Finding Light Through Advocacy in Stage 3 Synovial Sarcoma: Sorcha’s Experience
Before cancer entered her world, Sorcha’s life in El Paso, Texas, was full of family, engineering work, and hands-on creativity. She spent her days as a mechanical engineer in the oil and gas industry and her evenings quilting, crocheting, or making friendship bracelets with her young daughter. Their bond showed up in bright, memorable moments, like planning a Taylor Swift concert trip together and crafting bracelets in anticipation. It was within this full and grounded life that Sorcha first began navigating what would become a diagnosis of stage 3 synovial sarcoma.
Interviewed by: Nikki Murphy
Edited by: Katrina Villareal
Before her stage 3 synovial sarcoma diagnosis, Sorcha’s days were defined by work, parenting her daughter and son, and finding joy in movement and learning. She went to New Orleans for a Taylor Swift concert, which she remembers as a safe, joy-filled space, especially for girls, women, and families. She, her daughter, and her sister immersed themselves in the music, traded hundreds of handmade bracelets, and created memories that would later stand out as a “protected, beautiful time” just before everything changed.

Soon after, Sorcha began noticing symptoms: right-sided abdominal pain, changes in her breast, and a frightening episode of vision loss in her right eye. Despite seeing multiple doctors and being told the symptoms were likely stress or migraine-related, she continued to push for answers. Her stage 3 synovial sarcoma experience quickly became one of self‑advocacy as she tracked patterns, returned to primary care, and insisted that seemingly “unrelated” symptoms might, in fact, be connected. Eventually, severe pain, nausea, and vomiting led her to the emergency room, where a chest CT revealed a large mass.
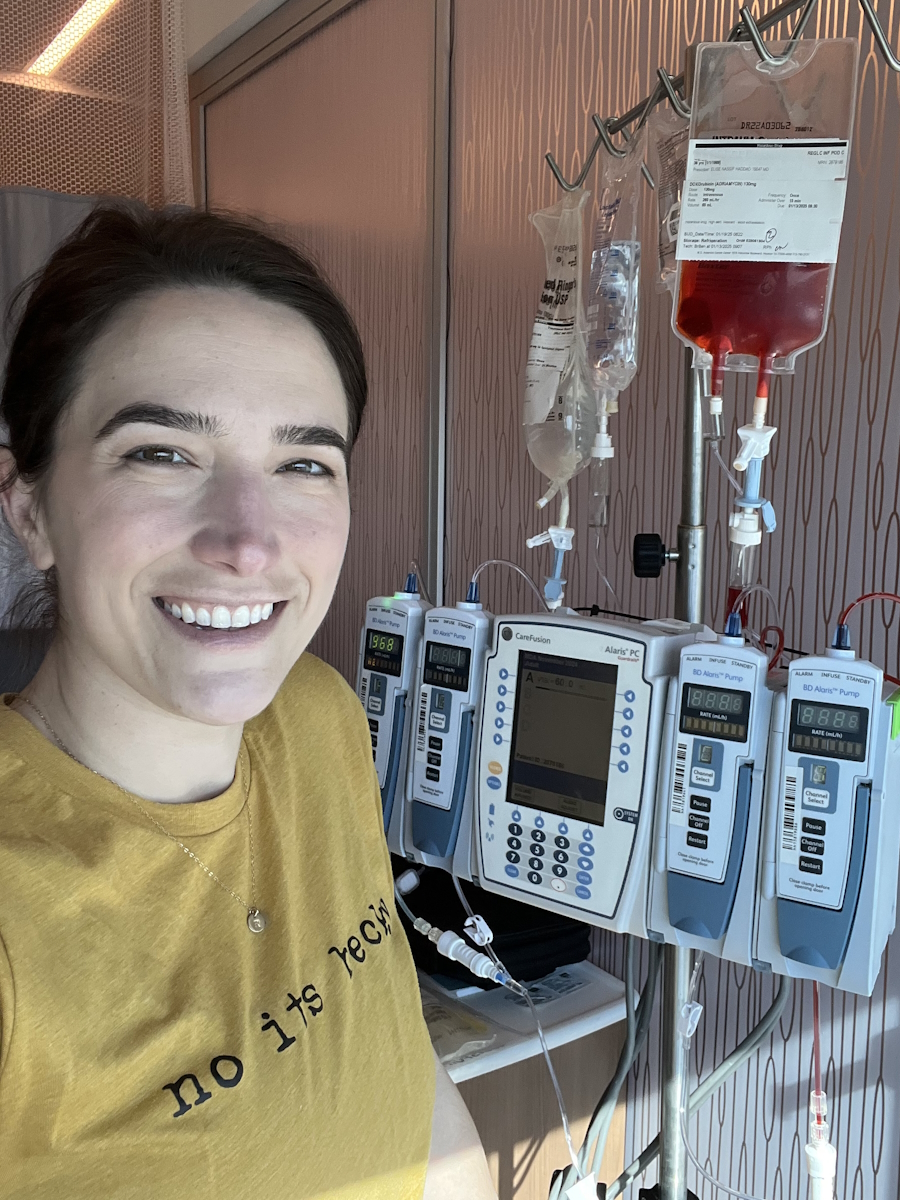
From there, Sorcha moved into an intense treatment path that included chemotherapy and protective medications to shield her kidneys and bladder. She describes the shock of sudden hair loss, shaving her head with her kids at a local salon, and the mounting fatigue and cognitive effects that linger even now. Yet she also highlights support from friends who flew in before surgery, an employer who offered housing during treatment, and a tight “village” of long‑time friends who celebrated “No Mo’ Chemo” with a beach photo shoot. Through it all, her stage 3 synovial sarcoma experience is defined not just by medicine, but by motherhood, community, and a fierce commitment to self‑advocacy.
Watch Sorcha’s video or read her interview transcript to find out more about her story:
