and no cancer in the omentum after the first surgery. Because of that, my staging was adjusted; I was discharged as stage 3A.
That was a big relief, knowing I came out of surgery tumor-free with nothing left in my body that they could see. I also went into surgery with the possibility of needing a colon resection (colectomy), but that didn’t need to happen. My doctor said the “teeth” of the cancer hadn’t sunk in far enough to require that, and they were able to get everything.
After that, I had six rounds of chemotherapy.
Recovering from the cystectomy and waiting for pathology
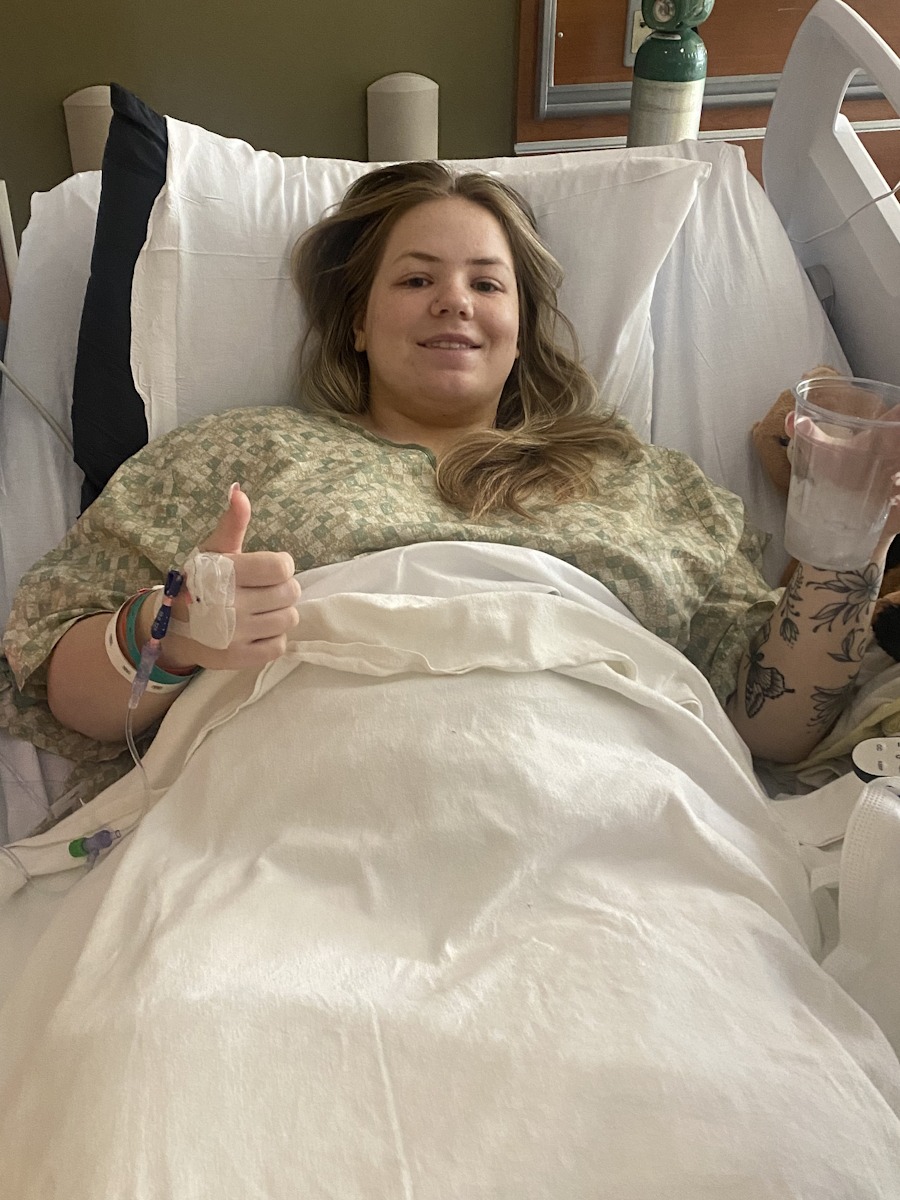
Recovery from my first surgery was difficult. I was in the hospital for three days. I remember looking at my nurse and thinking, “How do people have children after this? This is crazy, and they have to actively take care of a child after this.”
