The Power of Personalized Medicine: Biomarker Testing Guided Maggie in Her Stage 4 Lung Cancer
Interviewed by: Taylor Scheib
Edited by: Katrina Villareal
In May 2021, Maggie celebrated her 60th birthday with a profound sense of optimism, believing it would be the best year of her life. However, a series of peculiar symptoms — including ocular migraines, a blood clot in her leg, and vision problems — soon derailed those plans. Following a misread EKG and a persistent cardiologist appointment, a CT scan eventually revealed stage 4 non-small cell lung cancer (NSCLC) with metastases in the brain. Despite the devastating news, Maggie’s narrative shifted from a fear of immediate decline to a focus on scientific advancement when a blood biopsy identified an EGFR mutation.

The emotional turning point of Maggie’s experience occurred when she realized that cancer treatment is not one size fits all. Initially expecting the carpet-bombing approach of traditional chemotherapy, she was instead prescribed a targeted therapy pill that led to no evidence of disease (NED) within just two months. This revelation transformed her from an overwhelmed patient into a dedicated advocate who views her scans as vital information rather than sources of terror.
Over the last four and a half years, Maggie has navigated five lines of treatment, utilizing repeated biomarker testing to identify new resistance mutations like MET amplification and MET overexpression. Her experience highlights the critical role of genomic testing in accessing cutting-edge therapies, some of which were FDA-approved only a year ago.
Today, Maggie remains focused on the blue sky behind the clouds, using her voice to humanize the statistics for drug companies and providing peer support to those newly diagnosed.
Watch Maggie’s video or read the interview transcript below to know more about her story:
- Biomarker testing is the gold standard for personalized care: Maggie emphasizes that next-generation sequencing (NGS) and tissue biopsies are essential for identifying specific mutations that can be treated with missile-like targeted therapies rather than broad chemotherapy
- Persistence in the diagnostic process can be life-saving: Despite being told her heart rhythm was normal and she didn’t need a cardiologist, Maggie kept her appointment, which led to the CT scan that finally caught her cancer
- Research is the foundation of hope: Maggie views medical research as the engine that provides new treatment options, noting she is currently on drugs that did not exist when she was first diagnosed
