‘It Saved My Life’: Helen’s Stage 4 Colon Cancer and the Chemo Pump You May Not Have Heard Of
When Helen Demestihas first began experiencing pelvic pressure, a burning sensation when peeing (dysuria), and low energy in the spring of 2024, she thought UTI. She never imagined these common symptoms would lead to a diagnosis of stage 4 colorectal cancer with liver metastases at age 49. Her primary care team initially treated her symptoms as recurrent urinary tract infections and possible menopause. Consequently, she spent nearly a month on multiple rounds of antibiotics while working, parenting, and showing up for family milestones, even as sitting in a chair became painful.
Interviewed by: Nikki Murphy
Edited by: Katrina Villareal
A gynecologic exam shifted everything. Helen’s gynecologist felt a mass near the top of her rectum and colon, trusted her instincts despite a normal ultrasound, and pushed for a CT scan that confirmed sigmoid colon cancer that had spread to the liver. Hearing the words “stage 4” over the phone while her 16-year-old daughter stood in the doorway is a moment Helen describes as a complete freeze-frame in time. From there came a blur of colonoscopy, second opinions, and a whirlwind week by the lake in North Carolina, where she and her family processed the news, leaned on one another, and tried to hold denial and determination at once.

Treatment for Helen’s stage 4 colorectal cancer with liver metastases began with standard systemic chemotherapy regimens including FOLFOX, FOLFIRI, and targeted agents like panitumumab. Her care team also explored hepatic artery infusion (HAI) therapy, a specialized approach that delivers highly concentrated chemotherapy directly to the liver through an implanted pump. After initially being passed over for a trial elsewhere, Helen ultimately became the first patient at her Nashville hospital system to receive an off-trial HAI pump.
The results were remarkable. By November 2025, surgeons removed only a handful of liver lesions and ablated a few more, and her scans have shown no evidence of disease in the liver since. She has undergone a liver resection, colon resection, and full hysterectomy, and now continues systemic treatment as “cleanup,” aiming to live with cancer but be treatment-free as much as possible.
Along the way, Helen has turned outward. She connects with patients across the U.S., Canada, and the UK who are considering the HAI pump, sharing what daily life with the device is like. She reminds them that even with stage 4 colorectal cancer with liver metastases, there is room for hope, questions, and a fiercely advocated-for plan.
Watch Helen’s video or read the edited transcript of her interview to find out more about her story:
- Trusting your body and pushing for answers when symptoms don’t add up can be critical, especially when early signs are vague or dismissed as something “routine” like UTIs or menopause.
- A single clinician’s intuition can completely change the course of stage 4 colorectal cancer with liver metastases by uncovering the disease earlier and opening doors to treatment.
- HAI pump therapy combined with systemic chemotherapy helped transform Helen’s outlook, leading to a dramatic response after she became the first patient to receive the pump at her hospital.
- Finding community through family, social media, and other patients who “get it” can ease isolation, offer real-world guidance, and make it easier to face the unknown one day at a time.
- Helen’s experience reflects a powerful transformation from long-time healthcare advocate to patient-advocate for herself and others, using her story to challenge misconceptions about stage 4 cancer and to encourage people to ask informed questions about options like the HAI pump.
- Name: Helen D.
- Age at Diagnosis:
- 49
- Diagnosis:
- Colon Cancer
- Staging:
- Stage 4
- Symptoms:
- Pelvic pressure and pain
- Burning with urination
- Bloating
- Changes in bowel movements including constipation and pencil-thin stools
- Low energy or fatigue
- Discomfort sitting
- Night sweats
- Treatments:
- Chemotherapy: FOLFOX, FOLFIRI
- Newer hepatic artery infusion (HAI) pump therapy
- Targeted therapy: panitumumab
- Surgeries: liver resection and ablations, colon resection, full hysterectomy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Introduction
- When I first knew something was wrong
- How my gynecologist found the mass
- Symptoms I did and didn’t have
- When I wondered if it was something more
- The night everything became impossible to ignore
- My path to diagnosis and early testing
- Hearing the words “stage 4”
- Telling my husband and family
- My first consult and why I sought a second opinion
- Waiting a week on the lake before my colonoscopy
- My colonoscopy experience and switching doctors
- Meeting the surgeon in an empty hospital hallway
- How I emotionally processed my official diagnosis
- Building my treatment plan and confirming the cancer
- My full list of stage 4 colon cancer treatments so far
- Becoming the first hepatic artery infusion (HAI) pump patient
- Getting the HAI pump and what it was like
- My remarkable response and liver resection
- Living through major surgery, hysterectomy, and colon resection
- What it means to be the first HAI pump patient
- My long-term plan with the pump
- The treatment I’m starting now
- How cancer has changed my work, motherhood, and life
- Misconceptions about stage 4 cancer
- My biomarker testing and why some immunotherapies don’t apply to me
- My hope for the future
- My advice to someone who’s newly diagnosed
- Why I say the HAI pump saved my life
Introduction
Hi, I’m Helen. I’m originally from Virginia Beach, Virginia, but I’ve been living in Nashville, Tennessee, for about 10 years. I was diagnosed with stage 4 colon cancer in July 2024.
