Nicole’s Myelodysplastic Syndrome & Acute Myeloid Leukemia Story
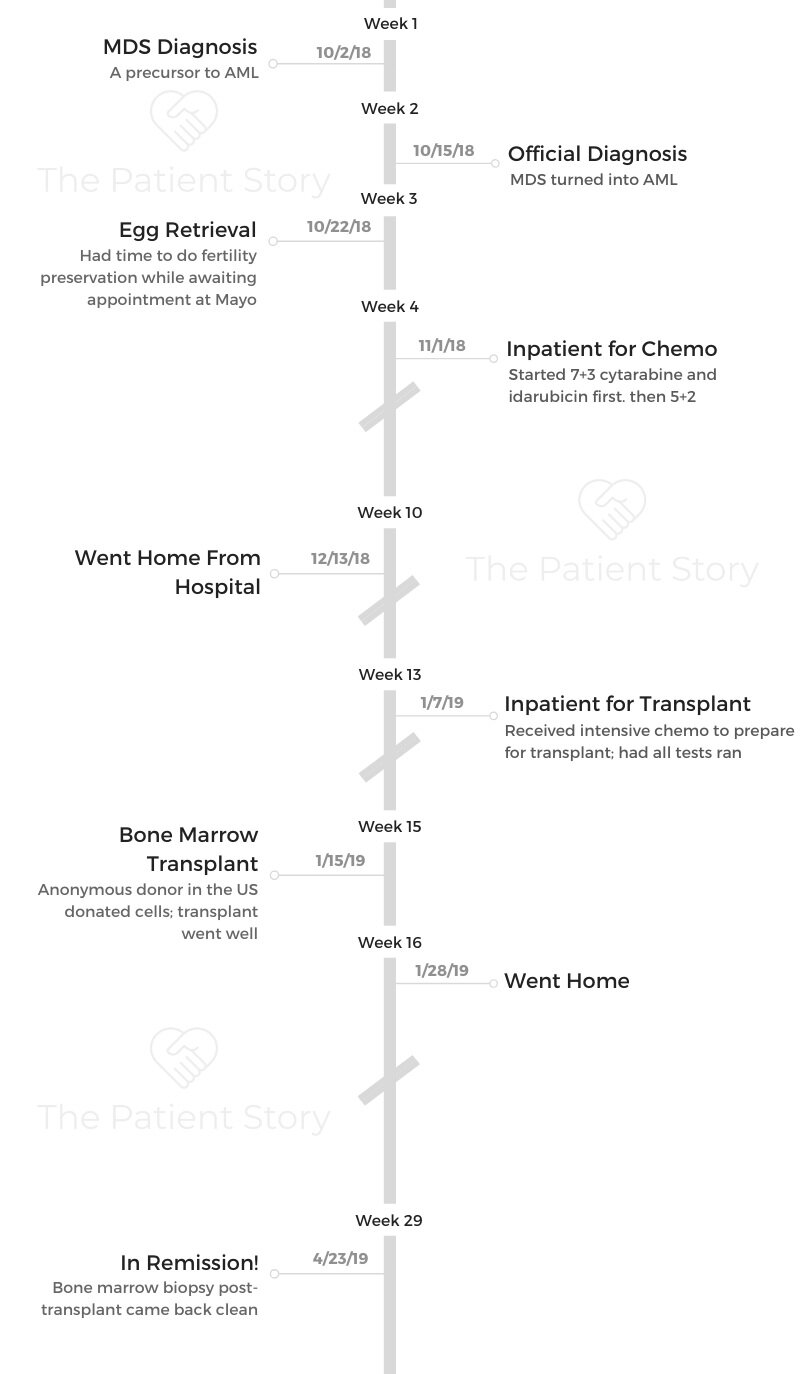
Nicole was diagnosed with myelodysplastic syndrome (MDS), a disorder when the bone marrow fails, stops making enough normal blood cells in the marrow, and sometimes turns into AML.
For her, it did. Nicole underwent chemo and a bone marrow transplant. She details the recovery from treatment, how cancer has changed her life perspective, and the support that helped most.

- Name: Nicole T.
- Diagnosis:
- MDS (Myelodysplastic syndrome)
- Rapidly turned into AML (acute myeloid leukemia)
- Staging: N/A
- 1st Symptoms:
- Severe itchiness
- Night sweats
- Fatigue
- Treatment:
- Chemotherapy
- Cytarabine & idarubicin
- 7+3
- 5+2
- Bone marrow transplant
- Cytarabine & idarubicin
- Chemotherapy
Talking about it with others is something I recommend. Stay positive. Having a good mindset and a can-do attitude really makes a difference in the fight.
Nicole T.
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Diagnosis
What were your first symptoms?