I was in bed almost every day. By about a week to a week and a half, I was up and walking — slowly but walking. It was nerve-wracking because I didn’t get my pathology results until about seven to nine days after surgery, so I was anxiously waiting for those results.
Recovery is tough because you use your abdomen for everything, but it has just been cut open. You can’t move; it’s uncomfortable. I was stuck in my apartment for almost two full weeks because even being in the car was too painful.
Reading “malignant metastatic” in an email
I actually read my final results via email. I got a notification that my test results were ready, and I wanted to see them. Coming out of surgery, I had been told I had a borderline ovarian tumor and that surgery was the only thing needed. I was still going to be an oncology patient so they could monitor me, but they thought they had gotten it all and that it was fine.
So I was thinking, “Great, this probably isn’t cancer.” Then I opened the pathology report while sitting in my apartment with my mom. At the top, it said “abnormal” and “malignant metastatic low-grade serous carcinoma of the ovary.” I was shocked. I remember asking my mom, “Does this mean it’s stage 3 or 4?” and she said she didn’t know. She was freaking out too, but she was trying to stay calm while also trying to reach my dad, who’s a teacher and was in class.
Every single biopsy said low-grade serous carcinoma. It was everywhere. I sat there in shock. My doctor was in surgery all day, so she couldn’t call me right away, and she didn’t know the results had been posted before she could explain them.
It was a surreal moment. I had been thinking, “I don’t have cancer,” and then I read “malignant metastatic.” I’ve always been very interested in healthcare, so I knew exactly what those words meant. I wasn’t reading them for the first time without context, which made it even scarier.
My surgeon called me at 8 p.m. after her full day of surgeries. She had told her staff that even though I had an appointment in two days, she was not going to wait to talk to me. She said, “Do you know what it’s like to be 21 and get diagnosed with cancer through an email? I’m calling her.” She talked me through what it meant and the next steps.
Five weeks later, I had my full hysterectomy, and six weeks after that, I started six rounds of chemotherapy every three weeks.
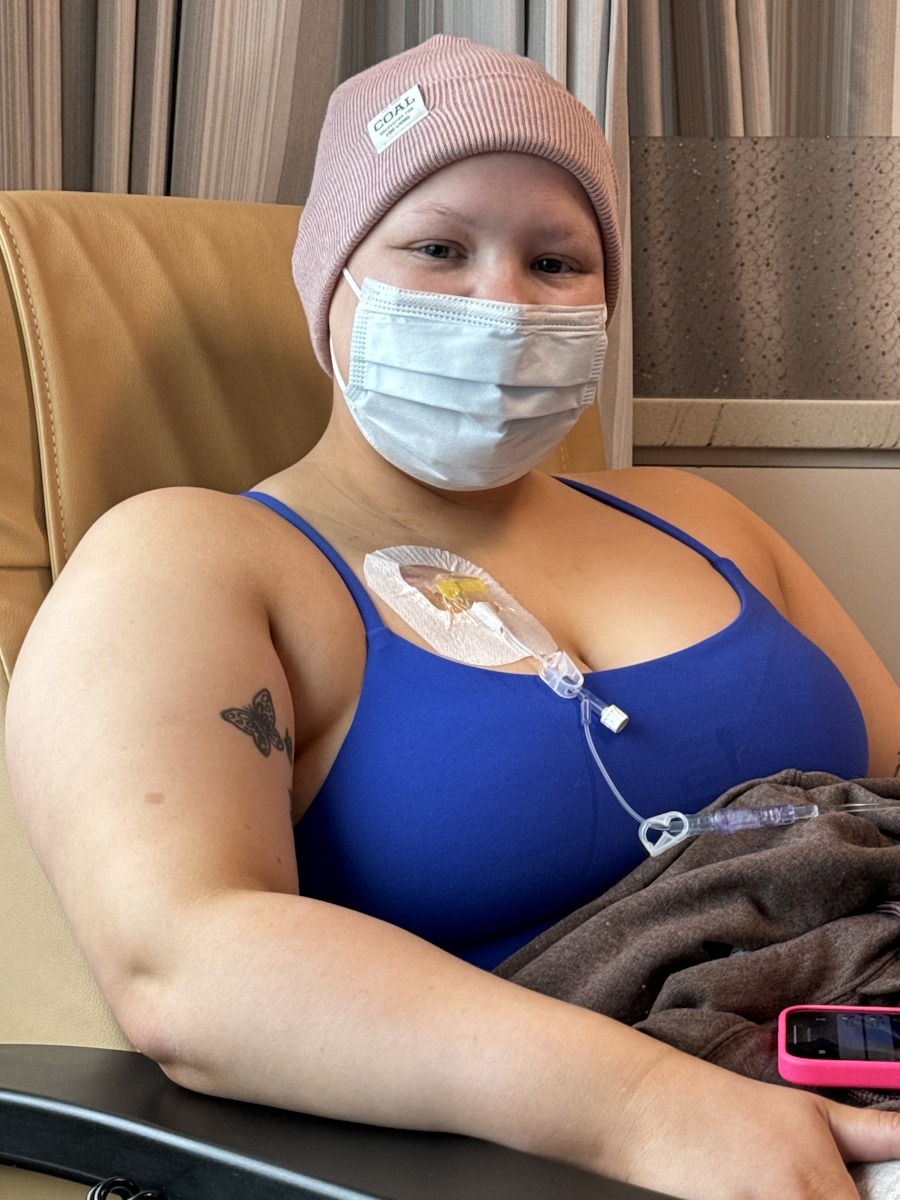
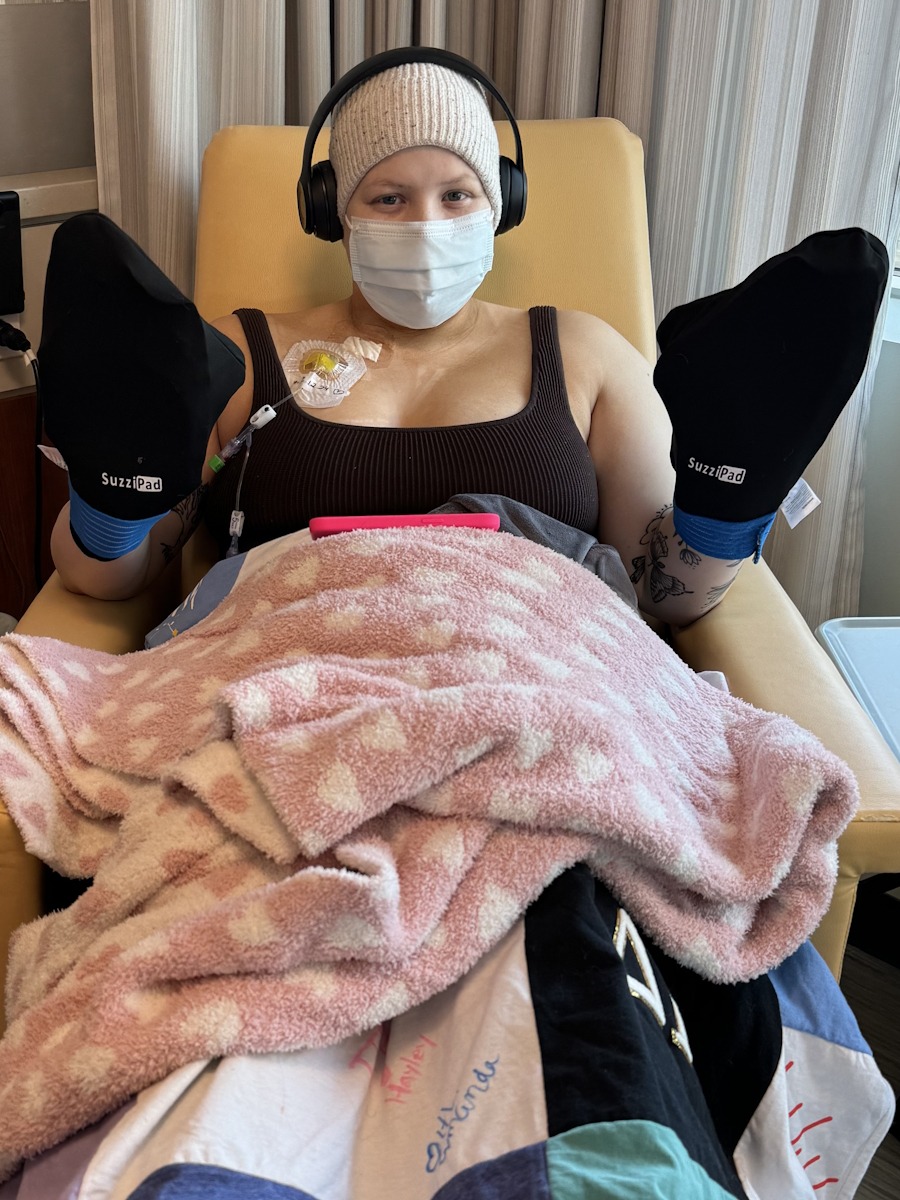
Chemo as ‘icing on the cake’ and what I went through
My cancer isn’t fully responsive to chemotherapy. My team described chemo for me as the “icing on the cake.” It was more of a preventative measure, possibly also because of the germ cell tumor, though I’m not entirely sure. They just wanted to make sure they had truly gotten everything.
