CLL Conversations
How to Work with a CLL Specialist and Build a Strong Team
Are you or someone you know navigating the complexities of chronic lymphocytic leukemia (CLL) treatment? We understand the importance of building a strong support system and collaborating effectively with multiple doctors. The Patient Story features a panel of experts and individuals with firsthand experience.
This discussion features Dr. Nicole Lamanna from Columbia University Irving Medical Center, Dr. Spencer Bachow from Boca Raton Regional Hospital, and CLL patient Lisa P. Our CLL patient voice leaders, Michele Nadeem-Baker and Jeff Folloder, moderated the conversation.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
- Introduction
- Finding a CLL specialist
- How CLL specialists work with local hematologist-oncologists
- Lisa’s CLL story
- Scott’s CLL Story
- How to find the right CLL specialist
- When to see a CLL specialist
- Patient’s perspective working with a local oncologist & a CLL specialist
- Communication between a local oncologist & CLL specialist
- Christy’s CLL story
- Different opinions among doctors
- Hematologist-oncologist vs. CLL specialist
- Limited options due to HMO restrictions
- Living your life with CLL
- Conclusion
Introduction
Stephanie Chuang: I’m Stephanie Chuang, founder of The Patient Story and a blood cancer survivor. It’s another edition of CLL Conversations and our topic is how to build a strong CLL team. We have an incredible group of people to help [give] some guidance, sharing their own experiences from the patient’s perspective as well as from the physician’s perspective.
Our goal at The Patient Story is for patients, by patients and to help those who have been diagnosed with cancer or those around them navigate life after that diagnosis. Our tagline is Humanize Cancer. We specialize in in-depth conversations with patients, care partners, and cancer specialists. Our goal is to help people through a really tough time.

Michele Nadeem-Baker: Thank you so much, Stephanie, for ensuring that the CLL and SLL communities are spoken to here at The Patient Story. I’m Michele Nadeem-Baker, a medical and health journalist and also a CLL patient.
When I was first diagnosed in 2012, things were so different in the CLL landscape. Once I started treatment, I made a vow to try to help other patients. Since then, I’ve been growing my patient advocacy and patient leadership and one of the people I do that with is Jeff.

Jeff Folloder: Hi, I’m Jeff Folloder, a passionate patient advocate. I really take this seriously because it’s really, really important for me to share that you can live a great life with CLL. Not just a good life; a great life.
I just entered my 14th year of dealing with CLL and it seems like yesterday I got the diagnosis. But what I’m really excited about right now is introducing you to Lisa, someone I met years ago in a waiting room and I’m so glad that she’s going to share her story.

Groups like this are so helpful so I’m very grateful, especially when you’re new and don’t know what lies ahead. There’s so much information.
Lisa P.
Lisa P.: I’m Lisa. I was diagnosed in 2012. I just went for a routine physical and got the diagnosis, which came as a surprise, but it doesn’t define who I am.
I’m a mom of three grown children. I’m a yoga instructor. I actually went to yoga after my diagnosis to help deal with it. I used to go to yoga as a workout and once I was diagnosed, yoga became much more than that to me. It became a mental practice that helped me not to spin the stories in a scary direction, but to stay grounded and focused on what was going on without being so fearful.
I was very grateful to have someone like Jeff to talk to; really comforting. I remember meeting in that waiting room after meeting online. Groups like this are so helpful so I’m very grateful, especially when you’re new and don’t know what lies ahead. There’s so much information.
Jeff: This is going to be a fantastic discussion. We also have two world-class medical experts joining us. Dr. Nicole Lamanna is a hematologist-oncologist at Columbia University.

Dr. Nicole Lamanna: I’ve been doing this for a long time. I started at Memorial Sloan Kettering and was there for 12 years. I’ve now been at Columbia University since we set up a leukemia service. I’m also a staunch CLL patient advocate as well as a CLL physician.
I had an interest in leukemia when I was in my early days of training. I found it a very complex and unique disease. I was very fascinated by the immunologic things that can happen with CLL patients. I had a mentor who did CLL and I decided I would continue research. I’ve been doing that ever since. Twenty years of doing CLL, at least.
It’s a disease that you live with for a prolonged period of time. I like taking care of other aspects also, not just CLL. Folks have been with me for 20 years so it’s almost like a primary care internal medicine clinic. I enjoy building relationships that last a lifetime so that has also been a very important aspect of my practice and one of the other things I like about treating patients with this disease.
Michele: Dr. Lamanna, it’s always such a joy to see you and to also be with you on these programs. You are such an advocate for all of us and what a specialist you are. It’s a delight to have you with us.
We have with us Dr. Spencer Bachow, a hematologist-oncologist at Boca Raton Regional Hospital.

