Anyone with Lungs Can Get Lung Cancer: Ashley’s Stage 4 HER2+ Lung Cancer Story Challenges the Stigma
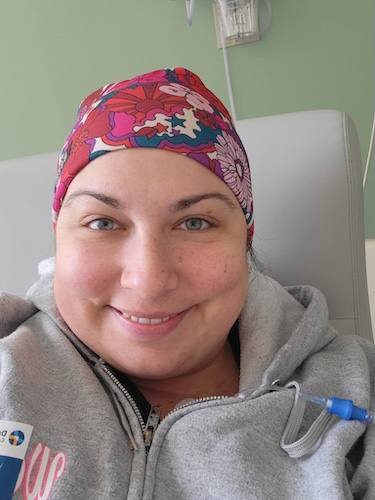
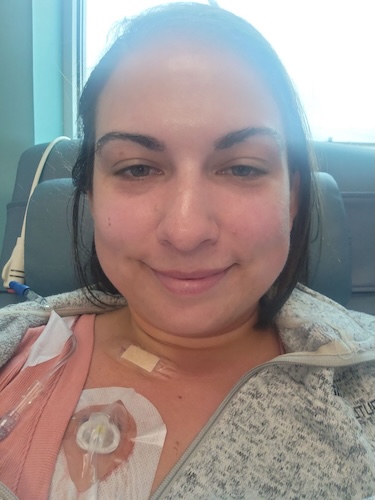
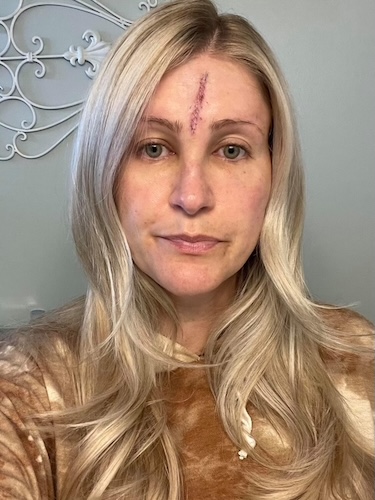
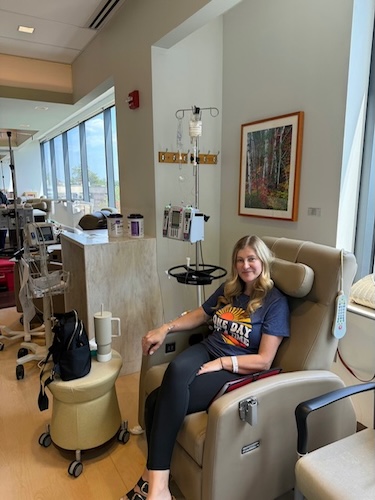
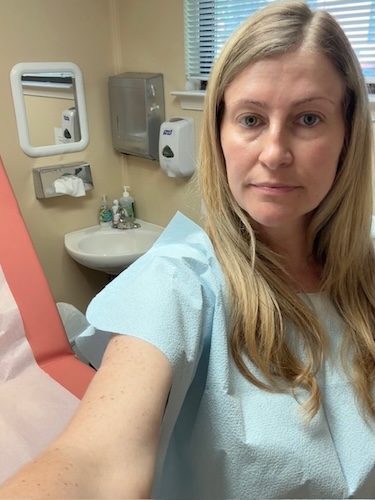
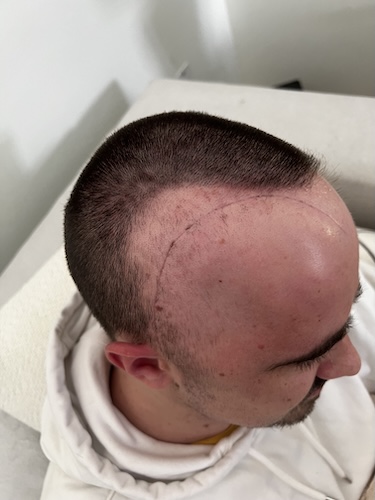
Ashley was diagnosed with stage 4 HER2+ lung cancer in August 2023. At 32, she was enjoying an active, healthy life, practicing yoga, hiking, and learning to ski, when she began to experience subtle but ominous symptoms. Over several months, she began to struggle with fatigue, breathlessness, and back pain. She went to see several doctors, but they thought she had bronchitis or musculoskeletal issues, mostly because she had no history of smoking.
