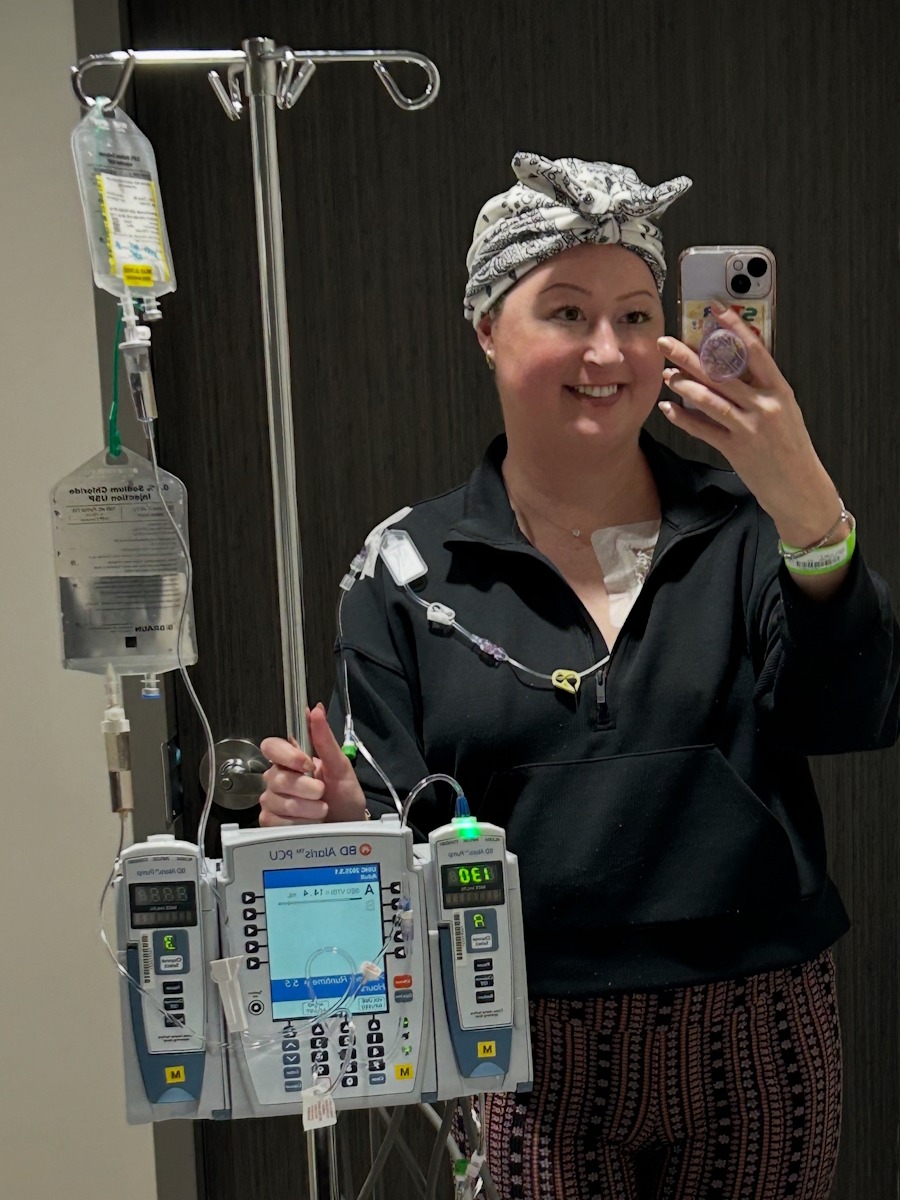From Chemo Exhaustion to Targeted Therapy: Clara’s Stage 4 ALK+ Lung Cancer Experience
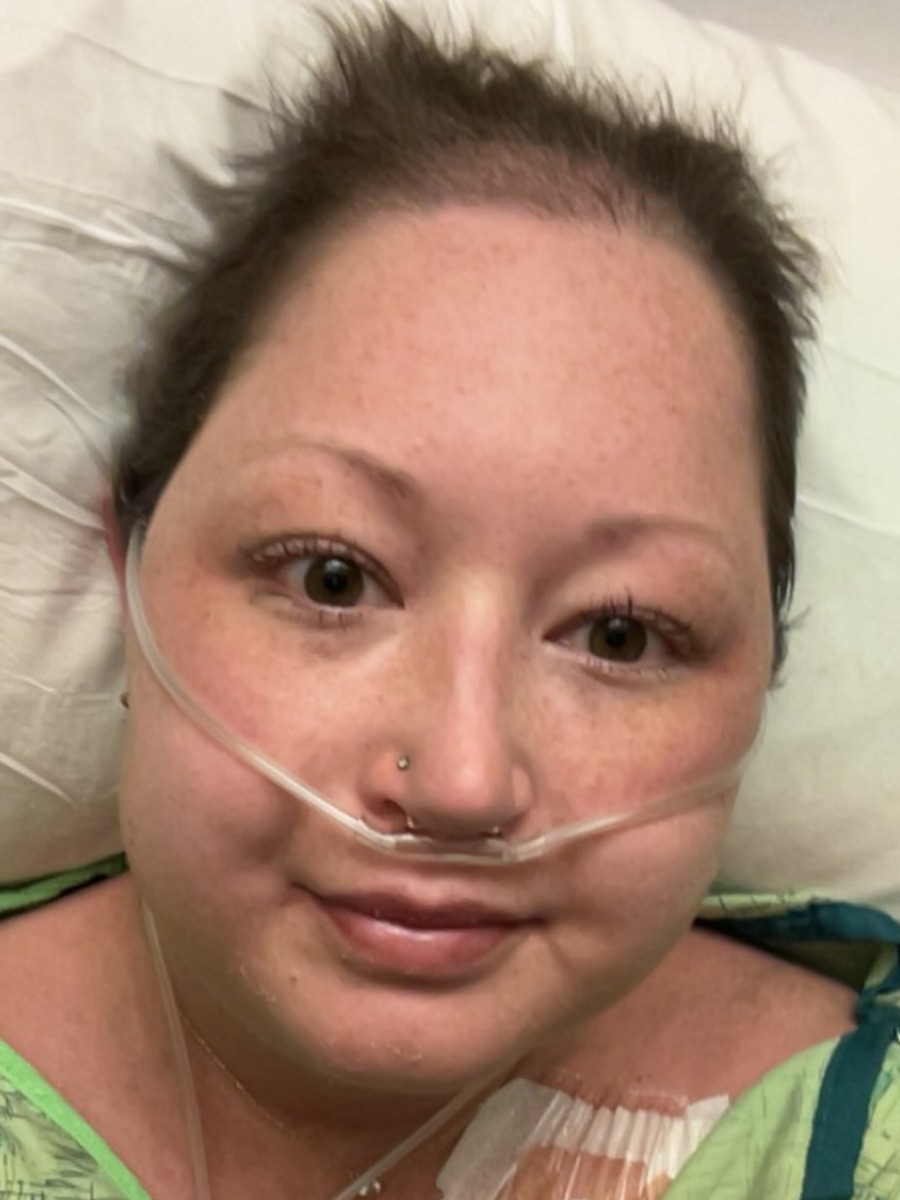
Living with stage 4 ALK-positive non-small cell lung cancer, Clara has had her entire life reshaped by diagnosis, treatment, and the constant recalibration that serious illness demands. She moved back home to Iowa after years in Colorado, trading her independent adult life for the familiar walls of her childhood bedroom and the support of nearby family. In the middle of all that upheaval, adopting her dog Bernie became a lifeline, giving her structure, purpose, and a reason to get outside, even as medications changed her body and added significant weight gain.
Interviewed by: Nikki Murphy
Edited by: Katrina Villareal

Her early treatment included chemotherapy and maintenance immunotherapy. For a while, the scans looked promising. Her tumors were shrinking or holding steady, which is a meaningful win with advanced disease. When a later set of scans showed worsening metastatic disease and new spread to her spleen, she faced another round of aggressive chemo that repeatedly landed her in the hospital. The physical toll, the constant sickness, and the feeling that she was doing chemo more for others than for herself pushed her to say, “I am done.” She made that choice fully aware that it could mean her cancer might worsen without more treatment.
At the same time, additional biomarker testing revealed that her cancer was ALK positive, opening the door to targeted therapy in place of chemo. Starting Lorbrena (lorlatinib), a third-generation tyrosine kinase inhibitor specifically for ALK-positive non-small cell lung cancer, shifted both her symptoms and her outlook. Instead of enduring relentless infusions and hospitalizations, she now takes a pill once a day with far fewer side effects so far, and she is hoping upcoming scans will show stable or shrinking disease.