I lost all of my hair. I finished chemo in April 2024. I had bad mouth ulcers. My lip was about three times its usual size because of ulcers inside my lip. I was nauseous. My taste buds changed a lot, which was interesting and strange.
I had extreme joint and bone pain. When I got out of bed, I had to hobble. I always had to wear shoes in the house because I couldn’t walk flat-footed. I gained 60 pounds from chemotherapy and was out of breath all the time.
Now I have neuropathy from chemo. My arms and legs go numb probably within a minute of being in certain positions, especially when I’m working out. My arms and legs go numb a lot. Working in dermatology, my arms go numb when I’m in certain positions helping the provider, but I make it work.
I also have very intense chemo brain. I will stop mid-sentence because I have no idea where I was going with my thought. I say things that, in my head, don’t make sense. My friends and family tell me they understand me, but while I’m speaking, I often feel like what I’m saying doesn’t make any sense.
The worst side effects were bone pain, loss of appetite, and mouth ulcers.
Finishing chemo and celebrating at the infusion center
I was able to ring the bell when I finished my last round of chemo. At my infusion center, you were only allowed to have one guest with you, but they let my whole family come back so they could watch me ring the bell. My sisters and my parents flew up to be there, which was incredible.
I’m an awkward person and don’t love a lot of attention on me, so it felt a little awkward. But I remember being in awe that I never had to be there again, that I never had to go into that infusion center again. It was a surreal moment. It finally hit me that I had actually gone through everything I had gone through and had finished chemotherapy. It wasn’t just like having a bad cold; it was a very serious illness.
Choosing to stay in Oregon while the family was in California
I was getting treatment in Oregon while my family was in California. I decided to stay because my friends and my boyfriend were there, and I knew they could all support me. My friends told me that if I needed to go home, I should absolutely go home, but they were willing to be there for me. My younger sister lived in Seattle, so she could easily take the train down to be with me if needed. My parents were with me every other week.
The hardest parts of having cancer
The hardest moment initially was my diagnosis and knowing how much my life was going to change. Emotionally, the hardest part was that no one else in my circle would ever fully understand what I was going through at the level that I did. There are still things people close to me don’t know about how hard it was because I didn’t want to burden anyone.
That feeling of burden is a common discussion in the cancer community — feeling like your illness is burdening other people and feeling bad that you have to ask for so much. I felt bad asking my friends to accommodate me constantly, so I didn’t share a lot of what I was going through. I didn’t want to take away from my friends’ senior year of college. My friends have been the best friends. My family and my hometown friends have been amazing. They always checked in on me. But I didn’t always share the nitty-gritty.
Another hard part was missing out on things because I was sick or knowing my body couldn’t handle them. My self-confidence andbody image decreased a lot, which worried me. I didn’t like the way I looked and had trouble getting myself to do things or trying to feel “normal.” I also didn’t want people to pity me because I was sick. When I went out bald and very clearly sick, I didn’t want to be treated differently, and that stopped me from doing a lot of things.