Interviewed by: Nikki Murphy
Edited by: Chris Sanchez
The stigma surrounding lung cancer often links it to smoking, which can lead to delayed diagnoses in non-smokers like Ashley. She was asked time and again about her smoking history, and learned to emphasize that lung cancer isn’t only something that smokers get. Eventually, thanks to her physical therapist’s persistent advocacy, she ended up having an MRI that revealed that cancer was at the root of her symptoms. Later on, she had a bone biopsy, which confirmed that she had stage 4 HER2+ lung cancer. (Editor’s Note: HER2, short for Human Epidermal Growth Factor Receptor 2, is a protein that regulates cell functions, including cell growth and repair. HER2 mutations tend to be more common in non-small cell lung cancer patients with little to no smoking history.)

Ashley’s experience highlights the challenges young cancer patients, especially women, can face. She was hit hard by the diagnosis, and it was all the more agonizing because she and her husband had to shift abruptly from thinking about starting a family to confronting the reality of lifelong treatment for lung cancer. But in the face of these challenges, Ashley’s spirit was buoyed by her support system, her abiding love for teaching, and the quickly evolving landscape of targeted therapies to treat cancer.
The HER2-targeted therapy Ashley is currently on, which was approved shortly before she needed it, has proven effective in controlling stage 4 HER2+ lung cancer. Although she sometimes struggles to deal with tough side effects like fatigue and nausea, Ashley is still very thankful for the quality of life her treatment affords her. She also wants to emphasize that palliative care isn’t necessarily the same thing as end-of-life care; it’s about enhancing one’s comfort and well-being alongside active treatment for cancer.
Ashley’s story is a reminder of the importance of self-advocacy, the need to challenge lung cancer stigma, and the hope that advances in medical research offer. Watch her video and scroll down to read her interview transcript for more about:
- How she lived an active and healthy life, yet was diagnosed with stage 4 HER2+ lung cancer — how her story challenges the stigma
- Why palliative care isn’t just about end-of-life
- How Ashley’s symptoms went unnoticed for so long
- The question she’s tired of hearing: “Are you a smoker?” Her story reveals why it matters
- From teacher to lung cancer advocate — Ashley’s resilience is truly inspiring
- Name: Ashley C.
- Age at Diagnosis:
- 32
- Diagnosis:
- Non-Small Cell Lung Cancer (NSCLC)
- Stage:
- Stage 4
- Mutation:
- HER2
- Symptoms:
- Fatigue
- Breathlessness
- Persistent back pain
- Multiple rounds of bronchitis
- Treatments:
- Chemotherapy
- Targeted therapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Hello, I’m Ashley
- When I first noticed something was wrong
- I have no smoking history
- What happened next
- The moment everything changed
- My family’s history of cancer led me to a new cancer center
- How I learned about my biomarker
- I trust my doctor’s treatment decision
- What life has been like on a targeted therapy
- I’m living my life in three-week increments
- The decision to have biological children was taken from me
- My message of hope
- What I want others to know
Hello, I’m Ashley
My name is Ashley. I have stage 4 non-small cell lung cancer. I was diagnosed in August of 2023.
My husband, in particular, tells me all the time that one of the things he loves about me is my compassion and empathy for others. It’s partly why I’m a teacher. I really care about others and helping my community. And I think that’s what all my friends and family like about me.
