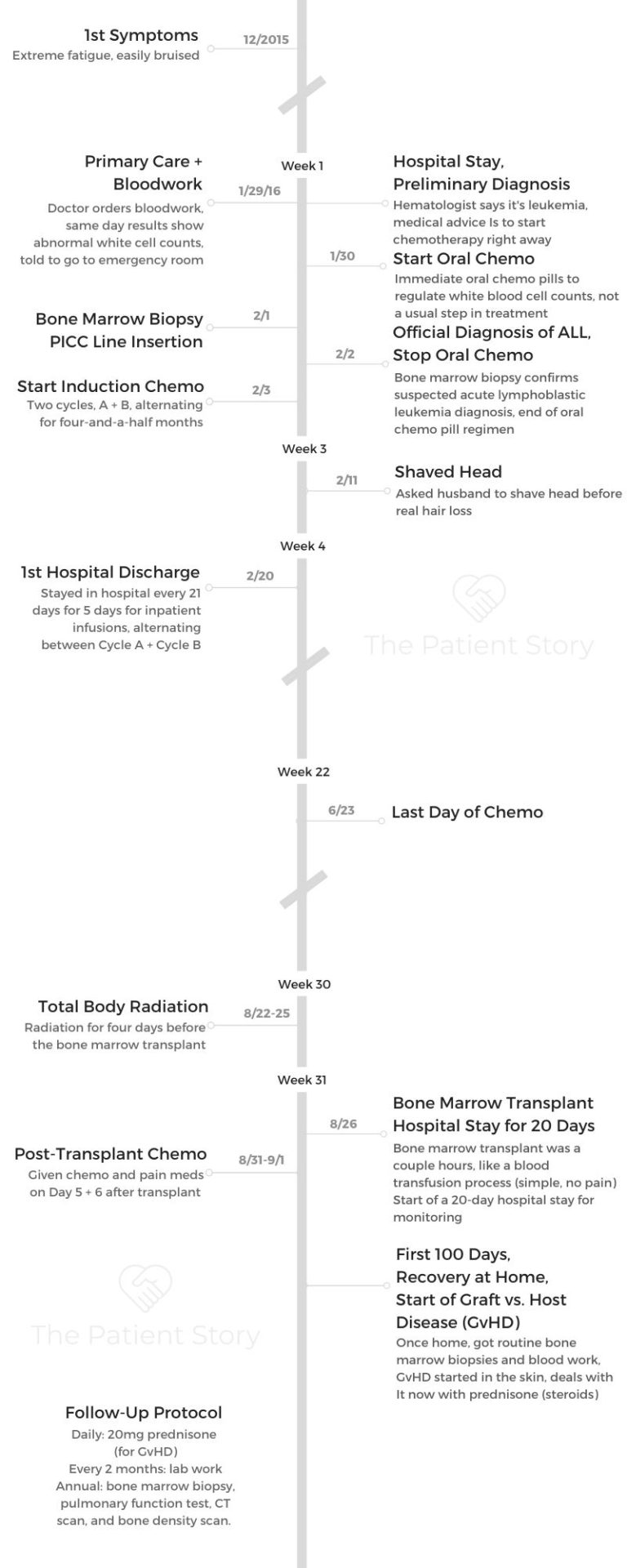
Lauren’s Acute Lymphoblastic Leukemia Story
Lauren was diagnosed with acute lymphoblastic leukemia (ALL) at 26 years old. In her story, she talks about undergoing chemotherapy, radiation, and a bone marrow transplant.
Lauren also highlights recovery from treatment and how the leukemia diagnosis impacted her relationships.

- Name: Lauren J.
- Diagnosis
- Acute lymphoblastic leukemia (ALL)
- Age at Diagnosis: 26
- Symptoms:
- Extreme fatigue
- Easily bruised
- Treatments:
- Chemotherapy pills
- Chemotherapy infusions
- Spinal taps
- Total body radiation
- Bone marrow transplant
Remain positive, remain strong. Fight it. Don’t let it get the best of you. Fight it with every inch and ounce of being. Fight it.
Don’t lay down. Don’t let it take your happiness, your joy. You’ve got to fight.
Lauren J.
- Diagnosis
- What were your first symptoms?
- What happened at the first doctor appointment?
- Describe the call from the doctor
- What happened at the emergency department?
- How did you process the diagnosis?
- Discussing abnormally high white blood cell count
- Staying at the hospital immediately
- Figuring out what to do with the kids
- Diagnosed with cancer so young
- Starting treatment right away
- Getting some perspective on the diagnosis
- Relying on family for all support
- How did you break the news to loved ones?
- Do you have any tips on sharing the news of a diagnosis?
- Treatment Decisions
- Deciding on an oncologist
- How did the hematologist describe your treatment plan?
- The oral chemo is not typically part of the treatment plan
- Cycle A and Cycle B of chemo
- Shaving your head
- How did it feel shaving your head?
- Getting a bone marrow biopsy to get your specific diagnosis
- Describe the bone marrow biopsy
- Advice on getting through the bone marrow biopsy
- Getting a CT scan
- Why did you get a PICC Line ?
- The PICC line mini-surgery
- Chemotherapy
- Bone Marrow Transplant
- Needing a match for a bone marrow transplant
- Preparing for the bone marrow transplant (BMT)
- Getting radiation before the transplant
- Radiation side effects
- Bone marrow transplant the next day
- Waking up from the BMT
- Recovering in the hospital
- The first 100 days
- Describe the recovery at home
- Monitoring post-transplant
- Graft-versus-Host Disease (GVHD)
- Reflections
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Diagnosis
What were your first symptoms?
