“Hope Always” — Hunter’s Inspiring Rare Desmoplastic Small Round Cell Tumors Story
When he was 21, Hunter balanced the roles of a full-time 911 dispatcher, a son and friend, and a gamer. But he was about to experience a rare and intimidating diagnosis, desmoplastic small round cell tumors (DSRCT).
Interviewed by: Nikki Murphy
Edited by: Chris Sanchez
When symptoms first appeared in late 2023, including sharp abdominal pain, nausea, and vomiting, Hunter initially brushed them off. But within days, an ER visit revealed abdominal and pelvic masses. That led to a biopsy at the University of Kansas Cancer Center, where he finally heard the frightening and alien words “desmoplastic small round cell tumors.” The internet offered its usual blunt statistics, but instead of letting fear take over, he chose to focus on the possibilities of treatment and the hope that lies beyond numbers.

Throughout the experience, identity became an anchor. Being a dispatcher and caring for others had always been central to Hunter’s life. Transitioning from caregiver to patient was jarring, but it also opened a new perspective. Now, he sees the subtle emotional weight that patients carry; it’s something that goes far beyond medical charts. That awareness doesn’t erase the difficulty, but it deepens empathy for others.
Hunter’s treatment path for this rare cancer was intense: multiple surgeries, rigorous chemotherapy cycles, a clinical trial in New York, and both traditional and radioimmunotherapy radiation. Every phase came with its own hurdles, from relentless nausea and hair loss to the emotional strain of living life in hospital rhythms. He leaned on surprising comforts, including peppermints that successfully warded off nausea, and the unwavering support of family, friends, colleagues, and a community that consistently stepped up.
Survivorship, for Hunter, isn’t just about returning to “normal.” It’s about discovering purpose. Feeling supported inspired a commitment to give support in return. Online DSRCT groups offered connection and a simple but powerful phrase: “Hope always.” That reminder became a guiding principle on days when his energy was low or uncertainty high. Hope wasn’t at all passive; it was active, a choice to find positivity even within the hardest moments.
Self-advocacy also emerged as essential. Hunter’s experience navigating referrals, accessing clinical trials, and learning to speak up within the healthcare system reinforced one vital truth: patients deserve to be heard. He encourages others to share their stories, ask questions, and build visibility around rare cancers like desmoplastic small round cell tumors. Open conversations create stronger communities and remind those going through it that they are not alone.
Watch Hunter’s video and read the interview transcript below. You’ll see how:
- A dispatcher’s life flipped from caregiver to rare cancer patient overnight
- Peppermints became Hunter’s secret weapon against relentless chemo nausea
- A clinical trial in New York offered new hope
- “Hope always” became Hunter’s guiding mantra through fear and fatigue
- Hunter now champions survivorship and the power of patient voices
- Name: Hunter D.
- Age at Diagnosis:
- 21
- Diagnosis:
- Desmoplastic Small Round Cell Tumors (DSRCT)
- Symptoms:
- Abdominal pain
- Nausea
- Vomiting
- Fatigue
- Treatments:
- Surgeries: debulking surgeries
- Chemotherapy
- Radiation therapy: radioimmunotherapy, under a clinical trial
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
My name is Hunter
I’m 23 years old. I was diagnosed with desmoplastic small round cell tumor, or DSRCT.
My hobbies mainly consist of playing video games with friends and spending as much time as possible with family and friends. I work a lot, but I do love my job.
I work as a full-time 911 dispatcher and currently serve as a supervisor. I’ve been a dispatcher for the last five years. I grew up in emergency services with both my parents doing it.
It’s definitely been an interesting transition, going from a caregiver side to the patient side of things. You know, I’m used to seeing and talking to patients every day as part of my job and hearing what they have to go through, but going through it myself has given me a whole new perspective — seeing how it is to be a patient, and living through some of their daily struggles.
I got diagnosed when I was 21. I’m sure everybody can think of what every 21-year-old would rather be doing than fighting cancer. But I’ve tried not to really look at it as getting robbed of my early 20s. I’d rather see it as having been taught how to live a better life, so that I can live the rest of my life the best way that I can.
My symptoms came on suddenly
It really only took one or two days of not feeling right to finally decide to go to the emergency room and get checked out. And it all really started around November 2023.
We had just come back from a festival a couple of towns over. The next day, I started feeling some pretty sharp abdominal pains, which wasn’t normal, but I just thought it was a stomach bug and I could sleep it off, and it wouldn’t be anything. But the next day, the pains got worse, and I started to have nausea and was vomiting as well. And as that worsened and went on through the day, I ultimately decided that night that it was time to go to the ER and get checked out. And during that visit, we discovered that I had a rather large mass growing in my abdomen and a smaller mass in my pelvis.
The people at the ER didn’t have an exact answer for what they were looking at because they weren’t sure at the time. So we were referred to the University of Kansas, or KU Cancer Center, for a biopsy and further diagnosis. And we actually had to self-refer ourselves because there were no local hospitals taking incoming patients at the time. So we had to take steps outside of the emergency room to take the next step in my treatment plan.
