Embracing Life with Chronic Lymphocytic Leukemia (CLL): Serena’s Empowering Story
Serena shares her experience of living with chronic lymphocytic leukemia (CLL). At just 26, she started to experience strange and worrisome health issues, including severe leg cramps, ovarian cramps, strange knots on her body, hormonal acne, night sweats, and extreme fatigue. She first thought that these were signs of benign conditions like ovarian cysts or perhaps a blood clot. Despite feeling something was off, she had to deal with skepticism from healthcare professionals due to her youth, which only added to her distress.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
Seeking answers, Serena struggled with a convoluted healthcare journey that included financial burdens and dismissals due to her insurance struggles. After months of elevated white blood cell counts and persistent advocacy for herself, she finally went to The James Cancer Hospital and Solove Research Institute. Her diagnosis of CLL came unexpectedly and left her to process the emotional impact of having a treatable yet incurable disease.

Serena’s treatment approach, “watch and wait,” seemed strange at first but was necessary. Her medical team decided against immediate treatment, as early intervention does not extend the lifespan of CLL patients. Despite the idea of waiting for her condition to progress, Serena found comfort and strength in the support network provided by the hospital, which connected her with resources to ease her financial and emotional burdens.
Throughout her experience, Serena has remained proactive and optimistic. She had neck surgery to remove lymph nodes when faced with the possibility of Richter’s syndrome, a more aggressive lymphoma transformation. This successful surgery brought her relief and renewed hope.