When I first noticed something was wrong
I’ve always been a relatively healthy person. I remember in the winter of 2023, I got really sick for like a month, and that was out of the norm for me. And eventually, I went to the doctor because I was just having trouble breathing. Going upstairs was difficult. And I was in really, really good shape at the time. So that was just weird to me. And they were like, Oh, yeah, like no pneumonia. We took an X-ray. It’s clear. It’s probably just bronchitis. Take some antibiotics. Here’s an inhaler. You’ll be fine. And then it got a little bit better. And then, in April, the same thing happened, where I just got sick for about a month. Really out of breath. It was very out of the norm for me. Even if I got a cold, usually I would be over it very quickly. And then around the same time, I was sitting at work, and I just readjusted myself, and I felt this weird, like, popping sensation in my back. And then over the next few days, it just felt like I had thrown my back out or like there was a muscle issue. Eventually, I went to the doctor and got it checked out. And because I was a pretty active person, I did yoga multiple times a week, I went hiking, and I was learning how to ski. They just figured I had just done something to mess up my back. And they said, Go to PT and get back to us if anything changes.
And while I was doing physical therapy, it just progressively got worse, to the point where we weren’t even able to actually like get into doing stretches or exercises because every appointment was just about sort of managing pain. And it was my physical therapist who finally reached out to my primary care doctor, saying, We need to do some more imaging because this is not normal. I’ve never seen someone my age in my condition without a really good explanation as to why I was experiencing the amount of pain I was in. And so that was when that kind of prompted my primary care to say, “Alright, well, let’s at least get an MRI, and we’ll set you up with a neurosurgeon because they deal with facts, and we’ll take it from there.” And that’s when it started to snowball into not necessarily a neurosurgery issue, but an oncology issue. It was pretty quick, right after my initial MRI, that the radiologist reached out to my doctor’s office, saying, “This is serious. This isn’t just an injury. This is something that needs to be biopsied and dealt with quickly.” That was the initial result before I underwent all sorts of tests. It was like they knew it was probably cancer, but what type of cancer? Everybody was really confused at that point. And I just looked everywhere because nobody seemed to have a great explanation as to why, without many other symptoms. I had already had signs of bone metastases.
I have no smoking history
They looked at breast cancer. I had mammograms done. They were looking at different blood disorders like leukemia, lymphoma, and things like that. They were doing tests for all of that. They weren’t looking for lung cancer. I didn’t have a CT scan until after they had already known it was lung cancer. And then in my initial diagnosis, I remember being asked multiple times by my oncologist, So you didn’t smoke, you weren’t a smoker. And it was pretty frustrating. And I remember my husband and I going, “No, I’m not a smoker. I don’t know how many times I can tell you.” They almost didn’t believe me at first. My parents were smokers, but they never smoked in the house or the car with us. It’s not like I was exposed to all this secondhand smoke either. I had pretty much the same exposure most people do, which is occasionally the people in your life are smokers, but not anything significant day in and day out.
What happened next
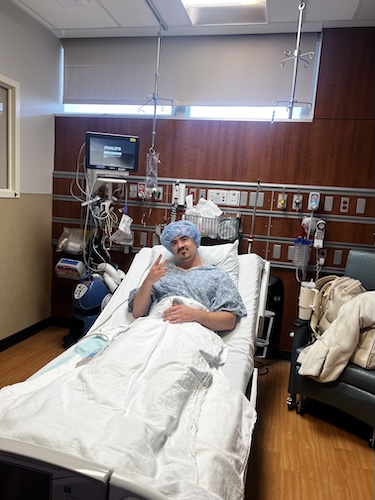
I was actually in the car going away for the weekend because it was my birthday. So we had planned a long weekend with some friends. I got a call from my primary care office, and the doctor said, “This is serious. They found a tumor.” Generally, he said, “In my experience, when we see this kind of imaging, it’s cancer somewhere else. So we need to find that.” And he was great because he reached out to the oncology practice associated with my primary office and said, “I want her to have an appointment next week.” He ordered a bunch of blood tests. In the meantime, he told me, “If you can get up to date on preventative vaccines and things like that, regardless of where this goes, I want you to be protected against things.” He put things in motion very quickly. I was very thankful for that. Once we met with my first oncologist, she had ordered a biopsy of the tumor that they had found in my back. And then other things like bone scans, blood tests, things like that. The biopsy of my bones was what revealed that it was lung cancer.
