Heidi’s Stage 3A Non-Small Cell Lung Cancer Story
Here at The Patient Story, we love stories of patients who’ve found purpose after their own cancer diagnosis, especially in grassroots efforts to help amplify the voices of countless others.
This is Heidi’s story. After her own stage 3A non-small cell lung cancer diagnosis at 55 years old, she experienced dealing with stigma and shame, so she decided to combat that with what’s now known as The White Ribbon Project.

- Name: Heidi N.
- Diagnosis (DX)
- Age at DX: 55 years old
- Treatment
- Concurrent chemotherapy & radiation
- Chemotherapy
- 3 cycles of cisplatin and pemetrexed
- 21-day cycles
- Radiation
- IMRT (intensity-modulated radiation therapy)
- Chemotherapy
- Concurrent chemotherapy & radiation
- Heidi's Lung Cancer Story
- Chemoradiation & Immunotherapy
- Navigating Life with Lung Cancer
- The White Ribbon Project
- The genesis of the White Ribbon Project
- Social media attention of the White Ribbon Project
- International presence!
- Tell us more about the White Ribbon Project mission
- What is your next goal?
- Encouraging others to share their lung cancer stories
- Importance of other partnerships
- The modern faces of lung cancer
- The importance of people from all walks sharing their stories
- Lung Cancer Stories for The White Ribbon Project
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Heidi’s Lung Cancer Story
Tell us about yourself
I have been a fitness trainer for 17 years, and I hold a master of science degree in health education. I have been a lifetime health enthusiast.
My husband, Pierre, is a primary care physician, and he has an MPH with a specialization in health education.
Having careers in prevention, we were blindsided by my stage 3A non-small cell lung cancer diagnosis.
How did you know something was wrong?
In October of 2018, at 55 years old, as part of an evaluation of a mildly suspicious ovarian cyst, my OB-GYN physician had me complete a CT scan of my chest, abdomen, and pelvis.
The ovary turned out to be benign, but the chest CT revealed an incidental lung mass, along with enlarged mediastinal lymph nodes.
What were the diagnostic procedures you underwent?
A subsequent biopsy, staging process, and evaluation by 2 different tumor boards confirmed that I had inoperable stage 3A non-small cell lung cancer.
Shocking, as I did not have any respiratory symptoms.
The initial message I got from the pulmonologist and available survival curves was that “I should get my affairs in order,” and that my prognosis was quite grim.
How did you and your loved ones process the diagnosis?
Despite a more positive message, the diagnosis of lung cancer remained a complete shock to my husband and me. Neither of us thought I was at any real risk of developing lung cancer.
»MORE: Patients share how they processed a cancer diagnosis

How did you break the news to others?
I was quite reluctant to tell anyone other than close family and friends about my diagnosis. Having careers in preventive health and having lived a clean life of good nutrition, fitness, and no smoking history, I still felt the stigma of my diagnosis.
»MORE: Breaking the news of a diagnosis to loved ones
Chemoradiation & Immunotherapy
Learning more about treatment options
After meeting my oncologist, he gave me much more hope, indicating that the treatment of lung cancer had greatly evolved over the past several years. One treatment had just been approved by the FDA a month before my diagnosis.
What did you learn from the genetic testing of your tumor?
While the genetic analysis of my tumor did not make me a candidate for targeted therapies, I was a candidate for immunotherapy after completing a course of chemoradiation.
What was your treatment path?
After the diagnosis on October 24, 2018, I met with an oncologist on October 31, 2018, who told me there was hope for curative intent with a new immunotherapy, durvalumab.
If I did not show progression through a CT scan after completion of chemoradiation, I would be a candidate for this immunotherapy.
After a second opinion with an oncologist specializing in lung cancer on November 5, this treatment plan was confirmed.
Since I was considered to be inoperable and did not have a targetable mutation, this was my only treatment option. I was told with chemoradiation alone, I would have a 90% chance of having a recurrence within 6 months.
If I took the immunotherapy, there was a chance of cure. It was not a difficult decision to make.
Describe the chemoradiation you underwent
Beginning November 14, I endured 3 cycles of chemotherapy, cisplatin and pemetrexed, given 21 days apart. I also underwent 30 radiation treatments (IMRT) concurrently with the chemotherapy.
After the seventh radiation treatment, my radiation oncologist showed me there was already significant reduction. By the end of chemoradiation, on December 26, there was very little left of the tumor. It was characterized as scar tissue. Lymph nodes were obliterated.
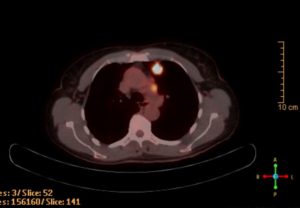
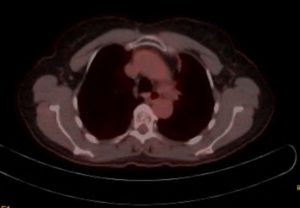
Describe the immunotherapy
Since chemoradiation was successful, I became a candidate for durvalumab and started every other week infusions on January 17. I had 26 infusions of durvalumab, taking a year to complete.
I officially ended treatment on January 8, 2020. Subsequent scans through January 2021 continue to show that there is no evidence of disease.
I do not assume that I am ‘cured.’ I do not know if that will ever be the case. I live my best life from scan to scan, which has been a challenge during the pandemic.
As scan day approaches, I do feel scanxiety, which is just a euphemism for anticipatory terror.
»MORE: Patients describe dealing with scanxiety and waiting for results

