Shari’s Stage 4 IDC Triple-Positive Metastatic Breast Cancer Story
Shari shares her metastatic breast cancer story, which began with her finding a lump in her breast. She details undergoing a lumpectomy, chemotherapy, and radiation.
In her story, Shari also describes navigating life with cancer, from facing metastasis, dealing with scanxiety and hair loss, being a self-advocate, and how the diagnosis impacted her marriage.

- Name: Shari S.
- Diagnosis:
- Metastatic breast cancer
- IDC
- Staging: 4
- 1st Symptoms: Lump in breast
- Treatment:
- Surgery
- Lumpectomy
- Oophorectomy (removing 1 or both ovaries)
- To get off the Lupron shot
- Chemotherapy
- Carboplatin & Taxotere
- 4 rounds with infusions every 21 days
- Herceptin
- Infusions every 21 days, still ongoing
- Carboplatin & Taxotere
- Radiation
- Stereotactic radiation therapy
- Surgery
Be able to accept the help of all the people that want to help you. Allow people to take things off of your plate.
Shari S.
- Diagnosis
- Treatment
- Metastasis
- Reflections
- Do you experience “scanxiety”?
- A “new normal”
- What has been the hardest thing for you mentally and emotionally?
- Can you talk about the hair loss?
- Do you have advice for other people who are going to lose their hair?
- Can you talk about self-advocacy?
- What advice do you have for other patients on advocating for themselves?
- Living with cancer as a chronic illness
- Cancer & Relationships
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Diagnosis
What were your first symptoms?
I noticed the lump in December of 2015. It appeared out of nowhere. It wasn’t sore or anything. It didn’t change or get bigger after I started watching it.
I really didn’t have any other symptoms that were apparent. I had decided to get back into shape in the fall. I had done that before and not had any issues. This time around, though, it was harder. It was weird for me.
I did notice a little heaviness in my chest, and now in hindsight, that might’ve been something that was a symptom of the cancer.
How did you get diagnosed?
I had a mammogram the next April. The radiologist saw that mammogram while I was still there and told me I needed to go see an oncologist.
I had saline implants, so instead of a needle biopsy, they went in surgically for a lumpectomy. It was a same-day surgery. The next week, I got the diagnosis of breast cancer.
Results of the lumpectomy
They took out the lump, and the margins were fairly clean. They said they had good therapies for triple positive and HER2, but then they wanted to check the lymph nodes. They did a PET scan.
The day I went back to the oncologist to start my chemo while waiting on the full diagnosis and staging, I found out it was metastatic and I was stage 4.
That was a lot to take in that day, but the treatment was still the same. My oncologist said it was a lot of information for me to take in on one day and was willing to reschedule my treatment, but I didn’t want to. We were treating it aggressively.
I was there and ready and wanted to get started.
How were you thinking and feeling after the diagnosis?
My original oncologist isn’t my oncologist now. His bedside manner isn’t the greatest. The day he gave me the diagnosis, he kept asking, “Do you have any questions?”
We didn’t know what to ask. Finally, my husband asked about prognosis. He said I had 2 to 10 years, depending on how well my body reacted to the treatment.
By the time I got home, I’m Googling everything. I read that the next place it can go is to your brain, which the doctor didn’t even mention. I’m thinking, “Is it there, too?”
We hadn’t done any testing for that. My surgeon ordered an MRI for me, and at that point it was clear, so that made me feel better.
My husband and I just thought of it as a chapter and something we were going to get through. It took a while to realize that this would be the rest of my life. We’ve definitely started living our lives how we want to.
There’s always a reason to not go on vacation or something, but now we don’t let those things get in our way.
»MORE: Processing a cancer diagnosis
How did you tell your loved ones about the diagnosis?
My husband was there with me. He’s always there with me. I have 4 adult boy children. I told them all early that I had cancer and thought it was early stages. I had to call them all back and tell them it was metastatic, and they all dealt with it like they do with Google and research.
My parents had a hard time with it. One of my first thoughts was, “Am I gonna outlast my parents?” We told our closest family first, and then I had to tell work because I knew I was gonna start losing my hair.
»MORE: Breaking the news of a diagnosis to loved ones
Treatment
What was the lumpectomy like?
It was same-day surgery. It was no big deal really. The biggest thing for me was after surgery and recovery and seeing the indentation in my breast on that side, because now it doesn’t look like the other one.