My first symptom was fatigue, followed by bruising. Lots of bruising. Started with simple bruising. I would touch my skin, and a bruise would pop up. It would look like somebody beat me up.
Started there, and I kept writing it off. “Maybe it’s stress.” My job at the time was very stressful. I work in the medical field, so it was very stressful at the time. I just wrote it off as that.
Shortly after about a week and a half, my mom finally told me, “This is not normal. You should not be bruising like this from stress. Something’s not right.”
She really pushed for me to get that first doctor’s appointment, which is when I pretty much found out everything.
What happened at the first doctor appointment?
Went to the doctor for the appointment on a Friday afternoon. The doctor thought everything was fine. He said, “It really could be stress and everything going on with your job. I want you to go home. Relax with your kids. It’s going to be nice weather this weekend. But before you go, I want to get some extra lab work. I want to cover all my bases.”
He drew a few more labs before I left. I went home, got my kids from daycare, and we were hanging out. Then about 6 p.m. I got a call.
I knew something was wrong because the doctor was calling me personally at 6 o’clock on a Friday. That’s never good.
Describe the call from the doctor
That call came down to say, “Hey, I need you to get to the emergency room immediately.” My response was, “Okay, you say the nearest emergency room quickly. Do you want me to go to your facility at Emory, or do you want me to go to the nearest hospital?”
He said, “I’d prefer Emory. I’m going to call the ER and let them know you’re on your way. Your white blood count is extremely high. Matter of fact, it’s the highest I’ve ever seen.”
I was like, “Okay.” At that point just freaking out, thinking in my head, “Maybe it’s just sepsis.” About 3 weeks before that, I felt like I had strep throat, and my doctor I worked for prescribed me medication for it. I took it, and it was gone for a while. It wasn’t hurting again or anything like that, so I was like, “Okay, that was strep throat.”
In my head I thought I should have had more medication. I took all the medication he gave me, but maybe I didn’t take enough. I’m severely infected if my white count is that high.
What happened at the emergency department?
I immediately dropped off my kids with my mom and went to the hospital. I got to the hospital, checked in, and sat there. There was no urgency at that moment.
I think I sat in the waiting room for about an hour and a half. Then they called me back to the triage area, but they didn’t do any vitals or anything like that, which I thought was funny.
Immediately, a doctor walked in, so I was like, “Okay, what’s happening?” The first thing he said to me was, “Wow, you look fine.” I’m like, “What’s supposed to be wrong with me?” The next thing he said was, “I’ve already consulted Hematology-Oncology.”
As soon as he said that, I was like, ‘Wait, oncology? I have cancer?’
He was like, “Oh, you didn’t know?’
I’m like, ‘No! I did not know!’
It was quite shocking at that moment.

How did you process the diagnosis?
I really think at that moment I was still in shock because I was actually sitting there in the triage room, playing on a tablet. I remember playing games on the tablet when he came in, so when he said it and then when he said, “You didn’t know?”
Me: “No, I didn’t know.”
Doctor: “Is there anyone here with you?”
Me: “Yeah, but I feel like they probably should have been sitting next to me when you told me, because now I just want to fall out.”
Doctor: “Who’s here?”
Me: “My husband is here.”
Doctor: “Okay, go ahead and grab him.”
The doctor walked out of the room, and my husband walked into the room. He’s like, “What’s going on?”
I said, “He just told me I have cancer.”
He’s like, “What?!”
I was like, “Yes, he told me he consulted Hematology-Oncology and a doctor would be here shortly.”
He was a lot more shocked than I was. He sunk down in the chair. I was looking like I didn’t know what just happened. I literally went from being pretty much healthy 3 hours ago to now someone telling me I have cancer.
»MORE: Patients share how they processed a cancer diagnosis
Discussing abnormally high white blood cell count
Then the hematologist comes in, and he says the same thing: “For your current white blood cell count, you look amazing. I would expect you to look very weak or even possibly be in a coma.”
That was quite shocking. I asked, “What kind of cancer is it?” He said it was leukemia. I asked, “How do you get that? Is it something I did?”
The hematologist said, “No, it has nothing to do with your lifestyle.”
He asked a lot of lifestyle questions like, “Do you smoke? Do you drink?”
I said, “No, I don’t smoke. I drink wine. If I do, I might go get Mexican and have some margaritas, but I’m not a lush. I’m not drinking all the time.”
He said this is one of those [cancers] where we can’t pinpoint where it came from.
Staying at the hospital immediately
I remember him asking me if I had any questions. I said, “Yes, what are the next steps? Do I go home?”
He said, “Oh no, your white count is way too high. We are not sending you home. You will be staying here and start on chemo pills.”
Just started rambling through stuff. I’m like, ‘Oh my gosh, this is real. This is real.’

Figuring out what to do with the kids
I have a daughter and a son. At that time, my daughter was 4, and my son was 2. That was over everything.
At the time, I was like, “I didn’t even bring clothes! You’ve gotta let me go home and be inpatient on Monday. You can’t keep me here. I just got here. I have no clothes, no toiletry bags. I didn’t get to say bye to my kids. I didn’t kiss them. Who’s going to watch my kids?”
All of that was what was on my mind, not, ‘Let’s go ahead and get started.’ That’s life, being a mother.
»MORE: Parents describe how they handled cancer with their kids
Diagnosed with cancer so young
At the time, I had just turned 26. My birthday is on January 12. I got diagnosed on January 30. They didn’t know exactly what type of leukemia I had, but I got diagnosed when I had just turned 26.
