Trust Your Body, Trust Your Care Team: How Aleeshia Faced Rare Burkitt Lymphoma at 33
Burkitt lymphoma and severe fatigue showed up in Aleeshia’s life long before anyone said the word “cancer.” Living in Milan but rooted in a multicultural family that spans Vancouver, Montreal, Egypt, and Italy, Aleeshia had always built a life around travel, food, and making every new place feel like home. When a strange, unrelenting fatigue settled in, she assumed it was stress, hormones, or lingering effects of polycystic ovary syndrome (PCOS), not an aggressive stage 4B blood cancer quietly growing in her abdomen and bone marrow.
Interviewed by: Nikki Murphy
Over a few weeks, subtle symptoms escalated into a cascade of red flags: deep bone-like shoulder pain that cortisone could not touch, severe ear pain, bloating, early fullness, nausea, and pelvic pain. One morning, the pain was so intense that she crawled from the bathroom to her bed. After an ambulance ride and emergency surgery came a shocking discovery: a 15-centimeter mass on her ovary, massive internal bleeding, and the first mention that this might be lymphoma.

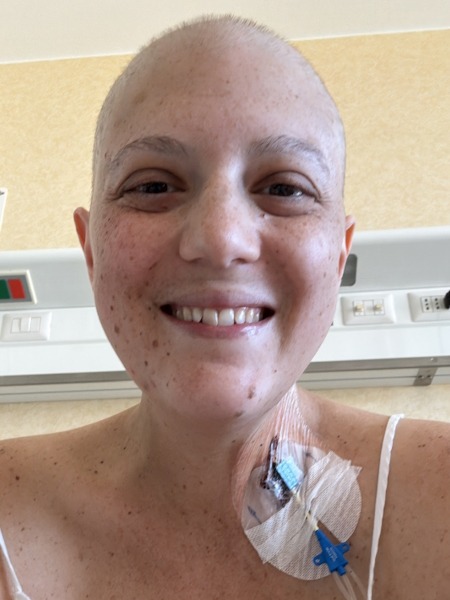
While she processed the loss of her left ovary and the fear for her fertility, the full diagnosis came in stages: large B‑cell aggressive lymphoma, then Burkitt lymphoma, and finally, stage 4B disease with bone marrow involvement. Hospitalized, unable to walk on her own, and rapidly getting sicker, she started intense, inpatient chemotherapy and immunotherapy almost immediately. The protocol demanded month‑long hospital stays, repeated infections, brutal nausea, and near-constant IV lines including a catheter in her neck when a PICC line failed.
Amid the physical toll, the emotional weight was just as heavy. Aleeshia grieved the possibility that menopause and infertility might outlast treatment, and she weathered moments of rage and despair where she wanted to rip out the IVs and go home. Her hematologist‑oncologist and a hospital psychologist became anchors, normalizing her feelings and giving her space to speak honestly. Supported by her parents and her husband, she kept returning to one grounding belief: trust in her care team and in her body’s ability to heal.
At the end of November, she heard the words “no evidence of disease.” Survivorship now means scanxiety, new physical limits, and ongoing questions about fertility, but it also brought her back to a more spontaneous, authentic self — someone who no longer needs a perfect plan to feel like her life is meaningful.
Watch Aleeshia’s story or read the interview transcript below to know more about her story:
- Fatigue that doesn’t improve with rest, deep bone-like pain, sudden changes in digestion, or pelvic pain can be meaningful signals that deserve thorough medical follow-up
- A rare, aggressive cancer like stage 4B Burkitt lymphoma can be extremely chemosensitive
- It is never a patient’s fault when treatment causes harsh side effects or long-term impacts; the burden belongs to the disease and the intensity of the therapy
- Honest, compassionate communication can ground patients in moments of shock and fear.
- Aleeshia describes a powerful transformation: from feeling trapped and powerless in the hospital to reconnecting with her spontaneous, joyful nature and considering advocacy around psychological care in cancer treatment
- Name: Aleeshia T.
- Age at Diagnosis:
- 33
- Diagnoses:
- Burkitt Lymphoma
- Staging:
- Stage 4B
- Symptoms:
- Severe fatigue
- Deep shoulder pain
- Ear pain with inflammation
- Abdominal and pelvic pain
- Bloating
- Early fullness
- Nausea
- Difficulty eating
- Inability to urinate despite feeling an urgent need
- Internal bleeding
- Delayed period/bleeding
- Intense whole‑body pain leading to collapse
- Treatments:
- Surgeries: emergency laparoscopic surgery with left ovary removal
- Chemotherapy: R‑CODOX‑M/IVAC
- Immunotherapy
- Hormonal therapy (to protect the remaining ovary)
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Who I Am
- When I First Noticed Something Was Wrong
- My Path to Diagnosis
- What Happened Next
- The Weekend That Changed Everything
- I Needed Emergency Surgery
- The Moment Everything Changed
- Waiting for Histology
- I Was Getting Worse
- Hearing My Full Diagnosis
- I Thought I was Going to Die
- Choosing My Care Team
- My Treatment Plan
- I Had to Submit Myself
- I’m Worried About Future Fertility Issues
- My Treatment Plan was Aggressive and Painful
- How I Coped Mentally
- The Hardest Moment of My Journey
- How Cancer Impacted Me
- I Was Declared NED Before the Holidays
- What I Want Others to Know
Who I Am
My name is Aleeshia. I’m from Vancouver, Canada, but I live in Milan, Italy, and I was diagnosed with stage 4B Burkitt lymphoma in May 2025.
