HER2+, HR-, Inflammatory Breast Cancer in Her 20s: Rebecca on Symptoms, Diagnosis, and Finding Community
HER2-positive inflammatory breast cancer in young adults is often aggressive, fast-moving, and too frequently dismissed by healthcare systems that are not built for younger patients or Indigenous communities. In her late 20s, Rebecca, a First Nations woman originally from Wrigley in the Northwest Territories, noticed a sharp pinch in her armpit while working long hours at a paralegal desk job. She found a cluster of swollen lymph nodes and repeatedly sought help at walk-in clinics in Alberta, only to be brushed off as too young for anything serious.
Interviewed by: Tory Midkiff
Edited by: Chris Sanchez
Months later, after finally convincing a physician to feel the nodes the way she described, a biopsy on January 15, 2020, revealed breast cancer. The doctor told her she might live only three to four years. Stunned and feeling like a shell of a human, Rebecca learned that her disease was HER2-positive (HER2+), hormone receptor-negative (HR-), and inflammatory, with extensive lymph node involvement up to her collarbone, classified as stage 3.

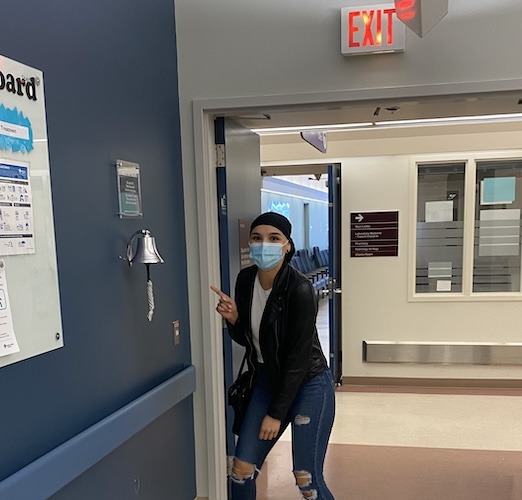
Rebecca then began intensive chemotherapy just two days before Canada’s COVID lockdown, which meant sitting alone through three- to four-hour infusions, managing severe side effects, and living far from her immediate family. The treatment stripped her hair and sense of control; as an Indigenous woman whose hair is deeply spiritual, Rebecca chose to cut and then shave it herself as an act of reclaiming power.
Isolation pushed Rebecca online. Sharing her experience on social media connected her with a network of young people across Canada with similar diagnoses and treatment plans, many also facing aggressive HER2-positive disease in their 20s and 30s. That peer support reshaped how she saw her experience and reminded her she was not alone.
Today, as she approaches six years in remission, Rebecca still lives with scanxiety, yearly scares, and the trauma of nearly being turned away from life-saving care. She channels that experience into her social work, first on the front lines supporting Indigenous patients in hospitals, and now in program and system-level work aimed at dismantling harmful structures. Rebecca is pursuing a master’s degree in community development, determined to change policies so that Indigenous patients and young adults with HER2-positive inflammatory breast cancer are believed, supported, and able to access the care they deserve.
Watch Rebecca’s video or read the edited transcript of her interview to take a deeper dive into her story:
- Self-advocacy can be life-saving, especially when early symptoms such as swollen lymph nodes are dismissed in young adults. Rebecca kept returning to clinics until a doctor finally listened.
- HER2-positive inflammatory breast cancer can present in the lymph nodes without a clear breast lump and may be diagnosed at an advanced stage in younger women.
- Isolation during chemotherapy and the COVID pandemic increased Rebecca’s emotional load, but connecting with peer communities like Rethink Breast Cancer transformed her experience and reduced her sense of aloneness.
- A universal truth for patients: It is valid to feel everything, like grief, anger, fear, and hope, and avoiding those feelings during treatment can make the emotional work of remission even harder.
- Rebecca’s transformation, from feeling like a shell of a human to training as a community development leader focused on Indigenous health equity, shows how lived experience can fuel powerful system change.
- Name: Rebecca W.