Alongside physical treatment, Clara is weighing deeply personal decisions about pelvic tumors, potential surgery that could remove her ovaries, and the grief of likely not having biological children. She is processing the realities of disability, financial toxicity, and a world not built for walkers and wheelchairs, even as she regains independence by driving again and leaving the walker behind. Through her “Cancer Questions with Clara” videos, she speaks candidly about taboo topics, like adult diapers and body image, to help others feel less alone, while reminding herself and her community that evolving research and new treatments can offer real, hard-won hope.
Watch Clara’s video or read the edited transcript of her interview for a follow-up to her story. Read how she first found out about her cancer here:
- Targeted therapy for ALK-positive non-small cell lung cancer can offer meaningful options, including oral treatment with fewer day-to-day side effects
- You are allowed to prioritize your quality of life and make treatment decisions that reflect your values — even when others may not fully understand
- Biomarker testing can change the entire course of care, opening doors to personalized therapies
- Clara’s experience shows how serious illness can reshape family roles, home, work, and even geography, while still making room for joy and reclaiming independence
- Her transformation included moving away from chemotherapy, which she felt she was doing for everyone else, to advocating for herself, choosing targeted therapy, and using her story to educate and normalize difficult topics for other patients
- Name: Clara C.
- Age at Diagnosis:
- 30
- Diagnosis:
- Non-Small Cell Lung Cancer (NSCLC)
- Staging:
- Stage 4
- Mutation:
- ALK
- Symptoms:
- Pelvic pain and discomfort
- Bladder issues related to pelvic tumors
- Incontinence
- Pain in the lower back and hip
- Treatments:
- Chemotherapy
- Immunotherapy
- Radiation therapy
- Targeted therapy: lorlatinib
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Adopting my dog Bernie and moving back home
- Leaving Colorado and saying goodbye to my old life
- How we discovered my cancer progression and changed treatment
- How cancer research and funding directly impacted my treatment options
- Learning about ALK positive and finding community
- My treatment plan going forward, scans, surgery, and clinical trials
- Why surgery is only planned for my pelvic tumors and how it affects my fertility
- The hardest moments and what keeps me going
- Why I share my story on social media and “Cancer Questions with Clara”
- Topics I want to talk about more: dating, disability, and financial toxicity
- Ditching the walker, driving again, and getting my independence back
- Writing a love letter to my body and coping with weight gain
- How targeted therapy has given me new hope and my message to others
- Living with the uncertainty of cancer and rolling with the punches
Adopting my dog Bernie and moving back home
I was living at my mom’s house right outside of Des Moines, Iowa, but now I’m at my dad’s house in a very small town a little further away from Des Moines. My dad still lives in the house I grew up in, so it has been nice to come back to my childhood bedroom.
What’s nice about my dad’s house is that he has a big yard, so I was able to adopt a dog, which has been a great addition to my life. I got him from the Animal Rescue League of Iowa. He has given me so much purpose and has definitely been a reason to wake up in the morning. He has provided me with a lot of structure and routine, and has made me active, taking him outside for walks, which has been great to get outdoors. It has also been great in helping me be active because I gained a lot of weight from cancer medication, so I am trying to lose that weight. Bernie, my dog, has been helpful in that regard.
Leaving Colorado and saying goodbye to my old life
After treatment, I thought that I would just return to my apartment in Colorado, go back to my old life, and everything would be fine. At that time, I learned that I would have to be on immunotherapy for the rest of my life. Traveling back and forth between Colorado and Iowa would be too much, so I decided to give up my apartment. I was unwilling to transfer my care to Colorado because I love my team in Iowa so much. I decided to clean out my apartment and be done with it, which has been a weight off my shoulders financially because I had been paying for it the whole time.
It was very emotional and very bittersweet to leave Colorado because I had spent my entire adult life there. I had a lot of life lived, a lot of memories, and a lot of friends.
It was good to reflect and to reminisce. I invited a bunch of my girlfriends out for dinner while I was there, and we had a “goodbye Clara” party. It was fun and special to have those women there. I wrote each of them a letter about our friendship, why they were important to me, and how sad I was to leave Colorado. We were all in tears at dinner, but it was a good send-off.
It’s good to be in Iowa permanently. I enjoy being close to family, so that has been the biggest perk of being back in Iowa for good, I should say.
How we discovered my cancer progression and changed treatment
The last round of my first cycle of chemo was on July 3rd. That round and the one prior to that sent me into the hospital for 10 days, both times. Obviously, I was glad to be done with chemo and be on maintenance immunotherapy. I was doing immunotherapy throughout the summer.
