Sammie’s Stage 4 Diffuse Large B-Cell Non-Hodgkin Lymphoma Story
At age 21, Sammie began experiencing new and unusual symptoms every few weeks. Symptoms ranged from chest pain, back pain, and difficulty swallowing to developing a bump on her neck and experiencing extreme night sweats. Multiple urgent care visits resulted in her being told by doctors that her symptoms were nothing.
Months after her symptoms first began, her face became swollen which led her to the ER. Blood work revealed that none of her levels were within range and a biopsy uncovered a stage 4 diffuse large B-cell non-Hodgkin’s lymphoma diagnosis.
Sammie shares her cancer story with us, including her experience with medical gaslighting, how she learned to trust herself and be a patient advocate, the challenges she faced of being a young adult with cancer, her experience with chemo and CAR T-cell therapy, the importance of finding a cancer community and her advice for those on their own cancer journeys.

- Name: Sammie F.
- Diagnosis (DX):
- Non-Hodgkin’s Lymphoma
- Diffuse large B-cell
- Non-Hodgkin’s Lymphoma
- Staging:
- Stage 4
- Symptoms
- Chest pain
- Back pain
- Bump on neck
- Night sweats
- Fatigue
- Vomiting
- Swollen face
- Age at DX: 21
- Treatment:
Stay strong and fight as hard as you can because it’s so, so worth it.
Sammie F.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
Symptoms & Diagnosis
Tell us about yourself

My name is Samantha. I was diagnosed with diffuse large B-cell non-Hodgkin’s lymphoma just over a year ago. I am from a small town. I like hanging out. I just got a dog which has been super fun, and I’m back to college now studying social work.
What were your initial symptoms?
Back in November of 2021, I started getting chest pain, and I really thought it was my heart because it was on my left side. Every time I took a deep breath, I felt it. Right after I felt it, I went [to the doctor] and they did a few heart tests and told me that everything looks pretty normal. They did EKGs and x-rays and sent me home.
A couple weeks later, it was still happening. I went in again and they thought that I had pulled something in my chest or said it was anxiety, and said it was nothing. Again, they did a few more tests. From then on, it was every couple of weeks, a new symptom started to develop. The next was my back was hurting super bad. That’s when they sent me to the chiropractor and thought that I had scoliosis. From there, I started developing a bump on my neck and I was having a hard time swallowing my food. I go in again and they say it’s probably just an infection, they don’t think it’s anything and they kept sending me home with steroids or something to ease the pain. It wasn’t long-term, it’d make me feel good for a couple days and then something else would happen.
It wasn’t until the end of May, I woke up, my face was super swollen and puffy, and I could barely open my eyes. I went to urgent care again. They tested me for mono and strep and said that I was negative and that it’s probably nothing, sent me home with steroids again. Throughout this time, I’m having extreme night sweats, fatigue, sleeping all of the time, and my stomach started to hurt. I started vomiting.

Getting a cancer diagnosis
It was advocating for myself and my parents advocating for me that I was able to get a diagnosis.

