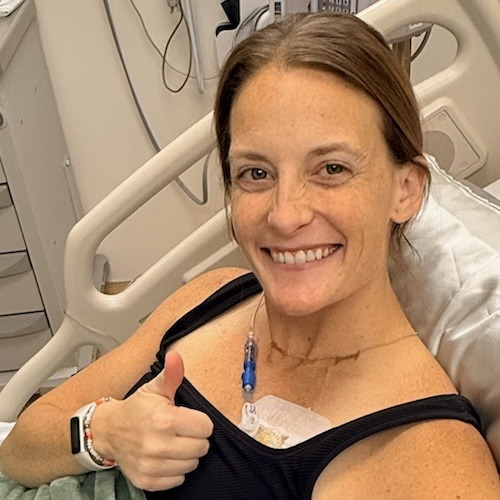
Jill Feldman’s EGFR+ Non-Small Cell Lung Cancer Story
Jill Feldman has become one of the most recognized names in the lung cancer advocacy space, not just for other patient advocates, but also for key lung cancer doctors and researchers.
A dedicated lung cancer advocate from Chicago, Jill’s story begins in her youth, with the losses of her grandparents, father, mother, and aunt to cancer, all within a relatively short time frame. It drove Jill to advocate for lung cancer research and early detection, including through assuming leadership roles at the LUNGevity Foundation.
Then she got her own lung cancer diagnosis.
Interviewed by: Stephanie Chuang
Edited by: Chris Sanchez
In 2009, doctors diagnosed Jill with stage 1A lung cancer during routine surveillance she had pursued due to her family’s history. Her EGFR-positive status allowed her to benefit from targeted therapies, and she highlights the critical role of biomarker testing in personalized cancer care. Her cancer responded to the treatment, but returned some years later.

Jill emphasizes the stigma surrounding lung cancer, often tied to assumptions about smoking. She argues that such misconceptions detract from providing patients and families with proper support and compassion. Her advocacy aims to shift the narrative and ensure that every patient receives understanding, regardless of their history.
Jill underscores the importance of building trust and empathy between medical professionals and patients, advocating for clear and compassionate communication throughout the diagnostic and treatment journey. Her advocacy extends beyond her diagnosis as cofounder of the EGFR Resisters nonprofit whose mission is, in their own words, to be a “patient-driven community dedicated to improving the outcomes for those with EGFR positive lung cancer. She continues to educate others, including on social media, about lung cancer screening and the advancements in treatment that save lives through biomarker education and testing. Jill believes that empowering patients with knowledge about biomarkers can help them make informed lung cancer treatment decisions and feel more in control during a challenging time.
Jill’s personal life remains a source of joy and motivation. She cherishes time spent with family and friends, outdoor activities, traveling, and volunteering. She explores new hobbies and finds solace in giving back to the community that supported her.
Jill’s message focuses on hope, resilience, and the power of advocacy. She encourages others to confront stigma, share their stories, and lean on one another for strength. Her journey, intertwined with loss and triumph, illustrates the importance of raising awareness, fostering empathy, and supporting ongoing research for better treatment outcomes. Jill concludes by reminding listeners that every story holds power and that no one should face their journey alone.