- Strong self‑advocacy helped Sorcha push past initial “it’s probably stress” responses and eventually get imaging that revealed her synovial sarcoma
- How small, joy‑filled experiences became powerful emotional anchors once symptoms and treatment began
- Maintaining a “village” of long‑time friends across multiple moves created a support system that showed up in tangible ways
- Learning that patients often need to trust their own sense that “something is wrong” and keep asking questions until their concerns are fully addressed
- How Sorcha’s perspective shifted from simply enduring treatment to intentionally using her time and health to be present with her children and to share her experience to help others
- Name: Sorcha B.
- Age at Diagnosis:
- 36
- Diagnosis:
- Synovial Sarcoma
- Staging:
- Stage 3
- Symptoms:
- Right upper quadrant pain
- Changes in the right breast
- Temporary vision loss in the right eye
- Nausea
- Vomiting
- Treatments:
- Chemotherapy
- Cytoprotective therapy: mesna
- Surgery: lobectomy of the middle lobe of the right lung and associated ribs and soft tissue
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My Name is Sorcha
- Taylor Swift Trip to New Orleans
- Girls’ Beach Trip and No Mo’ Chemo
- Wigs and Hair Choices
- Early Sarcoma Symptoms and Dismissed Concerns
- Primary Care, Tests, and ER Referral
- Emergency Room Visit and Mass Discovery
- Timeline to Official Diagnosis
- Hearing the Diagnosis and Treatment Plan
- Telling My Husband, Parents, and Friends
- Researching Care Teams and Protocols
- Chemo Before Surgery
- Hair Loss and Shaving My Head
- Chemo Side Effects and Lasting Impacts
- Anticipation and Strategy for Surgery
- Surgical Outcome and Sharing Tumor Photos
- Sharing on TikTok and Helping Others
- NED Status and Upcoming Surgery
- My Biggest Emotional Challenge
- Parenting Through Treatment
- Meaning of Survivorship
- Hopes, Dreams, and Everyday Goals
- My Advice and Message to Others
- My Thoughts on Mental Health and Hope
My Name is Sorcha
My name is Sorcha. I was diagnosed with stage 3 synovial sarcoma at the beginning of 2025, and I live in Texas, in El Paso.
I am a mechanical engineer by degree, and I work in oil and gas. I have worked at the same company my whole career. I’m passionate about learning. I’m curious about the world and the people around me. I think the stereotype of mechanical engineers is that they do stuff with cars. I don’t do anything with cars. I like to make stuff with my hands, though, so I enjoy crafting, arts and crafts. I quilt, crochet, knit, and make friendship bracelets. I’m a big Taylor Swift fan and so is my daughter. I am married with two kids. I have a daughter who is six and a son who is four. I also like to read and lift weights.