I went to the ER and they finally started looking at me more seriously, but they still were looking at me like “You’re 21 years old. You don’t have any health history. We really don’t think that it’s anything, but we can do tests if it’d make you feel better.”
It was advocating for myself and my parents advocating for me that I was able to get a diagnosis. Finally, when they took my blood, which wasn’t until June, none of my levels were in range. That’s when they started doing the ultrasound and the CT scan and from then on it was, you have cancer.
Processing A Cancer Diagnosis
Did you anticipate having cancer?
From being in the hospitals and going to see my primary doctor, nobody had said one thing about cancer. That was never brought up at all. If it weren’t for myself Googling my symptoms, which everybody says not to do, but I diagnosed myself before any medical professional diagnosed me. I was saying, “I’m pretty sure I have lymphoma.” I had every single symptom.
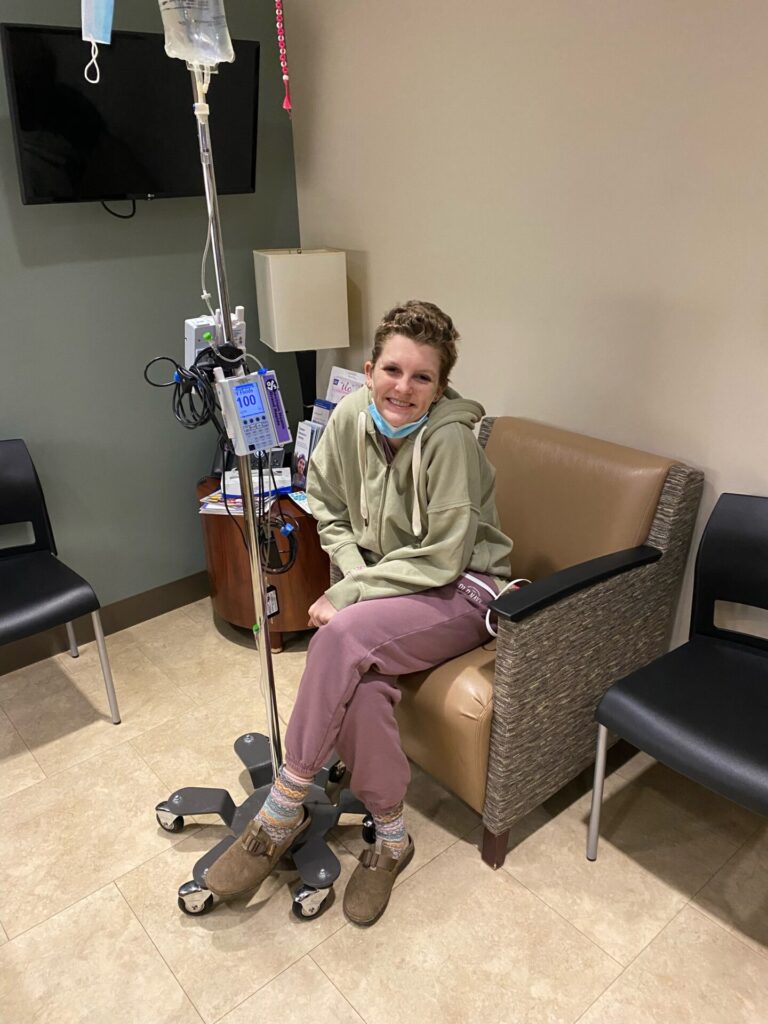
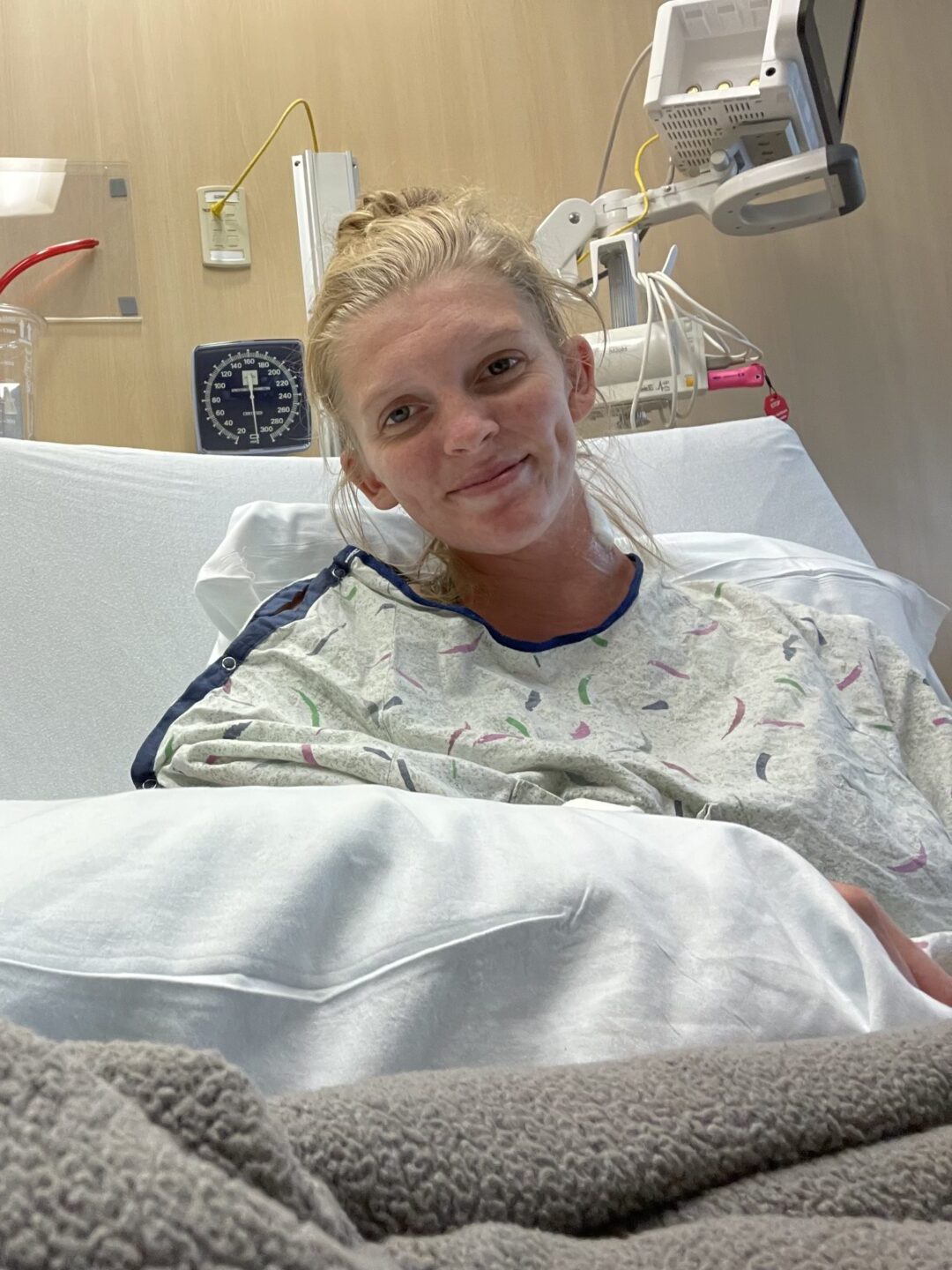

