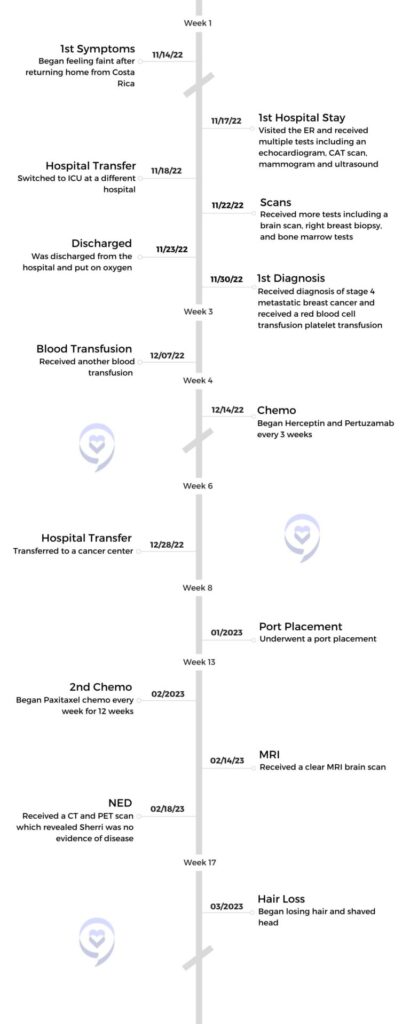
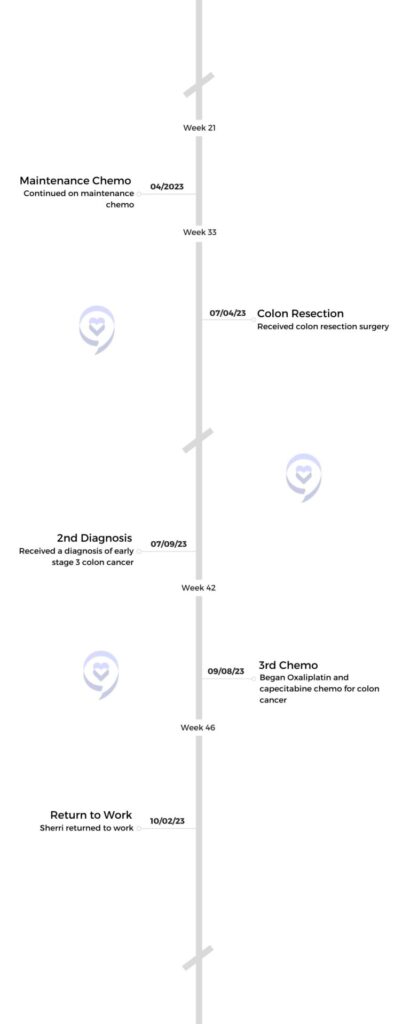
Sherri’s Stage 4 HER2+ Metastatic Breast & Stage 3 Colon Cancer Story
After retiring from the Air Force, Sherri became a mental health therapist and ran a private practice while being a mother to her three children. Feeling burnt out, she took a week’s trip to Costa Rica and noticed feeling out of breath.
This feeling continued when she returned home which led her to the ER where doctors discovered her oxygen levels and blood count were extremely low. After many tests and exams, a mass was found in her breast. Soon after, she was diagnosed with stage 4 metastatic breast cancer.
Sherri was put on 12 rounds of Herceptin chemo and began transfusions. Three months after her breast cancer diagnosis that had spread to her bone marrow, Sherri was no evidence of disease. However, doctors wanted her to undergo a colonoscopy after finding blood in her stool. The colonoscopy revealed early stage 3 colon cancer unrelated to her breast cancer.
Today, Sherri is currently undergoing Oxyplatin chemo and transfusions for colon cancer. She shares her story with us, including how she deals with anxiety, how cancer has catalyzed inner healing, her experience with chemo and its side effects, starting a podcast to spread hope, and her advice to those on their own cancer journeys.