Taylor Swift Trip to New Orleans
That trip was on Halloween weekend, which, if you’ve ever been to New Orleans around that time of year, it’s like festival season but spooky. There are a lot of locals, music, and artistic expression. It’s such a cool city for a ton of reasons, but also very cool to be there the week of Halloween, and the concert was that weekend. I went with my daughter and we got the tickets a year beforehand, so we had made our costumes. It took about a year for me to make my costume. It was very intricate, and my daughter went from knowing the songs to knowing all the lyrics to all the songs because she’s developing and growing up, so it was so cool. It was a fun mother-daughter time.
We handmade hundreds of bracelets together, and then we got to hand them out and trade them with people in New Orleans. We have a little memory box with all of our bracelets. She has a whole bunch in her room, but those are the ones that I have little memories about.
My sister came down. It was a cool experience. That whole concert vibe is very girlhood. It’s safe. Everyone’s so positive and kind, and it was a great experience for my daughter. It was a whole bunch of moms and sisters and kids and women of all ages, also some men, too, but just a very safe place for her to experience the city for the first time. It was a beautiful experience.
I went to the emergency room for the first time a little less than a month later, so it stands out for me as this gem of this protected, beautiful time before I became ill.
Girls’ Beach Trip and No Mo’ Chemo
As part of my career that I’ve chosen, I’ve moved a lot. I’ve probably moved, I want to say, seven times. It becomes important not to rely on an external village. You need to make your village. I think part of that is making sure you maintain strong, connected, intimate friendships even as you move. That takes work and effort, and it has to be reciprocated.
This group of girls, not all of them are there in that picture, but that group represents that village of adult friends I’ve had now for, I mean, a couple of the girls since I was two or three, and I think the newest friend I have is maybe 12 years ago. They’ve been extremely supportive through this whole experience. We wanted to celebrate the end of chemo, so we did a “No Mo’ Chemo” photo shoot and had my family come in right after. We actually had a photographer take pictures and memorialize that experience of being done with being sick and turning the page towards surgery and recovery.
Wigs and Hair Choices
Everyone thought I would wear wigs, I think, so it was a little bit like, hey, wigs are cool, wigs are in. But I never did. No shade or hate to anybody; I just found them a little bit itchy. So it was kind of fun to wear them for the first time and then be neon, you know.
Early Sarcoma Symptoms and Dismissed Concerns
I would say in the summertime, maybe July, I had some right-quadrant pain. It was dull, aching pain over the course of a few days, with some sharp stabbing pains. It lasted for a couple of days and I thought, “That’s kind of weird. Maybe I hurt myself. Maybe something happened.”
A few weeks later, I had the pain again, except it was bad enough that I couldn’t sleep. It affected my sleep, and the sharp pains were really sharp. I was on Google asking what it could possibly be and came up with it’s probably gallstones. I had lost weight. I’d finished nursing my kids and was coming back to my normal weight, so maybe that’s what it was. That was around July, and then I had the pain again.
Along with that, I had had a couple of other symptoms and I thought they were unrelated. I thought I felt something in my right breast. Something seemed different. Something seemed off. I went and saw a gynecologist to check me. He said he didn’t feel anything. Everything felt normal. I was like, “Well, one of these feels different. My right one feels like something’s off with it. I can’t really explain why; it feels higher or something.”
Around then, within those weeks, I lost vision in my right eye while I was getting ready for work. It was as if you stared into a light and you can’t see for a while, except it didn’t recover and my eye looked normal. My pupils were equal and reactive. I saw several doctors. I saw the gynecologist, an optometrist, and an ophthalmologist about my eye. They said I was probably having a migraine. I didn’t have a headache, but they said an aura around a migraine can result in that vision loss. After seeing a few doctors with all these unconnected things, it came down to I was probably stressed out.
Primary Care, Tests, and ER Referral
Then I had the pain again in August, and I went to a primary care doctor and said, “Hey, look, I’m having A, B, C, X, Y, Z. I know I’ve been told by other doctors that [they] are unrelated. I think they’re related. I think there’s something wrong.” She took me very seriously. She ordered a whole bunch of tests. She ordered a head CT. She ordered an ultrasound of my gallbladder area, just checking on that. I also saw a gastroenterologist.
