Hannah’s Chronic Lymphocytic Leukemia (CLL) Story
Hannah’s journey with chronic lymphocytic leukemia (CLL) that later developed 17p deletion includes a backdrop of family bonds and healthcare exploration. Amid the pandemic, she and her husband started an at-home bakery. Parallel to her bakery venture, Hannah is a parent to two teenagers who she adopted from foster care.
After her CLL diagnosis, Hannah was propelled to actively engage with healthcare professionals. She pursued second opinions and a CLL specialist, highlighting the importance of informed decisions and collaborative medical approaches.
Her ability to navigate treatment-related hurdles has made her an expert in self-advocacy. She explains how she manages the side effects of ibrutinib (Imbruvica), venetoclax (Venclexta) and why she believes everyone deserves high-quality medical care.

- Name: Hannah D.
- Diagnosis:
- Chronic Lymphocytic Leukemia (CLL) with 17p deletion
- 1st Symptoms:
- Fatigue
- High white blood cell (WBC) count
- Treatment:
- Ibrutinib (IMBRUVICA))
- Venetoclax (VENCLEXTA)
- Monotherapy
- Rapid ramp up
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
- Diagnosis
- Finding the Right Doctor
- Treatments
- Being on ibrutinib (IMBRUVICA)
- What was switching to ibrutinib (Imbruvica) like?
- How did you work through the initial side effects of ibrutinib?
- Did the side effects subside, or did you tough through them the entire time?
- What was effective in managing the side effects?
- What made your doctor want to switch you on to ibrutinib?
- Is it important to mention the little changes happening between visits?
- Can you describe why another treatment decision had to be made after six years?
- Being on Venetoclax (VENCLEXTA)
- What conversations did you have with your doctors about changing your treatment regimen?
- Why did your doctor want to put on venetoclax instead of a combination therapy?
- Describe the ramp-up with venetoclax
- Did you experience side effects with venetoclax?
- What was the ramp-up with venetoclax like?
- What is the everyday regimen like with venetoclax?
- Did taking venetoclax make you think about your future differently?
- Being on ibrutinib (IMBRUVICA)
- Discovering the 17p Deletion
- More CLL Patient Stories
Diagnosis
What would the back cover of a book about you say?
It would say “on her third life in the 57 years that she’s been alive.” When COVID happened, my husband and I started an at-home bakery. Something I’ve wanted to do my whole life, and now I’m doing it.
We also never had children biologically, and we are currently in the process of adopting two teen boys from foster care. They are amazing.
I have a fantastic husband who’s an executive chef, and he’s fantastic. I’m completely spoiled by that. I have so many wonderful blessings in my life, but those are just a few of them.

What were the first symptoms of CLL?
I didn’t have any symptoms that I noticed. I dealt with fatigue off and on, and I just thought that was just part of who I am because I don’t really remember a time I didn’t deal with that.
I had seen my general practitioner (GP), and she informed me that I had a high white blood cell count. My response was, “Well, I don’t remember a time where a doctor hasn’t said that to me, and they always followed it up with, ‘Look, it’s nothing. You probably have a little infection getting started, or maybe you’re nervous about being here.’” I never had that white coat syndrome. I was never nervous about going to the doctor, but they always chalked it up to a combination of those things.
Back then, my husband and I had placement of six kiddos from foster care, and he was out of town for training for his new job. My GP said, “Look, I’ve told you that you have a high white blood cell count. I’m setting up an appointment for you with an oncologist.”
I went to the oncologist and had a bone marrow biopsy, and she said, “Yes, you have chronic lymphocytic leukemia.” I said, “I can’t. Don’t have time. My husband’s out of town. I’ve got six highly traumatized kids. Can’t do that. What else could it be?”
She said to me, “Listen. You have two options. You can do treatment or just wait and see what happens. If we do treatment, it might come back in a year, or it might literally never come back. Or you could just watch, hang in, and see what’s going to happen.”

