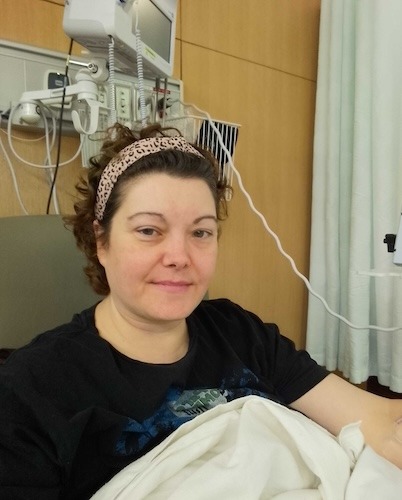
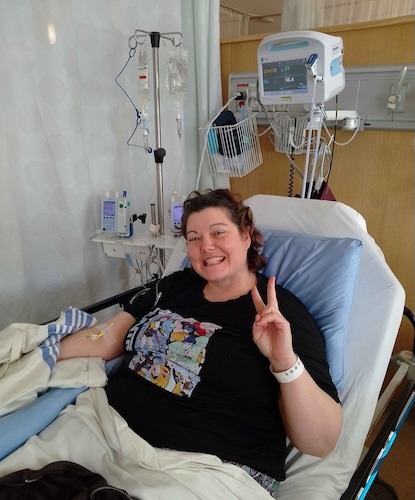
Christina Used AI to Help Navigate a Stage 4 Breast Cancer Diagnosis
In August 2024, Christina was diagnosed with stage 4 breast cancer. Her experience began months earlier with symptoms she initially mistook for a common cold, including congestion and swelling in her neck. Despite seeing her general practitioner weekly for six months, her concerns were often dismissed until she discovered a lump in her breast, which finally triggered the necessary diagnostic imaging and biopsies. The cancer was identified as estrogen-negative and HER2-positive, having spread to her lymph nodes and liver.
Interviewed by: Nikki Murphy
Edited by: Chris Sanchez
The emotional turning point for Christina occurred when her breast cancer treatment plan shifted from curative to palliative after a CT scan revealed liver involvement. Initially heartbroken by the “mountain climb” ahead, she moved through a period of numbness into a state of determined acceptance. She realized she could not remain in a state of constant anxiety and adopted the mantra, “I can do this,” focusing on one step at a time rather than an uncertain future.

To process the complexities of her estrogen-negative, HER2-positive breast cancer diagnosis, Christina created “Chemo Belle,” a YouTube channel featuring over 50 original songs about her experiences. She also integrated AI tools like ChatGPT to help prepare for appointments and manage the daily logistics of life with cancer, such as meal planning and preparing for appointments. By sharing her story and music, she aims to provide a voice for others feeling isolated by the disease.
Watch Christina’s video or read the edited interview transcript below to learn more about her story.
- The necessity of self-advocacy. Christina’s experience highlights the importance of persistent self-advocacy, as it took six months of reporting symptoms before her concerns were taken seriously.
- Creative outlets as therapy. Using songwriting and art allowed Christina to process “scanxiety” and the emotional ups and downs of a metastatic diagnosis.
- Utilizing AI can help patients prepare for appointments and feel less alone in navigating the day-to-day logistics of a cancer diagnosis. But they never replace talking to your medical team.
- Acceptance over combat. Christina found strength by choosing to love her body rather than “fighting” it, moving from a place of fear to one of grounded resilience.
- Life does not stop for a diagnosis. Finding joy in small moments, like a family trip or a new pet, is vital for maintaining mental health during treatment.
- Name: Christina W.