Serena’s strength and resilience are deeply inspiring. Her advice to others about navigating cancer is to live life fully and focus on joy and self-advocacy. She now knows that it’s crucial to listen to your body and trust your instincts. Even though she isn’t currently on active treatment, she has still made herself part of the CLL community. By joining clinical trials, she also helps contribute to future treatments.
Watch Serena’s video and read this story to learn about:
- How she defies expectations by advocating for her health.
- The “watch and wait” approach to cancer treatment.
- Finding strength in community and support.
- Inspirational insights on living fully in the face of adversity.
- Groundbreaking highlights on CLL from the world’s largest gathering of blood cancer and disease experts.
- Name:
- Serena V.
- Age at Diagnosis:
- 26
- Diagnosis:
- Chronic Lymphocytic Leukemia (CLL)
- Symptoms:
- Night sweats
- Extreme fatigue
- Severe leg cramps
- Ovarian cramps
- Appearance of knots on body
- Hormonal acne
- Treatment:
- Surgery: lymphadenectomy


Thank you to AbbVie for supporting our patient education program. The Patient Story retains full editorial control over all content.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Focus on living. It’s way better than to focus on dying.
Introduction
Serena V.: Hi, I’m Serena. I live in Columbus, OH.
I have CLL, which is chronic lymphocytic leukemia.
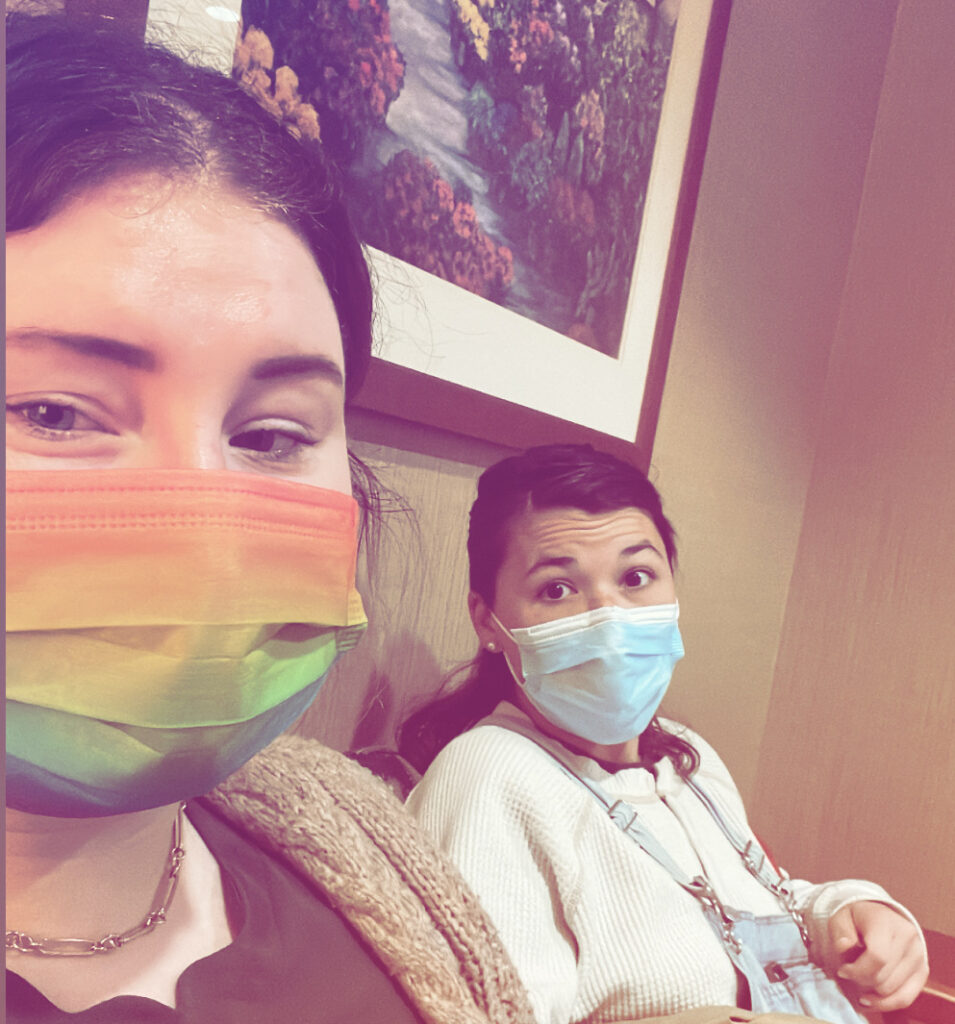
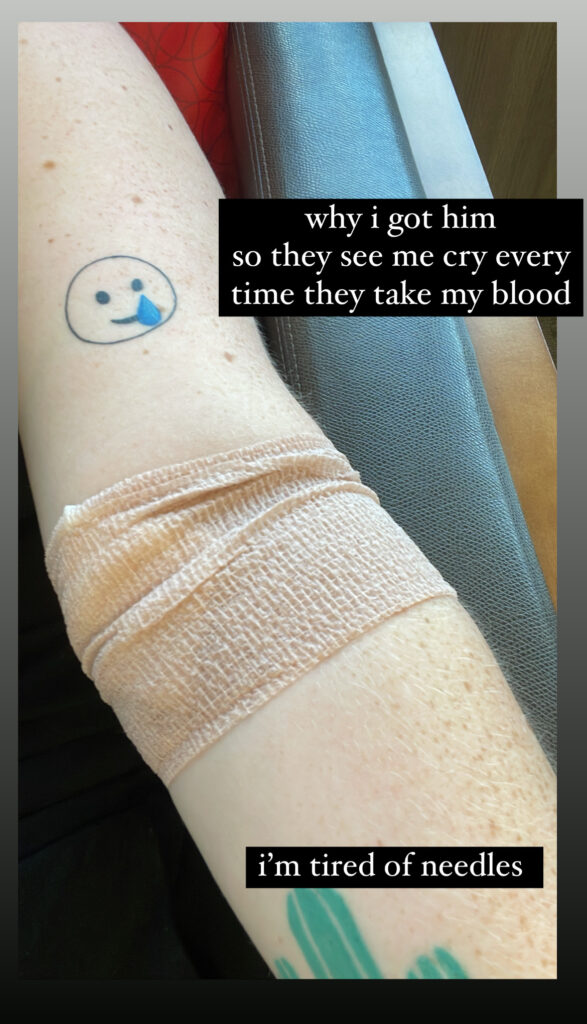
Before My Diagnosis
Serena V.: In the summer before I was diagnosed, I kept getting cramps in my legs and ovarian cramps, and I also kept getting these knots all over my body. My complexion was off, and although I didn’t realize it until later, I was also having horrible hormonal acne on my chin. I was in a lot of pain, too, and I was sleeping all the time and having night sweats. I thought I might have a cyst — a lot of friends had had ovarian cysts and things like that. I also wondered if I was getting a blood clot or something like that because of the knots. It all got me thinking: am I a hypochondriac?