Starting treatment right away
They did tell me I would have no option. Unless I went AMA (against medical advice), I had to stay. We had to start the treatment.
He told me, “Your levels were extremely high, so high that if you had not jumped on this, I would have given you maybe a week before your organs started to fail.”
That’s when it kicked in for me, and I was like, ‘Okay, yes, this is serious. Forget everything else. I have to get started because I have to live for my kids. I don’t want to go home and have something happen to me, so we just have to go ahead and get started.’
They took me to a room and told me I was going to be in one of the overflow rooms until they could get a room for me on the leukemia floor.
We went there. I got in. They got me in a gown. From the time I got into that room, I was in there for maybe an hour or hour and a half, and the nurse was coming in with chemo pills.
I was like, “Oh, we start this tonight, like now.”
She’s like, “Yes, ma’am, here are the orders,” and starts going through telling me everything I have to take and how they might make me feel.
I was like, “This is crazy!” I did take everything I needed to take. I think at that point is when it finally hit me, and I kind of broke down. I had a whole meltdown at that point. It’s like, “This is real. I just took chemo pills. I have cancer.”
Getting some perspective on the diagnosis
At that time, I was actually working for an oncologist. It was awkward because we treat cancer all day, and now I have cancer. I remember sending him a text message. It was probably about 1 or 2 in the morning.
I texted my doctor I worked for and said, “This is crazy. I know you know I left work early to go to the doctor. I am currently in the hospital and have been diagnosed with leukemia.”
He immediately called me and was like, “Lauren, what?” I’m still thinking about everyone else, like “Why are you up at 2 in the morning?” He’s like, “I was getting coffee on my way to work, and you sent me that, so I had to call you.”
I started telling him everything, explaining everything to him. He said, “Don’t worry. I’m going to be blunt. If you had to get cancer, this is one of the best cancers to probably get at this point. If you were going to get it, now is the best time to get it, under 30. Your treatment is going to be pretty rough, but you’re in good health. You can fight it. You’re going to be okay. You’re going to get through this.”
That was what was reassuring for me because he was in the field. He’s seen a lot. That’s what he has done for the last 15 to 16 years, so to hear that from him helped me stay positive in that moment.
Okay, you’re going to get through this. You just have to fight it. He definitely changed the outlook of the whole situation.

Relying on family for all support
My husband stayed for a little while, until the next morning about 5 a.m. Then he left to go home, get the kids, and actually had to go to work. He didn’t work at home at the time, so he worked away and did a lot of traveling.
He was already scheduled to leave that next morning when all of this happened. He got the kids settled. My mom ended up coming to the hospital. My mom actually worked at the hospital where I was diagnosed.
It was convenient, but she was there pretty much on and off all weekend because my husband couldn’t be there. My kids stayed between my aunt and my grandparents at the time while my mom was at the hospital. That was an adjustment because I was used to always being with my babies.
How did you break the news to loved ones?
I didn’t. My mom did. I couldn’t do it. She pretty much told everybody in my family. My family’s pretty close knit, so you’re going to tell one person, and they’re going to tell everybody else. My immediate family knew from my mom, so pretty much from a direct source.
[For] everybody else, I started a Facebook page that was named “Fight Like a Girl.” It followed my entire journey, and that’s how everybody else found out I was diagnosed and how everybody followed my chemo treatment. My feelings, emotionally, physically — the whole journey was there for the world to see.
Do you have any tips on sharing the news of a diagnosis?
Do it in your own way. There’s no correct way to break the news.
There’s no balloons going off. A lot of people may not want to share the news. It may be something they want to deal with privately. You just have to do it in your own way.
For me, I was already into social media a lot. I was on Facebook a lot, on Instagram a lot. To me, it was okay for coworkers and everyone else who were calling and texting to let them know, “I’m not ignoring you, but right now I’m kind of going through something. Here’s what I’m going through so you all will know.”
It was easier for my extended family to keep up with me that way, even my kids’ teachers and things like that. The schools were doing things for me, sending me things, and it was just easier for everybody to keep up with me just through social media.
People may not want to do that. It may not be their thing; they don’t want the entire world to know their business. You just have to speak your truth in your own way.
Do it how you want to do it. If you don’t want people to know, that’s okay, too. The world doesn’t need to know you have cancer if you don’t want them to know.
»MORE: Breaking the news of a diagnosis to loved ones

Treatment Decisions
Deciding on an oncologist
The doctor I worked for already knew the top doctor that treated leukemia. He asked me, “Who’s your doctor?” I told him who my doctor was.
He said, “Nope, you’re going to have another doctor.” I said, “Okay.” He said, “You got who was on call at the ER. It’s not who I want you to see. I need you to see the best. I need you to be okay.”
I said okay and switched doctors on me. That doctor was actually on vacation when I got diagnosed, so I was seeing the nurse practitioners and physician’s assistant until he came back. They were the best. They were super thorough.
I will forever be grateful for them.
They were the ones who actually told me, “This is the treatment plan. This is what we’re going to do,” along with the doctor who also diagnosed me because he was around that weekend.
How did the hematologist describe your treatment plan?
He told me what the next steps were going to be. He told me about the induction phase and how I was going to have to be in the hospital anywhere from 27 to 33 days. That kind of took me over the edge. I was like, “I can’t be in the hospital that long! I have kids; I have to go home.”
He was like, “No, but you won’t be able to be with your kids if we don’t get this done. We want you to continue to be around for your kids for a long time.”
At that point, he started telling me about all the different chemotherapy drugs I was going to have to take. I was going to have to do 2 cycles of things, but first we needed to get through the induction and go through the first few days of the pills.