- Name: Sherri O.
- Diagnosis (DX):
- Breast Cancer
- Metastasized to bone marrow
- HER2+
- Breast Cancer
- Stage: 4
- 2nd Diagnosis (DX):
- Stage: 3
- Symptoms
- Shortness of breath
- Lump under armpit
- Not feeling herself
- Treatment:
- Chemotherapy
- Pertuzumab
- Herceptin
- 12 rounds
- Oxyplatin
- Every 3 weeks
- Transfusions
- Chemotherapy
There’s not enough hope and inspiration. That’s what I want to give to the world.
Sherri O.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Symptoms & Diagnosis
Tell us about yourself

My name is Sherri and I am a single mom. I have 2 adult children, which is so weird to say. I have a daughter who just turned 21 in August, my other son is 19, and I have one left in school. He is a senior this year and he’s 17.
I served in the Air Force for 23 years and retired in 2017. I’m not really active in this now because of everything that happened in the last 9 months, but I became a mental health therapist. I went back to school in my 40s, got my master’s in clinical counseling, became a therapist, and ran a full private practice for about 5 years.
I have a dog named Chief and we also have a bird my daughter named Pickles. We have a cat named Maui. I had a house built a couple of years ago. We’re living in a farming community in Colorado, which I love.
What were your first symptoms?

Hindsight is 2020. I was having signs of some things that were off that I was downplaying. I thought I was healthy. I was working out, I was running my business, and I was feeling a little bit burnt out so I decided to take a trip to Costa Rica. I thought this was going to be great. I’ll take some time away from my business, settle down, and do some unwinding in a beautiful place.
I went for about a week. I did notice when I was there that I was out of breath a lot more. I was like, it’s probably the shift in altitude or maybe it’s jet lag. I went on a little bit of a hike and I was out of breath and it wasn’t too bad.
I didn’t really have anything significant happen until I got back, which is a blessing in disguise. I was walking up to the post office and I was carrying a couple of boxes and I thought I was going to pass out. My heart started beating really fast and I was like, okay, there is something really going on here. I might have a virus or something.
Taking a trip to the ER
I met one of my friends for brunch and I said, I just don’t feel right. I feel off. I’m not sure what’s going on. I came back home and I called the nurse triage line and I was telling them my symptoms. She was like, “You need to go to the ER,” so I went. I drove myself to the ER because I thought that I picked up a virus or something from Costa Rica.
I got to the ER and they were like, “Your oxygen is at 70. You have to stay here.” It was very weird. It was a whirlwind of things going on. They did blood tests and they they said that my platelets and my hemoglobin were tanking. I needed a blood transfusion. I need a platelet transfusion. It was very weird for me. I was like, What? This is insane. I felt fine two days ago.

I started getting transfusions, they admitted me to the hospital, and they were like, we don’t really know what’s going on. They did find a mass under my right breast because they were turning over everything and they were testing me for everything. We needed to do a mammogram and sent me to another hospital.
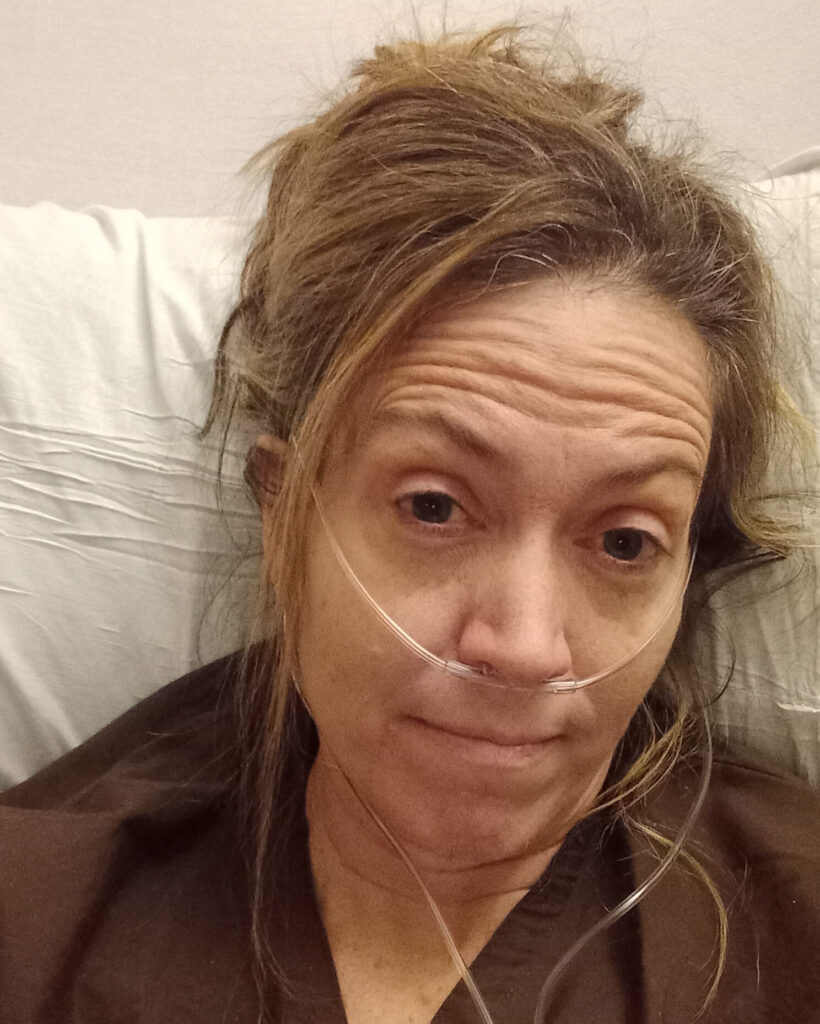
What was your diagnosis?
I got transferred to an ICU in Denver and they ended up finding out that the mass under my right breast was cancerous, and the reason why my blood was tanking was because it had metastasized to my bone marrow. After Thanksgiving, they diagnosed me with stage 4 metastatic breast cancer. That was the beginning of the whirlwind story. This was November of 2022.
Did you suspect you had cancer?
It’s not anything that crossed anybody’s mind. In fact, the doctors were very focused on a parasite, on a virus, because I’m pretty healthy. I’m 52 now and I’ve always been in good shape. They were very perplexed as to what was going on. They did a really good job though of turning over everything. They tested me for everything you could think of. That’s what it ended up being, unfortunately.
Did you ever feel a lump?