Navigating Life with Lung Cancer
Finding a cancer community
The cancer community was not easy to find. I asked my oncologist about support for me and Pierre, and we were told there really wasn’t anything in terms of finding others we might fit in with.
We could not be given names of other survivors, as that would violate HIPAA laws. When sitting in the radiation oncologist’s waiting room, we saw a lot of literature and information about support groups for other cancers, but nothing for lung cancer. We felt alone until 10 months into treatment.
After 10 months of feeling alone, by chance I met another lung cancer survivor much younger than me: an athlete living with stage 4 disease.
She introduced me to 5 other stage 4 survivors with similar stories. They had no known risk factors.
I became convinced that I had a responsibility to share my story and do what I could to increase awareness about the true nature of this disease.
Fighting stigmas with lung cancer
When I was first diagnosed, I felt traumatized due to the prognosis and the complete shock that I was diagnosed with lung cancer. As a public health educator, our training was this disease was primarily linked to a history of heavy cigarette smoking.
Being a health and fitness professional, I asked myself why do I feel defensive, having to explain that anyone with lungs could get lung cancer and that I did not have a history of smoking? Many people did not believe me and questioned my integrity.
This hurt a lot, professionally and personally, and I remained quiet about my diagnosis to people outside of close family and friends. Today, I understand our lack of knowledge and empathy for lung cancer is directly related to public health education and messaging.
The impact of stigmas on research and treatments
Such a terrible stigma has hindered research funding. It’s completely unjustified, considering the tobacco industry was indicted for manipulating marketing and increasing levels of nicotine, making cigarette smoking highly addictive to young people when they are at an age of experimenting and exploring things they might not have as adults.
Not an easy addiction to break, so yes, many people cannot stop smoking. Does that mean they deserve to have a hideous and cruel disease and death sentence?
Having worked with the HIV/AIDS community in the early 1990s, I sat with dying patients, many of whom were discarded by their families because of the stigma associated with the diagnosis. How sad, horrible, and unfair. Did people with HIV/AIDS deserve this alienation, dreadful suffering, and death sentence?
I thought about how the community of survivors, caregivers, celebrities, athletes, and physicians humanized the disease by standing up and telling their stories. They received empathy and compassion. They had nothing to be ashamed of.

Without shame, there is no stigma. They showed the lives and families impacted behind the staggering statistics and demanded to be cared for through fierce advocacy. Funding increased dramatically, and research accelerated.
Today, HIV/AIDS is no longer a death sentence. It is a chronic, manageable disease, and people are living with a high quality of life.
Historically, this is what it has taken. It was the same for the breast cancer community. Women felt stigmatized, mutilated, and embarrassed.
The brave women who stood up over the years and brought about awareness through fierce advocacy, with the medical community supporting them, have achieved great success and high survival rates.
After I thought about this and having been disrespected and demoralized by the cancer centers that were supposed to be caring for me, I thought a way to tackle the stigma I was feeling was to stand up and scream through my white ribbon door hanger.
It would send the message that I was not ashamed to say I have lung cancer.
The White Ribbon Project