How did it feel to be referred to an oncologist?
My husband was out of town. My next-door neighbor said, “I had a cancer diagnosis once, and I’m sure you’re not going to get that diagnosis, but I’d like to go with you because no one should ever go to a results appointment alone,” and I said, “Well, that sounds like a good idea.”
She came with me, and she heard that diagnosis with me, and again I just responded with, “I can’t. I’ve got six kids. I can’t. But I’ll think about it, treatment or no treatment.”
My doctor said, “In my opinion, let’s be aggressive.” She never explained watch and wait to me or any of those options. It was just: do you want to be aggressive and treat it, or do you just want to wait and see what happens? Well, I want to be aggressive and treat it. I don’t even understand the question. Let’s do it.
On the way home, my kind neighbor, who had the foresight to invite herself to that appointment with me, she said, “You know, Hannah, it sounds like from the little bit that the doctor said, “Thank God you don’t have a worse cancer.”
I always look to the positive during times like this, especially when something is scary, and cancer is scary. No matter what kind of cancer it is, it’s scary. Any disease is scary. But there’s something about that C-word that terrifies us all. My initial response, aside from I don’t have time for that, was just, “All right, let’s do this. Let’s do this thing. Let’s get it over with. Let’s put it behind us.”
Whoever you are. Don’t care what your life is. Don’t care what your disease is. Don’t care if you’re sitting in a prison cell right now. You deserve to be alive and healthy.
Hannah D.
What kind of doctor were you seeing?
I was in New Albany, Indiana, which is basically a suburb of Louisville, Kentucky. I saw a local small-town hematologist. I don’t see her anymore; she is no longer practicing.
The lesson I learned from seeing that first hematologist was very important. First of all, it should have been a red flag from the beginning that she didn’t explain my options to me. She just said, “Here’s your two options.”Had she explained those to me, I would never have chosen to get FCR (fludarabine, cyclophosphamide, and rituximab), which is chemotherapy that’s not really even used for CLL anymore.
As we have learned about CLL, it learns the treatments and grows stronger. It eventually comes back, and you can’t use that same treatment anymore because the cancer itself has already figured its way around it.
Watch and wait is actually an excellent thing. I know it doesn’t sound like that, but if I’d understood my choices from the beginning, I would not have started treatment.
I’m now on my third line of treatment. I did the FCR. I did four treatments. After the first month, the nurses looked at my blood work and said, “It doesn’t even look like you’ve ever had cancer. This is fantastic.” I asked the hematologist, “Should I continue, or should I stop now?” And she said, “We’re going to do all four. Better to be safe than sorry. We’re going to do all four.” I wish I’d known to dive deeper and ask more questions about what she meant by that.
Then, about a year and a half later, at a follow-up, my hematologist came into the exam room and said, “Well, my dear, it’s time for us to do treatment on you.”
I said, “Again? Treatment again? Will it be the same treatment?”
The hematologist said, “Wait a minute. Have we done treatment on you in the past?” I’m going to need my doctor to know what she’s already done with me.
Watch and wait is actually an excellent thing. I know it doesn’t sound like that, but if I’d understood my choices from the beginning, I would not have started treatment.

The hematologist said, “It’s going to be Imbruvica, that’s what we’re going to do, and it’s just a pill. You’ll come here to my office and pick it up every month.”
I said, “Oh, okay. Well, why are we choosing that one?”
My hematologist responded, “Well, how am I supposed to know? I just know it’s the next line of treatment. There are too many things out there for me to know everything. I just know it’s the next line of treatment.”
I said, “All right. I work full-time. How am I going to figure out how to come to a cancer center that has the same hours as I work to pick it up every month? Isn’t there any way it could be shipped to my home?”
She said, “No, Imbruvica doesn’t do that. They’ll only ship it here.”

Getting a Second Opinion
I got a second opinion. I went to the University of Louisville because I always liked the idea of a teaching hospital, and that doctor spent almost two hours with me on our initial visit.