When I first knew something was wrong
Around the end of April to the beginning of May, I started to feel pelvic pressure and pain. I was 49 at the time and because of my age, I thought that menopause was coming on well before any heavy symptoms led me to my diagnosis. I was also having night sweats. Anything that typically comes along with menopause, I was feeling.
At the beginning of May, it increased. I was having that pelvic pressure and felt a burning sensation when I would urinate. I went to my primary care physician and when I had a urine analysis, it came back with bacteria. My blood work was okay, so we assumed it was a urinary tract infection (UTI), so I was treated with antibiotics for about 10 days.
After the round of antibiotics, I still noticed the symptoms. They weren’t quite as bad, so I returned to my PCP, who prescribed more antibiotics, but a different brand, which targeted a little bit more of, I guess, the specific UTI that he was tracking. That prescription was for only five days.
Within two to three weeks of taking that medication, I noticed a difference in my bowel movements (pencil-thin stools) and the pressure from my pelvis was moving up toward my gut. I went back to my doctor and we agreed that the antibiotics might have been causing some gastrointestinal issues. We were still seeing a little bit of bacteria in my urine, so we were assumed it was toward the end of the infection or the beginning of another round of a UTI, so back on antibiotics I went. This is now the third round.
I started to feel better, which was around the end of May. For majority of the month, I was on antibiotics, assuming I had a UTI. I went on vacation in June and noticed a little bit of fatigue and low energy. I wasn’t napping, but I had low energy. My bowel movements and the pelvic pressure were improving, but then came this new symptom, which was low energy. I brushed it off and talked about it with my family. We were all in agreement it was probably menopause coming on.
How my gynecologist found the mass
I had my gynecological appointment in July and discussed my symptoms with her, saying, “Hey, this is what’s been going on since May. I think it’s menopause.”
She did some tests and when they came back, she said, “It’s not looking like hormones are being affected too much. Let me do a pelvic examination, and we’ll go back to discussing the symptoms that you’re having.”
When she did the pelvic exam, she felt a mass at the top of my rectum to my colon. From there, we went to testing. I went for an ultrasound directly following that appointment, which came back negative.
To this day I praise my gynecologist, because if she didn’t follow her gut, I wouldn’t know if I’d be here today. She said, “Even though everything’s coming back negative, I don’t feel good about this. Let’s go ahead with a CT scan.” By July 13th, I was diagnosed with stage 4 sigmoid colon cancer that had spread to the liver.
Symptoms I did and didn’t have
I had no blood in my stool. I didn’t even have the symptoms that a lot of people talk about. I only had constipation for a very small period of time. I still do believe it was the cancer, but also the antibiotics, because I was on a lot of antibiotics.
I had relief after diagnosis because I started to feel better. I even called my doctor and said, “Is it at all possible that the test is false? Because now I’m having regular bowel movements. I feel a little better. I’m feeling like myself.”
I didn’t have massive weight loss like most people. At the time I was normal, exercising, and active.
From May to July 9th, I was experiencing symptoms before diagnosis.
When I wondered if it was something more
I did have moments where I thought it might be something more. When you go on Google and search your symptoms, colon cancer would always pop up. I thought, “Oh no, not me. I’m too young. I’m 49. No way I could get cancer.”
If I would Google menopause symptoms or a symptom with menopause, it would still come up colon cancer. But I was like, “Nope.” Denial kicks in. You’re like, “No, it couldn’t possibly be me. I’m too healthy.”
I’d never had bowel movement issues or GI problems. I very rarely had to go to the doctor, so it was very unusual for me. I still find it very surreal that I have cancer.
