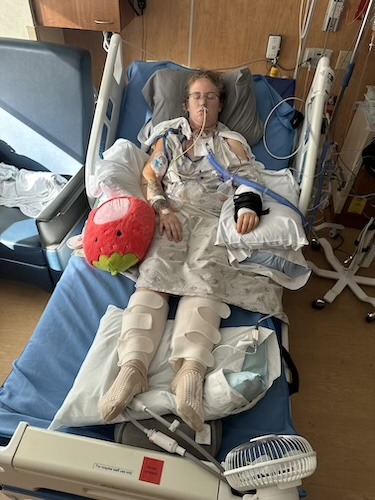
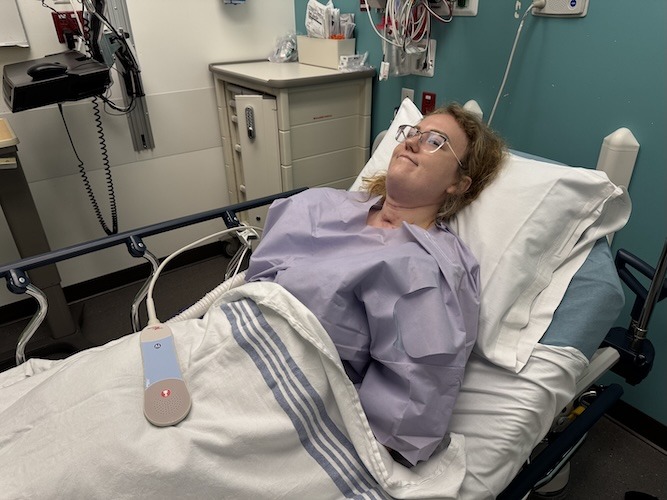
From a Small Cut to Tongue Cancer: Katelynn’s Story
Stage 3 tongue cancer (squamous cell carcinoma of the tongue) is not something Katelynn expected to hear at 28, especially when her earliest sign felt like a minor wound on the side of her tongue. She describes initially assuming the sore was from clenching and stress due to temporomandibular joint disorder or TMJ. Then came fast weight loss, reduced appetite, and severe right-sided ear pain that made sleep difficult, all signals that pushed her to seek medical care.
Interviewed by: Carly Knowlton
Edited by: Chris Sanchez
Katelynn’s primary doctor initially considered stress and even Crohn’s disease, noting that mouth ulcers can be associated with digestive conditions. An ENT visit changed everything: the specialist wanted to rule out tongue cancer and similar kinds of cancer, and performed a biopsy. Katelynn learned the biopsy result alone through MyChart on a Saturday, an experience she describes as deeply traumatizing, before care was coordinated with Oregon Health and Science University in Portland for surgery.

Katelynn had surgery the month afterwards: a 10-hour reconstruction that included a hemiglossectomy (removing about half her tongue), a neck dissection with lymph nodes removed, multiple drains, and a tracheostomy because of swelling. She also had a nasogastric (NG) feeding tube during her 10-day hospital stay and later faced an insurance denial for a necessary skin-graft step, adding avoidable stress and delay until an appeal was approved.
Radiation began in October 2024: 30 sessions, five days a week for six weeks. Katelynn describes the mask, the mounting fatigue (“dragging metal”), burns on her neck and inside her mouth, nausea, and profound side effects, including significant weight loss (about 85 pounds total across her experience). Over time, she rebuilt: physical therapy for shoulder weakness after reconstruction, speech and swallowing therapy to address a new lisp and limited mobility, and intensive outpatient therapy to process the emotional aftermath. Today, she speaks about living more openly: less ruled by anxiety, more willing to take up space, and more honest about how isolating cancer can feel once the initial wave of support quiets down.
Watch Katelynn’s video and scroll down to read the edited transcript of her interview to delve into her story.
- A persistent tongue sore, unexplained weight loss, appetite changes, and ear pain can be easy to dismiss, especially when stress feels like a “good enough” explanation.
- It’s okay to ask for clarity and next steps when something doesn’t add up; early persistence can change the course of diagnosis and care.
- A universal truth for patients: Support often gets quieter over time. Reaching out and naming loneliness can help people show up again.