- Age at Diagnosis:
- 20s
- Diagnosis:
- Inflammatory Breast Cancer
- Staging:
- Stage 3C
- Biomarkers:
- HER2+
- HR-
- Symptom:
- Appearance of a lump in the right armpit
- Treatments:
- Chemotherapy
- Surgeries: mastectomy, lymphadenectomy
- Radiation therapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Introduction and background before diagnosis
- First breast cancer symptoms: swollen lymph nodes in my armpit
- Being dismissed by doctors and pushing for answers
- How medical gaslighting impacts Indigenous patients
- Starting cancer care after diagnosis
- Undergoing scans and feeling alone at the cancer center
- Meeting the surgeon who changed my mindset
- Surgical decisions and wishing I’d had a double mastectomy
- Starting chemotherapy at the beginning of the COVID lockdown
- Chemo alone, isolation, and dangerous side effects
- Finding the young breast cancer community through social media
- Cutting and shaving my hair: Indigenous identity and chemo hair loss
- Shaving my head to take back some control
- Reaching six years in remission and wanting to confront that first doctor
- Life after treatment: anxiety, trauma, and the challenges of remission
- How cancer and lived experience shaped my career path
- From frontline social work to system change and policy
- Processing cancer trauma and the need to grieve
Introduction and background before diagnosis
My name is Rebecca. I’m First Nations, mixed, and originally from the First Nations community commonly known as Wrigley, Northwest Territories. It’s up in Treaty 11 territory in Canada.
Before my diagnosis, I was in my late 20s and finishing up my social work schooling when that happened. I was in an interesting position in my life. I was transitioning out of the frontline social work field. At that time, in the province that I was living in, there was a political climate change, so there weren’t a lot of jobs for myself working frontline in something that I was passionate about, so I shifted back to what I was doing before going to school, which was a paralegal, so I had shifted into a corporate paralegal position, which I’m very grateful for, because around the time of my diagnosis and throughout my treatment, I was working from home because of COVID. That was also happening during my diagnosis and treatment time. A lot was happening during that time, I will tell you that. I was a newly graduated social worker, just navigating my life with a lot of day-to-day stress, especially the stress of trying to find a new job that aligned with my passion.
First breast cancer symptoms: swollen lymph nodes in my armpit
What initially came to my attention, I think, was in fall 2019. I don’t know exactly which month — it’s October or November-ish. I was a paralegal at the time, so I was spending a lot of time sitting at a desk, and I don’t sit well. I was leaning to my left side, and I felt a pinch in my armpit. I was leaning on my left side, and I felt a pinch in my armpit. I thought, “Oh,” and I went digging around in my armpit, and I felt a swollen lymph node.
I thought, “Okay.” I’ve had swollen lymph nodes throughout my life, on and off. Typically, anytime a doctor has seen them, they were just like, “Oh, it’s fine. You might have an infection somewhere, a bug bite, or something. It’ll go down.” So that’s initially what I thought. I figured I would keep an eye on it.
A couple of weeks — maybe even a month — went by, and I was continuously checking it. I noticed a few more, so that set off some red flags in my head. At that time, I didn’t have a practitioner. I didn’t have a doctor, like a family doctor or anything like that. I just had walk-in clinics. I was living in Alberta at the time, and I went to quite a few walk-in clinics. I had essentially just been brushed off by a few doctors. They were just like, “You’re fine.” Some of them didn’t even really check my armpit, even though I knew exactly how to find it. My arm couldn’t be up; it had to be down, and your fingers had to be in a certain way. I knew exactly how to find the lumps.
I probably saw three or four different doctors. I just kept advocating for myself. I kept going. I kept saying, “There is something wrong. It’s been a month. These are still here, and I feel fine.” There was nothing else that I could feel was wrong with me, but I knew something was wrong. By the fourth or fifth doctor — I honestly can’t be sure exactly — I went in and said, “Look, you have to feel this. Something’s wrong.” I’m grateful for that one last doctor who felt them. He said, “Oh, interesting. And it’s been this long?” I said, “Yeah, and I’m really sick of constantly going in to see these other doctors that just don’t listen to me. I know this needs to be looked at.”
Being dismissed by doctors and pushing for answers
The doctor said, “Yeah, this is interesting,” and he asked me if I had been breastfeeding and all these other things. I said no. At that time, I truly had no idea that the lymph nodes in my armpits were connected to this part of my body, my breast. I honestly had no idea. I don’t have a medical background.