I had scans in August and they were great. They showed that my treatment had been working. There was a lot of shrinkage. Different parts of my cancer were either shrinking or staying stable, and that’s the goal with stage 4 cancer: to keep things shrinking or stable. Stable is great.
I continued with immunotherapy throughout the fall. I had my next three-month scans in early November, which came back horrible. They showed that everything was growing, and my cancer had also spread to my spleen at that time. The report literally said “worsening metastatic disease,” meaning everything was getting worse. That was devastating news because three months prior, the scans were great. I had a lot of hope and optimism. To get those results in November was devastating.
We had a scheduled surgery on my pelvic tumors for December 1st, but because my cancer had come back so aggressively in terms of growth, we decided to start an aggressive chemotherapy regimen again. It was a different drug. We started it immediately and had to push off surgery indefinitely at that point. That was hard for me because I so desperately wanted to get these pelvic tumors out since they cause so much discomfort and pain. One of my pelvic tumors is on my bladder, which causes me a ton of issues.
I did chemo round seven, which again put me into the hospital for another 10 days. I was getting sick again and again. After that seventh round, I was in the hospital up until the day before Thanksgiving, which was so frustrating. I decided, “I am done. I am done with chemo.” I felt like I was putting my body through so much.
I also felt like I was doing it for the wrong reasons. I felt like I was doing chemo for everybody else and not for me. I felt like they wanted me to do chemo because they wanted me to stay alive. Of course, I want to stay alive too, but I’m the one who has to go through it. I’m the one who has to put my body through treatment. It’s so hard on my body to get that sick all the time.
I decided I was done with treatment. I wasn’t doing it anymore, which was a hard decision because I knew what that meant. That means my cancer may get worse and there is nothing that can be done if I am not willing to do treatment.
At the same time, my oncologist had ordered another set of Tempus testing, which is testing for genetic mutations. They sent another biopsy sample in. We found out that I wasALK positive, which my oncologist was shocked to see because he had not seen anybody evolve into a mutation that was not there previously. The whole reason he sent a biopsy sample again was that Tempus testing can also determine what chemotherapy to use. Not only does it identify genetic DNA markers, but it can also help guide treatment options. He did it for the purpose of making sure he was giving me the correct chemo this time around.
When it showed ALK positive, he said, “Okay, we are going to stop chemo,” which I had already decided to do anyway. He said that with ALK-positive, they have a targeted therapy available. Targeted therapy is a pill that I take every day. It is not chemo at all. It is in replacement of chemo and has far fewer side effects than chemo does.
The specific one that I am on is Lorbrena (lorlatinib), which is a third-generation tyrosine kinase inhibitor (TKI) of the targeted therapies that are available for ALK-positive patients. That is specific to non-small cell lung cancer, I should mention. It is a very specific and very personalized treatment. I started the targeted therapy pills in December 2025. After being on them for about one month, I have had very minimal side effects, and I think I am responding to it pretty well.
With targeted therapy, it sometimes takes a lot longer to show results. Even though my next three-month scans are in February, they may not show exactly if it’s working yet. I am hoping they will at least show that everything is stable, if not shrinking. I am hoping for stable, and then maybe another three months after, the scans will show some improvements and positive results from the targeted therapy.
That has been a good thing. I am so happy that I’m ALK-positive and that the targeted therapy was available. I had decided I was stopping treatment. Who knows what would have happened to me and what that would have entailed?
How cancer research and funding directly impacted my treatment options
I am grateful for the targeted therapy. These drugs are available because of the funding for cancer research, and all of the cancer patients who came before me who participated in clinical trials and research that made these drugs available.
It’s interesting how some of these drugs were only approved within the last couple of years. If I had been diagnosed with cancer a couple of years prior, who knows what kind of treatment I would be on today or if I would be able to be on this? Everything worked in divine timing for me to be on this. It has been going well.
Learning about ALK positive and finding community
I knew about different biomarkers. I had heard of ALK, but I did not know much about the treatment available for them. It turns out there is a whole community of ALK-positive patients. It has been nice to connect with others on social media and other platforms.
I’m on the third-generation TKI. I have talked to other patients who are on the first- and second-generation drugs. Those ones seem to have more side effects. As research progresses, it seems like they are trying to get rid of the side effects, which seems to be working because I have had very minimal side effects. It sucks that every medication for cancer that I take has weight gain as one of the side effects, which has been frustrating. But other than that, it’s going well.
My treatment plan going forward, scans, surgery, and clinical trials
My next scans will be in February 2026. Based on those results, we will determine if I am still eligible for surgery. That’s why I’m hopeful that things are stable or shrinking so that I can have those pelvic tumors removed. They cause me so much discomfort and so many issues. Getting rid of them would be the best for my quality of life.