They ended up finding out that the mass under my right breast was cancerous, and the reason why my blood was tanking was because it had metastasized to my bone marrow.
No, I didn’t feel anything. In fact, my last mammogram, they were like, “Your breasts are very dense.” I guess the older you get, your breasts get more dense and I never felt anything. I also had a swollen lymph node in my armpit and I just didn’t recognize any of that.
Again, hindsight is 2020 and it’s really important to check those things and to pay attention to your labs. That was one of the big things I’ve learned is that I was anemic. I had been anemic for a really long time and I just didn’t do anything about it because I just listened to what the doctor said. They’re like, “You’re fine as long as it doesn’t go below this number.” However, I think it’s really important to look at those things and to go, okay, what could I do differently to get out of anemia? It is possible to not be anemic, because I’m not anemic now, which is crazy because I was anemic almost all my life.
Processing A Cancer DX
How did you react to your cancer diagnosis?
I didn’t. My sister was with me at the time they said that. I knew it wasn’t good, and they also said it was aggressive. They use that actual word. I just left my body. I think that being in mental health, we can go into fight or flight or freeze. I totally froze. I don’t think I was even in my body, to be honest with you. I left the building, basically.
My sister cried, and she said, “You didn’t even have a reaction.” It wasn’t hitting me. It didn’t hit me until way later. I think it took me a couple of months to really get out of the fog. Part of it was I had low blood count, so I had no energy. I was tired, I could barely walk from the couch 5 feet to the kitchen, that’s how tanked I was. I think part of that was why I didn’t have a reaction is, I was in a fog and I only wanted to rest and everything was wearing me out.
It wasn’t until a couple of months later that I attended a support group, which I wasn’t ready for. It was people that had been going through cancer and they were all younger than me. Very young. They were all at different stages. I was the only stage 4. I’m listening to their stories and I’m like, I’m doomed because they had all gone through all these things. I’m like, well, what about me? I’m stage 4. I don’t even have a chance. That’s how I was taking it. What I learned from that was, that my story is different than their story. We don’t all have the same story.
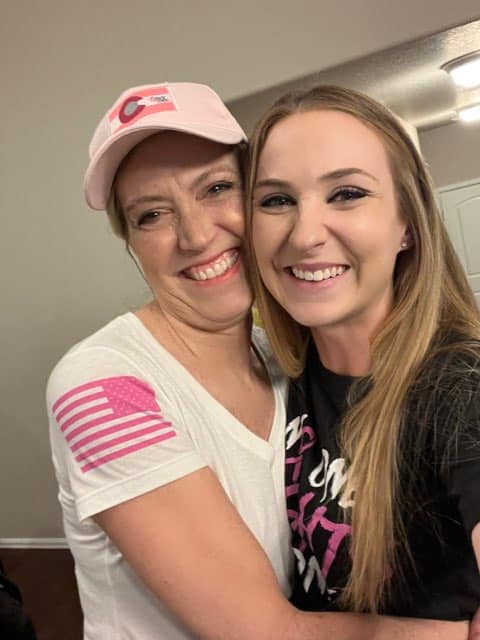