Dr. Spencer Bachow: I knew I didn’t want to do internal medicine; I wanted to be a subspecialist. It wasn’t until I did my malignant hematology rotations as an internal medicine resident that I had role models. These were the types of doctors that I always dreamed of. The way they thought about patients was very different and I knew this was the type of doctor I wanted to be.
I got into it from great role models and the same with CLL. Dr. Lamanna was my fellowship mentor and you could really feel the excitement she and everybody else had in this field.
A lot of the cancer advances that we’ve seen in CLL are some of the biggest. The transformation of the treatment of CLL is one of the biggest cancer advances of the 21st century.
Finally, like what Dr. Lamanna said, it’s a very heterogeneous disease where a lot of patients do well long term. You could establish long-term relationships with them. You get a chance to help people during some of the most difficult stages of their lives.

Finding a CLL specialist
Jeff: One of the things that Michelle and I constantly hear, constantly see, especially in online groups, is the recommendation to get a CLL specialist. It’s almost always the first thing that’s tossed out to someone new who shows up. Go get a CLL specialist.
I’m fortunate I live in a metro area. Michele’s fortunate she lives in a metro area. Getting access to a CLL specialist is not very difficult for us. We have them around.
Not everybody who gets diagnosed with CLL has that access. Or maybe they do. How do you build a strong CLL team when you might not necessarily have one in your hip pocket?
My first doctor wanted to start a treatment program that was ancient by CLL standards and I quickly learned that it wasn’t right for me. I had to make changes. I had to get a CLL expert on the team. I did just that and here I am 14 years down the road, doing great because I built a good team.
Michele: Jeff is the second CLL patient I ever met and that was probably a year or so into knowing I had CLL. He came up to Boston and we both spoke at an event. It has been wonderful having Jeff as my CLL buddy and all the things that we’ve been doing together. We are both so passionate about this.
I didn’t even know what a CLL specialist was. I did know there was such a thing as a hematologist-oncologist, but just because I knew one personally doesn’t mean I really knew exactly what all this meant. I think that’s how a lot of us are when we’re first diagnosed.
I was first diagnosed while I was working in South Florida. I had the job of my dreams. I was at the C-level of a major international company with a corner office overlooking Biscayne Bay.
I was diagnosed by someone at a hospital nearby except they didn’t explain anything about CLL. They told me to come back in four months. They had nothing to give me when I asked. But again, this is back in 2012. Things have come a long way since then, thank goodness.
I left everything behind; I really didn’t have to. I quit my job. I was living between Boston and there. I moved back north because I knew Boston has a plethora of healthcare.
When I was diagnosed, I didn’t even know there was such a thing as a CLL specialist. I didn’t even know what CLL stood for. I started seeing a CLL specialist once I heard about one and that’s how I started building my medical team.
Since then, I have been a huge proponent of having a CLL specialist on your team. You don’t have to have one to see all the time if you don’t live near one. Jeff and I were very blessed in that we happen to have centers near us.
Jeff, when you heard about specialists, did you get to one right away or did you take your time in seeing one?
Jeff Folloder: For me, it was right away. I did not feel comfortable with the advice that I was getting. I leaned on a family member who worked at a large research facility in Houston and they got me hooked up.
What you and I have been doing over the past years is encouraging people to get in touch with a CLL specialist, no matter where they are. That’s actually something that Lisa was encouraged to do.

