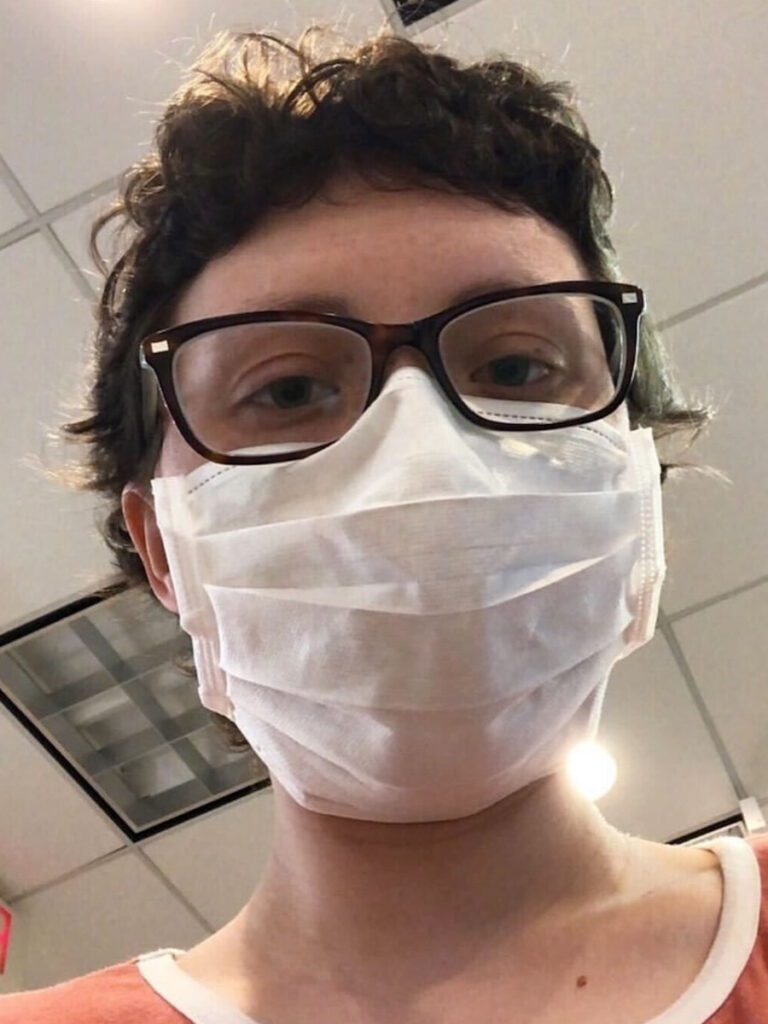
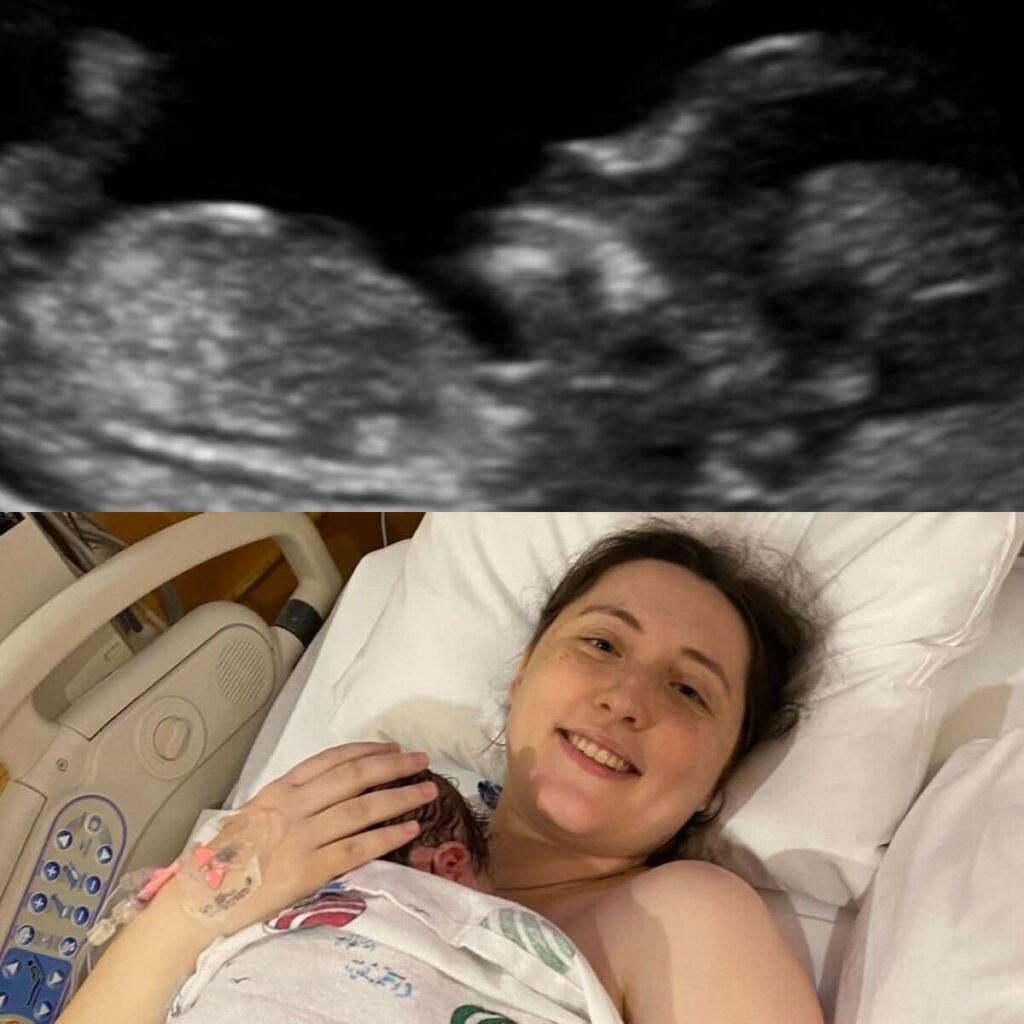
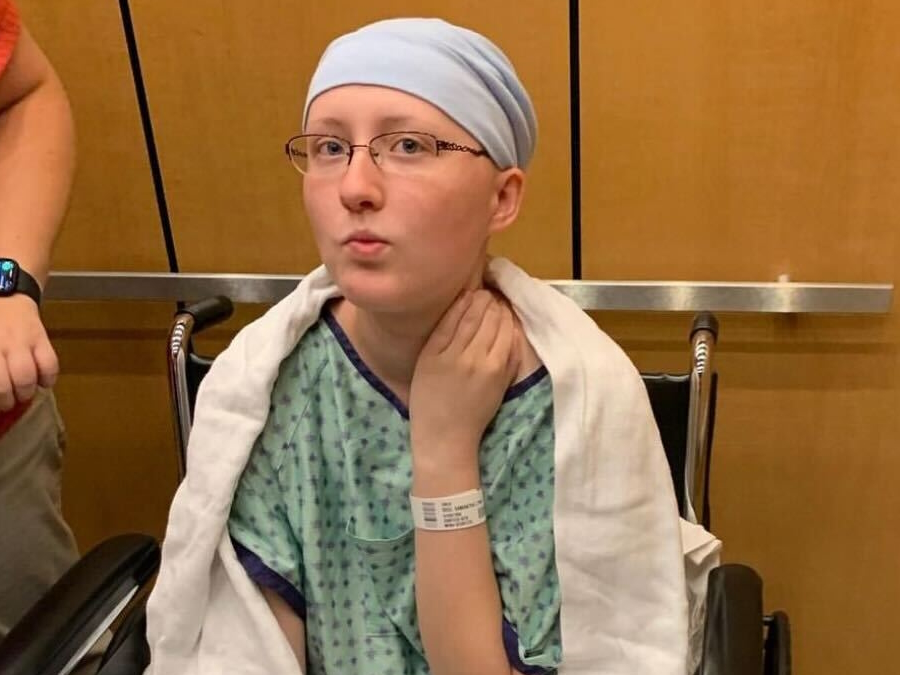
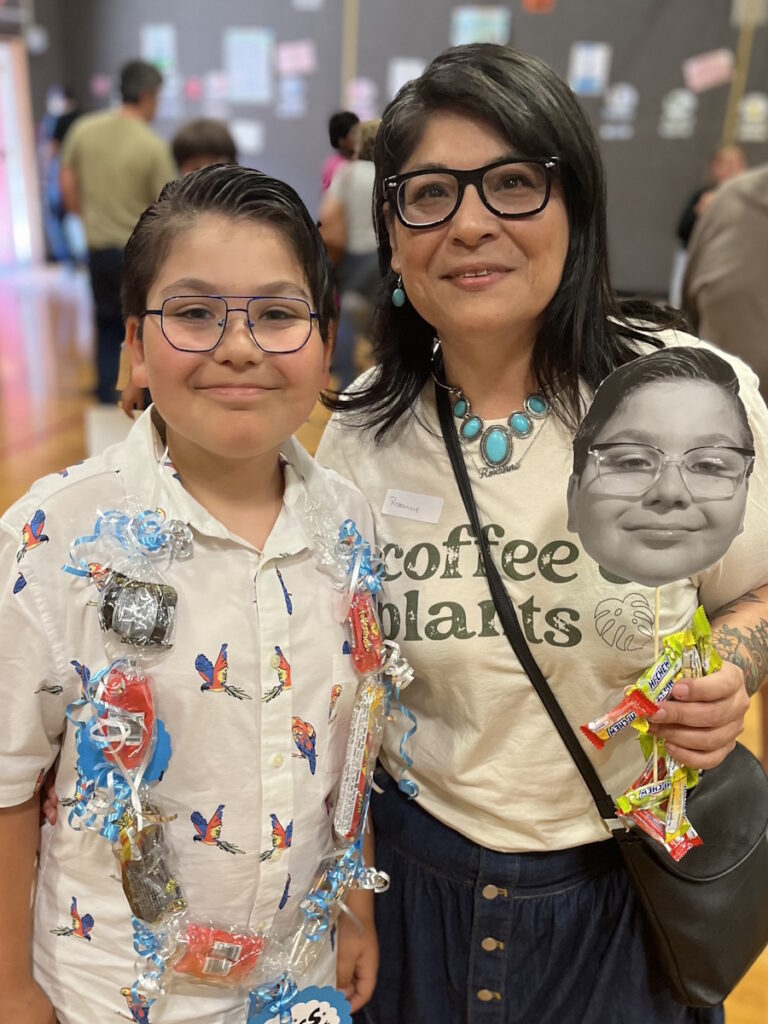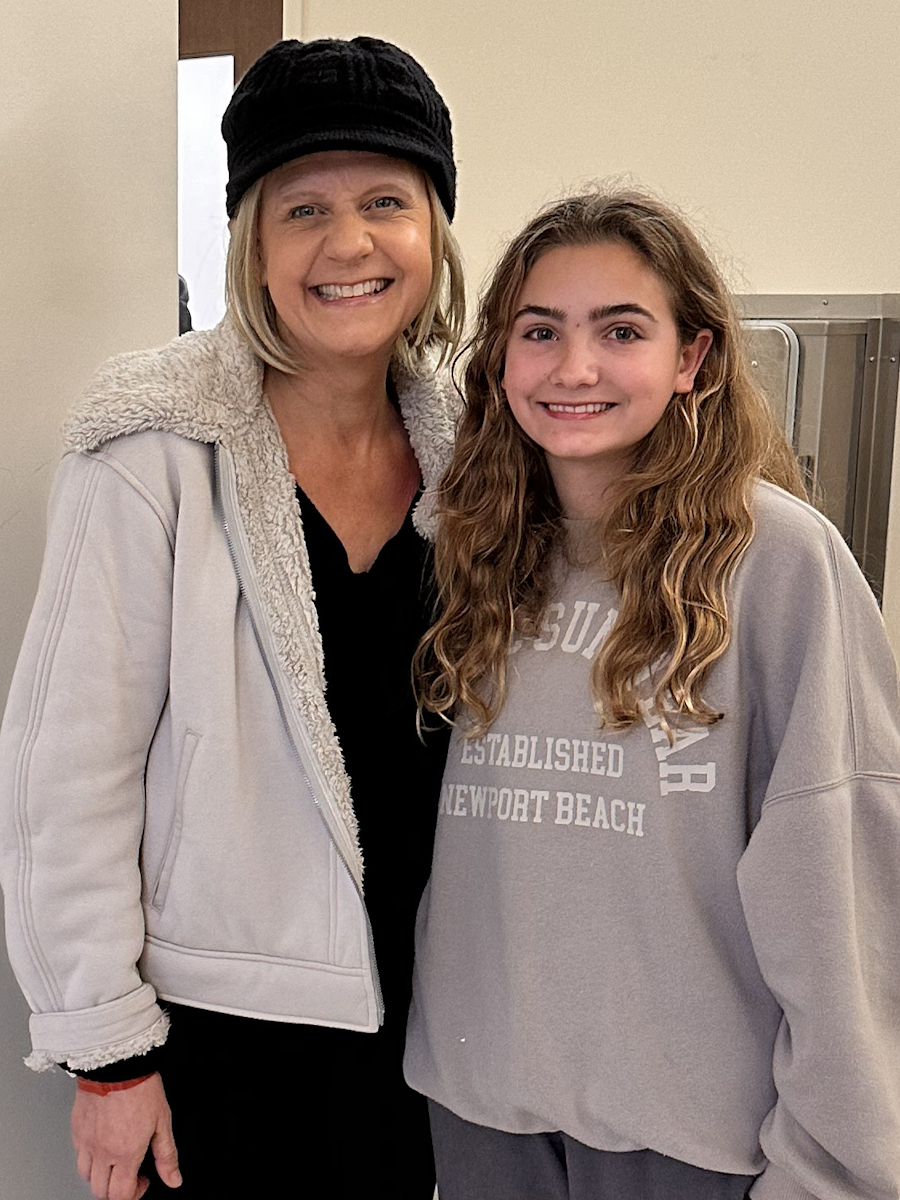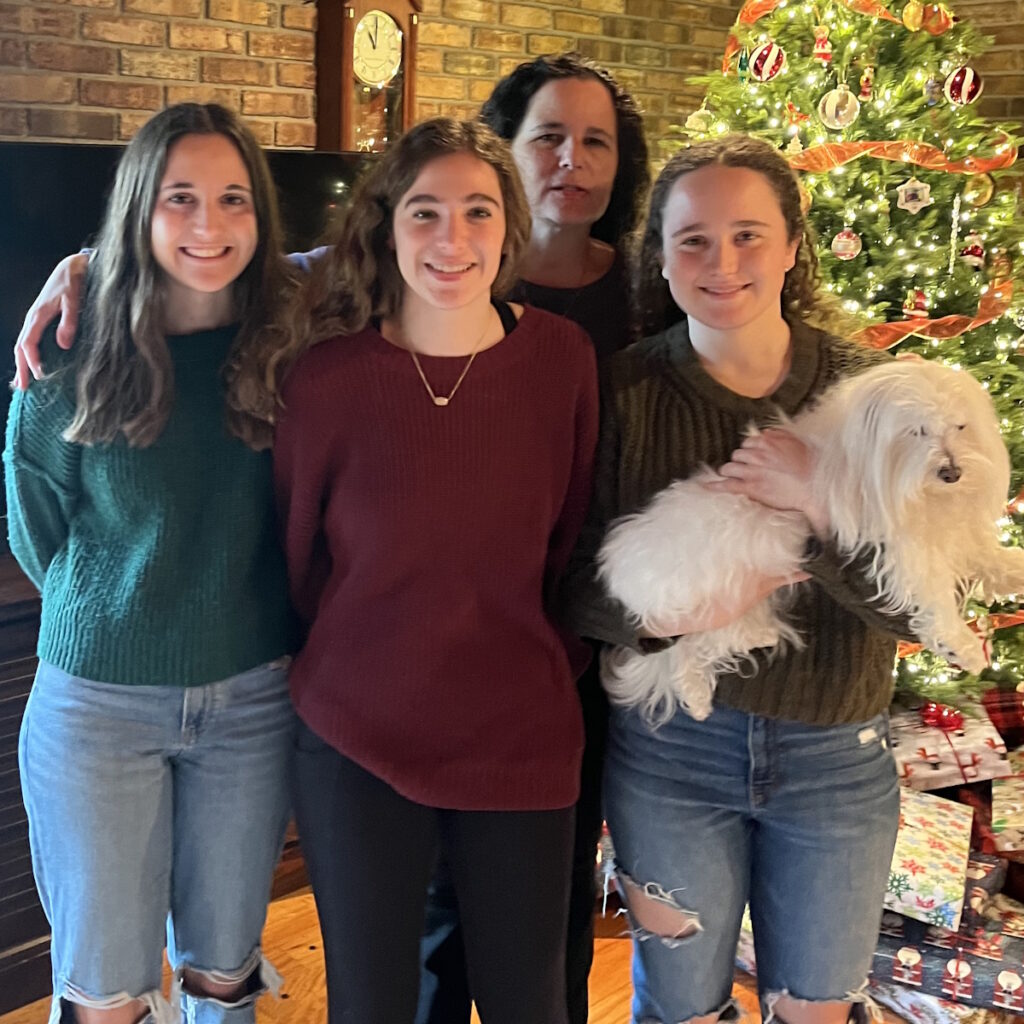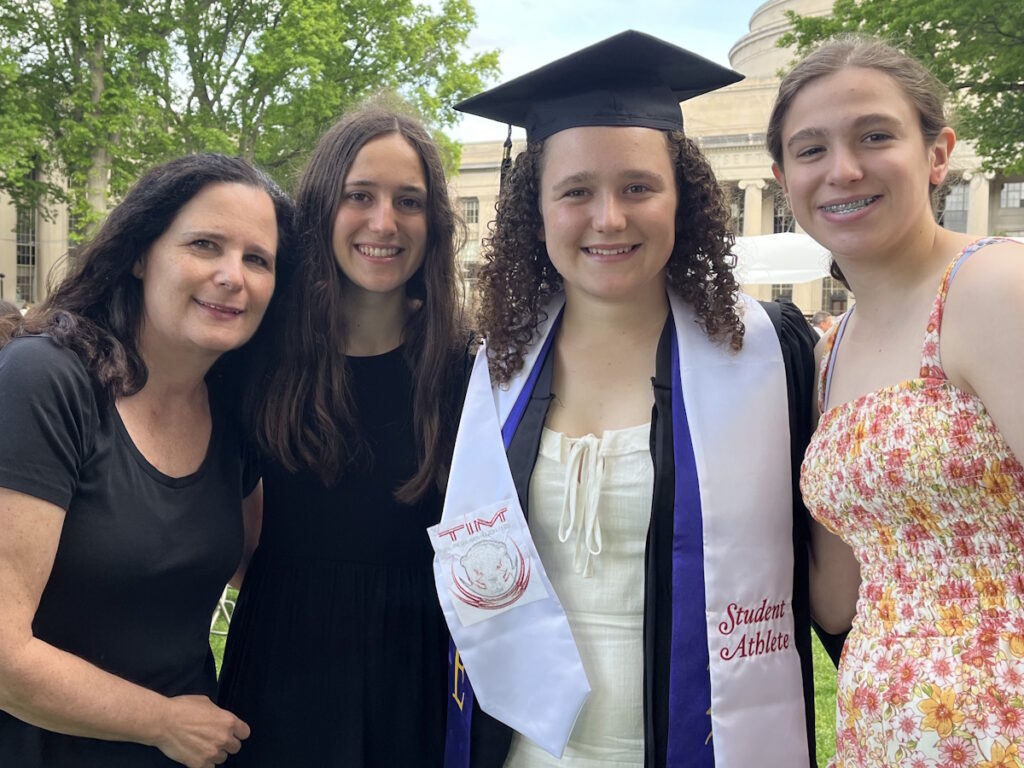Living Every Breath: Megan’s Stage 4 ALK+ Lung Cancer Experience as a Young Mom