He explained to me my white blood count was so high that if they started intravenous therapy, they were afraid that the cells would disperse, literally go to my lungs, and cause me to die.
They wanted me to start on the pills first so that we could get the number of cells down before we started intravenous therapy.
The oral chemo is not typically part of the treatment plan
That was before the induction. Everybody doesn’t need to do the pills. From what I was told, it was just because my count was so high that they could not start with intravenous. They didn’t want me to have those possible side effects from starting intravenous because my white blood count levels were so high.
They wanted to start me on the pills to at least wean down those white cell counts until there was a safe level. I was on the pills for the first 5 days before we started doing anything intravenously.
Cycle A and Cycle B of chemo
After that, everything was pretty much intravenous at that point. I wanted to forget those drugs that I had to get for chemo.
They explained there would be Cycle A and Cycle B.
Cycle A, I would have to come in once after this induction phase. I’d have to come to the hospital every month for 4 to 5 days to get all of these drugs.
For the induction phase, it started off with chemo every day being inpatient. They explained I was going to be super weak. I was going to be nauseous. Then after the first week of my intravenous therapy, they started explaining the drug they were starting the second week was what was going to take my hair out.
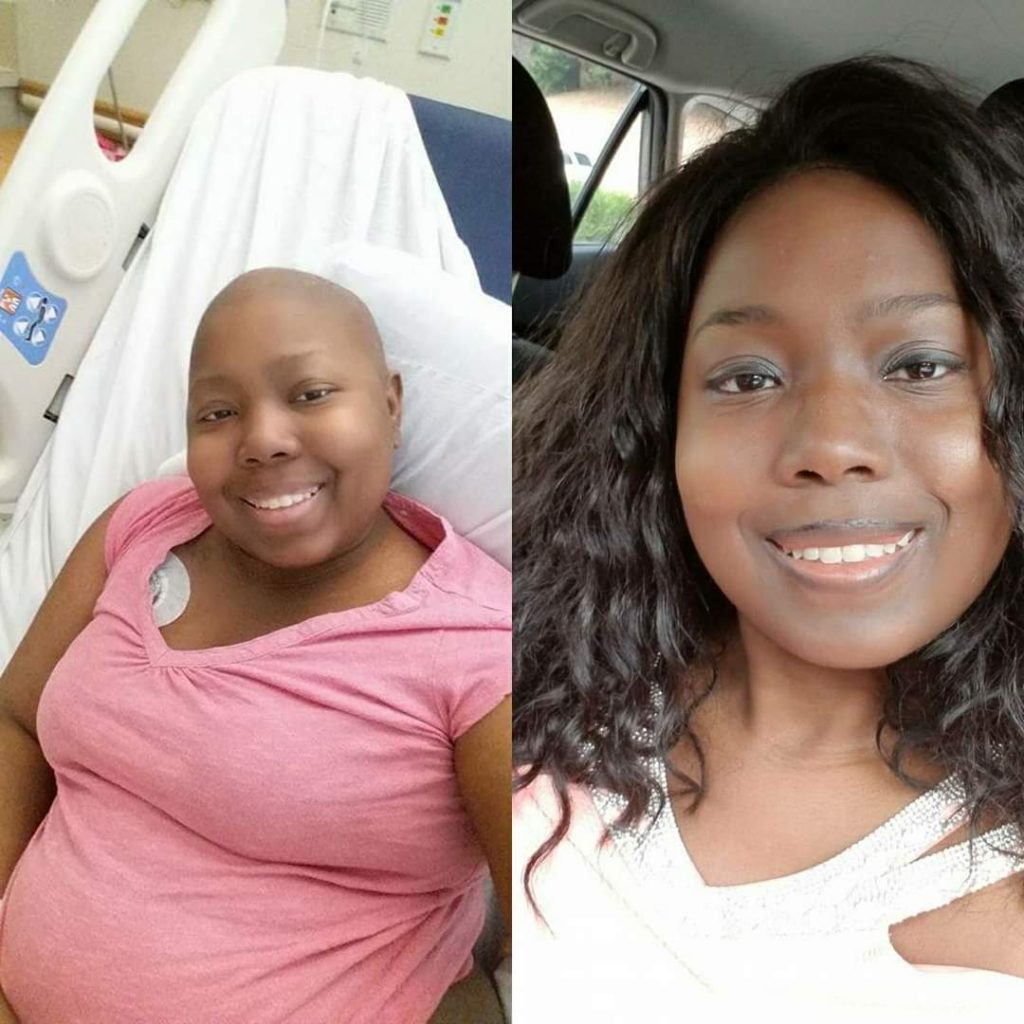
Shaving your head
At that point, I just made the decision of shaving my head because I knew, personally, that I could not take seeing my hair fall out in clumps. That process would be harder for me.
I had my husband come to the hospital with his clippers and shave my head in my hospital room.
I literally told him, “Today they told me that starting on Monday, the therapy I’m going to start is going to take my hair out. I can’t do that. That’s going to break me down. Can you just come shave my head? Because I don’t want the patches. I don’t want to look like that. It’s going to make me look sick. I don’t want to look like that. I’m still doing live videos on Facebook and all types of stuff. I don’t want patches in my head. Please come cut my hair.”
He said okay. He came, showed up, had scissors and his clippers. He said, “Do you want to cut it down and then shave it?”
I said, “Yes, I do.” I literally stood there, cut my hair down, and then he shaved my head, standing in the mirror in the hospital.
How did it feel shaving your head?