- Healing is both physical and emotional; therapy, mindfulness practices, and rehab services (PT, speech/swallow therapy, lymphedema therapy) can be part of recovery, not an “extra.”
- Transformation can be real: Katelynn describes moving from debilitating anxiety to living more authentically and taking up space in ways she couldn’t before.
- Name: Katelynn R.
- Age at Diagnosis:
- 28
- Diagnosis:
- Tongue Cancer (Squamous Cell Carcinoma of the Tongue)
- Staging:
- Stage 3
- Symptoms:
- Ulcer on the side of the tongue
- Loss of appetite
- Extreme weight loss
- Fatigue
- Severe right ear pain and pressure
- Treatments:
- Surgeries: hemiglossectomy, radial forearm free flap, radical neck dissection, lymphadenectomy, tracheostomy, skin graft surgery
- Radiation therapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My tongue cancer diagnosis story
- My first tongue cancer symptoms and red flags
- My initial doctor visit and possible Crohn’s disease
- Reading the biopsy result alone on MyChart
- The details of my ten-hour tongue and neck reconstruction surgery
- Feeding tube, tracheostomy, and denied skin graft surgery
- Hospital traumas, an allergic reaction, and panic with a trach
- Appealing my denied surgery and a second skin graft
- Starting radiation for tongue cancer
- Ringing the bell after radiation
- Returning to work after tongue cancer treatment and juggling rehab
- Comparing myself to before tongue cancer and starting therapy
- Speech and swallow therapy after hemiglossectomy
- The rarity of tongue cancer in young adults and finding peers
- Oral cancer walk, giving a speech, and community
- Ambivalence, gratitude, and ongoing healing
- New identity, less fear, and living authentically
- My advice for others going through cancer
My tongue cancer diagnosis story
My name is Katelynn. I live in Corvallis, Oregon, and I am currently 29 years old. When I was 28 years old, I was diagnosed with tongue cancer: stage 3 squamous cell carcinoma of the tongue.
I’m very passionate about animals. I like to spend time with my dogs; it is my favorite thing to do. And then I’m also passionate about coaching the dance team. I coach a high school dance team, and so that is where I invest a lot of my energy and where I like to spend a lot of my time.
My career as a stylist and cutting my hair after surgery
I began my career as a hairstylist and esthetician about a year before I was diagnosed, so I was kind of just getting started in my career. As far as my hair, I would say it was probably about six weeks ago that I was kind of feeling like I just wanted to cut off whatever hair was from before my surgery, because hair holds a lot, and I really felt like I didn’t resonate with that person anymore. So I went to work and asked my coworker if she would cut my hair. She’s been cutting my hair for a long time, and I asked her if she would cut the remainder of the previous color off my hair, and I was prepared for however short that was going to be. We ended up cutting off about 6 to 6.5 inches. So it was just a fresh start.
My first tongue cancer symptoms and red flags
Originally, what I first noticed was on the right side of my tongue, I had what I thought was just a small wound. It kind of just started as a little bit of a cut. I suffer from TMJ, so I have a lot of teeth clenching, even before all of this, and I just figured that because I was stressed at the time, I was probably clenching and rubbing my tongue a lot on my teeth. So I would say I ignored it. I kind of ignored it and just kept going about my life. I first noticed that probably around February 2024.
The next thing that I started to notice was that I was having some weight loss. Again, I was attributing that to stress in the beginning. Then I started realizing that it was happening pretty quickly. I started going down in clothing sizes pretty quickly, and other people were commenting, “You look like you’re losing weight, you look so good,” and I was like, “Thanks,” but I felt that something wasn’t quite right. That went on for a couple of months. Then my appetite changed. All of that I felt at the time that I could attribute to being stressed because life is stressful, and that is what I was chalking it up to.
Then I started having some pretty severe ear pain on that right side that was not going away, and a lot of pressure. It was making it really hard to sleep at night, with lying down and having pressure on my head. That is what finally, after all of those things, brought me in to ask my doctor.