We would like to thank The White Ribbon Project for its partnership.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
- Name:
- Jill F.
- Age at Diagnosis:
- 39
- Diagnosis:
- Non-Small Cell Lung Cancer With EGFR Exon 19 Deletion
- Staging:
- Stage 1A
- Symptom:
- Nodule found during periodic scan
- Treatments:
- Surgery
- Targeted therapy
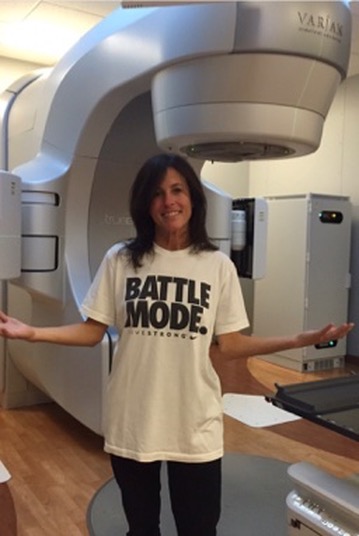
- Radiation
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- About me
- A family affected by lung cancer
- Finding a way in
- Early losses and stigma
- Watching lung cancer return
- My search for answers
- Learning to advocate
- At my brother’s appointment
- Receiving the lung cancer diagnosis
- Conversations and communication
- Biomarker testing, its importance, and its impact
- Treatment decisions
- Progression and rebiopsy
- Impact and hope
- My closing reflections on lung cancer and hope
I always say to oncologists, “You are not going to save every life. But if you help patients and families find their hope, you will make a difference in every single life, and that matters also.
Jill Feldman, lung cancer patient and advocate
About me
Hi, my name is Jill Feldman. I was diagnosed with lung cancer in 2009 at 39 years old.
I am married, and I have four kids and a dog. I live in the Chicago area. I love to spend time with family and friends. I am an active person outdoors, especially when it is not winter.
I love to travel. I love to volunteer; I love to give back. I try to get involved in different things and take up new hobbies here and there, although I have not tried pickleball yet and am not sure if I will. That seems to be the new trend.


A family affected by lung cancer
My story is quite different from others — because it started long before I was diagnosed with lung cancer.
When I was 13, I lost two grandparents to the disease within weeks of each other. Then, my dad was diagnosed six months later with lung cancer, and he died three months after that at the age of 41. After that, when I was in my twenties, both my mom and my aunt died of lung cancer. My mom was diagnosed, and she died six months later at the age of 54. Then, two and a half years later, my aunt, her sister, died. My aunt was like my second mom. We were raised that way.
We were a very close family, so I was devastated. I was a hot mess, to be honest.
Finding a way in
This was back in 2000, and I desperately tried to find something to get involved in. I needed to find a way to confront this disease that had devastated my family, and there was nothing. Nothing for the first year that I looked — and then, as I always say, “Coincidence or fate?” — the first organization in the country dedicated exclusively to lung cancer research was founded in my community on the north shore of Chicago.
A friend introduced me and took me to my first meeting in 2001. I did what I could to advocate and educate myself. While doing so, I was diagnosed with lung cancer in 2009 at 39 years old.
My kids were 6, 8, 10, and 12, and their only association with the disease was death. They were scared, and my biggest fear became reality. I was following in my family’s footsteps.


Early losses and stigma
So, I have had a front-row seat in this rapidly growing field as a patient. I have benefited from many of those treatments. When I was first diagnosed in 2009, I was originally stage 1.
As I mentioned earlier, my grandparents died of lung cancer; my mom’s mom died, and 13 days later, my dad’s dad died. So, it was a shock, and those were my last two living grandparents. My grandmother, who lived close to us, was very, very close to us. I knew nothing about lung cancer specifically at the time.
My other grandparents died of cancer as well, of pancreatic cancer and lymphoma. So, to me, at the time, lung cancer was another cancer, but then, when my dad was diagnosed with lung cancer, I was in 8th grade, and I could not believe it.
Now, there is still a stigma associated with lung cancer. I did not know many people who had lost a parent to cancer, but I did have one other friend whose dad died probably six months before mine, and I just remember thinking, “How come no one is asking Shelly if her dad did something to deserve or die from colon cancer?” People I know asked, “Your dad smoked, didn’t he? Your dad has a smoking history, didn’t he?” and so immediately, the compassion and the empathy given to other people were not given to us. I struggled with that for a very long time.
My dad was a contractor, and he worked with asbestos. He was 41 years old, and we do not know what carcinogen caused his lung cancer. But does it matter? Does that mean he deserved to die? Did that mean that our family deserved less empathy and support? No. What matters are the people. Nobody deserves this awful disease. Certainly, nobody deserves to die from it.
Nobody deserves this awful disease. Certainly, nobody deserves to die from it.
Jill Feldman, lung cancer patient and advocate
Watching lung cancer return
Yeah, so it was my aunt first, and she had been diagnosed twice before. You know, her third time was when she died. It was exactly ten years after my dad died. My aunt had gotten a CT scan for something else, and they found a nodule in her upper right lobe.
I remember exactly where I was when I heard the news, and it totally took me by surprise. It totally brought back awful memories, and I was freaked out, as was everybody else in my family, but it was caught early, so she had surgery and was considered cured. Two years later, just five weeks before my wedding, she had surgery for another stage 1 cancer that was supposedly caught early.
She had an upper left lobectomy and was considered cured. Then, two years later exactly, she had clean scans, and we celebrated. We were like, “Oh, my gosh, this is wonderful!” But not for long, because that is when we learned that my mom was diagnosed with lung cancer, only her lung cancer was not caught early.
I remember exactly where I was, exactly what I was wearing, and I just thought, “There is no way this is happening again.” My aunt had had adenocarcinoma. My mom was diagnosed with small-cell lung cancer. So it can be more aggressive. I was 27 years old when she was diagnosed. I did not believe that she was going to die. I could not even fathom it.
She had a wonderful response to treatment, but the cancer came back shortly after, and she ended up dying six months after she was diagnosed. I was 28. I had a 15-month-old. I was nine weeks pregnant with my daughter, and it was gut-wrenching. I really could not believe that this insidious disease orphaned me.
I remember thinking, “Thankfully, I have Dee Dee,” who is my aunt. She was a second mom to me. I mean, I talked to her every single day, and my mom was her big sister, so she was devastated. My mom, we all called her Mother Earth; she took care of everybody, and my aunt really struggled with it, but I was grateful to have her.


