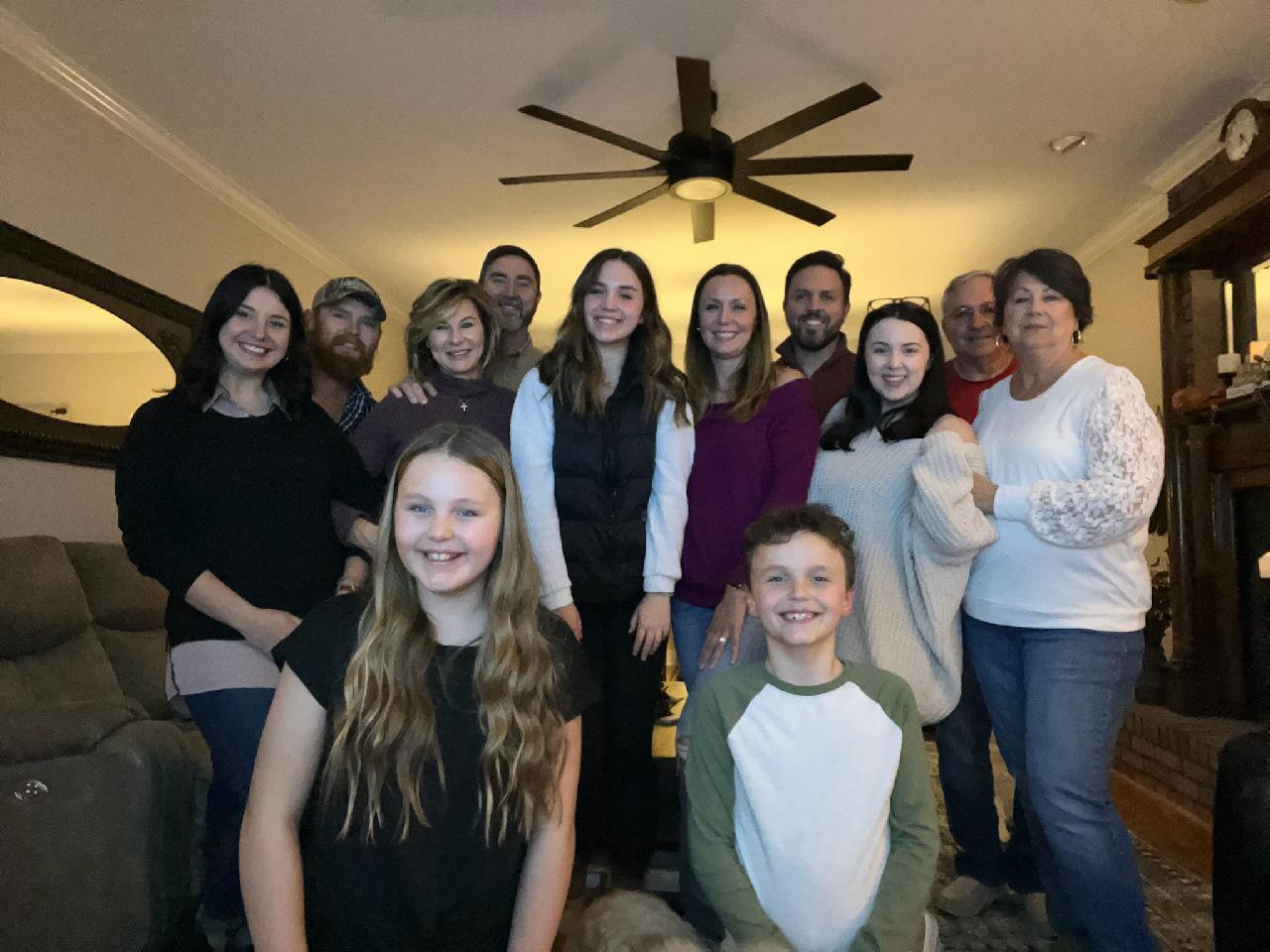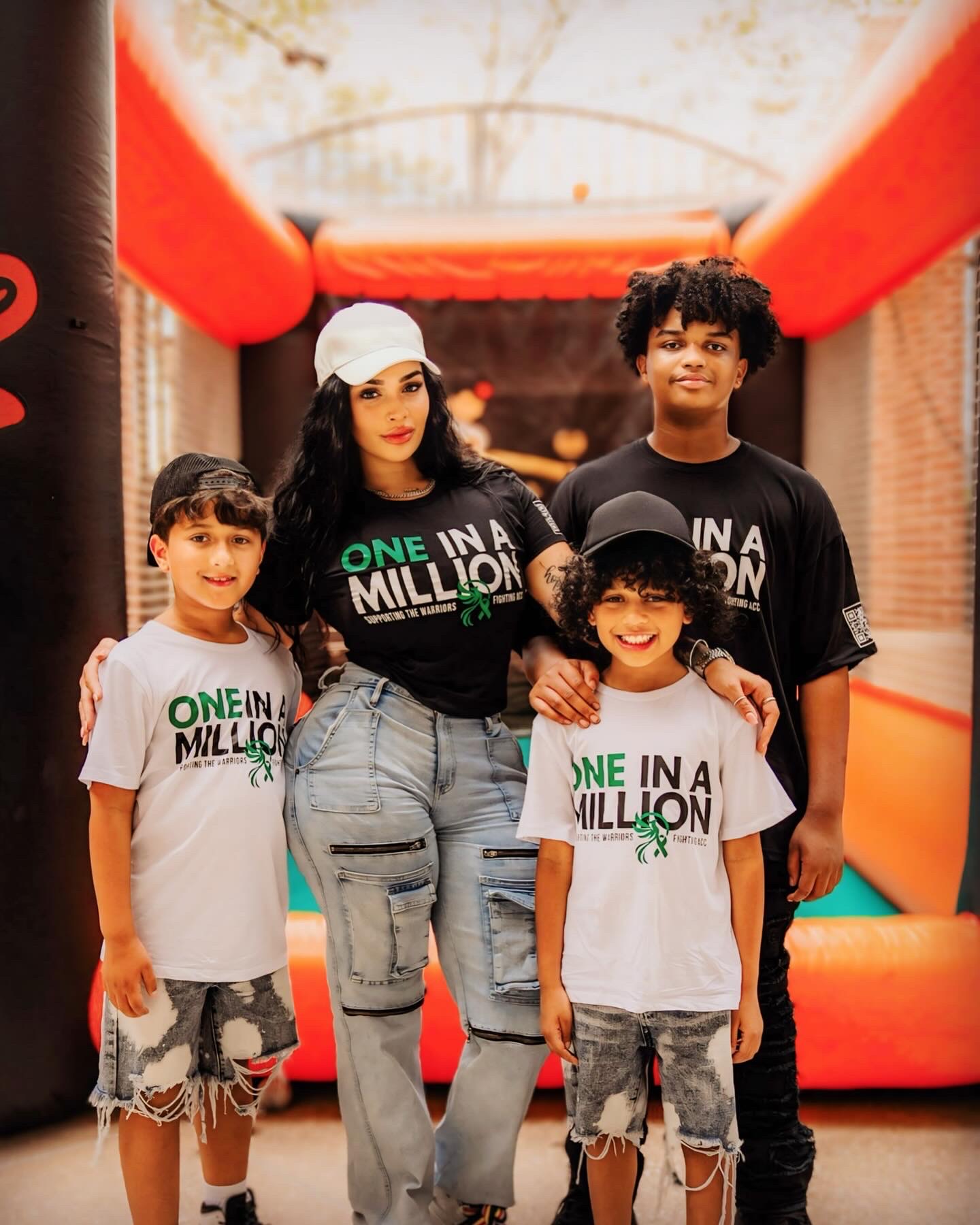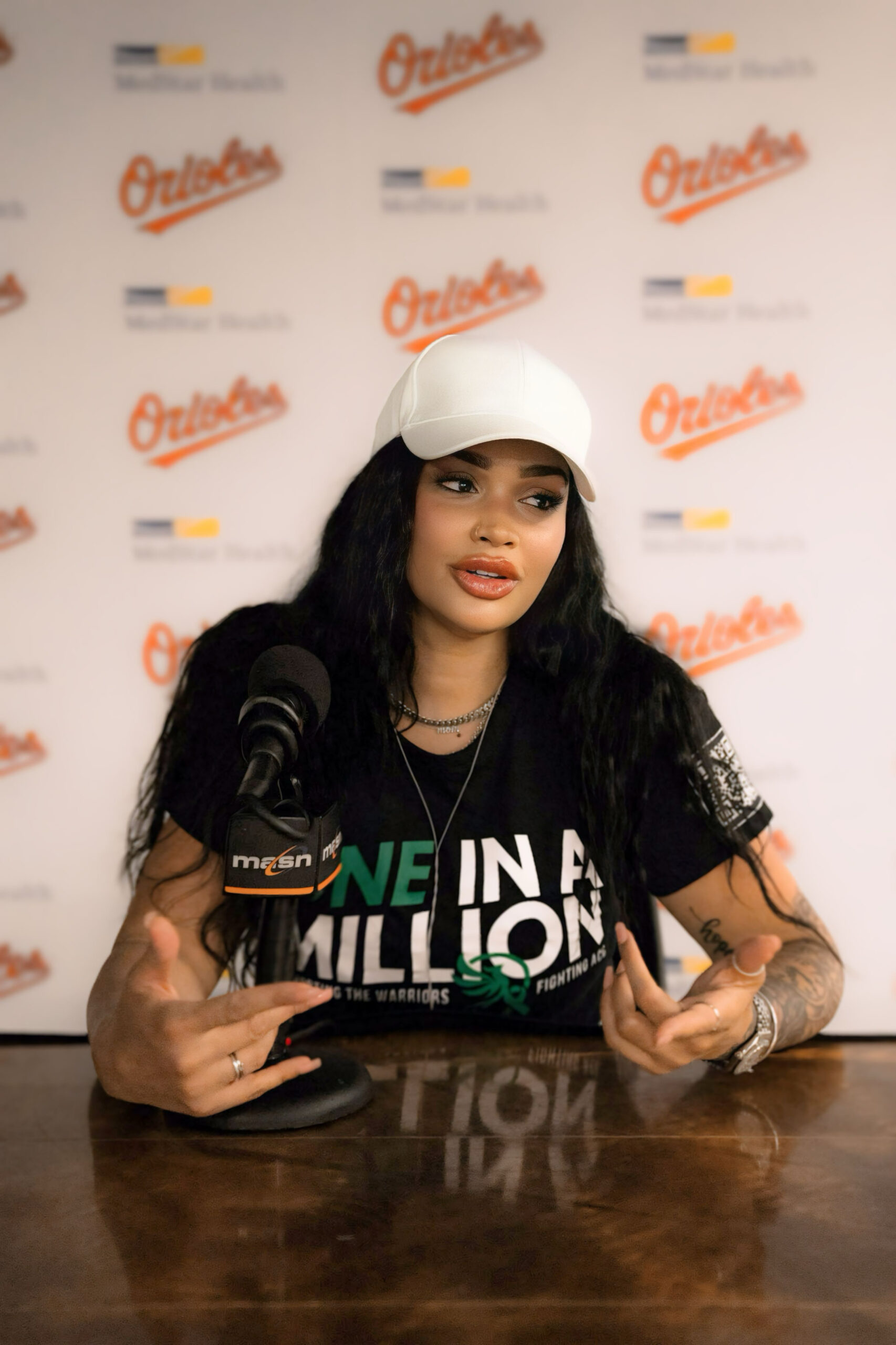Amanda’s Stage 4 ALK+ Lung Cancer Story
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez

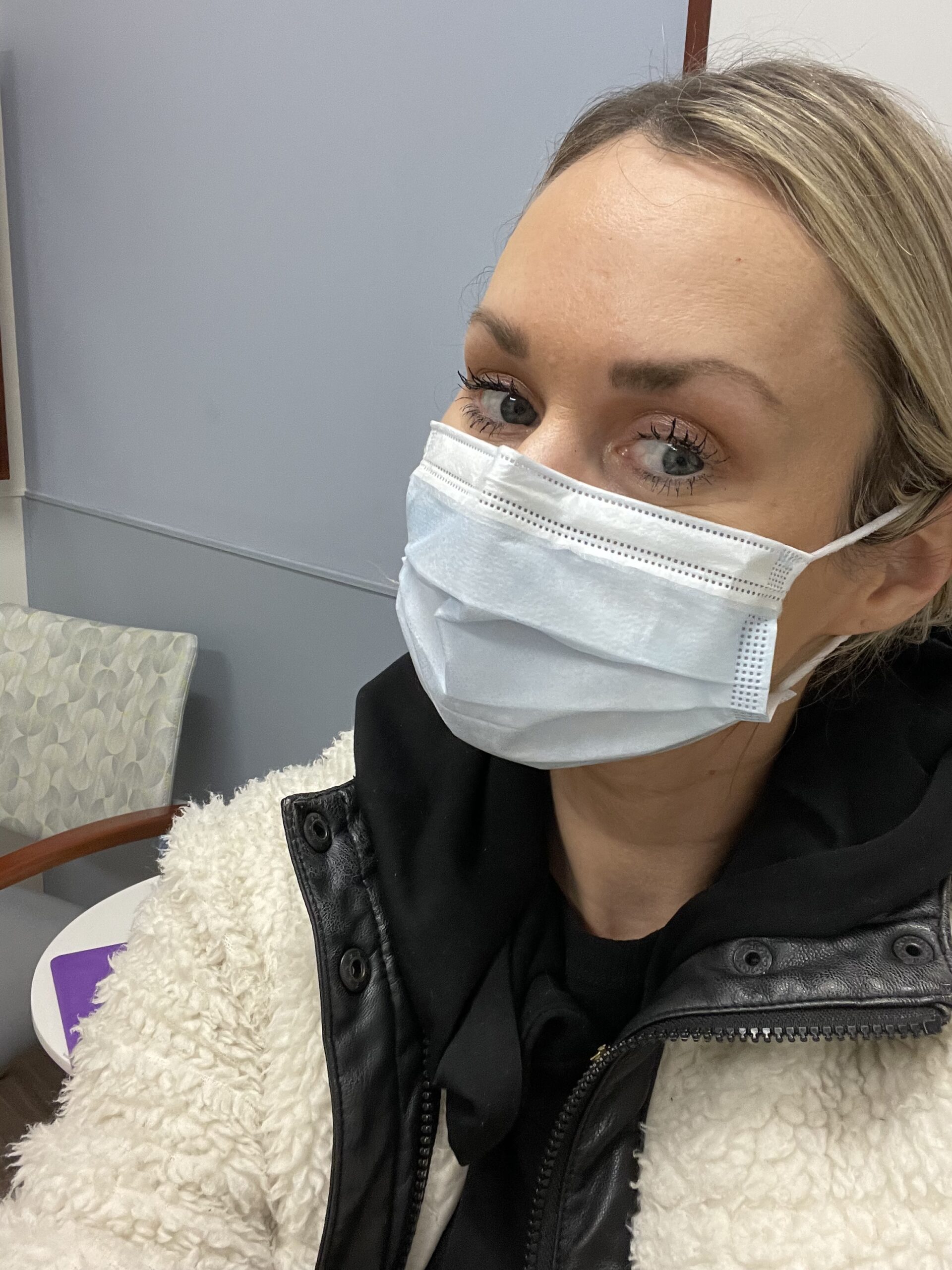
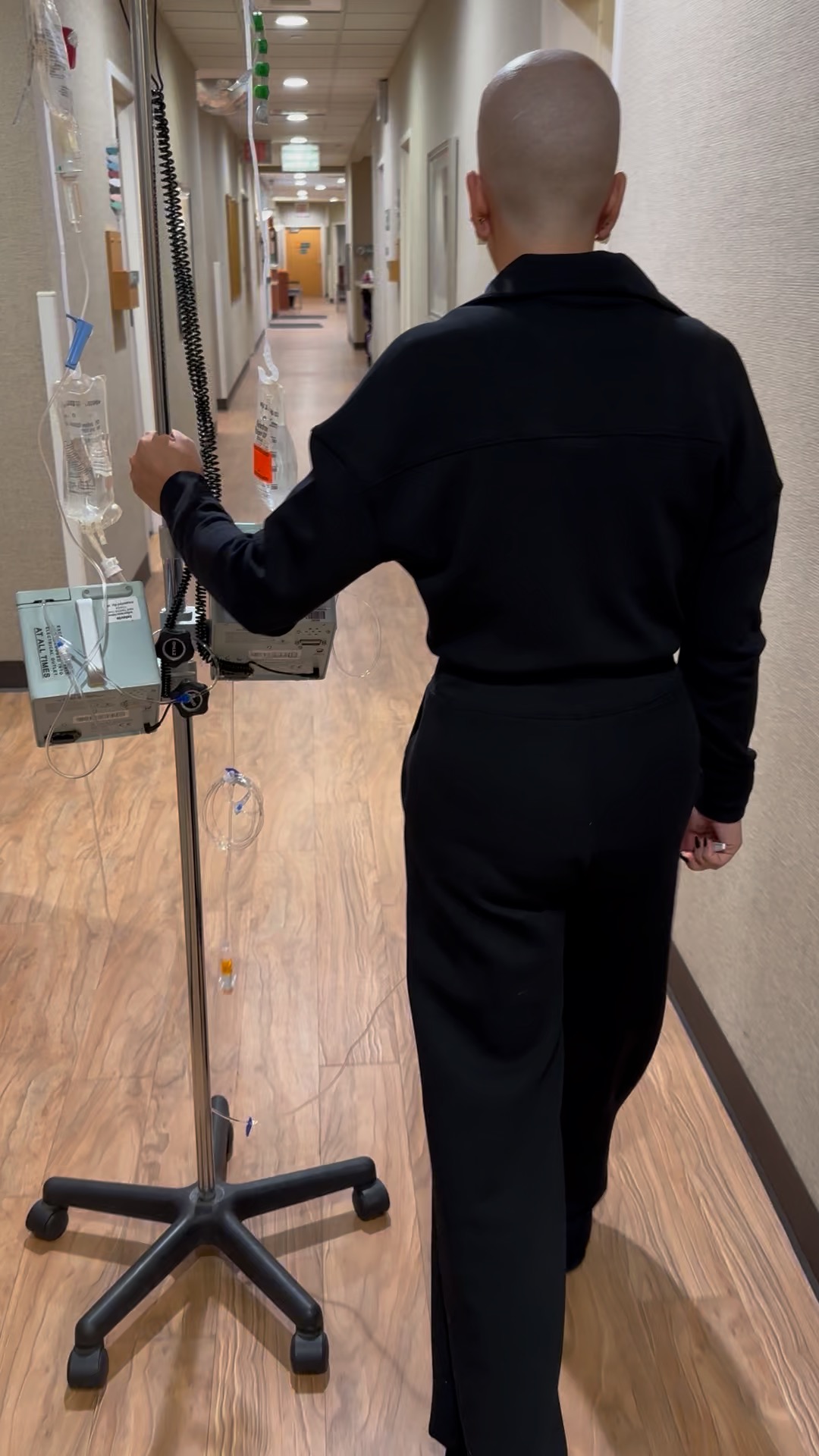
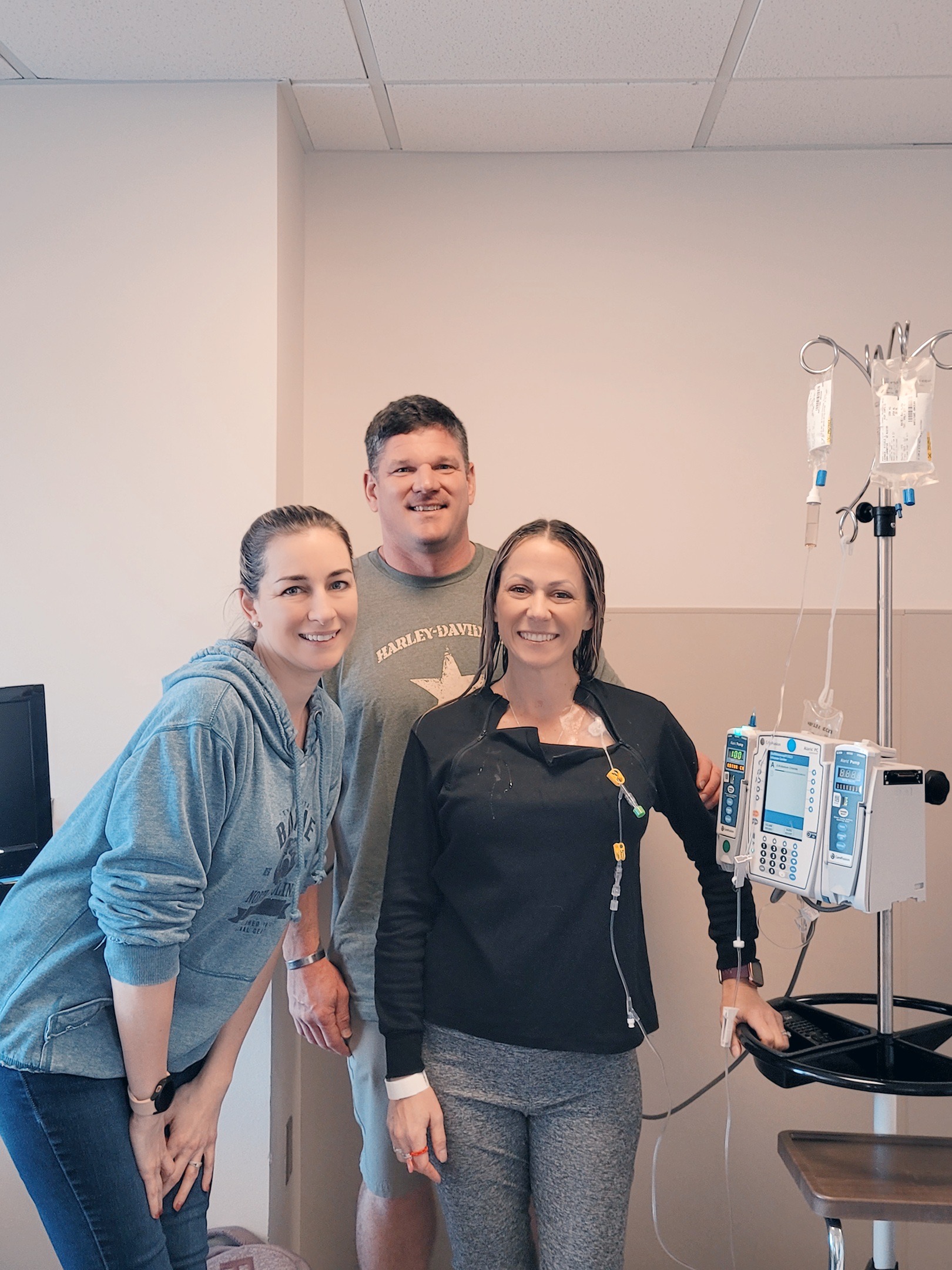
Amanda, 38, was diagnosed with stage 4 ALK+ lung cancer 10 days after giving birth to twin boys. Reflecting on her journey, she shares how her life transformed drastically within 18 months—from a single, active woman who had embraced life for years after having overcome crippling panic attacks in her early 30s, to becoming a fiancée, stepmother, and mother to twins.
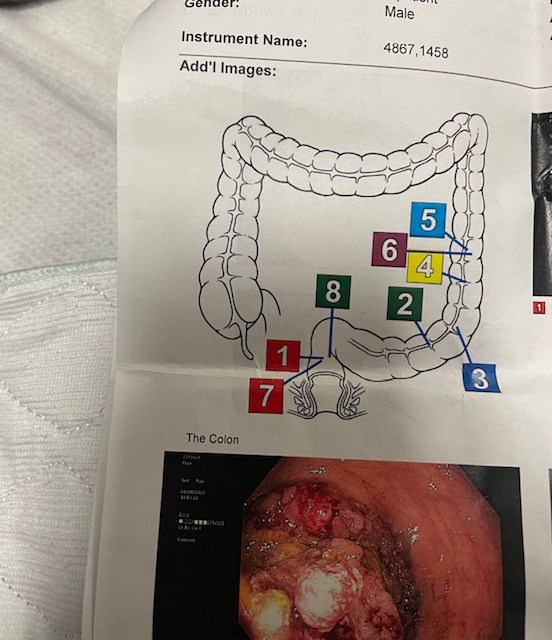
Amanda’s diagnosis came at an unexpected time, during what should have been a joyous postpartum period. In November 2021, she experienced a brief, unexplained breathing episode, but was reassured by her doctor that it was likely a fluke. She let it go, focusing instead on her unexpected twin pregnancy, which physically challenged her. She began to experience a nagging cough that doctors initially attributed to her pregnancy. After her twins’ birth, Amanda’s cough persisted and worsened. She returned to the emergency room, where tests uncovered a pleural effusion and ultimately led to her lung cancer diagnosis.
The confirmation of stage 4 lung cancer was overwhelming, given Amanda’s recent pregnancy and previous healthy lifestyle. Despite the challenges, she showed resilience, navigating postpartum recovery while coming to terms with a terminal diagnosis. Amanda credits her husband with helping her emotionally, as he remained steady amidst the whirlwind of emotions, and her family for also helping keep her grounded.
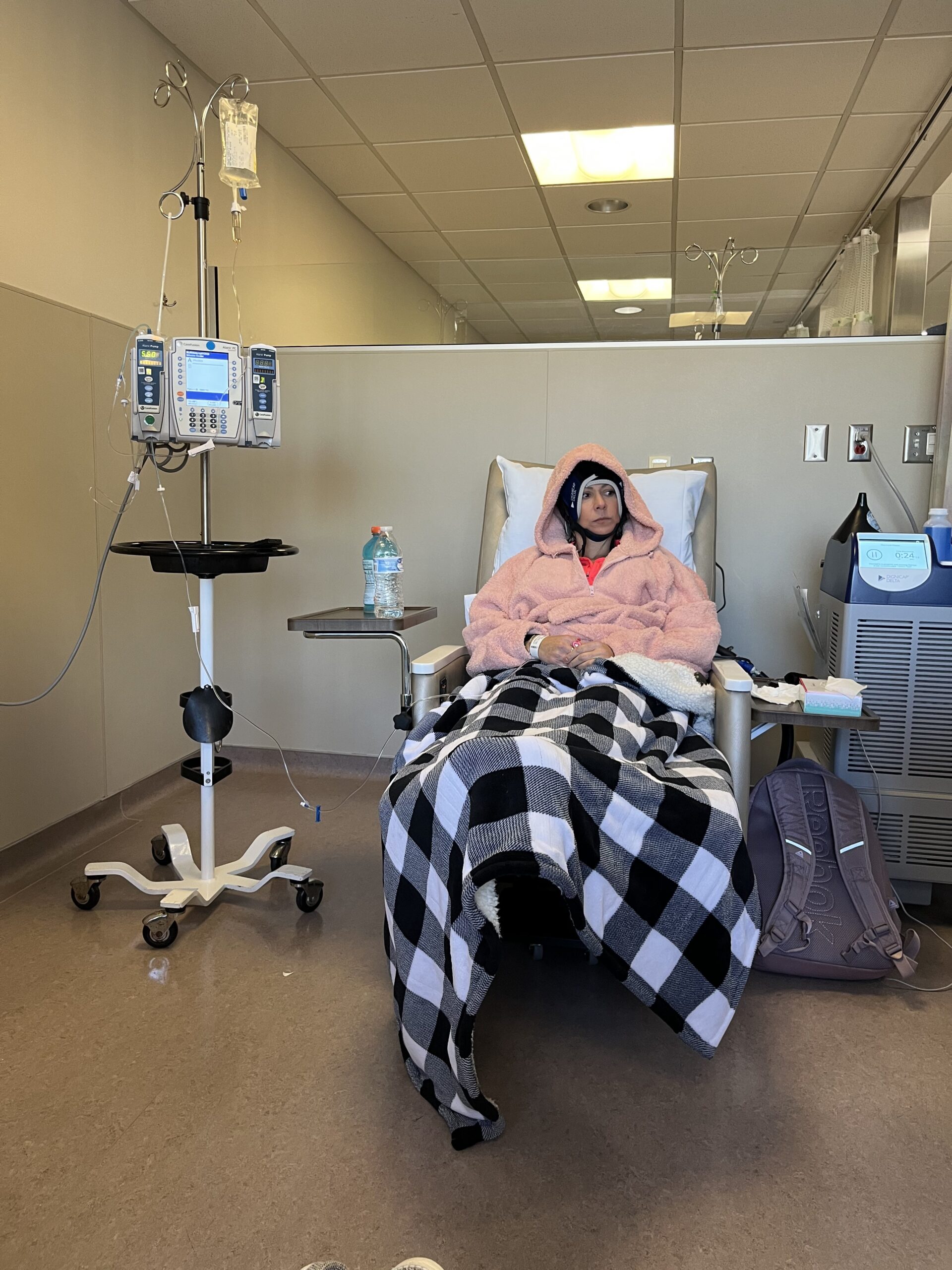
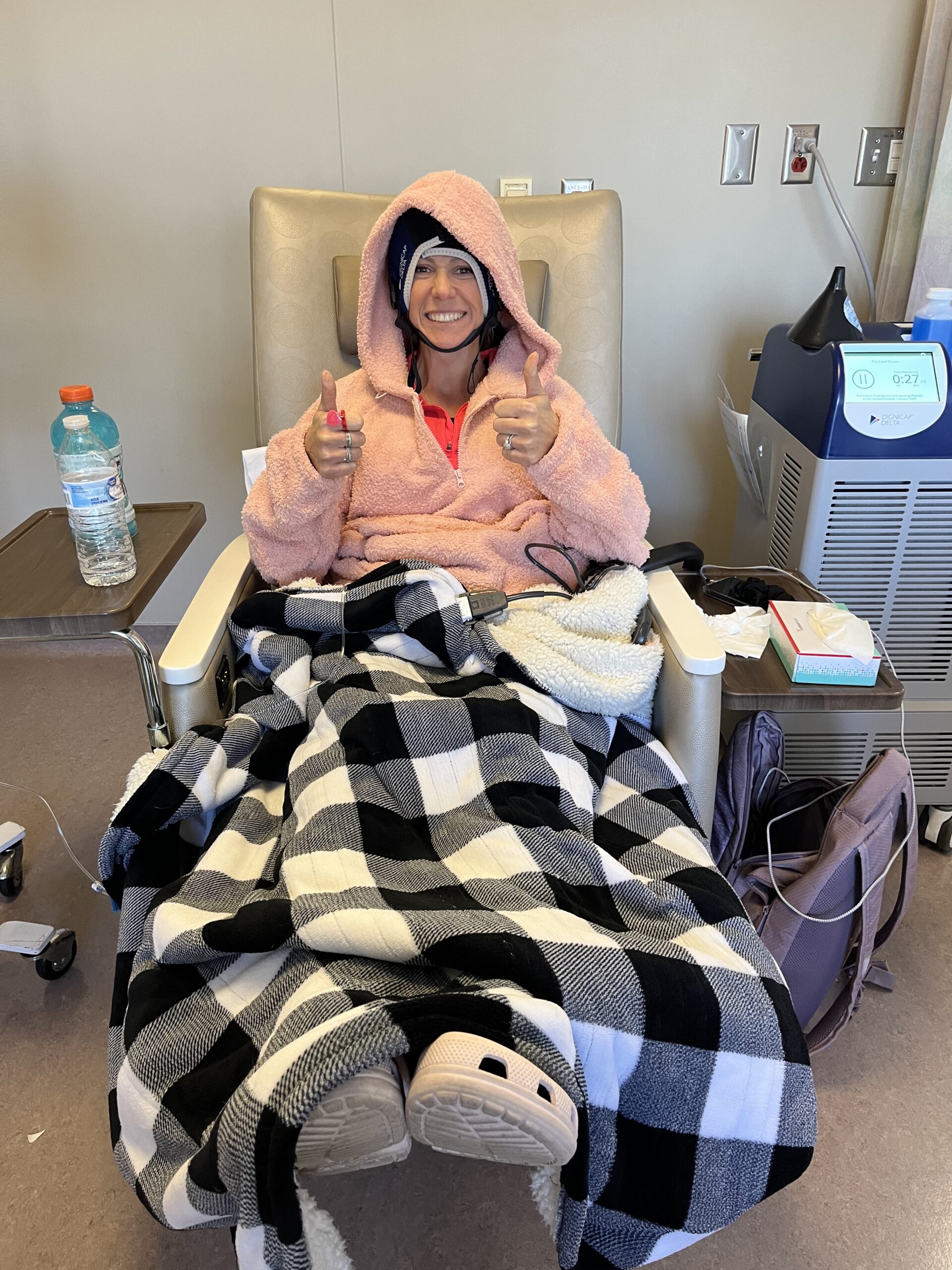
Amanda’s oncologist offered a glimmer of hope when they discovered that her cancer had the ALK+ mutation, allowing her to receive targeted treatment rather than traditional chemotherapy. This moment sparked a sense of optimism and opened the door to her discovery of a supportive community, especially Summer, another young woman with ALK+ lung cancer. Their connection was a lifeline, offering mutual understanding and hope. Amanda eventually joined the board of the ALK Positive nonprofit alongside Summer. There, she advocates for other young lung cancer patients, and also does so through her Instagram account.
Today, Amanda balances hope with realism. Living with stage 4 cancer, she finds strength in her connection to advancing science and medicine, which enable her to lead a near-normal life. She takes daily medication and has resumed her athletic activities, and is even training for a 10K run, with people often unaware of her diagnosis. Amanda attributes her resilience to her family, the ALK+ community, and her optimism. She embraces each day, focusing on the balance between staying grounded and hoping for continued medical breakthroughs.
- Name:
- Amanda B.
- Diagnosis:
- Lung Cancer
- Staging:
- Stage 4
- Initial Symptoms:
- Trouble breathing
- Elevated heart rate
- Persistent cough
- Treatments:
- Targeted therapy


