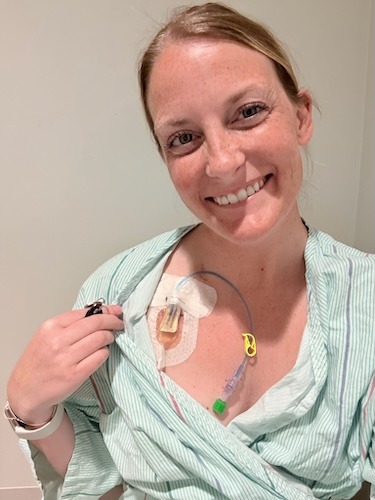Reclaiming Movement: Kelsey’s Stage 4 EGFR+ and ALK+ Non-Small Cell Lung Cancer Story
Kelsey was a 36-year-old fitness professional and mother of four living in Lake Stevens, Washington, when she began experiencing debilitating back spasms that would eventually lead to a diagnosis of stage 4 non-small cell lung cancer. A self-described workout junkie and fitness studio manager, Kelsey initially attributed her pain to the physical demands of her job, aging, or a potential injury. However, after several incidents where her back completely collapsed, including one during her sons’ baseball tournament, she realized the issue was far more significant than just a pulled muscle.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
The emotional turning point in Kelsey’s experience occurred when she received her prognosis in writing through adoption paperwork. While doctors had previously sugarcoated the severity of her lung cancer, seeing the words “prognosis is less than two years” forced her to confront her reality head-on. This moment of clarity shifted her perspective from simply managing metastatic non-small cell lung cancer to “living like she’s dying,” a transition that led her to transfer her care to Fred Hutchinson Cancer Center and prioritize reclaiming her quality of life through advanced treatments and clinical trials.
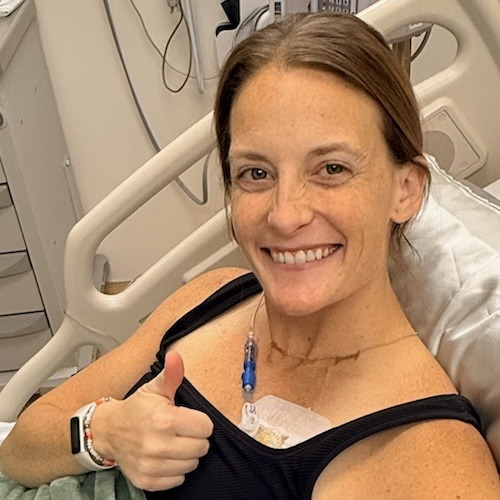
Today, Kelsey lives with an extremely rare combination of both EGFR and ALK mutations. After a life-changing spinal fusion surgery that replaced her collapsed L5 vertebrae with a titanium cage, she has returned to the physical activities she loves, including riding her Peloton and coaching her boys. By focusing on the “new normal” and leaning on a supportive community, she emphasizes the importance of self-advocacy and treasuring every moment of physical health.
Watch Kelsey’s video or read the edited transcript of her interview below to delve into her story.
- Advocate for answers: When initial X-rays came back normal despite her inability to walk, Kelsey pushed for an MRI that ultimately revealed the lesions on her spine and pelvis.
- Rare mutations require specialized care: Having both EGFR and ALK mutations is extremely rare, leading Kelsey to join a clinical trial to target the disease when standard data was unavailable.
- Surgery can restore quality of life: A spinal fusion surgery allowed Kelsey to move from living an “eggshell life” back to lifting weights and playing with her children.
- Let people help you: Kelsey learned to accept care packages, hospital visits, and emotional support without the guilt of “assigning” tasks to her loved ones.
- A universal truth: Physical health is often taken for granted until it is restricted; reclaiming movement provides a unique motivation to “leave nothing behind.”
- Name: Kelsey D.
- Age at Diagnosis:
- 34
- Diagnosis:
- Non-Small Cell Lung Cancer (NSCLC)
- Staging:
- Stage 4 (Metastatic)
- Biomarkers:
- EGFR exon 19 deletion
- ALK
- Symptoms:
- Severe back pain
- Falling due to collapsed spinal vertebrae
- Treatments:
- Radiation therapy
- Targeted therapy (tyrosine kinase inhibitor): osimertinib
- Surgery: spinal fusion surgery
- Chemotherapy through a clinical trial
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My life as a fitness professional before diagnosis
- The first signs: Back spasms and physical collapse
- Navigating the healthcare system and seeking an MRI
- Receiving the news: "Are you sitting down?"