For about 8 months before getting diagnosed, I was itchy. When I would get out of the shower, I itched. I went to the dermatologist in February, and she said it was the changing of the seasons, and I probably had dry skin. May came, and I started itching at times other than just getting out of the shower.
This wasn’t like a bug bite itch. It was an internal itch. It felt like my legs and arms were crawling. It was so uncomfortable.
On June 3rd, I moved to Arizona. I moved 3 minutes from Mayo Clinic, actually. Within the first 3 weeks of moving here from LA, I noticed I had bruises up and down my legs. I had bruised easily my whole life, but this was so many. I thought that was weird, but I figured it was from moving.
I was also having night sweats. I never put it together, though, because I thought I was just adjusting to living in Arizona in the summer.
What made you seek medical treatment?
In about July, I was in LA visiting my mom. I woke up and was miserable and crying. We decided to go to urgent care and have some blood run.
They said my numbers weren’t perfect, but there wasn’t much to go on. They said my platelets were pretty low and I was anemic, but not iron deficient.
They gave me some steroids for the itching, and I tried those for 2 weeks. They didn’t work, and it was to the point where I was just crying all the time.
Getting misdiagnosed
In mid-August, I looked up an internal medicine doctor who took my insurance in Arizona. He basically told me he had seen something like this once before. It was all in the girl’s head, and it went away eventually. That was defeating.
He referred me to an allergist, and I didn’t have an allergy. He had been taking my blood every week, and he started to notice it was changing each week.
Another week or 2 went by, and he sent me to a hematologist. He said, “Don’t be afraid. She’s an oncologist.”
Path to figuring it out
It was the first week of September at this point. She ran all kinds of tests on me as well. She said nothing stood out as wrong with me, but obviously something was wrong with me. She said she was just going to have to start testing me for different things and use the process of elimination.
I started out having to give myself B12 shots every day. For a couple of days, I didn’t pay attention to the itching because of the energy spike from the B12.
At one point, I was headed to Europe for my brother’s wedding, and she had told me, “If you’re still itching really bad, let’s set up a bone marrow biopsy for when you get back to rule out the worst stuff.”
She told me in the worst-case scenario that maybe I could have Hodgkin’s lymphoma. She didn’t think I had that, though.
When I was in Italy, the fatigue hit me so hard. I was at my brother’s wedding. It was about 8 p.m., and I couldn’t even hardly keep my eyes open. No one could figure out what was wrong with me.
I had the bone marrow biopsy when I got home on a Thursday, and then I had a full PET scan the next day. On Monday, they called me and said, “She wants to see you tomorrow.”
I had started doing my own research, and I was already thinking I had leukemia. I knew something was wrong if an oncologist wanted to see me that quickly.
Getting the diagnosis
I remember walking into the room, and I started crying. She asked, “You know something’s wrong?” I said, “I do.”
That’s when she told me about the MDS. It’s basically pre-AML.
The best way someone explained it to me was, “When you get AML, it’s like somewhere along the way in your cells, bad cells came along and messed up the good ones. MDS is your body developing those bad cells.”
When it turns from MDS to AML, it can be really deadly, so they wanted to start me on treatment quickly.
»MORE: Patients share how they processed a cancer diagnosis
What were your next steps after diagnosis?
My dad called non-stop to Mayo to try and get me in there. I thought if I was going to be in Arizona, I might as well get treated at Mayo.
She had told me in that appointment that since I had MDS leading into AML, I was going to need a bone marrow transplant no matter what.
I wouldn’t be able to have children after doing that, so since we had to wait a week to get into Mayo, I went ahead and got scheduled with a fertility doctor to freeze my eggs.
Getting a second opinion with Mayo Clinic
I got an appointment with Mayo about a week later, and I saw my current oncologist. He wanted to do another biopsy so his pathologists could read it. I had 12% blasts when I had the first biopsy done, and within a few weeks, when I got this one done, I was at 23% blasts.
My oncologist gave me the choice between inpatient or outpatient, but he said it was best to just hit it hard inpatient.
I got my eggs retrieved about the 20th of October, and I moved into Mayo to start inpatient chemo on November 1st.