The recovery was very quick. We were back in surgery the next week to look at my lymph nodes and to get my port put in.
The lumpectomy was no big deal. It was a couple of stitches, and that’s about it.
What was your chemo regimen like?
I had 4 rounds of Herceptin, carboplatin, and Taxotere. I had infusions every 21 days. I would get infused on Fridays. The first couple really weren’t too bad. They didn’t feel great, but it wasn’t bad.
After the first one, I went back to work on Tuesday, and I realized I had been walking around in a fog all day. We started working from home the week after the infusion. I would go to work when I was able to and just did what I could.
The CT scan I had at the end of the chemo, that showed significant improvement. The oncologist said I didn’t have to do any more yucky chemo at that point unless something changed, but I did continue the Herceptin once every 3 weeks. I’m still on that.
What was the worst side effect you experienced from chemo?
I never threw up really, but I had underlying nausea all the time. The one time I threw up was after my second round.
I started feeling better, but I did too much. It was 10 p.m., and we had been out. My husband kept saying, “Are you okay? We can’t overdo it.”
Around that time, I had violent throw up for a couple of sessions, and then that was it. It had to have been that I just did too much.
My body was trying to tell me to rest. After that day, I knew.

Did you achieve NED (no evidence of disease)?
By the next March, I had another repeat scan, and I had no sign of any active disease.
I switched oncologists. Nothing changed in my treatment, but now there’s a person I can talk to about anything. I went in for the results, and he says, “I understand you thought you got the wrong results.”
I asked him what no evidence of active disease meant. I asked if I was in remission, and he said no. I had to remember how much cancer was in my body and that it was stage 4 and metastatic. They don’t necessarily say remission, but they did say no evidence of active disease.
That didn’t mean there was no cancer left in my body, but it just means that everything that we’re doing is keeping the cancer at bay.
It was after that that I started wondering what the rest of my life was gonna look like. That’s when I started to go on Facebook groups and things like that. I tried to find other metastatic cancer patients.
Metastasis
Metastasis to the brain
In July, I was out for a walk after work, and I started having this really weird thing go on with my ears. It was more on one side than the other, but it was like my ears needed to pop. I knew that wasn’t what it was, though.
It concerned me. It wasn’t going away. The next time I had my regular visit, my oncologist wasn’t there. I talked about it, and I felt like they just brushed it off. I paid attention to it. It didn’t go away.
The next time I saw the oncologist, I told him I was having an issue, and sure enough, I had mets in my brain. I had stereotactic radiation. It was pinpointed to the spots.
How do the brain mets affect you mentally and emotionally?
The brain stuff scares me more compared to anything else. I’ve always worked, and I wonder if this is going to eventually take that away from me.
I worry about my memory. I’m always really paying attention to that, and so far it hasn’t been an issue.
Once I went in and had my first radiation, I found out it wasn’t that big of a deal. I had a headache later on that day, and I was tired until the next day, but other than that, it wasn’t really hard.
After that, I started having an MRI every 3 or 4 months. Before, I was like, “Oh my gosh, what am I gonna do when it goes to my brain?”
Well, now I can go in and get treated with pinpointed radiation, and I know what that’s like. It’s not scary anymore.
When I hear whole-brain radiation, that freaks me out, but I’m not to that point yet. When I do get there, I know I’m probably done working.
That’s what I gather from other people’s experiences I’ve read about. I try to not get too tied up in it. It can be pretty scary when you read how bad it can get.

What’s the targeted radiation like?
They do the mask. It’s like going in and having a facial first because they have to make the mask, which is no big deal.
It’s weird, though, because they screw that mask down onto the table. You have to be very still.
I always keep my eyes shut when I go into all the machines, but even still, I felt like I could see some light or something.
The first time is scary because you don’t know what to expect.
It’s noisier than your scans. You’re in there longer. I was in there for an hour and a half like that the first time. It’s scary, but it’s doable.
The next time I did it, it wasn’t scary anymore. You just have to go somewhere else in your mind to get you through it, and then it’s over.
It’s weird how you get used to all these things you have to do.
Reflections
Do you experience “scanxiety”?
Originally, yes. When I think back on my first PET scan that showed I was metastatic, I wasn’t freaking out waiting for those results.