- My stage 4 non-small cell lung cancer diagnosis
- Facing a prognosis and transferring care
- Reclaiming my life through spinal fusion surgery
- Managing rare mutations: EGFR and ALK
- The importance of self-advocacy and support
- Awareness: Anyone with lungs can get lung cancer
My life as a fitness professional before diagnosis
Before cancer, I was very active. I was almost obsessed with working out. I grew to love fitness so much that I wanted it to become my career.
I started studying to be a personal trainer and group fitness instructor, and I was planning my workouts as if it were my job. I was doing three workouts a day — before work, during lunch, and after work. It just fueled something in me.
I love working out because it just ignites something in me. I feel so strong physically and mentally, and it just makes me a better person. It flips a switch in me that makes me nicer, more motivated, and changes the trajectory of my day every time.
The first signs: Back spasms and physical collapse
Leading up to my diagnosis, I was managing a SoulCycle. In May, I was dealing with really bad back pain that prevented me from working out. I was gaining weight and making excuses — maybe I was getting older or going through menopause. But the pain got so bad that if I took a wrong move, my back and hips would completely spaz and lock up, and I would fall to the ground.
I was at one of my boys’ baseball tournaments, and a sprinkler surprised me. I flinched, my back locked, and I collapsed in front of the whole team.
I played it off as a joke, but deep down, I knew something was really wrong.
Navigating the healthcare system and seeking an MRI
After the first collapse, it happened again at home. I got out of bed and collapsed to my knees; I had to crawl to the bathroom. We realized this wasn’t just a pulled muscle. I went to the chiropractor, but nothing worked.
I was recommended for an X-ray, which came back normal. They told me I had to go to physical therapy for four weeks before I could get an MRI. I went to physical therapy once and said, “I’m not waiting four weeks.”
I pushed for the MRI, and, thankfully, insurance approved it. Those results are what led to my diagnosis.
Receiving the news: “Are you sitting down?”
I was at work when I got the call from the orthopedic doctor.
He asked me if I was sitting down, which is a sign of bad news you only hear in movies. He told me the scans showed lesions in my pelvis and on my spine. I was so blissfully unaware of the cancer world that I asked, “What is a lesion?” I thought it was a scrape. He explained it was like a tumor and told me to reach out to an oncologist.
I sat in my car in silence for an hour and a half on my commute home, just processing. When I got home, I saw my kids first and tried to pretend everything was the same. Then I found my husband, Anthony, in our office and told him, “They think it’s cancer,” and I just collapsed in his arms.
My stage 4 non-small cell lung cancer diagnosis
We were told it was cancer on June 6th, but we didn’t know what kind. That month was spent living in limbo — appointments, scans, and researching.
On July 1, I was at work when my oncologist called and said, “We found your tumor. It’s in your lung. You need to get to the ER immediately.”
I went to work that day as a studio manager and left that night as a cancer patient. They showed me the scans; the tumor was a couple of centimeters large, and we knew it was stage 4 because it was in my bones.
At the time, I didn’t even know that stage 4 meant it wasn’t curable.
Facing a prognosis and transferring care
The reality really hit me when I needed paperwork for the adoption of my two oldest boys. The doctor had to fill out a form asking if I was capable of parenting. The doctor wrote “Yes,” but added that my prognosis was less than two years. That was the first time I had officially heard a timeline.
I ended up transferring my care to Fred Hutch. My new oncologist was amazing; she gave it to me straight. She told me, “Your life will never be the same. You need to get used to a new normal.”
I broke down because it put this invisible pressure on me to live like I’m dying, which is much harder than it sounds.