He submitted a referral for an ultrasound. I had my ultrasound around the end of the year in December. I went in for my ultrasound; everything seemed fine. They didn’t tell me anything. They said I would get my results within the new year.
Early January, I got a call from that doctor. He said, “They want to send you in for a biopsy.” I said, “Okay.” My biopsy was scheduled for January 15, 2020. I went into the hospital by myself because I didn’t think anything of it. Nobody thinks of cancer. Even if you’re a mild hypochondriac like myself, you think of anything else, but truly, the last thing you think of is cancer.
I went for my biopsy. The doctor and a nurse were there, and they were both very kind — almost a little too overbearing for my personal taste. We did the biopsy. It was painful. It honestly wasn’t the greatest thing. I remember the doctor took the sample and walked like four steps to his little microscope or whatever it’s called, turned around, and said, “Rebecca, I’m sorry. It’s cancer.”
I sat up, and the nurse tried to comfort me. I said, “No, I’m good.” I looked at him and said, “What do you mean it’s cancer? I’m in my 20s.” He said, “Yeah, there are a lot of cancer cells in this sample that we took. I’m really sorry.” I asked, “What do you mean? What kind? What are you talking about?” He said, “It’s breast cancer.”
I remember all the moisture in my mouth was gone, and I started making these really odd jokes. It was such a blur while this doctor was talking to me, and the nurse was trying to squeeze my hand and rub my back. A lot was coming at me. I remember specifically looking at the doctor. He asked, “Are you okay?” because I was laughing. He said, “It’s fine. You’re in shock.” I said, “Yeah, I’m in shock. You just told me that I’m essentially going to die.” I was joking, but that’s how it felt.
He looked at me dead in the eye and said, “No. I’m not telling you you’re going to die. People with this diagnosis typically can live three to four years.” Everything came back to reality. I thought, “I’m in my 20s. You’re telling me now that I have a life expectancy of three to four years?” I thought, “I’m good, I’m done.” I got up, grabbed my clothes, and said, “I’m out.” That was how it ended. I didn’t have any more information after that.
I left with that doctor’s sentence in my head — that I could live up to three to four years. I’m in my 20s. That’s not something you want to hear. I gathered my things, and at the time, my partner picked me up. He surprised me outside of the hospital and said, “I’m here.” We went and debriefed, had some dinner. I don’t think I slept that night. It was such a weird, surreal feeling because nothing really lands when you get that information. Your body and your brain are battling each other for what is real and what’s not. You’re trying to find ways to cope, but it’s just a lot. That was January 15, 2020.
How medical gaslighting impacts Indigenous patients
I don’t think there was any inclination for me to think that I had cancer, but I knew something was wrong. I was frustrated. I felt like all the doctors looked at me like I was being a hypochondriac and that I was too young for anything serious. Being turned away that many times is so defeating.
This is a main reason why my social work has led me into the healthcare field and advocating for Indigenous populations. I think of other Indigenous people going into these systems, like healthcare, that have historically harmed our people. We already have a mistrust of a system like this. To be able to go in and be vulnerable — saying, “I’m seeking help” — and to be turned away so many times, no wonder Indigenous people, Indigenous women, are being diagnosed at later stages.
I’m a stubborn person. I have a history of advocating for myself because I was fortunate enough to go to school, especially in a field like social work, where you’re trained to advocate for people. That is mostly what education is and what the careers are: advocating. I already knew how to advocate for myself. I was already a very stubborn woman. But my brain automatically thinks of all the women and people who go and seek help from these systems and are getting turned away.
Starting cancer care after diagnosis
It makes me sick to my stomach and honestly ignites this passion for my work. In terms of myself, there was never a feeling that it could have been cancer. I just knew there was something wrong. I was defeated and very frustrated that nobody would listen to me. I even had my boyfriend at the time and my family members saying, “You’re fine, you’re fine.” And I was like, “I know I’m not.” I know I’m a little bit of a hypochondriac, but I just needed somebody to listen to me and not brush me off.