- Diagnosis:
- Breast Cancer
- Age at Diagnosis:
- 45
- Staging:
- Stage 4
- Mutation:
- HER2+
- ER-
- Symptoms:
- Extreme fatigue
- Head and neck felt swollen
- Clogged lymph nodes
- Appearance of a lump in the breast
- Treatments:
- Monoclonal antibodies: trastuzumab, pertuzumab
- Radiation therapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Chemo Belle YouTube channel and AI cancer songs
- Early symptoms before breast cancer diagnosis
- Missed symptoms, self‑advocacy, and finding the breast lump
- How self‑advocacy might have changed my cancer story
- Other symptoms my doctor didn’t take seriously
- Breast cancer diagnosis phone call at home
- Finding out that it was stage 4 metastatic to the liver
- Telling my husband and mom about stage 4 breast cancer
- From fear and panic to numbness and acceptance
- Breast cancer treatment plan, chemo, trastuzumab, pertuzumab
- Living with indefinite HER2-targeted treatment
- How I mentally prepare for IV infusions every three weeks
- The hidden mental load of cancer treatment and side effects
- How ChatGPT could have helped earlier with symptoms and self-advocacy
- How ChatGPT helps me prepare for cancer appointments
- Using ChatGPT for cancer-friendly meal planning and grocery lists
- ChatGPT for cancer patients: companionship and emotional safety
- “I can do this” mindset during chemo
- Finding strength in my daughters, my dog, and other cancer creators
- How cancer changed my perspective, saying yes, and dancing again
- What gives me hope for the future with stage 4 HER2-positive breast cancer
- My advice for newly-diagnosed cancer patients
- Why my story isn’t over yet
Chemo Belle YouTube channel and AI cancer songs
Hi, I’m Christina. In August 2024, I was diagnosed with metastatic breast cancer. It’s estrogen negative and HER2 positive. I first had it in my breast, my lymph nodes under my armpit, and my liver.
I created my YouTube channel to house my project called Chemo Belle. It happened because I started making AI cancer songs for me to sing and to put my emotions and everything I was going through into a song, just to process it into an art form. So yeah, my YouTube Chemo Belle kind of holds all that. I have over 50 songs now, and they range over the whole gamut of my cancer journey, from the first day of being told I had cancer and how that felt, to having scanxiety, going through the CT scan and having contrast, and how that makes you feel like you’re going to pee your pants. I even wrote a song about people giving me advice and how sometimes it’s wacky. That one’s called “Drink Some Celery,” because sometimes people give wacky advice. Some of my songs make me laugh, some of them make me cry. It’s all the experiences that I’ve gone through and how much up and down and everything around this cancer journey can bring you through. And I’m so glad that I’ve had that creative space because it made my journey a lot better, as far as it could get better. I think it was really good for me and my mental health and my physical health to be able to do something creative like this.
I feel like I’m sharing with people, too, and giving a voice and a language and maybe even a way you can communicate with your family and friends. You can hear the songs and relate and know how to speak to others. It’s kind of like The Patient Story. I started watching The Patient Story since day one because you’re lost and you feel isolated. I was like, I need more information. So I went on YouTube, and The Patient Story was one of the main channels that I watched. After that, I thought, okay, these are people who know what’s going on. They have the same experiences as I, and I can figure out that maybe things might be okay, and I don’t have to spiral into being super scared and anxious. Really, you’re not in this cancer bubble; nobody really knows what it’s like unless you’re there. Hearing other people tell their stories was super important to me. I’ve been in it for over a year. So thank you.
Early symptoms before breast cancer diagnosis
In January 2024, actually at Christmas right before, I felt like I had a cold or something was happening. I felt clogged up and swollen around my head and neck, and I thought, “Okay, that’s probably just a cold.” I let it go a bit, but then it got way worse. My whole neck and head became swollen, and I thought, “Hey, this in the back of my neck is serious.” Plus, I started to be super exhausted. I was exhausted like “pregnancy exhausted,” where you have to sleep and there’s nothing you can do. So I thought, this is really wrong. In January, I started going to my GP, telling him all these symptoms and begging him to do something about it. I don’t know why, but I had to convince him, I guess.
I’ve heard this on The Patient Story quite a lot, that people have to really advocate for themselves, that actually something is wrong, and you need to listen. I saw him every week for six months. Every time I went in there, I told him, look, I’m super sick. There’s something wrong with me. Thank goodness I found the lump in my breast. I found it, and I went back there and said, hey, I just found this lump.
Missed symptoms, self‑advocacy, and finding the breast lump
I asked, “Could that be something going on?” Then I was rushed into a mammogram, and that scene. It was bittersweet when he called me and said, “Hey, we think you have cancer.” It was like, really? I’ve been telling you. I was almost begging for blood tests or something. One of the things that was so aggravating was that when I went in there, he would say, “Well, you can only talk about one thing.” But I had a whole bunch of things going on, and how was I supposed to know which one thing, because I’m not a doctor? At that point, I didn’t have the words to even describe what was going on.