My initial doctor visit and possible Crohn’s disease
My doctor originally was not sure. I was going through some pretty big life changes at the time, and he said my symptoms could also be stress. But with the weight loss and the lack of appetite, he said that raised a red flag for him for Crohn’s disease or some sort of digestive condition. He said that a symptom of Crohn’s disease can be mouth ulcers, and he thought that that could potentially be what was going on with my tongue.
He put in a referral to the ear, nose, and throat doctor in Albany. He said that I was going to get a swab for Crohn’s disease. When I got there, and the doctor from the ear, nose, and throat office looked at it, he immediately said he wanted to rule out that it was tongue cancer and asked if we could do a biopsy. I was like, “What?” That was the first time that I had heard of it. My doctor and I, that was not the first place that our minds went, and I had never really heard of this type of cancer before either.
I was diagnosed in August. My symptoms originally started in my mouth in February, so it was for a pretty good chunk of time that I was chalking it up to being stressed out.
Reading the biopsy result alone on MyChart
The reaction was pretty traumatizing because I did not actually hear it from anyone. They did not call me. I read it in MyChart when I was home alone on a Saturday, so I could not call the office, and that was pretty traumatic. My mom and my brothers came over and were helping me stay distracted until we could call the doctor’s office on Monday.
We called, and then the ear, nose, and throat doctor called us back and confirmed that tongue cancer is what it was. They got the ball rolling by talking about doing a referral to OHSU in Portland, which is about an hour away. That is where I ended up having my surgery.
I was diagnosed in early August, and my surgery was on September 13th.
The details of my ten-hour tongue and neck reconstruction surgery
We went up to Portland because the surgery was really early in the morning, and all of my family was there waiting for me. It was really helpful to wake up to and have people there. The surgery was ten hours. It was a total reconstruction. I had a total neck dissection with lymph nodes removed because when they got into the surgery, they looked enlarged or inflamed, and so they removed them to be able to get clear margins.
I had two drain tubes on the right side and one drain tube on the left side, and that was pretty gruesome. I had those for almost the whole hospital stay. I also had a tracheostomy tube for my airway because there was so much swelling in my mouth.
As far as the actual reconstruction itself, they removed about half of my tongue; I had a hemiglossectomy. They replaced it with tissue from my arm. There are pictures, but it is a pretty good size. They also used this artery right here in my neck to reconnect the blood flow so that the tissue on my tongue could continue to get blood flow to stay alive.
Originally, when they first did that, my tongue was the color of my arm, which is pretty pale, and now over time it has adjusted. It is still lighter; you can tell, but it picked up color after the first couple of days, which my family and I thought was really interesting. So it was a pretty intense surgery and a lot of anesthesia.
Feeding tube, tracheostomy, and denied skin graft surgery
I was very groggy for a couple of days. They placed a feeding tube in; I had an NG tube in my nose because I was not able to eat at first. The hospital stay was ten days, and I had my NG tube removed on the last day.
The trach tube I got sent home with was an airway for the second surgery because after they took the skin from my wrist and put it on my tongue, they had to replace that skin with something else. Science is very cool. They took a patch of skin from my thigh in the second surgery and replaced it with the tissue here on my arm because that is the most similar.
Originally, I got sent home from the hospital with the trach tube before that second surgery in case of swelling. I got a notification the day before my second surgery that my insurance had denied the second half of the skin graft, which was pretty traumatizing. The trach in the hospital and afterwards was probably one of the biggest sources of trauma for me. It is just not a fun experience, and caring for it at home was not overly fun.
Having to have that for that extended period of time and then going up to the hospital to have it removed without having the surgery was kind of a bummer. I was like, I could have gotten that out a whole week earlier. Of course, we did not know that, but it was tough when they canceled the surgery.
Hospital traumas, an allergic reaction, and panic with a trach
From the jump, I do not want to say every single thing that could go wrong went wrong, but there were a lot of things throughout the hospital stay. From the very beginning, it was kind of a feeling of, “Of course, this would happen to me.” There were a lot of emotions happening, but there was also a lot of pain medication, and I was very confused. I was part of the time checked out, part of the time pretty devastated, and part of the time almost laughing, like, “What is next?”