- Scans are information, not just a source of anxiety: By reframing scanxiety as a tool for data collection, Maggie feels more empowered to collaborate with her oncology team on next steps
- Community is a vital resource for navigating side effects: Joining mutation-specific groups like EGFR Resisters and MET Crusaders allowed Maggie to exchange practical advice on managing treatment-specific issues like skin conditions or edema
- Even in the face of a terminal diagnosis, it is possible to find a life that is more fulfilled and grounded in gratitude than it was before the illness
- Name: Maggie M.
- Age at Diagnosis:
- 60
- Diagnosis:
- Non-Small Cell Lung Cancer (NSCLC)
- Staging:
- Stage 4
- Mutations/Biomarkers:
- EGFR mutation
- MET amplification
- MET overexpression
- Symptoms:
- Ocular migraines (kaleidoscope vision)
- Partial blood clot (DVT) in the leg
- Vision and balance problems
- Minor chest pain
- Treatments:
- Targeted therapy: tyrosine kinase inhibitors (TKIs)
- Radiation therapy: stereotactic body radiotherapy (SBRT)
- Clinical trials
- Chemotherapy: combined platinum-based regimen


Thank you to AbbVie for their support of our independent patient education program. The Patient Story retains full editorial control over all content.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Living fully with stage 4 lung cancer
- Passions, purpose, and the healing power of cats
- Why advocacy became a core part of my cancer journey
- From birthday optimism to a shocking stage 4 lung cancer diagnosis
- Learning about my EGFR mutation and that lung cancer isn’t one-size-fits-all
- The emotional whiplash of a cancer diagnosis
- My treatment journey through five lines of therapy
- Why biomarker testing is critical for every lung cancer patient
- How lung cancer communities and mutation-specific support groups change everything
- What I learned about biomarkers and personalized medicine
- How shared treatment decision-making can transform your care
- How advocacy, research, and letting go sustain me through stage 4 lung cancer
- Living fully with stage 4 lung cancer through gratitude and reframing
- Why every lung cancer patient should consider clinical trials as an option
- Starting a fifth line of treatment and preparing emotionally for a new drug and renewed hope
- My advice for patients who don’t know about biomarker testing
- What hope means to me
- My message of hope for anyone feeling hopeless
- Gratitude, oncologists, and a life without an expiration date
Living fully with stage 4 lung cancer
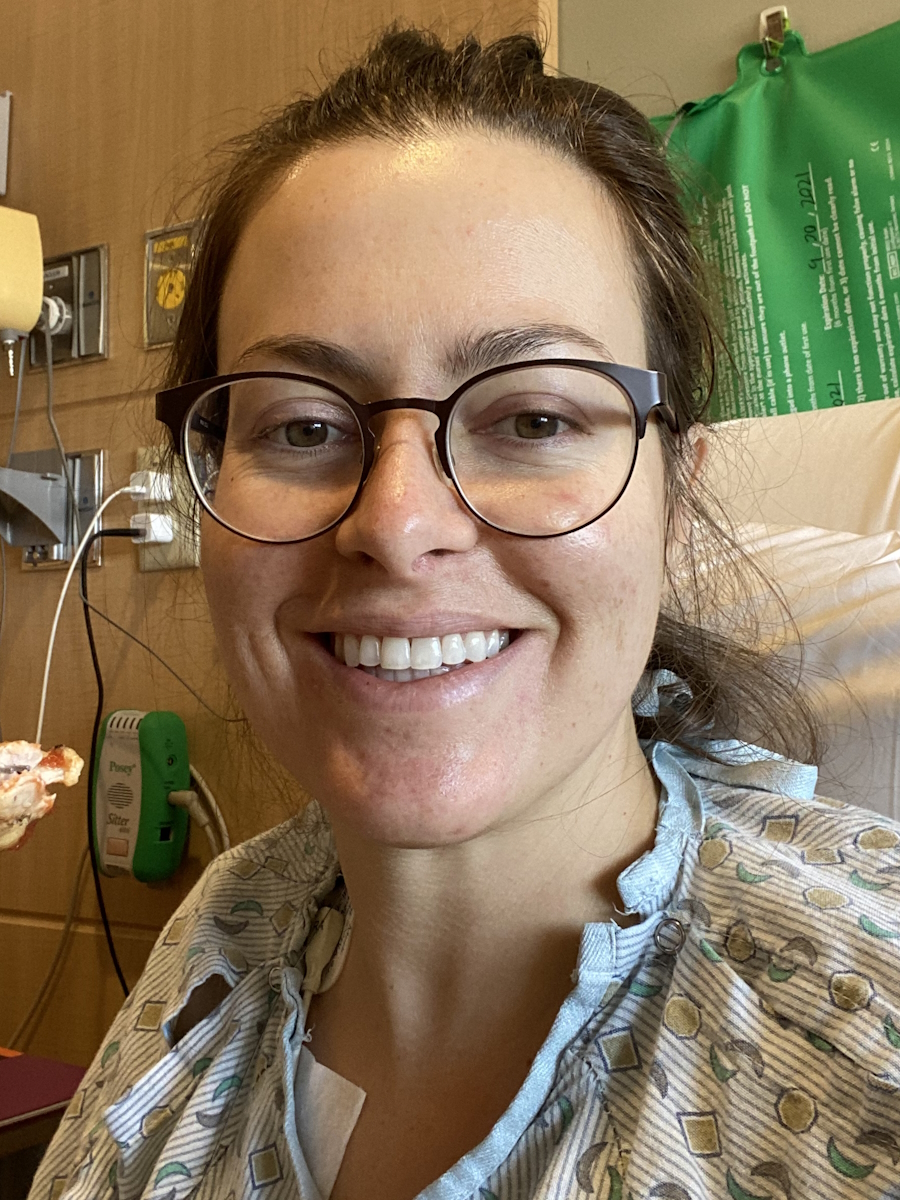
Hi, I’m Maggie and I live in Northern California. I have stage 4 lung cancer. I was diagnosed in the summer of 2021.