How CLL specialists work with local hematologist-oncologists
Jeff: I want to toss this to Dr. Lamanna. How do you work with a local hematologist-oncologist? How does this whole concept of having a CLL expert quarterback actually work in real life?
Dr. Lamanna: You both have been blessed by being in cities that have major academic centers that have CLL specialists.
CLL is not a common disease like breast cancer or colon cancer. CLL is relatively small when we compare them to solid tumor cancers. Most oncologists might see a little bit of this and a little bit of that, and that’s fair.
Although I would love for every CLL folk to come and see me in New York, we know that’s not feasible or possible. Oftentimes, folks will come for an opinion, to discuss their disease, or at a crux where they might need treatment.
I will communicate via phone, email, or message and start a relationship with their local person to help guide them, particularly if this is not a disease they typically treat.
As Dr. Bachow alluded to, there’s such an explosion of treatment options. Depending on other factors, navigating these treatments and choosing between different drugs can seem a little daunting. I’ll try to communicate with their local physician to see if I can help them, guide them, and be a link between the patient and their local physician.
Sometimes it’s extremely easy because their physicians are very willing to have that extra specialist help them in an area that they’re less familiar with. Sometimes it doesn’t go as quite smoothly as I’d like.
My patients know me. Oftentimes, if I think something’s a red flag, I will speak honestly about that. I need them to find somebody that I think is going to be in their best interest. This isn’t about egos. I know many patients actually feel uncomfortable about having a team because they don’t want to upset their local physician.
Remember, this is all for you. This isn’t for me. This isn’t for your local physician. This is really about you getting the best care that you need for your CLL. If you’re uncomfortable talking about that with your physician, that could be a problem.
You want to be able to communicate with your physician and the physician team about your needs and any issues that arise. You’re going to build a long-term relationship so you want to find a local physician that you can trust, that you can work with throughout the years, and then if advice is needed from somebody like myself, they’re willing to take it because the likelihood is I probably see more CLL patients than they do.
Most of the time, it works well. Occasionally, there may be some issues that need a little bit of hand-holding until they smooth out over time so that you can also include the specialist, particularly at certain cruxes that might come along on your CLL journey.
Dr. Bachow: Echoing what Dr. Lamanna said, the CLL specialist is very important. There’s a huge landscape of all kinds of different treatment options that we didn’t have several years ago. Knowing when to use them and how to safely use them can be tough for anybody. Employing the CLL specialist is very, very, very helpful as a local CLL doctor and a local hematologist-oncologist.
A lot of times, we don’t have access to certain clinical trials that our patients may be candidates for and may be interested in and that is a huge plus you can get when you have your patient meet with a CLL specialist. The local doctor is still important because things happen. Complications happen, hospitalizations sometimes occur, and if you don’t live near your CLL specialist, having somebody there who knows your care is very important.
Additionally, a lot of the CLL treatments these days can be very labor-intensive and require very frequent follow-up. Unless you’re planning on moving to where your specialist is, having a local person that you can trust, that your CLL specialist trusts and that can work together as a team is so important.
Lisa’s CLL story
Michele: I met Lisa about four years ago. We’ve been buddies virtually but she lives near where I used to live in Florida. We even know some of the same people.
I was really touched by how you educated yourself on CLL. You learned a lot. You were able to be your own advocate, which is so important, and I’ve always noted that. Could you share when you were diagnosed, your experience, and how you ended up being educated and advocating?
Lisa: I was diagnosed during a routine physical with my primary care doctor. She re-did the blood work, thinking it was a machine glitch, and it wasn’t.
I was immediately sent to this wonderful local doctor at the time and I adored him. He gave me some information, but he wasn’t a CLL specialist by any means and he was very open to me going to other places.
It was really the resources online, support groups that I found, and Jeff that I got directed, speaking to people who had already lived this experience. They pointed me to the current treatments. Oral BTK inhibitors were just starting to explode at that time. Infusions were more common back then.
How to find a CLL specialist
Michele: How did you find your eventual specialist?
Lisa: Once I was diagnosed and starting to get thrown into the trenches of what the reality of this was, I became very involved online, met Jeff, met some other people that had been dealing with CLL for longer, and you hear, “Find a specialist.”
There is a lot of information out there. I would watch Patient Power videos. The Leukemia & Lymphoma Society offers a lot of panels of doctors’ discussions. I would listen to them and listen to the new research. All these specialists are generous, giving their time, and that is how I found both specialists that I went to just by watching videos and being my own patient advocate.
Dr. Lamanna sits on a lot of panels. I would watch these videos and hear her on these panels. On some of them, she was sitting right next to my other specialist. He was getting older and was going to retire, too.
I was just drawn to her. I loved how she spoke and how she relayed information. I loved her personality. I said to my husband, “I really like her. I want to go have drinks with her.” That’s how I felt watching the videos.
It was a small world. I had a visit with my local doctor at the time and I mentioned Dr. Lamanna to him. He literally looked at me and said, “I don’t know why I didn’t think of this before.” They knew each other very well. He texted her and said, “I have a patient and I’m sending her to you.”
My daughter was moving to New York. She was just graduating college. You have to find what’s going to work in your life and it makes sense. I was going to New York anyway so why not have a specialist there?
The puzzle pieces came together and I had this wonderful team. I felt that my local doctor had a better means of communication now. I love and trust my specialist and my local doctor. They communicate well.

Scott’s CLL Story
Michele: We have Scott who talks about how he found a CLL specialist and his path to getting one.
Scott W.: Hi, Michele. My name is Scott. I’m a news photographer in Cincinnati, Ohio, and I was diagnosed in November 2019.
Finding a CLL specialist
Scott: At first, I didn’t know what a specialist was. I was assigned a hematologist at one of the hospitals here in town. It was a shock to find out that there’s this thing called watch and wait, which just didn’t make sense to me, as I’m sure it didn’t make sense to a lot of other first-time folks diagnosed.
I started doing some research and found that there’s some controversy, I guess, and some progress being made on whether watch and wait is appropriate or not. I started questioning my hematologist-oncologist about it and he didn’t really have any answers for me.
I sought out another hematologist, still didn’t know what a specialist was, and was getting sort of the same thing. “Well, you’ve got about five years to live, but you’re not sick enough to have treatment.”
I got frustrated and, by good fortune, my general practice doc said that one of the premier specialists in the world was coming to Cincinnati and that he is accepting patients for CLL.
I signed up and was one of his first patients here in Cincinnati. Within five minutes of our first meeting, he said, “Yes, we can start you on treatment right away. And I can say with 95% certainty that we can put you in remission and reset your lifespan to pre-diagnosis limits.”