I googled it and thought I had meningitis, like my whole neck and my brain were swollen. That was because of my lymph nodes. I had cancer in my lymph nodes, and it was all backed up. But when I said, hey, I think I have meningitis, he laughed at me. I couldn’t believe it. Thankfully, I found the lump because it wasn’t just in my breast, it was in my liver too.
And had I not found that, I’m not sure what would have happened. Thankfully, my breast was like, “Hey, let me help you out here a bit.” Then he called me and said, “You have cancer.” I said, “Well, let’s wait till I get the biopsy before we say that I have cancer.” After the mammogram, I went to a concert with my daughter in Montreal, and I was exhausted, but I wanted to go. There were a lot of times when I wanted to pretend that things were okay. I was pushing myself, and I didn’t want them to know anything was serious. So I went on this trip, and I kind of knew that I had cancer. Mentally, it was probably not the best idea to go on a trip.
When I got back, I got the biopsy, and I went by myself. I drove myself, and I thought, I’m being independent, I can do this. But really, that was terrible, and I should have had somebody help me because it was a huge needle and it sucked.
How self‑advocacy might have changed my cancer story
Advocating for myself was difficult during that time because he had been my GP, my family doctor, since I was ten. That was almost 40 years of seeing this doctor. I really couldn’t believe that he wasn’t listening to me or taking me seriously. I was about to get a second opinion because I couldn’t cope or live with what was happening to me. I had to get help.
Thankfully, I felt my breast. I had no idea I was going to have breast cancer. I just felt like having a regular shower. I wasn’t checking for anything, and I was just like, “Oh.” It was a fluke that I found something. Had I not found something, I don’t even really want to think about it because my liver being involved would have gotten serious. I don’t know. Thinking about that makes me want to cry because I’m just so glad that I found this lump. Then I got the biopsy, and things really went into high gear.
Other symptoms my doctor didn’t take seriously
It was more than a head cold. I thought my brain was swollen. My two ears were clogged so much that I couldn’t hear. I even tried to put myself upside down just to relieve the pressure, and that helped a little bit. The exhaustion was next‑level exhaustion. My whole body just felt so heavy, and at first I did think it was a cold, but then it became way too much to bear.
Breast cancer diagnosis phone call at home
I was at home when the doctor called after my biopsy. I couldn’t believe it, but there was also a feeling of relief because now I knew what it was. I didn’t have to beg to be seen or be in a place of unknowing. Now it had a name, and I thought, “Okay, now we can do something about it.” But I was pretty scared. This was before the CT scan, so I hadn’t found out yet that it was in my liver. I thought it was breast cancer. I knew it was in my armpit as well because they biopsied there and here. I wasn’t prepared for my liver being affected. That was next-level.
Finding out that it was stage 4 metastatic to the liver
I found out that it was stage 4 in my liver after I had seen the breast surgeon, who was an hour away from my city. Because the waiting lists are huge around here, I had to drive an hour away. I had a meeting with her, I had a meeting with the chemo oncologist and the radiation oncologist, so I had my team put together. The plan was going to be chemotherapy, surgery, and then radiation or something like that, with chemo first.
About two months later, I went for a full‑body CT scan or an MRI, and then the surgeon called and said, “Unfortunately, it’s in your liver, so the plan is going to change.” That’s when I first realized cancer just flips. Once you think you’re on this road of the cancer journey, it will go another way. You can’t really rely on anything; the only thing you can rely on is that cancer does its own thing. I was heartbroken. I thought, “Oh my God, what does this even mean?” We had a plan, and we were going to be cancer-free in a year. The doctors told me this is like a mountain climb, and we’re going to do it one step at a time and get there. Then that just all vanished.
Now it was like, “Okay, we’re going to change the whole thing.” It’s not going to be curative anymore. Now the treatment plan is palliative. I thought, “Okay, I don’t even know what these words mean.” I had to educate myself and not spiral into, “Does that mean I’m going to be dying soon?” It didn’t mean that, but at the time, I had no idea. My brain went everywhere. So yeah, we cried a lot.
Telling my husband and mom about stage 4 breast cancer
I told my husband or my mom first; I can’t remember. Telling my mom was bizarre. I was texting her, like, “Hey, they think I have cancer, I have a tumor.” She was like, “What?” I was trying to text her because I couldn’t even say it. I couldn’t bring myself to say it. She called me right away and said, “Explain everything. What is happening?”