The night everything became impossible to ignore
There was a moment when the symptoms became impossible to ignore. During the third week of May, it was my daughter’s softball party for her school. I was sitting with other moms, and they said, “Helen, are you okay?” I said, “I’m just not feeling good.”
One of the moms happens to be a nurse. I leaned over to her and said, “Here are my symptoms. It’s just so weird. I’m in a lot of pain and uncomfortable. Even sitting in a chair hurts.” At that point, it was intensified because I kept shifting, which brought a lot of attention to me from the other parents.
I leaned over to one mother who’s a nurse and said, “I think I have to go home and try an enema. I think I’m constipated from the antibiotics. I’ve never done one. Are there any tips?” We even chuckled, because who wants to have this conversation while your daughter is receiving an award?
I came home and did the enema, which didn’t work. I thought, “This is strange.” I was yelling for my husband from the bathroom, “Excuse me, can I get a little help?” He was like, “No, but I’ll talk you through it. I don’t want to be part of this. I think you’re thinking too much about this.” I said, “No, I just need to figure this out.”
I started to feel bloated at that point. I did another one, so two enemas back to back, and absolutely nothing happened.
I was crying because I couldn’t take not knowing why I couldn’t go to the bathroom. It wasn’t fear that I thought it was cancer; it was just, “Why am I not going?” I was so uncomfortable. I couldn’t sit or walk. The bloatedness was very, very intense. I always tell people it was incredibly uncomfortable. That feeling probably lasted for a good month.
At one point, I just hid that I was uncomfortable, because I refused to let that be what brought me down or stopped me from doing my day-to-day work and being involved. It was the beginning of summer. You have a pool in your neighborhood and your friends are all gathering. I chose to ignore it and powered through.
My path to diagnosis and early testing
My PCP prescribed the antibiotics. I even did a telehealth visit in between. At this point, I think I might have delayed my diagnosis. Maybe I would have gone a little further with testing, but I kept thinking, “I’m going to my gynecologist in July. I’ll just wait.”
The symptoms were very inconsistent. You read a lot about that with colorectal cancer.
My gynecologist, in the building where she practices, has testing downstairs, which is an important part of the story. I didn’t have to make appointments and travel for the testing. I was fortunate enough to go downstairs directly following my initial exam on July 9th.
The first test was an ultrasound, which came back negative for any findings in the area where she felt the mass. In the middle of this, they did find a cyst on my ovary, but that was benign.
Then my gynecologist called me and said, “I would like to make the appointment for you to come back and do a CT scan of your pelvic area,” which I did. Because it was an abdominal and pelvic exam, when that came back, it showed the mass and the lesions on my liver.
I received a call from her on July 13th, where she said, “Here’s what our findings are: rectal cancer, stage 4, spread to the liver.” Everything froze at that moment.
Hearing the words “stage 4”
I had to have her repeat it multiple times. It’s amazing how it still makes you cry. Hearing you have a mass is one thing; hearing stage 4 and spread is another. I was in my bedroom, writing these notes down, and I was shaking. I still have the piece of paper where I wrote them down.
I kept saying, “Can you repeat that again?” All I could hear her say was, “I’m so sorry that I have to call you with this news.”
I turned around and saw my daughter, who was 16 at the time. She was standing at the doorway, so she heard the whole conversation. That is how she found out before my husband did.
I had to tell my daughter, “You need to text Dad and have him come home right away.” As I was talking to my doctor, she said, “I’ve set up an appointment with you with a colorectal surgeon tomorrow for a consult,” so I went to see the colorectal surgeon the following morning.
Telling my husband and family
My husband was home in about 20 minutes. He works in healthcare as well. I called my sister, with whom I’m close. She’s a hospice nurse, so I’m somewhat surrounded by people in the healthcare field.
I called my sister and had her on speaker. We refused to believe it and kept saying, “Are you sure?” My sister kept asking me, “Did she say this about your liver? Did she mention the sizes of the lesions? Did she mention the mass in your tumor? Are we sure it’s not from the constipation?”
I said, “No, unfortunately not at all. She was 100% correct on her findings and what the CT showed.”
After we got off the phone with my sister, when it was just my husband and me, the first thing I said was, “All I know is we’re going to fight whatever this ends up being. We’re fighting.”