I am quite passionate about traveling. I have been traveling my whole life. My dad worked in the airline industry for a big chunk of my childhood. My sister is a flight attendant and I also work in the industry; I work for a tour operator. I come from a very multicultural family. My dad is Italian-Canadian. My mother is Egyptian-American. They grew up going to a lot of places as well and passed that down to my sister and me.
I love exploring new places, but what I like is getting to a place and making it feel like home in a way. I have not been to the most countries or done the most things in the world, but I have spent a significant amount of time in places that I have been interested in. It has been 10 years since I came to live in Italy and I have moved around a lot, which is not typical of a North American expat who comes to Italy. They usually pick one place and stay. I love it because you see a slice of life in other parts of the world and how people live. I love to connect with people in that way.
A couple of other hobbies or things that I am passionate about are food and cooking. I actually came to Italy to get my master’s degree in food studies. Hand in hand with traveling, I am interested in understanding why people eat what they eat, how it gets to their table, traditional family recipes, and that kind of stuff. I cook a lot. Whenever I am at my grandmother’s house in Montreal, I’m usually writing down her recipes, cooking, and taking pictures so that I can preserve all of that knowledge.
I also read a lot. My undergraduate degree is in English literature. When I am not somewhere else in the world, I am usually on my couch reading a good book.
When I First Noticed Something Was Wrong
The fatigue was probably the very first symptom. I did not have night sweats. I was not losing weight. For most lymphomas, the classic B symptoms are rapid or unexplained weight loss, night sweats, and fatigue. I think I only had fatigue. It was a strange sensation because I felt tired, but sleep and rest did not make the fatigue go away. It felt more like my energy was completely depleted, and the effort needed to do certain basic things was almost non-existent. But I did not feel unwell.
Those very first signs of fatigue and energy loss did not register with me as anything wrong besides something potentially stress-related or health-related, but not cancer. At the time, my husband and I were trying to get pregnant. I had received a PCOS diagnosis the year before, so I thought something was going on there. It did not at all register that it could be a tumor.
My Path to Diagnosis
After the trip, I came back, and almost the day after I landed, I had this pain in my left ear. I thought I had picked up a little ear infection or a sinus infection that had traveled to my ear or something. I went to a walk-in clinic near my house, and the doctor did an exam and said it was definitely severely inflamed. I remember her saying that the lymph nodes in the area were not swollen but that the nerves were swollen. She said it was probably an infection, gave me some antibiotics, and I went on my way.
About five days into taking these antibiotics, I felt so much worse than I did originally. I had a fever and bad stomachaches, and that sense of fatigue and zero energy made it difficult to get out of bed. I called my GP and said, “I need to see you today. I cannot work. I am ill.” In Italy, you need your doctor to give you a note to say that you are sick so that your sick days get paid out. She said she had about a half-hour gap and if I could come at that time. This was the second week of April, and I dragged myself over to her studio.
In that visit, she looked at my ear and said she did not think those antibiotics were the right ones for the ear infection, so she switched the antibiotics. Given that I had a fever and stomachaches, she did an abdominal exam as well and chalked up the pain in my abdominal area to a bit of gastrointestinal inflammation because of the antibiotics.
The other thing is that my period was two weeks late. This is important for when I get to the hospital. I had been doing regular at-home pregnancy tests, and they were negative. She said, “I will prescribe you a blood test, and we will rule that out,” because I had cramping in the pelvic area. She said, “I think it is mainly due to the antibiotics, but we will rule that out if you do this blood test and then we can go from there.”
I changed antibiotics. I never made it to doing the blood test she prescribed. Three days later, the pain in my ear was through the roof, to the point where I thought maybe I needed to go to the emergency room. My husband said, “Why don’t you just go see an ENT?” I made an appointment with an ENT at the hospital. At that visit, he said, “You do not have an infection. It is severely inflamed. I am going to give you cortisone.” That was a bit of a switch in my mind because I thought, “Okay, it is not an infection. Why would my ear just randomly get inflamed?” But we decided I would take the cortisone and see what happened.
When I started on this course of cortisone, my ear pain went away almost immediately, but then my shoulder started acting up. I had this severe, very deep pain in the point of my shoulder, and it felt like it was coming from inside my bone. Stretching and exercising did not help, and it was worse at night. That was very worrisome for me because I could not understand why I would have a pain that would worsen during certain parts of the day and be more tolerable at other parts of the day.
I was still taking cortisone, which is an extremely powerful anti-inflammatory, so I thought if it was muscular or if there was an inflammatory response causing this pain, the cortisone would be knocking it out. Instead, it was not. I was quite worried about that, but I said to myself, “You have not been well this whole month, and you still have not had your period.” So there was still this potential underlying hormonal diagnosis brewing in my mind and in my doctor’s mind.
What Happened Next
I said, “Okay, I will finish the cortisone and we will see what happens.” I did finish the cortisone, but I could not hold out on the pain. About five days into the cortisone, near the end of April, the pain in my arm was so bad one night that I woke up around 3 a.m. and said to my husband, “You have to take me to the emergency room. It is searing. I cannot think about anything else.” I was seeing white from how bad the pain in my shoulder was.