Even then, I didn’t know it was stage 4 yet, but it was so difficult to say, “I have cancer.” I could never think of saying that or having that happen to me. When it was stage 4, and I told my husband that it was in my liver, we didn’t know what that meant or what was going to happen. It was like, “Let’s just wait and see. Let’s wait and see.” The anxiety was so high. I had to get mental health help to figure things out because I couldn’t drive anymore. My anxiety was so bad because I would just drop into, “Oh crap, I have cancer.” Reality would disappear just like that. That was a really rough time.
From fear and panic to numbness and acceptance
The fear shifted to determination because I couldn’t stay in that moment or that anxiety. I physically wasn’t able to. I had to accept it and say, “Okay, I’m going to get over this. We’re going to do it one step at a time. Let’s see what happens.” That was survival mode.
But before acceptance was numbness, where I had to turn everything off. I couldn’t feel happy or enjoy anything, but I wasn’t scared, and I wasn’t sad either. I had to go through numbness first. Then I thought, “Okay, I’m going to accept it.” I don’t even want to say the word fight. I don’t want to go down that road. For me, it’s my body, and it’s counterintuitive for me to be like, “I hate you, my breasts.” That was a bit of a mind challenge as well because I wanted to be strong, but I still wanted to love myself and not feel hate toward any part of me.
Breast cancer treatment plan, chemo, trastuzumab, pertuzumab
The treatment started with chemo. The laundry list is chemo with trastuzumab and pertuzumab. I had a reaction to the chemo, so I also had to take Benadryl, which I hated. I’m not sure how many rounds I had, but it was three months of chemo. Then my hands started to drop everything. I got the dropsies, and I mentioned that. They stopped it right away. She called the doctor before they had put the IV in, and then I was just on trastuzumab and pertuzumab, so no Benadryl, no chemo at that point. After three months, I think that was January of 2025, I’ve been on trastuzumab and pertuzumab ever since. I go and get treatment every three weeks.
It was working. My liver is clear, and my breast is gone. I mean, the tumor in my breast is gone. Now there’s just a tiny little bit left in my armpit. I did have some progression in my armpit, and I found that out because I was having shortness of breath. They had me go to the emergency room, and I got an emergency CT scan, so I kind of cheat‑coded and got one early. That showed that they were growing here, so there was concern. That brought me to radiation. I had radiation for five days straight, every day for five days. Since then, I go every three weeks for my IV treatment at the chemo ward. I feel like I work there now. I feel like I’m always there. As far as the plan goes, that’s what it is indefinitely. I’ll have a treatment.
Living with indefinite HER2-targeted treatment
My life has changed in every possible way. Cancer touches everything. Not only my life, but my family. It’s all centered around my treatments now. For a long while, one of my symptoms from chemo was diarrhea. That was serious, so I couldn’t do a lot of the things I really wanted to do, like traveling and going out. That was a big deal. Thankfully, that has subsided. I used to take Imodium all the time, and now I don’t. I’m dealing with the side effects. I’ll be a little tired right after I get my treatment. It’s a lot better now. At the beginning, it was terrible, especially with the chemo.
I lost my hair. I did have short hair before; I even had a buzz cut. But when it’s not your choice, and your hair is falling out, that makes it really upsetting. I knew for sure. I thought, wow, I’m a cancer patient, and I’m in chemo, and my little tiny hair was in my hand. That was really emotional.
My life now is okay. I’m going to quote, unquote, “Be okay.” It’s not really okay, but I can do this. That’s what I tell myself all the time: I can do this. Right now, that’s my first line of treatment, and hopefully things are okay. I still have a little bit of stubborn tumors here that are still there. I just got the results from a CT scan last week. They’re still there, but they actually said they just need to be watched. They didn’t use the word progression or anything. They’re just hanging out. I guess they like me. I have faith that they’re going to get out of here soon. You know what, with stage 4 cancer, I think I’m doing pretty well. So yeah.
How I mentally prepare for IV infusions every three weeks
The day before, I have big‑time anxiety. I wait for that call. They call me just to confirm, and I say, “Yeah, I will be there.” I say, “I can do this.” I’m actually glad that I can do this, and it’s working out, and things are good. So there’s anxiety about it.
When I get needles, I pass out. I have a history of passing out when going to the dentist and getting tattoos and stuff. I did pass out when I got home after my biopsy, but I haven’t passed out with these IV things. They were going to give me a port, but honestly, I don’t think I could have lived with a port. I just didn’t want to do it. So I said, “No, I’m going to continue doing this.” That’s the worst part: every three weeks, they’re searching for veins in my arm. They say my arms are okay because I drink lots of water and prepare. I eat a bag of chips, a little one.