The beginning of care started the next morning after my confirmation that it was cancer. I didn’t know anything else, and I did my best to stay off of Google because I knew that would spiral me. I still do that to this day — if I have something wrong with me, I’ll Google it. But at that time, I was grateful I stayed off Google. I didn’t know anything. I knew it was breast cancer and that a doctor told me I could live three to four years. That was all the information I had.
The next morning, I got a phone call from the cancer care clinic. A lovely nurse said, “I am so sorry for your recent diagnosis. We got your file. This is what the plan is moving forward.” Because I didn’t have a family doctor, they were going to take over my file. Any updates on tests and things? They would be the main contact people.
She said I had a referral to an oncologist and would eventually see an oncologist. I also had a referral for a surgeon. But before seeing them, I had tests: a CT scan, an MRI, a PET scan, and a bone density scan. I had four or five scans all in a row. That week, moving forward, I was just in scan after scan.
Undergoing scans and feeling alone at the cancer center
Before that, I had never even broken a bone. I had never needed a scan. I didn’t know what I was going into. I had never spent so much time in a hospital. It was weird because I would go into these rooms waiting for scans, all through the cancer center, and I was the youngest person in the room. It felt really isolating. I felt so alone.
I had people look at me oddly, almost pitifully. I didn’t even know what was going on. Weeks after my official diagnosis, I did all my scans and had an appointment, my initial appointment with a surgeon. I met with the surgeon before I met with my oncologist. I mildly remember the appointment. I’m mostly going off what my boyfriend at the time relayed, because I was in full shutdown mode. There was no information that anybody could give me that I would retain. It was just in and out. I was like a shell of a human, truly. My full fight-or-flight mode was nonexistent.
Meeting the surgeon who changed my mindset
I was truly existing as a shell of a human. It was an odd sensation for sure. I met with a surgeon, this young, badass South Asian woman. She looked at me and said, “How are you feeling?” I said, “I feel nothing.” Anybody who knows me, especially my therapist, would laugh because I say that a lot. “I feel nothing.” It’s an odd coping mechanism, but I said, “I feel nothing. This has been a lot.”
I told her, “I don’t know anything. It’s been weeks of scans. All I know is I have breast cancer, and it’s really bad, because I’m only going to live a few years.” She looked at me and said, “You’re in your 20s.” I said, “I’m aware of my age.” She said, “I’m not signing your death certificate. I don’t care what is going on or what anybody told you before. We’re throwing the entire kitchen sink at it. I’m not scared of what’s going to happen next. You’re going to be fine.”
I think that was the first time that I actually felt a mild sense of peace. I still didn’t really know what was going on, but nobody had really talked to me like that before. She was so confident in everything she was telling me that I felt mildly okay. I came back into the room a little bit.
She said they didn’t officially stage my diagnosis yet, but at that time, I knew exactly what kind of breast cancer I had. I had HER2-positive breast cancer, hormone-negative, and the inflammatory kind. She said, “We don’t know the stage yet; we’re still waiting for your PET scan results to come back. The plan moving forward: you’ll get more information when you meet your oncologist, but we’re going to do chemo first, and then this is where I come in. We’re going to do surgery, and then, I assume, radiation after that. I’m in charge of the surgery. We’ll see what we want to do depending on how you react to chemo.”
Surgical decisions and wishing I’d had a double mastectomy
She said that, depending on the lymph nodes, how many are impacted, and how many we need to take out, we would decide. At that point, I didn’t have a tumor. Some of the scans showed my lymph nodes in my armpit were so cancerous — using that really scary word “metastasized.” They were so heavy in cancer, but there was a spot in my left breast on the far left that had pre-cancer cells. There was no actual tumor, so they think the cancer originally started in my armpit.
She said we would go from there and see how the chemo goes. I remember looking at her and saying, “Take everything.” She said, “What do you mean?” I said, “I want a double mastectomy. Take it all. I’m pissed off now. I’m pissed off that I’m sick. I’m pissed off that a doctor told me I’m only going to live a couple of years, and I’m pissed off at my boobs. They’re trying to kill me. Take them, take them.”