I had that ultrasound on my neck and that didn’t look good. Two days later, I had my CT scan and within a half hour of the scan, they called me and said, “We think you have lymphoma. You need to go to the hospital.” In the back of my head, I knew something was off. I knew it wasn’t going to be good, but I wouldn’t think that I actually had it.
How did you react to your cancer diagnosis?
It was a lot. It happened very quickly and it changed very quickly. I think that a lot of people might have tests for a couple of weeks at a time, thinking that they have cancer. But for me, it was like no one had expected me to have cancer. I don’t know how because I had every single symptom. But because I was healthy and had no complications ever, nobody expected it. My life changed very, very quickly and it was very scary.
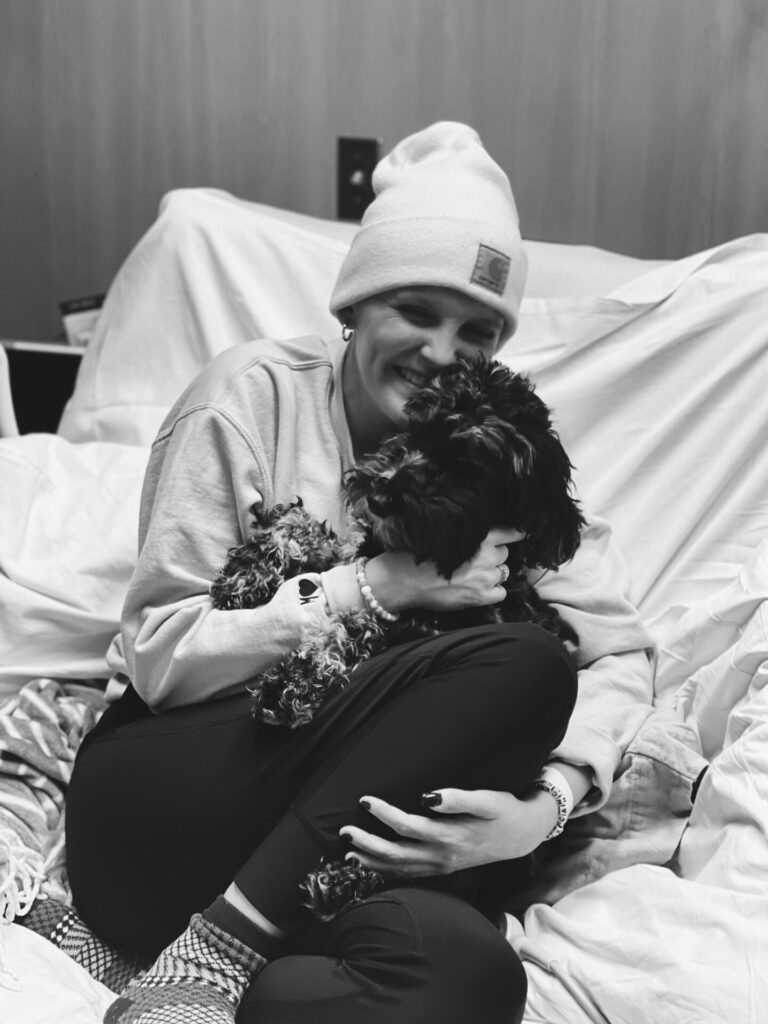
I was saying, “I’m pretty sure I have lymphoma.” I had every single symptom.
»MORE: Reacting to a Cancer Diagnosis
Describe the medical gaslighting you experienced
I felt like every time I went back, I’m just saying the same things over and over and over again. Every time, I would tell them every symptom from November that I had and it was something new every couple of weeks. It started with the chest pain, then the back pain, then the lump, then vomiting and getting sick, being so tired, and super intense night sweats. They would just say, “Oh, you probably just had a fever and you broke your fever.” But it wasn’t like that. It was really, really intense night sweats. It was super frustrating.