We would like to thank The White Ribbon Project for its partnership.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Thank you to Johnson & Johnson for supporting our patient education program. The Patient Story retains full editorial control over all content.
… the two lives I had [I’m a mom to twins, I’m a wife, I’m a stepmom, and I work full time] are completely separate.
And cancer happened to come right in the middle of them.
Introduction
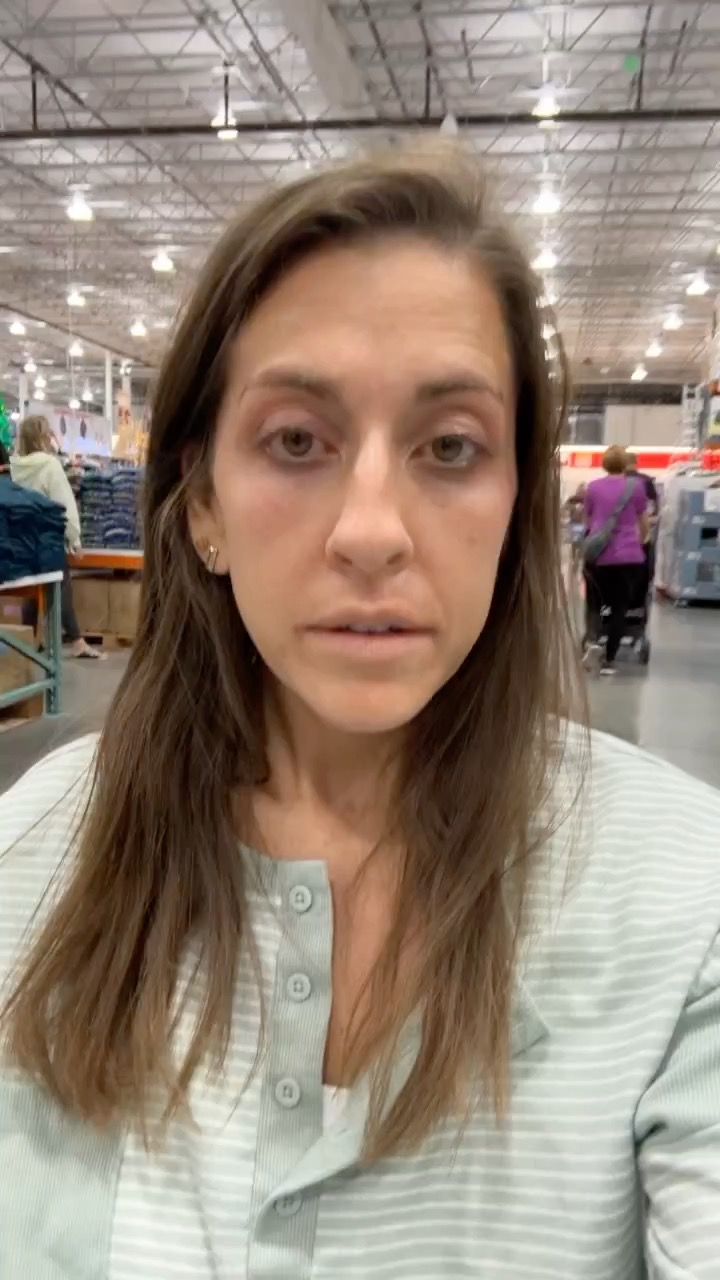
Hi, I’m Amanda. I’m 38 years old and I was diagnosed with stage 4 ALK+ lung cancer when I was ten days postpartum.
It’s kind of hard to talk about who I was before versus who I am after, only because so many huge milestones all happen right at the same time that I got diagnosed.


Pre-diagnosis
So, prior to diagnosis, I was a single girl living in my bachelorette apartment with her dog. I was a runner. I worked out, I lived my best life all the time.
I had a really big thing happen with me when I was in my early 30s, and I decided to overcome it. I had panic attacks, and I decided that I had to overcome them, because I needed to live my best life. And Lord, let me tell you, I did live an incredible life from like 30 to 36.
And then the big life change started in February of 2022. I surprisingly got pregnant by my then boyfriend and it turned out we were going to have twins.
And then during my pregnancy, we moved in together, with my mother-in-law. We blended as a family because he had a son already from his first marriage, so I became a stepmom.
Then during my pregnancy we got engaged. Then I delivered the twins. And so in an 18 month period, I went from this single bachelorette girl living her best life, with a dog as my “child”, to a girlfriend, to a fiancee, to a wife, and then to being a mom of twin boys. And then I went from living alone to living with all of those people.
So today, the life outside of cancer would be I’m a mom to twins, I’m a wife, I’m a stepmom, and I work full time. I still live my best life like, thank God for medicine. But the two lives I had are completely separate. And cancer happened to come right in the middle of them.
Initial symptoms
My first experience with any symptoms was in November 2021, about 11 months before my diagnosis.
It was a breathing episode that I had overnight. All of a sudden I couldn’t breathe. It lasted for about 20 seconds and it was very scary.
And I went to my primary care doctor and they did a chest x ray and a breathing test and everything came back fine. And she said to me, you know, you’re 35, we can do more diagnostic testing. But the truth is, it was probably just some crazy fluke. We can do more testing if you want to, and if not, oh, well, you’re 35.

And I really did just let it go because a couple of months later, I ended up pregnant, and focused on that. And I was 35, so it was considered a geriatric pregnancy. And then it was spontaneous twins. So it was a whole thing. And for me, pregnancy was physically the hardest thing. For the first 4 months, everything was just hard. I was nauseous, for instance.
I felt like I needed to rally to do stuff, and I did. I worked out every day of my pregnancy because I kept thinking that if I work out, things are going to get easier. So I was doing my peloton bike, Pilates, weight lifting, swimming. And I did all of that until I was 8 months pregnant. And it was a real rally because I had no energy left. My heart rate was high all the time.
And then somewhere in my pregnancy, I developed a cough that wouldn’t quit. All the doctors were like, don’t worry, the cough will go away. They had the same attitude regarding my heart rate. When you deliver the babies, your heart rate’s going to go down. Everything was just a consequence of my pregnancy. So then I delivered the babies… and the cough didn’t go away.
So that was that led me to my diagnosis, because then I ended up in the emergency room with the cough. So the only real symptom that I know that I had was the cough.
And one more word regarding the breathing episode I had 11 months prior. Had we done any further diagnostics and looked into it, we might actually have caught my cancer early. But I don’t ever think about that—sure, I might have caught my cancer at an earlier stage, but then I would have been in cancer treatment and I wouldn’t have gotten pregnant. So this mind game is completely null to me.
When I look back at all that, it was really a miracle that I was able to get out of bed every day.
But… I needed to keep rising to the occasion.
And I did.