We went to the emergency room, and they treated it like it was just a muscular situation. They gave me an injection of a high-dose painkiller, and I was sent home. That helped with the shoulder situation, but I was still having cramps, abdominal pain, and just feeling unwell in my belly in general. It was difficult to eat, and I would get full quickly.
During that last week of April, I was also noticing that I was very bloated all the time and eating had become difficult. I would get full almost instantly and feel nauseous after I ate. It was a lot of things all at once and very quickly.
The Weekend That Changed Everything
I went to the ER twice. The first time my husband brought me in the middle of the night for my shoulder was a Friday. That weekend, my sister was in Milan on a layover. My mom had been here; she had come for Easter. The three of us went on a little day trip. I was feeling all right. I could still feel this pain in my shoulder, but overall, I was feeling okay. We were out all day long and had a great time.
On Sunday, my mom and I had plans to do another day trip to Como, and I woke up and said, “Mom, I do not feel good. Do you mind if we stay home?” She said, “Yeah, sure, no problem.” We ran a couple of errands but stayed home for the rest of the day, and I slept most of that afternoon. What changed on Sunday was that I started bleeding. I thought my period had finally arrived a month late, which resolved the potential pregnancy situation. But it did not ease up any of the pain I was feeling in my pelvic area, which was strange because I normally do not have cramps or a difficult period.
My mom was a bit worried because she said, “I had an ectopic pregnancy, and it can be life-threatening. Is it painful?” I said, “No, I think it is just weird cramps. It is not that bad. I just feel tired. I will be okay.” I slept off most of the afternoon on Sunday, then had dinner, and went to bed super early. Around 5 a.m. on Monday, I woke up in pain that I do not even know how to describe. I was not in my body. The pain was so overwhelming that I felt like I had zero control over my body. The pain was controlling everything.
I got out of bed, went to the bathroom, and fainted. I was only passed out for maybe five or six seconds, but it was 5 a.m. My husband and my mom were in a deep sleep. I thought, “Something is wrong.” I had to crawl back from the bathroom to my bedroom. I could not stand straight. I was bent at a 90-degree angle, almost on all fours, because the pain was so bad.
When I got into my bedroom, I do not 100% remember what happened. But I was lying on my back and must have been screaming in pain because my mom and my husband both woke up and immediately asked what was wrong. I remember my mom screaming, “Call 911. Call 911.”
I Needed Emergency Surgery
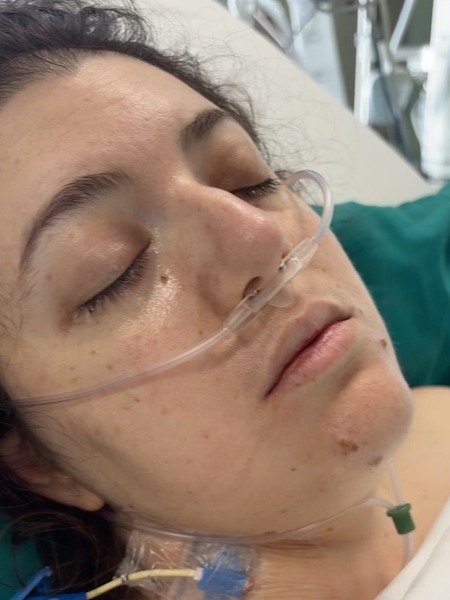
My husband called an ambulance, and they arrived within about five minutes — super quick. I was awake but not super lucid. The paramedic helped me get onto the gurney, and when they picked me up, there were about three liters of sweat on the ground below me. My body was in shock. I was super pale, sweating profusely, and in so much pain that I could not walk or straighten my legs. They rushed me to the hospital. Thankfully, we live within a 10-minute drive of where I was treated.
They took me straight into the ER, and everything was very rapid-fire. It felt like an episode of a medical TV show. There were three or four nurses around me, stripping me, putting in IVs, and asking me questions. The emergency room doctor immediately had an ultrasound out. They called an anesthesiologist. With the ultrasound, they started saying there was a lot of fluid in my abdomen, which was the concerning bit. They said it looked like there was a shadow over one of my ovaries, and they were asking me if I had my period, if I was pregnant, and all of that.
In between all the pain, I was trying to explain that I was about a month late, that I had taken pregnancy tests and they were negative, and that I had just started bleeding the day before. They said, “This could be an ectopic pregnancy.” Everything my mom had said the day before was there on the table. They said, “We are going to have to go in for emergency surgery. We will go laparoscopically. We have to figure out what is happening, but we are going to call in a gynecologist.”
They explained everything to me as it was happening. They had me sign a bunch of consent forms. The anesthesiologist was prepping me for surgery because they said I was going to be put fully under. My husband was there, also signing consent forms so that if things happened during the surgery, he could make decisions on my behalf. It was full on. Within 25 minutes of being admitted into the ER, they had me moving toward an operating table.
The gynecologic surgeon came down and introduced himself. He had been briefed on the situation. They passed me off from emergency medicine into emergency gynecology because this hospital has an emergency obstetrics department and there was a suspected ectopic pregnancy. In the midst of being rolled into the operating room, this doctor said, “Hello, my name is Leonardo. I am going to be operating on you,” and I said, “Okay.” I was pretty much out of it, and that is the last thing I remember because they administered the anesthesia, and I was out right away.