“I remember her saying, ‘Okay, I understand. What you’re feeling is valid.’” But she also said, “You’re in your 20s. You don’t have kids. I don’t want to do that yet. I want you to be able to, if you do end up having kids, maybe breastfeed.” She gave me that option, but she didn’t really consider the double mastectomy.
Looking back, I really wish she did. I wish she had listened to me a little more in terms of me wanting a double mastectomy because years later, I’m still dealing with a lot of fallout from that choice.
From there, I met with her and then got the PET scan results. I met with my oncologist and was officially staged at stage 3 — so the last stage before it becomes stage 4, which is classified as incurable. The cancer had spread all the way up to my collarbone in the lymph nodes, and there was no detection of it anywhere else. I was very grateful for that diagnosis. Then I started chemo. I started chemo two days before Canada officially went into COVID lockdown. Two days before.
Starting chemotherapy at the beginning of the COVID lockdown
I lived eight hours plus from any of my immediate family. I had friends and my boyfriend at the time was there with me. But because of COVID — and as you know, chemotherapy really messes with your immune system — I was absolutely terrified to be anywhere.
I got my first infusion of chemo on a Saturday. Then, I think it was Tuesday or Wednesday, I was in the office. I hadn’t felt the side effects from the chemo yet; it usually took a couple of days. We got sent home. They packed us up with all of our stuff, and the country was officially in lockdown. I went back home, and that was basically my life from there. Then the chemo effects started coming up.
Chemo alone, isolation, and dangerous side effects
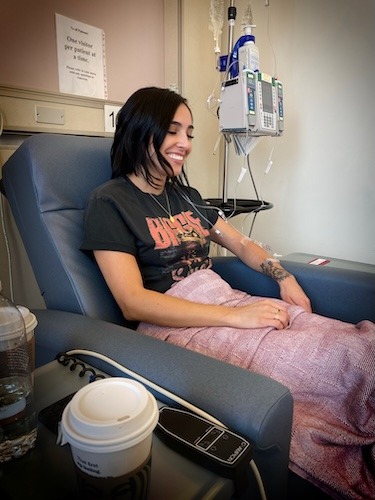
In terms of isolation, my first appointment, my partner at the time did come with me, which was great. There wasn’t a mask requirement at that point. But for my next treatment, scheduled every three weeks, I had to go in with a full mask. My hair had already fallen out by then. I walked in, and the hospital was scary. There was nobody. There usually weren’t many people because it was a Saturday, but this was a bare-bones staff. Everybody there for treatment was on their own. I couldn’t bring anybody. It sucked for sure.
You have a lot of time to sit in your own thoughts, which can be a good or bad thing. I found ways: I listened to music and podcasts. My chemo infusions were three to four hours long. I was also living alone. Throughout a lot of my chemo infusions and the whole process of chemo — I had six infusions — it was scary because I was alone for a lot of it.
My side effects were quite consistent, but at first I didn’t know what to expect. I had a list of potential side effects, but, obviously, it depends on the person. It’s funny because I got it down to literal days when I felt certain about things. I knew what was coming. It was definitely scary.
I had times where, in the third week after my infusion — just when my body would start feeling better — I’d get hit with a massive nosebleed to the point where I passed out because there was so much blood. I would wake up and think, “Oh,” seeing blood all over the floor. I would be alone. Thank God I woke up. There were scary moments like that. I did a lot of this alone, and it was very isolating.
I had nobody in my life who knew what this felt like. I didn’t know anybody with a young cancer diagnosis. I had grandparents who had colon cancer, but they were in their 90s, and I remember how horrible that was. But during COVID and cancer, I had nobody to lean on.
Finding the young breast cancer community through social media
I decided, about a month after I was diagnosed, to share it online. I thought, “There have to be other people out there,” and I needed that because, after my diagnosis, once I started getting more information about my staging and the chemotherapy I was on, I started going on Google, learning more about my survival rate and all this horrible stuff. I don’t recommend anybody Googling anything.
I put it out there on social media and started sharing my journey. Actually, I shared my journey, period. I shared it all. I was connected to this community — shout out to Rethink Breast Cancer. They’re an Instagram page and social media platform designed for a young community impacted by breast cancer and other cancers. I found women all over Canada, literally diagnosed with either the same staging or a similar kind of breast cancer, at my age. I recall a young girl in Ontario. We had almost a mirrored experience, except she had hormone-positive breast cancer. It was the same staging, our treatments were around the same time, and we connected online.