I have an enlarged lymph node pressing against my vocal cords, so it makes my voice sound hoarse.
Passions, purpose, and the healing power of cats
I have several passions. One of my biggest passions is travel. I grew up with my dad working for an oil company, so we lived in various countries around the world. I got used to traveling to exotic places. I love to go on vacations, whether it’s around the world or locally.
Another passion is animals, cats especially. I stopped working in 2022 and was looking for things to do during my free time. A local animal rescue near me, called Joybound, was looking for people to volunteer for cat socializing and feeding. I went through the training and signed up. When I started volunteering, I’d go once a week. It basically involves playing with cats or socializing them; bringing them out of their shells if they’re shy cats or having them learn better behaviors if there are some problem behaviors.
It’s something that has helped me since my diagnosis. When I’m focusing on a cat and in the room with them, if I have upcoming scans, doctor’s appointments, or treatments, those are completely out of my mind because I am so focused on that little animal. It has been helpful. It’s like therapy for me. They give us back unconditional love.
Why advocacy became a core part of my cancer journey
Part of my personality and how I’ve always been is that I like to help others. Not long after I got diagnosed, I signed up with an organization that does peer mentoring for newly diagnosed lung cancer patients. That’s how I started my personal advocacy, by helping other people who were going through a similar experience to what I had gone through to navigate the unknown and how we all feel at the beginning of a diagnosis when we hear those words: “You’ve got cancer.”
I got involved with different advocacy groups: the Lung Cancer Research Foundation, the LUNGevity Foundation, and The White Ribbon Project. I would get to know other people with lung cancer and expand my personal community of friends and learn from them.
The advocacy where I got hooked on telling my story was in 2024. I went to Washington, DC, for the Rally for Medical Research; it wasn’t just cancer, but all kinds of medical issues. We went and talked with our representatives and senators about more funding for the National Institutes of Health (NIH) for different kinds of research. I got to tell my story about lung cancer and the importance of research. If there were a headline for my life, it would be, “Keep hope alive — why research matters,” because without research, we can’t have hope.
I realized that I could have an impact on the lives of others by telling my story. I got more involved with The White Ribbon Project, ribbon builds, and going to various events. With the Lung Cancer Research Foundation, I am part of their peer review, where patient advocates review grants for funding for different research projects. These are things where I feel like I can make a difference and learn.
From birthday optimism to a shocking stage 4 lung cancer diagnosis
In May 2021, I turned 60 years old. I remember waking up on my birthday and having this feeling that this is going to be the best year of my life. I don’t always feel that on my birthday, but I remember feeling that on my 60th.
About a month and a half later, I had an ocular migraine while I was working. There was no pain involved. It’s like looking through a kaleidoscope with white glass and typically lasts 30 seconds or a minute in one eye and maybe the other. I Googled “kaleidoscope vision” because I remembered experiencing something similar a few years before. Sure enough, it was an ocular migraine. I talked to my optometrist about it several years ago and learned it can be brought on by stress. It was a stressful time at work because we were getting ready for an audit, so I didn’t think anything about it.
Then, a couple of weeks later, I had this pain in my leg after standing up and it didn’t go away. I thought it was a muscle cramp. It turned out to be a partial blood clot in my leg. I continued to have weird symptoms. This was around June and July.
I had other vision problems. I was referred to an ophthalmologist who ran a bunch of tests, including a complete blood count (CBC). The white and red counts were off, but nothing that would raise any big red flags. In the meantime, my optometrist suggested I get a physical because I was having all these weird symptoms, so I made an appointment to see my primary care physician (PCP) at the beginning of August.
A couple of days before the appointment, I experienced pain on the left side of my chest and then again a couple of days later. I mentioned it at my PCP appointment, so they did an EKG. The results indicated some abnormality with my heart rhythm, so I was referred to a cardiologist with an appointment for a couple of weeks out. In the meantime, I got a message from my PCP’s office that either the machine had made a mistake or somebody had misread the results. There was nothing wrong with my heart rhythm, so I didn’t need to see a cardiologist. But I decided to keep the appointment.