I woke up around seven hours later in intensive care. My doctor was the first person there again. I said, “Hello, Leonardo,” and he chuckled a little bit because I was just waking up after anesthesia, with no idea where I was or how much time had passed. My husband was also there, and I did not realize that pretty much the whole day had elapsed. When I woke up, I thought maybe half an hour had passed. I said to my husband, “What are you still doing here? Are you not supposed to be at work?” He said, “The whole day has gone by. You have been on the operating table for hours. I have been here the whole time.”
Then the doctor said to me, “We had to remove your left ovary. It had died. It was not an ectopic pregnancy. Instead, we found a 15-centimeter mass. I have sent it for a full histology. I think it might be lymphoma, but I do not know which kind. The mass had caused massive internal bleeding. You had lost nearly three liters of blood. We had to do transfusions during the surgery. For right now, all seems well. You are going to spend the night in intensive care, and then you will probably be in the hospital for a bit of post-op recovery.” That was the very first time cancer was mentioned as a potential diagnosis.
The Moment Everything Changed
I was processing what he was telling me in a certain sense, but I do not think the cancer part stuck. I remember being most concerned about my fertility. I think the only thing I asked him was, “Will I still be able to have babies? I only have one ovary left.” He said, “We cannot say that for sure right now.” He was good in his responses. He said, “I did not remove the other ovary because it looked healthy enough. Given your age and the fact that you and your husband were trying, I wanted to give you a chance if there would be one.”
I was focused on that, and I do not think the cancer element did much that day. I remember thinking, “They found this mass; that is scary,” but because they found it on my ovary, I thought it might be a cyst, maybe something related to PCOS. I think there was a part of my brain that thought lymphoma was a possibility, but that there were many other possibilities. I do not think I understood how accurate his presumed diagnosis could be in that moment.
He was very careful to say, “I think it might be this, but I am not giving you this diagnosis. We have sent the mass for histology. I know that it is not a sarcoma because during the operation, we ran a rapid biopsy. If it had been sarcoma, I would have performed a complete hysterectomy because it would have been too dangerous.” I clung to that: it was not sarcoma, not that “dangerous cancer,” so it might be something completely unrelated. I was more focused on the loss of my ovary and what that would mean for my future fertility.
Waiting for Histology
I spent a week in the hospital after the surgery. I stayed one night in intensive care, and the next day, they said I was stable enough to be moved to gynecology. That first week, there was no more talk about cancer or histology. It was focused on post-op care. Every day, they checked my sutures. I still had a drainage bag, so they checked that, changed bandages, and so on.
That week in the hospital, the pain in my shoulder came back, and I started to dwell on it. They sent me for an X-ray to rule out any fracture. The X-ray came back totally normal. Because I was in the gynecological ward, I was only seeing gynecologists. Since the histology was still being performed, they were very careful about saying anything that could sound like a diagnosis. When I would bring up my shoulder, they would say, “The X-ray came back clean, but we are still waiting on the histology. It might be related. We do not know.” I think they were aware it was a symptom, but did not want to tell me it was related to cancer, because they did not want to give me a cancer diagnosis.
I was discharged and went home for a week. I had nothing planned that week. They told me we needed to wait for the histology report to come back. They set up an appointment a week after my discharge for a post-op check-in and said they would have the results at that point. This was the middle of May when I went back into the hospital.
I Was Getting Worse
The week at home, I deteriorated rapidly. During the week in the hospital, my shoulder had started acting up again, but coming off the anesthesia and painkillers was manageable. At home, the pain was through the roof again. I had been eating well enough in the hospital, but at home, I went from feeling okay — sore and tender from the operation — to being sick. I was throwing up everything I tried to eat. I could not go to the bathroom. I felt constantly like I needed to pee, but no urine was coming out. I was very thirsty and was drinking a lot of liquids.
I said to my husband, “I think we should go back to the emergency room,” and he said, “No, it is probably just your body reacting to a huge surgery. You were under anesthesia for at least five hours. They said there might be some tummy aches and stuff like that. You do not have a fever, your stitches have not ruptured, and you are not bleeding. Let us just wait until the 13th.”
On the 13th, we went back into the hospital. I was sick. I needed my husband to push me in a wheelchair. I went into the gynecologist’s office, and next to her was my hematologist-oncologist. At that point, I knew what I was going to be diagnosed with. He was there to tell me that the histology report had come back and that they definitely knew it was a large B-cell aggressive lymphoma. He thought it might be Burkitt lymphoma. He said, “You are going to be hospitalized today, and there will be a couple more diagnostic tests before we decide what your treatment plan will be.”
My diagnosis came in steps. It was discovered in the emergency room. It took two weeks from that emergency operation to a cancer diagnosis and then another week to the complete diagnosis with a treatment plan. In those three weeks, I spent two of them in the hospital.
Hearing My Full Diagnosis
The testing all happened while I was hospitalized. They would say, “Today you are doing an MRI; tomorrow you are doing a PET scan.” I had to do a bone marrow biopsy, which required a lumbar puncture. I had many lumbar punctures. It was probably the worst procedure out of all of them. It was extremely painful for me. I also had a CT scan.
I was hospitalized again. The very next day, I was sent to urology to have stents put into my ureters because the masses were basically blocking them, which is why I had not been able to pee. I had a diagnosis, but it was not the complete diagnosis. I spent another week in the hospital while all of these tests happened. I was very sick, so they wheeled me on beds into all of the different rooms in the hospital to get the CT, the PET, and all of these things. About five or six days after that, I had the Burkitt lymphoma diagnosis, and we had my treatment plan in place. I started chemo immediately the next day.