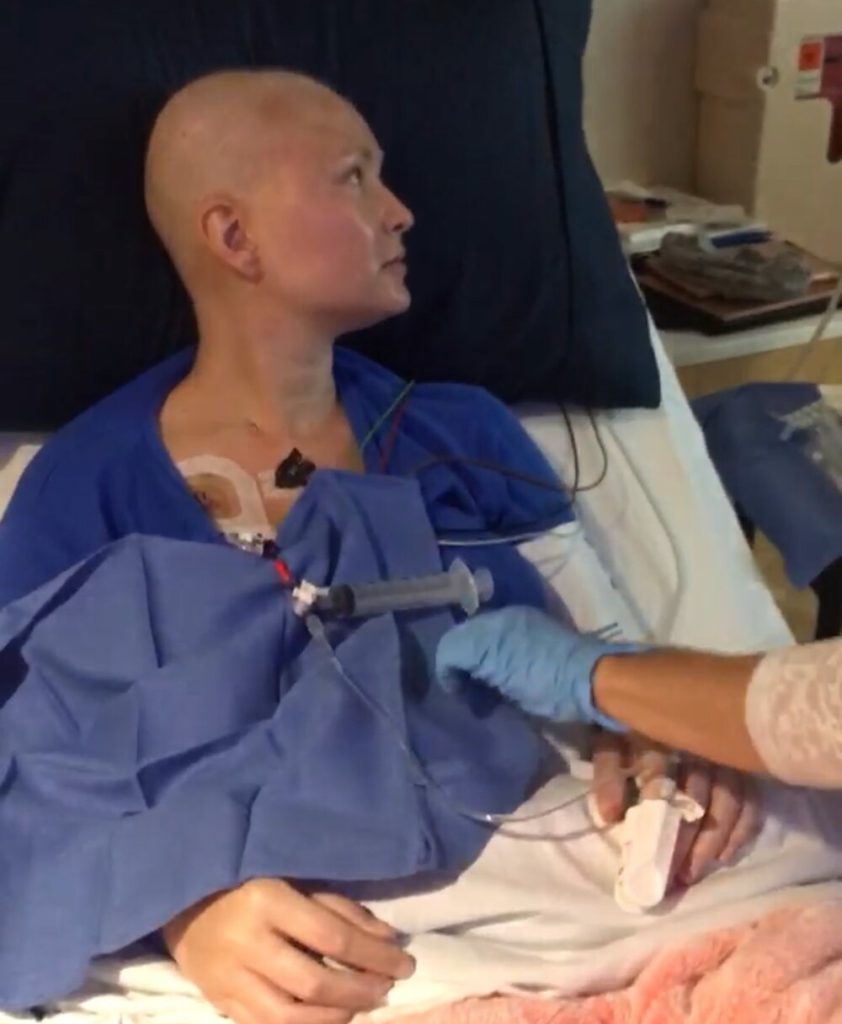
Chemotherapy
What was your chemo regimen?
I did 7+3 cytarabine and idarubicin first. For 7 days you’re on cytarabine, and then for 3 days you’re on both. I did that for a week, then I had to wait a week, and I got another biopsy to see if my blasts went down.
If they go down, you typically stay another 2 weeks to make sure your counts come up.
Unfortunately, my blasts went up. Then they put me on 5+2, which is the same thing. It’s just 5 days with 1 drug and 2 days with both. I was in the hospital for 6 weeks for the whole inpatient chemo experience.
What side effects did you experience from chemo?
As far as the side effects you would expect from chemo, I did pretty well.
I stayed on top of my Zofran. I never felt super nauseous. I wasn’t as tired as I thought I would be. For the first 3 weeks of my stay, I did pretty well. I was hanging out and playing games.
When I started the second round, which was the 5+2, I got my first fever. I got staph through my blood, so they had to pull my PICC line. I got a small brain bleed, I had fluid in my chest, and my heart went into failure. My ejection fraction tanked. Everything just went so far downhill in a week, and I’ve never been sicker in my life.
Because of the brain bleed, I had a spinal tap. They put chemo in my spine just in case it was in my brain. It was a crazy week. I recovered, though, and I went home for 3 or 4 weeks for Christmas and New Year’s.
»MORE: Read other cancer patient experiences with chemotherapy
Can you talk about hair loss?
My hair started falling out around week 3 or 4 during inpatient chemo. Once it did, it was getting in my food, and I just didn’t want to deal with it.
I knew I was going to lose it, so to me, prolonging it another couple weeks was silly. I had them shave it pretty early on. It grows so slow now.
Transplant
What was the preparation for transplant like?
I went back into the hospital to do extra chemo before transplant on January 7th, 2019. I had to get my line in my chest. I started on a different chemo. It was crazy strong.
As soon as the chemo started going in, the wallpaper was spinning. I never threw up, but I felt sick. I had diarrhea. It was awful.
Describe the bone marrow transplant
I had an anonymous donor. He lives in the U.S. and was a perfect match. The transplant is similar to a bag of blood. The cells are in the bag, almost like platelets.
Because things could escalate so quickly, your nurse is in your room with you all day. They’re checking your temperature, blood pressure, and everything every 15 minutes to make sure nothing is changing.
You just have to be hyperaware of what’s going on during that time. Other than that, you don’t normally feel anything. I got some terrible stomach pains really quickly after, and that’s kind of wild because usually you don’t have symptoms until about 5 days after.
What was recovery from the transplant like?
I had really bad stomach pain within a day after, and to this day, we still don’t know what that was about. The closest thing my nurses could compare it to was contractions. Any time I ate, drank, moved, someone touched me, or anything, my stomach was just going crazy.