I’m super grateful that I had my parents advocating for me too, because I was starting to doubt myself. I’m like, am I just being dramatic? What is going on? I’m not one to complain about stuff like that. I knew deep down, something’s definitely wrong, but when you’re constantly being told you’re fine, nothing’s wrong with you, you start to believe it.
Chemotherapy
Beginning chemotherapy
Once I got to the hospital, I was admitted into the ER and then they sent me up to oncology. Still, at that point, nobody had answers for me. Nobody really knew what was going on. I was admitted on June 22nd and I was there the next 11 days. We had to wait a couple days because of the biopsy and you have to wait for results. Basically, they had a set plan of what we were going to do.
»MORE: Chemotherapy FAQs & Patient Stories
The second I got my official diagnosis, we started treatment right away. Starting treatment, within the first hour of chemo, my bump was completely gone on my neck and I instantly was starting to feel better. It was crazy how fast that happened. They knew exactly what chemo to do. I did the R-EPOCH regimen. It was 5 days of chemo, 5 days straight, and I would go in on Wednesdays to get my bag changed. I could take my chemo home with me, which was super nice, but it just wiped me out completely. It made me super, super tired.
My body handled the chemo pretty well, I think because I’m young, but it made me super exhausted. I did 6 rounds of that R-EPOCH chemotherapy, and then I did 2 rounds of methotrexate.

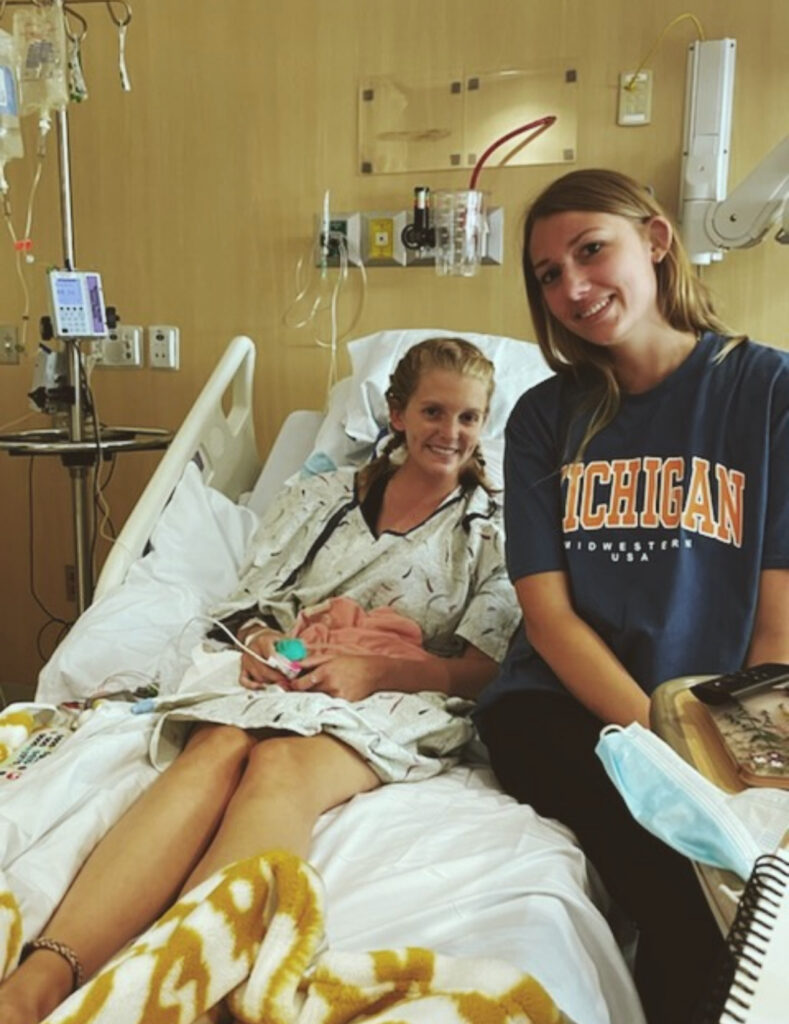
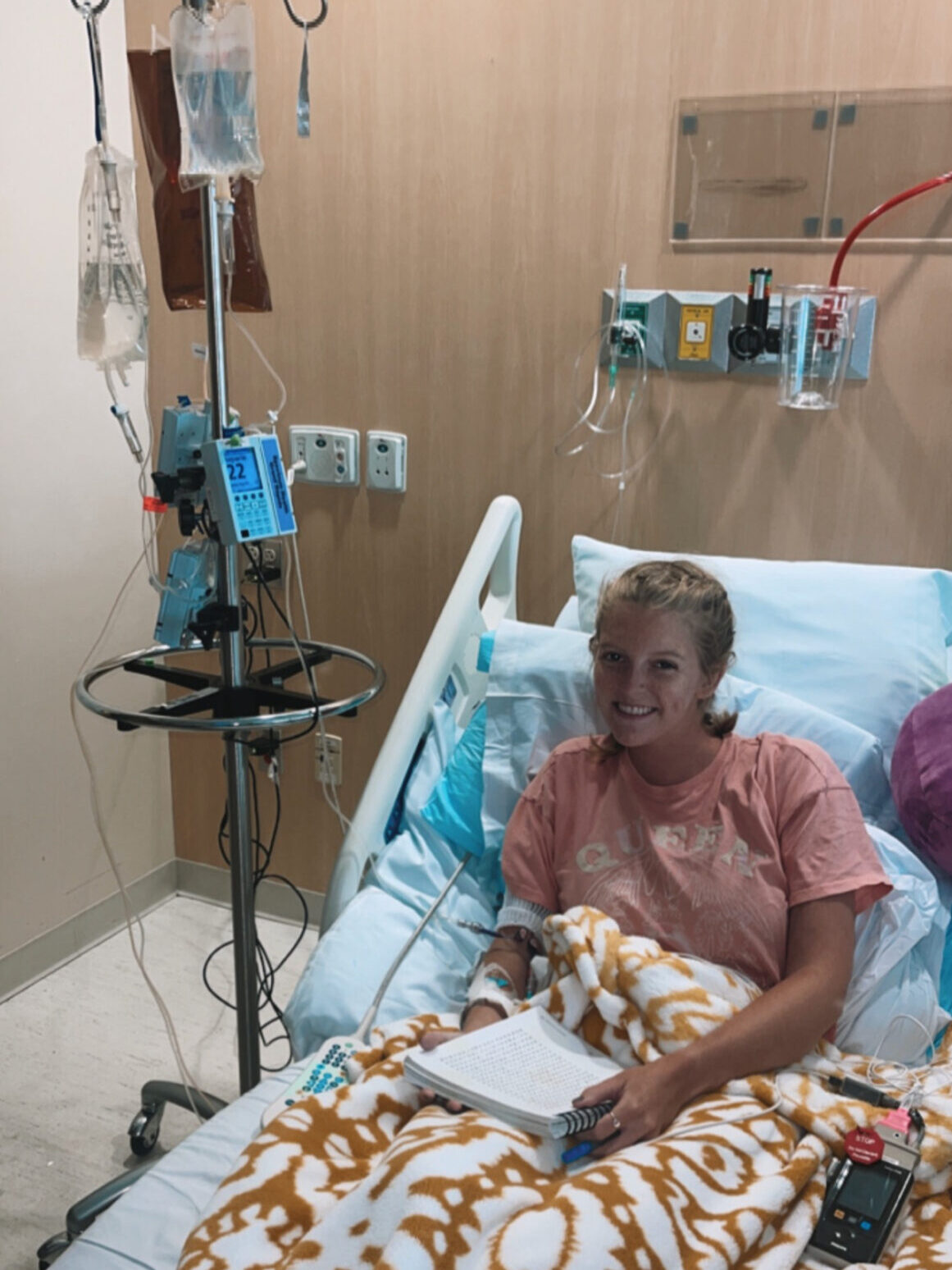
What side effects did you experience from chemo?
The first round of chemo that I had, they discharged me from the hospital. I was doing good at that time. The next day, I got super, super sick. I was super dehydrated and could not stop vomiting. At this point, they didn’t send me home with any nausea meds or anything. We didn’t know what to do. I couldn’t keep any of my meds down.
I instantly started feeling better because I didn’t realize how sick I had been the whole year prior. Finally, my body was being treated for what it needed for so long.
The next day I was home from the hospital, I went back to where I get chemo at. They pumped me with fluids, but other than that, I handled the treatment very well. I mean, other than fatigue. I had some random stuff that happened, but it wasn’t anything other than that first time getting sick, I never got sick again. It just made me super tired. I would sleep for 3 days straight and I was exhausted.