How to find the right CLL specialist
Michele: Dr. Lamanna, how can anyone find the right specialist? Is there a list? Lisa had one, but this is a long-term relationship. This is probably the person you’re going to be with for the rest of your life so it’s really important that it works.
At what point do you need to bring a CLL specialist onto your medical team? Do you do it just after you were diagnosed? Do you wait until it’s time for treatment? How do you even know?
We want to ask the doctors because we all seem to have our own opinions as patients. This is not meant to take the place of someone’s local hematologist-oncologist who works in conjunction with them.
Dr. Lamanna: You all have already mentioned a couple of areas. One is these online forums, The Leukemia & Lymphoma Society, Patient Power, and the CLL Society. There are lists of CLL specialists in states all across the country so that might provide a starting point, depending on where you live.
You might be restricted because you need to see someone in the area where you live because of your circumstances and so you want to do local. You have to do what fits you. There are people like Lisa who can travel to another state to see a specialist.
Ultimately, your personality and the personality of another physician have to jive, too. Not everybody may jive with a particular person so that’s another layer to add in.

When to see a CLL specialist
Depending on when someone’s initially diagnosed, if you’re not receiving the information so you understand the disease and where you’re at, having that first consultation is very helpful.
If the local physician isn’t spending enough time to explain things because you don’t need treatment and they’re rushing you out the door and saying, “You have a good cancer. You don’t need to see us. You’re great,” that’s not really satisfying to many patients when they’re first diagnosed with any cancer. Sometimes that initial consultation is important.
Another very important time, which Dr. Bachow brought up, is when you’re told you might need therapy. The question is: do you need therapy? What kind of treatment is being recommended? There are new agents and each patient might have a little bit of a different nuance to their disease so that’s really another key point to see a specialist.
Then there are clinical trials. There might be some options that could be really important as well.
Certainly, any time is a good answer, but if you don’t have the ability to do it very frequently, those key time points might be important.

Dr. Bachow: As Dr. Lamanna said, a good time is if you’re at diagnosis and you don’t feel like you’re getting all the information that you need to feel comfortable with the diagnosis.
One time that you really should it’s when you’re going to need treatment, but you can also take it a step further — you don’t want to wait too long.
In some cases for patients with very high-risk disease, their disease can grow exponentially and it may be tough to get in to see a CLL specialist. They’re all so great that they’re booked out weeks and weeks and weeks and they’re doing favors all the time, double-booking patients to bring them in.
I wouldn’t necessarily say just when you’re told that you need treatment. You and your doctor should try to talk together. “Am I more likely to need treatment in the future rather than not need treatment?”
Maybe now’s the time to go get more information, hear what trials are out there, and hear what the treatment landscape looks like now. If the time does come, you’re not rushing to see somebody.
Michele: That’s such an important point, Dr. Bachow. You want to have that established relationship in case it is more of an emergent time.
My CLL relapsed really quickly and I was looking for a second opinion because I was given so many choices. That’s the beauty of research right now. We have so many choices between what’s been approved and what’s in a trial. I didn’t have time to find someone. I had to start treatment the next week.
Thankfully, I had a great relationship and established one with Dr. Lamanna. Knowing you, it’s not like I had to wait months to get to see you so it was wonderful. There can be challenges in getting in to see one.

Patient’s perspective working with a local oncologist & a CLL specialist
Michele: What are the challenges and workarounds of working with different teams in different healthcare systems? Lisa, what did you experience here? You were working with different healthcare systems.
Lisa: The biggest challenge with the first CLL specialist I went to was communication as well as changing doctors when my first doctor suddenly left for a different facility.
My local doctor struggled with getting calls and emails returned. He would voice a little bit of frustration when I would come in for appointments. He hadn’t gotten the information he needed and if I could call and see if I could get things sent. That was the biggest challenge and part of what made me feel I didn’t quite have my right team yet.
One thing I always heard was to go to one of the world-renowned places for leukemia and lymphomas. My local doctor at the time encouraged me because he was also looking forward to having this be a learning experience for him. I went and it was great. They were wonderful.
I don’t have anything bad to say about my experience there other than it wasn’t the right place for me. It was difficult to travel to and I was hearing frustration from my local doctor. When I first went, I didn’t need treatment. After all the testing they did, I was told I’d probably need treatment in about three years and they were absolutely right.
The first doctor I saw was lovely. Shortly after my first appointment, I ended up getting a letter that she was no longer there and had moved to a different facility in California. Then I was on my second doctor so the next time I went, I was meeting a new doctor again.
I started my treatment there. I did my first course then they sent the protocol home so I could finish here. He was frustrated with the lack of communication. It’s a very big, well-known hospital and doctors are busy so he wasn’t getting responses to emails in a timely manner. You can’t expect anything right away.
What was frustrating to me was that he was frustrated. We ended up finishing after three rounds because that treatment didn’t really work well for me.
Dr. Bachow wasn’t my original local doctor. He came into the picture later. Unfortunately, my local doctor passed away unexpectedly so I was left with this situation where now I didn’t have my team.
The first time I ever went to Dr. Lamanna, Dr. Bachow happened to be her fellow. When we met him, we adored him. We thought he was great. We both went to the University of Florida. We knew he was moving back to Florida.
When I was in this position, I called Dr. Lemanna and she said he was in Boca Raton. I was really lucky. He’s just as wonderful. You need to have trust in both your doctors. To me, the biggest thing is communication.
Nowadays, we have telemedicine visits. If you can’t travel as much, it’s really important to try to get in the system with a specialist so that when they are needed, if your disease does accelerate, you’re already in the system.
I can see Dr. Bachow here and if we have questions, if there’s an unknown, or if we’re unsure, I can see Dr. Lamanna via telemedicine visit through Columbia Health. We can send my lab reports.
It’s the communication, the ease of appointments whether you’re traveling or doing virtual, trusting both doctors and the doctors willing to have a shared patient relationship with each other. That’s what I have been fortunate to find, not once but twice and I feel so grateful for that.
Jeff: I would love to tie two thoughts together. You went through a lot in the beginning. You had to deal with different doctors. You had to deal with travel. You had to deal with different levels of comfort. Ultimately, it was your comfort, your ability to mesh well with the doctor as opposed to being abrasive that guided your decisions. That’s really, really important.
We’ve got two doctors who are enthusiastic and their personalities are top of the scale. That doesn’t always happen with every patient relationship. The goal is a long-term relationship so you have to be comfortable with the team that’s taking care of you.