He did say, “Yes, Imbruvica is fantastic, and it is my recommendation to you, but you’re not ready for it. You don’t need it right now. I don’t see any reason for you to start Imbruvica now.” We waited a whole other year before I started on Imbruvica, which I ended up being on for six years.
Get a second opinion. Ask your doctor questions. If you don’t know what questions to ask, find a support group. I was very lucky in the support group I found on Facebook, frankly. I tried a few different support groups, but some of them didn’t fit me. Keep looking until you find the people who speak your language. I found the people who spoke my language, and they will help you with what questions you need to ask because that’s very, very important.
What questions should you ask your doctor on your initial visit?
Regarding the treatment, on that very first visit, where my hematologist gave me those options, I would have asked more questions. I wish I had asked what I was thinking, which was why on earth would someone not jump right into treatment? What are the pros and cons of either choice? That was a really important question to ask, and I didn’t ask it.
Now, knowing the experience I had with her, I don’t know how thorough she would have been in the answer. I feel like she made up her mind. She already knew what she wanted me to do, and I don’t know her reasons for wanting that. I’m just going to leave it at that.
It’s important to have a good relationship with your doctor, and you don’t want to do anything to disrupt that. But I asked her, at the advice of my CLL support group, I brought up the topic of also seeing a CLL specialist.
She reacted negatively. She said, “Well if what you’re wanting is a second opinion, Doctor so-and-so is my partner. We’ll get that second opinion for you.”
I said, “Well, it could be a second opinion, I guess, but I think it is ongoing. I would like to have my local oncologist and specialist work in concert. Would that be okay?”
She did not react favorably. She invited me to go find another doctor if I wasn’t happy with this, but that she was a local expert.
I let that be her response without really realizing that it should have been my decision right there to leave and find another doctor altogether, not just a second opinion.
That oncologist is no longer practicing. I don’t know why. I don’t know the story about it, but it’s kind of comforting to me. Do you know what that tells me or what I’m letting it tell me? My instincts, in hindsight, about her were accurate, and that’s important. Listen to your instincts.
Finding the Right Doctor

You want someone who’s going to go and have dinner with one of your other doctors and talk about you.
Hannah D.
Is it important to have a care team that works together?
Yes, absolutely. It’s crucial. For a few years, the first couple of years in that support group, all I just kept saying was everybody posting about, “See a specialist, see a specialist,” and I wish I hadn’t taken so long to let that drill into my head.
Now I have a local oncologist right across the river in Louisville who’s amazing and a fantastic specialist who’s about an hour and a half away in Cincinnati, Dr. John Byrd. He is outstanding. Dr. Byrd and my local oncologist, Dr. Stevens, work so well together.
One time, I was visiting Dr. Byrd, and it was one of the early visits with him, and I said, “Now, okay, so Dr. Stevens, he’s able to go in your system, and he can see your notes and everything about me, right?”
He said, “Well, yes, but I’m having dinner with him tonight, so we’ll probably discuss it then. I plan to talk about you.”
That’s kind of funny, but also how personal is that? You want someone who’s going to go and have dinner with one of your other doctors and talk about you — hopefully about your cancer and your situation. Not, “Oh, that Hannah. She asks too many questions.” It’s wonderful how they work together, and they both think so highly of each other. Can I tell you how comforting that is to me? It’s magnificent. It’s a huge part of my treatment for me.
I want to make sure everybody gets this message. I see one of the top 10 specialists in the US, therefore, in the world. I did that on purpose because I deserve to see one of the top 10 specialists in the world, and so do you.
Hannah D.
Why is it important to find a doctor locally in the community who you have a great relationship with?
You’re going to be getting regular blood work. If you want to only have a specialist, I think that’s doable, but you may have to travel to them. If you have someone local who has mutual respect for whatever specialist you choose, that’s really crucial.