It felt fine. I think I took it better than anything that happened. I said, “Oh, I actually look cute!” My son looks just like me, and I didn’t realize that till I had my head shaved.
The response was quite interesting as well. After cutting it and posting the picture on Facebook, all I got was, “Oh my gosh, your son literally looks like you. He’s your twin.”


Getting a bone marrow biopsy to get your specific diagnosis
I had to get the bone marrow biopsy once the doctor I switched to had come back on Monday. When I had started the intravenous chemo, he told me everything that was going to go on and told me I was going to have to get a bone marrow biopsy.
They needed to lock down exactly which kind I had to make sure I was going to get the right therapy. He told me he was pretty sure I had acute lymphoblastic leukemia (ALL).
Describe the bone marrow biopsy
They did the bone marrow biopsy. The biopsy was interesting because I work for an ortho oncologist, and we did those all day long. It was kind of interesting because it was in the hospital. I was not under sedation; I was wide awake. I was literally telling them everything that they were going to do.
The nurse practitioner doing it thought it was interesting. She was like, “I’ve never had a patient who could tell me what I’m about to do and all the instruments I’m using.”
That was my way of calming down. I was talking myself through it, “Okay, they just put the lidocaine in. Now they’re going to make the incision.” The fact they were following it step by step, I was like, “This is good. Nothing is going to go wrong. T this is a routine procedure; it happens all the time. They’re going to get it right because they’re following all the right steps.”
Advice on getting through the bone marrow biopsy
When I’m talking to other patients, I just say you have to remain calm. Even though we want to look up things on the internet, don’t. That was the worst. Looking up things, you’re going to get a lot of negative things out there, and it’ll scare the crap out of you.
I would prefer just to talk to the physicians and the nurses. The nurses see tons of the patients day in and day out. They see people get better. They see how people cope with things. They are a really good resource because they have the time to spend with you.
The doctors do, but they’re in and out. They’ve got so much they have to do. The nurses have their time to spend with you to explain what’s going to happen, to say, “They said you would have this symptom, but you may not have this symptom. If you do, these are different ways we can treat it. It doesn’t necessarily have to go down this path you saw online.”
Getting a CT scan
I did not do a scan before I started treatment. I did one right before I started the intravenous treatment. It was a CT scan with contrast, which was the first time I had that. I remember it feeling warm and feeling like I was going (to the bathroom) during the scan.
They did that to see how my lungs looked, to make sure I didn’t have any lung nodules because my count was so high. They didn’t know how long I had been dealing with it. They wanted to make sure I didn’t have any metastasis. It came back clear.
Why did you get a PICC Line ?
I had a PICC line. I did not get a port. My doctor wanted me to have a PICC line because I did a lot of trials with my therapy because of my age, and the fact that I was completely healthy and didn’t have cardiac issues or anything like that.
I did the pediatric treatment for ALL instead of the adult treatment. He told me my chemo and my treatment was going to be a lot more rigorous than a lot of people on the floor with me.
He wanted me to have the PICC line to have a little more freedom than with the port. I actually wanted the port. I didn’t want the PICC line on the outside, but he convinced me to get the PICC line.
It worked well. It wasn’t bad. You can see my scars. It was in my chest; I didn’t get it in my arm. I had it twice. It was easier maintenance, maybe.
It never gave me any issues. I never had the infection at the PICC line or anything like that. Everything with that was very smooth.
»MORE: Read patient PICC line experiences
The PICC line mini-surgery
It was the people in the room, the nurses and the OR techs, who were very calming. They were like, “Okay, this is what’s going to happen.” I was in the room freezing cold.
They gave me an extra blanket and said, “We want you to relax.” They put a towel over my eyes before they gave me the anesthesia because I was freaking out.
It’s a sterile room. There’s nothing there. You’re like, “I don’t want to lay on this table and have something happen. You’ve got to go straight into my arteries. I want to live through this.”
I had already started to develop anxiety from it. They put a towel over my eyes just so I didn’t have to see the lights and all the equipment around. Then shortly after prepping me, they were like, “We’re going to go ahead and give you a little sleepy medicine.”
They walked me through the whole process. They told me how it was going to feel when I woke up before they put me to sleep, so I knew what to anticipate when I woke up.
Chemotherapy
Cycle A chemo
Cycle A was every day. I had chemo every day for 5 days. It was for about 3 or 4 hours a day. I would get 2 chemo drugs at that 1 time.
The longest one I had was what they call “the red devil” (Adriamycin or doxorubicin), and that was a 12-hour infusion. I think it was maybe 4 drugs total.
Cycle A chemo side effects
The red devil made me very nauseous. I dealt with it via ginger chews. I chewed a lot of ginger chews. My mom went and bought me bags and bags. I also did a lot of smoothies that contained ginger as well.
The part that freaked me out is that it turns your urine that ugly color, a red-orange kind of color. I remember I was so open on my Facebook page, I took a picture of it in the little urine hat and being like, “Y’all, look at this! What is happening to me?”
Nausea was bad for the other drugs as well. I didn’t have too many other side effects other than nausea, which was amazing, apparently. The nausea was horrible.
They had given me pain medicine. Occasionally, I’d get some joint pain or bad headaches. The pain medicine they were giving me caused constipation.
The worst part of being in the hospital was hemorrhoids. That was worse than pain I felt from any infusion during treatment. I had never had anything like that.
That’s when the doctor kept telling me, “If I could get you to feel better from these hemorrhoids, you’d be cruising through everything!” They tried creams. I had the little balloon-donut thing to sit on. I had sitz baths, everything. It was horrible.