Honestly, I instantly started feeling better because I didn’t realize how sick I had been the whole year prior. Finally, my body was being treated for what it needed for so long. My weeks off of chemo, because I had 2 weeks in between each treatment, I felt so good. I had felt better than I had felt in a year.
What was your staging?

Lymphoma staging is a little bit different, and they explained this to me right when they told me my stage because I was stage 4. My oncologist explained that that doesn’t mean what it means for other cancers. Mine was on the lining of my lungs, which made it stage 4, but I didn’t have it in any of my organs. But lymphoma, no matter what stage it is, it’s just as treatable, just as curable.
Hair Loss



Describe your experience with hair loss
One of the hardest side effects that I had was losing my hair. That wasn’t even something that had crossed my mind when I was sitting in the hospital because I had so much to think about, and losing my hair wasn’t on my priority list. When I finally asked my doctor, “Am I going to lose my hair, because I know everybody doesn’t lose their hair.” She said, “Yeah, you’re going to lose your hair.” I was in denial.
I thought that that was the biggest deal of my life at the moment. Now, looking back, it was such a small part, but to me, it was so big. It was really, really traumatic to lose my hair. I eventually reached that point, like I think everybody does, it’s just time to shave your head because I was completely balding on my head. I waited a long time, but it started falling out about a week after my first treatment. I was shocked at how fast it was falling out. I chopped my hair pretty short so it wouldn’t be as dramatic. That was definitely the hardest side effect that I had experienced.
One of the hardest side effects that I had was losing my hair.
Trying on different wigs
We have a nonprofit organization close to my home that gives out wigs for cancer patients. I got a couple of wigs before shaving my head, which made me feel a lot better. I did not want to shave my head if I didn’t have a wig ready to go.