My first consult and why I sought a second opinion
When I went to the colorectal surgeon the following day, he provided some hope. He said, “A lot of times, lesions that end up on your liver can be benign, especially if you did, in fact, have a UTI. Those can create lesions that look malignant. Until I do an actual colonoscopy, we can’t sit here and assume it’s stage 4. We can’t assume that it’s cancer. Let’s just wait for the colonoscopy.”
My colonoscopy was scheduled a week after the appointment. When I came home, I literally stood in the middle of my living room and when my daughter came downstairs, we were standing there and asked, “What’s next? What do we do for the next week?” I said, “We’re packing our bags and going out of town.”
We booked flights to go to North Carolina so I could be closer to my family. My brother and my parents live there. My sister was trying to get there as well to meet with me. We booked our flights, threw a bunch of stuff in a suitcase, and were out of the house within an hour after we got home from that appointment.
When we arrived at the airport, it was very busy. We were at the kiosk and it wasn’t taking our tickets. I thought, “You’ve got to be kidding me.” It kept saying invalid. The line to get to the ticket agent was literally out the door because it’s constantly busy in Nashville. I was starting to process everything that was going on and said, “No, this is not happening.” Probably a good 40 minutes to an hour had gone by, and the line to TSA was growing. We were going to miss our flight if I didn’t get these tickets validated.
I called the airline right outside of TSA and a gentleman named Frank answered the phone. He heard my voice and said, “Are you okay?” I said, “Frank, I’m not. It’s been quite the day. In fact, it’s been quite a few days.” I told him what happened and said, “I was just diagnosed with stage 4 colon cancer,” which was the first time I said it out loud. I started crying a little bit.
He said, “Sweetheart, don’t cry. Let me tell you a story. My father-in-law arrived at my house one day, pale, looking awful, couldn’t breathe, and very sick. I had to rush him to the emergency room. After several tests, they diagnosed him with stage 4 — actually terminal — colon cancer. We had to prepare ourselves,” he said. “And you know what? That was 10 years ago. Now he’s living, thriving, and doing amazing. He’s healthier now than he was before. So you’re going to be okay. Do you hear me? You’re going to be okay.”
You could hear him clicking on the computer, and he said, “By the way, you booked the wrong date to get on the flight. That’s why the tickets weren’t working. But don’t worry. I just changed you. You’re getting on a flight in the next two and a half hours.” He rebooked the family, and I just crashed out emotionally.
When I was formally diagnosed, I named the mass Frank, so Frank would always be with me. A lot of people ask, “Why did you name your tumor Frank?” I tell the story and they say, “Poor Frank.” I say, “No, it’s just interesting how that story happened. It’s almost divine intervention.”
Waiting a week on the lake before my colonoscopy
My family lives on a lake and it was almost too perfect. There was a lot of sunshine and we were sitting, relaxing, and processing as a family. We talked a lot about it. During some conversations, we were still in denial. We kept saying, “We have to wait for the colonoscopy. We can’t say for sure.” I said, “Well, no, it’s for sure. I think the colonoscopy will just tell us how severe.” Then we’d find time to shop and swim. It was just a pure getaway to clear my mind.
I started clean eating right away. It’s amazing. The first thing you do is start eating healthily, as if the damage hasn’t already been done. Eating that bag of chips is not going to do anything, but right away, you want to make your body healthy.
We came back after that week refreshed and ready to battle.
My colonoscopy experience and switching doctors
The colonoscopy was not as bad as I thought it would be; it’s the prep that’s horrible. If they could only make the prep better, I think more people would actually get screened.
My husband had to leave Charlotte, North Carolina, to go to work. He was supposed to be back for the colonoscopy, but, unfortunately, he was not. It was my poor daughter with me for the colonoscopy prep and it was not pretty.
When you have an obstruction, your prep is not only about bowel movements. I was vomiting all night. It was the sickest I thought I’d ever feel. I wasn’t thinking it was the prep. I thought, “The cancer is spreading as the days go by.”
Once I got to the colonoscopy, it was very easy. I woke up from it 30 minutes later. But I never got to meet with my doctor nor heard from him. That led me to change doctors, which happened pretty quickly. I didn’t let that linger too long. I gave it a couple of days.
I feel like, as a doctor, especially when diagnosing cancer patients, you should have a conversation immediately after the colonoscopy. It might have been four or five days, but I never heard from him, so I went to another doctor, who I’m with now.