My search for answers
Less than a year after my mom died, my aunt developed a third cancer. At the time, she had already had two lung surgeries. She had an upper right and upper lobectomy. Well, the lung is finite. I always say she ran out of real estate. She could not have any more lung removed. You cannot live without your lungs.
She went through traditional therapy, which, back in 2000, covered chemotherapy, radiation, or surgery. There were no targeted therapies. There was nothing else. She started with chemotherapy, and unfortunately, the cancer spread, and she died about a year and a half later. That was when I really spiraled downward.
I could not even believe it, and again, nobody would entertain the idea that this disease could have a hereditary component. It was so easy to say, “Well, they had a smoking history.” Well, my mom had quit 15 years prior. I mean, I do not even know if she would have been eligible for screening at this point, because if you quit for more than 15 years, then you are not eligible. My aunt, too.
I just remember really trying to understand how this happened, that it could not be a coincidence. That is really, I think, when I started advocating, without even knowing it, by pushing doctors and asking, and finally getting my doctor to say, “You know what, I do not think it is a coincidence, and I think you should get a scan for a baseline, and we will go from there.”
Learning to advocate
Yeah, I used to doubt myself. I really was doing that, and I still do at times, with the “Oh, I do not know if I want to bother them. Maybe I am wrong, or I should not bring this up.” I do self-doubt over and repeatedly, but I think really the most important thing to remember is that if we do not advocate for ourselves, nobody else is going to advocate for us, and this is life or death when it comes to health.
We are the CEO of our health, and if we were the CEO of anything else, say, a business, we would make sure the I’s were dotted and the Ts crossed.
I just think that everybody should ask questions. It is not just about asking the question, but it is about understanding the answer, so if a doctor or nurse or any type of healthcare professional gets irritated or is not answering the question, then that is a sign that you should reach out and try to talk to other people and maybe try to find a community that can help you with finding the right doctors or finding the right people to talk to. There is nothing wrong with that.
For me, considering two generations on both sides of my family, I spoke with my internist, and he said, “I think you should get a baseline scan and let us go from there.” I got the scan, and the scan was clear, and I am glad I got it. Then, through my mom and my aunt, the work that I did in advocacy, there was a pulmonologist I knew well, and he recommended that I go three years later, and I did. I was 30. Everything looked good. Then I had four kids, so I skipped, and kind of waited five years, and I got a scan at that point, and they found a nodule.
Now, at that time, I had been really involved in advocacy. I think I was vice president of LUNGevity Foundation because, by the time I was diagnosed, I was president. For some reason, I was not scared. Back then, in 2006, we were just learning about ground-glass nodules, and we watched it.
So, I got another scan six months later, and another six months later, then a year later. At that point, they said, “Oh, there has been no significant change; no further follow-up is necessary.” My doctor and the pulmonologist said, “Yeah, I think you probably should have a follow-up.” We all deferred to the pulmonologist as to when I should follow up, and he said, “Just do it yearly, Jill, because then you are not going to forget, and they are low-dose.”
Sure enough, a year later, that ground-glass nodule took a nasty turn, and there was a little brother there as well. That was when I was diagnosed. I was very thankful that I did not listen to the radiology report, that I discussed it, and talked about my risks versus radiologic risks in general when they are looking at scans.