Once I chopped my hair, my hair was falling out in clumps and I was getting to the point where I didn’t want to get my hair wet in the shower. It got to be so much that I had accepted it. It was fine. Me and my sister shaved my head and it was fun. We didn’t make it a sad thing. We made it the best that we could. Past that, I haven’t even been sad about my hair at all. Looking back at it, I’m like, it was so silly for me to be so devastated by it because I’m so lucky to still be here and have this life. Something like losing your hair, in the big picture, does not matter.
What advice do you have for someone experiencing hair loss?

Shave your head when you are ready. If you’re good with it and you want to, you’re ready to shave your head, then do that. I had to do it when I was ready. I think that helped me get closure. I knew it was time. You will get to that point where you need to shave your head, versus in the beginning when I still had my hair and it wasn’t falling out yet. Don’t shave your head, just wait and get a short haircut. Then it’s not as drastic as a change for you. I think that helped me a lot.
Recurrence
What did scans reveal during your cancer treatment?
I got one scan in the middle of my treatment, which showed significant improvement in my mass that I had in my chest. Then I had one right after treatment. My follow up scan was February, so a couple months after. In the moment, it seemed like it was taking forever. Now looking back at it, it seemed like it went by so fast.



Halfway through my treatment when I got that scan, you could totally tell that it was so much better than what it was. It gave me so much hope and motivation that this is working. This is doing what it needs to be doing. It gave me more motivation to keep going. Because, in the back of my head, I’m going through this chemo and I’m like, what if this isn’t working? What if I’m doing this for nothing? When I would get those scans and they’d be good, it made me feel better.
I got the last scan after I’d finished all my treatment and it looked way better than what it did, but it still wasn’t great. But they didn’t want to do any further treatment, so they said, “We’ll just scan again.” I think it was 3 months after, so that was February. I got another scan and that’s when it showed that my cancer was back. The same spot lit right back up.
What was the timeline between the end of your treatment and when you received that last scan?

I finished my chemo in October 15th, and then in December, I had 1 round of methotrexate. January was my second round of methotrexate and after that I was supposed to be completely done and it was supposed to take care of the cancer. Then in February, a month later after methotrexate, that showed that my cancer was back.
How did you process having recurrence?
That was really, really hard. At that point, I was signed up to go get a new job. I was planning on going back to college. I had so much stuff lined up and I was so ready and excited to get my life back. Seeing that was just as bad as the first time, honestly. The first time getting diagnosed, it was like, okay, I’m going to do this. I can do this. I’m so strong. But the second time it was like, oh, I have to do this again. That was my mindset. I was not ready to go through that again. It sucked. It really sucked.

CAR T-Cell Therapy
What was your next course of treatment?
They again knew exactly what to do. We were going to do the CAR T therapy, which is an immunotherapy that basically uses your specially altered T cells which are part of your immune system to fight the cancer. They explained the whole process and how they take my T cells out, send them to California, they’d genetically modify them, and send them back to me.
They started the process right away. They also started the stem cell transplant process, just in case it had to come to that. They started doing a bunch of blood tests and getting stuff ready just in case this CAR T therapy didn’t work.
Everybody that I had talked to in the medical field, if they’d asked me what my plan was and I’d say CAR T therapy, they were all so impressed with this new treatment.

At first it sounded super overwhelming, hearing that I had to do this transplant. I shouldn’t call it a transplant, but immunotherapy, and being in the hospital for 2 weeks. I couldn’t drive for 2 months. It sounded like so much. I had went from finally getting a break from being in the doctor’s office and getting my blood drawn to right back to where I was back in June. I had to go get my blood drawn every week.
April 10th was when they started my CAR T therapy, and I was there for 2 weeks taking my cells out. It took about 6 hours, but putting them back in after they had came back took 12 minutes to do. It was very quick. I just sat in the hospital for 2 weeks and they monitored me very, very closely.
What did you know about CAR T-cell therapy?



It was very crazy. I had never heard of that. Everybody that I had talked to in the medical field, if they’d asked me what my plan was and I’d say CAR T therapy, they were all so impressed with this new treatment. A lot of my oncologists explained it like, “This is going to be the new chemo that people use because it’s very effective and it’s way easier on people’s bodies than chemo. It’s still new, so there’s not a ton of data on that.”
Instantly, I’m Googling, what is CAR T therapy? It’s crazy stuff. The machine that they hooked me up to, they had to put a line in my neck to get my cells out. It really is amazing what technology has come to and what it’s continuing to do.
Describe your experience getting CAR T therapy
The whole going through CAR T therapy was pretty easy. I don’t want to use the word easy, but there wasn’t a ton happening. The only thing that really sucked was you have to give CAR T therapy time for the cells to do what they’re supposed to be doing. It was a big waiting game to see if this transplant had even worked. That was the hardest part. I just wanted to know the 2 weeks that I was in the hospital.