So, I got medical help. The urgent care that I went to said that I might have some sort of mass or something internal and sent me to my gynecologist. But at the time, I didn’t have good insurance, so my gynecologist deferred me. I ended up having to go to the emergency room (ER) instead.
At the ER, they did an internal and external ultrasound, but it didn’t find anything wrong. The only thing the visit turned up was a slightly elevated white blood cell count. The ER then referred me to primary care, but I didn’t have one at the time. So we called a family friend who was a nurse practitioner. She found out that my white blood cell count was elevated, too.
All in all, it took six months for me to get referred to a cancer hospital because my white blood cell count just kept being elevated. I did have health insurance, but it didn’t really help me with my payments — for instance, I would get a $5,000 bill for the ER — and that stressed me out. And especially since I was just 26, people kept gaslighting me and doubting that I could be seriously ill. They would say, OK, there might be something off, but you’re fine. But I did know that something was wrong with my body. I mean, because of the cramps, I would be lying in bed all day with a heating pad because if I moved, I would be in awful pain.


So I didn’t really know what answers I was seeking, but I was afraid. I think what added to my fear was the fact that my brother had Hodgkin’s lymphoma at 22, and he had fortunately beat it, but it was still scary.
Even when I finally did end up going to a cancer hospital and seeing a hematologist, she literally told me that I was pretty healthy. A person only has a 2% chance of getting a blood cancer, and she told me that she thought I would be one of the 98% who wouldn’t get one. Plus, there’s a lot of uncertainty that comes with my age because most people who do get CLL are much older, and there’s just not much data about patients my age.
… since I was just 26, people kept gaslighting me and doubting that I could be seriously ill. They would say, OK, there might be something off, but you’re fine. But I did know that something was wrong with my body.
My CLL Diagnosis
Serena V.: So I was working at a career fair at a school and was driving back to my office, and I had to pull over because my doctor called all of a sudden. I thought, oh, she’s probably calling to tell me I’m fine. But she went, “Hey, Serena, we got your blood results back a day ago. However, I had my coworker double-check my work, which took an extra day. I’ve never seen this in my entire career.” And my stomach dropped.