I totally froze. I don’t think I was even in my body, to be honest with you.
Learning to accept a cancer diagnosis
I had a massive breakdown, which I think needed to happen. Coming out of that, that was when I came into acceptance. I was accepting that this was what was happening and what can I do now.
The other important piece is that I’m still alive. I’m here, I’m not dead yet, so what can I do now that I’m here in this moment? I can succumb to it. Or I could just live. I started to put one foot in front of the other and go, I’m alive and I’m going to make it count. I believe that mentality has been so crucial to my healing. I don’t think I would be healed if it wasn’t for that piece of it and the attitude.

What were the first steps in your cancer treatment?

The first part was I had to have my blood levels at a certain point before they would do anything with me. They wouldn’t treat anything, they wouldn’t do surgery, nothing. They didn’t want to touch me because my blood counts were so low. To put it into perspective, my platelets were about 20,000 and to be at a healthy level, you need to have 150,000. I wasn’t even close and they were not going up very fast.
I started to get really diligent about seeing the numbers go up in my mind. I asked, what number do I need? You need at least 90,000. I started to picture 90,000 and then it happened. Then every time I would ask, what do I need next? I would visualize it and then it would happen.
Pretty soon they put me on a targeted treatment and pertuzumab and I started to get better. I kept getting better and better. Even the blood transfusions helped me to get better as well. I ended up transferring from VA in Denver to Banner MD Anderson and then they started me on Herceptin and I was on that for 12 rounds of chemo. I lost my hair. I had really long hair, and now it’s growing back, which is great.
Reframing a cancer diagnosis
I’ve had such great care from VA to Banner, everybody has been so good to me and so supportive. Sometimes the language would get to me. One of the doctors said, “It’s aggressive, you’re really sick.” She kept using those types of words and I was like, I have to switch that in my mind because if I focus on that, I’m going to be depressed. I started saying, that’s an opinion. A diagnosis is an opinion also. What can I do differently within my body, myself, and my mind? I started visualizing myself healthy and on that track, and I just kept getting better and better. Language is everything. Your words, the things that you say, really do matter.



Realize that stage 4 is not the end. I think when you hear cancer, at least when I used to hear the word cancer, I’m like, that person’s just done. It’s just not true. It’s a misconception. I’ve learned that you can still live a long time.
There’s so much misinformation. When I was first diagnosed, I was like, I got to figure this out. I started going on all kinds of crazy diets and supplements to have some sense of control. I let go of that and realized I didn’t need to do all this crazy stuff. I’m going to be okay. I’m going to live in the moment as much as I can. The truth is that nobody knows our timelines, even a doctor doesn’t really know. They can speculate. I think the most important thing is listening to yourself, and listening to what your body is saying to you, is key to the whole thing.
I’m here, I’m not dead yet, so what can I do now that I’m here in this moment?
Healing the heart

One of the things that has come up for me with all of the cancer stuff is that there were things in my body that needed to be healed. It sounds a little weird. However, I will ask my body, what does this mass mean to me? What is it wanting to tell me?
I’ve healed so many mother wounds and nurturing that I was missing. The breast is all about nurturing yourself. I wasn’t taking good care of myself like I thought I was and giving myself what I needed. I remember somebody asked, “Well, what do you need?” I automatically was like, I don’t need anything. I didn’t even check in with myself to ask myself what I needed.
Remission
Taking a sabbatical to focus on health
That’s been a whirlwind too, all the appointments. At the beginning of it, I was looking at my calendar and I was like, there are so many appointments. How is this going to work? I decided to put myself on a sabbatical, which was one of the best things I could have ever done for myself, to just stop everything else and really focus on my health.
Did your body have a positive reaction to cancer treatment?