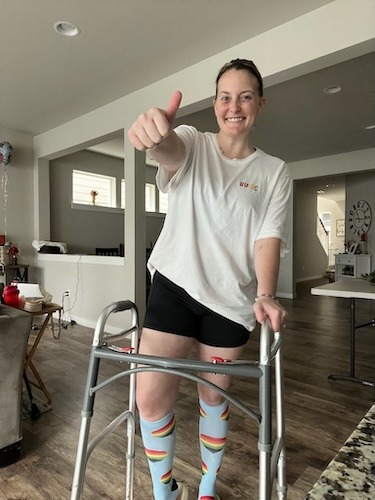
Reclaiming my life through spinal fusion surgery
My spine was collapsing by over 60%, which is why I kept falling.
In November, I had a spinal fusion surgery. They went in from the front and the back, removed my L5 vertebrae, and replaced them with a titanium cage. I had to relearn how to sit, stand, and walk.
But that surgery gave me back everything. I was living this “eggshell life,” terrified that one wrong move would break me. Now, I can move freely. I can play catch with my kids, go on daily walks, and lift weights.
It was literally life-changing.
Managing rare mutations: EGFR and ALK
I initially started on osimertinib for my EGFR mutation. It was a pill with minor side effects, and I almost felt like I had imposter syndrome because I felt so good. But eventually, the cancer progressed.
I pushed my doctor for more tests because things felt different. When I got my new oncologist, she did biomarker testing again and found I now also have the ALK mutation.
Having both is an extremely rare combination with very little research. We decided on a clinical trial that targets EGFR.
So far, it’s going amazingly. Things are shrinking, and the goal is to stay at this plateau for as long as I can.
The importance of self-advocacy and support
Advocating for yourself was the first piece of advice I received, and it’s so true.
I am on my third oncologist because you need to be with someone who listens to you and believes you. It’s okay to be “annoying” when your life is on the line.
The second piece of advice was to let people help. The people in my corner didn’t ask, “What can I do?” — they just showed up with care packages, texts, and visits during my seven-hour chemo sessions.
I’ve never felt so loved. It’s a beautiful thing to receive that love while you’re still here to feel it.
Awareness: Anyone with lungs can get lung cancer
I want people to know that anyone with lungs can get lung cancer.
I was a non-smoker and fairly healthy; I didn’t even know this was an option for me. It’s not just a “smoker’s disease.”
Spreading that awareness has been a blessing because nobody I know thought I could get this either. Now, I move every day — even if it’s a 30-minute low-impact ride on my Peloton. I tell my kids to take advantage of their healthy bodies.
Don’t leave anything behind.

Inspired by Kelsey's story?
Share your story, too!
Related Cancer Stories
More Lung Cancer Stories
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
...
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
...
Natalie B., Non-Small Cell Lung Cancer, Stage 4 (Metastatic)
Symptoms: Extreme fatigue, severe cough
Treatments: Chemotherapy, immunotherapy, clinical trials, radiation therapy, surgery (double lung transplant)
...
Stephanie K., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent and intense cough, general feeling of sluggishness
Treatments: Chemotherapy, targeted therapy through a clinical trial, radiation therapy
...
Jennifer M., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptoms: None per se; discovered during physical checkup for what seemed to be a sinus infection
Treatments: Radiation therapy (stereotactic body radiation therapy or SBRT), targeted therapy
...
Laura R., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent cough, fatigue, bone pain
Treatments: Targeted therapies (tyrosine kinase inhibitors or TKIs, including through a clinical trial)
...
More Non-Small Cell Lung Cancer Stories
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
Roxanne C., Non-Small Cell Lung Cancer (NSCLC), Stage 3
Symptoms: None; incidental finding
Treatments: Surgery (lobectomy), chemotherapy (cisplatin), radiation therapy, targeted therapy (tyrosine kinase inhibitor/TKI)
Natalie B., Non-Small Cell Lung Cancer, Stage 4 (Metastatic)
Symptoms: Extreme fatigue, severe cough
Treatments: Chemotherapy, immunotherapy, clinical trials, radiation therapy, surgery (double lung transplant)
Maggie M., Non-Small Cell Lung Cancer, EGFR+, MET Amplification & Overexpression, Stage 4 (Metastatic)
Symptoms: Ocular migraines (kaleidoscope vision), partial blood clot (DVT) in the leg, vision and balance problems, minor chest pain
Treatments: Targeted therapy (tyrosine kinase inhibitors or TKIs), radiation therapy (stereotactic body radiotherapy or SBRT), clinical trials, chemotherapy (combined platinum-based regimen)