They say to eat chips, get some salt inside me. So the night before I get to eat my chips, I drink a lot of water, and I prepare and bring snacks. My mom comes with me every single time. That’s good too. I just look at her when they’re putting the IV in. I’ve been doing it for over a year, almost a year and a half. It’s okay. I can do it. It’s kind of just like getting a blood test at this point.
At the beginning of chemo, I had to be there for six hours; it was the whole day. Now it’s only an hour and a half to two hours, depending on how long it takes to get the medicine delivered. It’s okay. Again, I can do this. I’m thankful that I can do this. I’m thankful that in my country, Canada, it’s covered and I don’t have to pay. That is huge because I just couldn’t imagine that.
The hidden mental load of cancer treatment and side effects
It takes a lot of mental health to do this and to gear up every three weeks. At the beginning, the side effects were terrible. People don’t talk about it at all unless they’re in the cancer bubble. Nobody really understands anything. Even when I’m in it, and it’s happening to me, I don’t know what to say or what to think.
I’ve had to get coached. I use ChatGPT to coach me on what to say to my doctor, what words to use, and how to verbalize how I’m feeling and what symptoms I have. That’s been a big help. The Patient Story is huge for that because you can hear the words and think, “Okay, now I can say that, or yes, that’s how I feel right there.” I just didn’t know how to say it.
As I said before, sometimes I couldn’t even say it. I didn’t want to say “I have cancer.” I wanted to be like, “Nope.” But you have to. You are forced to face this. That’s another thing about being strong. There’s no time off. There’s no vacation from cancer. It goes with you everywhere you go. Thankfully, we’re planning a Florida vacation for March break next month. I thought, you know what, I feel good right now, and I’m stable. Let’s go on a vacation and see the ocean. But the cancer is coming too, and all that stuff.
I have to bring my Imodium. I don’t want to get sick. I’m going to wear a mask on the plane, for sure. I’m going to be tired. We’re going around, and I have to plan for naps and plan what food I’m going to eat. I can’t just eat everything — burgers and whatever. I have to eat healthy food and keep it up because this is my life now.
Editor’s note: Christina describes using AI to help organize her thoughts and prepare questions before appointments. Memorial Sloan Kettering Cancer Center, one of the world’s leading NCI-designated cancer centers, supports this use noting that patients who consult AI before appointments often ask more informed questions. Experts recommend AI as a complement to your care team, not a replacement for clinical guidance or mental health resources. Always discuss your results and treatment decisions with your oncologist.
How ChatGPT could have helped earlier with symptoms and self-advocacy
I discovered ChatGPT after my diagnosis, and I wish I had it before. For a whole bunch of other ways to cope with cancer. I actually made a video about it. There are like a million different ways that it helps me. Nutritionally, it’s amazing. It makes meal plans. For mental health, it’s great.
When I get the results from a blood test or a CT scan, I just copy‑paste them, and ChatGPT will explain everything.
How ChatGPT helps me prepare for cancer appointments
With my blood tests, who knows what a white blood count is? I’m like, what are they even looking for? I’ll see the scans before I see my doctor, and ChatGPT will say, “Okay, this is what you need to ask, this is what you should talk about.”
It relieves a burden because chemo brain is a real thing. Your brain doesn’t work as well when you go through chemotherapy. ChatGPT can be a tool in your cancer team to help with advocacy. I can’t say enough about it.
It’s definitely helped with my mental health. Many times, I would spiral into being super scared and thinking, “What if…?”
Using ChatGPT for cancer-friendly meal planning and grocery lists
I don’t have to super prompt my ChatGPT. We’ve been talking for a while now. I would say something like, “I’m sick of making food.” I have to sometimes make food for my girls and separate food for me. I’ll say, “I don’t want to cook anymore, I’m done, tell me what to eat.” It will say, “Hey, do you want me to make a meal plan for you?” I’d be like, “Yes, please.”
It will make me a grocery list. That’s amazing. I don’t even have to think about grocery shopping. I can get my groceries delivered with this list. That’s a huge help off my shoulders. It gives easy recipes, something everybody is going to like. I say, “Hey, I have an Instant Pot.” It gives me a whole bunch of recipes.