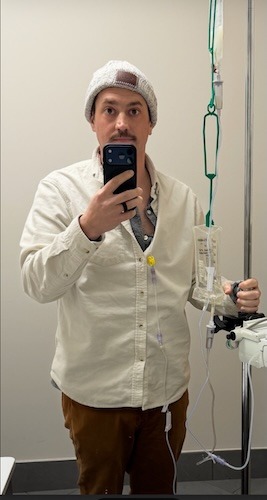
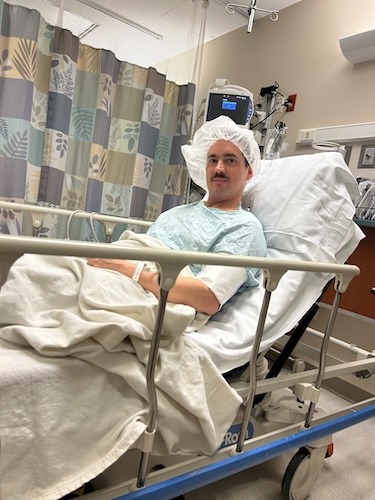
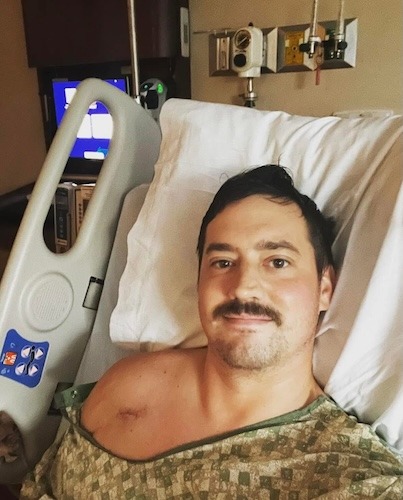
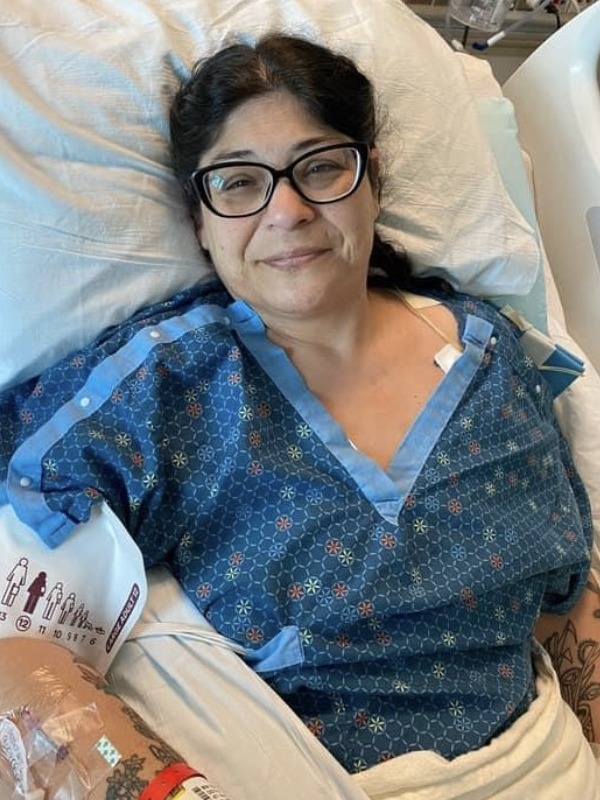
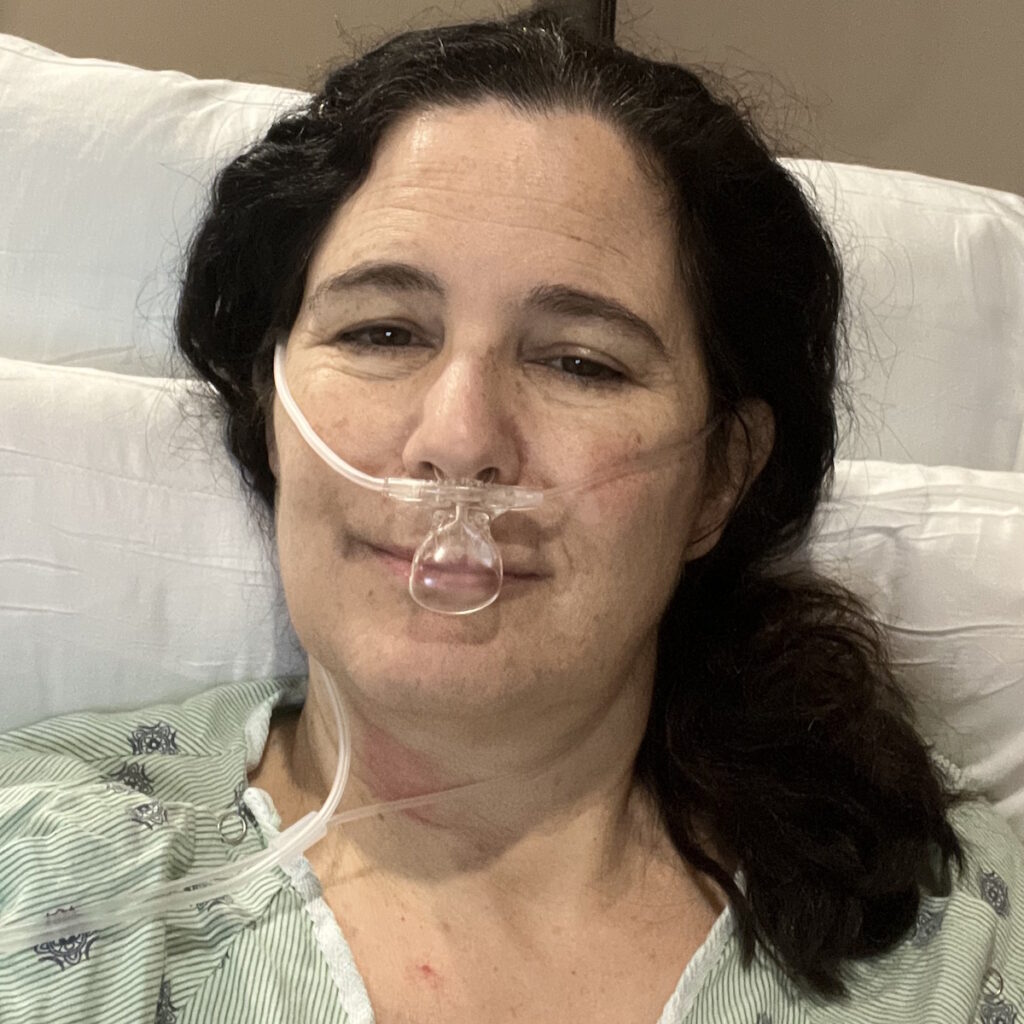
For Megan, a young mom from Massachusetts, stage 4 ALK-positive lung cancer arrived without warning. Like many