The genesis of the White Ribbon Project
In the spring of 2020, as a result of Zoom calls amid the pandemic, I partnered with my survivor friends, and we attempted to get some local hospitals to get more active in promoting Lung Cancer Awareness Month, which is November, just as they do for Breast Cancer Awareness Month, which is October.
We were largely ignored or dismissed with what we felt were patronizing and humiliating responses.
Since the cancer centers and hospitals were not going to promote Lung Cancer Awareness Month, out of frustration, I asked my husband, Pierre, if he could make me a large white ribbon. It is the symbol for lung cancer awareness, and I wanted to hang it on my own front door.
No permission required or red tape to deal with. I could take control and spread awareness literally from my front door. As he had just taken up woodworking, he was able to make me a 2-foot-long wooden white ribbon.




I could open the door to conversations and start educating others about lung cancer facts. I could try to increase general awareness about lung cancer and let other survivors know that they are not alone.
Suddenly, I felt I had some control and power back in my life. It feels good not to hide, not to be invisible and perpetuate the myths.
I can think of far worse things people can do in their lives than smoking cigarettes. Does this addiction truly warrant horrid pain and suffering to approximately 235,000 people every year and death to approximately 132,000 of them?
No shame, no stigma. Stand up and educate. It is up to us, the lung cancer community — survivors, caregivers, physicians, researchers, cancer centers, advocacy organizations — to stand together and break the stigma. We are worth it!
Social media attention of the White Ribbon Project
I subsequently put a photo of it on a private Facebook page for lung cancer survivors in Colorado. Almost immediately, people were asking us to make them for them.
We have been happy to do that, and the demand grew quickly.



International presence!
We now have White Ribbons across the country, in Canada, one in the Philippines, one in Germany, and one on the way to the Netherlands. We have made more than 500 of them. We have not been accepting any money for the ribbon or the shipping.
Tell us more about the White Ribbon Project mission
The White Ribbon Project ( The WRP) promotes awareness about lung cancer by changing public perception of the disease. Anyone with lungs can get lung cancer.
We want people to know that the White Ribbon Project ribbon is a symbol of lung cancer awareness and lets them know that they are not alone. They are loved, and there is a huge community of lung cancer survivors, caregivers, and advocates there for them.
Each ribbon is handmade by a survivor or someone who loves a survivor.
A lot of time and effort goes into crafting each ribbon. Our hope is that when a survivor receives their ribbon, they know that it was made for them with love and care, and they are worth it.
We have been inspired by many longstanding survivors and advocates, especially Chris Draft, former NFL football player, whose wife died of lung cancer in 2011. He has been one of the strongest supporters of the lung cancer community, along with his foundation.

What is your next goal?
Unify the disparate lung cancer communities by forming The WRP as a means to increase awareness. We plan to do this by sharing the white ribbons and the WRP logo with lung cancer advocacy groups, health care institutions, and other supporters.
We also aim to increase public recognition of the white ribbon as a lung cancer symbol. The White Ribbon Project is unbranded.
Encouraging others to share their lung cancer stories
Since the inception of the project, we continue to connect with people who were reluctant to share their diagnosis but are now excited to have a white ribbon and let others know they have lung cancer.
They have been posing for pictures in front of their cancer centers or their homes and posting them on social media.


Thanks to many strong survivor advocates, several comprehensive cancer centers and organizations are now displaying these ribbons, along with awareness and educational materials from LUNGevity, the GO2 Foundation for Lung Cancer, and the IASLC (International Association for the Study of Lung Cancer).
The white ribbons are currently on display at 24 NCI-Comprehensive Cancer Centers, 25 VA hospitals, 17 community cancer centers, and 7 lung cancer advocacy organizations.
Importance of other partnerships
Yes, partnerships with caregivers, other advocacy groups, pharma, genomic testing companies, lung cancer clinicians, primary care physicians, scientists, and cancer treatment centers are crucial.
We have already gotten great responses from these stakeholders, and many have accepted and are displaying the ribbons we have made for them. One primary care physician is taking the ribbon to base camp at Mt. Everest in April!
The Chris Draft Foundation, LUNGevity, The GO2 Foundation, and The City of Hope Comprehensive Cancer Center have all been very supportive of our efforts. Many other cancer centers, physicians, researchers, and social workers have all been very supportive of our efforts.