Communication between a local oncologist & CLL specialist
Jeff: How do you coordinate between a local oncologist and a CLL specialist at a distance? This can be a lot of heavy lifting.
Dr. Lamanna: As long as the CLL specialist and the local physician communicate, there are lots of different ways that they can build a relationship. Phone, messaging, and texting are one way of getting records seamlessly. Sometimes via email attachments and faxes.
Remember, different physicians may want to communicate in different fashions, but as long as you can make a connection between the two and they figure out which way works best for them, that’s fine.
Again, as Lisa noted, if there seems to be a struggle, then obviously something’s not working well and that needs to be addressed. You want records and things to be done in a decent time frame, especially if it impacts you.
There are many different varieties to establish that communication given the technology that we have today so it’s not difficult. Technology has gotten better. It’s become easier to communicate so there are a variety of different ways that two physicians and the patient can do that.
Jeff: Dr. Bachow, how do you keep everyone in the loop when everybody’s using different medical record systems? I know we’d like to think that everybody’s on the same page, but that’s not always the case. How do you guide patients? Can you tell us some of your experiences when the platforms don’t sync up quite perfectly?

Dr. Bachow: Office notes and consultations should be faxed back and forth. As Dr. Lamanna said, every doctor is different. The best way of communicating is probably more direct: email and cell phone.
Do the two doctors have a prior relationship together? Do they see each other at national meetings? Luckily, the hematology and CLL world is somewhat small and people do know each other quite a bit. The two doctors having a prior relationship is important but that doesn’t always happen.
You have to recognize that doctors are busy. Discuss with your local hematologist-oncologist what kind of changes would really warrant us reaching out to the CLL specialist sooner rather than later. We’re sending office notes, letting them know the most recent CBC results or physical exam, etc. What kind of changes would warrant us to pick up the phone and call them?
Working with other CLL doctors around the country, I also found that not all of them are like that and that’s okay. Everybody’s extremely busy, but some of them are very busy. They’re running a lab or traveling all the time and getting access to them is not always very easy. Sometimes you do have some important questions for them.
I’ve had an experience where I learned that it doesn’t matter how much you email or if you happen to get their cell phone; I’m just not going to be able to talk to this doctor. But I’ve learned to build relationships with that doctor’s staff — the nurse practitioners, physician assistants, advanced clinic nurses — who have direct access to the CLL specialist and they’ve been able to convey information. I feel comfortable with that and as long as the patient feels comfortable with that, then it turns out to be okay.
Michele: Thank you, doctors, for those answers because that is something we all worry about.
Jeff: One of the bright faces that we have on the support group on Facebook is a young lady by the name of Christy and she’s got a story that she would like to tell.
Christy’s CLL story
Christy V.: Thanks, Jeff. I was diagnosed with CLL in 2017 and that’s when I was referred to an oncologist. From that point, I started considering seeing a CLL specialist based on things that I had seen online from other CLL patients who said that that made a world of difference in their treatment.
Getting pushback from the oncologist
Christy V.: When I asked my oncologist at the time about seeing a CLL specialist, he pushed back a little bit. He seemed to think that it would be fine to proceed with just my local primary oncologist.
I was a little bit concerned about that because I feel that any patient, regardless of their disease or their diagnosis, should be able to seek a second opinion, especially in this case because CLL is a potentially serious diagnosis. Based on what I have been reading in CLL patient forums and support groups, it’s vital to seek the opinion of a CLL specialist.
Finding a new oncologist & a CLL specialist
Christy V.: Based on the hesitancy of my first oncologist to “allow” me to see a CLL specialist, I determined that it was probably better that I find a local oncologist who is a better fit for me and is more open to working with the CLL specialist.
At that point, I found a local oncologist that’s actually closer to me. I also found a CLL specialist within about three hours so that was very helpful. That got me started and feeling a little bit more confident about my diagnosis and that I was going to get good information.
My CLL specialist works very well with my local oncologist. I have some complicating factors with my diagnosis. I have rheumatoid arthritis and it can get a little bit tricky managing both. It was really important for me that my oncologist, my rheumatologist, and my CLL specialist work together to make sure that we are treating both while not harming one or the other.
Finding a CLL specialist
Christy V.: It’s very important to find the right fit for you. Don’t feel intimidated or feel guilty for switching oncologists or deciding that you need to find somebody who you trust. Not only do they need to have the knowledge to treat your disease, but you also have to be able to trust them. For me, that’s really important.
I have to be able to speak to them, feel comfortable speaking with them, and feel comfortable that they are considering my best interests so that’s why I made the switch.
This is a lifelong illness and sometimes people spend more time studying about a new car they’re going to buy than researching the doctor that they have. I did some research and found a CLL specialist that I like and that my oncologist was comfortable working with and that’s worked out very well.