In fact, I recently changed my treatment and was admitted to the hospital for one week for precautions. I did go to Cincinnati, where my specialist is, but he even said to me, “If you would prefer to do this locally, I have all the faith in Dr. Stevens and his team at Norton that they can handle this well.” That’s crucial in your treatment, having that type of trust in your providers.
I see Dr. Stevens regularly. Sometimes it’s every three months; sometimes it’s every six months. Over the past year, I was seeing him monthly. I can’t always go to Cincinnati. I’m still working full time, so that’s at least half a day off work, sometimes a whole day off work.
I can just scoot over to Dr. Stevens across the river, get my blood work done, see him, and then get into work. Maybe I’ll miss 2 or 3 hours of work. Maybe I can go early enough that I don’t even miss any work. It’s really good to have those options.

Why is it important to see a CLL Specialist?
I want to make sure everybody gets this message. I see one of the top 10 specialists in the US, therefore, in the world. I did that on purpose because I deserve to see one of the top 10 specialists in the world, and so do you.
Whatever your diagnosis is, find a person who knows the most about it. Find the person who’s at the forefront of treating it and of new treatments because you deserve that if you can travel.
We are not made of money, believe me. My husband and I, we’re both hard workers. But I’ve been so lucky that this guy is only an hour and a half away. If you can find someone, if you have a car, can you get there? If I needed to fly to someone, I think I would try to figure that out. Even if you have to travel to someone, it’s worth it. It is 100% worth it.
People who are in the top 10 are the top 10 for a reason. Who else would you want leading up to your medical care? Whatever your diagnosis, you are worth it. You deserve the best that’s out there.
What if your insurance doesn’t cover the doctor you want to see?
Work with your insurance. When you find someone you want to be one of your providers, call that provider before you call your insurance. What I’ve experienced is — and this has been many years over different insurance companies — that provider will always be listed as one that they cover, but when you call that provider, and you try to get set up for that initial appointment, and you give them your insurance information, they say, “Oh, we don’t accept that. We haven’t accepted that for years.” It’s important to reach out to your provider first. Look for the best. There’s no reason not to. Don’t let anything stop you.
Treatments
Being on ibrutinib (IMBRUVICA)
What was switching to ibrutinib (Imbruvica) like?
My insurance rejected it. It’s horrifically expensive. It’s something like $16,000 a month. Who do you even know who can afford that? I had to call it off. The hospital said, “No, no, no, no, no, no. That’s just our first attempt. We have other ways.”
They reached out to the makers of Imbruvica, and I was put on a plan called Imbruvica By Your Side, where I paid a $10 co-payment monthly for six years.
I had some really bad side effects, and I remember seeing a lot of different people on the Facebook support groups who said, “Well, I did try the Imbruvica as long as I could, but the side effects were so painful I had to quit.”
I knew from what I was hearing through the research through the hospital that Imbruvica was doing amazing things. I told myself right then and there whatever side effects I have, I’m going to tolerate. I just am, and I’m going to get through, and I’m not going to quit because of how hard the side effects are. I’m not going to quit. I have to give myself every chance here.
Sure enough, I had terribly swollen and painful joints. It was really rough. I also had pretty severe fatigue. You often have fatigue from CLL anyway, so that was a real double whammy.
The first few weeks on it, maybe 2 or 3 months, were pretty rough. I would sit at work with my hands on the mouse with a heating pad on top of that, and half the time, there were just tears in my eyes because it really hurt.
All along, I was telling myself, “I know that the side effects are temporary. As with many medications, the side effects are temporary. That’s going away.” And also, it’s a reminder to me that Imbruvica is at work on my cancer. That pain really was a double-edged sword because it was rough. But it was also my reminder that good things were going on inside of me.
Whatever pain you’re going through, work through it. Don’t look away from it; then you get stiff, and the pain doesn’t leave.
Hannah D.

How did you work through the initial side effects of ibrutinib?