Diagnosis
Stage 4 lung cancer
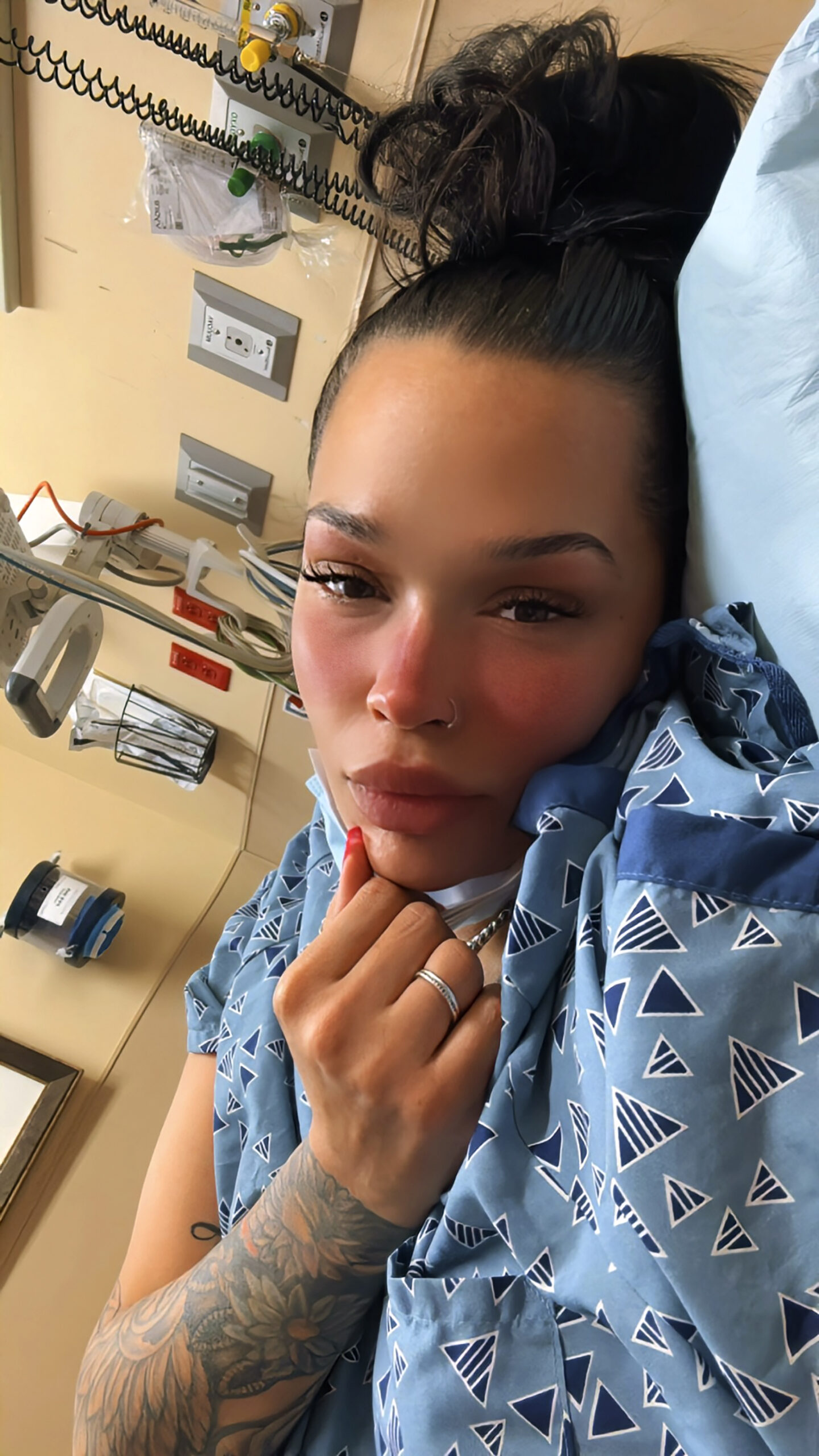
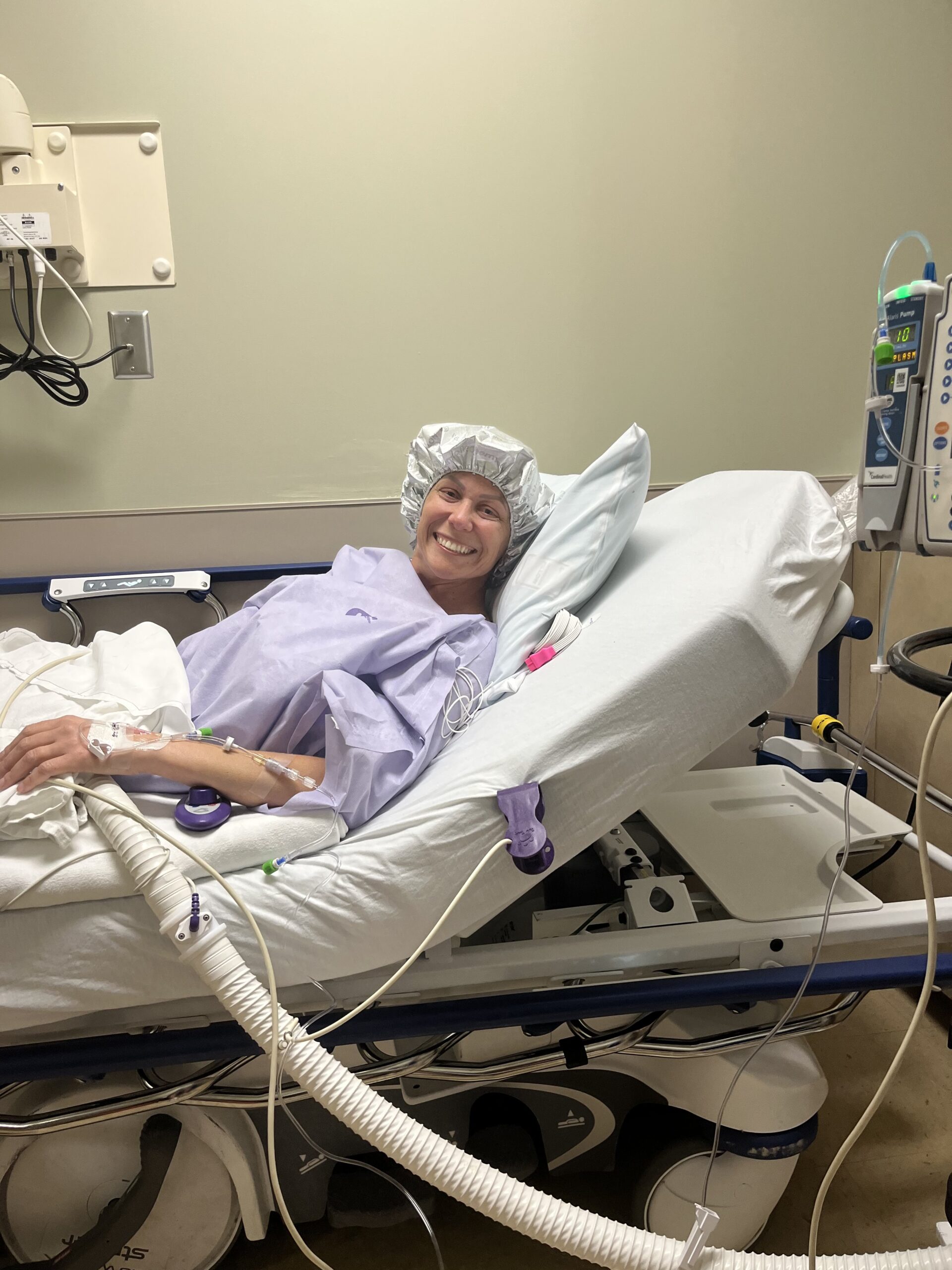
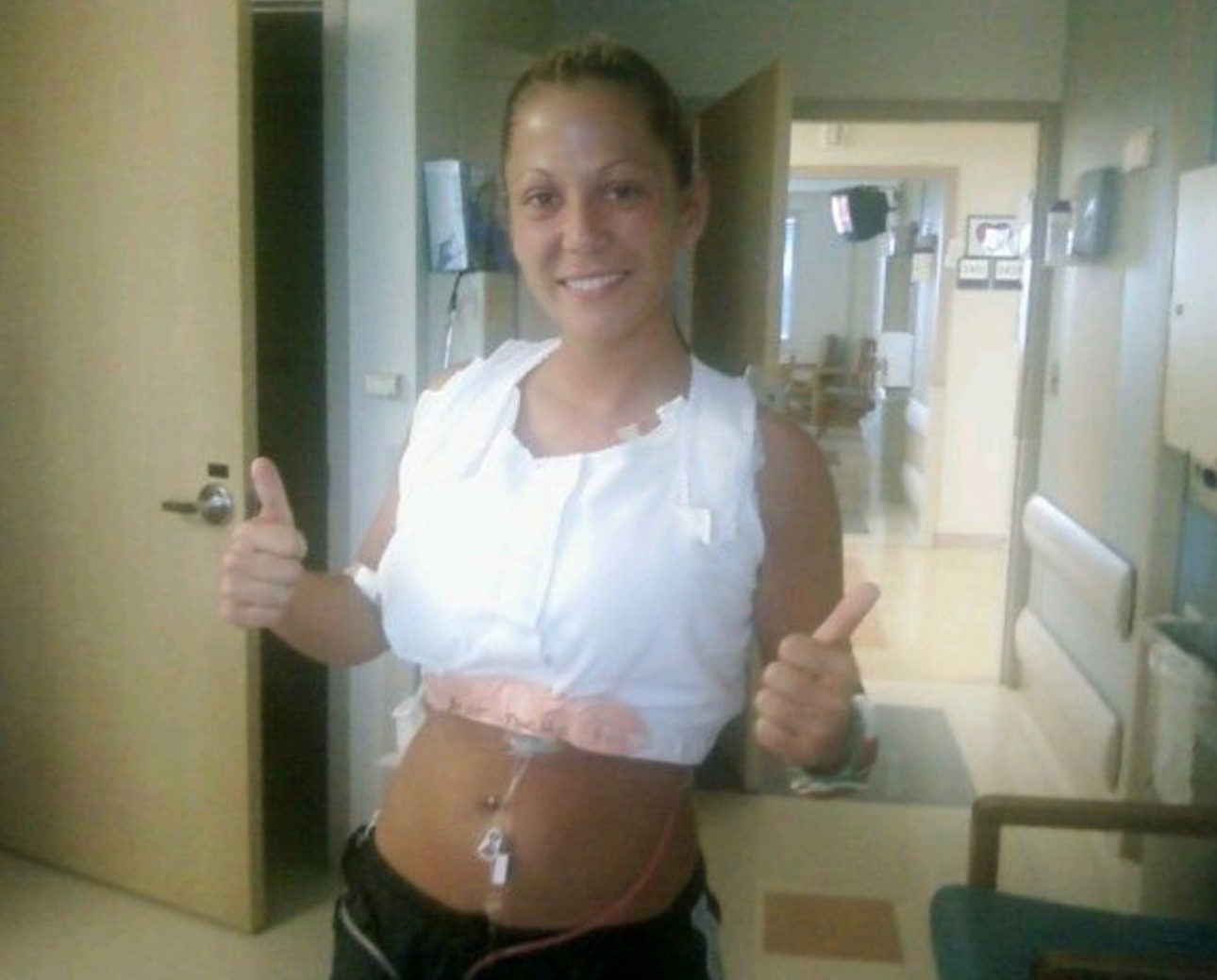
10 days after I delivered the twins, I was diagnosed with lung cancer.
I had given birth on the previous Monday and had been released on Wednesday. I had been rushed back to the ER on Saturday because of my cough. And it was super hard because I was also struggling with breastfeeding, as a first-time mom.
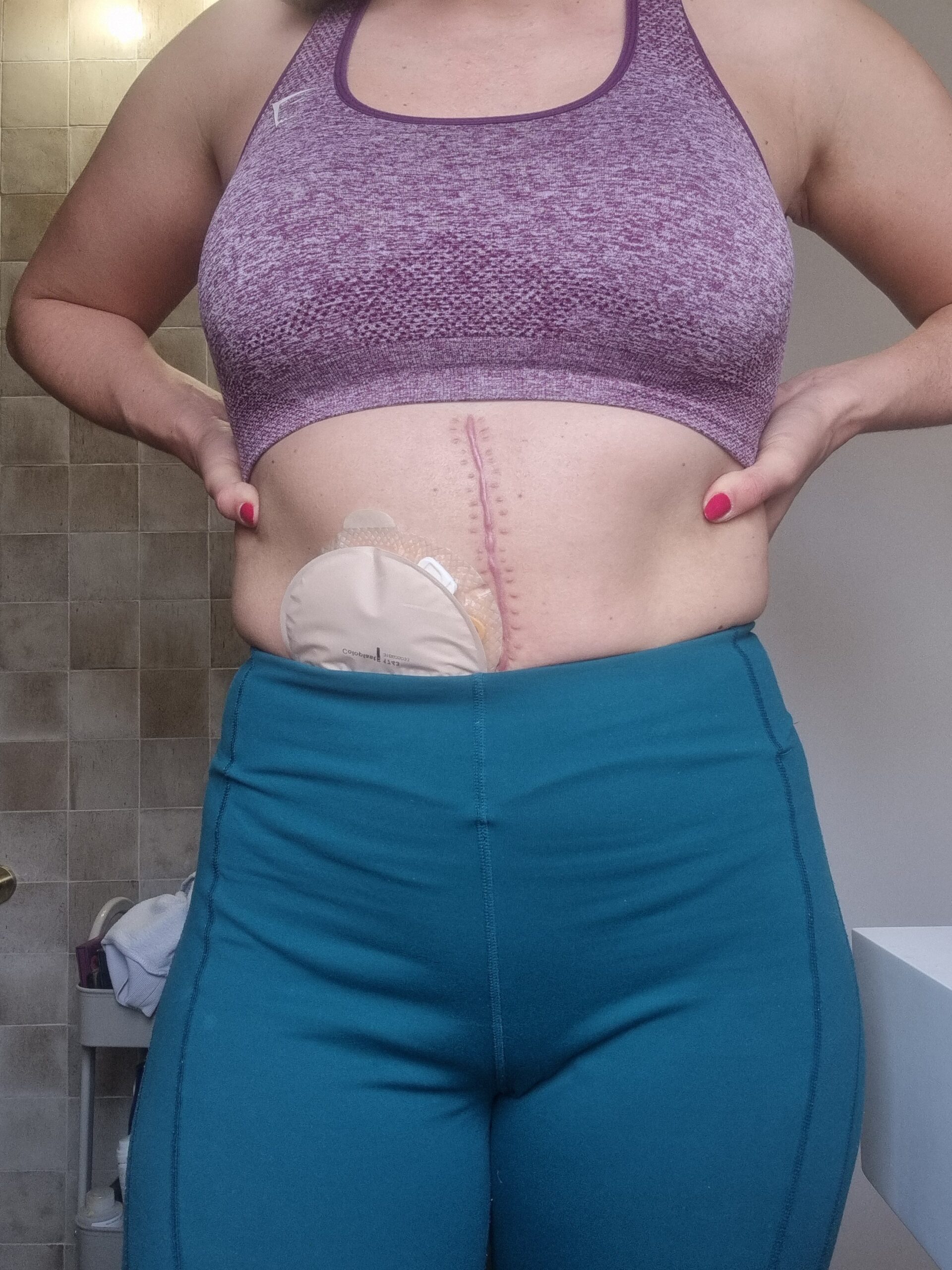
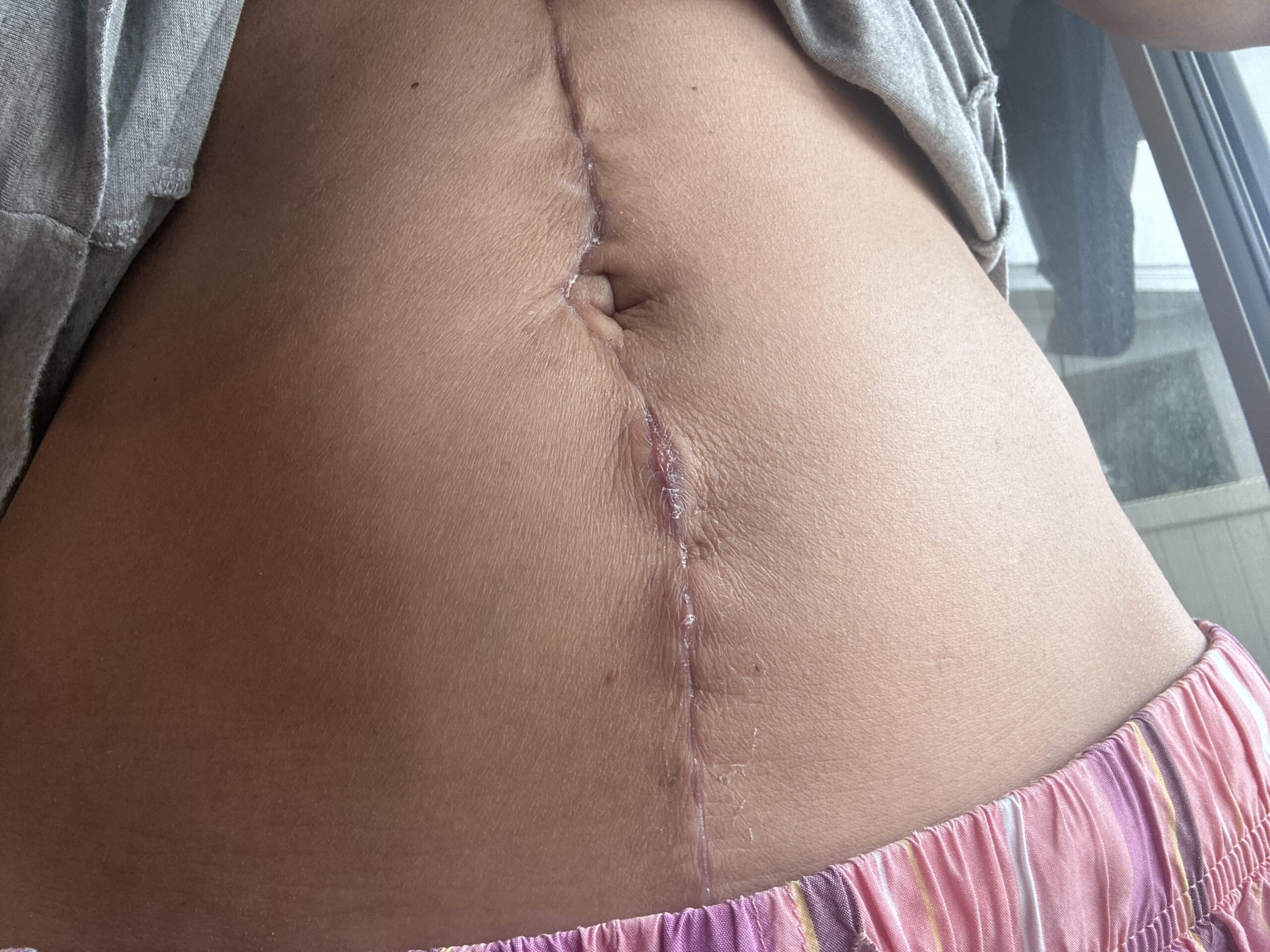
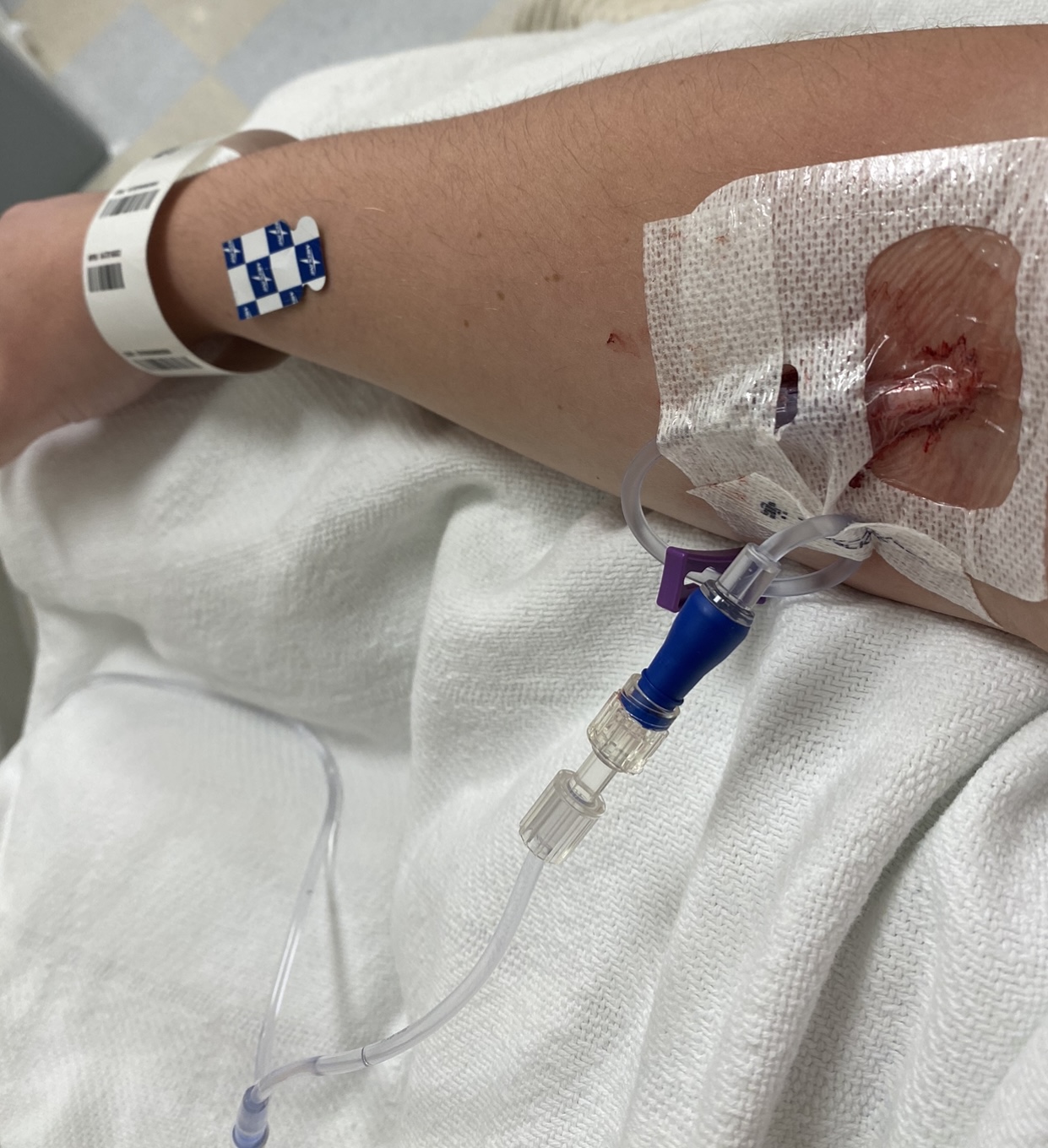
So in the ER, they did a chest x ray, and they found a pleural effusion. They also brought in an OB to look at my C-section incision because I felt like it was bleeding. And I had a hematoma to boot.
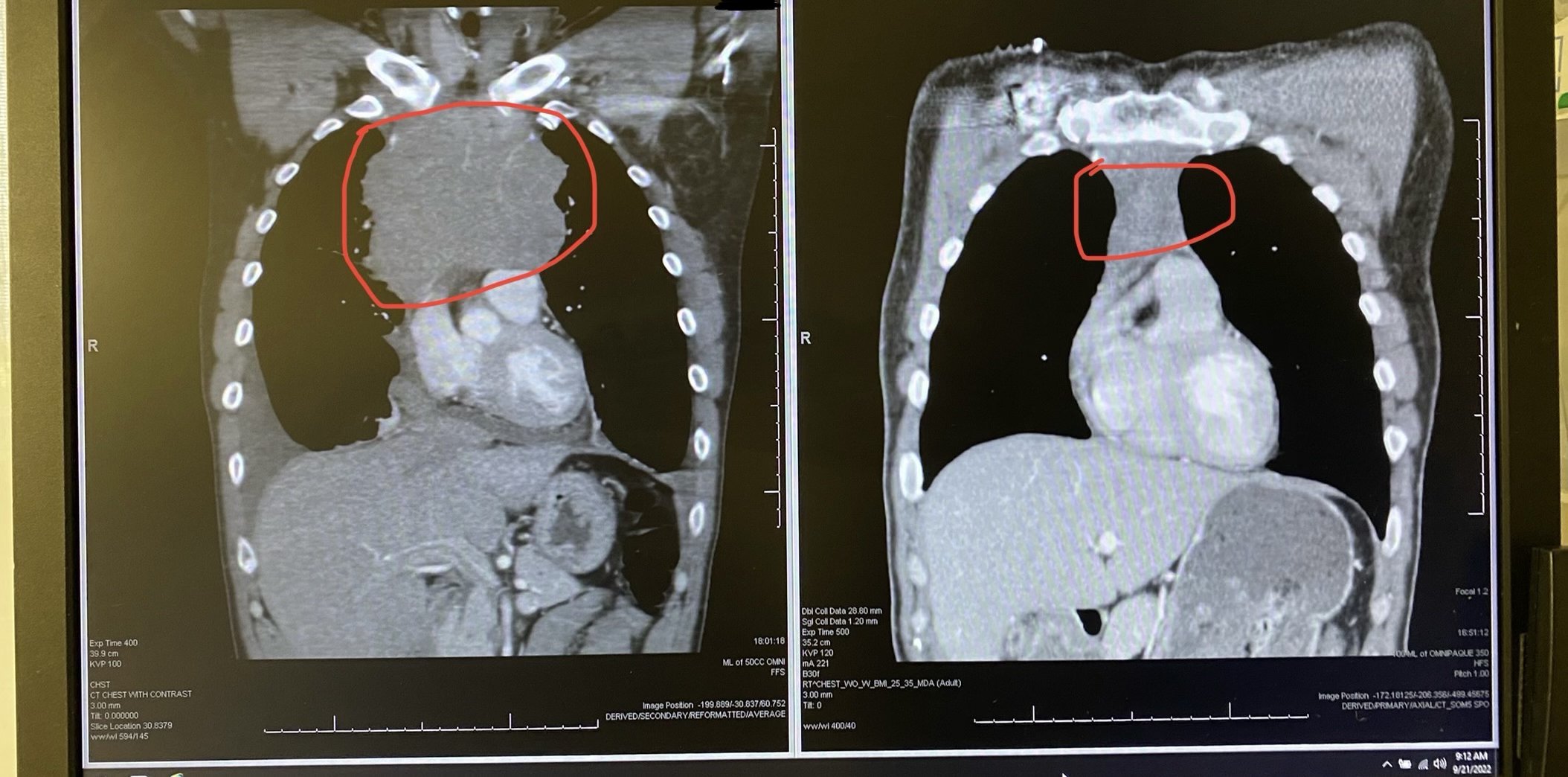
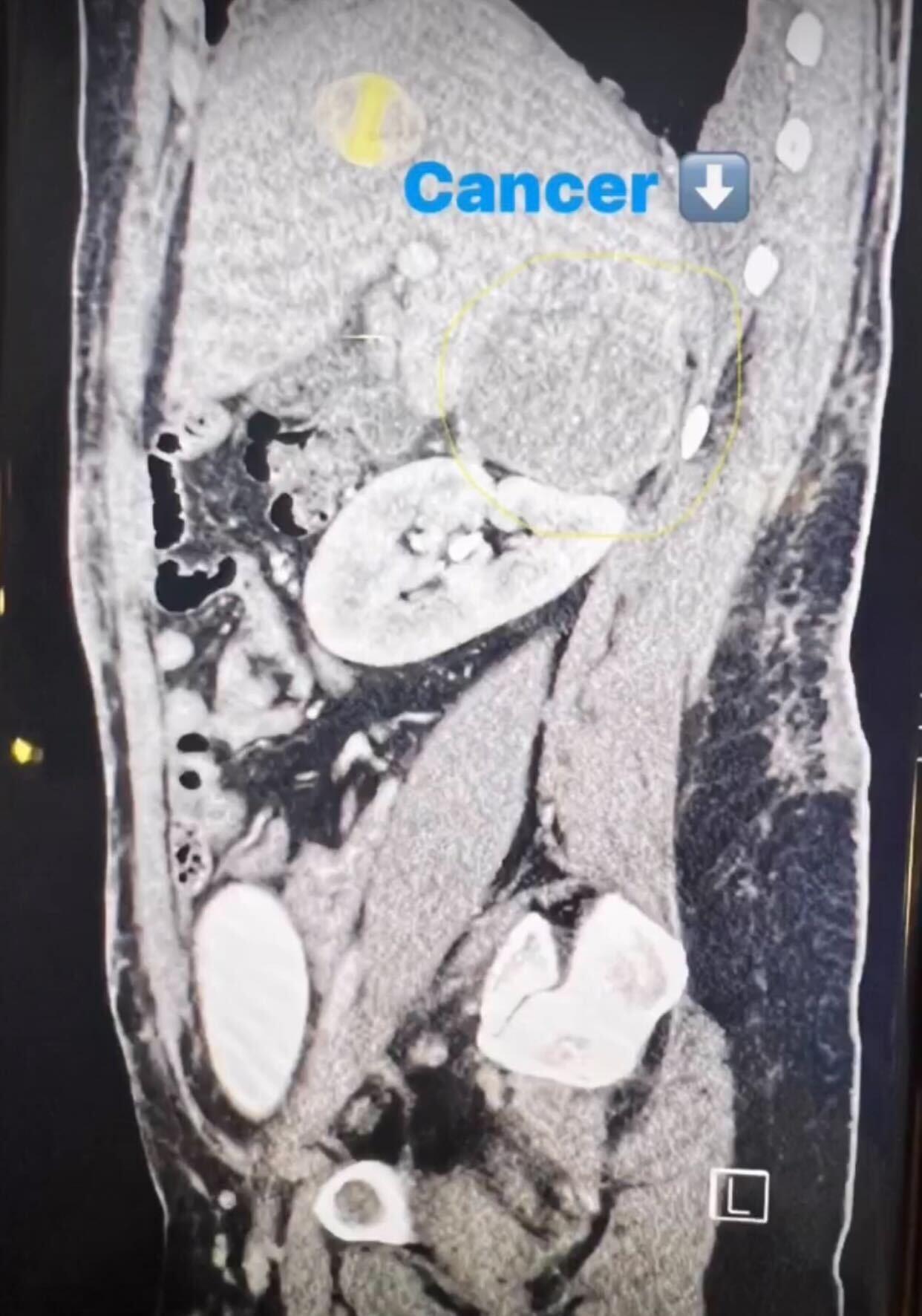
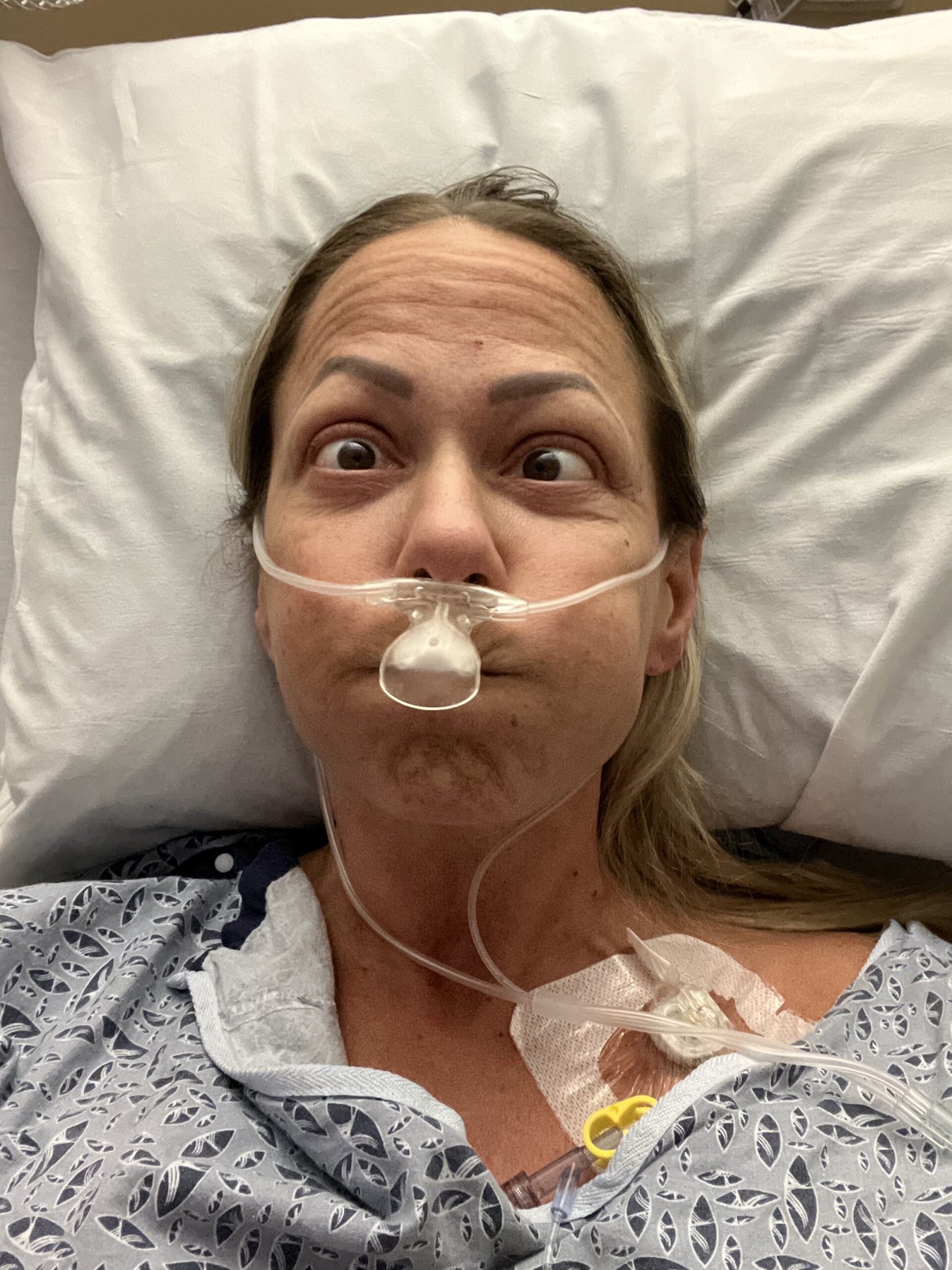
So the pulmonologist comes in and goes, that heaviness that you’re feeling on your chest is because of fluid in your lung. I then got a lung tap and they drained a liter of fluid out of my lungs. And the pulmonologist could see the coloring in it. We don’t know what this is, he said, but we’ll send it to pathology. And he sent me in for a CT.
The next 5 days, from October 22nd to October 27th, were the hardest days of my life.
On Wednesday, the doctor calls me and says, we’re starting to get the pathology back. There are some cells of concern. That was his exact words. And I’m like, is it possible that this is going to be cancer? And he said, yes. And I said to myself, there’s no way this can be cancer.