At my brother’s appointment
There is a little side story for my advocacy, too. So, I knew somebody in my family would be diagnosed with lung cancer. I have a brother 18 months older than I am, and he is a brilliant child. He was diagnosed with schizophrenia when he was 19, and he had been rolling and smoking cigarettes since he was 16.
I feared that he was going to get lung cancer. I would go with him to the pulmonologist to get scans every six months because, at 30, he was diagnosed with emphysema. When I was diagnosed, it was at one of my brother’s appointments.
My brother and I had gone to this particular pulmonology appointment, and, thankfully, my uncle was there too. The pulmonologist went through his tests and went over his medication, and was going to send him for pulmonary function tests, when he was walking out of the room. I said, “Hey, you know, Dr. Becker, did you look at my scans?” He said, “Yes. I will be right back.”
He went and ordered the test for my brother, then he came back in the room, and he pulled up the scans, and he kind of turned the screen for me to see them. I had worked with him within the advocacy world, so he knew that I knew what he was talking about.
He just pointed to last year’s scan and this year’s scan, and he said, “I do not like what I see. I do not like it at all.” I did not say anything. I just remember my brother was like, “Oh, my God!” He was freaked out.
… if we do not advocate for ourselves, nobody else is going to advocate for us, and this is life or death when it comes to health.
Jill Feldman, lung cancer patient and advocate
Receiving the lung cancer diagnosis
When I was diagnosed, all I could think about was that I literally was diagnosed with the same disease that I watched kill my mom and my dad. I still get emotional when I think about it because those were the two most difficult, worst times of my life.
They were the two most important pillars of my life. There I was, at 39 years old, my kids are 6, 8, 10, and 12, and I was just consumed by the thought of, “Are they going to go through what I went through?”
The only thing worse than being diagnosed with cancer and the fear that you live with is watching the people you love suffer, and seeing the fear in their eyes because of your diagnosis. I could almost feel it because I could totally identify with it.
So that was it. That really paralyzed me for a little bit. But then I thought, “Okay, I am going to be the story of hope.” I am going to be the poster child for early detection because I was originally diagnosed with stage 1, and it took a lot of work.
Anytime anyone is diagnosed, none of us are exempt from going whether we are cured or not; we all must go through that deep, dark tunnel because it is a life-changing experience, and it is traumatizing in many ways. I did not get to where I am in a day or overnight. It was a process.