I learned how to work through those swollen and painful joints because I used to flip furniture. It’s just a hobby that kind of paid for itself because I love doing it. I had this China cabinet that I’d bought months prior that I hadn’t been able to do because I couldn’t hold a paintbrush. I just couldn’t; I couldn’t hold it. I couldn’t make my hand fit around it and embrace it. It was too painful.
My husband, one Saturday morning, got up really early and woke me up and said, “Come on, let’s go. I know how you’ve been depressed because you haven’t been able to work on this China cabinet.”
He had taken a paintbrush and tied a big rag around it. And it worked! I was so happy that about an hour after painting with the giant handle of a paintbrush, I realized I didn’t need it anymore; I was working through that pain.
Within an hour’s time, I took the rag off, and I was holding a paintbrush normally, and I finished painting. That was one of the most transformative moments for me because I knew that whatever I had to deal with, there was always a way to figure out how to deal with it. Those terribly swollen knuckles, I got them all the time, and I figured out how to literally work my knuckles to where it wasn’t so painful.
I’ve kept that lesson with me about a lot of things in my life. Whatever pain you’re going through, work through it. Don’t look away from it; then you get stiff, and the pain doesn’t leave.
Did the side effects subside, or did you tough through them the entire time?
Probably the first year and a half, maybe even two years, the side effects were still there. After that, they just faded, and I had the occasional bouts of side effects. The side effects were mostly temporary.
What was effective in managing the side effects?
Let me introduce you to my water glass. It sounds funny. I know I sound like everyone’s mother, and I kind of am. I’m a foster mom. Drink water like it’s the only thing keeping you alive.
I have 2 or 3 of these a day during the business day, and that does a few things. Staying hydrated is one of the best things you can do for yourself, whether you’re in treatment or not in treatment. It really does a lot for you.

What made your doctor want to switch you on to ibrutinib?
My white blood cell count just kept climbing and climbing, and my fatigue just had a big impact on me. There was a point where my office was in a far corner of the universe of my office building, and when I would have to go to the ladies’ room, I was so tired. I would get up and walk outside my office door to go to the ladies’ room, which was maybe 20 steps, and I would already have to sit down. I would rest for a moment. Then I would get up, and I would purposely take a long way because it was a back hallway where people didn’t usually go. I had to lean on the wall the whole time because I was that fatigued.
Is it important to mention the little changes happening between visits?
Absolutely, It’s really crucial. You might experience some symptoms and side effects and or whatever that you think, “Well, this is just part of it. The doctor must already know I’m dealing with this because it’s part of CLL.”You have to say those things even if you think it might seem he already knows all this; there’s no point in bringing it up. You must tell him or her everything you’re feeling.
The symptoms that you’re experiencing are meaningful. They might be temporary. It might be one of those things that come and go and to be expected, or it might be a sign of disease advancement. It’s important to be vocal and have a good line of communication with your provider.
Can you describe why another treatment decision had to be made after six years?
At about four years, my numbers started not responding quite as well as they had in the past. My local oncologist and my specialist had said to me, “We know that Imbruvica is eventually going to fail you, and it’s begun. That has begun. It’s still doing very well. But we need to start talking about what changes we’ll make in the future.” It was exactly as they said. It’s interesting because they said, “Imbruvica is beginning to fail you.”
At that point, there was a mix-up between the specialty pharmacy and my insurance company. They have to go and file it every month, even though it’s going to be a rejection. It’s just part of the process, and I went for four days without taking Imbruvica.
I think my CLL was getting so much worse; being off Imbruvica for four days, I almost ended up in the emergency room. I was so ill from it. My lymph nodes got big. I started having lymph nodes swell and be very painful in places I did not know I had lymph nodes. I couldn’t lie back on a pillow because the back of my head was in pain. It was horrible.
In my mind, “Oh, Imbruvica is really failing me,” but look what it was still doing for me while I was taking it. While it became obvious that it was going to soon be time to switch treatments, it was also comforting to know it was still doing something for me.