What helped and what to say (and not say)
One of my sister’s best friends, who is like a little sister to me, sent me a text when I was first diagnosed. She said, “You’re not okay, and I know you’re not okay, and this whole situation is not okay.” She told me it was okay not to be okay and okay to be angry, and that she would support me in being angry.
I don’t remember the exact wording of the whole message, but that was the gist: it’s okay to not be okay and to be angry. That meant a lot because when people get diagnosed with cancer, a lot of people say things like, “You’re so strong,” or “Stay strong,” or “You’re going to be okay.”
I’m not judging anyone for what they say because it’s hard to know what to say when someone gets cancer. It’s an uncomfortable situation to address. But for me, I didn’t like being told to “stay strong” because I didn’t have another option.
Knowing that someone acknowledged that the situation wasn’t okay, that they knew I wasn’t okay, and that they supported me in whatever I was feeling meant so much. I appreciated all the support I got, but that one text stands out the most.
That’s an example of how to support someone, not just with cancer but with any chronic illness or difficult situation. I often say, “This sucks.” There’s no better word; it just sucks. If you acknowledge that to the person you’re caring for and say, “This situation sucks. I wish it wasn’t happening, but I’m here for you, I’m thinking of you, and I love you,” that goes so far.
You’re not telling them that they’re going to be okay; you’re just being there. A lot of people going through cancer don’t want to ask for help. Small things my friends did meant so much: going to Costco and picking up things for me, getting groceries they knew I liked, or just coming over to watch a movie.
Friends from home did things too. One of my best friends got me a blanket and just wanted to sit on the couch and watch movies with me when I came home. Not having to tell people what I needed or wanted was awesome.
My boyfriend was also amazing. I remember having insane cravings when I had no appetite. At one point, I wanted New York-style pizza from downtown Portland and Chick-fil-A from Beaverton, which was 20 minutes away. He took me to get both. I only ate half, but he still took me. Just being there and supporting me in those small ways was incredible.
My younger sister’s sorority sent me flowers and a basket with skincare products, heating pads, and things to take care of me during chemo. That was cool because it showed my sisters were being supported, too, not just me. My older sister lives in San Diego and called me as much as she could. Her friends reached out to me as well. I had a huge support system, and I was grateful.
Living on hormone blockers and adjusting to a new normal
Now I’m on a maintenance drug called exemestane, which is a hormone blocker. I’m pretty fatigued a lot of the time; I could lie in bed all day if I wanted to. Chemo brain is still rough.
I’m slowly getting back to how I was before cancer, both physically and in my personality. It has definitely changed the way I view things and what I like to do. I don’t like going out much anymore. I will go out with my friends, but I don’t drink and don’t enjoy going to bars the way I did before.
In your 20s, going out is such a normal thing. I’m 23 now, but my 21-year-old life looked very different because that’s usually what people that age are doing. I still need accommodations sometimes, but now it’s more about the mental side of things.
It’s hard for me to be around conversations about getting pregnant. I have multiple people in my life who are pregnant or have just had babies. I’m so excited for them; it brings me so much happiness. But it’s still hard to hear conversations like, “We’re trying to have another baby.” People are very considerate and don’t talk about that around me, which helps.
At one point during the conversation, I had to hand my sister the office keys so she could leave. We work at the same office, and I have the office keys, so when she leaves before me, sometimes I forget to give them to her.
Emotionally, this whole experience has hit me the hardest. It hits me when I’m doing or not doing things I used to love. When I don’t want to do those things anymore, I get down on myself and feel guilty.
Physically, I think I’m doing okay. I love my scars; I see them as signs of what I’ve been through. I have no shame in them at all. I love talking about my story and bringing awareness. Getting people to listen to their bodies is important to me.
It still affects me emotionally, and I still get mad about it sometimes. When I go back to Portland to see my doctor, it hits me every time. It’s like a wave; it still bothers me, but I’m processing it.
Saying yes, following my own timeline, and advocating
Survivorship, to me, means saying yes to things I would normally say no to. I want to experience more things now. I recently got back from Colorado with my friends, and in the past, I might have said no because I didn’t want to miss work. Instead, I went and had so much fun. I’m so glad I said yes.