Conversations and communication
The conversations patients have with doctors, with their families, are so important. I think one of the things that we do is put the burden on newly diagnosed patients and families that they need to be educated. The burden should never be on them.
There should be resources available. We need to know when to have the conversations, how to have the conversations, and think about the way we are talking to people, think about the context of their life, their family.
I am really hoping we move more towards empathic communication. It is not something that oncologists learn in school. Their degree does not depend on it, but it is at the heart of the patient experience. I feel like those conversations should be guided by the care team, and I do not think there is one perfect time for them to happen.
I think it depends on what patients and families can really absorb. But I do think that the conversation about biomarker testing and lung cancer should happen right away.
So, it is almost like they test right away to see whether you have a small cell or a non-small cell cancer, and they test right away to see whether the non-small cell is adenocarcinoma, squamous cell, or large cell. I am hoping we are moving towards now testing even further, because whether you have a biomarker or not, the right treatment depends on that answer.
Biomarker testing, its importance, and its impact
When I was first diagnosed, they had just started testing for EGFR and KRAS, and I had known about EGFR just because when I was diagnosed, I was president of LUNGevity Foundation, and we had funded some research in that area. So, I got the testing done, and I was EGFR-positive.
That result guided my treatment from that point onwards. Adjuvant therapy for lung cancer at the time had very minimal benefit, but I needed to be able to look my kids in the eyes and know I did everything in my power. I had already planned that I would look at adjuvant therapy or therapy after surgery as almost an insurance.
I thought I would probably have chemotherapy because that is what the adjuvant therapy was, but because I was EGFR-positive and because I knew what was going on in the field at the time, I talked it over with my doctor, and I ended up going on targeted therapy. There was a clinical trial in Boston, but I had four kids. I could not travel; I could not afford it, and I did not have the time. So, I took the drug off-label, which means I took it off the trial for about 16 months. It is the only time in the past 15 years that there has not been any visible cancer.
It worked while I was on it. I look back, and I think about it, and I think, “Well, was it worth going on the treatment?” The side effects were not great. In fact, they were horrible. I will not lie. Was it worth it since the cancer came back? For a while, I thought, “No, I would never do that again.” But, you know, reflecting on it now, I think, “Well, what if it did prevent the cancer from spreading elsewhere? What if it did slow it down?”
I don’t know. But I do know that, for me, it was the right decision at the time. My oncologist said to me, “Your emotional well-being is just as important to me as your physical well-being.” That’s how I knew it was the right decision.
Within the lung cancer space, usually, diagnosis is through the biopsy of the tumor, and there is a blood-based biomarker test as well. What it entails is looking at a whole huge group of different alterations, if you will, or different expressions in the tumor that can indicate what is driving the cancer.
A lot of the time, currently, when we think about biomarkers, we think about oncogene cancers. Whether somebody is EGFR, ALK, ROS1, or RET positive, there are many different types of what they call oncogene cancers. And that just means that this gene is what is driving the cancer. The brakes do not work anymore. The light switch was turned on. But biomarker testing can also look at a protein that is showing a certain expression.
So, for immunotherapy, they are looking at the PD-L1 (opens a pdf at Cancer Support Community) expression, and if they find that, then they can guide the treatment that way. So, really, a biomarker is just a piece of information that can help guide the treatment.
Usually, you would hope that your doctor would discuss with you: “Okay, we are going to take a biopsy of the tumor so we can understand this cancer better,” and hopefully they will mention biomarker testing as part of that process. Now, the one thing about biomarker testing is that it is done after they have already looked at what type of lung cancer it is. They must get that information first, and then some places have in-house testing. Most places still send a piece of the tumor to a company that will do the biomarker testing. The process takes a couple of weeks, which is very anxiety-provoking. I just had a biopsy in the spring, and I am a veteran patient, and the anxiety is consuming.
You want to know, and you do not even know what you want to know necessarily, but you just want to know because one of the worst parts of all of it is waiting. It is like hurry up and wait, and then you are waiting. Then, once you get a plan in place, the anxiety does not necessarily go away, but you are less anxious because now you have a plan.
One of the things that I actually advocate for is the creation of a service like FedEx or UPS, where patients are just notified when that tumor is sent out, when the lab has received it, when it’s going through testing, and so on. We do not need the information on what it finds right away because we are not going to get that information until our doctor does. But just knowing it is in the process helps alleviate that anxiety, because it’s so important to wait to start your treatment until you have all the information.


Treatment decisions
When doctors are doing biopsies, they are not thinking about the impact on patients and families. But it really is about the impact. How is this diagnosis and the treatment going to impact my family and me? It really does impact you and your family. It makes the biggest difference in the world.
You want the best treatment upfront. You want the right treatment upfront. There are many reasons why, but the biggest reason is that it is more durable, and it works better and longer than other treatments. I do not doubt that it does not just help with living longer; it helps with living better as well.
Now, I think a lot of times in a community setting, a general oncologist is treating so many different cancers, and I do not think we do a great job of helping them seamlessly implement biomarker testing in the education. I hope to see more coordination within the academic and major cancer centers, working more with community centers to raise awareness, and helping provide more education out there.
Any way we can help them is good, because the reality is, as newly-diagnosed patients, we do not know what we do not know. Make sure that you get enough tissue so that you can do the regular testing and the biomarker testing because having to re-biopsy is not always possible, and it’s certainly not easy. These are the things that a lot of patients do not know that really impact their path and their experience with treatment.
… one of the things that we do is put the burden on newly diagnosed patients and families that they need to be educated. The burden should never be on them.
Jill Feldman, lung cancer patient and advocate
Progression and rebiopsy
Yes, if you are someone who is on treatment or whose loved one is on treatment and has experienced progression, you absolutely must have that conversation. Having another biopsy also at the point of the cancer starting to grow again is critical in guiding which treatment you have next.
Too often, people will say, “Well, my oncologist did not recommend I get a biopsy, just that I go off of the treatment I am on and start a different treatment.” But the reality is, you do not always have to go off the treatment you are on. Sometimes, they will add a treatment, or sometimes, they will add either radiation or surgery, and you can stay on the treatment.
That just happened to me in the spring. I had progression, and I ended up being able to radiate the area where the cancer was growing. Now, I stay on the same treatment, which is so important to be able to do that and get more mileage out of that treatment.