people, she had no idea lung cancer could happen to someone her age, with no symptoms she recognized as warning signs. When chest pain, shortness of breath, and sudden arm swelling led to an ER visit, the scans revealed extensive blood clots, a tumor in her lung, and cancer in her spine and lymph nodes.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
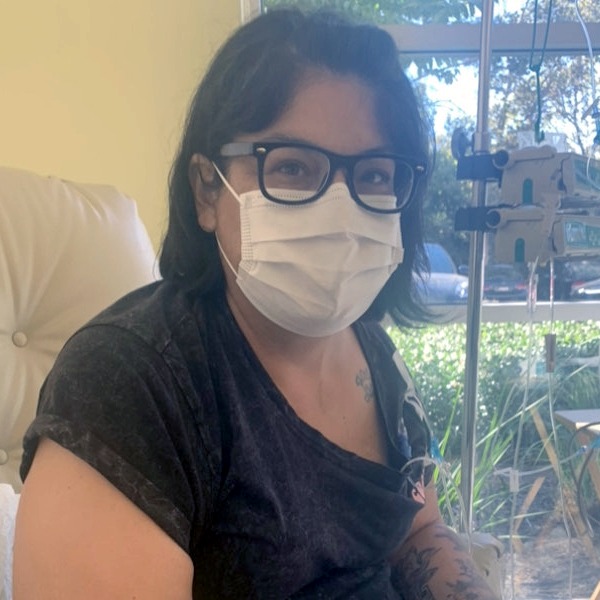
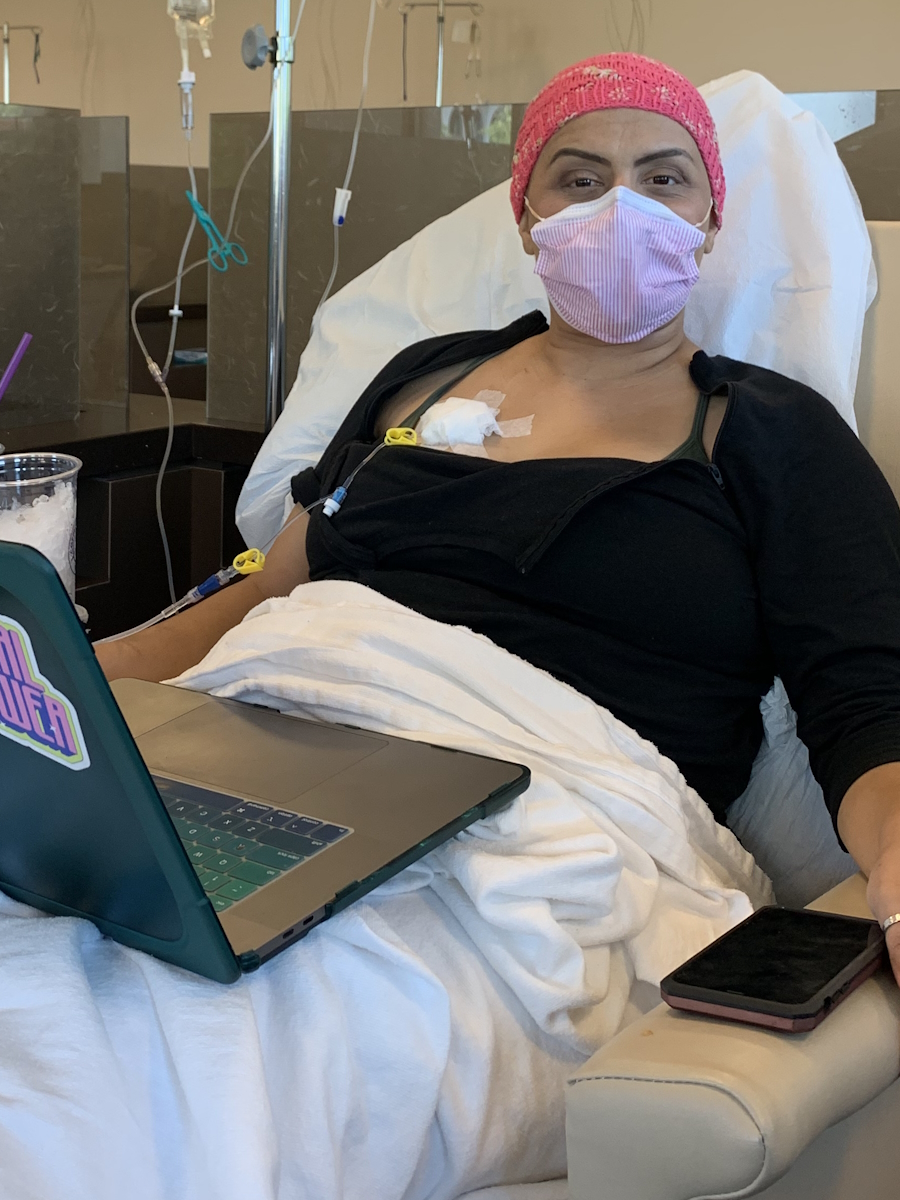
Before her diagnosis, Megan’s days revolved around breakfast with her daughters, trips to the gym, errands, and mommy-and-daughter classes. After ALK-positive lung cancer entered the picture, her life narrowed to pain management, hospital visits, and time on the couch when spinal pain made it hard to move by lunchtime. Her children, who were just one and three at the time, did not understand what lung cancer was; they just wanted their mom to read books and play. Even when a coughing fit interrupted a children’s story, Megan kept showing up for them in the ways she could.