I’m so grateful to be connected to a community that knew what I was going through. It shows the importance of peer support — knowing you’re not alone, even if you are physically alone. That online community really changed my outlook on my treatment and my overall expectations and realities, just knowing that I’m not alone.
Cutting and shaving my hair: Indigenous identity and chemo hair loss
It was a lot. That was my first infusion, and about one week after. My hair was quite long; it reached my hips. When I knew I was going to get chemotherapy, I cut my hair super short, collarbone length, because in my head it would be less traumatic for my hair to fall out shorter than if it were 22 inches long. I got a bob cut by this lovely lady whose mom had also had breast cancer. She knew exactly what she was doing. She said, “I cut her hair before she started chemo. It definitely helps with the process, because losing your hair is traumatic.”
As an Indigenous woman, I really value our hair. It’s an extension of our spirit. Losing my hair was honestly horrible. But being able to decide to shorten it at that time was empowering. It sucked that I didn’t have people with me. I had my partner at the time, but I had plans to share this moment with many of my girlfriends who understood the importance of my hair from a spiritual perspective. Because it was COVID, I didn’t have that support, unfortunately.
But on a positive note, I was able to share it online. I received a lot of support that way. One morning — not even a week after my first infusion — I woke up and my scalp hurt. I put my hair in a little scrunchie to wash my face. When I pulled the scrunchie out, a massive clump of hair came with it. I thought, “Okay, it’s happening.” I looked at my scalp, and it was covered in red bumps and was so inflamed. I couldn’t even brush my hair. I ran my fingers through it, and clumps were falling out.
I called my boyfriend and said, “Hey, I’m going to need to use your shaver. This is painful, and it’s traumatic that it’s just coming out in clumps. I don’t want to deal with this.” I asked him to record it, and I shaved it.
Shaving my head to take back some control
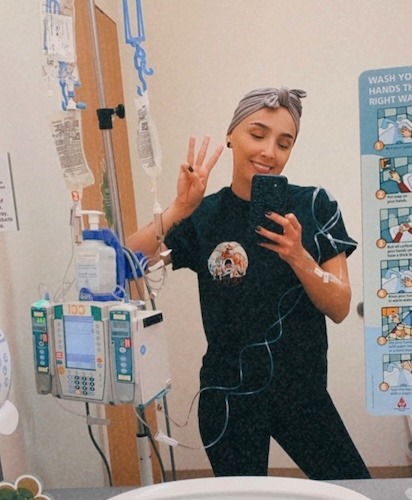
It’s so hard to lose all control. You don’t have any control. You’re just there, hoping the chemo does what it needs to do. It literally takes the life out of you. It took my hair.
I think making that choice to shave it at that time was like taking a little bit of power back. I could have just left it and let it fall out in clumps. I shaved it short, and I didn’t lose all my hair right away. It wasn’t until the third infusion that I was slick bald — no hair, nothing. But I’m glad I decided to shave my head when I did. At least this I could control. I was taking a little bit of my power back. It was a decision I was making, not the chemo.
Reaching six years in remission and wanting to confront that first doctor
It feels good. I honestly want to go up to that doctor and tell him to go f*** himself, to be honest with you. I hope he somehow sees that and thinks, “Oh, okay, maybe I shouldn’t say this to people.” Or maybe my oncologist or my surgeon figured out who he was and told him, “Can you stop and maybe have some bedside manner?”
But it feels good. It feels good to get to that point. I think you always carry a fear of recurrence. I’m going into my sixth year of remission, and I’m still dealing with a really deep fear of it coming back. Any headache that lasts too long, any bone pain or discomfort, you’re immediately brought back to that state where you’re just like, “Oh, okay.”
Your oncologist teaches you that if something sticks around for more than two weeks, they’ll ask you to come back. I don’t have an oncologist anymore, and that’s another thing I don’t really enjoy being this far back. For myself, I really got attached to my oncologist, my follow-up oncologist. He was in my life for five years after the hardest time.