Being on Venetoclax (VENCLEXTA)
What conversations did you have with your doctors about changing your treatment regimen?
In the beginning, venetoclax was always thrown in there. There were some trials we discussed, and I was very interested. I love a good trial, and I think they’re fantastic.
Then I started thinking, “In a way, I feel like I was already in a trial, and it didn’t work by seeing my first oncologist,” which FCR was great at the time, but I shouldn’t have done that.

At this point, I wanted to go for something a little more proven. We discussed venetoclax. There was another trial at the time where my specialist said, “We’ll do venetoclax, for sure, but there’s a very interesting trial in China that I think is going to be a game changer for everyone.”
However, it failed in China because the dosage was not high enough, which is exactly what they predicted. Over here, the FDA did not approve the higher dosage. That trial was not ready for me yet.
He said to me, “Venetoclax is what we’ve been talking about all along. I think it’s tailor-made for you.” In fact, when I was in the hospital getting my rapid ramp-up of venetoclax, he came into my room and said, “You are responding immediately to venetoclax. This is actually quite remarkable.”
I don’t even remember what my white blood cell count was when I went to the hospital. I think it was in the 50,000s, which we know really shouldn’t be over 10,000, or something is wrong. On the third day in the hospital, my white blood cell count was 5,000. You can imagine how amazing that feels.
I went the other day for a checkup, and it’s at 4,000. It’s impressive, and it’s amazing. But Dr. Byrd said to me, “Let’s look at maybe eight, nine months at the most on this, and then we’ll look at a good 2 or 3 full remission. What do you think?” And I said, “Well, I think yes! Let’s do it!” That just shows again that Dr. Byrd is trustworthy, as trustworthy as a doctor can be. I have faith in him, and it proved to be a good decision.
Why did your doctor want to put on venetoclax instead of a combination therapy?
He gave me the basics, which is if he couples venetoclax with something else, we don’t want to expose me to too many types of treatment for this because of the nature of CLL. He’d like to be able to have future options, and I’d like him to have future options.
Venetoclax is working amazingly. Again, that just proves him right. I know that I made the right decision in trusting the right person. He gave me enough information at the time to help me understand it, and I’ve let go of that because there’s been no point for me to hold on to all that.
Describe the ramp-up with venetoclax
The options are either you do the rapid ramp-up in the hospital, and after the week, you’re up to your dose. There’s the other option where you go once a week or maybe even once a month, and you have to be in the hospital for a day or two each time you go.
My doctor said, “This is the way we do it here. You spend as much time in the hospital when you stay here for the first week or when you go and spread it out over however many weeks or months, you spend just as much time in the hospital, but you’re not driving back and forth every time for every visit.”
He said, “I like having the view of you and your body and your response the entire time when you when you come, and you get a treatment, and then you leave, and you come back for another week.”
He explained to me that the wing we would be in is not the ICU, but it is treated just like the ICU. While mask restrictions and COVID restrictions have been lifted everywhere else on the planet, not so much in this ward so I knew I’d be safe there for a week.
Did you experience side effects with venetoclax?
The idea was that I would be on Imbruvica for maybe a month or two or four at the most and then taper off of that. Well, I had such strong gastric issues between venetoclax and having both venetoclax and Imbruvica, and I was concerned because it was severe.
My doctor said, “You’re responding so well to venetoclax. I think you’re having this severe issue because you’re on both. So let’s go ahead and say goodbye to Imbruvica.”

Within a couple of days, I was completely healed from that. That was a huge concern of mine because I couldn’t leave the house. I do have some strong fatigue that I deal with, but it’s already lightening up. So is my dizziness, which I think is almost gone; that’s something I’ve had to deal with vertigo for years with Imbruvica. I didn’t know if it was CLL or Imbruvica, frankly, but that’s almost gone. That’s been pretty amazing for me.