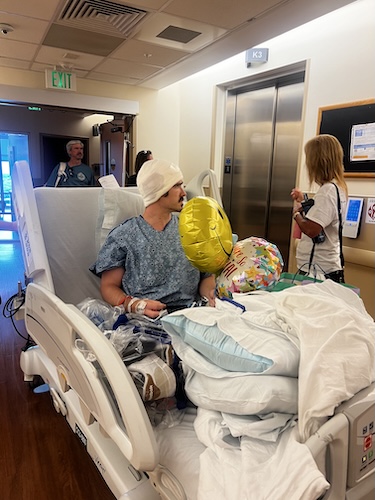
The bone biopsy was the hardest part of this whole process. It’s probably one of the worst medical procedures I’ve had in this whole process. Thinking back to it gets me all flustered again because it was a really sort of traumatic day. I had no idea how difficult it was going to be. And up until this point, I had been really healthy. It was the first time I’d ever really been in the hospital for a procedure. At that point, we didn’t know what to expect. I just wasn’t thinking that it was going to be a big deal. Neither was my husband. And I remember calling him afterwards and telling him, “You need to come back now.” And now with that experience, he’s pretty much always with me because we just never wanted to experience that again.
I ended up with, I think, a total of seven vertebrae that have tumors in them. I have a fractured rib that just won’t heal because of all of this. The crazy part is I only had one tumor in my right lung and a couple of nodules in my left lung. It had already spread to other parts of my body. I was lucky that it was just bones and lungs. Two years later, it’s still just bones and lungs, which is great. I’ve never had issues with my liver or my brain, which are two common places for lung cancer to spread. I have had more nodules pop up in both lungs. But for the most part, it’s been pretty well controlled. The confusing part for me was that I had chest X-rays done. And they didn’t see it, but I guess my tumor was small enough. It’s only when people have really large tumors and lung cancer that X-rays pick them up, which was not something I knew. They said, “Your tumor is small enough that a few months ago it was probably even smaller. We’re not surprised they didn’t see it on an X-ray. That was my big question, I asked, “I had a chest X-ray four months ago. Wouldn’t you have seen it?” And they said, “Not necessarily. Your tumor is really not that big.”
“You’re going in, you’re doing the right thing. You’re getting looked at. And the easiest, most basic test isn’t sensitive enough to pick it up. I’m sure if you looked at it knowing where the tumor was, I’m sure you know, knowing what we know now, you might be able to see it, but if you’re not looking for it, I guess it’s just not that obvious.”
The moment everything changed
I laugh because I feel like the media, like movies and TV shows, has put this perception in our head that, you get to a moment where you’re told, “Okay, you have cancer,” and it’s the first time you’ve ever heard it. In my case, it was more like drips and drabs. After my first MRI, we were pretty sure that I had cancer. It was more like, What kind of cancer? After the bone biopsy, that was when I knew it was lung cancer, because the bone biopsy had shown it. Basically, they can tell where the primary tumor is. And I actually got that through MyChart. And I remember I was sitting, I was out on vacation with my husband and several of our friends, and I got the notification on my phone. And we were out at dinner. And that’s when I pulled up the report and saw what the report said, took a deep breath, put my phone away, and then just tried to continue with dinner and having fun. And later that week, we went in for an appointment. And that’s when they started to explain what it all meant. I didn’t realize the full severity of my diagnosis until about a month later, when I was getting a second opinion at Dana-Farber. And my oncologist really kind of laid it out for me that my cancer wasn’t curable. It was very serious. That, although it would probably not be my case, because I was young and I was otherwise healthy.