And then the next day, he called and said, OK, it is cancer. You’ve got lung cancer. And I said, I’m going to be diagnosed stage 4, aren’t I? And he said, yes. You know, the fluid is already considered a metastasis.
Reaction to the diagnosis
The whole situation was just too tragic. People around me were crying constantly.
That diagnosis just seemed impossible. There’s just no way. I’m a runner. I worked out until I was 8 months pregnant with twins. I was 36 at the time of diagnosis. And I’ve had an amazing life to date—and now cancer hits.
What am I going to do?
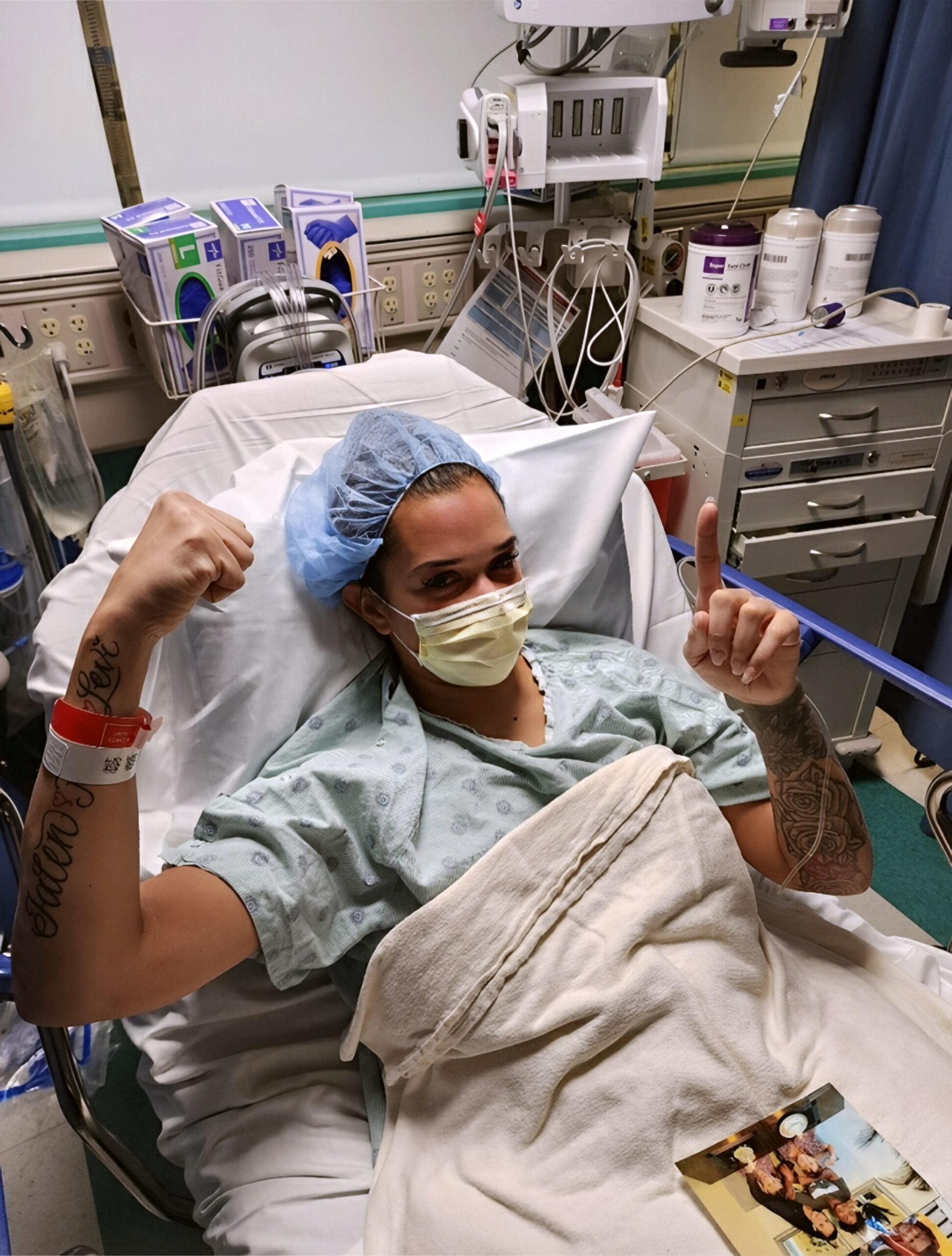
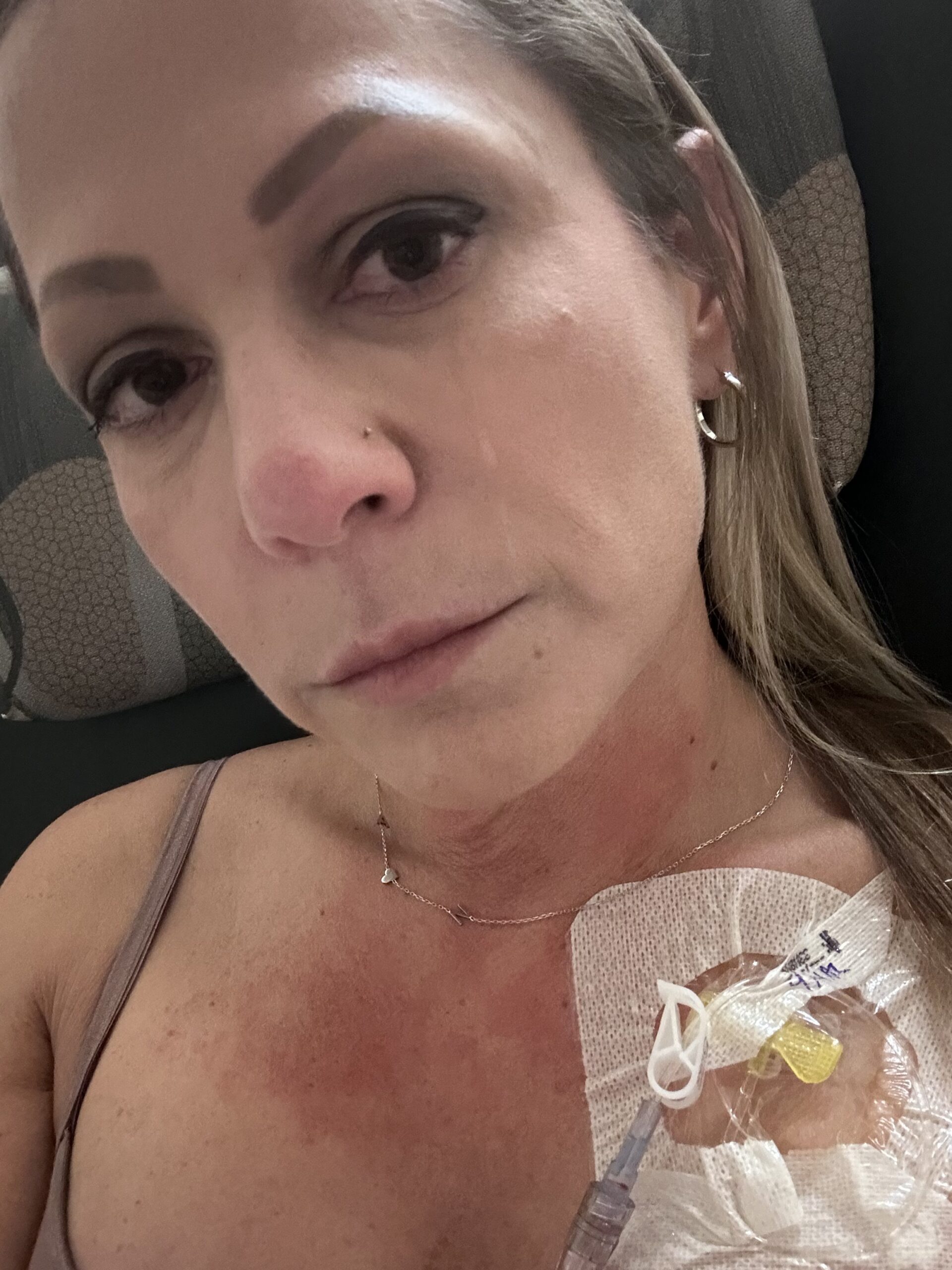
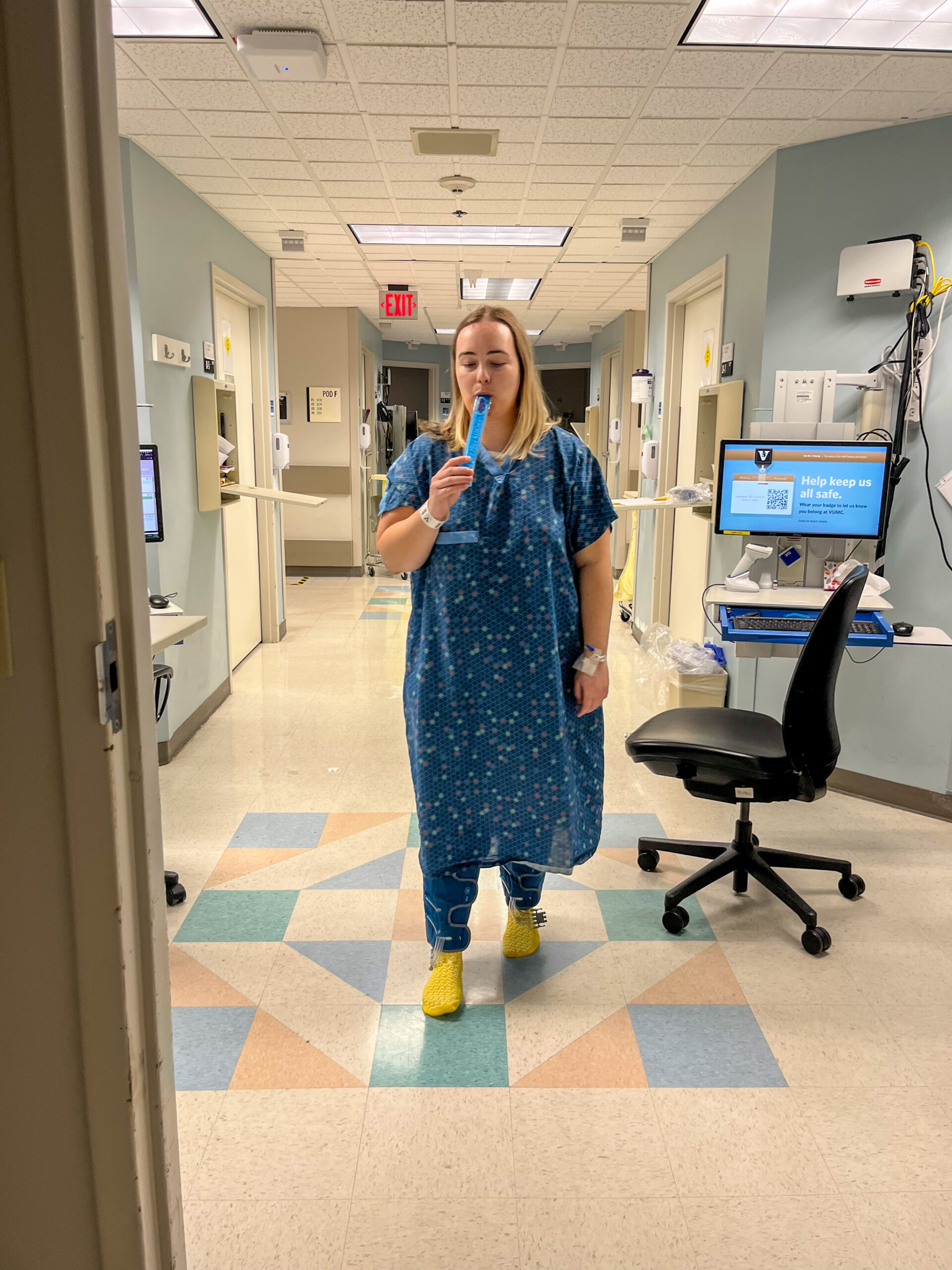
On Saturday, I went in for my Pet scan. I was asked, are you breastfeeding? If so, you need to pump and dump today because you’re radioactive. As a matter of fact, you can’t be around your kids for 24 hours after the scan. So the rest of the day, my mother in law and my husband had to take care of the kids. It was so awful to be apart from them. I spent the whole day crying.
The whole thing was an ordeal. I wanted to go running again, I wanted to feel like me again.
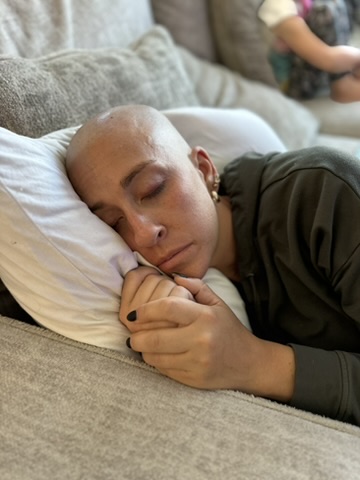
And then I just kept thinking, I’m going to have to go straight into cancer treatment. I’m going to be so sick. I’m going to die and I’m never going to be me again. And then I’m going to leave these babies that I just had.