The moment everything changed
We visited the doctors at KU and got a biopsy scheduled. And from that point, we were trying to put the next steps in place. It wasn’t until we got the biopsy done and I had a port placed in my left shoulder that we found out that I actually had a desmoplastic small round cell tumor, a rare type of cancer. And then I was referred to the specialist that they have at KU.
Getting my diagnosis — there are actually two parts to that story. The first had to do with the initial findings in the ER when they had to come in and break the news that I had my tumor. My mom, who has been a nurse for years and years and has seen everything, was a little bit of an emotional wreck. And my knee-jerk reaction in that situation was to try and make things funny. So I was trying to make jokes out of the situation. While it was a rather serious topic at the time, I was doing my best to make light of the situation and keep a positive outlook.
The second part came two weeks later, a week after my biopsy, when we received the official results. I was with my best friend at the time, and we were in my basement when I got the call from my doctor. And we rushed up to my mom to see what the news was, because at this point, we were thinking it was a more controllable cancer, such as a testicular cancer or a lymphoma. But I was told that I had what’s called a desmoplastic small round cell tumor and that I have an Ewing sarcoma genetic trait to it as well. So it was a little difficult finding out that I had such a rare disease. And of course, we didn’t know anything about it at that point. We had never heard of it before; most people haven’t.
The more that we were researching this, the more worrisome it became, because Google will be pretty straightforward and will give you some sad statistics, but luckily, that doesn’t seem to be the case with most cases these days.
My treatment plan
We knew pretty early on that no matter what it was, we were going to be hitting it pretty hard with chemo. So I had a port placed within about a week of getting out of the ER, just as a precaution, in case we needed it. And it turns out that we did end up needing it.
It wasn’t long after my diagnosis that my doctor at KU was on the phone with me, talking about the treatment cycles that I was going to be on. He didn’t give me a lot of options, but that’s just because there weren’t a lot of options to effectively fight this. So I was put on a pretty rigorous chemo cycle that did quite a bit of damage for a while, but I had switched around between a few different treatments and been in and out of the hospital for transfusions and IV antibiotics. I’d been admitted a multitude of times due to complications with chemo alone. And you know, I was putting my body through all of that, but I just had to keep thinking to myself during that time that there was an end to it and that there was a reason I was doing all of it.
So the overall treatment plan was to hit it early with chemo to hopefully shrink any tumors, and after that, to go in and remove those tumors surgically. And once those tumors were surgically removed and they could no longer see or detect any disease or scans, they were planning to going to do a whole abdominal radiation therapy as well as a clinical trial. And over the years, all of those treatments just added up and got me to where I am today.
But yeah, three different surgeries. The radio immunotherapy trial, a month of standard radiation or traditional radiation, and then chemo on top of all of that, and then finishing it off with maintenance chemo.
I took part in a clinical trial
The doctors say the most effective treatment plan for desmoplastic small round cell tumor is to hit it early on with surgery, followed by traditional radiation treatment. The main kind of surgery for this type of cancer is called a debulking surgery. And to my understanding, that’s where they go in and try and remove any physical mass that they had seen on scans that they can physically get hold of. And once those are removed, they try and target that area with a traditional type of radiation to kill any residual cells that were left over. And there are also many other trials offered for this type of cancer that patients have access to.
I may not remember everything, but to the best of my memory, the clinical trial that I took part in was a radioimmunotherapy trial offered by Dr. Slotkin’s team at Memorial Sloan-Kettering in New York City. Simply put, they surgically removed the masses from my abdomen and put a radioimmunotherapy fluid into my abdominal cavity to sit there and absorb over a few days. And that would hopefully mark the targeted cells for radiation to be killed later on during the traditional radiation process. So with the clinical trial, I also had my third and final exploratory surgery, where they went in and cleaned up any scar tissue or anything else left behind, and made sure I didn’t have anything else growing.
After the clinical trial, they followed up with a month of traditional radiation. So we were living out of the Ronald McDonald House in New York for about a month straight while I received radiation treatment.
The plan moving forward
My maintenance chemo was scheduled for about a year. We started around January of 2025, and I’ll hopefully be wrapping up around January 2026. I don’t know exactly how many treatments I’ve had, but I’ve had them pretty consistently every three weeks. So once or twice a month, I’ll go in for a week of chemo and then have two weeks off. So the cycles are definitely up there. I’ve stopped keeping track after so long, but hopefully I’ll be wrapping up soon.
We’re planning a final trip out at the first of the year, hopefully a remission trip, and ring the bell out there and have my remission start in New York, where my big medical journey started.
The side effects I experienced during treatment
The most significant side effects that I first experienced when starting chemo and having my other treatments were the nausea and vomiting. They were relentless. There wasn’t really anything I could do to stop them. There was no medication I could take. Nothing would help. Food smelled different. Food tasted different. The only thing that helped get my nausea under control was peppermints. Because peppermint oil is supposed to naturally help soothe the stomach and treat nausea. So everybody would chip in and help buy me peppermints whenever I was doing my chemo weeks because they knew that was the only thing that really helped keep me from getting sick.