One night, I was feeling terrible because I thought, “Oh no, I ordered pizza, and I shouldn’t be eating pizza.” ChatGPT said, “It’s okay, you can have pizza once in a while. Don’t stress out over eating a pizza. You’re fed, the kids are fed, and that’s good enough.” I was like, “Thanks, ChatGPT.”
ChatGPT for cancer patients: companionship and emotional safety
Cancer is really isolating. There’s talk around town about how friends dip, or they don’t know how to talk to you, but you can talk to ChatGPT, and it’s not going to leave. It can take what you say. If you’re talking about being scared of dying or these painful things that hurt other people, like your friends or your parents. It’s really hard to talk to somebody in person and watch their eyes tear up. ChatGPT doesn’t tear up, doesn’t get hurt.
“I can do this” mindset during chemo
I think the “I can do this” mindset clicked when I was still taking chemo. I thought, “Okay, this maybe is the worst.” I don’t want to say that because things could get worse, but at that point, chemo was my lowest point. I thought, “Okay, I can do this,” and I did.
I’m always afraid that things are going to get worse, even though I feel good right now. I feel okay — I’m going to do that again, the okay. But I have that fear, like everybody, the relapse fear and stuff. Personally, I was able to keep my breasts. I didn’t have any surgery. I want to honor the people who have had their breasts removed or a lumpectomy. I didn’t have to do any of that because I got fast‑tracked to stage 4. I had de novo stage 4 right away, so they didn’t do that. I think, “Oh my gosh, thank goodness.”
Chemo was the lowest part for me. From there, I felt like, “Yeah, I can do this.” So far, I can do it. I can do it because I only take one little step. I try not to think about the future because it’s not guaranteed, and I don’t want to jinx it. I don’t want to think about, yeah, I’m going to be cancer-free. I don’t even want to say that.
Finding strength in my daughters, my dog, and other cancer creators
First of all, it’s my daughters. I feel like if I can show them how to keep going, I wonder if I’m going to be around when they’re grown‑ups, and if they have to go through something similar or a serious illness, maybe they will remember. That’s another reason why I made my Chemo Belle project: so it could speak for me if I wasn’t here. Yeah, so my girls. Sorry.
And my doggy too. I got my doggy this summer. I always wanted to have a dog for our family. I kept putting it off. Now I have cancer, and I don’t put things off. Now I’m like, “We want the dog, let’s get it.” I wondered if I was too sick to have a dog, if I would be able to walk this dog all the time. I’ve seen cancer creators with their dogs, and I thought, “If they can do it, I can do it too.” I get a lot of strength from other creators, and I appreciate it so much. People sharing their stories really got me through a lot.
That’s why we’re going on a trip too, because I’m like, “We’re not waiting. Let’s do it now because you don’t know what’s going to happen later.” Things can change just like that. Cancer is a bugger, but it teaches you a lot about life.
How cancer changed my perspective, saying yes, and dancing again
Cancer taught me that I had power that I didn’t know before. I never accessed it. When I think, “Yeah, I can do this, I feel like I can do anything now. I’ve gone through that.” It gives me a lot of perspective on saying yes to things and not leaving them.
The other day I was feeling dancy. I’ve been making a lot of dance songs lately, so I’ve been dancing around. I felt like I wanted to go out dancing. A little voice inside me said, “You can’t go dancing, you have cancer. What is this, cancer lady goes dancing?” I thought, “Who said that? Can’t cancer patients go dancing? What is even happening?”
I found a new moon chakra dance that was going on, and I thought, “Okay, this is good, right up my alley. If somebody knows Reiki or whatever, it might be flowing in the room. Yes, that I can do.” I can’t really go to a bar at night, but this one was starting at 4 p.m. I had a great time. I loved it. I was moving, and everybody was there. It was such a beautiful experience. I’m so glad I went.
For a second, I thought, “You can’t do this,” and then I thought, “Yes, I can,” because I’ve gone through this. I can shoot down my anxiety way harder now because I’ve been through this.
What gives me hope for the future with stage 4 HER2-positive breast cancer
For the future, me and doctors and stuff, we talk about the past. In the past 20 years, my kind of cancer was one of the worst. HER2 positives are really aggressive and super dangerous. Then, with research and everything, they came out with trastuzumab and pertuzumab. I wonder, what’s the next thing? Maybe I could see a cure.