Life after treatment: anxiety, trauma, and the challenges of remission
The treatment — the 11 months of treatment — sucked. It wasn’t fun at all. But looking back now, you were dealing with effects that were there and immediate. You felt them and processed them because they were right in front of you.
In terms of moving forward after cancer treatment and after everything, remission is just as hard, I find. It’s more mentally exhausting. My anxiety is through the roof. I’m fully on anxiety medication; my anxiety is constant. Having cancer and going through something like that is trauma. You’re dealing with that aftermath, and I don’t think you really realize it until you’re on the other side. It’s great, and we’re happy that we’re here, and it was a hard road to get there. But remission and moving forward are still really hard, and it’s still a battle.
I’m very grateful for my oncologist. He knows that I spiraled and that I continue to spiral. He was always very upfront and frank with me: “Rebecca, calm down. Rebecca, don’t do this. Rebecca, don’t do that.” He was very direct with me, and it’s something I needed.
Every single year since being in remission, I’ve had some scare. I’m actually dealing with that right now. Last summer, I had a scare because I found a swollen lymph node in my armpit, and I spiraled because that’s exactly how I found my original cancer. After further investigation, they said, “You’re good.” I thought, “Perfect.”
This year, because I still get scans every year, I just got my scan, and they found something suspicious. Now I’m waiting for an ultrasound. It is truly never-ending. You just have to have faith that everything happens for a reason and that you’re going to be okay. Whatever the future holds, you can deal with it. But it’s always going to be scary, especially now that I don’t have an oncologist anymore. I do have a family doctor now, and I’m very grateful for her and her communication.
It’s nice to be on this other side, of course, but cancer is a disease and something that is unfortunately going to be there for a long time.
How cancer and lived experience shaped my career path
My line of work is kind of all over the place, but if I were to describe it succinctly, I just want to be able to change systems.
Seeing the way people look at you, being turned away from services, being treated differently because of the way you look or speak or the color of your skin or the way you choose to practice your spirituality — that shouldn’t be the life we’re living, especially in 2026.
After my cancer, I moved to British Columbia, where I live now. I went straight into a frontline hospital role. That was still peak COVID because I moved in December 2020. I had just finished radiation. In my brain, I needed change. I couldn’t sit in Alberta anymore. I needed to go somewhere and find a place where I was actually doing social work. Thankfully, I received a position where I would be on the frontline in a hospital, working alongside and with Indigenous patients in a hospital setting. I moved and relocated for that job.
For two years, I was working on the frontline with individuals coming in and out from rural and remote communities and urban Indigenous populations in a hospital. As somebody with experience navigating hospital systems — which are horrible, large, and difficult to navigate, and also terrifying in themselves — it was a lot. Healthcare historically has harmed our people and continues to do so. It’s a scary place as an Indigenous person.
I had really short hair, and I felt really empowered. I felt that sense of passion again because I was able to advocate for those people who felt like they didn’t have a voice. It was really powerful. I had numerous patients. It took me a while; there were times I had young Indigenous patients dealing with cancer diagnoses, and it took me time to have the courage to talk to them. It really was a trigger for me. It probably took six or seven months before I could go and speak to these young, later-stage diagnosed Indigenous patients.
I’m really glad I took the time I needed to heal that trauma or trigger within me. Once I was able to talk to them and tell them my story — because I knew how much peer support helped me during my diagnosis and treatment — that changed the game for me. That became my thing.
From frontline social work to system change and policy
I would talk to all of these young or older Indigenous people — whatever stage in life they were at — getting the news of their diagnosis and whatever stage in treatment they were at. Cancer looks different for every person, but many of the processes and stages going through the hospital system are similar. Sharing my story and letting them see me on the other side is really important.
I’m no longer working on the frontline. I needed a break. Ten years of frontline social work takes a lot out of you, and I felt ready for something bigger. I moved into more of a program development role. The cancer diagnosis and my experience working on the frontline have shaped my career in a way that I want to change policies and systems. Someone who has had their feet on the ground and experienced these systems — the good and the bad — has a voice that’s missing from many bigger systems, from people who sit in those ivory towers.