A turning point came when testing confirmed an ALK mutation, and she met Dr. Flores, a specialist who offered targeted therapy instead of traditional chemotherapy. Within 10 days of starting the oral treatment, Megan was back on her feet, and a month and a half later, her scans showed a 40% reduction in cancer. Subsequent scans revealed more than 50% reduction and, eventually, no visible cancer to the naked eye. Today, she is considered no evidence of disease (NED) and continues taking targeted pills daily, with manageable side effects like neuropathy and bowel changes. She expects to stay on treatment long-term, and finds hope in data showing many people with stage 4 ALK-positive lung cancer remain stable for years on targeted therapies.
This experience has reshaped Megan’s priorities. Dishes and chores can wait; if her daughters ask her to play, she says yes. She is vocal about self-advocacy after initially being misdiagnosed with a pulled muscle and anxiety despite worsening symptoms. She encourages others to push for answers, seek second opinions, and surround themselves with a strong support system. With the help of her family, including her husband, who stepped into nearly every household role, and a community that sent cards and bracelets, she now channels her energy into her podcast, “Livin’ Every Breath,” where she talks about cancer, self-advocacy, and finding silver linings in hard times.
Watch Megan’s video and read her story below to find out more.
- Anyone with lungs can develop lung cancer; young people like her who have no known risk factors can be diagnosed with stage 4 ALK-positive lung cancer.
- Targeted therapy can dramatically change quality of life, as Megan went from couch-bound with coughing fits to walking, parenting, and reaching NED within months.
- Self-advocacy is essential: she kept pushing after initial misdiagnoses and used personal connections to access biomarker testing and ALK-targeted treatment.
- A strong support system, from family members moving in to help with childcare to friends and strangers sending small gifts, can lift patients emotionally through a difficult experience.
- A universal truth: many patients discover that priorities shift after a serious diagnosis, with relationships, presence, and small daily moments becoming more important than chores or perfection.
- Megan’s transformation shows how living with stage 4 ALK-positive lung cancer moved her from shock and physical limitation to renewed presence with her children, advocacy for others, and creative expression through her podcast.
- Name: Megan F.
- Age at Diagnosis:
- 33
- Diagnosis:
- Non-Small Cell Lung Cancer (NSCLC)
- Mutation:
- ALK
- Symptoms:
- Chest pain
- Anxiety
- Shortness of breath
- Arm pain and swelling
- Back pain
- Treatment:
- Targeted therapy: lorlatinib


Thank you to Pfizer for supporting our patient education program. The Patient Story retains full editorial control over all content.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make treatment decisions.
- Biomarkers and ALK-positive lung cancer diagnosis
- Why I researched lung cancer and biomarkers
- How my biomarker result shaped my treatment plan
- How biomarkers changed what I thought lung cancer looked like
- Why hope matters and how research gives it to me
- What I wish I’d known at diagnosis about biomarkers and community
- Why biomarker testing and “scary” medical terms matter
- How my doctor explained my treatment options with ALK
- Chemotherapy conversations vs. targeted therapy conversations
- How I chose my targeted therapy
- Key questions I asked about treatment and side effects
- Questions I’d tell other patients to ask their doctor
- The power of my oncologist’s encouragement
- What it meant to go from being couch-ridden to playing with my kids
- When daily mom life became something I could celebrate again
- Scan results, tumor shrinkage, and quiet celebrations
- How I cope with “scanxiety” and waiting for results
- What I knew about clinical trials before targeted therapy
- How I humanize the importance of cancer research
- What I’d say to people hesitant about clinical trials
- My go-to support and education resources for ALK-positive lung cancer
You never thought you would cheer so loudly for a genetic mutation.
Megan F., ALK-positive lung cancer patient
Biomarkers and ALK-positive lung cancer diagnosis
We found out that I had lung cancer. We Googled it, and we were obviously not happy with what Google was telling us was going to happen. Shortly after, I was linked up with the doctor that I have now, and she mentioned that they were going to test for biomarkers. Once we Googled biomarkers, we were actually relieved, because I feel like it just sends you on a different path.
I remember the exact time she called me to tell me I was ALK-positive. I was out with my family, and we were all at a restaurant, and I stepped outside. I got the news and was super excited because I know just how far ALK research has come in the last few years. When I went inside and told my family that I had the genetic mutation, everyone went crazy, and we were all laughing afterwards. You never thought you would cheer so loudly for a genetic mutation.
Why I researched lung cancer and biomarkers
I’d say that we were lucky. My husband’s cousin is an oncologist, and from the start, when I was in the hospital before we even knew it was cancer, we were already communicating with him. I was lucky to have him on my team, but he is not a lung specialist, so he did not know as much about ALK or anything like that.
It is a lot to take on at first. There is a lot out there, especially on social media. You look it up, and somebody is telling you to do this cleanse, and then this other person is telling you that you need to see this person, so it can get a little crazy. I was lucky that the doctor I have now, who is absolutely amazing, specializes in young lung patients, and a lot of them have the ALK mutation. I feel like I was lucky to connect with her early on, and the information was narrowed down from a wide scale.


How my biomarker result shaped my treatment plan
From the beginning, the oncologist that I had said, “We’re going to do this, girl.” So I had confidence that it was going to go differently from what Google was telling me it was. But, you know, first, being a young woman, the treatment that I’m on right now, you cannot get pregnant. That was part of the conversation.