I went into all of this with pretty big anxiety in general, but specifically around medical needles. I am well over that now because of exposure therapy. But going into it, when I had the IV placed before I was wheeled back for surgery, the nurse had placed the IV, and my surgeon came back to go over paperwork with me and said, “Oh, they placed it in the wrong arm.” I was like, “Do you think maybe we could wait until after I am under for you to move that?” Because I am actually terrified of needles, and that was a big deal for me.
Then a couple of fairly traumatizing things happened in the hospital. The first day, I had an allergic reaction to the IV medication they gave me during my hospital stay. For the first five days or so, while I was adjusting to the trach tube, I was not able to talk.
So I was communicating by writing on a whiteboard to my mom, relaying that way, and writing notes. Having an allergic reaction with it in your bloodstream and not being able to communicate what is going on, and that triggering a panic attack because of the anxiety from the hospital, made it a very exhausting first day. That was pretty emotional because in the moment, there was a lot of “Why is this happening to me? Why is this happening to me?”
Vomiting with a trach and ongoing hospital challenges
The second day, with my NG tube, my stomach was not reacting very well to the tube feed. I kind of have a hard time with eating stuff anyway. Sensory-wise, I have struggled with food already from before, and my stomach was very queasy.
On the second day, my stomach was not having it, and I started projectile vomiting in the hospital room. Having a trach tube in place made that very traumatizing. I could not talk, and the nurse and I were just looking at each other wide-eyed, like, “I really hope this does not turn into a choking situation.” It was very traumatizing.
By the time all of these things had happened, and then for my insurance to say, “Well, actually this is cosmetic,” is what it was first referred to as, I was like, of course, of course that would happen. You get to the point where you are like, yeah.
My emotions throughout were all over the place. Once I started moving more into treatment and radiation, there were a lot more down days and sad days. But freshly after surgery, my emotions were honestly kind of all over.
There was one time when we had first gotten home, and I still had my trach tube in. My mom was driving; I was not driving. All of a sudden, her car just started dying, and we had to pull off onto the side of the road. I do not know if it was the pain meds or part of this mindset of “Of course this is happening,” but I laughed — uncontrollably laughed — for like 15 minutes. She was at the point where she was concerned.
It was just trying to find something light-hearted throughout because, overall, tongue cancer is a very devastating experience. Being able to look back and laugh a little bit at some of the times that were a little light-hearted is helpful in healing.
Appealing my denied surgery and a second skin graft
We ended up not having to pay out of pocket. We had to file an appeal. My mom was helping me a lot through this, so I do not know exactly how it all worked, but I know that we called and filed an appeal. The appeal got denied at first.
During that time, I went up and they removed the trach tube. My surgeon checked in, and I had a bolster on my arm that was covering the donor site while the skin was healing. We did an exam during that time, and my surgeon said, “I have never seen an insurance do this before.” Of course, you have not.
She went to bat for me and wrote a letter for me to send, explaining why this was a necessary surgery. Right, we had already taken the skin off; we had to put it back on. That was helpful. We did a second appeal, and after that, it got approved.
I ended up having my second tongue cancer surgery, I think it was October 10th. My original surgery was on September 13th. I was in the hospital for ten days, so I think it was about two and a half weeks by the time I was able to get in for the second surgery.
Starting radiation for tongue cancer
I started radiation on October 31st, 2024, and I finished on December 11th, 2024. So yesterday was one year since I got to ring the bell after completing treatment.
My daily radiation schedule and mask fitting
I did 30 rounds of radiation. It was every day, five days a week, for six weeks, so Monday through Friday. I remember they gave me an option on the time of day, and I did most of my appointments in the morning so I could get it out of the way.
Thankfully, I was able to have radiation down here in Corvallis instead of up in Portland, so I was not having to commute an hour to go. I was only going to the hospital in Corvallis, about ten minutes away from my house. My mom, my dad, or my partner, whoever was available, would take me because it was a good chunk of time.
Radiation was tough. They had warned me about it. By the time I started radiation, I had healed for about six weeks after surgery. They want you to heal from surgery before you start so that everything can heal before it gets damaged again. During that time, I had started to feel a little better.