Meeting the surgeon in an empty hospital hallway
I switched to Sarah Cannon Research Institute (SCRI) because I’m here in Nashville. There’s also Vanderbilt-Ingram Cancer Center. My husband works for HCA, and he was able to get some conversations moving with his peers.
We scheduled an MRI, but I still had no doctor at this point. I had an MRI on a Sunday morning. To have this MRI, you had to go through the emergency room and nobody was in there. The halls were empty.
There is a surgeon who is very well-known in the area that I had planned on calling. His reputation is that he’s difficult to get in with. As I was leaving the imaging room, out of nowhere was the surgeon that I planned on calling the following day.
The halls were completely empty, so it was a very eerie meeting. I saw him and thought, “It’s probably my head playing tricks on me,” but I said, “Doctor Aston?” He turned around and said, “Yes?” I said, “I’m supposed to call you tomorrow.” He said, “You are? What for?” I said, “Here’s my situation and here’s what’s leading me to get in touch with you.” We had a 20-minute conversation outside the imaging room. He said, “Call my office tomorrow. I’ll see you Tuesday at 8 a.m.,” and he walked away.
He spent about 20 minutes with me in this hallway. Before he walked farther, he turned around and said, “Interesting that we ran into each other.” I said, “It is. Thank you so much. I’ll see you Tuesday morning.”
I went to see him on Tuesday morning and that’s pretty much where everything started: our planning, what to do next, all of that. That was when I got the official diagnosis of stage 4.
How I emotionally processed my official diagnosis
By the time I had that Tuesday meeting, I had already processed it. I already knew how I was going to fight, how I wanted to fight, and what my attitude was going to be like. I told my family and friends. I was speaking high volumes by then.
I didn’t have fear. I just wanted to know the plan. While I was in North Carolina, I made a post on Facebook semi-announcing my diagnosis to find other people who shared the same diagnosis. If you Google colon cancer, all you see is survival rate and I didn’t want to hear that. I wanted to hear from someone who has battled it and survived it. Even if it was a friend of a friend who lost somebody to the diagnosis, I wanted to start talking to people and have them share their stories with me.
By the time I had my appointment, I was ready. I was ready for the plan.
Building my treatment plan and confirming the cancer
With my diagnosis, the standard first line of treatment is chemotherapy. The type of chemotherapy was FOLFOX. Dr. Aston told me, “I believe your body will respond well to it. We’re going to hope for that, but I have a good feeling.” I said, “Okay, that’s all I need. I know no one can guarantee anything. I just need to know that my body is strong enough at this point that it’s ready to take in this chemotherapy.”
From there, I went to Sarah Cannon within a few days and met with my oncologist, Dr. Pelster. From Dr. Aston’s office, he scheduled what’s called a flexible sigmoidoscopy, a type of colonoscopy that’s a little bit more invasive and gets closer to the tumor, so he can see more.
He did the flex sig and biopsied the mass. The pathology report came back as high-grade dysplasia, which means almost cancer. I went back and said, “Okay, so do I not have cancer?” He said, “No. I saw it. It looked pretty cancerous to me. I think what we need to do is get you in touch with Dr. Pelster and discuss the next steps, because I’m pretty sure what I saw was cancer.”
When I met with Dr. Pelster at Sarah Cannon, she scheduled a liver biopsy. She wanted to get a sample of one of the lesions. If that came back positive, then we knew we were dealing with a positive diagnosis.
For a good month, we were back and forth. I make jokes about it now. It was like I had cancer one day, not the next, had it again, not again. There was a lot of back and forth, but it was no one’s fault; we were just trying to figure it out.
Before I could start chemotherapy, I had to get a confirmed diagnosis from one of the lesions. The liver biopsy came back positive, so we went back to the drawing board and discussed my treatment plan.
My full list of stage 4 colon cancer treatments so far
I’ve done 27 rounds of chemotherapy. I started with FOLFOX. By round two, we added panitumumab, which is a type of immunotherapy. It doesn’t use your immune system; it uses antibodies, so that makes it under the immunotherapy umbrella.
Then I went to FOLFIRI. I also had a pump placement, hepatic artery infusion therapy, a liver resection, and later, a colon resection and a full hysterectomy.
Becoming the first hepatic artery infusion (HAI) pump patient
My treatment started on September 3rd. By October, we started talking about the hepatic artery infusion (HAI) therapy. At the time, Sarah Cannon was not offering it. It’s very limited in the United States. Not every hospital, not every cancer center offers it. There are many surgeons out there who are even unaware of this particular treatment.