All my tests came back normal. All my blood work was normal. My head CT looked normal. Although my doctor was very supportive and said, “I agree, if you say there’s something wrong, there’s something wrong, maybe it’s something hormonal. Let’s meet back again in six months and see if anything has changed. But in the interim, if you experience this pain again, immediately go to the emergency room because they may be able to image and see if there’s some intermittent thing happening. They may be able to see it while it’s happening.”
Emergency Room Visit and Mass Discovery
That was in August. September, October: Taylor Swift concert. Towards the end of November was the next time I had the pain. I had discomfort, pain, and nausea at work after eating a meal, which again sounded consistent with gallstones. I went to see our LPN, and whenever he was probing around to see if everything was okay, I started vomiting and I couldn’t stop. Concerned that this might be something cardiac or more complex or serious, I went to the emergency room. At the emergency room, I was triaged and waited several hours to be seen.
Once I was seen, again, scans were showing nothing. I said, “Hey, I really think something’s wrong over here. Can you please look over here, see if you see anything?” They went back and consulted and said, “Okay, we might see something. If you’re saying you’re having pain there, we see a little, it might be a blood clot. We can’t really tell. We’ll do a chest CT.”
Once the chest CT was done, everyone’s mood changed. I wasn’t given the results immediately. I have an idea of how long the results should take. They said, “We’re going to wait. We’re going to put you in a room.” I had just been behind a curtain before then, so I thought a room opened up. They put me in the room. I think they were trying to be very considerate of my feelings and my experience, but they put me in the room privately so that they could tell me that they found a large mass and it didn’t look good.
Timeline to Official Diagnosis
I had an emergency room visit where they found the mass, and then we drained the fluid, re-inflated my lung, biopsied the mass, and then they tested the biopsied tissue. I was diagnosed on January 2nd. My ER visit was around Thanksgiving, and my diagnosis was in New Year’s.
Hearing the Diagnosis and Treatment Plan
What’s crazy is I knew what it possibly could be, and I had self-referred to the sarcoma group at MD Anderson before even having the FISH result that confirms sarcoma. So I knew that this was a significant chance, but I hadn’t done any research into what the treatment protocol would be because it’s so different based on your individual case. It basically went, “Hey, yes, we have this result, you have synovial sarcoma, you have this high-grade malignant mass that makes you stage 3, we need to start chemo immediately, it’s going to be really bad, you’re going to get really sick, and you’re going to be rendered infertile. So, are you done having kids?”
In their defense, they’re not saying this stuff boom, boom, boom, but the experience of it is like, “Oh, that’s a lot of information,” trying to take it in. She said, “If you want to have more kids, we need to freeze these eggs now, and we need to get you in here next week to start chemo. You’re going to be out of work for six months, and then you’re going to have surgery, and it’s going to be this significant surgery.”
I was clinical in my response. I was like, “Yep, I’m done having kids, that’s perfect. I’m young, I can handle difficult chemo, but I’m old enough that I already have my children. Okay, perfect. We live close to MD Anderson.” I was responding in a very unemotional way, but I think that I just wasn’t able to experience the emotions in the moment.
Telling My Husband, Parents, and Friends
My husband was with me in the room the first time. At first, we were amongst ourselves, like, “It has to be benign, it has to be benign. I’ve never smoked. I work out. I eat healthy. I’m a healthy person. Of course, I don’t have cancer.”
When I found out that they had ruled out a benign mass, I came in and woke him up and told him it was cancer. I think we were both surprised, asking the same questions over and over again, like, “Well, why? You don’t do any of this stuff that makes a risk factor.” But that was his biggest shift, realizing that it was cancer.
The actual diagnosis of the sarcoma and the treatment protocols were more intense than I expected, but we didn’t know that much about what cancer patients go through. Most of my friends who had had cancer had had skin or breast cancer that was mild enough not to affect their life or their appearance significantly during the treatment, just because of the type of cancer they had.
I called my boss on the way home and said, “Hey, I have to be out of work for six months. I need to leave immediately.” He said yes and even offered his home to me. They had an apartment that his wife and daughter were using while she was in her last year of high school, and they offered to let me stay there while I was going through treatment. That was generous and helped support me a lot.
Then I called my dad. He was distracted and packing and said, “Hey, can you call your mom? I’ve got to get this done.” I said, “No, it’s serious. Can you sit down for a second?” I told him, and I asked him to call my mom first so that she could have a reaction to it and not feel like she had to not react to protect me or something.