I explained to the physician’s assistant in cardiology what had been going on that summer: the vision and balance problems, the deep vein thrombosis (DVT) in my leg, and the pain in my chest. She thought I could be developing a pulmonary embolism, even though I was on blood thinners. She ordered a CT scan and an ECG.
I had the CT scan on August 31st at 8:00 a.m. and got the results in my health portal by 9:30 a.m. Of course, I opened it and immediately read words like “metastases.” I thought, “Wait, what? What’s going on?” I was able to get in to see my PCP at the end of the day. My PCP and the PA in cardiology were very apologetic that I got the results before they had a chance to tell me. I asked my PCP, “What are the chances that this isn’t cancer?” She said, “There’s about a 1% chance that it’s not cancer.”
A subsequent biopsy confirmed that it was non-small cell lung carcinoma. I had a brain MRI that found metastases in my brain, which were causing the vision and balance problems. I never had any lung symptoms, so it was shocking to me to have lung cancer. Of all the cancers to get, it was a complete shock.
Originally, before they found the brain mets, they thought it might be stage 3 cancer. I remember seeing a thoracic surgeon first, thinking I could have surgery. But then they did the brain MRI, so it was now stage 4. In my extended family, nobody had lung cancer, but there were people who have had stage 4 cancer and didn’t live very long. I thought all cancer was the same. I thought, “Stage 4. Okay, it’s September, I’ll get chemotherapy and lose all my hair, then I’ll be dead by Christmas.”
Surprisingly, that’s when I first learned that cancer wasn’t one-size-fits-all. My oncologist fortunately ordered a blood biopsy, which is how I found out that I had an EGFR mutation and that there was a targeted therapy pill I could take. I started taking that pill in October and by December, scans showed that there was no evidence of disease anywhere. There was nothing in my brain and my lungs.
Going back to the pain on the left side of my chest, there was no cancer there. The cancer was in my right lung and right lymph nodes. I never had that pain again. I take it as a sign from above, as if somebody was shaking me, “Maggie, come on. You need to get this tested.” I’m absolutely grateful for a machine that made a mistake.
Learning about my EGFR mutation and that lung cancer isn’t one-size-fits-all
At the time, I remember my oncologist doing a blood draw. I don’t remember her explaining about biomarkers. She might have, but in those first few months, I felt like I was in a fog. It was such a shock to have lung cancer, and then finding out that I wouldn’t have chemo, it was different.
Because I had a mutation, my oncologist had me get a second opinion from an oncologist at the University of California San Francisco (UCSF) who was more familiar with my mutation and explained a little bit more about it. She guided me to some different groups, like EGFR Resisters and Lung Cancer Research Foundation. That was when I also started my quest for knowledge about lung cancer. I’m not an expert, but I sure know a lot more than I did four and a half years ago.
The emotional whiplash of a cancer diagnosis
The brain fog comes in from being so overwhelmed. Part of my personality, in addition to liking to help people, is that I like to be in control of things, so cancer threw me for a loop because it was not part of my plan. When I woke up on my birthday in May and when I felt it was going to be the best year of my life, this was not what I had envisioned.
I started with the targeted therapy pill in October and had scans in December, which showed no evidence of disease. I felt like I’d been punked. Like somebody would come out and say, “Hey, Maggie, sorry; we were kidding,” that the machine made a mistake, or maybe someone else’s test results somehow got dropped into my chart, as crazy as that sounds.
One thing somebody told me early on was to make sure that I brought somebody else with me to my appointments. Fortunately, for all those appointments at the beginning, I had somebody with me who was hearing these words that I wasn’t hearing. But still, having cancer, and then suddenly they couldn’t find the cancer? I remember a friend even said to me, “Maggie, you don’t seem as happy as you should be. You don’t have cancer.” I was thinking, “I’m getting my head around the fact that somebody told me that I did have it. What do you mean I’m not happy enough?”
My treatment journey through five lines of therapy
My targeted therapy resulted in no evidence of disease after two months. I stayed that way from January through September 2022. Then a scan in September showed that the cancer had come back at the original tumor site, which was in my upper right lobe. One of the options was radiation or stereotactic body radiation therapy (SBRT). I had a cruise planned over Thanksgiving, so the radiation had to get done in November before my cruise, which thankfully worked out. Doctors are so accommodating. I find all the cancer doctors are wonderful.