It’s a 6 to 12-month survival type diagnosis. He was confident that that wasn’t going to be my situation. But, he’s also very much a data-driven provider. He said, “I can’t make any guarantees. This is just what we see in the data. But the vast majority of people are much older than you. They’re smokers. They have other health issues. You’re young, you’re not a smoker. The rest of you is perfectly healthy. I have faith that we’ll be able to give you a lot more time.” But we were really angry that this severity wasn’t stressed to us by my first oncologist because they were they were still talking to me about wanting to have kids, wanting to freeze eggs, things like that, which sends the message of, you’re going to get beyond this. There’s going to be a day after treatment. Which is not the case. I mean, hopefully, there’s some breakthrough, but realistically, that’s not what’s going to happen. That was really tough. It was kind of sort of like drips and drabs of learning I had cancer and what my diagnosis meant.
My family’s history of cancer led me to a new cancer center
My father had gotten care at Dana-Farber, and they were amazing. And my sister in law had breast cancer, and she had gotten care at Dana-Farber too. So we already knew several people who had gone there. And we always knew that, at a minimum, we wanted a second opinion there. We were willing to give my local hospital a chance. And we also didn’t want to delay initial treatments or anything like that. I did start chemo locally. But then, once we kind of realized that they were downplaying my diagnosis, we decided to make the switch. For anyone who is reasonably close to Dana-Farber, I always say call them because they know how difficult it is with insurance and scheduling, and appointments. They know how challenging that can all be. And they do work hard to streamline it. All I had to do was make a phone call, and they took down my basic information and who my doctor was. And next thing I know, they’re calling me and they asked, “ Do you have an appointment on this day?” And I was like, “Do I have to do anything else? Do I have to send you things?” They went, “No, no, no, we got it.” They did all the heavy lifting. And now to this day, whenever I have scans, appointments, anything like that, they’re great at scheduling things. And really doing a lot of the heavy lifting. It was definitely more challenging. At first, before I was getting my care there because I was having to do a lot of that. I was having to do a lot of calling and follow-ups, and trying to make all the appointments work, and making sure I was getting to the lab on time, and making sure I was getting this done in time.
Now that I’m in the Dana-Farber system, they just do a great job at scheduling all that. I’m thankful that I’m part of a healthcare organization that tries to put patients first and helps us navigate that easily.
How I learned about my biomarker
They did a blood biopsy pretty much right away once they knew it was lung cancer. And then they also once took a biopsy of my actual tumor. They did additional testing because I guess sometimes there are some tests that on the physical tumor, it’s a little bit more sensitive than the blood biopsy. I saw that it was HER2, but at my time of diagnosis, there were no approved treatments for lung cancer. This will be good in the future, either for clinical trials or if things do get approved. About four months before I saw progression on my first line of treatment, the FDA approved a HER2-targeted therapy. So I’ve been on that now for almost a year. It’ll be a year in August. And I still have no progression. We’re hoping that more HER2 treatments get approved before I see progression. Unfortunately, because of where my tumors are, it’s hard to measure tumor growth in bones. I’m just not a great candidate for clinical trials, because with clinical trials, you need to be able to really measure bone growth, our tumor growth. And in bones, it’s not the same as if it’s in your liver or your brain or things like that. So while I’m thankful I don’t have tumors there, it is also nerve-racking because I’m worried about progression without other HER2-targeted treatments available.