Survivorship also means pursuing my dreams and goals and not waiting anymore. It means living on my own timeline. In the past, I might not have done certain things because the people in my life weren’t on the same timeline. Now I think, “Who cares? That’s life.” Anything can happen. I never expected to get cancer at 21, but I did, so all I can do is try to take control of my life again.
For me, that means pursuing my dreams. I want to go to nursing school and am doing everything in my power to get there. I work in a medical office that I love. Living on my own timeline and not waiting for everything to line up perfectly is what survivorship looks like.
Survivorship also means being an advocate. I speak with survivors and teach students through the Ovarian Cancer Research Alliance. That is important to me because getting people to hear my story matters. You don’t often hear about a 21-year-old being diagnosed with a rare ovarian cancer. I think people should listen more.
I’m not saying people don’t listen, but I want to share my story and have people hear it.
Being young, fertility loss, and wanting to be treated as ‘still me’
As a young woman with ovarian cancer, a lot of people I meet are in their 40s, 50s, or 60s. Many of them have already had children and experienced life stages that I won’t have in the same way, which is hard for me.
When I was going through cancer, all I wanted was for people to treat me normally — as their friend, sister, or daughter. Everyone did a great job of that. My parents were amazing. They flew up to see me, listened to me, and still talked to me about what was going on in our family and in their lives.
Being young with cancer doesn’t mean you stop being all the things you were before. Treating people with a sense of normalcy is important. My friends later told me they didn’t want to burden me with what they were going through because I was already going through so much. I would have loved to hear it. It would have made me feel normal.
Treating someone with a sense of normalcy and still seeing them for who they are is important. Seeing me as still Julia, even though I have cancer, is the biggest thing. My sisters still joked with me. I cope with humor and loved that they would still joke and tease me, while also being careful and more sensitive. They treated me like I was still me, which I loved.
On the fertility side, there are a lot of emotions that come with knowing I can’t carry a pregnancy. That’s one of those experiences where if you get it, you get it, and if you don’t, you don’t — and that’s okay. It has definitely changed conversations with my friends. We talk a lot about what IVF will look like. I make jokes like, “At least I get to choose what my baby looks like,” because I cope with humor.
It’s hard being young and having to go through all of that. A lot of my thoughts are about what my future will look like. But I would rather be alive and healthy than have skipped the hysterectomy or only taken out part of what needed to go.
In a way, I’m grateful I went through what I went through because it has changed me, and I’m grateful for that growth.

Inspired by Julia’s story?
Share your story, too!
More Low-Grade Serous Ovarian Cancer Stories
Julia T., Low-Grade Serous Ovarian Cancer, Stage 3C
Symptoms: Unexplained weight loss and then rapid weight gain, chronic acid reflux and heartburn, persistent bloating and abdominal distension, early satiety, frequent urination with hip pain, extreme abdominal pain and tenderness
Treatments: Surgeries (abdominal surgery to remove large ovarian cysts, full hysterectomy, debulking surgery), chemotherapy, hormone therapy (exemestane)
…
Kacie K., Low-Grade Serous Ovarian Cancer, Stage 3
Symptoms: Pelvic pain, sharp pains during menstrual periods, inability to urinate normally, bleeding
Treatments: Surgeries (full hysterectomy, ostomy surgery, ostomy reversal surgery), chemotherapy
…
Cheyann S., Low-Grade Serous Ovarian Cancer, Stage 4B
Symptoms: Stomach pain, constipation, lump on the right side above pubic area
Treatments: Cancer debulking surgery, chemotherapy (carboplatin & Taxol, then Doxil & Avastin)
…
Alisa M., Low-Grade Serous Ovarian Cancer
Symptoms: Occasional rectal pain, acid reflux, bloating, night sweats
Treatments: Debulking surgeries, chemotherapy, immunotherapy
…
Maurissa M., Low-Grade Serous Ovarian Cancer
Symptoms: Pressure on bladder, throbbing pain, could feel growth on right side of abdominal area
Treatments: 5 surgeries (official diagnosis after 3rd)
…











Leave a Reply