In the spring of 2023, another scan showed some more progression. My oncologist ordered another blood biopsy and also a tissue biopsy from my lung tissue. The blood biopsy came back and showed that I had developed a resistance mutation: MET amplification. This can happen a lot of times for EGFR patients who are on tyrosine kinase inhibitors (TKIs). It’s a resistance mutation that develops.
What was fortuitous was that the clinic I was going to happened to have a phase 2 clinical trial that was opening up and accepting new patients for people in my exact situation: EGFR patients who had progressed on a TKI because of MET amplification. I went on that clinical trial. I was in the control group, so I stayed on the targeted therapy for EGFR and added a targeted therapy drug for the MET amplification. That treatment regimen worked for nine months. It seems I could go in nine-month intervals.
Then a scan showed the cancer had come back. The site had grown more than 20 or 25%, whatever the cutoff was for the trial, so I got dropped from the trial. I had some more SBRT. More scans in the summer of 2024 showed more progression.
The next option was chemotherapy. On World Cancer Day, August 1, 2024, I started chemotherapy. I did six rounds of platinum-based therapy and some more rounds of the other chemo drug alone.
Then in January 2025, a scan showed progression again. The chemo had worked for a while. I had stayed on the targeted therapy pill. Blood biopsies, since the first one in 2023, have never shown MET amplification. But I’ve had tissue biopsies from lymph nodes and those showed that I still had the MET amplification in addition to EGFR. My doctors knew that we needed to treat both mutations in order to be successful in pushing back the cancer.
I was on combined drugs for the MET amplification and a different drug for the EGFR mutation from March through October 2025. But one of the typical side effects of the drug for the MET mutation is edema. I ended up getting severe edema in my lungs as pleural effusion, so I had to have thoracentesis procedures to remove fluid. I was short of breath all the time. The side effect of the drug outweighed the benefit. It was working, but it was just outweighing the benefit, so I had to stop treatment. That was my fourth line.
Recently, I started my fifth line. Another test that my oncologist did was immunohistochemistry (IHC) testing. You do a FISH test to get the MET amplification result, and you can do IHC, which tests for overexpression. In addition to amplification, I also have MET overexpression. It’s a double-edged sword in a way, but this one opened up a new line of treatment, a new drug that will work better for me because it targets the overexpression. I’m going on that and then back on another drug to target the EGFR mutation.
I’ve gotten used to seeing progression in my scans. I look at scans as information. I used to get freaked out by them, but not so much anymore. If something is going on, it’s going to help direct my oncology team and me to figure out the next line of treatment, and I’m always hopeful that there will be a next step.
Why biomarker testing is critical for every lung cancer patient
Biomarker testing is critical for getting patients the right treatment, especially for lung cancer. It’s not one-size-fits-all. It’s not just chemo for everyone. You have to know what your biomarkers are. You have to get genomic testing, next-generation sequencing (NGS), and RNA and DNA testing, because there are drugs out there that have been developed to target specific mutations. If you have a specific mutation, then you can get access to the drug that’s going to work for you.
It’s not throwing everything at it and hoping something will stick; it’s a dart. It’s a little missile attacking your mutation. I have this analogy in my head. The cancer cells are like sleeper cells, the little spies that look like everyone else. They come into a town, and everybody accepts them. They’re a little bit different, but they seem fine. Then suddenly, these sleeper cells get activated and they start killing the other cells in the town.
The first method of attack can be chemotherapy, which I consider like carpet bombing. You’re killing those sleeper cells, but you’re also killing everybody else. But then you’ve got the SEAL team that comes in, the snipers. That’s what the targeted therapies are like. Those are drugs that go in like little missiles and target those cancer cells, leaving the healthy cells alone. The healthy cells can still live and thrive in your body, but the cancer cells will be gone.