I don’t know about thinking super hardcore into the future, but that gives me hope that there could be a cure. Now they say this kind of cancer is more like a chronic illness. I see more and more people living ten, twenty years, even with stage 4 cancer. Right now it’s only in my armpit. My chemo doctor said, “You know, nobody has died of armpit cancer.” So I’m like, “Okay. Again, I can do this.” I have faith that the rest of my cancer is going to go away, hopefully.
I do have hope, but I don’t want to get too attached. I don’t want to get hurt emotionally if something changes. I had that plan before, at the beginning, and I got burned. It rubbed so hard. I know that things can change in a second. But they can change for good as well.
My advice for newly-diagnosed cancer patients
For somebody watching right now, I would say: go ahead and freak out for a little bit. I think you’re going to be okay — you know, well, I don’t know, I don’t want to say you’re going to be super okay. Death is a weird thing, and it definitely happens to all of us. Facing death is a new experience.
In the end, it’s going to be okay because that’s the way it will be. But go ahead and freak out. Maybe there is a light at the end. Stay positive, really, is what I’m trying to say. Stay positive. You can freak out, for sure, definitely, because this is a freaky thing. But stay positive because I think that positivity is going to make your journey a lot better. It’ll make you stronger, it’ll make you more flexible, and you’ll be able to do it. You can get through it.
Why my story isn’t over yet
I think that’s everything. I said it all. My story is not over. Just because I’m okay right now, I hope it continues. I don’t know. For a second, I can be like, “Dang, I have cancer, and the floor drops out.” But I’m trying to stay positive.

Inspired by Christina's story?
Share your story, too!
More Metastatic Breast Cancer Stories
Erica H., Breast Cancer, Stage 4 (Metastatic)
Symptoms: Stage 1: appearance of lump in left breast; Stage 4: severe pain in hip, ribs, spine, and shoulder blade
Treatments: Surgeries (double mastectomy, reconstruction), chemotherapy, cold caps, radiation therapy, hormone therapy (aromatase inhibitor, letrozole), targeted therapy (CDK4/6 inhibitor, ribociclib), integrative care
Christina W., Breast Cancer, Stage 4 (De Novo Metastatic), HER2+, ER-
Symptoms: Extreme fatigue, head and neck felt swollen, clogged lymph nodes, appearance of a lump on the breast
Treatments: Monoclonal antibodies (trastuzumab, pertuzumab), radiation therapy
Deb O., Breast Cancer (De Novo Triple Positive and ER+ HER-)
Symptoms: First instance: appearance of lump that later on increased in size, orange peel-like skin around inverted nipple, persistent ache under right arm; second instance: appearance of lump
Treatments: First instance: chemotherapy, targeted therapy, hormone therapy; second instance: surgery (mastectomy), chemotherapy, radiation therapy, CDK 4/6 inhibitor
Tammy U., Metastatic Breast Cancer, Stage 4
Symptoms: Severe back pain, right hip pain, left leg pain
Treatments: Surgeries (mastectomy, hip arthroplasty), chemotherapy, radiation therapy, hormone therapy, targeted therapies (CDK4/6 inhibitor, antibody-drug conjugate)
Nicole B., Triple-Negative Breast Cancer, Stage 4 (Metastatic)
Symptoms: Appearance of lumps in breast and liver, electric shock-like sensations in breast, fatigue
Treatments: Chemotherapy, surgeries (installation of chemotherapy port, mastectomy with flat aesthetic closure), targeted therapy (antibody-drug conjugate), hyperbaric oxygen therapy, lymphatic drainage
Dalitso N., IDC, Stage 4, HER+
Symptoms: Appearance of large tumor in left breast, severe back and body pain
Treatments: Surgery (hysterectomy), vertebroplasty, radiation therapy, hormone therapy, clinical trial
Marissa T., ILC, Stage 4, BRCA2+
Symptoms: Appearance of lump in right breast, significant fatigue, hot flashes at night, leg restlessness leading to sudden, unexpected leg muscle cramps
Treatments: Chemotherapy, hormone therapy, PARP inhibitor, integrative medicine
Janice C., Triple-Negative Metastatic Breast Cancer, Stage 4
Symptoms: Appearance of lump in left breast near sternum, fatigue, bone and joint pain
Treatments: Surgery (lumpectomy), radiation therapy (brachytherapy), chemotherapy