My first feeling was relief to have an answer, especially for the pain in my shoulder and how ill I had been. There was some release in finally not having to sit with the unknown. Now we knew, and that meant we could do something about it. At the same time, I was completely shocked, numb, scared, and bowled over by the fact that I was 33 years old and had just gotten a cancer diagnosis.
A small part of me was hyper-curious because I had never heard about Burkitt lymphoma. I knew, broadly, about Hodgkin’s and non-Hodgkin’s lymphoma. I have had relatives and other close people in my life who have had cancer or passed away from cancer, so you broadly know about breast cancer or colorectal cancer. Nobody is ever talking about Burkitt lymphoma. I thought, “What is this?”
There was a tiny part of me that was very curious to learn more and to think, “I guess I am going to be a human experiment in a way,” because it is a rare form of cancer. It has fewer than 100 diagnoses in Italy, fewer than 400 in the European Union, and around 200 in the United States, from what I remember looking up. It is classified as a rare cancer.
There was a small part of my brain that was intrigued by learning about something I would never have stumbled upon otherwise, but that was a very small part. It was mainly fear, shock, and a lot of “Why me? What did I do? Was there something I could have done?” It was a weird mixture of relief, fear, and curiosity.
I Thought I was Going to Die
The staging confused me. When I first heard stage 4, I panicked and thought, “I am going to die from this cancer.” My doctor said stage 4 for non-Hodgkin’s lymphoma is a very different diagnosis than stage 4 in other cancers, especially those with solid tumors. It is not that tumors do not grow with lymphoma, but you cannot simply cut lymphoma tumors out. They will keep growing because the cancer is in your blood. He said a stage 4 liver cancer diagnosis is very different from my diagnosis.
Ultimately, the staging was because they found masses all over my abdomen, both above and below my diaphragm, which made it stage 3. Then they also found it in my bone marrow, so it had traveled to one site outside of a lymph node area. Because it was in the bone marrow, it was hurting my shoulder so much. But my lymph nodes in my neck, behind my ears, and in my clavicle were not swollen. The lymph nodes that had swollen, where the masses originally grew, were deep in my abdomen. That is why I never saw a mass anywhere in my body.
Choosing My Care Team
I found my care team because I was already at this hospital. We have a national health service in Italy, so there was never an element of an insurance company needing to approve or not approve certain treatments. At the hospital where I was treated, they said, “Here is the standard of care. This is the protocol used pretty much everywhere in the world as the first-line care for Burkitt lymphoma. Your state of illness is so advanced that we need to start treatment immediately. It is extremely life-threatening, and that is what is going to happen.”
I did not have a chance to ask for a second opinion, shop around hospitals, or speak to other doctors. At one point, especially in that first week after we knew it was cancer but were waiting on the full Burkitt lymphoma diagnosis, I thought, “What if I fly home to Canada? Would the situation be better?”
My parents rapidly came to Italy to be by my side through all of this. My dad said, “We can make it happen if you want to.” It seemed comforting for a second, but the reality was that I was way too sick to travel. I had been living in Italy for nearly a decade; this is my home.
I was worried about doing care in Italian, but my doctor also spoke English quite well. I was nervous about things that were not going to impact my care. The hospital where I was treated is the number one in the country, and it is in the top five oncological centers in all of Italy. I was in good hands, and I happened to stumble into good hands. Once I realized that, I knew I did not need to go anywhere else.
My Treatment Plan
My doctor said, “Here is the main protocol. It is called R-CODOX-M/IVAC.” I thought, “Cool, I do not know what any of that means.” I wrote it down and later that evening did a bunch of Googling. He explained that it is administered in four cycles and that, given my age and the staging of my cancer, we were going to treat it very aggressively.
The good thing about Burkitt lymphoma, to my knowledge and from what my doctor shared with me, is that it is the fastest-growing blood cancer known to man. The masses can double in size in less than 24 hours. He said the good thing about it being so aggressive is that it is extremely chemosensitive. The faster and more aggressively we treat it, the quicker it dies.
He explained that because I was young and had no underlying health conditions, they thought my body could tolerate it, so we were going to go with the most aggressive version of this protocol. I had all high-dose chemotherapy. Because of that, I would need to be hospitalized every single time. I was not able to do day-hospital; I had to be in the hospital.
Each round of chemotherapy required me to be in the hospital for about a month to manage infections and the period of having no white blood cells. He said, “It will be four rounds. We will be done by the end of summer, beginning of fall.” I said, “Okay, fantastic. When do we start?” He said, “We will basically start tomorrow.”
I asked about side effects. I said, “I know what the typical side effects of chemo are. What can I expect here?” He said, “You are going to lose your hair. You are going to feel nauseous.” He told me that neuropathy was a potential side effect — thankfully, that did not happen to me. He said the higher-risk side effects with this chemo protocol, being so aggressive, were potential infertility and damage to other organs, and they would be monitoring that closely. He also mentioned tumor lysis syndrome (TLS), when the tumor rapidly dies and releases a lot of toxins into your bloodstream that make you ill. He said those were the side effects most concerning to them.