The doctor said, “You have a disease called chronic lymphocytic leukemia or CLL.” And even now, I remember how I reacted at that moment. Your body doesn’t forget how you feel at a moment like that. My chest tightened up. And I asked her, “What is CLL?” And my next question was — “Am I going to die?”
She replied, “CLL is the most common type of leukemia. It’s treatable but incurable. But I will say that the average age of patients with CLL is 72.” I was so much younger than that.

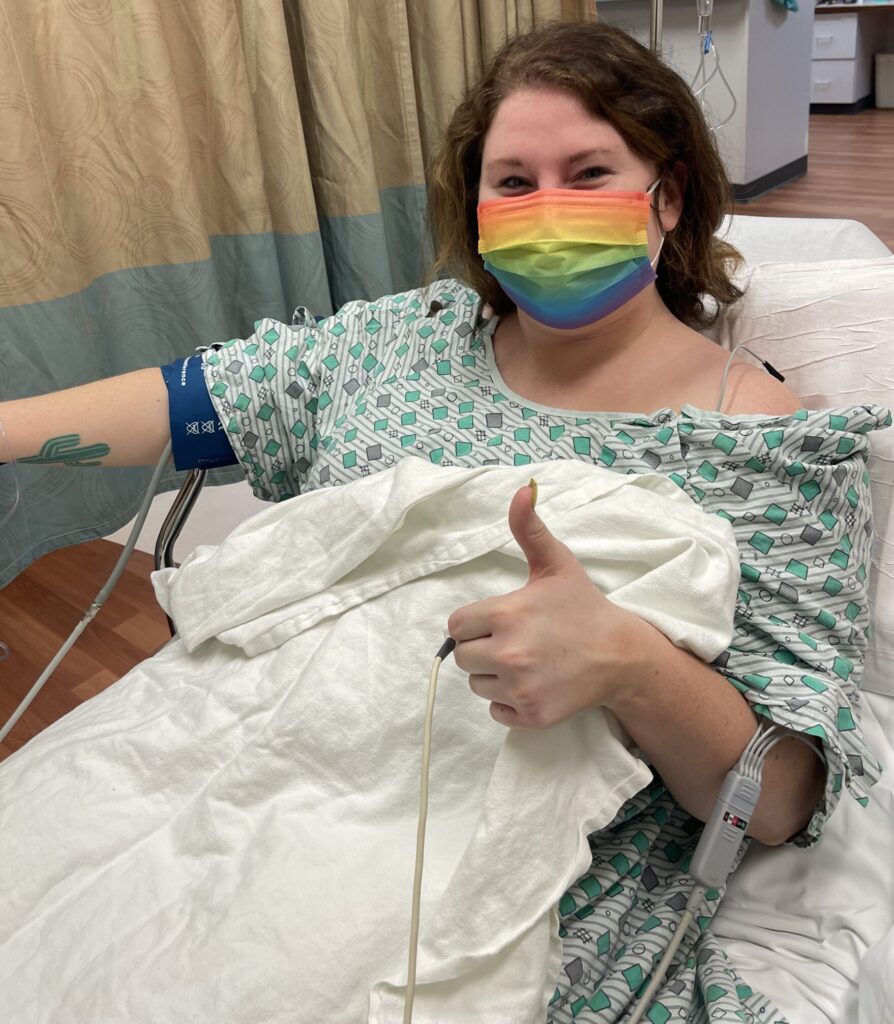
My Search for the Right Doctor and Treatment
Serena V.: I got transferred to The James Cancer Hospital and Solove Research Institute, where we took things forward. I was expecting to start chemotherapy right away because my other doctor said, “We’re probably going to have to start treatment soon because you’re young, and we don’t want your CLL to get worse.” But when I got to James, they found that my counts were great, and they also told me that for CLL, early treatment doesn’t help with the disease and doesn’t increase the longevity of CLL patients’ lives.
They told me, “We’re going to put you on watch and wait”, which is a treatment approach under which my doctors would watch my condition but not treat me just yet unless and until my condition changes for the worse.
I remember feeling like that was the weirdest thing, because not only was I diagnosed with incurable cancer, but my medical team and I would need to wait and watch for it to get worse before I would start getting treated. Moreover, I was still experiencing those debilitating symptoms. So I was quite anxious.
I was grateful, though, that in the first year of my treatment, I was able to go to James every three months, and they also gave me access to some incredible resources. For example, James linked me up with a young adult cancer social worker who helped me connect with The Leukemia & Lymphoma Society for grants — which was massive considering the financial stress I had been under from the start. And she also gave me some important “cancer 101” tips regarding how to prepare for my appointments.
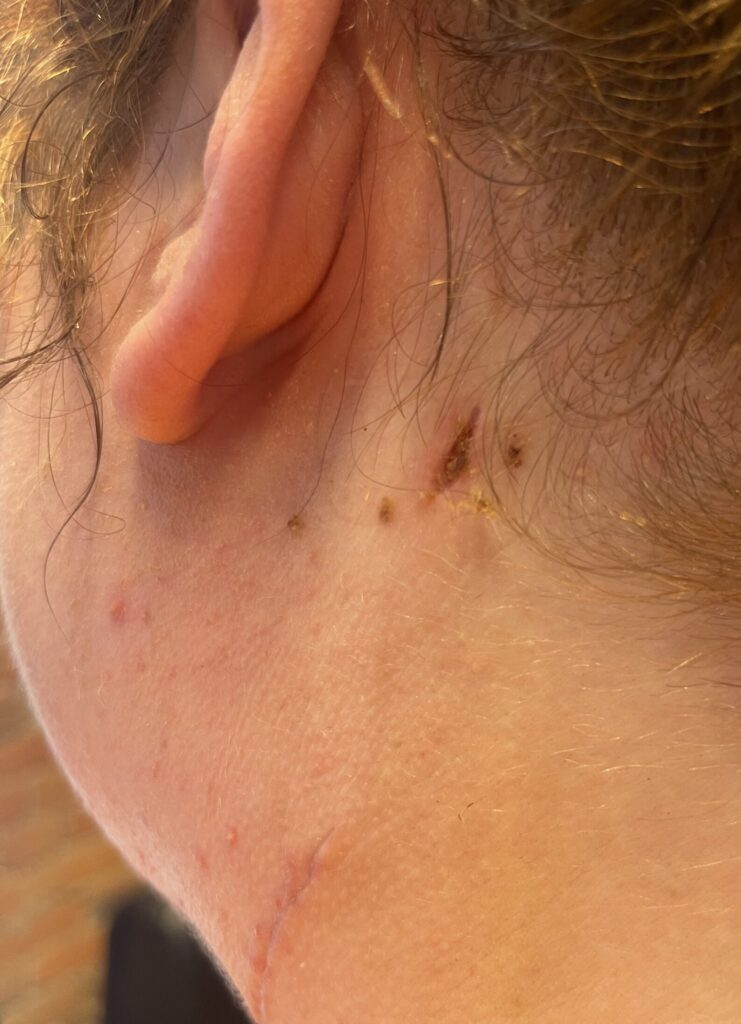
Overall, I’m optimistic. I think the science is really there, and my doctors are here for me — and they are optimistic about my lifespan.