My financial status at that time was also a concern. Given that I was coming off my past lifestyle, I didn’t have too much saved. And then all of a sudden I have a terminal illness and it’s like, am I going to be able to work? Like, what is this going to look like? So there was a lot of fear around all of that stuff.
When I look back at all that, it was really a miracle that I was able to get out of bed every day. But I had these babies that I had to take care of. I needed to keep rising to the occasion. And I did.
I tell my husband every day, you have no idea how lucky you are that I am so resilient, because I could have so easily had a full on, fully justifiable mental breakdown. I could have run away, abandoned him and the kids. Or be so crippled and depressed that I couldn’t get out of bed.
But I got up every day, reminded myself that I could handle whatever is thrown at me, and just kept moving forward. And it’s crazy. I’m amazed with myself for being able to do that.
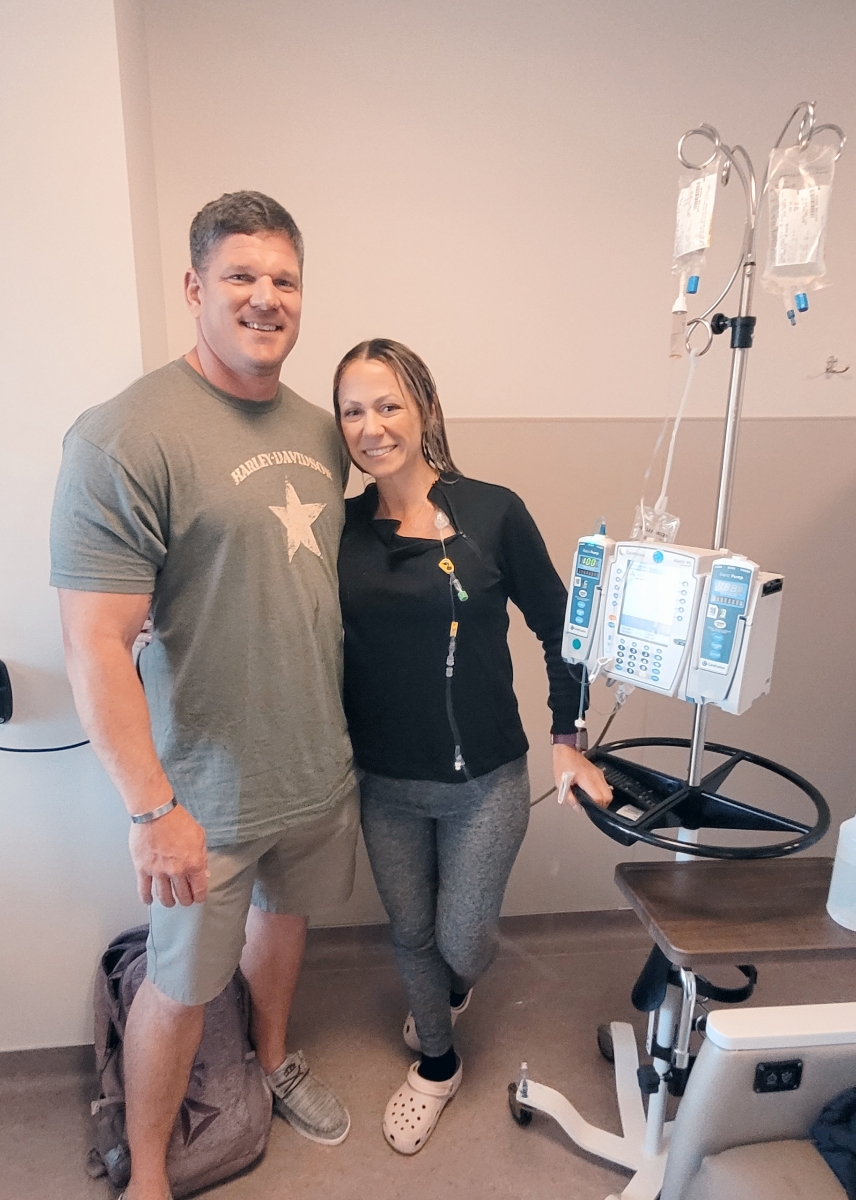
My husband’s a military man, so he does well in awful situations. And he just knows that he can handle whatever is thrown at him. He just has to assess it, and then he’ll keep figuring it out and moving forward.
Hopeful is the only way that I know how to be.
I’m a glass half full optimist all the time.
And I try to find a good balance between the hope of science and medicine and the reality of my situation.
Treatment
ALK+ mutation
Then on Saturday I went in for my Pet scan, and on Monday I went to the oncologist, and that point was where things turned around for me.
Prior to that, I didn’t have any resources. All I knew was that I had lung cancer. I knew nothing about how anything worked. I didn’t know how lung cancer was treated other than chemo, radiation, and surgery.
And I’m thankful for her because was the first person who had optimism, and she gave me some hope.
She said, I have a very strong feeling that you have a genetic mutation. I had no idea what that even meant. She explained, if you do have a mutation, we get to give you a different type of treatment. You’re going to get targeted treatment, and it’s going to go after your cancer’s specific driver.
And I was just so hopeful at that point that I was going to have a mutation.