Vanderbilt has it as a trial. We started the discussion, and my oncologist sent me to them to talk with the team about it. We quickly learned that I was a very good candidate for it. I was healthy with vessels and arteries strong enough to handle the type of drugs that would be placed in my liver.
Then you go through a trial process, which I’d never done before. There are several tests. The way the trial worked for this particular program — though I don’t know how other programs work — was literally computer-chosen. Once they put in all my information and the doctor cleared me as a candidate, they entered it into a computer, and it randomly selects whether you are or are not chosen. I was not selected, so I went back to Sarah Cannon and back to the drawing board.
In the meantime, HCA Healthcare was in the process of meeting and discussing starting the program through their healthcare system, which meant they would provide HAI therapy off-trial to patients at Sarah Cannon, where I already was. But I had to be patient.
I went back to chemotherapy while they were working on it. Surgeons and doctors were getting together and trying to figure out how they could start this program at the hospital. This was around November to December. By February, we found out that it was approved to begin at TriStar Centennial, which Sarah Cannon is part of. I was the first patient to receive the hepatic artery infusion pump from HCA in Nashville.
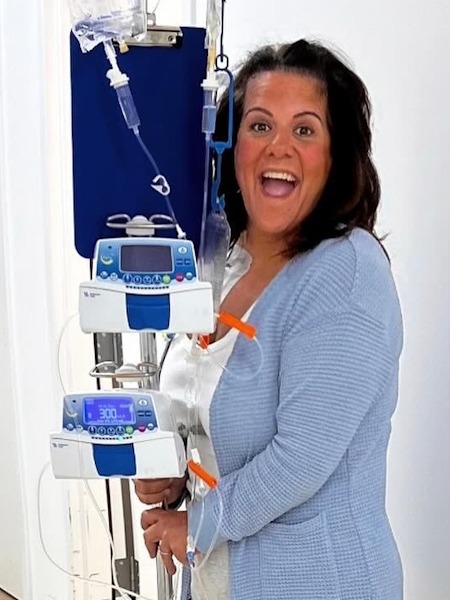
Getting the HAI pump and what it was like
In April 2025, I had the pump implanted, which goes into your abdomen. It’s a surgical procedure having the pump placed, so I was in the hospital for four or five days. I had a big scar, like having any other type of abdominal surgery.
Once I was ready to receive treatment, which was about four weeks following the pump implantation, we began the HAI therapy. The device is the size of a hockey puck. There’s a catheter from the pump to your arteries and vessels to your liver, which is like a direct line for the drug to go right to your liver. The direct line of chemotherapy going from the pump to my liver is about 400 times more potent than getting it systemically.
The amazing part is that you have zero side effects with this type of treatment. You’re given a lot of steroids. Personally, I had no sleeping issues, though everyone’s different. You have no side effects like you do with systemic treatment. You just wait, let it do its job, and hope that it’s working on shrinking the tumors and you’re responding to the treatment.
My remarkable response and liver resection
By November 2025, I was back at the hospital for a liver resection. I was told by several surgeons and radiologists that they’d never seen such a response from this type of treatment.
We only had to remove three lesions and do an ablation to two out of the 12 to 14 lesions. I had the liver resection. Following the liver resection, I healed and got scanned a few times. So far, I have been clear. There has been no evidence of disease in my liver since November.
In March 2026, I had a foot of my colon removed and Frank was removed. Between the liver resection and my colon resection, the cancer metastasized to my pelvis. I had about a softball-sized mass that was found while we were doing the scan to prep me for the colon resection. The timing was quite perfect. It was unfortunate, but it was also perfect.
Along with the colon resection, I had a full hysterectomy. Then I go back to treatment for cleanup.
Living through major surgery, hysterectomy, and colon resection
The hysterectomy and colon resection were done together. The surgery was only supposed to be about four and a half hours long, but it ended up being almost eight. Dr. Aston was very thorough and he took his time.
I feel like it’s anticlimactic a little bit. My guard is up. I feel better, but I haven’t processed that I currently have no active tumors. It’s a very strange feeling. You’re afraid to even say “no evidence of disease.” People have asked me, “Are you in remission?” No, I’m not in remission. People have asked, “Are you cancer-free?” I don’t consider myself cancer-free. I think I’ll always have cancer.