It was really bad stomach pain. Nothing would make it go away. I just had to breathe through it. That was brutal.
I was also just really tired after the transplant. I didn’t really want to move. I also got mouth sores, awful diarrhea, and I never wanted to get out of bed. It was good that they made me, though.
I was discharged on day 11 after transplant. I guess I was doing super well. I came off IV meds, and the next day I went home.
How were you able to go home so quickly?
I guess my counts came up pretty quickly. I was able to go home because I lived only a couple of minutes away from the hospital. If you don’t, you have to stay in a lodge next to the hospital for 100 days or so post-transplant.
I would go every day for the first couple of weeks, and that frequency gradually decreased. For the first little while after transplant, though, I went in all the time to get things checked out.
I still needed platelets and blood. I needed magnesium a lot. I still spent a ton of time at the hospital. About a month after the transplant, I had the flu. It took me a full 5 weeks to get rid of it because I had no immune system.
I also had some really bad pain in my feet. I couldn’t walk hardly. They gave me steroids for about a week, and that went away. I’ve never had that since.
One of the worst things I experienced in recovery was my body just burned from the inside out. My private area, armpits, my stomach, and everywhere, my skin turned dark, peeled off, and just went through a burning process. I lost all my nails. I’ve lost my eyelashes several times now.
I’d say it took me about 4.5 months to start to get to a turning point. I put myself in physical therapy, and that’s when things started getting better.
Results after transplant
My first biopsy after transplant showed I didn’t have any disease. You can’t do a transplant unless you’re in remission or at least almost in remission.
Technically, the first time I was ever in remission was before transplant, but we count it as the first biopsy after the transplant. In April, after the transplant, I had 100% donor cells and no evidence of disease. All of my biopsies since have shown good news.

Reflections
How does it feel to be done with treatment?
I look at life so much differently, and I’m much happier now. I just feel like I’m never going to be fully done with it, though. I still see my doctor once a month. I still get blood drawn once a month. I just had my last round of shots.
I had a bone scan recently, and I have osteoporosis as a result of everything now. I’m getting set up to get an infusion once a year for that. It’s nice to be cancer-free, but with leukemia, it’s like it just takes years to be actually over.
How has cancer changed your life perspective?
I definitely do everything I can possibly do now. I don’t let little things bother me anymore. I’m always happy. People make comments about how positive I am.
I probably shouldn’t have lived through everything I lived through, and I know that, so having a second chance at life is amazing.
I want to do everything I can possibly do and experience, and I want to live a happy life. Life is just too short not to.
How were people able to show their support for you?
Honestly, just sending a text message saying they were thinking of me meant the world to me. When the situation is flipped, I have a hard time finding what to say to people, but when you are in the situation, anything is nice.
I did also love the care packages I received. They always got me super excited when my family brought them to me in the hospital.
What was your lowest point mentally and emotionally, and how did you get through it?
The 2 hardest times for me were being diagnosed and not knowing what would come of that. The worst was around 3 to 6 months after the transplant when all I wanted was to feel normal, have energy, and get back to normal life.
When I was going through treatment, I had the attitude that I just had to do this, and I pushed myself. I never really did the whole “why me?” questioning thing. I stayed really strong throughout, and I knew I would fight it one way or another.
Any advice for someone who has just been diagnosed?
A lot of people say don’t read online, but joining support groups on Facebook helped me a lot. I learned a lot there about what to expect, and I met a lot of people going through the same stuff as me. Also, being fully open helped me tremendously. Talking about it with others is something I recommend.
Stay positive. Having a good mindset and a can-do attitude really makes a difference in the fight.


Inspired by Nicole’s story?
Share your story, too!
Acute Myeloid Leukemia Stories
Russ D., Acute Myelomonocytic Leukemia (AMML), with NPM1 Mutation
Symptoms:Flu‑like symptoms, profound fatigue, blood pressure drop, shortness of breath
Treatments:Chemotherapy, clinical trial (menin inhibitor)
Shelley G., Acute Myeloid Leukemia (AML) with NPM1 Mutation
Symptoms: Fatigue, rapid heartbeat, shortness of breath, low blood counts
Treatments: Chemotherapy, clinical trial, stem cell transplant
Joseph A., Acute Myeloid Leukemia (AML)
Symptoms: Suspicious leg fatigue while cycling, chest pains due to blood clot in lung
Treatments: Chemotherapy, clinical trial (targeted therapy, menin inhibitor), stem cell transplant
Mackenzie P., Acute Myeloid Leukemia (AML)
Symptoms: Shortness of breath, passing out, getting sick easily, bleeding and bruising quickly
Treatments: Chemotherapy (induction and maintenance chemotherapy), stem cell transplant, clinical trials







Leave a Reply