I had felt bad for so long with fatigue, ear pain, mouth pain, and all the things. Even though the surgery was gruesome, after I had started healing from it, I was like, “Okay, I am feeling better because I am not feeling all of these things I was feeling before.” I was also on pain medication during that time, which helped. I was starting to feel almost back to normal.
Then I got started with radiation. The first couple of times are anxiety-inducing. For the original appointment, they fit you for the mask, which you have to wear every day. They bolt you down to the table, and it is pretty much as tight as your skin. There are little holes in it that you can kind of breathe through, and then there is a mouthpiece that goes inside your mouth.
The first couple of days were really stressful and scary, but there were not really any physical side effects right away. So I thought, “Maybe this is not as bad as surgery, maybe I got this.” Then you get through the first couple of weeks, and you start to feel a little tired, but it is not so bad. Then, by the third week through the sixth week, it really quickly goes downhill. That was a struggle, after feeling like I was starting to make progress, to start feeling so bad again.
Radiation side effects: weight loss, burns, and fatigue
Some of my side effects during radiation: I continued to lose weight throughout this time. Over my entire tongue cancer journey, I lost about 85 pounds, and that was in a fairly short period of time. I was feeling really puny, frail, and very weak overall.
By the fourth to sixth weeks, I started to get pretty significant burns on my neck. My doctor gave me a cream to help with it, but if you are getting hit with a laser every day for 30 days, it starts to take effect over time. That was happening inside my mouth as well. That contributed to the weight loss because you have to eat to stay sustained, and that is hard to do when you have blisters, burns, peeling skin, and just really not fun stuff.
That was pretty tough. Fatigue was a big one. People warned me, people I know who had not gone through the same type of radiation, but other types. They tried to warn me, but it is like a kind of fatigue where your bones feel like you are dragging metal. It is really hard to even stand up to go to the bathroom because you are so tired.
I have stairs at my apartment, and doing that every day to go to treatment started to get really tough towards the end. I would say those are the major side effects. My nutritionist weighed me once a week during radiation to make sure I was not losing a significant amount of weight, because that is common. It affects your appetite; your taste changes, things taste metallic, and nothing sounds good.
They try to keep an eye on that, and you work with a nutritionist so they can recommend protein shakes or whatever. There were a couple of times that my nutritionist was maybe urging me to consider getting another feeding tube, not an NG tube, but a PEG tube in my stomach, to help balance the nutrition I was lacking.
After my experience at the hospital, I really did not want to do that. Maybe I should have accepted, but it felt like too much for me. So I pushed through and tried to maintain. I was drinking a lot of very high-calorie shakes, lots of smoothies, lots of ice cream, to try to maintain or lose very little weight at a time. That was hard.
The emotional toll of daily radiation with no light in sight
To be honest, there really was no light at the end of the tunnel until weeks after ending treatment. I cried most mornings before I had to go. I experienced a lot of nausea. I would be crying and gagging and saying, “I do not want to go,” and my mom would say, “Honey, you have to.” The people around me literally scooped me up and picked me up and made me go.
It is hard to explain. I have gotten a lot of comments over time, and everything is well intentioned, but I hear a lot of, “At least you’re young, so maybe it is not affecting you as badly, or maybe you can bounce back quicker.” But it was the most tired I have ever been. Even though I was the most frail and the lightest I have ever been, it was the heaviest my body has ever felt. It literally felt like I was dragging around a bunch of concrete bricks.
By the time the burns started happening, it was even more so that I did not want to go. When you put the mask on, you are lying on the cold table, the mouthpiece is inside your mouth, you have burns everywhere, and it tastes bad. There is literally no other way to explain it than you just have to go.
By the time it was, “Okay, you have one treatment left,” that was when I felt a little bit of light. But I did not have it in me to be excited about finishing because of how tired I was.
Ringing the bell after radiation
I was able to ring the bell. I had two radiation providers. I had my oncologist, whom I met with once a week, and that was pretty much just a “hanging in there, okay?” visit. We did medication check-ins, and he was able to prescribe me some lidocaine that I could use on a Q-tip in my mouth. It was short-term, but it helped me try to get nutrition.
I would meet with the nutritionist, but I saw my radiation techs, the same two, every single day. On the last day, they said all of my family could come back, and they were all back there with me when I rang the bell.