My goal since I’ve had surgery, which has been an epiphany over the last several days, is to live with cancer but to be treatment-free.
What it means to be the first HAI pump patient
I feel like I wasn’t supposed to be on the trial at Vanderbilt. I feel like my path was to be the first patient at HCA. I quickly figured that out. I wasn’t disappointed that I wasn’t chosen for the trial. I kept my faith that there was a reason why I wasn’t selected. When I was told I was going to be the first patient, I knew I wanted to be strong enough to pass on that hope to others.
I went back and thought of that very first conversation I had with the gentleman from the airline company. He gave me hope. A total stranger gave me hope. I’ve met strangers along the way who have done that for me. I thought, “This is my purpose. I think I am supposed to do that for others.”
Some are good at telling folks to go get colonoscopies and raising awareness. I actually very rarely tell people, “Go get screened #colonoscopy.” I’m the one saying, “Don’t give up.” One day, I didn’t have the device; the next day, I did. I thought I was going to be on chemotherapy for life to keep my liver going. I haven’t had to talk about transplants. There’s never been a discussion of my prognosis. My medical team has always focused on hope, being aggressive, and advocating.
Even as wonderful and skilled as my medical team has been, they have allowed me the opportunity to advocate. I ask questions and sometimes they say, “That’s a good question. It’s not been asked before. Let me look into that and I’ll get back to you.” Sometimes, what I ask, they choose to do. “Okay, let’s try this.”
Along the way, I’ve had patients reach out to me when they learned that I’ve received the hepatic artery infusion pump. I’ve had people from California, the UK, and Canada. Strangers will reach out and say, “I’m supposed to get this hepatic pump. My surgeon doesn’t give me too much information on it. I want to know what to be ready for after surgery.”
They ask, “Can you live with it?” Because when you have the pump, you can’t enjoy the hot tub. When you fly, you have to prepare for flying. You can’t just hop on an airplane and go. You can’t have heat directly on the device. You have to be careful about what type of exercise you’re doing, because it’s in a sensitive location. You don’t want it to flip.
It’s an investment in your life. You’re taking such good care of it. When you’re going into this type of therapy, you want all the information.
When patients call me, I tell them that I forget that I even have it. You don’t realize you have it in your stomach. It takes a little bit of time to get used to, but it saves your life. You shouldn’t worry about whether or not you can go in a hot tub. I’m direct with some: “Do you want to live or die?” They say, “I want to live.” Then there’s your answer.
My long-term plan with the pump
Yes, I still have the pump.
Once you get to liver resection and they’ve removed all the lesions, you go from treatment every two weeks with the pump to glycerin treatment. You’re filling your pump every 6 to 8 weeks with glycerin to keep the catheter clear, almost like flushing it, to keep it ready if it ever has to be re-activated and chemotherapy is placed back into the pump for recurrence.
It’s up to you as a patient how long you want to keep the pump. Some leave it for a year, some for up to five years. I’m going to keep it for as long as it’s not bothering me or causing pain.
If I have a recurrence in the liver — which, with colorectal cancer that has metastasized to the liver, there is a high risk for recurrence with lesions — I’d much rather go through the chemo through the pump with no side effects versus systemic treatment with side effects.
The treatment I’m starting now
I’m going back to systemic treatment. Based on my colon resection, there’s always a chance of microscopic cells left behind. We want to go full throttle and get it all now. I’d rather get it now and go aggressive, so hopefully I can enjoy a summer of possibly no treatment or limited treatment; maybe maintenance. That’s our plan for the next four to six months.
How cancer has changed my work, motherhood, and life
This is probably one of my favorite questions.
I have been in the nonprofit healthcare industry for about 30 years. I’ve spent that long advocating for cancer patients. I currently work with multiple sclerosis patients. I’ve been doing that for three decades: advocating, campaigning, events, and fundraising.
Now the roles have reversed. I’ve met parents of children whom I helped get bone marrow donor matches. Many of their kids are now in remission and grown; they’re adults in college, living and thriving. Many of those parents have now heard about my story, and they’re there for me as I was there for them.
The most impactful piece has been the community: friends, people from my past, and new friends I’ve met along the way. You hear every day on social media about the world and the things happening around us. Cancer has made me stop and see the beauty in our world and in people. I’ve seen true friendships.