Maybe that’s because I didn’t know much about it. Ever since that first one that shook me, now the follow-up scans do make me anxious. My husband and I deal with that, though.
First of all, we don’t talk about it. We know it’s on the calendar. We get up that morning, and we both know we’re going to a PET scan before work. We just don’t talk about it.
At this point, I don’t tell too many people I’m having a scan because I don’t want them bringing it up and reminding me.
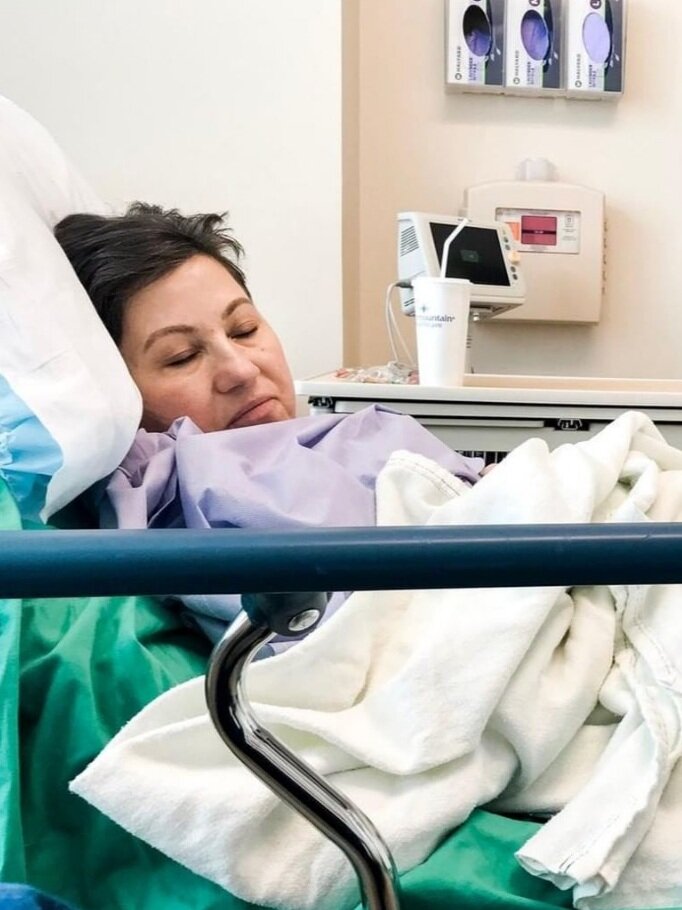
We do a couple of things that help a lot. We tend to plan our vacations around the time of the scans. Sometimes, we’ll go right before a scan. I might be on a 2-week cruise, and 2 days later, I’ll have a scan. Other times, we’ll schedule a trip for right after a scan.
We do that because we figure if I get a really bad scan result and I have to change my treatment, it’d be really nice to have a break from life beforehand.
We have gone on a 2-week trip every year since my diagnosis and a bunch of little ones in between. I would rather look forward to the next trip than dread the next scan. That’s helped both of us. It’s always in the back of your mind, but that helps.
Another thing that’s helped is control. With cancer, you’ve lost control. When I have my PET scan, I have it early in the morning and early in the week.
That way, I know I can get my scan, go to work, and that day after work, I can go pick up my results. That way, I know right then whether I need to be freaked out or let it go.
So far, things look good, and I don’t have to worry. Same thing with my MRI results. They usually pop up on my portal the same day if I get them done early.
»MORE: Dealing with scanxiety and waiting for results

A “new normal”
It probably took me more than a year to get there. You read people talking about a new normal and how to find it, but for me and how I choose to deal with things, it took me a while.
It was hard for me when my hair started coming back and people didn’t think I was sick anymore.
They started saying, “Shari is a survivor!” Am I? I like to think of myself as a thriver, but I guess as long as you’re alive, you’re surviving.
Dealing with people thinking you’re fine when you’re not just because you don’t look sick anymore is really frustrating. I’ve gotten really active on social media because of that.
This isn’t just about me. This is about anybody that has any kind of illness where they don’t look sick. There are so many kinds of cancer. Not all chemo makes you lose your hair. You don’t barf with every chemo. Even if it does, there’s a lot of nausea meds.
I’ve done a lot of educating people because of this and that mindset shift. I’m an open book because I don’t want people to be naive.