They tell you that if you develop symptoms, it’s a good thing because it means that it’s doing something and it’s working, but I really wasn’t getting many symptoms, which freaked me out. I’m like, what if this isn’t working? I have no idea and the doctors can’t tell you if it is or not. There’s no way to tell. The waiting game was super hard.
I got a scan a couple months after and it had showed good progress, but I still didn’t hear the word “remission” until July 20th, this last July. It took a while because I had my CAR T on April 10th and I didn’t hear remission until July, which isn’t that big of a difference. Those times, and especially those weeks waiting in the hospital sucked. I just wanted to know, is this working? Was this worth it? Looking back, it was worth it. But the waiting game was the hardest part.
Being monitored post-cancer
In July, I was told I was in remission. I get scans every 4 months. I had the PET scan in July, but now we’re doing CT scans from now on. I’m checking in with my doctor every few months to see how I’m feeling. They won’t order any more scans unless I give them a reason to and unless I’m not feeling good.

My oncologist always warns me, “You know your body the best. If you don’t feel good or you feel like something’s off, please tell me.” That’s super important to remember, but also, I still don’t feel like this whole last year and a half was real. I don’t even feel like this happened. Being told I’m in remission is still so new to me. It feels really weird. I’m so thankful and grateful, but it’s just a lot to process.
Reflections
Do you feel like you’re still processing your cancer journey now?

I think so, because in the moment, I was fighting for my life. Now when I’m going back to college and right before college started, I’m freaking myself out. I’m like, what just happened last year? This doesn’t feel like it even happened. I do think that I spend a lot of time looking back at the last year and a half because my life changed so, so fast.
The importance of finding a cancer community
I don’t know anybody my age going through what I’ve gone through. I had a great support system with my friends and family, but I would highly recommend finding a community online, like through social media. I’ve met a lot of great girls my age that are going through what I’ve gone through. It was refreshing to hear people are going through what you’re going through. I have my friends and family here, but they can’t sympathize or know exactly what you’re going through unless they’ve gone through it themselves. It’s scary.

»MORE: Read More About Cancer Support
Finding people that you can talk to that have gone through it feels really good. That helped me a lot too. Even though I had so much support here, I think meeting people online too that were specifically my age made a big difference.
It was super hard, when I got diagnosed last June and all my friends are starting to go back to college and I had just turned 21, so my friends are turning 21 and it was really hard. My friends are going out, going to college, graduating college, and I’m sitting there hooked up to chemotherapy. It sucked.
I would highly recommend finding a community online.
Did you preserve fertility?
I’m glad you brought that up because I did want to touch on that. When I had first got diagnosed and I’m sitting in the hospital, I had a ton of social workers and a lot of different groups and support systems come talk to me. One of the teams that came in was a fertility team. I had these 4 ladies come in and talk to me. At first I was like, that wasn’t even something that had crossed my mind. I was not even thinking of that. They gave me a little pamphlet of options that I could do.