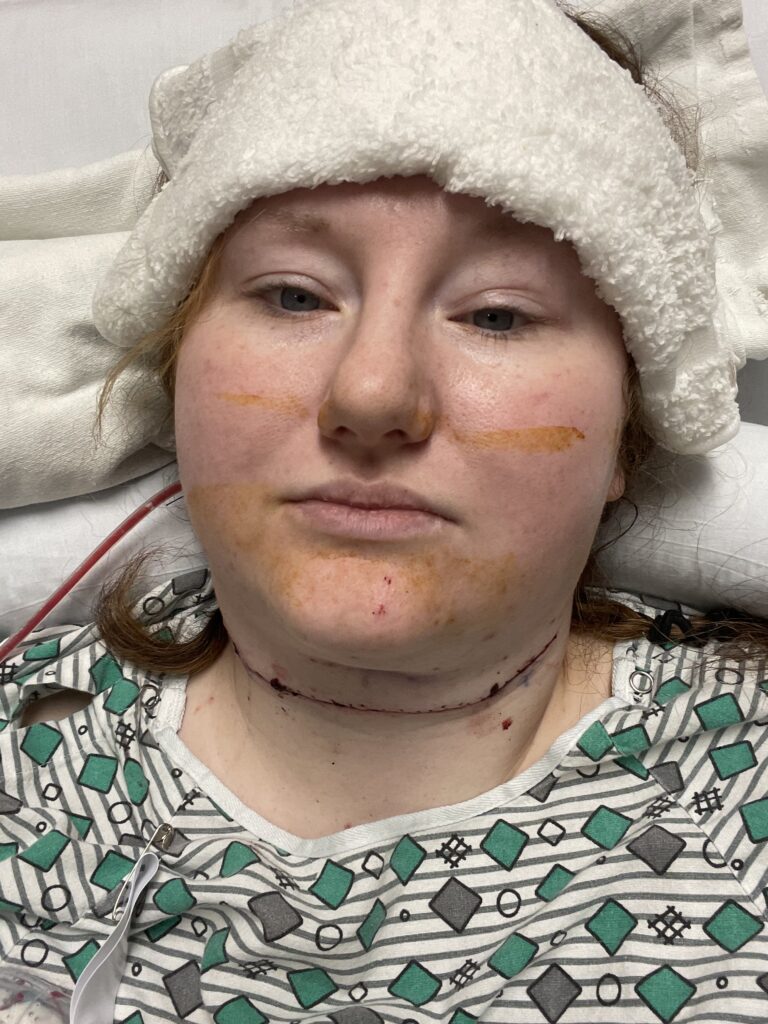
My Reaction
Serena V.: I had so many questions for the social worker and in general. Since I’m so young, will I need to be treated multiple times? What does treatment look like for me? What would remission mean for someone like me who has an incurable cancer when “remission” means that there’s no more cancer in your body? So, things like that confuse me sometimes. But I do find a lot of hope in going in this direction.
Last year, I had neck surgery to remove five lymph nodes because we thought I was transitioning into Richter’s syndrome, which is a rare complication of CLL in which it quickly transforms into a more aggressive form of lymphoma. That was a horrifying experience. I thought, “Oh, what does my future look like now?” I thought I was going to die. But the operation was successful. My hematologist, for instance, is extremely optimistic that I’m not going to need treatment for a while, especially after that surgery.