How lung cancer communities and mutation-specific support groups change everything
Find your people, people with the same mutation. First of all, finding other people with lung cancer is so important. I went to a LUNGevity Foundation event. They hold an annual event called the HOPE Summit, which I went to for the first time in 2024. I was skeptical. I thought, “What’s this going to be like, being in a room with a bunch of people with cancer? Is it going to be depressing?” On the contrary, it was uplifting. You see other people and they’re thriving. You can learn from other people.
Then, drill down further to the specific groups. There are the MET Crusaders, which I’m involved with, and EGFR Resisters. Within those groups are your people, because those are people who are on the same drugs as you are. They may even be seeing the same doctors and specialists. If they’re on the same drugs, they’re probably having the same side effects. Let’s face it: these drugs are killing cancer, so they’re probably going to have some not-so-pleasant side effects from time to time.
Being with other people in your mutation community, you learn from them. I can also give advice but not medical advice. You can share, “From my experience, these are the lotions that I’ve used that have worked well on this skin situation I had. But be sure to ask your dermatologist first.” You don’t feel alone, like you’re the only person with this situation.
I’ve met so many amazing people since getting diagnosed with lung cancer. I laugh sometimes: get lung cancer, double your friend count on Facebook. It’s an amazing community. I’m sure other cancer communities are exactly like that. I’m not grateful that I have cancer, but I’m grateful that I met all of these wonderful people and have had opportunities presented to me that I wouldn’t have had without lung cancer.
What I learned about biomarkers and personalized medicine
Biomarkers allow for personalized medicine. It’s about finding the right treatment for that patient at the right time. Any time I’ve had progression, I’ve either asked for a blood biopsy. It had been a year since I had a tissue biopsy, so I asked my oncologist, “Can we do another tissue biopsy?” Tissue biopsies are the gold standard to find out what’s going on with the cancer. A blood biopsy is only as good as what happens to be circulating in your bloodstream at the time.
It’s about personalized medicine and tailoring the treatment to the patient. The patient and the oncologist need to be able to work together and come to an agreement on what that treatment will be. Educating myself on what drugs are important for what treatment and what drugs are for what biomarker is critical.
Recently, I was going to go on a drug for the MET overexpression, and I asked about a drug for EGFR. Initially, my oncologist said, “The drug for overexpression has some chemotherapy with it, so it should be able to take care of the other mutation.” I remembered reading something and talking with another oncologist in the past, so I reached out to that other oncologist, who then directed me to a clinical trial that had been done. In that trial, people who had MET overexpression and EGFR did better if they were on drugs for both mutations. I was able to look at the clinical trial results and cite results from that study back to my oncologist. I brought that information to my oncologist and he agreed. Now I’ll be on drugs for both mutations.
How shared treatment decision-making can transform your care
I’ve always gotten second opinions. My oncologists have always been supportive of that. At the beginning, I was seeing a general oncologist, and she encouraged me to get second opinions. When I had progression at the beginning of 2025, I switched my care to a thoracic oncologist. This far in, I want to be with a lung cancer specialist.
My oncologist and I make the decisions together. He never acts annoyed when I bring up other perspectives. The other people I consult with all know each other. If I say, “I talked to Dr. So-and-so,” he can talk with that doctor himself or look up a study.
Not everyone knows everything, even if you’re an expert. I’m so appreciative of my oncologist and the input that I have, because it’s ultimately my life. If he doesn’t agree with something, he explains why he doesn’t agree with it. It’s not like I always get my way, but I feel heard.
How advocacy, research, and letting go sustain me through stage 4 lung cancer
I like to have a plan for things. A friend of mine told me that for someone like me, getting something like cancer, where you can’t control what’s going to happen, has been a good learning experience to let go of some of that control, to let things play out, and see what happens.
I do what I can to control what I can. I can control my advocacy efforts. I can control my research, like looking up new drugs and going to conferences. I like going to lung cancer and cancer conferences. I feel like I can learn a lot about new treatments on the horizon. I can also let people see what someone with stage 4 lung cancer looks like. To the people at the drug companies, this is who you’re making these drugs for. You’re not doing it for some faceless person. You’re doing it for me.
Living fully with stage 4 lung cancer through gratitude and reframing
Even before I had cancer, I learned that we all have emotions. We feel happy, sad, and anxious, among other things, and there are thoughts that go along with those emotions. I learned early on that I can control my thoughts. I can decide how I want to look at something.