Eventually, they had me drink the magnesium, and I ended up having to drink 3 of those to finally go. It was painful when I finally went. I was in tears.
Ask for help with side effects
They were like, “It’s going to pass.” I said, “No, I need help.” The nurses were saying, “You’re not on the call often, but when you’re on the call button, you need help!”
Cycle B chemo and side effects
There was a break between cycles. It was chemo every day. I rarely had any side effects with Cycle B. They were giving me sodium bicarbonate prior to the cycle, about 5 days before coming in for Cycle B, because of the type of drug I was getting. I had no side effects.
Cycle A compared to Cycle B
A was very harsh. B was more mild. I loved B compared to A. I would be excited when I finished that first Cycle A. After maybe about 4 days of bad nausea and bad side effects, it’d be like next time is the good cycle, and you don’t get any side effects after Cycle B.
When I was in the hospital for an induction phase, there was a 2-week break. I really dealt with a lot of the side effects from that first round. Then they had me on the anti-nausea and watching my counts. I had 2 bone marrow biopsies in that time.
»MORE: Read other cancer patient experiences with chemotherapy
Chemo through spinal taps
They started the spinal taps. I had to get the chemo in my spine. They had to do that because they said the chemo given me intravenously does not go to my spine. A lot of times, people will continue to have ALL, and those cancer cells will still be there. So they had to do the spinal taps to put chemo directly into my spine.
That was painful. That hurt. There’s nothing you can really do for it. They would give me anxiety medication before they started because I would just freak myself out. They’d give that to me about 45 minutes prior to me getting the spinal taps.
After the first time, it was pretty standard for me to take the anxiety medicine prior to, otherwise I’d be a nervous wreck. I would have to sit on the side of the bed. They would bring my bedside table in front of me and put a pillow on it. I’d lean forward, my face in the pillow.
It’s a very quick process. It’s just nerve-wracking because you know someone is at your spine. For the first 3 times that I had it, I was inpatient. They were great. I generally had the same nurse practitioner who did it every time.
The fourth time, I had it outpatient. Because I had had it so many times at that point, I knew what it felt like. When I had it outpatient, it was painful. I was telling him, “You’re not in the right spot.”
He was like, “I’m there.” I was like, “No, you’re not.” It hurt really badly. Every time afterwards, if I had to have a spinal tap, please let me do it inpatient before I go home or whatever needs to happen.
Once you get comfortable with different people, this is going to be fine. When you have that bad experience, that’s the one thing that sticks with you.
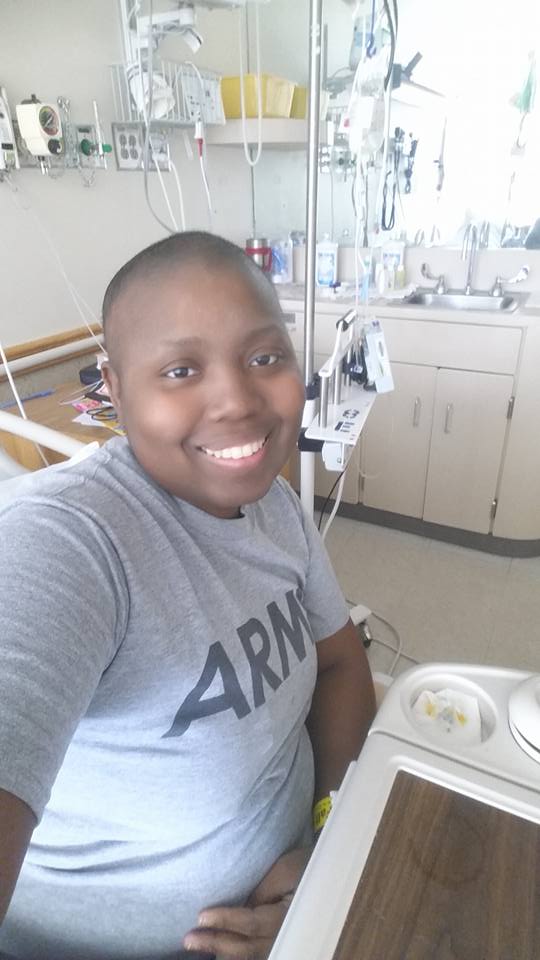
The inpatient experience
Both were inpatient. Then after the first B cycle, I went home for 2 weeks. Then I had to come back in the hospital for 5 days to start it all over again. Every 21 days I was back in the hospital, from January until July.
It was chemo every day when I went for Cycle A, when I would get the red devil at the end of that. Once I finished that, I would go home, no matter what time I finished.
If it was 10 o’clock at night, they’d discharge me because they knew I didn’t want to be there. I’d rather be with my kids and lie in my bed.
I’d do chemo the first 3 days, then a day break. Then they would start the red devil that evening or, depending on what time I got into the room, would determine when they’d start the red devil the last day and when I would leave.
What helped pass the time in the hospital?
I started a business while I was in the hospital. I started that from the hospital bed. I watched so much Food Network and HGTV. I had all sorts of plans for everything.
I couldn’t have that many visitors because you have no immune system, so they have you on the contact precautions, where not everyone can see you.
I did a lot of FaceTime and talking. I started that Facebook group, so I was on there a lot. I got involved with other groups on Facebook, support groups for leukemia and lymphoma, where I could ask a few questions and say, “Hey, I had these side effects. Did anybody else have them?” It helped me see I wasn’t alone.
I did a lot of researching on the symptoms and what I could do with the symptoms. Everybody deals with it in a different way.
Just from being in those groups and talking to people, even talking to people when I was getting laps in in the hospital, everybody deals with it differently.