I just remind myself that whatever I might be feeling, which could be a side effect or a symptom, is likely temporary. I still talk to my doctor about it every time.
What was the ramp-up with venetoclax like?
The day I arrived at the hospital, it was a Monday, and they gave me my first pill that day. I was on 100 mg. Then, the next day, they doubled it, and the next day they tripled it. Then, on the fifth day, I was on 400 mg, and that’s my desired dose, which is where I am.
I did the first day, you know, brought my full set up for my office so I could just work from the hospital. The first day was great, and I worked and got some good hours in.
Then the second day, I woke up, and I was like, oh, I’m a little sleepy, but I’ll do this. I walked over to where I had my whole little office set up in the corner of the hospital room, and I couldn’t focus. I was nodding off and thought, Well, I’ve just had a terrible night’s sleep in a hospital bed. That’s going to be part of it.
Then, the next day, it was even worse. I could not focus. I just couldn’t. I live in an Excel spreadsheet. That’s my happy place. And I knew when I was trying to do some work in Excel, and I just couldn’t focus. Couldn’t figure out where I was in that sheet or what I was doing. I’m used to working with some pretty advanced and intricate spreadsheets. I got really down, and I started to tear up in the hospital bed because now you’re taking away my livelihood and the way I spend my days. Don’t take my ability to master Excel away from me.
I just needed a moment. Don’t dwell on things, but I knew I needed a moment. So I started to tear up. And in walks rounds. They’re doing rounds into the hospital rooms, and it’s the changing of the nurses. So I’ve got all the doctors doing rounds and all the nurses, the outgoing and the incoming. I’m sitting there teary and frail feeling, and I got this immediate, ‘Wait a minute. What’s happening here? You have a positive attitude and are patient. You’re always so cheerful. You have the best attitude.’ I would go and walk up and down the hallway, and they love that. They would cheer me on, and they were happy to see that. So when they saw me sitting in my hospital bed tearing up, feeling frail, they said it was like the record scratched.
When my liver has a break from processing those oncology meds for two or three years, that will be fantastic.
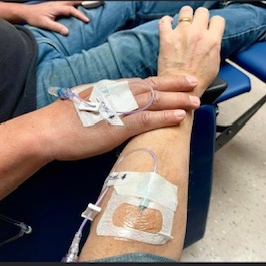
They all said, What? Talk to us. What’s happening? And I just said, What I just told you. I can’t focus. I’m feeling like I can’t function in my life the way I need to function. They all responded to me with; you are not realizing what your body is going through right now. Your body is doing big, big things, probably bigger than it has ever done before. And so I gave myself that. I gave myself that. So that was a comfort to hear all of them say that – the nurses, the doctors, everyone. They were so supportive but had to realize that my body was, I don’t want to say, taking a hit, but that sure is how it felt.
The way they put it is best. My body was doing big things. You know, they said this is an oncology med, not a new headache medicine. You forget that because you’ve taken Imbruvica for six years as though you’re taking Advil. You don’t think about it. You take it. It works fantastic. But you just have forgotten. This is huge, and you’re okay. This is quite expected for what you’re going through. So that was comforting to me. But that’s that’s what I dealt with. And I still have lingering fatigue. It’s getting better every single day.
What is the everyday regimen like with venetoclax?
I take it at night. I was told it might cause some issues. It’s good to take it at night because [you can sleep] through. I haven’t had any issues, so I started out taking it in the morning, and then I heard that some people recommend taking it at night. So I did that. And that’s not been an issue for me.

Did taking venetoclax make you think about your future differently?
I know that this is CLL, and it’s chronic. So I’m not confused about the fact that I might get a 2 or 3-year remission out of this. Don’t confuse that with the cure. I think I started thinking of my life differently when I was first diagnosed ten years ago, and that was sort of at work in me when I didn’t even recognize it. But I did start doing things a little differently. The thought that venetoclax is going to be a limited duration for me like that lets my body have a break for a while. I’m on a lot of other meds, too, for high blood pressure, type 2 diabetes, etc. So, let my body have a break. When my liver has a break from processing those oncology meds for two or three years, that will be fantastic.