After that, I will have scans every three months. I don’t know what my options would be if the targeted therapy stops working, but hopefully, I do not have to worry about that. I guess another option would be clinical trials. I am open to them, but I would need a lot of information to make a well-informed decision about whether or not to participate. I am open to it if that is my only option down the road. For me, whatever I have to do to live that is not chemo, I am okay with.
Why surgery is only planned for my pelvic tumors and how it affects my fertility
There has not been talk of surgery on any other organs. They explained to me that if they were to go in and get rid of some of the cancer, it would not make that big of a difference. I have so much cancer in so many places that it would not do much, which is hard to hear.
I am grateful that they are willing to consider surgery on those pelvic tumors. One of them had shrunk back in August, but then in November, it had grown back to its original size, which is the size of a softball. I have a softball-sized tumor on top of my ovaries. If I go through with the surgery, they will remove both of my ovaries, which will deprive me of the opportunity to have biological children. I do not have any kids right now and that is something I have had to wrestle with.
I looked into freezing my eggs, but it is so costly and out of my budget. Plus, with how much I want the pelvic tumors out, I guess I am okay with taking out my ovaries, but that is something you have to grieve —the kids that I thought I would have that I will no longer have. I know there are other ways to have a family, but it’s hard to think that I will never have a kid that looks like me or inherit traits that I have. I am very artistic, and I would want my kid to be artistic and creative. That has been something I have struggled with and talked about a lot in therapy. That is not something I thought that I would have to spend so much time thinking about at 31. It has been a hard topic for me.
The hardest moments and what keeps me going
With the idea of giving up on chemo and feeling like, “If I do this, I do not know what is going to happen,” what gets me through is having faith that it is going to all work out. I lean on my faith and my religion.
Sometimes, I want to give up. It’s hard to be positive all the time about cancer or the fact that I still have cancer. It’s frustrating because I’m a year into this. I have gone through all this treatment. I have done seven rounds of chemo and ten rounds of radiation. It’s frustrating to compare myself to others who, once they are done with treatment, have clear scans and put their cancer journey behind them. I get upset that I still have cancer and that I will always have cancer. Why did this happen to me and to this extent? It’s frustrating that I do want to give up sometimes.
What keeps me going is that I want to keep living. My dad always tells me to focus on the big things and the fact that I am still alive. I’m grateful to still be alive and that I still get to spend time with my loved ones. It has given me this perspective that other people do not have: to focus on what matters. Not that other things do not matter, but at the end of the day, your loved ones and experiencing life are so important and something to be grateful for. I think that’s what keeps me going.
Why I share my story on social media and “Cancer Questions with Clara”
I do a series on TikTok called “Cancer Questions with Clara,” where I answer any questions related to cancer. I am very open. I will talk about topics that other people are uncomfortable with. I do not mind sharing at all.
It’s important because a lot of people do not know anything about cancer. A lot of people have not been touched by cancer in any way. They do not know anybody who has had cancer. Maybe their grandparent had cancer, but they were not close to them or did not see them go through it, so they don’t know anything.
I approach it by speaking to the person who does not know anything. I think that is important because it educates people on what others are going through. I also want to normalize a lot of things because many topics are very taboo.
For example, sometimes I have to wear adult diapers. I’m not ashamed to admit that, but a lot of people would be uncomfortable sharing that. I do not want people out there to feel alone. I know there are plenty of other young women who have to wear adult diapers due to incontinence they developed from something else or from cancer treatment. That sucks, but I do not want people to feel alone. I want people to know that it’s okay and normal, and that other people go through that, too.
That is why I share a lot of this stuff. I want to educate people, to help people feel less alone, and to normalize different side effects. Those are my main motivations for sharing. It’s also a little bit selfish because I share updates on my journey. I got tired of repeating myself all the time to friends and family. It has been nice to point them to my social media to see my latest update about where I’m at with treatment.
Topics I want to talk about more: dating, disability, and financial toxicity
I need to talk more about dating and intimacy for young people with cancer. That is a big one that could be talked about, and I have not touched on it.
Another big one I have shared before is that I was heavily relying on a walker and I have moved away from that. I no longer need a walker or a cane, which has been fantastic. I’m able to drive again, which is so nice and gives me more independence. I could talk more about different tools and things that go along with disabilities.