Different cultures, different backgrounds, so the biggest thing is talking about it. Don’t hold it in.
»MORE: Mental and emotional support when leaving the hospital

Bone Marrow Transplant
Needing a match for a bone marrow transplant
I ended up in June learning I had a donor. They immediately told me I needed to have a bone marrow transplant and needed to have a donor. They looked at Be the Match. There was nobody who was compatible for me at that time.
They told me they would start testing family members and if they wanted to volunteer, I could let them know. I have no siblings, so they were going to start with my mom and dad. Any other family and friends who wanted to volunteer, they would test them.
They started with my dad, who is terrified of hospitals. So terrified that my dad never came to see me in the hospital; he only FaceTimed me.
They tested him and did the lab work. Then they did lab work on my mom and one of my cousins. They kept calling my mom back and needed to get more labs from her.
At the end of June, my doctor told me that I had a match. He said, “Next week we’ll start the process of everything.” I was so excited. My mom went to the appointment with me, as she normally did.
The doctor said, ‘You’re here because we found you a match.’
I said, “Great! When does all this happen? I didn’t have to do my last cycle of chemo. This is great. We’re moving forward.”
She was like, “Yeah, so here’s your match.” She handed a piece of paper on it, and it had my mom’s name on it. She said a lot of times parents aren’t a good match, but my mom was a 7 out of 10. She said in these days that are so advanced, 7 out of 10 is perfect.
So my mom ended up being my donor!
Preparing for the bone marrow transplant (BMT)
In between that time, my mom had to go through all of her testing and found out that she had a sickle cell gene. They told us we couldn’t do it with just her doing the intravenous where they extract. She had to do the surgery where they did the multiple extractions of her bone marrow in her back.
She started prepping for that. They had given her different medications to build up the cells. Then 2 weeks prior to the actual transplant, I went to the hospital.
Getting radiation before the transplant
With people, it’s different. Sometimes they have to target certain areas of your body. They did total body radiation. My doctor said, “It’s small amounts of radiation, but through your whole body. You shouldn’t be burned anywhere.”
I would lie on the table for about 45 to 50 minutes twice a day for radiation for 5 days. It was like a big ray gun that was over the top of me. They would play music for me in the radiation room. I just had to lay there, getting radiation to my entire body.
They had a face shield they put over me so I wasn’t getting radiation to my head. It looked like a helmet they would put on me. This machine would just go side to side, then tell me to turn to my right side, then turn to my left. All I could see was these lights moving around.
That was hard. That broke me down. That made me super weak. My mouth was always really dry and hurting. Eventually, it felt like your skin was peeling a lot. That was the first point where I was like, “This is hard. This is cancer, and it’s not fair.”
»MORE: Read other patient experiences with radiation therapy
Radiation side effects
Summary: Weakness, fatigue, dry mouth, a few mouth sores
I didn’t get those side effects with chemo, but with chemo I had my mouth soreness and dryness, total weakness. I only got a few mouth sores. That’s what people kept telling me. Even my doctor was like, “You probably have mouth sores. Most people get really bad mouth sores.”
I had 2 mouth sores, and they weren’t bad. The biggest thing with the mouth sores is the cells that rapidly multiple is what it targets, so your mouth won’t heal as fast.
There’s really nothing you can do to prep for it, unfortunately. With the mouth wash, I think they give everybody the Biotene, so use it. It’s definitely helpful even if you don’t have mouth sores. Just swish it around when you’re sitting there with nothing to do.
Keep your mouth moist. Drink if you can. It took my appetite away, so I didn’t want to eat after radiation. Be prepared for that. I drank a lot of smoothies. I had my mom bringing me a lot of smoothies, and apple juice was my favorite.
It kept me going because I didn’t want to eat during those 5 days of total radiation. My stomach just didn’t want any food. Nothing tasted the same. The taste was gone from my mouth.
Bone marrow transplant the next day
It was very fast. That’s how they planned it, immediately putting the donor cells into the body. My aunt was there with me in the room. My mom was downstairs getting the harvesting. The doctor immediately came upstairs. They had the bag that looked like I was about to get a transfusion.
It was huge. She said, “These are your cells,” and she hooked it up. They put it into my PICC line, and it immediately started going. There was no in between, no pause. It looked like she got dressed in the OR and immediately brought it up to me. It was less than 30 minutes.
My aunt called me and told me my mom was fine and in recovery. When I started getting my transplant, I fell asleep. They gave me something to sleep.
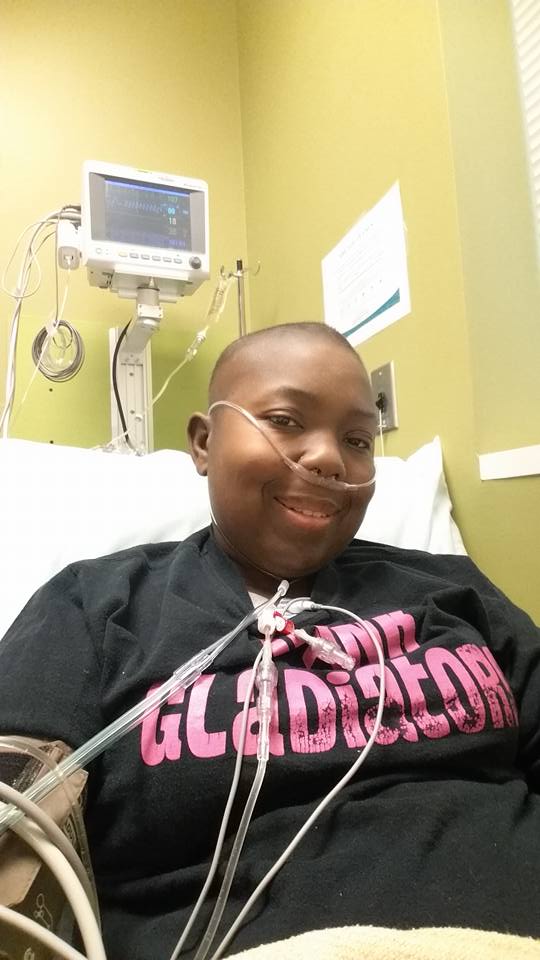
Waking up from the BMT
When I woke up, I was so hungry. I just wanted to eat. I don’t remember who was there because it was blurry at the time. I remember telling them I wanted a 10-piece nugget from Chik-fil-A. I got that 10-piece nugget. I have pictures of me sitting there with a big platter of nuggets in front of me. That’s all I’m eating.