I trust my doctor’s treatment decision
It’s crazy how fast the cancer space can change as new drugs come online. My current treatment, which is a targeted therapy for HER2, is now being considered part of the first-line treatment. Whereas, for me, it’s been my second line. My first line was a more traditional chemotherapy. And I did four rounds of heavy chemo before my body started showing signs of not being able to handle it anymore. I was having a lot of liver enzyme issues and things like that. We dropped one of the drugs I was on and then just stayed on basically a maintenance chemo dose, and that was able to keep me progression-free for about a year; that was my whole treatment regimen. We made the switch to the targeted therapy when I had two PET scans in a row, six weeks apart, showing a lot more activity, not just in the bone metastases, but there were also multiple nodules popping up in my lungs. And that’s when we made the decision. My oncologist has been really good about being like, “If we’re just seeing a teeny tiny bit, we can probably hold off switching.” He always uses the expression, we only have so many tools in the toolbox. So we want to use all the tools till they’re not useful anymore. We have talked about radiation on individual spots, particularly the bone metastases. But again, we’re holding off on that because you can only do so much radiation. And then, through all of this, I did find out I have a rare genetic disorder that makes me predisposed to cancer. Radiation is very highly discouraged for individuals with this genetic disorder. It’s kind of like a last resort option. Because I’m at just such an elevated risk for developing additional cancers, we don’t want to set that off.
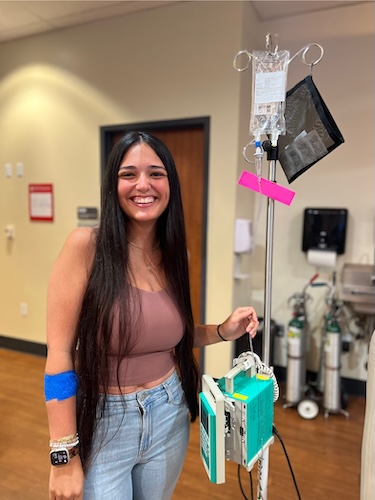
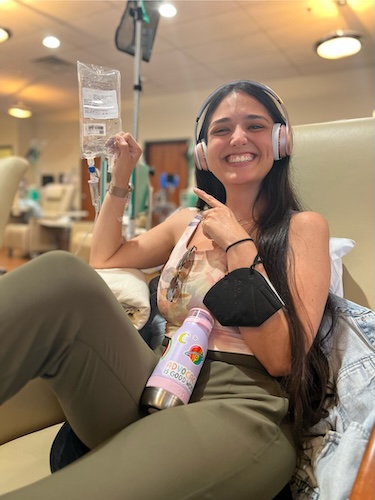
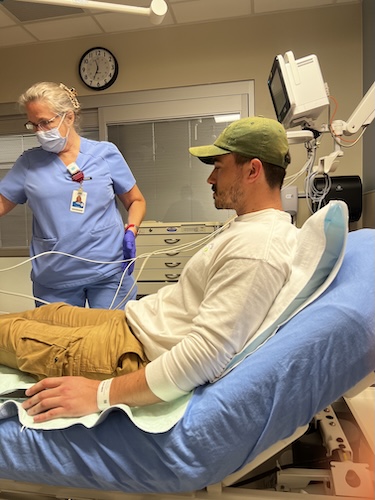
What life has been like on a targeted therapy
I’m going into my 18th round in a couple of weeks of my targeted therapy. I did have to take a break for a while because I was experiencing some lung inflammation, which is a known side effect of this particular drug. And we were trying to suss out whether it was due to the drug or just due to being sick and having lung cancer. My lungs are just more apt to experience inflammation. Eventually, we determined that it was more likely than not just being sick and my body trying to heal, and not the drug. Luckily, that was proven to be true. Because if it were the drug, then I wouldn’t be able to continue on the drug, because the lung inflammation is such a serious issue. The guidance is that once you experience this kind of inflammation, you have to discontinue the treatment. I think there’s a perception that because it’s targeted, it’s somehow going to be easier. And it’s actually been a really challenging drug to be on.
I’ve had multiple dose reductions. And I’ve also had to add in a bunch of extra things like extra fluids and stronger nausea medicines than I had been taking before. That’s been challenging. I’ve had to take off a little bit more work after treatments than I had in the past. Because I’m just very fatigued and nauseous. And that’s been challenging. Luckily, I have awesome nurses who work hard to make sure I’m in the best shape possible, leaving there and then. I now work with a palliative care team that has been good about adjusting medications and finding sort of different routines for me to help make that post-treatment week a little bit easier. But overall, I’m grateful that this drug was approved when it was, because had it not been, I would have had to go to a harsher, older chemo that is less effective. And I might have been in the position where I might have had to stop working or things like that because, as difficult as this drug is, I know it’s not as difficult as some of those older ones.