My dad’s an engineer. My mom’s more like a biologist-artist type. That just felt like the right way to do it. Then, everybody else, I sent a text message that said, “Hey, I have cancer, and here’s this three-paragraph-long thing of all your questions answered. I pre-wrote it with everything and put it in my notes.” Everyone got the same message. This is what I’m comfortable with you sharing with others and this is what I’d like you to wait to share. So I guess being my friend is kind of a wild ride. You might get that text one day, I don’t know.
Researching Care Teams and Protocols
I reached out to a few places. One place in the Northeast, I’m blanking on what it’s called, and I self-referred to Mayo Clinic and MD Anderson. I called a few people I knew and trusted. I reached out to my family and said, “Who do you know that works in oncology? Who do you know that knows about clinical trials or knows about this type of cancer that I believe I have?”
I wanted to understand who is most respected. I did a lot of research going into it before I had that January 2nd meeting, not so much about what protocol they would prescribe, but which care teams are respected and have the most options and the most robust systems for support.
The care team came in and said, “This is what it is. In general, sarcoma is resistant to chemo; you’re going to have to have an intense chemo regimen. Our goal is to prevent or reduce the chance of recurrence.” They were transparent that this is not going to solve my cancer. This is going to make it less likely to recur. It probably will come back, but this is going to hopefully make that further away or less likely.
They were direct with me and clear about the chances and the intent behind each portion of the protocol and the surgery. They recommended that I reach out to other people. They said, “Here are your scans. Here’s your information. You can send it to these people or whoever you choose and see what they recommend.”
I had also seen a local oncology team in El Paso, and they said, “Full disclosure: we see certain types of cancer, and this is a really rare one. This is really aggressive. You need to go to the best in the country, and we’re not them. But here are different people to talk to.”
Everybody recommended pretty much the same protocol. All of what the best people in the industry recommended was consistent, so I didn’t have concerns around that. I felt like all my questions were answered. When it came to deciding whether or not to do portions of treatment, I decided to do every step that would increase my chance of success and decrease recurrence, and I had the benefit of having no risk factors that would preclude me from doing those things.
Chemo Before Surgery
I got my PICC line put in on January 13th, which was great, and started chemo around January 15th. I was on a pretty heavy dose. I think it’s called doxorubicin; it’s called Red Devil as a slang term. I had that on Mondays. Then I had four days of what’s called AIM treatment, basically a chemo that’s formulated for your size, spread out over however many days they need to give you your dose.
Then I had a Mesna bag, which is a continuously pumping bag that provides protection for my kidneys and bladder. The Red Devil is cardiotoxic and can be, I guess, brain toxic, so there’s medicine for that, and then I had the bag the rest of the time to continually flush my kidneys and bladder to help protect those. That would be a week of that, a week of feeling like crap, having all my levels go down — my red blood cells, white blood cells, and platelets — and then a week of trying to get back up into a range where I would qualify for chemo again.
It was that three-week cycle. I think I had six of those for 18 weeks. It ended up taking around 20 weeks because I wasn’t always able to qualify back towards the end of my treatment.