Unfortunately, I could only pick one of the options because I needed to start chemo right away. Some women can freeze their eggs, they have time to, but I was diagnosed and instantly had to start treatment. I got a shot once a month that shut down all my ovaries.
In the moment when they were explaining that to me, I started bawling. I remember specifically my oncologist said to me, “Samantha, this is scary, but it’s a good thing. We’re talking about you being able to have kids one day. Think of it that way, it’s good.” I’m like, “Yeah, you’re right. I’m going to be okay and I’ll be able to have my own babies one day.” But that wasn’t something that I had thought about. I think that is something that’s a big part of who we are too. That was super scary.
»MORE: Fertility After Cancer Diagnosis
Being a patient advocate
I feel like I trust myself more than I did before. I listen to my body more and I stick up for how I feel.
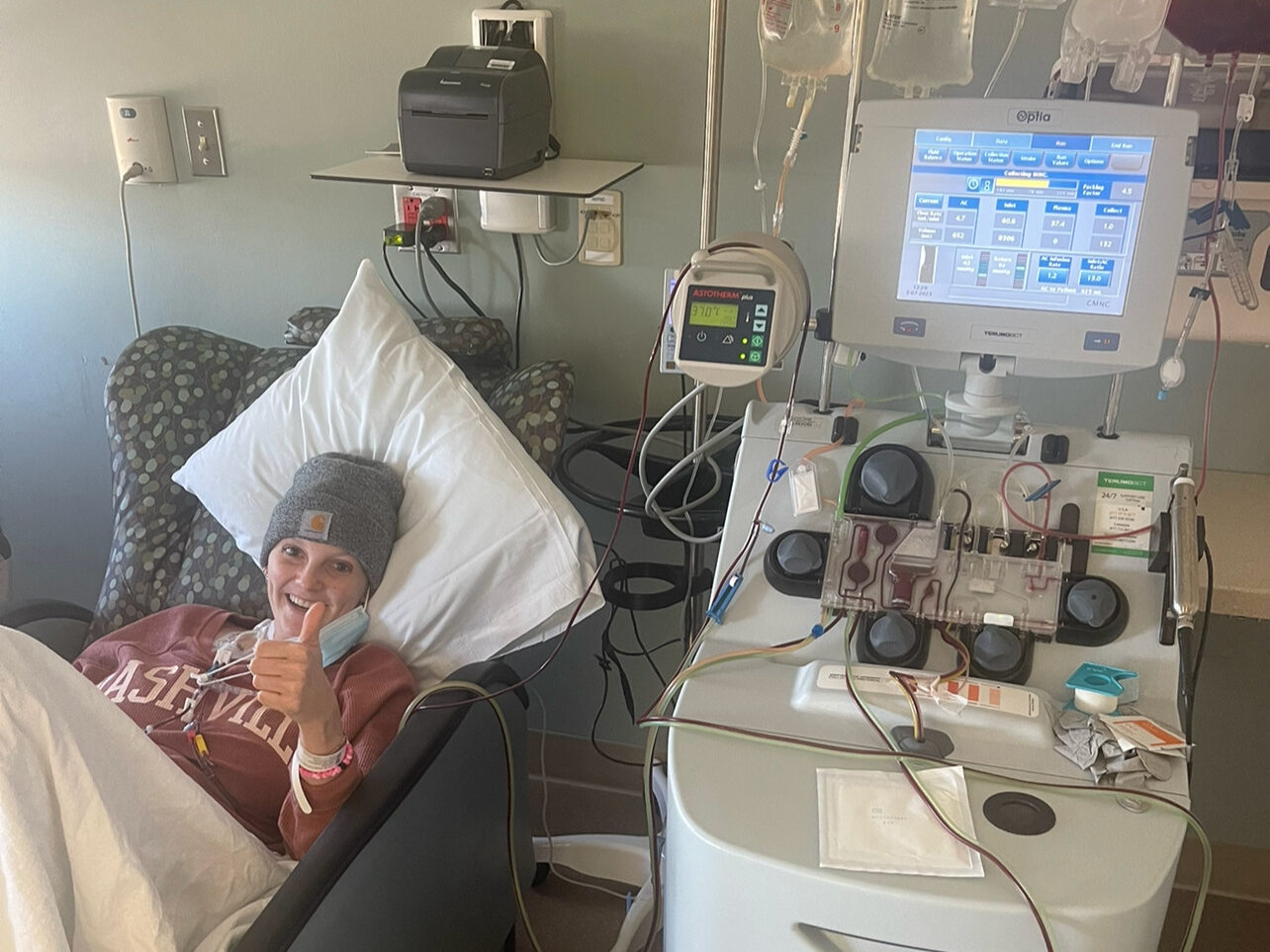
All my life, I had never really needed to go to the doctors. I had gone for maybe a yearly checkup, but I had always been so healthy, so I never really realized how big of an advocate you have to be for yourself. It’s kind of scary that you have to be an advocate for yourself. I wish that the doctors could just know, but obviously they don’t. They need a lot of data. They need symptoms, they need a lot of tests. Now I feel like I trust myself more than I did before. I listen to my body more and I stick up for how I feel.
What advice do you have for someone on a cancer journey?

Stay strong and fight as hard as you can because it’s so, so worth it. Find a good support system and surround yourself with people who make you feel really good. Also, be your own advocate. You know your body better than anyone else, and if you think something is wrong with you, it probably is. So just trust it. Trust yourself.
More Diffuse Large B-Cell Lymphoma Stories
Anna M., Diffuse Large B-Cell Lymphoma (DLBCL), Stage 4
Symptom: a rRapidly growing, painless lump on the breast
Treatment: Chemotherapy
Ashley P., Diffuse Large B-Cell Lymphoma (DLBCL), Stage 4
Symptoms: Feeling like holding breath when bending down or picking up objects from the floor, waking abruptly at night feeling “off,” one episode of fainting (syncope), presence of a large mass in the breast
Treatments: Chemotherapy, bridge therapy of chemotherapy and radiation, CAR T-cell therapy
Melissa B., Relapsed Diffuse Large B-Cell Lymphoma (DLBCL)
Symptoms: Lump in the left breast, persistent rash (started near the belly button and spread), intense fatigue and energy loss
Treatments: Chemotherapy (R-EPOCH), Neulasta, radiation therapy, surgery (to remove scar tissue and necrosis), autologous stem cell transplant
Jen N., Diffuse Large B-Cell Lymphoma (DLBCL), Stage 4B
Symptoms: Blood-tinged phlegm, whole-body itching, shortness of breath, lump near collarbone, night sweats, upper body swelling, rapid weight loss
Treatments: Chemotherapy, immunotherapy, lumbar puncture, autologous stem cell transplant