I feel like many of them don’t have that experience. They don’t try to uplift the voices of the people on the ground. For me, coming from the ground and moving up, that is the goal and will continue to be my goal.
I’m now going to do my master’s in community development, and I hope that manifests into something bigger. I want to move and shake and dismantle a lot of these systems that have harmed our people and continue to harm them. I’m hoping to continue uplifting Indigenous peoples’ voices, so there is hopefully a day when we don’t have to be scared to enter a healthcare system or any big system.
Processing cancer trauma and the need to grieve
I did want to touch on processing your diagnosis. I’m in therapy now. When you’re going through treatment, you’re offered support from a social worker or counselor. I tried all of that throughout my time in treatment, and I didn’t feel like I got anything from talk therapy. I felt like I needed a lot more.
I’m seeing a specialized trauma therapist now and have been for almost two years. I’ve learned a lot. I’ve learned that I haven’t actually processed the grief from my diagnosis. I haven’t processed a lot of things in my life, but one of the biggest things I’ve learned in trauma therapy is that I did not allow myself to grieve my diagnosis and my treatment, and those 11 months of going through some of the worst times in my life. I didn’t allow space for that. I didn’t even allow myself to cry.
I realize now you don’t think about it at the time. When I got diagnosed, I didn’t cry. I remember my mouth getting really dry, and I got angry, but I didn’t cry. I didn’t feel sad for myself. I didn’t feel shame or guilt. I didn’t feel anything. I didn’t feel grief like I should have. I think that is really important.
Moving through such a life-altering diagnosis, there is a time to be strong. Looking back, my brain shifted immediately into fight mode. I thought, “I don’t have time for anything else because I’m in fight mode. I’m going to do this. I’m going to beat this. I’m going to tell that doctor who said I would only live three to four years that I beat that.”
But I also think I did myself a disservice because now I’m dealing with a lot of the remnants from not allowing myself to grieve and not giving myself space to cry. I gave myself space to be angry, but not for anything else.
I think it’s really important to allow yourself to cry, to grieve, to be happy, to be angry — feel all the things. After getting a diagnosis like this and moving through all of the processes, allow yourself to cry. Allow yourself to grieve. Allow yourself to be happy and angry. Feel all of the things because when it’s time to fight, that will happen. At the beginning and in all the in-betweens, allow yourself to feel everything. Having that sit in and fester develops into other things like cancer, depression, and so many other things. It’s really important: feel everything.

Inspired by Rebecca’s story?
Share your story, too!
More Breast Cancer Stories
Amelia L., IDC, Stage 1, ER/PR+, HER2-
Symptom: Lump found during self breast exam
Treatments: TC chemotherapy; lumpectomy, double mastectomy, reconstruction; Tamoxifen
Rachel Y., IDC, Stage 1B
Symptoms: None; caught by delayed mammogram
Treatments: Double mastectomy, neoadjuvant chemotherapy, hormone therapy Tamoxifen
Rach D., IDC, Stage 2, Triple Positive
Symptom: Lump in right breast
Treatments: Neoadjuvant chemotherapy, double mastectomy, targeted therapy, hormone therapy
Caitlin J., IDC, Stage 2B, ER/PR+
Symptom: Lump found on breast
Treatments: Lumpectomy, AC/T chemotherapy, radiation, hormone therapy (Lupron & Anastrozole)
Joy R., IDC, Stage 2, Triple Negative
Symptom: Lump in breast
Treatments: Chemotherapy, double mastectomy, hysterectomy
Callie M., IDC, Stage 2B, Grade 2, ER+
Cancer Details: ER positive = estrogen receptor positive
1st Symptoms: Dimpling/lump found on breast
Treatment: Mastectomy, AC/T chemotherapy, hysterectomy, reconstruction
Monica H., IDC, Stage 2B & Undifferentiated Pleomorphic Sarcoma
Symptoms: Tightness and lump in left breast
Treatments: Chemotherapy, radiation, surgery
Stefanie H., IDC, Stage 3, Triple-Positive
Symptom: Lump in the breast
Treatments: Chemotherapy, surgery (lumpectomy), radiation














Leave a Reply