Hair Loss and Shaving My Head
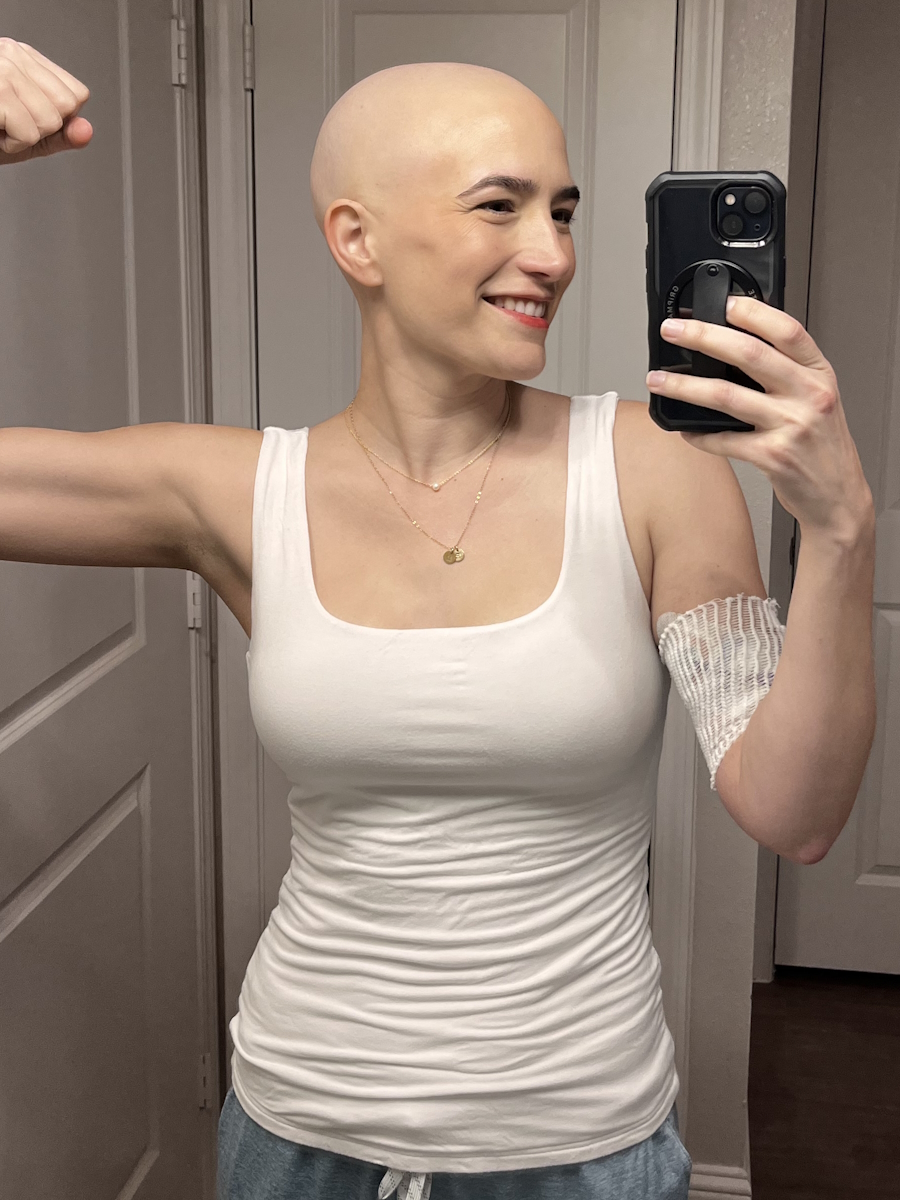
It was crazy how fast my hair fell out. I thought weeks in, I was going to start having hair fall out, and it was not like that. I think it’s that Red Devil; I think that’s what most people experience. It came out in clumps. I had long, thick hair, so I’m used to being able to play with my hair, pull on it, braid it, and it keeps on ticking. But I would run my hands through my hair and hair would be falling out everywhere, even my body hair falling out, which was weird.
When I was having all the clumps fall out, I was getting big bald spots and my part was super wide. There were big sections with no hair. I’d already cut my hair short coming into this, and I decided that the next time I was home — because I was trying to see my kids on my recovery week for the two days before I went back to restart chemo — I would like to shave my head since it looked like it was all going to fall out. That was after my first cycle.
I had my kids shave my head at a chain place that does free haircuts for cancer patients who are transitioning, so that was free of charge. They let my kids hold the clippers. My son didn’t want to, but he watched. I just wanted it to feel not scary, not for me to come back and look completely different. The hair was the first thing. I didn’t feel so bad at first, but each successive chemo cycle, each time I did chemo for a week and then recovered, it got worse.
Chemo Side Effects and Lasting Impacts
I was more sick. I had cognitive impacts from the Red Devil, like I didn’t know where I was or couldn’t think. I still have that. I have memory issues now, short-term memory problems, and it feels like a lot of my memory during that time was wiped. Almost all the stuff they list — fatigue, nausea, weight loss, weight gain, bloating, sensitive skin, hair falling out — you have at least some of it.
The thing that I didn’t experience, which I’m grateful for, is pain from the shot to stimulate T cell growth from my bone marrow. Bone marrow reproduces rapidly and is disproportionately impacted by chemo, hence your white blood cell, red blood cell, and platelet counts go down. You get this shot to stimulate T cells to get you some white blood cells. A lot of people have a lot of pain with that — acute pain — but I didn’t have any, so I was grateful for that.