Impact and hope
What’s the impact been upon me? Well, for me, the greatest impact is that my dad died three months after he was diagnosed, just a few weeks before I graduated 8th grade. My mom died six months after she was diagnosed and just six months before the birth of my daughter. But, because of advancements in research and treatments, I have lived for 15 years. I have celebrated moments and milestones with my family. I saw all four of my kids not only graduate 8th grade, but also graduate high school.
Those are the treasured milestones that were stolen from my parents and me because they did not have the treatment options that are out there now. The true value of all this research for patients and families is hope. Hope represents a chance, and every patient deserves a chance.
I think about that a lot because it does impact your treatment. I do not know if I would be here today, truthfully, because every single treatment that you have affects you; it affects your body. If you are not treating it the right way, it could really mess up kind of what your experience looks like, and I do not know if I would be here today.
We have these approved treatments. We need to be able to get them to patients. Michael Jordan used to say, “You make 0% of the shots you do not take.” That is how I feel about biomarker testing.
Again, the burden should not be on the patients, but I think it is an ethical matter here that patients should have biomarker testing. Every patient should have it. Doctors should not judge, “Oh, well, you know, they are too old or too young, or they have a smoking history.”
Whether they find something or not, whether they find a biomarker or not, that is important information to have to know which treatment path a patient should take.
My closing reflections on lung cancer and hope
I never used to use the word “hope” in the same sentence as lung cancer because, in my experience, there never was any, but there is now, and it encompasses a few things.
Hope and reality are not mutually exclusive. They both can live in the same space. I have learned that hope is more than a cure. I hope the treatment works. I hope I can live to see my child graduate or get married, or my grandson get married. Whatever it is, there is always hope, but there is palpable hope in lung cancer now, and I think my family history illustrates that hope.
I even got a tattoo on my arm as a permanent reminder, and I swore I would never get inked; I thought I would get sick of it, but I needed that permanent reminder that there is hope.
Again, I think my family’s history and my story illustrate hope and progress in lung cancer. It is a vital emotion, and it is something. I always say to oncologists, “You are not going to save every life. But if you help patients and families find their hope, you will make a difference in every single life, and that matters also.”

I never used to use the word “hope” in the same sentence as lung cancer because, in my experience, there never was any, but there is now…
Jill Feldman, lung cancer patient and advocate


Special thanks again to The White Ribbon Project for its support of our independent patient education content. The Patient Story retains full editorial control.

Inspired by Jill's story?
Share your story, too!
Related Cancer Stories
More Lung Cancer Stories
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
...
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
...
Natalie B., Non-Small Cell Lung Cancer, Stage 4 (Metastatic)
Symptoms: Extreme fatigue, severe cough
Treatments: Chemotherapy, immunotherapy, clinical trials, radiation therapy, surgery (double lung transplant)
...
Stephanie K., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent and intense cough, general feeling of sluggishness
Treatments: Chemotherapy, targeted therapy through a clinical trial, radiation therapy
...
Jennifer M., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptoms: None per se; discovered during physical checkup for what seemed to be a sinus infection
Treatments: Radiation therapy (stereotactic body radiation therapy or SBRT), targeted therapy
...
Laura R., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent cough, fatigue, bone pain
Treatments: Targeted therapies (tyrosine kinase inhibitors or TKIs, including through a clinical trial)
...