Overall, I’m optimistic. I think the science is really there, and my doctors are here for me — and they are optimistic about my lifespan. I did have that question for them, too: since I found out I had CLL at 26, will I die in 20 years or just five? Or will I live longer and die at 80? That’s a question that none of them can answer with any certainty, and of course, I can’t answer it either.
But what I found works is focusing on life, on what I have, on what I can do, and on what I’m in control of, instead of just focusing on the fear of death. Those fears and thoughts are obviously still present. But being able to focus on the good things and on what I already have has really helped me.

What I Think About Clinical Trials
Serena V.: I opted into Ohio State’s research when I was first diagnosed with CLL. They have a program that entails taking an extra tube or two of blood for research. I do think clinical trials are amazing. I was open to whatever I could find because I was desperate for a solution. I was thinking, “What’s going to help me? Are you guys going to do it for me?” It’s nerve-wracking because I’m putting all my eggs in one basket, so to speak. “Do you think this is going to make me better or will it make things worse?”
I do realize there is some uncertainty with clinical trials. It’s obviously a trial you’re undergoing. But you do have to have that trust in your doctors that it might be the right thing for you and your condition.
Serena’s CLL Story Continues Below
CLL Program Highlight
The ASH (American Society of Hematology) Annual Meeting is the world’s leading conference on blood cancers and disorders, like leukemia, lymphoma, and multiple myeloma where top doctors and researchers share the latest breakthroughs. The below program excerpt if from our recent discussion with CLL expert, Dr. Jeff Sharman on news that came out of that meeting that could impact CLL patients like Serena.
CLL patient advocate and long-time health journalist Andrew Schorr sat down with Dr. Sharman to break down the most important updates for you.

Insights on CLL Treatment Advances
Andrew Schorr: So, Jeff, I’ve been living for many years with CLL. Some people who will watch this program are newly diagnosed. I went through all the stages you go through, and I’m sure you see it every day in your practice. What is this? I’m really scared. I have a blood cancer. Will my life be shorter? Am I going to die anytime soon? Please, doctor, what do you have that’s effective to treat me? And if that doesn’t work, do you have something else? We’re going to get into all that, but just at a high level, Jeff, how do you feel for today’s patients?
Dr. Jeff Sharman: You know, Andrew, it’s a great question and I have a very large practice of CLL patients. I take care of about 400 CLL patients and meet each of them. For many of them, I’ve been their first doctor. That’s the nature of my practice. So, for a lot of folks I take care of, I’m their first contact with the medical system in terms of understanding CLL. And I think what you highlight is something I see time and time again, which is a very understandable fear patients come in with.
It’s very common, you say “leukemia” and you see their eyes widen, you see them sit up a little straighter, and what you recognize under there is just a great deal of distress that any cancer would cause.

That’s a really optimistic message that most patients aren’t going to pass away from their disease.
And I think that one of the things we do as a doctor is figuring out how to measure out and administer the unique medicine we give, which is the medicine of hope. And how do you communicate that to patients in the midst of some of the worst days of their lives where they’re like, oh my God, I’ve been diagnosed with cancer? And I do reference quite frequently; there’s a study done in the Italian group that showed that if you’re age 65 and above and have been diagnosed with chronic lymphocytic leukemia, they have demonstrated that you really can’t measure a statistical impact on survival, that most patients are going to outlive their diagnosis. And I think that’s a really optimistic message that most patients aren’t going to pass away from their disease. And my own experience bears that out. The number of patients that I can think of who die of complications of CLL is really a very small fraction even in my large CLL practice — only a small number, maybe two or three per year.

So, a lot of it is communicating that there’s a lot that we’ve got for you. And it’s not the traditional chemotherapy you used to have. We’ve got targeted agents, immunotherapy, and so forth.
Andrew: You already mentioned that sort of people aren’t going to need chemo. We’ve got this whole class of medicines, BTK inhibitors, and even new generations of that which we can talk about. So, first of all, the approved therapies. You have quite an arsenal now, where you can use drugs either by themselves or together, maybe for a bigger impact, right?

Dr. Sharman: Right. You know, I think the way I look at this is that there are three main classes of chronic lymphocytic leukemia drugs. You mentioned BTK inhibitors. I would add to that BCL-2 inhibitors, and then I would add immunotherapy to that.