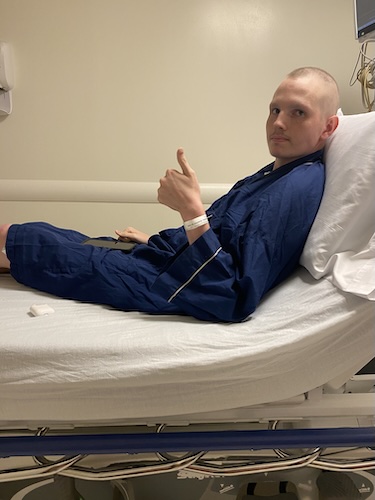
I also experienced hair loss. Luckily, I’m growing my hair back now, but my first chemo was pretty quick to take the hair out of my head whenever I started it. I was rocking the bald look for a while. But I feel like I look a lot better with hair. Luckily, I’m able to grow some hair now that I’m on my maintenance chemo.
The biggest challenge I faced
My biggest challenge is probably trying to feel normal after getting through it all again, because I’ve spent so long in and out of the hospital, in and out of doctors’ appointments, getting tested. People are constantly asking how I’m doing. And that’s something I constantly have to be aware of — how am I doing, really? I actively have to be watching everything that’s going on with my body and paying attention to everything that my body’s telling me.
But I’ve learned to stop worrying about things so much, to take everything day by day, and not necessarily be so anxious about every little thing that’s going on. I’m getting back to the normal side of life.
So early on, it was made very clear to me that I wasn’t going to have any problems finding support in my community. People really stepped up. They took time to make sure that I was doing okay during my treatment weeks and to check on me and make sure I and my family had everything we needed. I was also very lucky that my friends were able to support me through it. I wouldn’t have been able to get through it all if it weren’t for how well my employer treated me during all of it, too. They allowed me to keep my job while I was sick and kept my seat warm for me for whenever I was ready to come back.
What survivorship means to me
For me, survivorship means finding a higher purpose. Something that I’m more meant to do. For me, that’s helping others. I’ve found a lot of comfort in doing that. Well, it’s something that I already found comfort in doing before I got sick. But my experience has really resolidified that. Survivorship for me means advocating for others, moving on, not staying silent, and finding a voice. Not only for myself, but for others who are going through things like this. Because it’s not always easy to find yourself while you’re going through it.
I’m actually in a couple of online support groups for DSRCT. And one of the things that they say is, “Hope always.” And that was something I had never really heard until I started interacting with that group of people. But “hope always” has now come to mean to me that no matter how grim things look, all you can really do at the end of the day is hope. Because if you don’t, who will? Somebody’s got to have a little bit of hope in such a situation. I’ve had my hopeless days, but I’ve never let hopelessness consume me. I’ve always tried to try and take away at least one positive out of any bad situation, to kind of give myself a different perspective.
What I want others to know
One message that I definitely want people to take away is how important it is to find your voice and be heard. Because I don’t think anybody should go through this silently. They should absolutely fight cancer; they should be kicking and screaming. Since that’s how cancer tries to take you down, that’s how you should try and take cancer down, too.
I think finding a voice and being able to tell your story as a survivor and a patient is important not only to help give hope to others but also to be visible to other people, as someone who’s gone through it and someone who understands what other people are going through. I just want a stronger community.
I don’t want it to be such a hard thing for people to talk about. I want people to be able to talk about it more openly. Because when we talk about it openly, we can start tackling it. I feel like a lot of the problems don’t get talked about enough.
Patient advocacy is one thing that’s really important for me. After having gone through our own struggles with the American healthcare system, I am definitely a strong believer in finding your voice and self-advocating for yourself as a patient. Because if you don’t, who will?

Inspired by Hunter's story?
Share your story, too!
More Desmoplastic Small Round Cell Tumors (DSRCT) Stories
Hunter D., Desmoplastic Small Round Cell Tumors (DSRCT)
Symptoms: Abdominal pain, nausea, vomiting, fatigue
Treatments: Surgeries (debulking surgeries), chemotherapy, radiation therapy (radioimmunotherapy, under a clinical trial)
...
Gianna C., Desmoplastic Small Round Cell Tumors (DSRCT)
Initial Symptoms: Urinary tract infection (UTI), consistent pressure in stomach, stomach pains, passing out
Treatment: Chemotherapy, surgery
...
Hamish S., Desmoplastic Small Round Cell Tumors (DSRCT)
Symptoms: Persistent fatigue, nausea, weight loss, hard abdominal lump
Treatments: Interval-compressed chemotherapy, surgeries (cytoreductive surgery, peritonectomy, HIPEC, right hemicolectomy, low anterior resection)
...
Joe F., Desmoplastic Small Round Cell Tumors (DSRCT)
Symptoms: Mild abdominal pain, fatigue
Treatment: Surgery, chemotherapy, radiation
...