Different opinions among doctors
Michele: What do you do if your two doctors disagree or have differing opinions on the next steps for you? Talk about stress for a patient, right?
Lisa: Honestly, I haven’t had that happen. Should it happen, as the patient, we ultimately have the final say so.
Right now, I have two doctors that I love and trust so much. I would just have to go with my gut and trust in myself. Maybe bring in a third opinion, but sometimes too many cooks… I’d have to see because I have not experienced that.
Jeff: Way back, my first doctor wanted to start treatment immediately and aggressively. My CLL specialist was literally putting up the stop sign and saying, “No. Don’t do that. I helped invent that. It’s old. We’re going to do nothing,” which is a completely different program to talk about.
But, yes, sometimes doctors are going to disagree and like what Lisa said, this is when the patient has to take a deep breath and figure out which voice resonates best with them.
Michele: What do you do when you get two completely different recommendations from two CLL specialists? Dr. Bachow, what happens if doctors have varying opinions about the next steps for approach and care? How can patients and caregivers understand the right way to go? I know this is similar to the last, but it has a little bit of a different nuance.
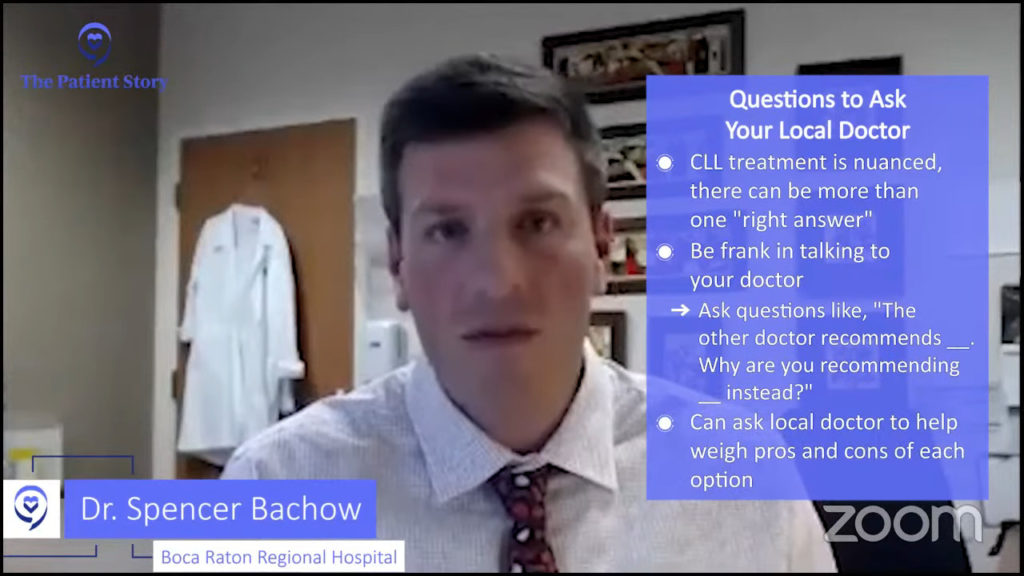
Dr. Bachow: If you’re going to have more than one CLL specialist — and some people get multiple opinions or have multiple people weighing in — there is a good chance that, at some point, there’s going to be a difference in opinion on how you’re treated and that’s not necessarily a bad thing.
The treatment for CLL has become very nuanced and sometimes there’s more than one right answer. If you put yourself in the patient’s shoes, it can be very frustrating and anxiety-provoking.
Speak to each doctor and be frank with them. Say, “I’ve seen other doctors and they’re recommending this. Why would you not recommend that and you’re recommending this instead?”
Something else you can do is if you develop analysis paralysis, if you have so many different opinions and you’re not sure what to do with them, use your local doctor to help bridge them all together. Weigh the pros and cons of each one to help yourself make an informed decision.
It’s a tough situation, but it’s also a fortunate situation in that you have the ability to have multiple opinions from multiple CLL doctors. It can be very frustrating, but it can be managed.
Michele: And local doctors generally see you more so they might know you better.
Dr. Lamanna: It’s very true. There are circumstances when there’s more than one drug that could be totally applied to a particular individual, which is a good thing because it means they have a lot of different therapeutics they can use. There are situations that might be a little different and we have different opinions about that.
Sometimes, there isn’t a particular right answer. But other times, if there’s more than one answer, then from a patient perspective, you’re also looking at other things like side effects of the therapy, social circumstances, and your ability to go to and from the clinic. One therapy might require hospitalization or more frequent monitoring and maybe that doesn’t work with your lifestyle right now.
There’s more than one thing that might also go into choosing an agent. If there’s more than one being offered, the decision will perhaps be more personal and not necessarily due to the specifics of your disease.
There’s no doubt that you can certainly get another opinion but sometimes, that can be a little bit limiting, too, because then it becomes a little bit difficult. As Dr. Bachow noted, that can be challenging sometimes.
When you’re getting five different opinions, then what do you choose? You’re the one who’s faced with that. Usually, it’s not that many differences of opinion, but it does occasionally happen.
Sitting down and talking about the different options with somebody who will be more than willing to go through all those options is important. You can level out the playing field and see where the differences really are and that will help guide you to choose something that works for you.