The way I chose to look at lung cancer is, “What am I going to learn from this?” I don’t look at it like, “Woe is me.” Some days, I feel that way, but mostly I think, “What can I do to live my best life? What can I do to be fulfilled?”
My life is so much more fulfilled now than it was before I had lung cancer. I have gratitude now that I didn’t have before I got diagnosed, because I know now what it feels like to not know if I’ll have tomorrow or next year. My goal right now is to make it to five years. If I do, I will have gone on this fantastic trip up to Greenland and Iceland to see the solar eclipse; that’s my plan for August.
I’m learning gratitude, how to control my thoughts, and how to reframe things. What can I learn from this situation? How can I look at it differently? Is this a helpful thought? I’m not ignoring my emotions or my feelings, but I’m trying to reframe and think about things in the best way I can.
Why every lung cancer patient should consider clinical trials as an option
Everybody should consider clinical trials. There are different phases of clinical trials and different trials. I’ve been in two clinical trials, and I’m in another one related to the radiation I had. As a patient, make sure the trial is explained to you, especially the benefits and risks. You’re getting access to drugs that you might not otherwise have. There may be drugs that your insurance won’t approve, but you can get through a trial. I feel good about having done the trial because I feel like I’m helping people in the future who will hopefully benefit from the experience I’ve gone through.
Starting a fifth line of treatment and preparing emotionally for a new drug and renewed hope
My biggest concern with a new drug is usually side effects. What are the potential side effects going to be, and how can I manage them if they come up? What’s the plan if the side effects get to be too much? I personally go in thinking that the drug is going to work; that’s not my concern. It’s just something new.
This new drug has been recently approved by the FDA. It wasn’t even available when I got diagnosed four years ago. I didn’t even know I was a candidate for it until October 2025. But when I first got the infusion, I thought that I would feel something. I didn’t, but I know that’s good. No side effects. I hope it’s in there, killing all those cancer cells and doing exactly what it’s supposed to be doing.
My advice for patients who don’t know about biomarker testing
Some of the different lung cancer groups have information on their websites about biomarker testing. Where I learned about it was the Lung Cancer Research Foundation. They have done webinars and past webinars are available on their website. There is one where they talked about biomarker testing and next-generation sequencing, the importance of tissue testing, and the kinds of tests to get for biomarkers.
Definitely ask your oncologist. If your oncologist isn’t doing biomarker testing, then you need to ask for it. There are different blood biopsy companies that do biomarker testing. Though tissue testing is still the gold standard, sometimes it’s difficult to get enough tissue samples. If you’re lucky, like me, to have lymph nodes that are easy to reach, where they can get more tissue, those are great for biomarker testing.
You won’t know what treatment you need without biomarker testing, even to know if you don’t have a biomarker. In addition to biomarkers, there’s PD-L1 and that can direct treatment, too. If you have a higher PD-L1 number, you might be more of a candidate for immunotherapy than someone with low PD-L1 numbers. These are important things to know that can direct your treatment as a new patient. Without that information, it’s like throwing a dart in the dark.
What hope means to me
Hope means a good future. It means research. Research means hope. Hope means research. Without research for new drugs and new treatments, treatment comes to a standstill. I’ve been on two different drugs that weren’t around when I was first diagnosed. Even the way my mutation is treated has changed; it’s treated differently now for newly diagnosed patients. That’s part of hope. For me, it goes along with gratitude and being more in the moment. Hope is so important because without hope, what is there?
My message of hope for anyone feeling hopeless
There was something I learned through meditation: the blue sky is always there. It’s covered by clouds sometimes, but the blue sky will always come back. You might be feeling hopeless in the moment, and it’s important not to ignore those feelings. You have to live that. You have to lean into those feelings. But that’s not a forever feeling. You will feel hopeful again. You will move through it. If you’re in a dark place, you will move through it.
Reach out to friends and family. If you’re religious, reach out to religious support groups. Talk with your oncologist. Talk with your oncology nurse. Talk with other people online. Look for a peer support partner. There is hope. There is blue sky behind the clouds. Trust me, it’s there.