I’m on lorlatinib, and as a first-line treatment, it is proven right now to be the best, although other things are in trial. If you get on that right away, it is the most effective. It does have the harshest side effects. So that was a conversation: you have to weigh your pros and cons. If I wanted to get pregnant, I would have had to go on a different medication. Luckily, at the time, I had a one-year-old and a three-year-old. They’re now two and four. We were totally fine with, “That’s our family. Let’s take the best line of treatment.” So we just went with it.
How biomarkers changed what I thought lung cancer looked like
I thought lung cancer looked like two to four months, and obviously, it was not a good two to four months. I thought I was going to be thrown into chemo and just see how long I could last.
Once I found out that I had the genetic mutation, I knew that there was treatment out there, targeted therapies. Mine just came out in 2021, actually, and more than 50% of people on my medication after five years still have no progression. I just thought, “That’s huge.” At the time, I was like, “Yes, five years.” I have five years now. I don’t have four months anymore. Now, the more that I’ve educated myself on it and the more chats that I’ve been in, I see people 20 years out. So I no longer limit myself to five years, although at the time, that sounded wonderful.
To really understand and to be an advocate for yourself is so important.
Megan F., ALK-positive lung cancer patient
Why hope matters and how research gives it to me
From the start, I have always had hope. Now, it is easy. I have no evidence of disease.
Of course I am hopeful. Day to day, I don’t really even think about cancer, so that’s great. But even when I first got diagnosed, and I was on the couch because of back pain, and I couldn’t even finish a sentence in my kids’ book, even then, I was hopeful, just looking at the future and the research and the medicine that is coming out. I know there’s some in the works right now. It is hard not to have hope.
What I wish I’d known at diagnosis about biomarkers and community
I was hesitant to join the chat rooms at first. I just think knowing that there is someone out there who has stage 4 lung cancer and they’ve been on medicine for 20 years, and they’re thriving… just knowing that would have been great.
You have to kind of search through the bad to find the good, and when you’re first diagnosed, I feel like that’s not beneficial to you.


Why biomarker testing and “scary” medical terms matter
I think that people should care because it really helps form their treatment, which is obviously the most important part of a cancer diagnosis. To really understand and to be an advocate for yourself is so important.
I am blessed to have a doctor who fights for me. I know even when I’m not present in her room, she’s out there researching. But not everyone has that connection to their oncologist. For your own research, you need to know these words. I joke that there should be a dictionary out there. There should be a cancer dictionary, because even words like “hospice” sound really scary. If you look at them down to the core, they’re really all here just to support us in our lives.
How my doctor explained my treatment options with ALK
She said, “I think you should get on it right away.” Once we decided that was the path I wanted to take, that that was the medication, she said, “Let’s start it.”
I did start at a lower dose, because the side effects could become really harsh. Luckily, I didn’t experience the really harsh side effects, just nausea and other things that I wish I wasn’t going through, but they weren’t that bad in the grand scale of things.
Ten days after starting the medication, I went from being couch-ridden and unable to breathe to playing with my kids in the backyard.
… just looking at the future and the research and the medicine that is coming out… It is hard not to have hope.
Megan F., ALK-positive lung cancer patient
Chemotherapy conversations vs. targeted therapy conversations
When I was originally diagnosed, I was in the emergency room. I talked about chemotherapy with the oncologist I was first linked up with, but I didn’t end up going with them. My first appointment was basically, “We’re probably going to end up with chemo, and we’ll see how long you can tolerate it.”
Later, when we started talking about targeted therapy, the conversations were so different. I also had two different oncologists, and that made a huge difference. My first conversation, when chemotherapy was introduced, was kind of sad. That was the way it was presented to me. There wasn’t a “We’re going to do this, girl.” I personally had hope either way. I was like, I’m 32 years old. This can’t be the end. But there was definitely positivity and an uplifting part of the conversation when biomarkers were talked about.
How I chose my targeted therapy
Honestly, the research decided it for me. I was ready to take on whatever side effects came with something that was going to potentially eliminate my cancer.
Just looking at the research out there, I also have a couple of lawyers in the family, and I sent them the information. They read what the medication does and how amazing it is. Everyone I talked to said, “You need to go with this. This has the best response rate.” That’s why we went with it.
Obviously, I have kids, so that would have been a big decision if I still wanted to have a family. I feel like I was blessed to be on the other side of that. Other than that, it was: whatever is going to get us the best results.


Key questions I asked about treatment and side effects
I wanted to know the results — how many people have had success with that medication and for how long. I also looked into neuropathy as one of the big side effects, which I did end up getting. Luckily, it was not as bad as some other people’s.
We were able to change the dose. Those were my questions: if we run into this side effect, what do we do? A lot of it was just changing the dose. Because I had a good response to it, it was easy to adjust as we went.
Questions I’d tell other patients to ask their doctor
It depends on the individual, but I would say to ask your doctor about pregnancy if that’s important to you. That’s one of the big things you should be asking about. Also, ask how to deal with side effects. I would ask ahead of time, “What are the side effects, and if these happen, what do we do?” You might be at your house, and of course, your oncologist is a phone call away, but if you’re experiencing neuropathy for the first time, you’d be like, “What is going on?”
If you already have in your mind how you can handle these steps, it’s more comforting. I’d also ask what supports are out there. You’re going to be taking this medication; there are Facebook pages, and the drug itself has support groups. If you have access to those, then maybe you don’t even need to call your doctor in a panic, because you’ve already educated yourself, and you have chat rooms and forums to go to.
Ten days after starting the medication, I went from being couch‑ridden to playing with my kids in the backyard.
Megan F., ALK-positive lung cancer patient
The power of my oncologist’s encouragement
My doctor asks if it’s OK to share my story with other patients. She’ll say, “I just got someone your age. Can I tell them about you?” I think that’s super helpful, because she did that with other patients for me as well. She’d say, “I’ve got someone’s permission to tell you this. They’ve been on your medication for the last five years. They’re doing great.”
I remember specifically, once I responded well to the treatment, she called me and said, “Lorlatinib is your drug,” and I was like, ”Yes, it is.” She’s always positive and always coming in with uplifting phrases.
What it meant to go from being couch-ridden to playing with my kids
It was really hard. I was a stay-at-home mom. I was looking to go back to work because I was like, “This is so hard,” because every day I felt exhausted.