The idea that I wouldn’t have to go through chemo just sounded so nice. And both this doctor and the pulmonologist from the emergency room were so optimistic that this was going to be the case for me.
She sent in my pleural effusion for biomarker testing. She said, we’re going to see what that says, and then that’s going to dictate our treatment plan.
And so my pulmonologist calls me and says, you know, there there was a hit on the biomarker testing. You’re ALK+.

Current status
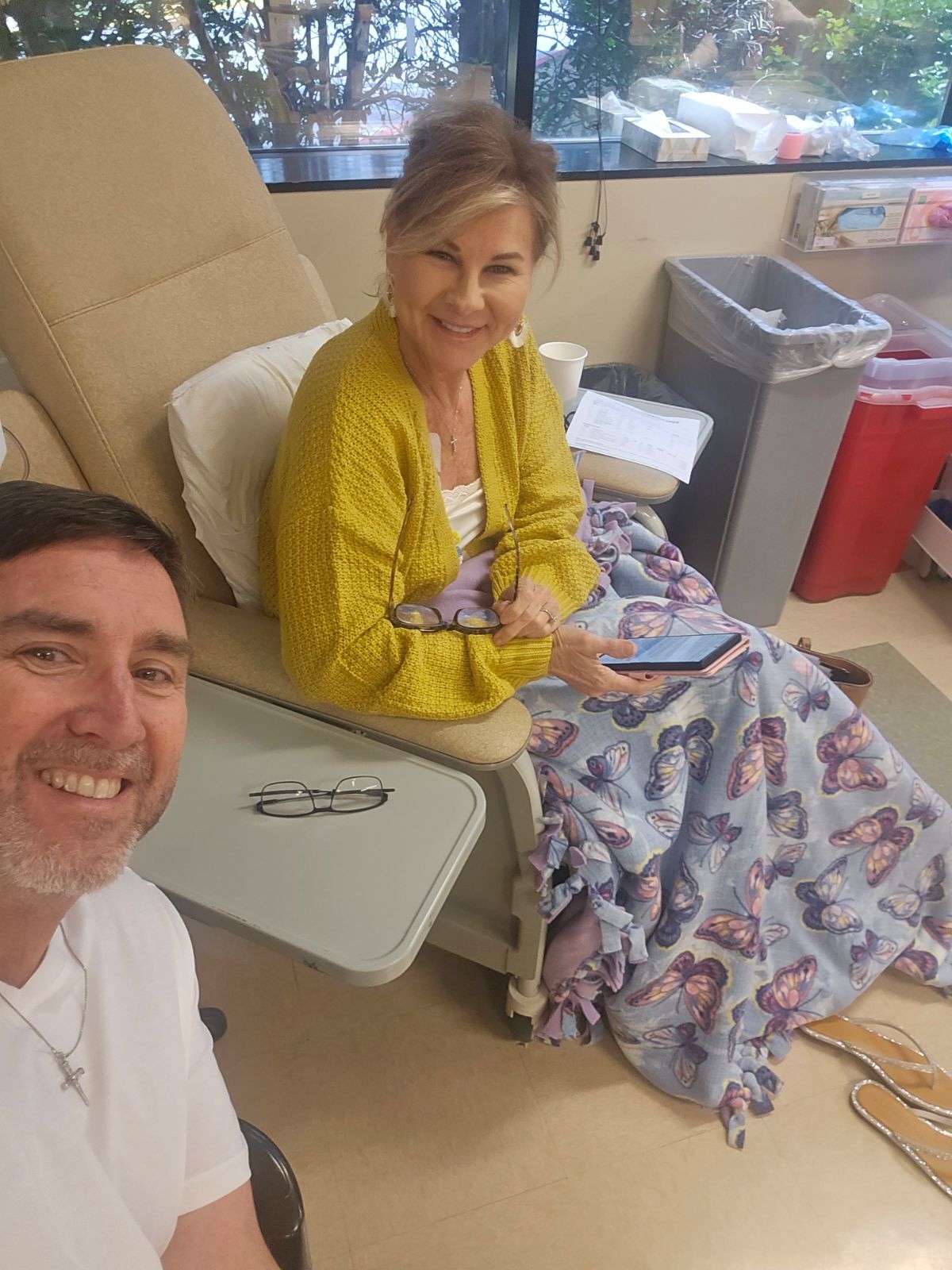
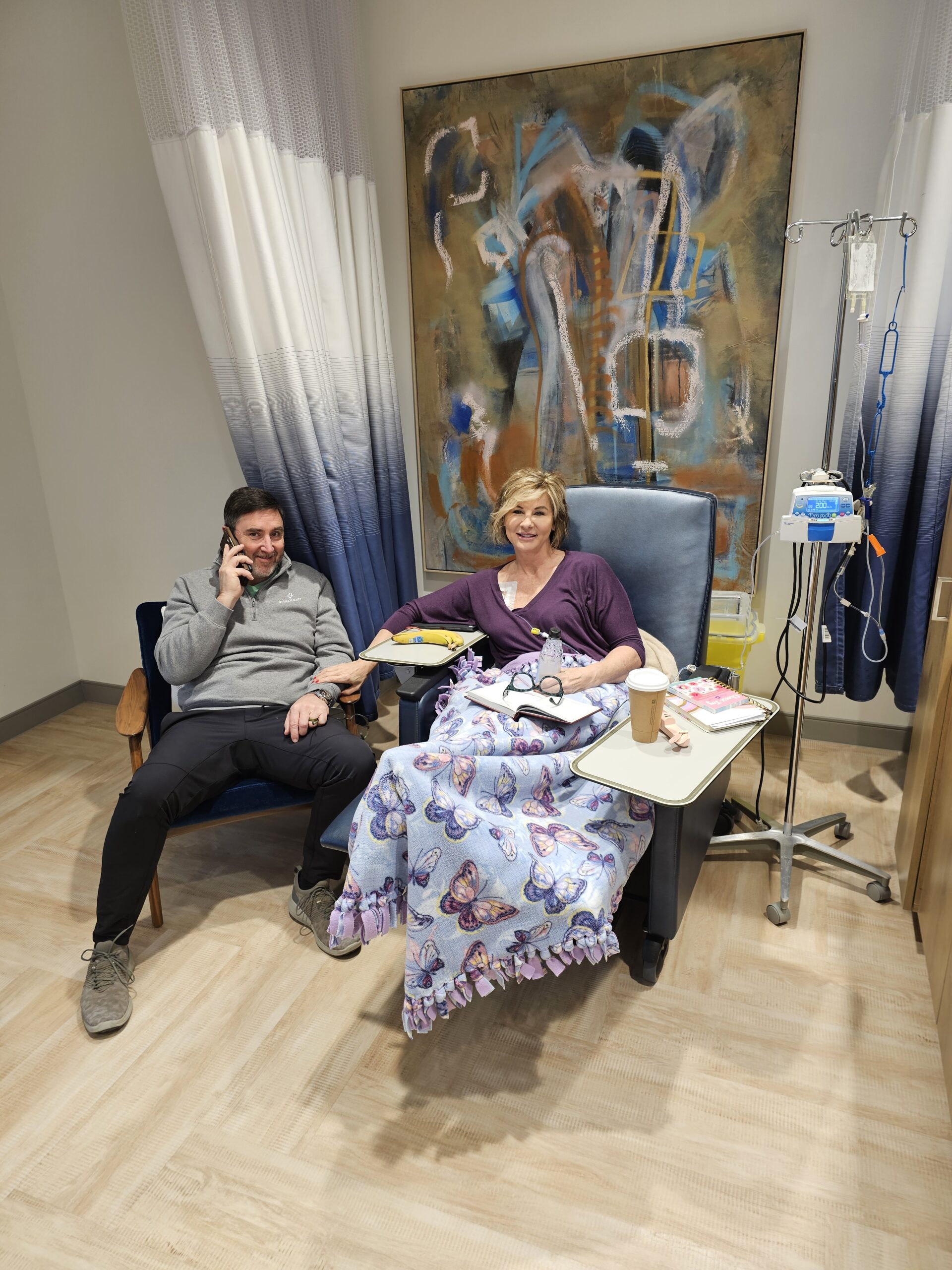
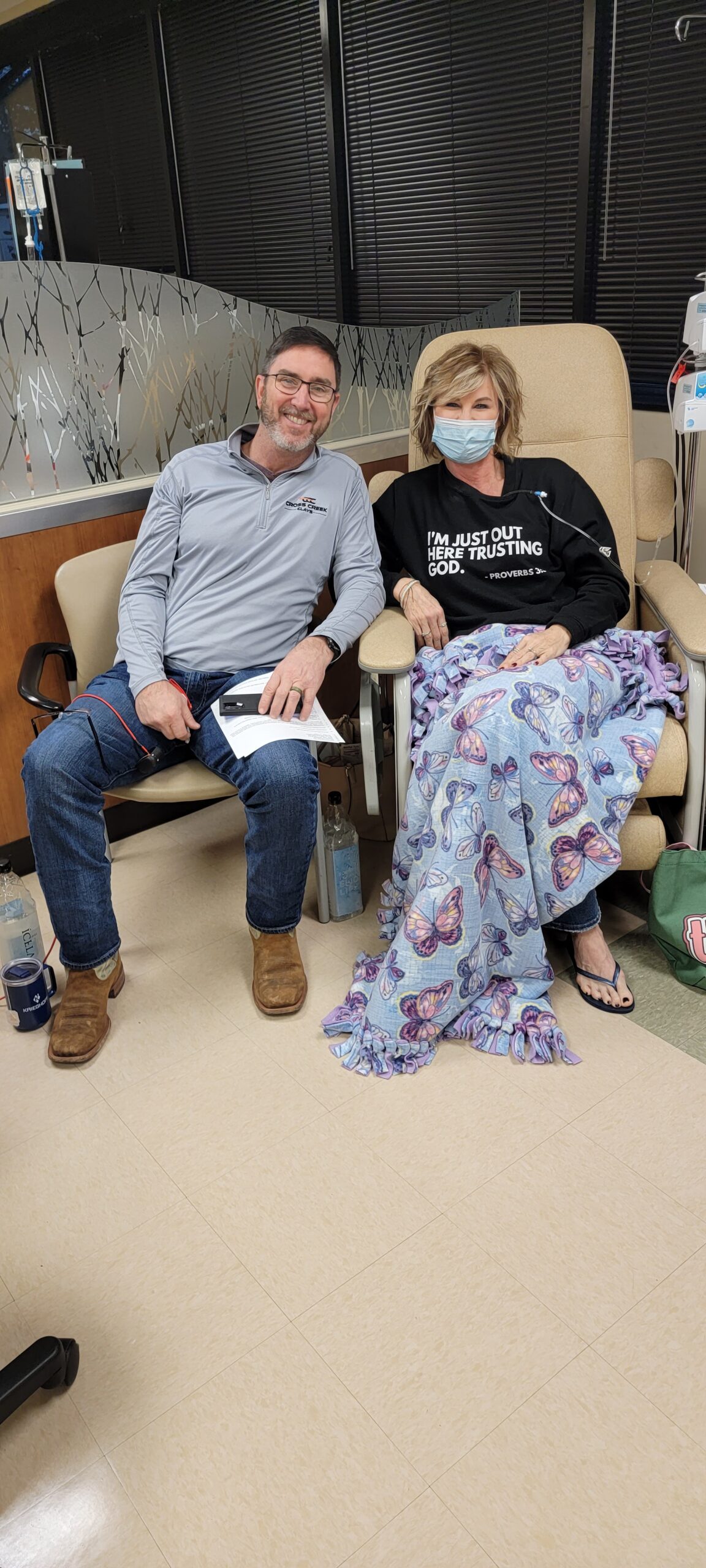
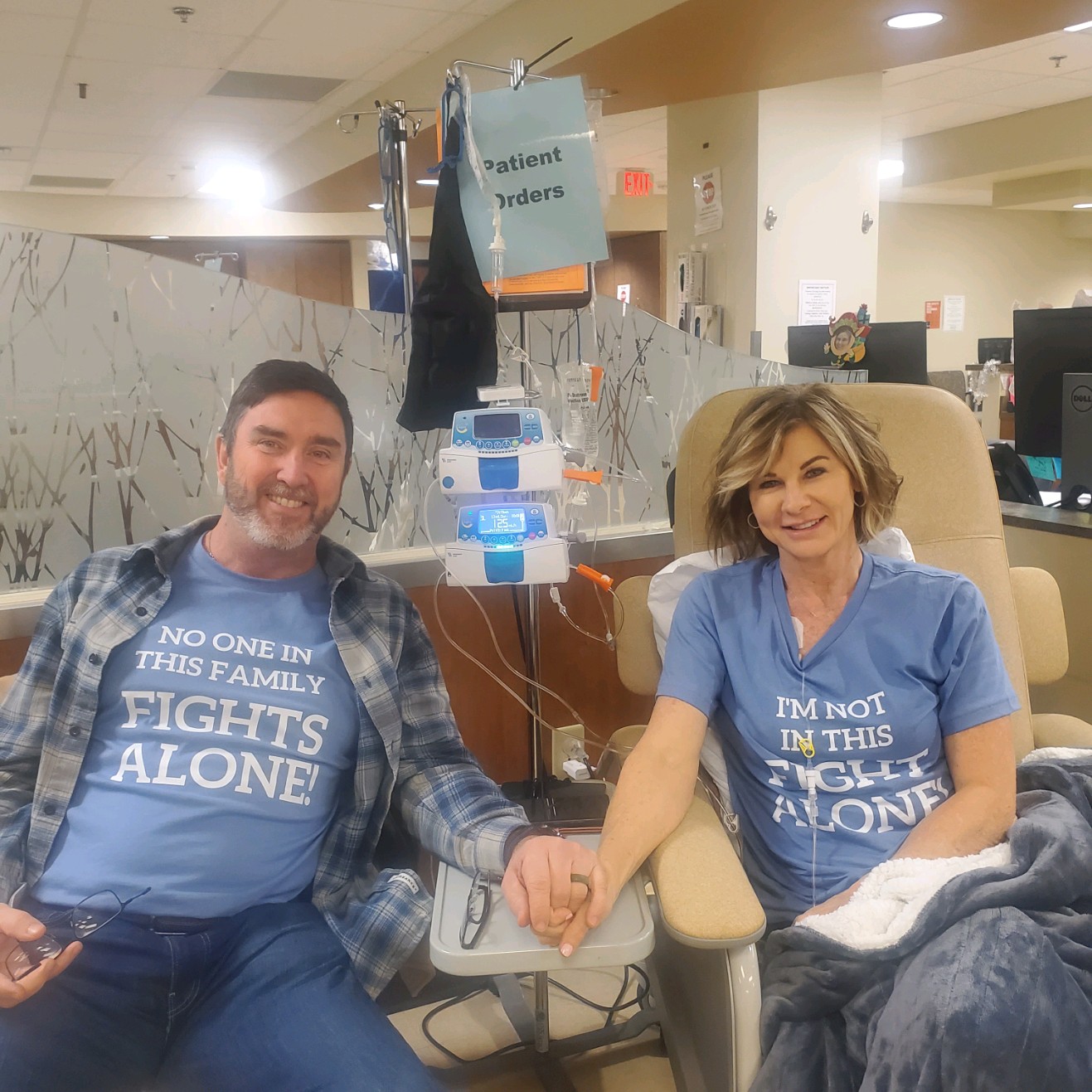
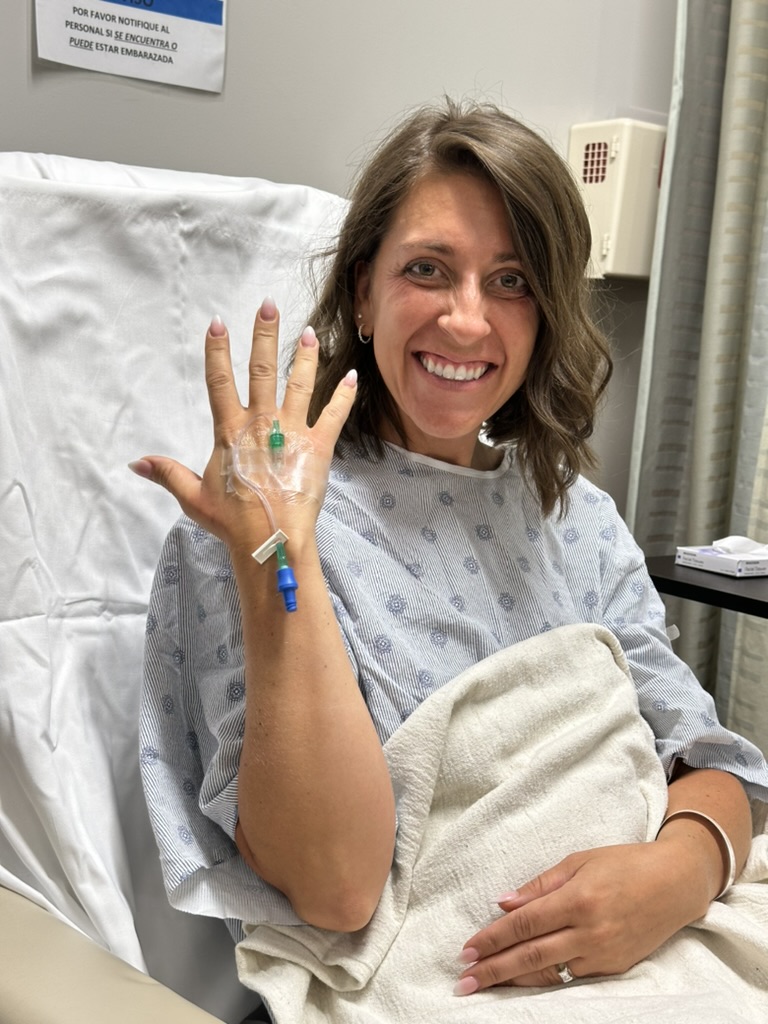
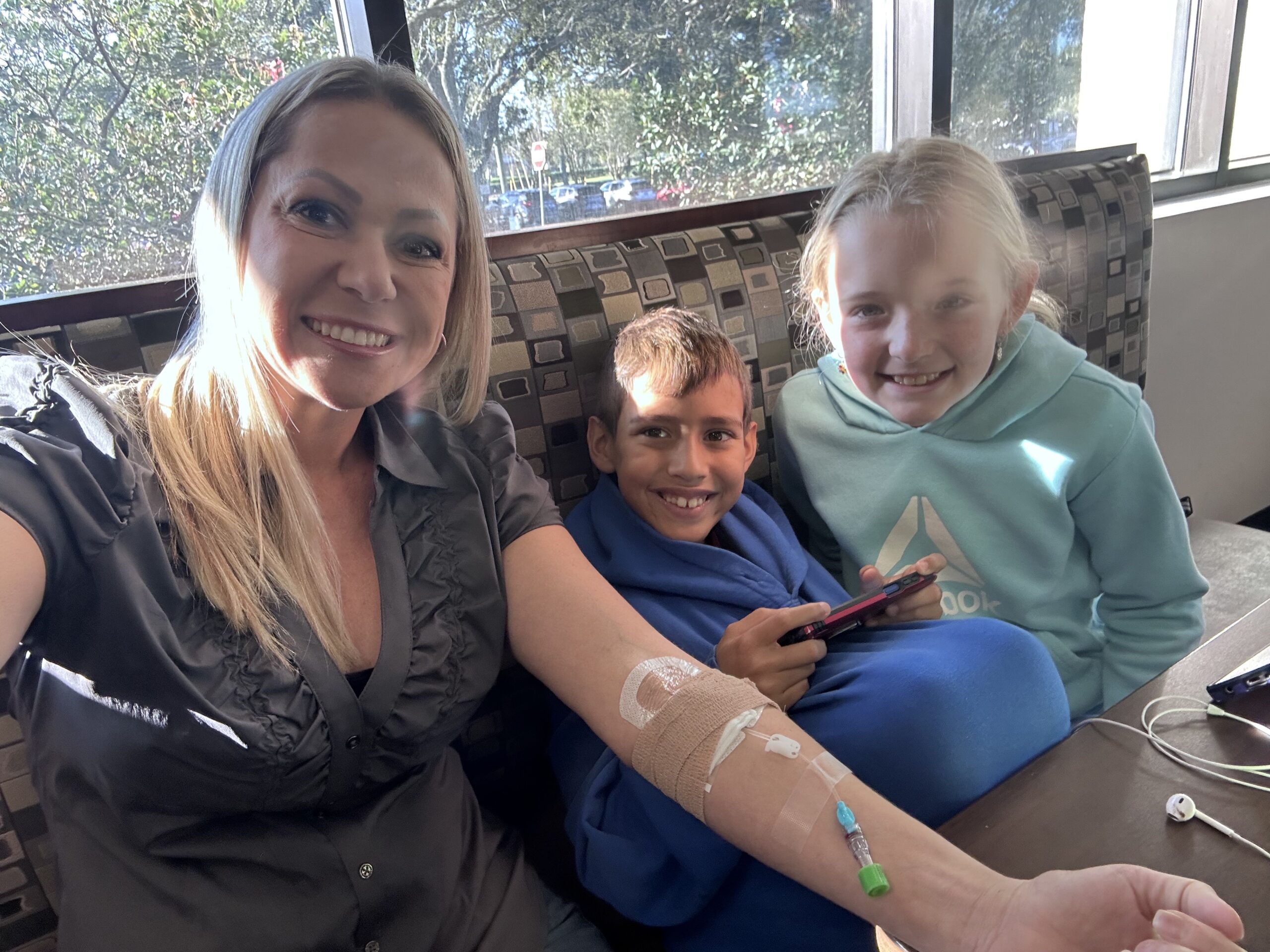
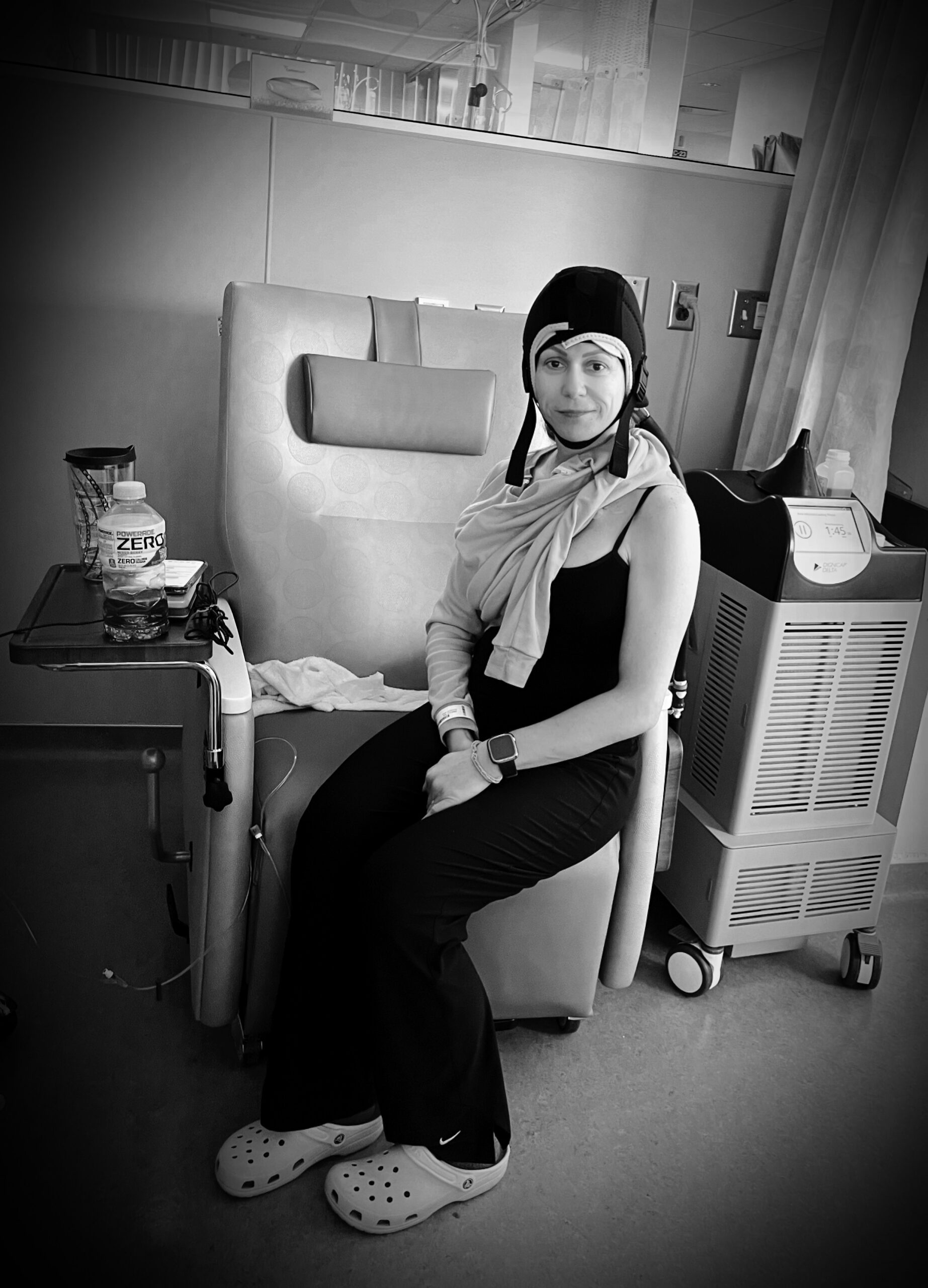
I have lived with stage 4 lung cancer for 2 years thanks to my treatments and the 8 pills I take a day. I live–everyone around me forgets that I have lung cancer.
Right now. I am doing scans quarterly. I was doing Pet scans, and I’m now ready to switch over to CT scans. My next one coming up is going to be the beginning of November.
The last Pet scan that I had was in July and it came back stable. There was a little spot in my lung that had been lighting up on two Pet scans prior to that, and the most recent Pet scan had showed that that had resolved itself.
I had one scan that came up as no evidence of disease. I have other ones that come up that say everything is fine and stable. There’s not really very much showing up right now.
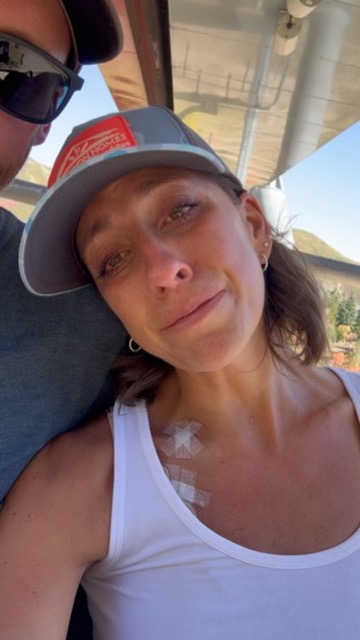
I do have permanent lung damage. My primary tumor was on my lower left lobe, and it hit a nerve. Sometimes I get tightness in there, so it feels like I can’t catch a full breath. One of my eyes is smaller than the other eye, and that drives me crazy. But like for the most part, other people don’t really care.
I haven’t started getting nervous about my next scan yet. Mostly because October is just way too busy for me to have time. We have the twins’ birthday, we have the holiday of Sukkot, and then next week I’m going to Boston to talk in front of a biotech company that’s working on clinical trials for a TKI for ALK positive patients.
So that’s just the next two weeks. So I don’t have time to be anxious.
Finding a Community
I was searching for resources about lung cancer for young people, and I somehow ended up on an Instagram page focusing on being ALK+, and I didn’t even know that that was a thing.
I ended up befriending the person who holds the account, Summer. I remember calling her and telling her about my ALK+ diagnosis.
It was awesome to find a resource like that and make a friend like her. To link up with fellow lung cancer patients who are also young, who can hear what I have to say, and who also know how this feels.
It was so nice to have someone that understood me and was able to help during that time.
So and now Summer and I are both on the board of directors for ALK Positive, the nonprofit.