I’m optimistic, but I’m realistic. I never know what the next scan holds or where I’ll be in the next 2 years.
If I go into remission — if someone wants to say it that way — fine, but I know it’s coming back. Don’t tell someone they’re cured, because the percentage of recurrence is so great.
Anybody who tells someone that they’re cured and their cancer is 100% not coming back is a liar. They can’t stop cancer yet, and there will be a cure when they can.
What has been the hardest thing for you mentally and emotionally?
The fact that people don’t know that I’m not fine. For a long time, I was really scared. Meanwhile, people think I’m cured and fine because I’m walking around with hair. Well, I’m also walking around with cancer in my brain.
When I realize that people still don’t get it, it’s hard to deal with. I used to get kind of pissed off about it, but I don’t anymore.
When someone would say, “This is Shari. She’s a breast cancer survivor,” I’d be like, “Wow they still don’t get it. How many times do we have to say metastatic?”
I don’t act like I’m sick, but I am sick. My life has completely changed because of it, so I don’t know how people can’t understand that.
You never know what someone is going through.
Before I got sick, I don’t think I had much empathy for someone who was going through a chronic illness of their own. That included my own mother.
Once I went through chemo, and even since, I realize now that life changes drastically because of illness. I’m much more empathetic now towards people because of that.
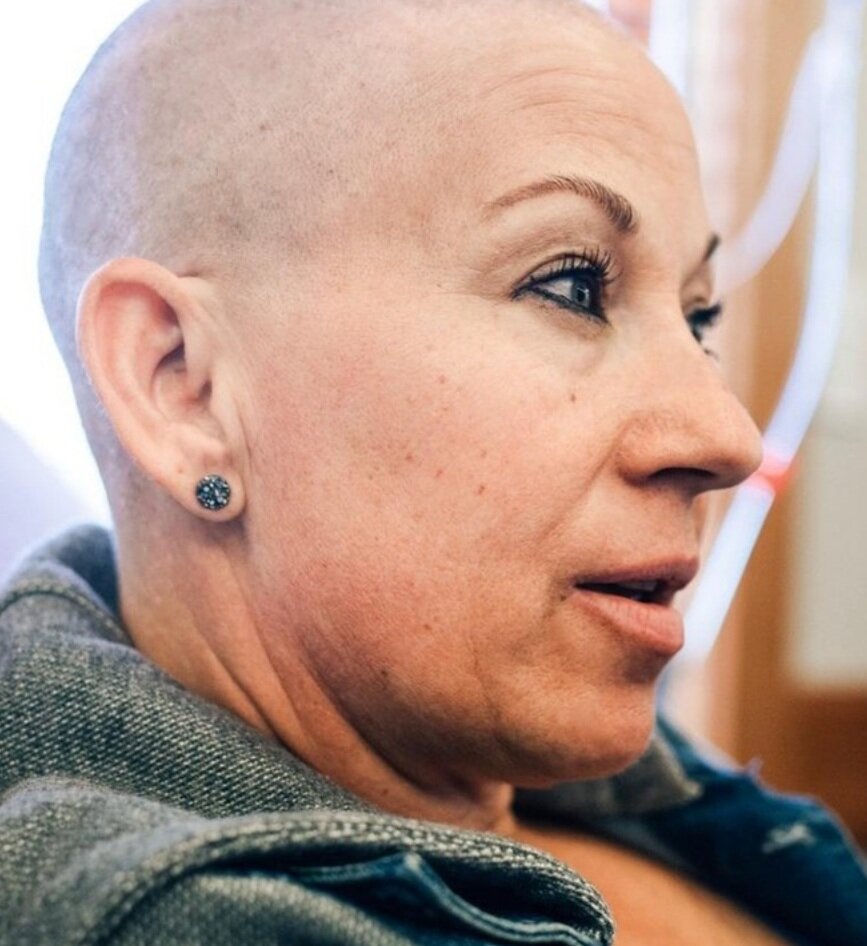
Can you talk about the hair loss?
I knew I was gonna lose my hair around 2 weeks after my first treatment. I ran my hand through it because it felt really dry, and it started coming out.
I made plans with my girlfriends. We had a shave party in my backyard 2 days later. I found out that my head is perfectly shaped.
I put a wig on that night, took it off, and never wore it again. I either wore hats or nothing.