For stage 4 HER2+ breast cancer that I have, I have to do an infusion every 3 weeks. I’m still on that every 3 weeks. I’m not done with the chemo for the breast cancer and I have had 3 PET scans since November.
I will tell you the good news, which is that the first scan was awful. They said that my bones were riddled with cancer and that it was not going away. That was in November. Then I had a scan 3 months later, in February I believe, there was no evidence of disease in my body. In that short amount of time, I have no evidence of disease in my body. Even I was like, are you sure? I was questioning it.
I had the same reaction I had when I got the diagnosis. I was numb. I didn’t have a reaction because I just didn’t believe it. I was like, how is that even possible? Two weeks later, I brought a friend with me and I said, “Can you listen for me? Be my ears?” That’s one thing I’ve also learned is you need to have an advocate. Because as a patient, you hear things totally differently than somebody outside of it. I think that’s important.
Becoming NED
I asked the nurse, “Do you call that remission? What do you call this?” She said, “No, there’s no evidence of disease.” They showed me on the scan that the mass and the swollen lymph node were gone. It still blows my mind. Those scans are every 3 months. I just had another one a couple of weeks ago and that one is also clean. There’s no evidence of disease on that one.
I had a fractured rib in January. They showed a fractured rib and they had some other stuff on the bottom of my ribs and those are completely healed as of this last scan. So the doctors are like, “You’re doing great. Your body is healing.” My infusions are every 3 weeks, which at first I was like, that sucks. However, I don’t have a lot of side effects from that infusion at all. It’s just like going and getting vitamins to me. I’m not going to lose my hair from it or anything like that.

Did you have side effects from chemo?
The chemo that I got, Herceptin, the side effects were feeling very heavy and I did a lot of resting. I didn’t have any nausea or anything like that. I didn’t have a lot of side effects. It was mainly just heaviness and wanting to lay down a lot. I didn’t do a whole lot during those 12 rounds. They were every week, so I was pretty tanked. When you do chemo, your blood levels tend to go down. I was in and out of anemia, like a roller coaster. I rested a lot during that time. I didn’t do a whole lot of anything. It wasn’t bad, it was just a blah feeling.
»MORE: Cancer Treatment Side Effects
2nd Diagnosis
A couple of days later, the doctor who did the colonoscopy called and said that it looked like I had cancer. That was really shocking.
Receiving a second cancer diagnosis
The good news about the [breast cancer] diagnosis is that I’ve had 3 scans. The last 2 scans showed no evidence of disease, I didn’t have to have any sort of breast surgery, the mass that was under my right breast disappeared, and I had a swollen lymph node in my armpit that is gone. The last scan was 2 weeks ago, so this is about 9 months after diagnosis, which is incredible. I was no evidence of disease on the last round of chemo treatment that I had for breast cancer. I got to ring the bell, which was awesome.
When I first went into the hospital for breast cancer, they tested my stools. They were testing everything. In January, they found traces of blood in my stool. The oncology team didn’t want to do a colonoscopy because I was in a very vulnerable state, body-wise. They wanted to wait until after I had done the 12 rounds of Herceptin. I did all of that and I waited a little bit. Then I got scheduled for a colonoscopy and did that procedure. A couple of days later, the doctor who did the colonoscopy called and said that it looked like I had cancer. That was really shocking and I did have a breakdown right away. I reacted a lot differently than I did the first time.
The first time, I was very numb. The second time, I was really mad and upset. I did have a meltdown. Then I came out of that and I was like, okay, I don’t know where it is exactly. I didn’t have a stage yet. They wouldn’t have been able to tell me that until after the surgery. They scheduled surgery. I had a polyp that they had to remove, and I also had something in my rectum. However, they wanted to break it up into 2 different surgeries. The one in the rectal area was not cancerous at all. They took the polyp out, they tested it and it was cancerous. They also tested 35 lymph nodes. Out of the 35 lymph nodes, 2 of them were positive for cancer. They classified me as very early stage 3 colon cancer, which is totally separate from the breast. Now I’ve got the breast cancer under control and have been diagnosed with colon cancer.

»MORE: Cancer Surgery Treatments
How long after your first diagnosis did you receive your second diagnosis?
I was diagnosed in November with metastatic breast cancer, then I was diagnosed with colon cancer in July.
Did you suspect you had cancer again?
I kind of suspected it. Again, when you’re looking back at something, it’s easier to see it. When you’re in it, you don’t really see it. I had downplayed some of my symptoms. During pregnancy, I got hemorrhoids. I have had those off and on. A lot of times there’s a little bit of bleeding that happens when you go to the restroom but I was like, it’s just hemorrhoids. It’s no big deal. It wasn’t, it was actually colon cancer.
If I don’t do it, it’s a 50% chance that it will come back. If I do the treatment, then it’s a 10% chance. It’s better if I do the treatment even though I don’t want to do it.