Bolstering hope

My ALK+ diagnosis and also being able to link up with Summer strengthened my capacity to hope.
Hopeful is the only way that I know how to be. I’m a glass half full optimist all the time. And I try to find a good balance between the hope of science and medicine and the reality of my situation.
Because the last thing that I want is to be caught off guard. And then I’ve known people who have died from cancer and weren’t in acceptance of it. And because of that, they didn’t get to say goodbye to people.
I’ve also seen those who accept it and who get a real, genuine opportunity to say goodbye and so nothing is left unsaid. And so for me, I need to find the balance between the two.
Science is helping me hope, and hope strongly. I mean, just look at where I am today.
No one treats me like any differently until you tell them what’s up. I don’t look any different than anyone else, I haven’t lost my hair, I’m not on oxygen, I’m not in a wheelchair. I work out every day, I chase after my children at the park. I mean, Hey, I’m training for a 10K right now.
And that’s where science is today. And if the medicines can help me live 10 years more, there’s even more hope, because by then we’ll be even more advanced than where we are right now. So there is real hope.
But, of course, it’s a balancing act because it’s stage 4 lung cancer and today there’s no cure yet for it.
On Being a Young Mom with Cancer
There’s a lot of grace and a lot of acceptance in how I’ve learned to bear all of this.
I learned everything all at the exact same time. How to be a mom, a wife, a stepmom—who is living with a terminal illness. At the same time, I was learning how to be an advocate for that illness.
This is my story, these are the cards I was dealt. I see friends of mine who have babies and come home from the hospital and get to spend 4 months snuggling with their babies. That’s just not my story. And I just have to be okay with that.
It’s sad that I didn’t get to just be a mom, a first time mom and do only that. I think that I make up for it now.

My babies are turning 2 tomorrow. It’s so crazy. But they’re so much fun right now.
And as for my relationship with my husband, we’ve been in therapy for 2 years now, and we know each other and we’re in a good place. And I feel like we really understand each other. And it feels like we’re a family. And you know, we have been able to work our way through everything that I had been scared of 2 years ago.
So I’m not sad about what it is that I didn’t get to have. I’m just so grateful for what I do have now and the life that I have today. I think that’s the best way of saying it.
All the stress that I had 2 years ago, I think that it’s finally evening out.
I’m not sad about what it is that I didn’t get to have.
I’m just so grateful for what I do have now and the life that I have today.

What Amanda Wants to Share
“Your only prerequisite for having lung cancer is having lungs.”
What do I want people to know about lung cancer?
The first thing is that your only prerequisite for getting lung cancer is having lungs. You don’t need to smoke. It doesn’t matter how active you are, how healthy you are, if you have lungs, you can get lung cancer. The number of people that I know who have lung cancer despite never having smoked is astronomical.
I did smoke, but I hadn’t in years before I got diagnosed—I smoked on and off for ten years in my early in my 20s, and I had quit before I was 30. I was a runner. I was doing half marathons.
I was also pushed outside of the lung cancer screening guidelines because of my age and because of my overall general health.
I wasn’t someone that anyone could think would have lung cancer.
And the second thing is how incredible science is in the lung cancer sphere right now. The amount of research going on in lung cancer is amazing and hopeful and incredible.
Don’t obsess over what might have been
Some advice for those who get stuck in all the what-ifs and might-have-beens.
I think that a lot of what I went through in the first year is just allowing time to pass and just allowing yourself to grieve the life that you thought you were going to have while you while you simultaneously learn to accept the life that you are actually living and you accept the things that you can, that you can’t change, and you change the things that you can.

And the attitude counts, too. A lot of it is just acceptance, acceptance and grace. And then of course giving yourself some time to be sad is okay, but you need to pull yourself up. There’s just no point not to. You only get one life to live.
If you want to spend a day in bed being sad, go spend a day in bed and do it. But remember that you need to get up. You need to go have some ice cream. Go for a walk outside and find some happiness somewhere.

Check on the people around you
Regarding the people around you, make sure that they’re OK too.
I’m an only child, and my mom has said to me in the last 2 years, what do you do when you think that there’s a possibility that you’re going to outlive your only child?
So I give everyone space for themselves to be able to do whatever it is that they need to do.
My parents were able to be around me without crying, but I knew that they were putting on a brave face. And I hated people putting on brave faces around me because I don’t like it when people aren’t genuine.
I think at the beginning it was just like, how do you look at this situation? It was a tragedy. And the idea that I was going to go straight into this awful treatment and it was going to kill me, and then I was going to die and never get to enjoy life again, was just awful.
So I think it took everyone in my life a little while to be able to look at the situation and say, she’s okay right now. If Amanda can get up and put a smile on her face, I can do that too.
And my friends started just treating me like I was their friend again, not their friend that has cancer. And my parents started treating me as their daughter again, not their daughter with cancer.
Find your community
Also, find the people that are going through exactly what it is that you’re going through. These are the people that can meet you exactly where you are and know exactly what it feels like.
When people say, you have a hard time making friends in adulthood, I think that that’s not true. You just have to find the people you can relate to.
And so I don’t need my friends to know how it is that I feel, because I have my support of the people that know exactly how I feel. And there is nothing better than getting to go out to lunch with one of them, or a few of them, and having people know exactly what this feels like from your exact perspective.


Deal with scanxiety
Lastly, on scanxiety.
The biggest thing that I’ve learned about dealing with scanxiety is: allow yourself to be scared. Allow yourself to just go through it. And at the end of the day, whether it’s good news or bad news, just deal with it and figure out what you need to do next.
I get scanxiety every single scan, and the flip side of it is like when a scan comes back good. Oh my God, it’s like the best day. It’s like, let’s eat ice cream sundaes!

Special thanks again to Johnson & Johnson for supporting our patient education program. The Patient Story retains full editorial control over all content.

Inspired by Amanda's story?
Share your story, too!
More Stories with The White Ribbon Project
No post found
More Lung Cancer Stories
No post found