I Had to Submit Myself
I had to submit myself to what was happening and put my faith in my doctor’s hands. I did a lot of praying to God and thought, “We are going to get through this.” I think, especially in healthcare communications, being in a European country is very different from North America. I say this not having experienced care firsthand in Canada or the United States but having family members in both countries who have had serious hospitalizations. I think in North America, we are more prone to asking a lot of questions and talking about advocating for yourself.
Culturally, I think that is different in Italy and in Europe in general, where it is more like the doctor says something and you accept it. I asked a lot of questions, and my doctor was amazing and answered them all, but there was never space to say, “I am not going to do something.” He would say, “This is life-threatening, and you are not a hematologist or an oncologist. I am.” It was never in a condescending way, but that is how healthcare communication tends to work in Italy. I noticed that even with my roommates in the hospital. They would say, “Wow, you ask a lot of questions. You ask all these informed questions,” and it is just not the norm there. People accept what their doctor says and go with it.
I’m Worried About Future Fertility Issues
At the time, my husband and I had been trying to have kids. Hearing that the treatment could affect my fertility was not an easy thing to hear. It is probably the thing I asked about the most during the entire treatment. Every single round of chemo, I would ask, “Do we know? Is there any way we can know?” Now that I have finished treatment, Leonardo is still seeing me, and I have picked up visits with gynecology as well so we can monitor if my ovary will start functioning again.
As of right now, I am still in menopause. It was not medically-induced in the classical sense, but they did give me a medication that stopped the production of estrogen as a way to protect my ovary. It is not a fully medically-induced menopause, but it is something that suppressed hormone production to protect the remaining ovary. As it stands, it is still dormant. We do not know if this will be permanent due to the chemo or temporary. It has been the most difficult thing and the element I still need to process the most.
When it came to chemotherapy, immunotherapy, and beating this cancer, I was very much like, “Whatever we need to do, we will do it,” and I tried to stay positive. But my darkest moments through the whole treatment — and even now — are when I stop to think about the fact that my dream of becoming a mother might not come true in the way I imagined it before getting ill. I still do not know how I feel about it, to be honest. Some days I am positive and think, “If it is a permanent menopause, there are other options available. My husband and I can get informed about adoption or other options.” Other days I think, “Hopefully I will be able to get pregnant one day and it will happen exactly like I intended it to.” Every day is a little bit different in how I feel about it.
I did ask about freezing my eggs. I said, “This is important to me. Is it an option?” My doctor said, “I completely understand. I wish it were an option for you. I do. But feasibly, to do that, it is going to be at least three weeks. You have to go through a round of drugs. They have to do some testing and so on. You do not have three weeks. You will be dead in three weeks if we had to wait to do that.”
I think if I had not discovered this through an emergency room visit, I might have been a little incredulous about that and thought, “No, we have time.” But because we discovered it the way we did, and I had already gone through an extremely life-threatening situation — the tumor causing such bad internal bleeding that I would have died if I had not ended up in the emergency room that day — the second he said that, I understood. I thought, “It sucks for me, and I am going to have to work through how much that sucks for me, but obviously I want to live, so we will go forward with the chemo.”
My Treatment Plan was Aggressive and Painful
I was hospitalized for every single round, so treatment definitely affected my day to day because I was sleeping in the hospital. From the middle of April until the end of October, I would spend four weeks in the hospital and come home for 10 or 12 days between rounds. I was put on sick leave at work, so I could not work at all during this period. It meant huge changes to my day to day and my whole family’s day to day.
My husband and I had just brought home a puppy in January, so we had a four-month-old puppy at home that needed a lot of attention. I work from home, so it had been great because I could take him for walks during the day. My husband is a chef, so he is out of the house. Suddenly, we were rapidly trying to figure out how to deal with our puppy, his work, and my hospitalization.
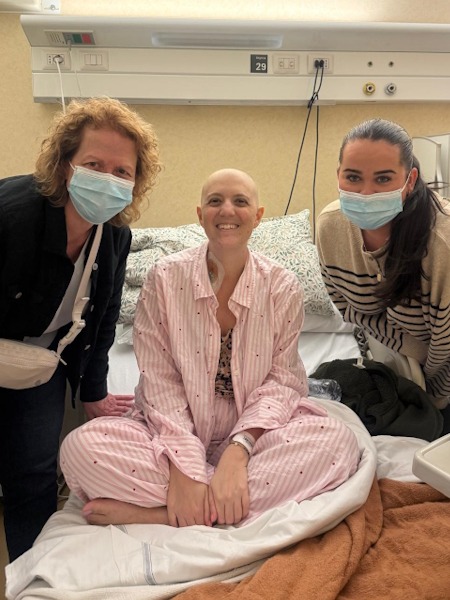
Thankfully, my parents were able to spend extended periods of time with us. My dad came for three months and then my mom came for three months. That was an immense amount of support. They did a lot of the day-to-day stuff, like buying groceries, cooking, and taking the dog out for a walk. They also came every single day to visit me in the hospital.
Treatment itself was difficult. Immunotherapy for me was a breeze. The way the treatment cycles worked is that it alternated between one chemo protocol and then a second set of chemotherapy drugs. Then we switched back to the first set, and round four was the second set again. Each round, I also did an immunotherapy infusion. Those never caused me any side effects. They had told me there was a potential for severe allergic reactions, but I never felt anything. The only thing was they gave me an antihistamine beforehand, which made me drowsy, so the immunotherapy days in the hospital were actually nice because I would just sleep through them.