The modern faces of lung cancer
We are hopeful this is a step towards cracking the unfair stigma that has plagued this disease for decades. All these survivors are stepping out and showing the modern faces of lung cancer. This is giving hope to so many.
We see ourselves as the modern faces of lung cancer. We are unified. Whether we have a smoking history or not, a targeted mutation or not, we show that anyone with lungs can get lung cancer and that research matters.
Messages and images of hope instead of frightening stereotypes are starting conversations across the country.

The importance of people from all walks sharing their stories
It is important to share all stories of lung cancer. The world needs to understand that anyone with lungs can get lung cancer.
Any age, gender, race, religion, those with smoking histories, those who never smoked, those who have targetable mutations, those without mutations, those on immunotherapy, any stage of diagnosis.
Unification is necessary to have a loud voice that advocates for the same thing and that we all have different unique stories that need to be heard.
No one deserves any disease, lung cancer included.
Learn more about the White Ribbon Project by following on social media.

Inspired by Heidi's story?
Share your story, too!
Lung Cancer Stories for The White Ribbon Project
Luna O., Non-Small Cell Lung Cancer, ROS1+, Stage 4 (Metastatic)
Symptom: None involving the lungs; severe abdominal pain
Treatments: Chemotherapy, targeted therapy
Calvin M., Lung Cancer, Stage 1
Symptoms: Frequent illness (monthly cycles of sickness), breathing difficulties
Treatment: Surgery (pneumonectomy)
Jill F., Non-Small Cell Lung Cancer with EGFR Exon 19 Deletion, Stage 1A
Symptom: Nodule found during periodic scan
Treatments: Surgery, targeted therapy, radiation





One reply on “Heidi’s Stage 3A Non-Small Cell Lung Cancer Story”
Hello Heidi,
I hope I find you well.
I happened to see your “Patient Story” YT video and was impressed with your passion to advocate for cancer patients and felt compelled to share my wife’s cancer journey with you in hopes you find some of what we discovered along the way of interest.
My wife and I are in year 10 of her struggles with adv stage 4 met breast cancer (liver/lungs/lymph/bones/brain). She is currently, and has been for the last year, cancer free per CT/PET/Signatera genetic tests. Ten years of constant research and trying everything under the sun (conventional/alternative) without success as the cancer slowly advanced until we finally shifted our thinking about the nature of cancer and found a viable solution.
Very briefly, what we learned is that cancer is not primarily about the cancer cell. It is about a failure of the immune/gut microbiota systems and runaway cancer creation is the result. Cancer is a symptom of this failure and focusing only on eradicating the cancer cell with surgery/chemo/radiation is only treating the symptom and not getting to the root cause and thus the high recidivism rate.
Among our 50-100 trillion cells, some small % will go off the rails (altered metabolism) and become cancer. It is the immune/gut systems whose job it is to eliminate those cells before they progress out of control. It is virtually impossible to sustain life threatening levels of cancer creation if the immune/gut systems are working adequately. Interestingly, people who have AIDS (broken immune system) and succumb to the consequences of AIDS, predominantly die of cancer. Having cancer is not so different than having AIDS. There is now ample evidence of the effectiveness of the immune/gut systems in eradicating cancer if these systems can be repaired and directed to the cancer.
While immune drugs such as checkpoint inhibitors show some promise in aiding in resolving cancer, getting them to work fully, safely and consistently has been a challenge. Unfortunately most oncologists are not aware that the presence of specific gut bacteria can make all the difference in determining the effectiveness of these drugs.
Cell Reports Medicine
Volume 3, Issue 5, 17 May 2022, 100642
Journal home page for Cell Reports Medicine
Spotlight
Too much water drowned the miller: Akkermansia determines immunotherapy responses
https://www.sciencedirect.com/science/article/pii/S2666379122001677
Just as there can be many factors that cause a cell to alter its metabolism toward cancer (poor diet/stress/environmental toxins/pharma drugs/vax…..) those same factors can impair immune/gut function and set the stage for uncontrolled cancer progression.
Unfortunately mainstream medicine continues to focus most of its efforts on killing the cancer cells with various interventions, some of which (chemo), further impair immune/gut health pulling the patient further away from a long term solution.
In our evolving view, cancer is not about the cancer cell, it is about the immune/gut system. Any long term solution requires a major shift in focus.
All my best in your awareness efforts,
Mike