Using a walker opened my eyes to how this world is not set up for people with wheelchairs or walkers. It was so frustrating to go into a building that only had stairs and no elevator. Maybe that is something I could touch on more because I know a lot of people who get cancer and end up needing a wheelchair or a walker.
Another topic that is uncomfortable for people to talk about is finances. Financial toxicity is a huge thing in the cancer world, with how expensive cancer treatment can be and insurance copays and everything. Some people shy away from talking about money. It is important to share what resources are out there to help lower or decrease costs for cancer patients, and what kind of financial assistance is available.
Ditching the walker, driving again, and getting my independence back
It has been so nice to have that sense of independence back. Using a walker, I had to rely on people to help me all the time, like opening doors and going up the stairs. It has been so nice not to have to do that.
Driving again has been incredible. I do not have to ask people for rides. I do not have to have people load the walker in the car. I did not drive for seven months, which was crazy to think about. It has been such a relief to have my own car back. My brother was borrowing my car since I wasn’t driving, which was fine, but he got a new car, so I got mine back. Now, if I want some pretzels, I can go to the store and get pretzels. It has been such a relief. It’s crazy when you do not have that independence. People take that for granted, being able to get in their car and go somewhere. I will never take that for granted again.
Writing a love letter to my body and coping with weight gain
I wrote a poem about my body, which was therapeutic to write down my emotions on paper. It helped to read it out loud. I hope it resonates with other people.
The cancer medications I have been on, especially steroids for inflammation and pain, did their job, which was great, but the biggest side effect was weight gain. I gained about 30 pounds in total, which is a lot considering I’m 5-foot-9 and usually weigh about 150 pounds. The jump to 180 pounds was a lot for my frame.
I never had weight troubles my whole life. I felt I had a good athletic build and a pretty normal-looking body. I did not worry about my weight until I gained 30 pounds. It was not overnight, but it was a slow increase. It felt like every time I went into my cancer center and they weighed me, I gained another five pounds. It was so frustrating.
I wanted to write this poem as a tribute to my body. Even though my body looks different now, it is not always going to look this way. I am going to lose the weight; it is just going to take time. I will lose it eventually. Bodies are malleable. They bounce back.
I wanted to honor my body for keeping me alive. Maybe I gained weight, but it kept me alive. It survived all these things I went through in the hospital. I went into sepsis. I almost died, yet my body still bounced back. It endured a lot of trauma, and I am still here.
Writing it was a way of getting my emotions out and processing what I had been through. That goes for any journaling. It’s a way to get things out. I sometimes need that release of emotions to fully process everything.
How targeted therapy has given me new hope and my message to others
Targeted therapy has definitely given me a new sense of hope. There are a lot of great things that can come from cancer research. The research is always evolving. They are always coming out with new things, new trials, and new ways of treating cancer.
Funding for cancer research is so important. It has given me a lot of hope. I feel very optimistic. I have seen a lot of good reporting on the statistics and data from the specific drug I am on. The prognosis of my disease has very much improved. I have a better outlook on what is to come, and hopefully, I will live for a long time on this targeted therapy. I’m grateful that they found the ALK-positive biomarker. Biomarker testing is so imperative.
My message for others would be not lose hope. Things are always evolving with cancer research. There may not be an option for you today, but give it time and maybe there will be something approved that can help you then. Do not lose hope. There is something out there that can help.
Living with the uncertainty of cancer and rolling with the punches
It never ceases to amaze me how quickly things with cancer can change. That is the hardest part. There are a lot of surprises with cancer at every turn. For me, it’s about not expecting anything and just rolling with the punches. Hopefully, that method will keep me alive for a long time.

Inspired by Clara's story?
Share your story, too!
More ALK+ Lung Cancer Stories
Megan F., Non-Small Cell Lung Cancer, ALK+ Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
Clara C., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Pelvic pain and discomfort, bladder issues related to pelvic tumors, incontinence, pain in the lower back and hip
Treatments: Chemotherapy, immunotherapy, radiation therapy, targeted therapy (lorlatinib)
Stephanie K., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent and intense cough, general feeling of sluggishness
Treatments: Chemotherapy, targeted therapy through a clinical trial, radiation therapy
Ruchira A., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Mild intermittent cough while talking, low-grade fever, severe nonstop cough, coughing up blood, collapsed left lung
Treatments: Surgery (lobectomy), targeted therapy
Laura R., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Persistent cough, fatigue, bone pain
Treatments: Targeted therapies (tyrosine kinase inhibitors or TKIs, including through a clinical trial)