I just kept downplaying my symptoms. It was a good thing that they did test that and caught it when they did. There’s a test that I highly recommend people get. It’s a Signatera test where they actually test if there’s any residual cancer in your bloodstream. I did the lab, and I did the blood test prior to the surgery and it was positive. That means that there’s cancer in the bloodstream. Then they said, “We’ll test you again afterward.” They tested me again after they took it out and it was negative, which is really a good sign that it’s not going to come back.
Did you go back on chemo after your colon cancer diagnosis?

To prevent reoccurrence, they wanted to do more chemo, which I wasn’t really happy with because I was like, I just got through this thing. I don’t want to do this again. I was in complete resistance to it. I had to really listen to my doctor. I said, “I don’t want to do this. What’s the risk-reward?” Basically, it’s 50/50. If I don’t do it, it’s a 50% chance that it will come back. If I do the treatment, then it’s a 10% chance. It’s better if I do the treatment even though I don’t want to do it. I made the choice to do it. I started it 3 weeks ago and it’s added to the infusion that I’m doing. The good news about this is that it’s only 3 months. I’m currently on that now.
Do you have a family history of cancer?
I don’t have anything genetic. I did the genetic testing and I don’t have the BRCA1 gene for breast cancer, so I don’t know. I’ve been investigating it a little bit and I’m convinced that it’s environmental. However, I don’t really know. I don’t know how to prove that. I don’t have any idea.
It is very odd that they’re 2 different separate cancers. I asked, “Is it because of the breast?” They said, “No, it has nothing to do with it.” I’m not a doctor, so I don’t know how they know all this. My instinct is that it’s environmental. I was in the military for a long time and I was exposed to fumes and asbestos and different things like that. It could be that, but I don’t know.
Quality of Life
Have you experienced side effects from your current chemo treatments?
I’m on Oxyplatin and that will be every 3 weeks. I did the first round not that long ago and my side effects are a lot different. I wasn’t expecting that. I was like, I got it. This will be a piece of cake. No, it’s actually way different. I have a lot more nausea with this drug. I have one of the things that Oxaliplatin does when you touch something cold, it burns or stings like frostbite. I do have that tingling in my fingers. I have a sensitivity to my jaw when I eat anything, it has to be very warm. Anything remotely cold sends a shock to my jaw. Sometimes I’ll have tingling in my hands and feet. That’s not too bad. The biggest thing is the nausea. It doesn’t feel great.

I eat a lot differently than I used to. I eat a lot more. I’ve actually gained weight this time, which is great because when I started the breast cancer treatment, I was 145 and I dropped to 120. When I found out that I needed to go into another round of treatment, I was like, I got to get my weight back up. I started eating differently. I went plant-based. However, I ate a lot more rice, potatoes, and carbs so that I could gain weight.
I started working out more, which has helped me tremendously get through this chemo. I’m going into this one a lot stronger. I think that the side effects are like 2 or 3 days. I haven’t had the tingling, the cold stuff doesn’t stay around. That’s been a good sign I can do this, I can get through this. I’ll be on this treatment for 3 months.

Has anything helped with the nausea?
Bananas and yogurt, for some reason, seem to be my thing. Walking and exercise actually really help with it as well. There’s an app called Couch to 5K, so I’ve been doing that. It’s basically interval training. It’ll be walk 5 minutes, run 1 minute, walk 2 minutes. It has really helped me a lot. I’ve been running a little bit more, which has been really great. I have more energy because I do that. The weight training has helped me gain weight back.
Describe prep and recovery for your surgeries
The first one, the prep was that I had to do 5 days of Ensure shakes, and that was a little rough for me because I had eliminated sugar from my diet. I didn’t eat a lot of sugar because sugar just caused my body to be more inflamed. I had to drink those for 5 days. It was 2 drinks a day and so many calories. That was the prep for the surgery. I had to do some fasting before. That surgery went really well.