Anticipation and Strategy for Surgery
I was excited; I was so excited for surgery. I knew there was potential for a negative outcome, but it felt like no matter what, it was probably going to be better after surgery in some way. Two of my best friends came in town — one I’ve known since I was two, and one I’ve known since sixth grade — and they stayed with me before surgery so I could say whatever I was feeling, just be honest, just experience it and not be performative.
On the day of surgery, I felt like I was informed about what the doctors were going to do. I felt supported by the care team. I asked a lot of questions and all my questions were answered beforehand. I was concerned they could go in and decide they needed to remove my whole right lung, which would have reduced my lung capacity and put strain on my heart, which was already affected by my chemo. That affects how you move around through the world and what other illnesses down the road may do to you. I knew there was this domino effect of how bad it was going to be when they got in there.
They were going to remove it en bloc, basically take everything out that it touches, plus a range around it. I knew it could affect my pec muscle and my breast — my pec muscle is function, and my breast is form, aesthetics, ego, and self-image. I knew I’d be waking up bald with no lashes, so I was like, “Okay, hopefully it’s the least scope possible.”
Surgical Outcome and Sharing Tumor Photos
When I woke up and they said they’d only taken one lobe of my lung and we thought they had clear margins, I was so thrilled. I was so excited. I felt so happy. The first thing I told my mom was, “Okay, now I can sign up for a marathon next year and do that. We’ll see.” It might be a walking marathon because I’m actually not that into running; I don’t know why I said that.
The reason I chose to share [tumor photos] is that I’d be super curious if someone said, “I had this tumor removed and it was this big.” I’d be like, “How big? How vascular was it? Where was it?” I have those questions, so I felt comfortable showing someone. I also thought it was cool that two ribs were involved. I thought it was cool that we have technology to still help me be fine with that.
Sharing on TikTok and Helping Others
After sharing my story on TikTok, I had a couple of people reach out and say, “What you’re describing, I experienced that, and I went to a doctor, they said it was fine. They ran my blood tests and they said it was fine. What should I do? What do you think?” I said, “I’m not a medical professional. I don’t have any medical training at all. But if you feel like your questions aren’t being answered by the doctor you saw, I think you should go see someone else and write down what you’re going to say and the questions you’re going to ask before you go in, so you feel less confused and more confident. This is what I asked for in your situation, but, obviously, yours might be different.”
Two people got back to me, saying that they had found out they had cancer. I’m sure thousands of people saw that video, but that was moving to me. It felt like even if there is a little bit of discomfort, I’d rather share my experience and hopefully one person gets a diagnosis a little bit earlier, so they have more options and treatment. That first video was before surgery, and that was part of what drove me to do my video after.
NED Status and Upcoming Surgery
I don’t think I’m in remission yet. Maybe I don’t know the right words, but I was allowed to go back to work. I went back four weeks after my surgery. I had scans after three months and my scans were all clear. I’m NED, or no evidence of disease. I have surgery scheduled next weekend on November 1st. I think after five years of being NED, I’m considered in remission, but I think that’s how the words work.
The surgery I’m having is a reconstruction. Not cancer-related. Just repairing and helping, hopefully, maybe some scar tissue adjustments.
My Biggest Emotional Challenge
I think the biggest challenge is the mortality aspect of it, the knowledge that no matter how this goes, I’m less likely to survive as long. I’m more likely to have a more complex health outcome if I live to an older age and have something else that’s just normal that happens to older people. It’s going to be more complicated because of my history.
There’s a chance it comes back and next time, it’s not something that can be surgically removed. I’ve already had the lifetime maximum dose of the Red Devil chemo, so I can’t have that again, and that’s one of the more effective treatments.
The thing that I struggle with is that my children didn’t do anything. They didn’t do anything to deserve to have a mom with cancer. I hate that they’ll be negatively impacted by my diagnosis. I don’t want them to wonder if their mom will be at their wedding, their high school graduation, or hold their first child. It’s not as much about me and what I may or may not experience, because I don’t worry about that. I just don’t want them to miss out on something or not have the support that they deserve.