Chemotherapy was rough. I would get infusions every single day, varying between five and 10 days, depending on which round we were in. The infusions would go anywhere from two to 24 hours, depending on which chemotherapy, because it was basically a cocktail of different chemotherapies, and each had its own infusion times and administration.
I was always hooked up to something, instead of having a port or a PICC line. I did have a PICC line, but it got severely infected, so I ended up getting a catheter in my neck every single time. I still have the two little scars there; I call them my vampire bites. I was almost always hooked up to something in my neck.
When I was not receiving chemotherapy, they had me on an immense amount of fluids. That made mobility in the hospital difficult because I always had something attached to me. I spent a lot of time in bed. The reason I had to be hospitalized for a month at a time is that in the first week or week and a half when we would do the chemotherapy, my immune system would be destroyed. Because the drugs were so aggressive, the period afterward, when your immune system is suppressed, was more acute for me than for people who can go home at the end of the day. I would get severe infections. I got a bad infection every single round, so then I would be on antibiotics for five to 10 days.
My hemoglobin levels would drop low, making me feel dizzy. I would not be able to walk because I would feel so dizzy. The nausea was something out of this world. I had no sense of taste, and most food was disgusting to me. Then I would throw it up anyway, so eating was difficult. It was difficult because you need to eat, or the nausea gets worse. It was a bad cycle of eating to throw up but also needing to eat to not feel nauseous. That was not fun.
Some of the chemotherapy drugs caused severe mucositis in some rounds. I would get bad sores all along my tongue and down my esophagus, and I could not eat, swallow, or talk. During one round of chemotherapy, it got so bad that they put me on an IV drip of nutrition because everything was so swollen and covered in sores that it was impossible to swallow anything. The side effects were intense and debilitating.
How I Coped Mentally
Losing my hair felt almost like nothing compared to everything else. My blood pressure would get low afterward, which, along with the low hemoglobin, made me dizzy; even just sitting up felt uncomfortable. It does not matter if you are in the hospital or at home; when you feel so uncomfortable in your body, nothing is a distraction. You are just stuck there for hours, not feeling well. It was difficult, and that would bring me to a dark place.
I got good at recognizing the patterns that set me off feeling bad, because each chemo round followed a pattern. By the last two rounds, I went in prepared. During the chemo days, I was able to get up every day. I would do some stretching, read books, and call friends and family. In the post-chemo period, for two weeks, I would disappear, feel terrible, and only see my parents and my husband when they came to visit me every day. I did not even try to make myself feel better because I knew the second my white blood cell count went up, the infections passed, and everything stabilized, I would start to mentally feel better. So I accepted it. It took me the first two rounds to figure that out. It was a lot.
The Hardest Moment of My Journey
The hardest moment was during my first round of chemo. I was hospitalized again mid-May. There was that week of testing with all the scans, and the second week is when we started treatment. My first round of chemo did not go well. I ended up doing a fifth round because I had to recuperate some of the chemotherapy I was not able to do in the first round. Tumor lysis syndrome occurred on day two, and I got a raging fever and became very ill. They had to stop chemo.
The hardest moment was about a week or two after that. I was still in the hospital because I had gotten a bad infection and was on antibiotics. I just wanted out. Because everything had happened so rapidly and as an emergency response, I think that was the moment when my body finally started coming down from the shock and adrenaline that had kept me going since the ambulance.
I had a temper tantrum like a toddler. I just wanted out of the hospital. I did not want any needles in me. I did not want anything anymore. I thought, “I want all of this stuff out of my body right now. I want to go home. I do not care about any of this. This is not what I signed up for. I do not know what the universe has against me, but I need out.” My hair was also falling out in massive clumps, which did not help my mental health. I wanted to shave my head. I did not care about being bald, but I did not want to look like that anymore, with my hair looking bad.
Instead of feeling safe and taken care of in the hospital, I felt almost like I was a prisoner. It was a deeply emotional response to everything that was happening. My parents and my husband were thrown into this by surprise too, so none of us knew how to handle the situation. They were telling me to be patient, trying to make me feel better, and that was making it worse. I was crying and crying and crying. I was ready to yank everything out of my body and walk out of the hospital, even though I could not walk.
My doctor came in, put his hand on my arm, looked at me, and said, “Everything you are feeling is normal. It is okay. I cannot discharge you yet. You are too ill. But you will be okay.” I immediately calmed down. I was still crying, but I calmed down. He said, “We will talk more tomorrow,” and I said, “Okay, that is fine,” and left it at that for that day.
The next day, when he came in for the daily debriefs, I said, “I am sorry for my behavior yesterday. I do not know what came over me.” He said, “You do not need to apologize. It is normal. You have overcome so much trauma in such a short period of time. It is normal, and I want you to know that it is normal. I have requested that when you come in for the second round, you will have psychological support for the rest of your chemotherapy treatment provided by the hospital, because this is a lot. You are young, this is life-changing, and it is totally okay.”
A week later, after that moment, I was discharged. I was able to go shave my head, which made me feel a lot better. A lot of people are scared of that moment, but it made me feel better because pulling my hair out for weeks was bad. When I went back into the hospital for round two, I met with a psychologist. For every other round, a psychologist came and visited me every week. It was a moment for me to speak to somebody whose emotions were not tied up in the situation. That was extremely beneficial.