Hematologist-oncologist vs. CLL specialist
Stephanie: Dr. Bachow, you’re in a different kind of group. You’re really working as a CLL specialist. A lot of the local hematologist-oncologists aren’t. There was a question referencing how long someone’s been a hematologist-oncologist and how close they would be to the research.
Dr. Bachow is young and closer to being a fellow at a time when there was a lot of research happening. There were some differences people were seeing locally, depending on if their local doctor was older and more set in their ways and maybe less open to the idea of clinical trials or new methods. Have either of you heard anything about that before?
Dr. Lamanna: To be honest, the relationship that Dr. Bachow and I have is a unique one so that’s a little unfair. He is closer to somebody who’s a true academic than not. He has access to clinical trials and things like that.
You’re talking about folks that are dealing with hematology-oncologists who also treat lung cancer and other things and one or two CLL folks. There’s no doubt that could be more of a challenge.
What it boils down to is having a good doctor who you can communicate with and who takes good and loving care of you. Then a CLL specialist can guide them in terms of the treatment options and help with the management of certain toxicities and issues with drugs that they need to look out for while they’re treating somebody.
They can have a very good physician who’s willing to talk with somebody, who has more experience treating CLL than they do, and really willing to hear them out.
I’m not expecting them to know the data. Somebody willing to understand certain things that I’m looking for or what they need to pay attention to versus somebody who really doesn’t, who is irritated by me calling, who doesn’t want to hear me, who doesn’t want to hear that I’m a specialist, let alone a female because they’re somebody who’s really stuck in their ways and they don’t want to deal with it, that’s a red flag to me.
Unfortunately, I don’t mind telling the patient that I have a problem with that. It’s up to them to choose whether they want to stay with that physician or not; that’s not my call. But if they don’t want to work with me and I’m trying to help the person, then that tells me that there’s a problem, right?
Sometimes we’ll use a call as a vetting, particularly if it’s somebody I don’t know, that I haven’t worked with before, just to see if they’re somebody that’s willing to work with a specialist if the patient needs it. As somebody who does this all the time, I can get a sense that that person is somebody I can work with.
Jeff: The CLL specialist as champion is very, very important for patients to hear. Patients need to know that they have someone in their corner who’s going to work towards their best care.

Dr. Lamanna: That’s what you want to do. I know that doesn’t always happen in practice. Some of us are more willing to do that than others.
To be fair, I’m sure not every CLL specialist wants to do that either because that’s a lot of extra work. I don’t want to say that all of my colleagues will be willing to do that, but I do think that most of us who love taking care of CLL patients want the best.
When people come and see me, I don’t stress that they need to stay with me, especially if they’re coming from far away. If they have future questions, they can email me. I recognize that they can’t always make that same connection so I’m really there for them and I’m willing to help. Everybody is a little different.
Dr. Bachow: Dr. Lamanna and I have a unique relationship with regard to CLL. I’m in a community setting where I can’t only see CLL patients, but I’ve been able to develop a reputation and build up my practice where I’m only seeing blood cancers for the most part.
For instance, multiple myeloma, which I’ve had to learn. I’ve had to learn how to reach out and find out who is big in the multiple myeloma field and what are some of the new things. Who can I contact to run cases by, especially for patients who have very aggressive managed care plans that can’t go for second opinions? I have a lot of patients that can’t go for a second opinion. Who can I run the cases by?
My perspective really is finding good people to run cases by, not just send patients for a second opinion. Those that can’t go and have an established specialist, at least. Being able to run new situations by them, they can give you advice on them off the cuff.
Dr. Lamanna: That happens, too, where doctors will just call because they know so-and-so treats this cancer or so-and-so treats that cancer and we have those relationships so they’ll email or just call us. We’ll be helping them and we know that their patients aren’t going to be seeing us. We’re just trying to help them because they need advice on a particular case. Many of us do that as well.
Limited options due to HMO restrictions
Jeff: What we’ve been talking about is something that’s actually a luxury. A lot of people have really great insurance that will allow this second opinion, that will allow the consultation with the CLL specialist. And if that doesn’t work, maybe a third, fourth, or, as you said, even a fifth consult.
What happens if you’re in a tightly managed HMO-style program? You’ve been assigned to a hematologist-oncologist at best, but more likely, you’re with a generalist who’s seeing everything from solid tumors to hematology patients.
Barbara, a care partner to her husband who’s had CLL for more than a dozen years, asks, “We are members of a closed healthcare system and are assigned an oncologist. Who needs to be on the CLL team? How do we get them on that team?”
Do you have any words of advice on how to navigate that?
Dr. Lamanna: You might be able to get a free consultation through some of the panels if you’re really strapped and not able to go for a second opinion somewhere due to insurance limitations. There are different ways through different patient advocacy groups to have access to CLL specialists like myself to go over your case for free.
We also take calls from local physicians without having seen a patient because of our relationships with physicians across the country. We’re willing to talk to them and help advise the physician about their patient who’s having issues.
Michele: There are programs to help access a specialist and one that a lot of patients we know have been using is the CLL Society’s Expert Access™, an innovative program offering free consultation to patients, providing them with expert opinions to share with their local treatment team. We urge any patient to consider using this service when they are unsure of their disease status or their treatment plan.
Jeff: It’s a really great program that we recommend quite a lot on social media.