That was pretty emotional in a way that felt like a big breath of relief — like, “Okay, that is the last time that I have to do that.” During radiation, both of my front teeth got chipped because dental care is very hard during all of this. There were lots of reasons I was eager to be done.
That final time and ringing the bell for completion was a big sigh of relief that I could go home and sleep for the next week and not have to get up for an appointment the next day.
Returning to work after tongue cancer treatment and juggling rehab
I am a year out. In the beginning, it was really rough. I returned to work at the beginning of February, about a month and a half after I completed my tongue cancer treatment. Physically, I was not quite ready, but I did not realize how mentally not ready I was until I got back into the swing of things. It is very weird to step back into your old life when you feel like a completely different person.
In the beginning, especially with what I do for work, it was tough. Being a stylist is a lot of standing and using your arms. I did a lot of physical therapy to regain strength in my shoulders because after the reconstruction, all of this was very weak.
I had to rebuild my stamina. It was tough balancing going back to work, tiptoeing back into dance a little bit because I was trying to heal my heart, too, not just my body, and also attending speech therapy once a week, physical therapy for my arms once a week, and lymphedema therapy once a week.
There were so many appointments. It felt like, for my energy level at the time, there were not enough hours in the day to do all of the things, and also rest and give myself permission to rest without being upset with myself if, on a Sunday, I did not have the energy to get up and clean because I was working.
Comparing myself to before tongue cancer and starting therapy
That was tough. I did a lot of comparing myself to my abilities before, which was really hard. I could not see as many people in a day, I could not work as long as I used to, and before, I was building my career and working all the time. Trying to chase that was hard in the first while.
It got to the point where I was really having a hard time around July last year. That is when I got back into therapy, which is something I probably could have used that whole time, but I did not have the energy for one more thing.
When I got to the point where I was a little more physically healed but feeling really mentally bad, I got myself into therapy. I enrolled in an intensive outpatient therapy program, which was ten hours of therapy a week. It was a lot, and I did that for about two months. It was pretty life-changing for me.
I had done therapy in the past, but being able to rebuild my tool belt of ways to process through things was extremely helpful. During that time, I started leaning into acts of mindfulness. I had spent a lot of time in my head and by myself.
I started finding ways for that to be more of an outlet: journaling, yoga, breathing exercises, all that stuff that people say is good for you. It is easy to feel like you do not have time, but I started carving out time to be intentional about finding ways to be present.
A big helpful thing is leaning into gratitude and finding things that I am thankful for. With all of the bumps in the road, I have had to find reasons to be happy to be alive when I was feeling near death. That is something I have tried to continue to lean into now because it helps reshape my mindset to get through the week.
Speech and swallow therapy after hemiglossectomy
I did speech and swallow therapy once a week for maybe three or four months. That was pretty interesting because speech is, for the most part, not something I ever thought about beforehand. It just happens naturally.
We had to find ways to break down how to talk: how to place your tongue, how to push air, and in what direction when you are talking. It was very interesting. When I originally had my surgery, and before I started speech therapy, I had a pretty strong lisp that I had not had before, because when they did my surgery and reconstruction, they essentially tongue-tied one side.
With the limited mobility in my tongue that I did not have issues with before, that really affected my speech. My surgeon had told me that swelling occurs for up to a year, so that was also a big thing: working through things while the swelling continued to go down.
Gradually, as that happened and through the speech and swallowing exercises, my speech improved. I would say if I am speaking to a client and they do not know about my history, and it comes up, most people say, “Oh, I would not even be able to tell.”
I am thankful because there was a point when I would get pretty down on myself if I was out and about or on the phone for doctor’s appointments, and people would say, “What?” or ask me to repeat myself. That was pretty emotional because I was trying.
I took my exercises very seriously. I would go in for my appointments, and they would say, “You have to read these words 30 times, enunciate, and slowly break them down.” I took all of that and went home and did all of my exercises because I am young and hopefully have a long time to live, and I want to be the best I can be for the rest of my life.
Even if I was tired, I was doing all of my physical therapy and speech exercises. My speech therapist told me she could tell I was taking it very seriously.