Parenting Through Treatment
To a pretty significant extent, it’s been a huge blessing to have children because it made all of this so easy, all the decisions so easy. I was going to do the hardest chemo. I was going to do the surgery. I was going to do all of it because there was no other option. After all, I needed to be there for my kids.
Maybe if I didn’t have those motivators, I would have thought longer or taken a little bit of time, or maybe I wouldn’t have gone back and asked for answers as many times as I did. But my health was more than just myself; it was for my kids. They responded in different ways to the stress of my being gone and being sick, but I don’t think they ever worried that I would be there. They were just sad at how long it was between seeing me. In that way, I was successful as a parent in protecting them from a lot of the worst parts, the uncertainty. I don’t think they felt that much. They were a very important part of my ability to move through the treatment.
Meaning of Survivorship
I guess technically it means living, right? I think it means using the time that I have and the health that I have in the best ways that I can, and never forgetting or letting go of that sense of vulnerability that allows me to appreciate my life and my kids as much as I do now. I think I took a lot for granted. I was hard on myself in ways I didn’t need to be. So I think, it sounds perverse, but I desperately want to hold on to some of the realizations that this experience has given me.
Hopes, Dreams, and Everyday Goals
I don’t think I have huge new dreams. I want to be a better friend. I want to be a better mom. I’m starting to think about giving myself a year from the date of my surgery to push myself in certain ways. I do want to do a marathon; I think I want to do it walking. I want to travel. I want to do an international trip. I have it planned a little bit. Between work and kids and everything, I want to do that. I want to be more in the moment and less in my own head, thinking about what the next thing is. I think I robbed myself of a lot of joy in fellowship with other people or being with my kids by thinking about the next thing I needed to do. That’s what I want to hold on to.
My Advice and Message to Others
My biggest message I would want people to take away is that of advocacy, self-advocacy, and trusting yourself. If you think something is wrong, you don’t think you’re getting the answers you need, or you don’t understand what you’re being told, ask again. Advocacy is not about being a pain. There’s nothing inconvenient about needing answers when you have something suspicious going on in your body.
I think that’s so important, especially in women’s health, because there are so many things going on between hormones and changes in life stages that can affect the way that you experience your own body. Those things don’t have to be mysteries. There could be something else going on. In my case, several of the doctors I saw were looking for horses. I joked with my mom: they were looking for horses, but it was a zebra. You have to keep asking questions and keep advocating for yourself.
My Thoughts on Mental Health and Hope
I don’t know that this is part of my story necessarily. It feels like it’s part of everybody’s story. Just the importance of mental health hand in hand with physical health, and not toxically positive, but a positively-oriented attitude. Visualizing success, making sure that you’re using resources that are available to you, and setting goals that are external and outside of your cancer treatment and diagnosis. Choose a concert you want to go to eight months after your diagnosis and start making plans and outfits. Whenever you feel bad, don’t feel like you have to hide it. Make sure you’re asking for help.

Inspired by Sorcha's story?
Share your story, too!
More Synovial Sarcoma Stories
Kara L., Synovial Sarcoma, Stage 1B
Symptoms: Pain behind left knee, needle-like sensation in left foot
Treatments: Surgery to remove what was thought to be benign tumor, chemotherapy, final surgery, radiation (36 sessions)
...
Jillian J., Synovial Sarcoma, Stage 3
Symptom: Pain in leg for over 15 years
Treatments: Surgeries (tumor resection, thoracotomy)
...
Marisa C., Synovial Sarcoma, Stage 4
Symptom: Small bump on the foot (stable for years, then grew during pregnancy), pain when pressed
Treatments: Surgeries (below-knee amputation, pulmonary wedge resections, segmentectomy), chemotherapy, radiation (lungs & hip)
...
Julie K., High-Grade Poorly Differentiated Spindle Cell Synovial Sarcoma, Stage 4
Symptoms: Chest and back pain after car accident, trouble breathing
Treatments: Chemotherapy, surgeries (lung resection, video-assisted thoracoscopic surgery or VATS, neurectomy, rib removal), radiation therapy (CyberKnife)
...
McKenna A., Synovial Sarcoma, Stage 3 Grade 3B
Symptoms: Insomnia, weak immune system resulting in persistent illnesses such as UTIs and strep throat, severe swelling in left leg
Treatments: Surgery (tumor excision), chemotherapy, radiation therapy (proton radiation), integrative therapies
...