Gratitude, oncologists, and a life without an expiration date
I’m so grateful to be able to tell my story and for people in the field of thoracic oncology. I’m appreciative of anybody who goes into oncology. I’ve been fortunate that everyone I know in oncology has been wonderful.
I’ve also never had anyone give me an expiration date. And I’m grateful for that.

Inspired by Maggie's story?
Share your story, too!

Thank you to AbbVie for their support of our independent patient education program. The Patient Story retains full editorial control over all content.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
More EGFR+ Lung Cancer Stories
Jennifer M., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptoms: None per se; discovered during physical checkup for what seemed to be a sinus infection
Treatments: Radiation therapy (stereotactic body radiation therapy or SBRT), targeted therapy
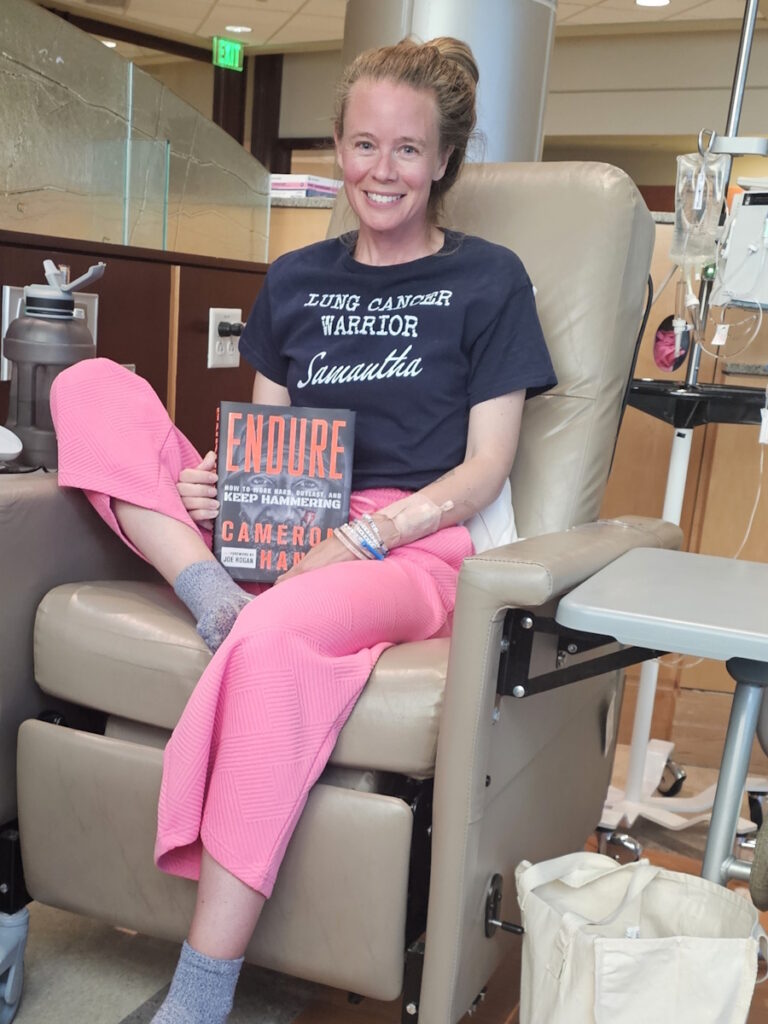
Samantha V., Lung Cancer, EGFR+, Stage 2, Grade 3
Symptoms: Breathlessness, hoarseness, sinus infections, fatigue, pain in left side
Treatments: Clinical trial (targeted therapy)
Natasha L., Lung Cancer, EGFR+, Stage 4
Symptoms: Hoarse voice, squeaky breathing, cough, weight loss, fatigue
Treatment: Targeted therapy
Jeff S., Lung Cancer, EGFR+, Stage 4 (Metastatic)
Symptom: Slight cough
Treatments: Surgery, radiation, chemotherapy, targeted therapy
Jill F., Lung Cancer, EGFR+, Stage 1A
Symptom: Nodule found during periodic scan
Treatments: Surgery, targeted therapy, radiation