With the swallowing exercises, during radiation, you can get some restriction in here or even fibrosis in your muscles from not using them and from them getting radiated. My speech therapist said that because I continued to use those muscles during speech therapy, for the most part, everything is operating at normal functioning, whatever that means. I do not have any restrictions, which is good.
The rarity of tongue cancer in young adults and finding peers
Tongue cancer is rare, but it is a lot less rare than you would think. I do not know specific statistics, but it is something that is becoming more and more common. When I was discussing it with my doctor, he said that the reason it did not originally come to mind is that I do not fit the typical criteria for who usually gets tongue cancer.
My surgeon explained that historically, tongue cancer is typically found in people who are 55 and older, people who have smoked for a really long time, and there are other factors. But it is becoming more common in young people.
As far as locally to me, I have not found a support group in person, but I did join several online support groups. Through them, I have been able to make connections and meet people from all over who are closer in age to me, which has been helpful in healing.
Of course, I can resonate with other cancer survivors at the radiation clinic, but when you are the only one below 60 in the room, it can be pretty isolating. Finding connections — being, as I sometimes say, in the club that nobody wants to be a part of — has been helpful when it is people my age.
Being able to see them continue to work, build their lives, and keep going provides me and others with some sense of community and hope. If you are earlier in your journey, seeing people similar in age get back to things they love is very healing.
That is part of why I am open to sharing. I have made connections through support groups with people who are earlier in their journey and looking at what I am doing now. That is why I am open about sharing that there is life afterwards.
Oral cancer walk, giving a speech, and community
Locally, I got connected with the Oral Cancer Foundation. Kyle Isaacs is the local organizer who sets it up and runs it. She works in the dental field and is just a great person. This was maybe the fifth year that they have done an oral cancer walk.
I got connected with her and was able to do that this past September. The walk fell on my first anniversary from my surgery, which was pretty cool. She invited me to come and give a speech, which was pretty cool. That is not something I would have signed up to do before, but it felt like it was meant to be.
That event was really, really cool because I could connect more face-to-face. There were a couple of other survivors or family members of people who had been affected by the same thing. Being able to connect more in person and have that face-to-face interaction was super healing.
I have been keeping an eye out for any other opportunities. It would be cool to find something like a group, because when I did therapy, it was group therapy, but online and not necessarily cancer-related. It was more general, which was helpful.
The feelings that come with having cancer and going through treatment, especially at a younger age, are very complex. It is hard to explain to people. Unless you have been through it, it is hard to fully get it.
That is still something I would be open to: finding something a bit more local because even though I am about a year out, a year and a half out from surgery, and I am doing well, there is still more healing.
Ambivalence, gratitude, and ongoing healing
Something I learned in therapy is tolerating feelings of ambivalence, which is feeling two emotions about a situation at the same time. As I go into my healing journey, there have been times when I have said, “I am healing,” but it is hard to move on.
Understanding that I can be grateful and also grieving and devastated at the same time is something I have had to learn to live with. Although I am having good days and finding ways to be thankful, getting back into the swing of things, and feeling like I am living authentically, I have equally bad days.
I think it would be helpful to find a more in-person, intimate group.
New identity, less fear, and living authentically
I would say that yes, I look at life differently, and I do feel like I have a new identity. Before tongue cancer, anyone who knows me in my personal life would say I was a very anxious person. Going to the grocery store by myself was scary. Playing my music too loudly at a stoplight was too scary. I never wanted to take up space or draw attention.
Now I live authentically, however I want. Within reason — I am very empathetic and deeply feeling — so it is not like I am living wildly, but I will go to a coffee shop, order coffee, and sit there and drink it by myself.
A speech like that oral cancer speech is not something I would have been open to doing before. Now I take opportunities. I say yes a lot more often. I do not live in fear of other people looking at me.
Any time the sky looks pretty, I pull over on the side of the road, get out, and take a picture of it, and I do not care how many cars drive by and see me doing that. Before, I would have never done that because I did not want people to see me or ask, “What is she doing?” I have now realized that none of that stuff matters.
I have said “new identity” a lot, and I have recently been feeling more like I have come back to myself. Day to day, every day, you are a new version of yourself because you are always evolving. But I feel like I live the most aligned and authentic and present that I have since I was probably a kid.