I was in a lot of pain coming out of it because it was a colon resection. They took out part of my colon and resected it, put it back together. I had a very non-invasive surgery. They did robotic laser surgery. You can’t even hardly tell that I have scars, which has been really nice. I am so grateful for technology now because, if this had been in the 80s, I might not be here. We’ve come a long way in science and how much we’ve advanced. The recovery time, I was in the hospital for 5 days after that one.
Then they did the other rectal surgery separately because they just thought that doing both of them wouldn’t be a good idea. I agree because the second one was very painful to go to the bathroom. That was only a day’s procedure. I was in and out of the hospital the same day. However, my recovery time for the second one was a lot longer because of where it was. That one was a little tough for me.
I bounce back pretty fast. I think part of that was because I had gone into it with my body a lot stronger. I had gained more weight. I was exercising. I bounced back quicker because of that. They told me, “It’s going to take 6 weeks [to recover] for both,” and it was really minimal. It was maybe 3 weeks for both, so half the time.

Did you have a colostomy bag?
No colostomy bag, Nothing like that. I do have to go back and get a scope just to make sure they got everything in a couple of months. I did the blood test again, the one that I did prior to when they found out I had it. It was positive for cancer. I just did it again and it’s negative. It’s a really, really good sign and now we’re on treatment to keep it from reoccurring.
How often are you receiving scans?
I just recently did the PET scan. I’m not sure if they’re going to move me to 6 months since the last 2 were clear. With scans, you’re putting yourself in radiation, so you have to be mindful of that. I don’t know if I’m going to be every 6 months or not. I’m assuming that’s what’s going to happen. I’ve had to have some brain scans just to make sure that breast cancer doesn’t metastasize to my brain. I probably have one of those coming up. Those are every 6 months. The more you’re healing, the less you have to do.
Reflections
Do you ever experience scanxiety?
I did go through that this last time, actually. I went through it more this time than I did the last time. The last time I was like, it’ll be what it is. I just didn’t really think about it too much. This time, I just really want a clear scan again. When you get your labs done, they look at all the cancer markers and everything has been good.
I did have a lot more anxiety come up this time, which was very interesting for me. I was walking it out and I’m like, I don’t know what I’m afraid of. I just started to ask questions. I think to alleviate anxiety is to face it versus running from it. A lot of times with anxiety it’s like, I have anxiety, I’m so anxious, take a deep breath. Well, that doesn’t really get to the root of it.
Facing anxiety
To alleviate anxiety is to face it versus running from it.
What helped me was asking really good questions like, what are you afraid of? I’m afraid it’s going to come back. If it’s going to come back, then what are you afraid of? I’m afraid I’m going to die. If you die, what else are you afraid of? I’m afraid my kids are not going to know what to do with themselves because they don’t have their mom here. Why are you afraid of that? The root of it was guilt that I hadn’t prepared them for life.
The thing that you think you’re afraid of is really not the thing. It’s important to ask those types of questions to get down to the root of it so you can pull the root out and go, okay, it’s guilt. I didn’t have any clue it was guilt. It really helped me alleviate that anxiety. Then I got a clean scan.
»MORE: Cancer and Mental Health


Finding gratitude in one’s cancer journey
I say that things don’t happen to you, they happen for you. It’s a weird thing to say that I’m grateful for cancer. It’s so true though, because I have healed so many things in my body and I have more inner freedom and peace than I ever have had in my life because I started to face it versus running from it. Fear happens. It’s like, what’s going to happen to me, and what’s going to happen to my kids? All of that is real. It comes up and it’s like, I have a choice. I could either face it or I could run from it.
Another thing I heard a long time ago was, get to know fear. If you get to know it, it dissolves. It starts to melt away a little bit and it’s like, okay, I could do this. There isn’t anything to be afraid of. We’re all going to die at some point. We don’t know when. For me, it was switching to, I get to live today. I’m so grateful to be alive because, in November, I could have been dead. I appreciate that I’m alive. That’s key. I’m breathing today, so I get to live today.
I started a podcast to help other people and that’s helped me because it’s like, I’m back to life. I realized that one of the big things for me was realizing how disconnected I was spiritually. That has totally changed. I feel so much more connected to God and my faith. It wasn’t something I think I would have had with all of these things. Again, the key for me is living, being appreciative and grateful for where I’m at, and also giving. This is one of the reasons why I wanted to do this story is because I do think that we need a lot of hope and inspiration in the world, especially around cancer and people having a disease. I think this could help lots of people have hope and faith in themselves.