Everybody gave me scarves, but I didn’t like them because they just made me look like a cancer patient. I didn’t like that. I didn’t look like me.
I shaved my head on Saturday and went to work on Monday with nothing. That’s when everyone knew something was going on.
Do you have advice for other people who are going to lose their hair?
Your hair is nothing. It doesn’t make you who you are. It’s what’s inside that makes you who you are. Your hair does grow back, and mine has actually grown back thicker. It grows back a lot quicker than you would think.
If you’re comfortable with a wig, wear one. If not, don’t. I had baby-fine hair and used to hate that. I have a video of the night we shaved my head. I have another one where I’d been without hair for 8 weeks or so, and I said something like, “I always talked really mean about my hair.”
Now, I’m like, “Hey, whatever you want to look like, go for it, hair. Whatever you’ve got.”
Can you talk about self-advocacy?
I didn’t really advocate for myself with the first oncologist much. I did ask about my brain stuff, and he said, “No, we don’t do an MRI unless you’re having symptoms.”
Then I saw my surgeon at a follow-up, told him what he had said, and he said, “I’ll order one for you.” The radiation oncologist said the same thing.
When my oncologist saw the results, he had a very “I told you so” attitude about it. I just said, “Yeah, it sure is nice to have peace of mind.”
I was going to worry, and then I didn’t have to because it came back clear. I was taking control of a situation that was going to keep me up at night.
Months into it, I started thinking, “Can I fire my oncologist?” I knew I was going to be seeing him for the rest of my life. The only reason I was going to see my oncologist was because I couldn’t get in to see the other one for 8 weeks.
I thought since I was going to be seeing him forever, I’d like to be able to see someone who cared about me and knew me. Every time my new oncologist walks in, he has something kind or helpful to say to me.
I consider him a friend. I’m a patient to him, and I understand that, but I see him as a friend. I never felt that with the first guy. I made the right choice.
»MORE: How to be a self-advocate as a patient
What advice do you have for other patients on advocating for themselves?
It’s all about how you ask questions. For example, I was on a Lupron shot. That medicine caused me so much pain in my joints. I couldn’t get down on my hands and knees to do yoga to try to stretch things out.
It took me a while to figure out that the Lupron was the culprit. My quality of life was declining because of it. I started reading up on it and what to do.
I asked my current oncologist one day, “Can’t we just take my ovaries out so I don’t have to take the shot?”
He said, “If you had a genetic mutation, then I would say yeah, but since you don’t, no, there’s really not a point.”
I didn’t get the answer I wanted. A while later, I was still having pain. I said, “What do we need to do for me to get my ovaries taken out?” He said, “You’ll need to do X, Y, and Z.”
3 months later, the ovaries were out. It was a simple surgery. By a month after that, there was no more pain.
It was all in how I asked the question. When I do have questions, I try to go in with the right words. If I don’t understand the medical terminology, I’ll ask him to explain it to me a little bit so I can ask what I really want to ask.
A lot of times, if you can come in talking their talk a little bit and be an educated patient, that will get you the answers you need.
Living with cancer as a chronic illness
During chemo, it’s really in your face because you’re so sick. When I was that sick, I realized how many little things I took for granted. I realized how thankful I was for certain things.
Then I started to feel better, and I got away from it again. I got back into my life. I realized I really like the person who was so vulnerable and so thankful for so many of those things.
It’s about remembering that. I think of it as waking up in the morning and being grateful for getting to go to work, because there are people who wake up and can’t get up and do anything.

Cancer & Relationships
How do you and your husband lean on each other?
If I need to talk about something, I tell him I need to talk. He may not want to talk about it, but if I need to, I let him know I need to.
I talk, and I make sure he hears me because both of us are going through it, and that’s that.
I think it takes a while for the patient to realize that the caregiver is dealing with just as much. It might even be harder for them sometimes.
I’m the one that’s going in for everything, but he’s just as scared of losing me as I am of dying. The fact is the person that’s dying is gone, but the person that stays is the one that has to deal with everything.
You don’t figure that part out for a while. When you realize there’s 2 sides to all the crap you’re going through, it helps put things in perspective.
»MORE: 3 Things To Remember If Your Spouse Is Diagnosed With Cancer

What advice do you have for other married couples going through something similar?