Living your life with CLL
Jeff: When I was first diagnosed, my CLL specialist told me that I wasn’t going to die from this disease, I was going to die with this disease and that was actually very comforting to hear. You hear the word cancer and you immediately think death sentence.
Here we are, more than a decade past that, and I had the opportunity to be with my first CLL specialist again. When he gave me a great big hug, he said, “You’re not going to die from this. You’re not going to die with this. You’re going to die from something else,” and it was really, really cool. That’s been like guidance for me.
Go live your life. Go live a great life. What kind of guidance can you give patients and their caregivers as far as living that great life?
Dr. Bachow: Live your life to the fullest. Stay in close touch with your family. If you’re working, continue to work. If you’re still able to, continue with your usual activities of daily living.
The CLL Society, The Leukemia & Lymphoma Society, and different social media networks are involved with CLL. Reaching out to other CLL patients is very important so you can learn that other people are living their best lives with CLL and you can, too.
Dr. Lamanna: I’ve always taught people that this is a chronic disease. People live with many other medical problems on a daily basis, like diabetes, heart disease, and hypertension. Some people take medications every day for some of their other medical problems.
You need to understand that this is a chronic medical condition, you’re living with this like other medical problems, and you move on. This doesn’t mean that this isn’t an important part of your life, but you need to live your life. This is a chronic condition that you can live with and that we can manage.

Lisa: Live your life. Enjoy. Do things that bring you joy, that relieve your stress levels, and then just be confident in the team you create once you find it and that can be a journey.
I’m lucky I am able to travel to New York, but I’m also lucky that I have Dr. Bachow here. I can honestly say I’ll be seeing more of Dr. Bachow and not necessarily as much of Dr. Lamanna because of the ease, my trust level in him, and knowing that he’s also well on his way to becoming a CLL specialist. How lucky am I? But I love traveling to New York so I’ll check in with Dr. Lamanna.
Find doctors you trust. Trust in yourself. Advocate for yourself, whether it be insurance, your treatment, or whatever comes up in your health care. Do the best you can.
I had two children get engaged four weeks apart so I’ve been planning weddings. In the midst of all that, we’re building our dream home. We just had wedding one, moved into our dream home, and now I’m well into planning bridal shower two, wedding two, and just enjoying all of it.
What I really find amazing is that 11 years ago, I wasn’t sure I’d be able to do these things. I didn’t know I’d be here. How lucky am I that I am? Hopefully, in the next few years, I’ll be able to say, I’m a grandma.
Jeff: Outstanding. That is the stuff that I love to hear. People aren’t just saying words, not just parroting things. They’re having those moments. Lisa, I am so glad that you are living well. I remember meeting you in that waiting room and it seems like a world away, but so much has changed for the better.
Lisa: We all are.
Jeff: We’re doing that and it’s a great story to tell.
Lisa: And through this pandemic. It was scary for us to get through these last few years and still is. We’re doing it.
Jeff: We’ve got hope for a cure for some of us. We’ve got great treatment programs. We can do this.

Conclusion
Jeff: We honestly hope that each of you has taken away useful tips, some clarity, and guidance on how to build a great CLL team and how to work with different physicians on your team. It makes a big impact.
We are so glad that you joined us today and we hope that you’ll look for more programs with more content.
Stephanie: Thank you to all who participated. It was really amazing to hear what everybody had to say.
Doctors Lamanna and Bachow, thank you so much for your time and your dedication to patients and their families. Lisa, hearing about all that you’ve been able to do; really appreciate you sharing your story. And, of course, Michele and Jeff, always a pleasure to work with you, and excited about more collaborations.
When you get the chance, don’t forget to sign up for our newsletter list so you don’t miss any of the content and the latest in these programs. Wishing you all the very best and really hope to see you at our next program and discussion. Thank you!








Leave a Reply