It has been healing, doing a lot of self-reflection. I have spent a lot of time alone, really learning how to get comfortable with myself, appreciate life, and figure out ways to heal and be present and thankful for this second opportunity at living that I was given.
My advice for others going through cancer
That is so hard because everybody is different. Part of me now wants to say, “Try to find the good,” but thinking back to the version of me in the thick of radiation, I am not sure she was able to see anything good. So I am hesitant to say that.
I would say, just hang in there, honestly. From my perspective, even though there have been rough things along the way, I have not had chemotherapy, whereas other people do, and I have never had a recurrence. Some people have a recurrence. Some people have totally different types of cancer.
It is hard to say “hang in there” because I am putting myself in my own shoes. Some people have a harder or more extended journey, or terminal diagnoses. It is hard for me to say “hang in there” if you have a terminal diagnosis.
Overall, if you can, try to find even one thing to be grateful for. Even if it is just, “I am thankful for my dog,” or “I am thankful to be able to take a nap after this treatment.” Find any way to get through the day because it can get pretty dark.
Isolation during tongue cancer and reaching out for support
I think the surgery, radiation, and what comes afterwards are the major pieces. Something I want to touch on a bit, that I have heard as a common theme, and maybe another PSA if you are early on, is that people talk a lot about how isolating cancer and treatment can be.
Going into it, I did not really understand what people meant. There is a period after you get diagnosed when you try to go a while without sharing. I am a pretty private person, and it was hard for me to announce that I had this big change happening. But with work and having to take time off, I had to.
When you first reveal devastating news like that to people, it feels like everybody drops what they are doing and is really there for you. There were so many people who stepped up in incredible ways that I am eternally grateful for.
But there is also this time period when that starts to quiet down, and you are still moving through the motions and going through these changes. Everybody still cares, everybody still reaches out, but they are also living their own lives.
If you are in the thick of that season right now, a piece of advice is to reach out when you have the energy. Try to find community, whether that is through a support group, your family, your friends, or however you need to keep people around you.
There is no ill intent, but it does sometimes feel like, where is everybody, where did everybody go, when it is so loud in the beginning. That was something that was hard for me to process. Looking back, there were still people showing up in beautiful ways all along.
When it is so loud and huge and big, and you are getting hundreds of people reaching out, and then you get into the thick of radiation, and it is real quiet, real dark, real lonely, that is when it feels isolating.
If you have the energy, try to reach out and let people know when you are having those feelings, and do not try to hold onto that by yourself.

Inspired by Katelynn's story?
Share your story, too!
More Head and Neck Cancer Stories
Vikki F., Head and Neck Cancer (Nasal Squamous Cell Carcinoma)
Symptoms: Nosebleeds that persisted for years, nose changed in shape, nasal pain, migraines
Treatments: Surgeries (subtotal rhinectomy, reconstruction surgery including radial forearm free flap, bone grafts, and cartilage), chemoradiation
...
Red S., Tongue Cancer (Squamous Cell Carcinoma of the Tongue), Stage 3
Symptom: Persistent tongue ulcer that increased in size
Treatments: Surgeries (partial glossectomy, flap surgery), radiation therapy
...
Alyssa N., Adenoid Cystic Carcinoma
Symptoms: Persistent jaw pain, lightning-like facial pain during the first bite of meals
Treatments: Surgery (tumor removal), radiation
...
Eva G., Oral Cancer, Stage 4
Symptoms: Sore on the tongue, which caused pain during eating and speaking; changes in the color and texture of the tissue where the sore was located
Treatments: Surgery (partial glossectomy, radical neck dissection, reconstruction), radiation
...
Teresa B., Recurrent Breast Cancer (Hormone-Positive), Oral Cancer (Lip Cancer), and Skin Cancer (Melanoma)
Symptoms: Lip cancer: chapped lips & a pimple-like growth on lip, breast cancer: enlarged left breast with lump, melanoma: none
Treatments: Surgeries (bilateral mastectomy with reconstruction, lumpectomy, craniotomy, Mohs, surgery, wide local excision), hormone therapy, radiation therapy
...