Go to somebody to talk. You need to see a relationship therapist. A man needs to hear the reality of what happens when a woman loses all her hormones.
There are still ways to find intimacy in a relationship, but you need help finding those ways. You need to know that going into it so you can start preparing and shifting.
What helped you through the hardest times?
During those first chemo treatments, I would have my husband just talk to me. He would talk to me about a trip we would take when I was feeling better.
After I found out I didn’t have to be on any more chemo, I looked at my husband one day and said, “I thought we were gonna plan a trip.”
That’s why we planned our first one, and we haven’t stopped. It’s a distraction. It gets us to do all the things we always said we wanted to do. It’s something fun and positive to think about rather than the what ifs.
The other thing is when I feel sorry for myself, I think of how much worse it could be. I would see people in the chemo room who were sicker than me, younger than me, or older people would be talking about hospice.
As soon as you have a story, somebody else somewhere already has a worse one than you. It’s a lot of wasted energy to sit there and feel sorry for yourself when it could be so much worse.
I took care of funeral arrangements and a will, which is something we had never had to think about doing, but now it’s taken care of. I don’t have to worry about it anymore. Dealing with those kinds of things and knowing now that they’re done helps, too.
»MORE: What kind of support cancer patients say helped the most
Being a parent with cancer
If my kids had been little and at home, I don’t know what I would’ve done. I was grateful that my kids were all out of the house. They’re all boys, and I think if they had been girls, they would’ve been more consistently involved. Whereas, with boys, they opened the door, asked questions, and then shut the door again.
My heart goes out to women whose kids are younger. I’ve already got to see one of my kids get married. I have a grandkid. I’ve gotten to experience these things that other women might not get the chance to. My heart goes out to them.
Last Christmas was hard because all my kids came home for the holiday. They’re all adults and have their own lives, but it worked out that they all got to be there. I was able to have all 4 boys home.
I did every single tradition we’d ever done, and I did it on purpose because I don’t know for sure.
I was thinking, ‘Am I going to have them all home again? Am I going to feel up for it again? So, I made the most of it.
Sure enough, I heard from each one of them how much they enjoyed it. It was the little things they appreciated so much. Other than that, things are the same. They’re boys. They don’t call their mom as much as they should.
»MORE: Parents describe how they handled cancer with their kids

Advice for someone with similar diagnosis
You might feel like you have to do everything really quickly. Everyone tells you you need to get more than one opinion, but you’re so scared that you feel like you have to do it right then.
You don’t have to do it that fast. If I had it to do over again, I would’ve probably taken a little more time. I could’ve probably waited the 8 weeks and gone to the good oncologist first.
I probably had the cancer in my body for years before it finally came out on my breast, so what was another 8 weeks really going to do?
Slow down. You don’t have to rush into decisions. It’s not going to make you die quicker because you wait for an appointment you’re comfortable with.
Whether you do it or someone else can do it for you, take care of it. The more you worry about things, the unhealthier you’re going to be.
Walk for 30 minutes a day, whether you feel like it or not. Things like that. Do anything you can do to keep feeling normal.
Be able to accept the help of all the people that want to help you. Allow people to take things off your plate. If something is bothering you, find a way of taking care of it.

Inspired by Shari’s story?
Share your story, too!
Invasive Ductal Carcinoma Stories
Amelia L., IDC, Stage 1, ER/PR+, HER2-
Symptom: Lump found during self breast exam
Treatments: TC chemotherapy; lumpectomy, double mastectomy, reconstruction; Tamoxifen
Rachel Y., IDC, Stage 1B
Symptoms: None; caught by delayed mammogram
Treatments: Double mastectomy, neoadjuvant chemotherapy, hormone therapy Tamoxifen
Rach D., IDC, Stage 2, Triple Positive
Symptom: Lump in right breast
Treatments: Neoadjuvant chemotherapy, double mastectomy, targeted therapy, hormone therapy
Caitlin J., IDC, Stage 2B, ER/PR+
Symptom: Lump found on breast
Treatments: Lumpectomy, AC/T chemotherapy, radiation, hormone therapy (Lupron & Anastrozole)
Joy R., IDC, Stage 2, Triple Negative
Symptom: Lump in breast
Treatments: Chemotherapy, double mastectomy, hysterectomy








Leave a Reply