Being a stay-at-home mom is hard, but it was different with stage 4 lung cancer, and I had no idea. From the diagnosis day to the day I took my medication, because there was about a month in between, it was just so hard.
My in-laws are amazing. They flew home and stayed at our house or at my sister-in-law’s down the street. My mother moved in, and my dad would come to and from work. I had all this help, but I wanted to be a stay-at-home mom. I wanted to play with my children. Watching everyone else was so beautiful and awesome that they came for me, but it felt like I was watching from the outside of things that I wanted to be on the inside doing.


When daily mom life became something I could celebrate again
I remember specifically, at that time, I had a one-and-a-half-year-old, and of course, they throw tantrums. During every tantrum, I was like, “That’s fine, everything’s fine.” I was almost happy about the tantrum. Just being involved in it was so awesome.
I don’t even remember the exact day-to-day; I just remember that on the tenth day, we were running around outside, and I thought, “How many days ago did I start this medication? This is crazy.” When we went back and looked, and realized that I had started just ten days before, I just couldn’t even explain how happy I was.
Scan results, tumor shrinkage, and quiet celebrations
When I had my scans a month and a half after I started the medication, I had a 40% reduction in cancer. My next one was even better; it was more than 50% gone.
At first, the big medical terms came through in the report as a message before the doctor called. We had to Google everything in there, because if you change a couple of letters in some of those words, they’re actually bad. We had to make sure we saw what we thought we saw.
We were ecstatic. I remember we read it in my husband’s office, and we were just silently dancing. We had gone in and shut the door, with all the family out there. I don’t even think we told them we were going to read it. We celebrated, and then we talked to our oncologist. She was so excited for us, but it almost seemed like she couldn’t believe it because it was so quick. A lot of people have this response, but it’s over a year or two. She seemed shocked by it, too, which was even more exciting.
When I had my scans a month and a half after I started the medication, I had a 40% reduction in cancer. My next one was even better; it was more than 50% gone.
Megan F., ALK-positive lung cancer patient
How I cope with “scanxiety” and waiting for results
Do you know the song “Good News” by Shaboozey? That’s our family song. It came out around the time that I was diagnosed, and now every time we’re going into a scan, we play “Good News,” because that’s what we need. So far, he’s come through.
I would say I live my life in three-month intervals. I have a scan, it looks really good, and then you’re fine for about two and a half months. Then, for the two weeks before the scan, you’re like, “Everything seems okay, but is that little pain something?”
For me, the day of the scans is fine. It’s the waiting for the results that causes anxiety. Last time, my husband and I went and shared some lunch, but we didn’t eat it. We just sat at the table and didn’t really speak. We just had the food in front of us and waited for the results to come through. That’s when I get the anxiety — afterwards.
What I knew about clinical trials before targeted therapy
Nothing. I honestly didn’t even think I could get lung cancer. You see the commercials with people who can’t speak, and I had never smoked in my life, so I thought I couldn’t get lung cancer. I didn’t even know it was something I could get.
Once I was diagnosed, even Googling it right off the bat, they don’t really break it down for you and tell you everything. It wasn’t until I got connected with this doctor, who said we would test for biomarkers, that I started doing the heavy research into what it could possibly be.
There are multiple mutations. I was most hopeful for ALK because I saw that there were already three generations of drugs out, and they’re working on a fourth. I hear things in other countries that are maybe coming along the line. It seemed like there was a lot of research and time put into ALK. But I know there are others out there, and they’re also coming up with treatments, so I’m happy for everyone in the targeted therapy community.


How I humanize the importance of cancer research
I actually spoke at Foundation Medicine, which is the company that does biomarker testing. I said, “You know, there are all these people in the lab, and they’re creating this drug or the latest thing. I’m at home planning birthday parties, and I’m at home running around in the backyard with my kids. This research is great on paper, and it’s great data, and it’s clearly doing us well, but I see it as more time. I see it as more hope, more tantrums that I can celebrate.
What I’d say to people hesitant about clinical trials
I’ve learned that there is extensive research that goes into a drug before it even becomes a real clinical trial that you can enter yourself into. Only a couple of years before I started taking my medication, it was also the subject of a clinical trial. There’s one out there now, and I’m in plenty of groups. A lot of people are responding even better than with the one that I’m on.
As I said, it’s all about time. I have stage 4 lung cancer with an ALK mutation. My cancer is constantly trying to get smarter than my therapy. You never know when that’s going to happen.
My next line might be a clinical trial. The reality is, if something happens in the next couple of years, that’s my next line. I understand that it’s scary, but looking at the research and the science and how far we’ve come, I fully put my trust in it.
My go-to support and education resources for ALK-positive lung cancer
I use the Young Lung group a lot. They were a community I joined early on. I would also say ALK Positive. If you go to their website, they have a lot of good forums and places where you can find other ALK‑ies. They also have a Facebook group for patients and their supporters. Other than that, I’ve found other ALK-positive people through Instagram.
To anyone newly diagnosed, I’d say don’t get discouraged, because there are a lot of people out there who might have, you know, drunk only green juice for three weeks, but they also probably responded well to a treatment. Sometimes it can get scary when you’re following someone on social media, so just be wary that it’s social media and you don’t know the whole story.
This research is great on paper, and it’s great data, and it’s clearly doing us well, but I see it as more time. I see it as more hope, more tantrums that I can celebrate.
Megan F., ALK-positive lung cancer patient


Special thanks again to Pfizer for its support of our independent patient education content. The Patient Story retains full editorial control.

Inspired by Megan's story?
Share your story, too!
More ALK-Positive Lung Cancer Stories
Megan F., Non-Small Cell Lung Cancer, ALK+ Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
Clara C., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Pelvic pain and discomfort, bladder issues related to pelvic tumors, incontinence, pain in the lower back and hip
Treatments: Chemotherapy, immunotherapy, radiation therapy, targeted therapy (lorlatinib)
Stephanie K., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent and intense cough, general feeling of sluggishness
Treatments: Chemotherapy, targeted therapy through a clinical trial, radiation therapy
Ruchira A., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Mild intermittent cough while talking, low-grade fever, severe nonstop cough, coughing up blood, collapsed left lung
Treatments: Surgery (lobectomy), targeted therapy
Laura R., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent cough, fatigue, bone pain
Treatments: Targeted therapies (tyrosine kinase inhibitors or TKIs, including through a clinical trial)