How Cancer Impacted Me
Psychologically, even now, this whole experience has impacted me a lot. My uncle had throat cancer and has been in remission for three years. We were talking about it over Christmas, and he said, “You are going to get a new lease on life.” I said to him, “I do not feel that. I do not feel a new lease on life. In fact, I feel like my quality of life has been decreased because of this.”
For the next five years, foreseeably, I will have regular checkups and scans, all of which bring a small set of anxiety. I had an MRI scan two weeks ago, and just a week of waiting for results brought a lot of stress and anxiety. I was worried about it, and I have never been a very anxious person. That is new for me. There is scan anxiety, the fear of it coming back, and a more heightened state of alertness about my body and how I feel. “Who would have ever thought shoulder pain was cancer?” That is something I am still working on with a psychologist.
At the same time, I feel like I came back to myself. In the few years before the diagnosis, I think I had lost touch with myself. When you make a big move to a new country, you usually do it because you deeply want to. You feel passionate, you are ready to risk a lot of things, and it is not the most traditional path forward. Right when I turned 30, we moved to Milan. It aligned with a more traditional path. My husband and I got steady work at that point and moved toward building a family, buying a house, and planning our wedding — all these stable elements of life that you think you are supposed to do and things we wanted to do.
With that came a new sense of responsibility to get there and be able to do those things. Before, it was, “I am just going to move to Italy,” or, “I am going to take this job because I feel passionate about it,” and it was not as much about long-term benefits. In the years leading up to the diagnosis, I do not think I was fully true to my slightly spontaneous nature.
Coming out of this, I feel like I have been able to reconnect with that version of myself. I have been reminded that you do not have to have a plan. You do not need to know exactly where you are going in life. As long as you stay open to what comes your way and are joyful about it, you will probably get where you want to go in the end. That has been nice. It has been liberating to let go of certain status quo norms I felt I needed to have in order to be successful in life. But there is still that element of increased anxiety that I never dealt with before.
I Was Declared NED Before the Holidays
Survivorship is still new. I was given the no evidence of disease or complete remission diagnosis at the end of November 2025. I almost do not believe it sometimes. When my doctor told me, I almost took it for granted. I thought, “Of course. We just did all of that horrible therapy, so this was the only outcome available.” I had never questioned that we would not get there. I was convinced from the very beginning that we would get there.
When he told me, I thought, “Fantastic.” Now, a couple of months out, I am starting to feel a little more like, “What if it comes back? What does this actually mean? I am now a cancer survivor, and I will be for the rest of my life.” I think I am still trying to figure out what that means. I am trying to understand my new limits, physically and mentally, and what rest looks like. I do not try to push myself as much. I love to travel. Before, I could spend most of the month out and about, between planes and trains and car trips, and I definitely cannot do that right now. I am trying to understand my new limits and be okay with constantly reassessing that.
The further out I go, most likely, the stronger I will get, and the more physically capable I will become. There are a couple of women in Italy who have also had cancer and do a lot of work sharing the importance of psychological care during cancer treatment. I am quite interested in that. If there is a way to get involved in promoting the importance of that, it might be something I want to do. For the most part, though, I think there is still a lot of processing left to be done.
What I Want Others to Know
Trust yourself and trust in your body’s ability to get better. One of the things hugely helpful for me was that from the moment we had the treatment plan, despite it being difficult, feeling horrible, and all the fear, I never once stopped believing in its ability to heal me.
I stayed quite positive — not in a way of forcing myself to be happy, because I was not happy about the situation. I did not want to be there; if this had never happened, that would have been fantastic. But I stayed positive about the power of being taken care of, of the treatment, and of having a care team. I stayed grateful for all of the support I had. My parents were able to leave Vancouver and come for an extended period of time. My work was extremely accommodating. My doctors and nurses were fantastic.
Staying extremely grateful for being able to get the care that I had and truly believing that it was going to make me better was the right mindset to get through something extremely difficult. Trust in your care team, but also trust in your body to get better. Accept the healing.

Inspired by Aleeshia's story?
Share your story, too!
More Burkitt Lymphoma Stories
Ashlee K., Burkitt Lymphoma, Stage 4
Symptoms: Abdominal pain, night sweats, visible mass in the abdomen
Treatments: Surgery (partial colectomy to remove 14 inches of intestine), chemotherapy
Emily S., Burkitt Lymphoma, Stage 4
Symptoms: Constant fatigue, tongue deviated to the left, abscess in right breast, petechiae on legs, night sweats, nausea and vomiting, persistent cough
Treatments: Chemotherapy, stem cell transplant, immunotherapy
Erin R., Diffuse Large B-Cell Lymphoma (DLBCL) & Burkitt Lymphoma, Stage 4
Symptoms: Lower abdominal pain, blood in stool, loss of appetite
Treatments: Chemotherapy (Part A: R-CHOP, HCVAD, Part B: Methotrexate, Rituxan, Cytarabine)
Aleeshia T., Burkitt Lymphoma, Stage 4B
Symptoms: Severe fatigue, deep shoulder pain, ear pain with inflammation, abdominal and pelvic pain, bloating, early fullness, nausea, difficulty eating, inability to urinate despite feeling an urgent need, internal bleeding, delayed period/bleeding, intense whole‑body pain leading to collapse
Treatments: Surgeries (emergency laparoscopic surgery with left ovary removal), chemotherapy (R‑CODOX‑M/IVAC), immunotherapy, hormonal therapy (to protect the remaining ovary)