Also, as we like to say in our house, #StillCOVID, for us, COVID’s not gone; I have to wear a mask everywhere I go. The thought that I’ll be a little less high-risk during those two to three years is really, it’s really appealing. So I’m really looking forward to that, and I’m already appreciative for what I know is going to happen.
Discovering the 17p Deletion
What have you learned?
Find the specialist. My husband has a diagnosis right now where there are no specialists supposedly in the world, so we’re trying to find the next best thing. Nobody really specializes in his disease. That’s not stopping us from looking for the people who know best how to treat it.
Also, look for cutting-edge stuff. Just remember that you deserve that. There’s no good reason. Whoever you are. Don’t care what your life is. Don’t care what your disease is. Don’t care if you’re sitting in a prison cell right now. You deserve to be alive and healthy. You deserve to have the person who knows the most about your disease, advise you, and treat you if possible.
Suppose you are running into roadblocks with your, say, your insurance. Ask that specialist. All right. Well, what? You can’t be my usual doctor. My insurance isn’t going to pay for it. What can you leave me with? What do you want me to know? What are the most important things you want me to leave here knowing, even though I’m not going to be coming back? You know, get out there and get what you can get. Information, education, knowledge. Go get it. Go get every piece, every piece of knowledge that’s not nailed down. Get it and bring it home with you.
What was it like picking up the 17p deletion?
When I went to Dr. Byrd for the first time, the specialist in Cincinnati, the nurse practitioner, was looking at my blood results. She said, ‘Now, had you already been told you have 17p deletion?’ I said, ‘What? No. Do I?’ And she said, “You do.”
That was hard for me to hear. I know through these ten years of support groups, I know people with 17p deletion who have died. I always used to say to myself, well, at least I don’t have 17p deletion or one of those horrible markers. That was a really scary moment for me. Dr. Byrd came into the room, and he said, “I’m sorry.” I said, ‘I don’t want you to say that to me. I don’t want to hear my doctor go; I’m sorry. No, I want to hear my doctor say, ‘Well, the 17p deletion isn’t the problem it used to be.’

And he stopped me right there, and he said, “I care, and I want you to know I’m sorry. But before you say another word, just so you don’t think I’m saying this because you want me to, 17p deletion is not as scary as it used to be. So many treatments that we have now make that a non-issue or less much, much less of an issue.”
He said, “As I’m sure you know, treatments are getting better all the time. This is a very big area of study. There’s going to be more and more and more in the future, so don’t let the 17p deletion make you feel like this is a death sentence because it is absolutely not. That is false. Get that out of your head.”
I didn’t have it in the beginning. I picked it up along the way. Now, who’s to say when that happened? We don’t know. We don’t know when that happened, but I had a FISH test in the beginning and did not have 17p deletion at the time. I guess mine is aggressive, but, you know, so is science.
More CLL Patient Stories
Lynn S., Chronic Lymphocytic Leukemia (CLL)
Symptom: Elevated white blood cell count
Treatments: Chemotherapy, targeted therapy (BTK inhibitor)
Serena V., Chronic Lymphocytic Leukemia (CLL)
Symptoms: Night sweats, extreme fatigue, severe leg cramps, ovarian cramps, appearance of knots on body, hormonal acne
Treatment: Surgery (lymphadenectomy)
Margie H., Chronic Lymphocytic Leukemia
Symptoms: Large lymph node in her neck, fatigue as the disease progressed
Treatment: Targeted therapy
Nicole B., Chronic Lymphocytic Leukemia
Symptoms: Extreme fatigue, night sweats, lumps on neck, rash, shortness of breath
Treatments: BCL-2 inhibitor, monoclonal antibody







Leave a Reply