It’s a weird thing to say that I’m grateful for cancer. It’s so true though, because I have healed so many things in my body and I have more inner freedom and peace than I ever have had in my life.
What advice do you have for someone on a cancer journey?
The message of hope I would give is that you have to remember that your story is different than everybody else’s. I think a lot of cancer patients go into comparison – this person did that, and this person did this, and this person died, and this person didn’t. The most important thing is that your story is your story. It’s not the same as everybody else. Your body is different than everybody else’s as well. That’s why it’s so important to listen to yourself.
I had dense breast tissue and I didn’t investigate it. Look at your labs and ask lots of questions. When COVID happened, I didn’t get a physical because they wanted to do it virtually. I asked questions like, well, what am I going to do? I need a colonoscopy, I need a breast exam, and I need all these things. “Don’t worry,” they said. “Everything was fine last time, so you’ll be fine.” It can change very fast. It’s really important to investigate yourself and definitely get your exams done on time every time and ask lots of questions, especially if you’re feeling like something’s off now.



My hemoglobin was off for a long time and the doctors downplayed that. I trusted what they were saying. I think that you should trust it to an extent and also ask lots of questions because it sure helps. Now I’m very hyper-vigilant. My labs, I know exactly what they mean.
Have a lot of people around you to support you. I’ve had so much support and I have really good people in my corner where I’m like, “Hey, I need you to come with me because I don’t know how I’m going to hear it.” That’s really critical because there’s been so many times on this path where I’ve heard something and it’s not what was said. Even with the clean scan, I just heard it’s getting better. I didn’t hear that there was no evidence of disease. When my friend went with me, I asked, “Did they say what I think they said?” She said, “Yes, that’s what they said.” Having that person in your corner is really, really important.
Spreading hope and inspiration
There’s not enough hope and inspiration. That’s what I want to give to the world.
In life, we’re going to go through ups and downs anyway. Just because I have cancer doesn’t mean I’m different than anyone else. We still all go through things and we’re all going to have ups and downs in life. The only guarantee about life is it changes all the time. We’re all going to go through something.
I think that it’s important to be kind to yourself and give yourself what you need. That’s one thing I’ve learned, I have to check in with myself and go, what is it that you need? Don’t dismiss what you need. If somebody asks you what you need, tell them because people want to give you what you need. I think that’s really helped me to navigate this.

A really good attitude has been appreciating where I’m at. I could make the choice to be in a corner and curl up in a ball. By giving back to the community, by sharing my story doing the podcast and videos, or whatever I can do to get the message out, I’m going to do it. Because there’s not enough hope and inspiration. That’s what I want to give to the world is more of that versus doom and gloom.
Wherever your focus is, if you’re looking at all the train wrecks, that’s what you’re going to get. Look at where all the miracles are happening. I would prefer to see that.
More Metastatic Breast Cancer Stories
Symptoms: Shortness of breath, lump under armpit, not feeling herself
Treatment: Chemotherapy, Transfusions
April D., Metastatic Triple Negative, BRCA1+
Symptoms: Four lumps on the side of the left breast
Treatment: Chemotherapy (carboplatin, paclitaxel doxorubicin, surgery (double mastectomy), radiation (proton therapy), PARP inhibitors
Bethany W., Stage 4 Metastatic
Symptoms: Lower back pain
Treatment: Chemotherapy, radiation, maintenance treatment
Abigail J., Stage 4, Metastatic
Cancer Details: HER2-low, node negative, PIK3CA mutation
1st Symptoms: Back and leg pain, lump in breast
Treatment: Surgery, chemotherapy, radiation, CDK4/6 inhibitors
Alison R., Partially Differentiated DCIS, Stage 4 Metastatic
Cancer details: Triple positive = positive for HER2, estrogen receptor (ER), progesterone receptor (PR)
1st Symptoms: Lump in underarm/breast
Treatment: Chemotherapy, surgery, radiation, targeted therapy
Erin C., IDC, Stage 2B/4, Metastatic, Triple Negative
Cancer details: Triple negative doesn’t have any receptors commonly found in breast cancer making it harder to treat
1st Symptoms: Pain in breast
Treatment: Surgery, chemotherapy, radiation
Shari S., Stage 4, Metastatic, Triple Positive
Cancer details: Triple positive = positive for HER2, estrogen receptor (ER), progesterone receptor (PR)
1st Symptoms: Lump in breast
Treatment: Surgery, chemotherapy, radiation
Renee N., IDC, Stage 3-4, HER2+
Cancer details: IDC is most common kind of breast cancer.
1st Symptoms: Lump in breast
Treatment: chemotherapy, bilateral mastectomy, radiation