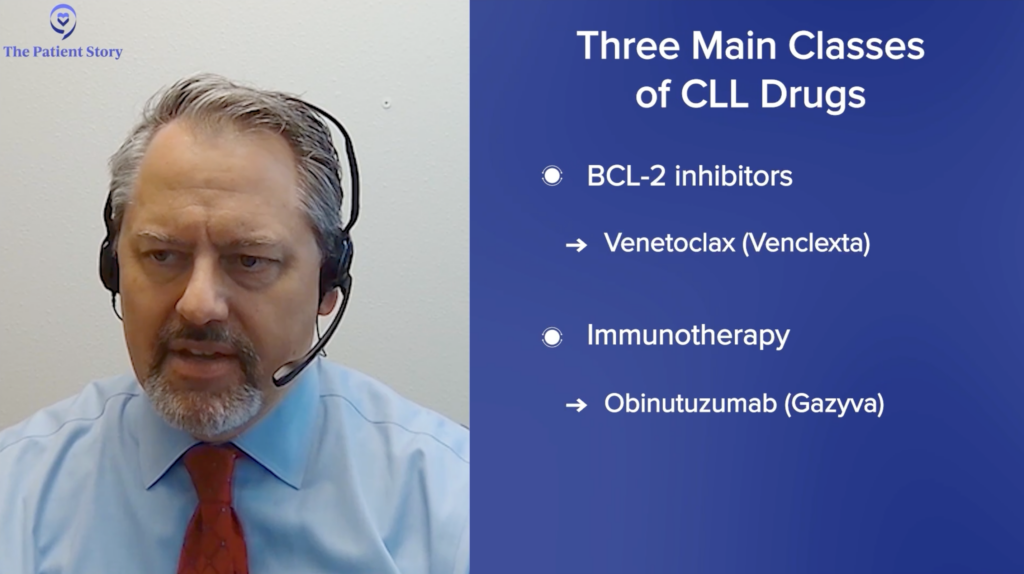
I think the status of the field right now is trying to figure out the best combination and the best sequence, and those are the big questions shaping the field right now. But the good news is, of course, these drugs are FDA-approved and they’re available to patients. So those are the kind of core questions.
Andrew: So, I’m sure there are patients listening, and their heads are spinning. And they’re saying, well, the different BTKs or a next-generation BTK, with or without venetoclax, with or without obinutuzumab. And I guess what I know is not all CLL patients are the same.
Dr. Sharman: Yeah.
Andrew: This is an individualized choice, right?
Dr. Sharman: Yeah, absolutely. Some patients take the physician’s perspective. Others are involved in their care and want to take an active part in the decision-making. I think that’s great. They should play an active role in it. And there are times when a patient might have their own preferences, but I may have different preferences based on how I’m thinking about their treatment. And sometimes, it’s a matter of calling to attention some of the potential side effects in a certain circumstance. Maybe somebody wants to do fixed duration, but their kidneys aren’t working too well any longer, or they’ve got a really bulky disease, or there could be various reasons why we might pick one over the other. Or even just how we think about, if we’re going to do this first, what do we do second? What’s going to be third? And if we’re going to pick this first, what’s the patient going to look like five to seven years from now when we might need to do the second therapy? So, you have to have a game plan in mind for somebody from the outset.
Andrew: Yeah, that is really well said. Now, I want to back up for a minute. We’ve got several questions from patients. One of them is like me. I said I went four and a half years without treatment. I felt pretty good. Then, I started to develop some lymph node issues, and my white blood count, fueled by lymphocytes, rose to about 283,000. My friend Dave is even higher than that. He hasn’t had treatment, and he feels fine. So, when should a new patient start treatment?

Dr. Sharman: So, for a chronic lymphocytic leukemia patient who’s climbing quite rapidly, what we talk about is the lymphocyte doubling time. Generally, when that number is going up more than twofold in less than six months, that’s our clue that we need to do something. But there are other reasons we might treat decide to somebody, such as bulky lymph nodes, if they start developing marrow dysfunction, if they’re getting anemic, or if their platelets are starting to go down — those can be reasons.
The one that does come up periodically is fatigue. Some patients have disabling fatigue. They might be 55 years old, they’re not depressed, their thyroid is fine, they’re not iron deficient, but they can only go to work for four hours before they have to come home.