I’m still working full-time with the MS Society. They’ve been incredible and very supportive. It’s interesting being an advocate and campaigner, and then becoming a patient. It’s almost an occupational hazard, but it’s been wonderful to see the outpouring of support from that community.
I don’t sweat the small stuff. I tell my family, “If the windows don’t get cleaned today, it’s okay. If you can’t pay a bill, we’ll get to it.” I’m almost probably a little too free, because my husband reminds me we still have a life to live, and in order to live it, we have to pay bills.
I want to do different things. I want to go horseback riding. My bucket list is not long. I haven’t even started a formal bucket list, which is interesting because a lot of people have.
I’ve been asked, “What do you want to do when you get to remission?” I said, “I may never get to remission, so I’m just going to start today and live in the moment, because it changes very quickly.”
Misconceptions about stage 4 cancer
I’m told all the time, “You’re not sick. You don’t look sick.” I say, “What is stage 4 supposed to look like?” I’m actually curious, because I probably would say the same thing.
Interestingly, the things I hear from people are no different than what I probably would have said. But now that I’m the patient, it’s interesting that apparently, you have to look sick for people to believe you’re sick.
The number one misconception is that you don’t have to look sick to be sick.
I truly believe that keeping it from your kids is doing them an injustice. Involving your children in your diagnosis, which I never thought I would do, has probably been the best thing I did. I’m teaching my daughter how to fight and about hope.
Another misconception is hope. There is hope every day. Treatments are changing every day. You just have to ask questions. We hear all the time to advocate, but not because you don’t believe your doctors or medical team. You advocate because the more you know about your diagnosis, the better you can treat it. It takes a team. It takes a village.
My biomarker testing and why some immunotherapies don’t apply to me
I got tested before I started treatment, right after my liver biopsy. We found out I was MSS stable. Then I got bombarded by people sending me links about new immunotherapies that have hit the market, which I appreciate, but with cancer — which I never knew — it comes down to the mutation and genetics of your tumor, your biology.
You almost have to have the “impossible” to receive a lot of these immunotherapies that are coming out, which is wonderful, but a lot of people don’t realize that. I get bombarded by, “I don’t know if you read this, but this is just coming out,” and I say, “Oh yes, I know all about that.”
My hope for the future
I’ve always told Dr. Pelster and my surgeons before every surgery, “I have to be here for Coco,” my daughter. They say, “You’re going to be here for Coco.” I say, “I know, but I want to be there for her, not just for when she gets married and has children. I just want to be here for her to graduate high school, which is next year.”
I actually wish I could just get her graduated now and off to college so I can help her decorate her dorm room. You want to speed up everything because you’re afraid you won’t be there.
I just want to be here. That is my goal. I just want to be here, and I’m hopeful it’s much further than five years. I’m very hopeful for that, because I won’t take anything less, quite honestly.
Yes, I need to be here for my family. It’s not just about me living. I’ve got to be here for my family. I don’t want to disappoint my family. I said I would fight, and I would fight hard, and that is my goal. I’m going to continue doing that.
I also want to give myself a bit more vacation time. I want to travel a bit.
My advice to someone who’s newly diagnosed
Stay strong. It was something that was told to me. Hearing somebody say, “I beat it,” “I’ve been in remission for two years,” or “I got through it. I got through 10 treatments and I’m okay. I was able to go to my daughter’s soccer game,” — that matters.
Live every day. Take it day by day. Take it one thing at a time, one step at a time. Go slow. There’s hope. Stay strong.
I would share my story. I was in the impossible and in 20 months, I’m tumor-free — and I shouldn’t be.
Why I say the HAI pump saved my life
The hepatic artery pump literally has saved my life. The colorectal surgeon told my sister before he wheeled me into the OR, “I didn’t think I’d even see your sister back to do the surgery. She’s a warrior. She’s supposed to be here to give the message.” He looked at me and said, “You’re remarkable.”
I can’t say it works for everybody, but it’s got pretty good success data behind it if you have metastasized liver lesions from colorectal cancer. If you have bile duct or any sort of liver disease, ask your doctor about this. It’s life-changing. I call the company and tell them all the time. I send emails: “I’m having a great day today because of this incredible device that I would have never known about had my doctor not advocated for me.”
There are a lot of surgeons out there, unfortunately, who don’t know about it. Patients need to start asking. Right now, if I could wear a t-shirt that says that, I would.

Inspired by Helen’s story?
Share your story, too!






Leave a Reply