I’m living my life in three-week increments
Sometimes you get invited to things and you have to tell people, “Hey, it’s really going to depend on where my treatment is and if I’m feeling up to it. And I’m really not going to know until we get a lot closer.” And that’s been really challenging, I think, to kind of get used to being comfortable saying that to people. Totally unrelated. I happened to change jobs right when I was getting my cancer diagnosis. And I always joked, “Who quits their job and then finds out they have cancer?” And it actually has turned out to be a great thing. Not that I didn’t love my current or my former teaching position. But the position I’m in now is so great, and my administration and school district are just amazing at making sure I have everything I need and the time off that I need. So professionally, that was just like a change unrelated to my cancer, but it has actually been a great move for me. They’re just very open and supportive of everything I need. Professionally, I think I need to get used to taking time off. I was just not someone who ever really took a lot of time off. So being comfortable doing that and not feeling guilty and not feeling like I’m letting my students down by being absent has been a big growth opportunity for me. And that was really challenging at first to be comfortable taking the time that I needed.
The decision to have biological children was taken from me
I was getting to the point where even things like going to the bathroom were difficult because I was just in that much pain. So the idea of delaying treatment to freeze eggs or embryos — I quickly was just like, “No, this is crazy. If we get on the other side of this, there’s always adoption and foster care and other options out there.” When I realized, though, that this is going to be sort of a lifelong treatment, that was hard because even though we had gone back and forth about having kids and hadn’t really made a decision yet, it then felt like the decision was taken from us, but it still does make me sad sometimes to know that I won’t have that opportunity. It gets exhausting sometimes. I find that I’ll go several months where I’m feeling good, and life is good, life is great. And then usually it’s around a week when treatment hits me really hard. I’ll get pretty down. And, you have those thoughts of, “How can I keep doing this?” I think mental health is a huge part of treatment. And I’m lucky that through my treatment at Dana-Farber, I’m able to get mental health counseling.
My message of hope
My mom passed away from cancer when I was a toddler. And when I talked to family about what she went through, the drugs were so harsh.
The fact that we’re living in an age where you can have these really serious diagnoses and still have a quality of life. And still work, still participate in your hobbies and things like that, that to me is amazing. And that’s what keeps me going. I remember all the people that we’ve lost in the past who weren’t able to have the quality of life that I have. Because the drugs have just gotten so much better, and treatments have just continued to improve every single day. So even if I never get cured, I’m hopeful that the next drug that comes on the market is going to be that much more effective and that much more able to be easily tolerated and will give me that much better quality of life.
What I want others to know
While you’re young and healthy, do the things that you want to do. If you want to go visit a country, figure out how to make it happen. If there’s a restaurant you’ve always wanted to go to, save up the money and go to the restaurant. Don’t wait because you might be too incapacitated to do that. The only other big thing in my story is just through the testing that we had done. And then my personal family history of cancer. I found out I have a genetic condition called Li-Fraumeni syndrome. And through that, I’ve told people that it’s not normal for there to be multiple people in your family tree having cancer. And if that’s the case, even if you are okay, I encourage people to talk to their doctors to look into genetic testing. Because if it’s not, it’s not normal to get cancer young, and it’s not normal to have multiple aunts, uncles, grandparents, and parents with cancer. If you’re going through your family tree and several people have had cancer, it’s definitely worth the conversation. Because even compared to ten years ago, what they know about cancer genetics has definitely grown. And if I had known that I had had this genetic condition years ago, I would have been getting screenings that would have been able to catch my cancer.

Inspired by Ashley's story?
Share your story, too!
More Metastatic Lung Cancer Stories
No post found