So, disabling fatigue, that’s a reason to treat it, but these are all pretty well spelled out in what we call the iwCLL criteria. Rate of change, symptomatic bulky lymph nodes, marrow dysfunction, and others as well. Those are the reasons we treat patients.
… our therapies are just as effective for younger individuals than for older individuals, and in some cases, maybe even more effective for younger individuals.
Andrew: Some people on Facebook, for instance, are under 50 with chronic lymphocytic leukemia. And I know it’s not all that common, but there are people like that. And they say, well, is my age of diagnosis a bad thing? In other words, am I going to have a rougher time with CLL because I’m diagnosed younger? Would I not live as long? What do you tell a younger patient based on their age?

Dr. Sharman: Yeah, that’s a great question. I like to think of these patients in terms of having to plan not for the next 10 to 15 years but for the next 30 years. And I think that, to some degree, we celebrate that we have a lot of these new tools to control the disease. But I think it is a reasonable question to say, can you use these tools to control it for twice as long or three times as long as somebody who’s diagnosed, maybe at age 80? So, it requires a different game plan. And yes, our therapies are just as effective for younger individuals than for older individuals, and in some cases, maybe even more effective for younger individuals. But I think it does require some thoughtfulness to consider that we need to come up with something that’s going to keep this disease in control for quite a bit longer.
Now, the other thing is, this field is moving so fast that those tools that we’ll be using five to seven years from now may not even have been conceived of yet. And we don’t have a ton of time to talk about bispecific antibodies or other drug targets and so on. But to benefit those who are diagnosed younger, I think it’s fair to assume that there will be more tools in the tool shed down the road.
For the rest of this interview, watch our program replay ON DEMAND.
Learn what’s changing, how it impacts treatment decisions, and what it all means for patients today.
More on Serena:
… what I found works is focusing on life, on what I have, on what I can do, and on what I’m in control of, instead of just focusing on the fear of death.
My Life on Watch and Wait
Serena V.: How do I live on watch and wait? I just live. I live life as much as I can, and that’s the advice I can offer people facing chronic lymphocytic leukemia, or similar situations.
Find something that brings you joy and focus on that. Focusing on watching and waiting — well, it just makes you wait and watch. Even worse, it really makes you hyper fixate on your condition.
And, while you’re at it, listen to your body, too. If you’re feeling off, advocate for yourself with your doctor. In my case, I did realize that for the first year, I felt bad the whole time, and I wasn’t communicating this because I didn’t realize that some of what I was doing, like going home and napping so much, wasn’t normal.
I also realized that my fatigue was keeping me from spending time with family and friends. And later on, those were things that I was told to look out for as symptoms. But I didn’t process that something was actually wrong with me — and I was gaslit about my condition, too. And that’s how it was until I finally listened to my body and realized that something was wrong.
So I say, trust your body, find something that brings you joy, and focus on it. Focus on living. It’s way better than to focus on dying.



Special thanks again to AbbVie for supporting our patient education program. The Patient Story retains full editorial control over all content.

Inspired by Serena's story?
Share your story, too!
More Chronic Lymphocytic Leukemia (CLL) Stories
Lynn S., Chronic Lymphocytic Leukemia (CLL)
Symptom: Elevated white blood cell count
Treatments: Chemotherapy, targeted therapy (BTK inhibitor)
Serena V., Chronic Lymphocytic Leukemia (CLL)
Symptoms: Night sweats, extreme fatigue, severe leg cramps, ovarian cramps, appearance of knots on body, hormonal acne
Treatment: Surgery (lymphadenectomy)
Margie H., Chronic Lymphocytic Leukemia
Symptoms: Large lymph node in her neck, fatigue as the disease progressed
Treatment: Targeted therapy
Nicole B., Chronic Lymphocytic Leukemia
Symptoms: Extreme fatigue, night sweats, lumps on neck, rash, shortness of breath
Treatments: BCL-2 inhibitor, monoclonal antibody




One reply on “Serena’s Chronic Lymphocytic Leukemia (CLL) Story”
I was diagnosed with CLL at age 37 stage 0 found on routine pre-op labs. I’m now 66 & stage IV. I’ve had multiple treatments over the years including a clinical trial. Hang in there. Treatments are much better now than when I was diagnosed in 1997.