I couldn’t taste them. I couldn’t taste anything. I remember they didn’t taste like nuggets. I dipped them in sauce. I couldn’t taste the sauce, but I wanted to eat those nuggets.
Recovering in the hospital
After that, I was in the hospital for another 20 days. After the transplant, they allow you to do engrafting. They allow your cells to rage and the new cells to try and kill off the old cells. They let them battle within your body, is how they described it to me.
Then they give you chemo that kills all the cells, and hopefully the only thing that comes back are the good cells. They gave me Dilaudid, high doses, which knocked me out.
I didn’t feel any of it because they said the side effect is your body feels like [it’s] on fire. Every morning at 8, at shift change, she would come in and push the Dilaudid. I probably wouldn’t wake up until 8 that evening.
The first 100 days
That was for 2 days immediately following the 4 days where they let the cells do what they wanted them to do. Days 5 and 6 they gave me the chemo and the Dilaudid. Then they let it do its thing.
That’s when you start your journey. ‘The first 100 days’ is what they usually call it.
Those were the hardest days — days you didn’t want to eat, don’t want to talk, days you may not even be able to get out of the bed. Those days are hard because your cells are rebuilding, and it’s going to take time. It’s not like they just click in and start rebuilding. You have to wait a few days.
I ended up being in the hospital 32 days before I could even go home. They label it the first 100 days because they’re hard.
Describe the recovery at home
I was having to go to the doctor every other day for 3 days a week. That was hard. I saw the doctor maybe once a week, and the other 2 days was to go to the lab so they could test my levels.
Then once a week, I had to go so they could look at my anti-rejection meds to see if they needed it to be altered or anything like that.
They’d look at my labs and say we need to go up or down on this one. I did really well, though, because in those first 100 days, I came off one of the drugs. It was too much for me and making me sick once my counts started to rise again.
They said we’ll take you off of this medication and leave you on the other, which worked out well because I was really nauseous from that medicine. It felt like I had ulcers because I was throwing up so much.

Monitoring post-transplant
They monitored me. I was still doing bone marrow biopsies at that point. Other than that, it was a lot of monitoring and lab work. A lot of weekly follow-ups. I think I followed up multiple times a week for the first 4 weeks, once I got discharged from the hospital.
Then it trended down to 2 times a week, to once a week, then once every other week. Then I started to backtrack because they started to try to wean me off of the medication.
Then I began to get GVHD (graft-versus-host disease). I am still battling that now. I’m still on 20 mg of prednisone every day.
Graft-versus-Host Disease (GVHD)
My GVHD targets skin. I started to get these rashes really badly. It targeted my lungs, where it has settled. I would get these coughs that would last forever, hard coughs, when we would try to decrease my medication.
I was able to come off the anti-rejection meds, but I came off them right before I hit a year. But I have not been able to shake the prednisone.
If I don’t take my prednisone and in the age now of coronavirus, someone’s going to think I have it, because I’m going to cough and cough. I get pneumonia during the year.
It has become a standard for me. When the seasons change, I feel it, and I literally just call the doctor. She’s like, “Okay, come in and get a chest X-ray. Yep, let’s get your antibiotics.”
This time was a little different because I got it in March. I now work at the same facility where I’m treated, same hospital. They had sent me home to work from home because they were like, “You’re extremely high risk. This is a respiratory virus. You’re high risk because you have GVHD in your lungs. You can’t work here. You have to go home and work.”
I came home, and that first week I was home, I was fine. But then I started to feel it. I got the cough. My chest started to feel heavy. I got a ton of inhalers, the nebulizer machine, started getting out everything. Making sure I took prednisone every day, same time.
Reflections
What helped move you forward during the lowest moments?
Through my whole entire journey, those 100 days mentally and emotionally were my hardest. I did a lot of crying when I first came home.
It’s like, “I beat this, I kept the transplant, and everything’s going back to normal. I can do 100 days!” And I couldn’t. I remember breaking down in the kitchen one night.
My neuropathy in my hands was so bad. One of my kids wanted a peanut butter and jelly sandwich. To take the twist-tie off the bread hurt so bad because my neuropathy was so bad.
I broke down in the kitchen like, “I’m not normal. This is not right. Why am I going through this? This is not fair.” That was hard for me. I look back on it now, and I’m like, “How did I get through that?”
It was a lot of crying in an emotional time. I also started going through separation with my husband, so it was very trying.
How cancer impacts relationships
I don’t think my husband had an outlet. He had an outlet, but because of the type of person he was, he internalized a lot of things.
The way he dealt with it every time I was doing therapy in the hospital or outpatient in the clinic, I said, “Go with me to therapy.”
He said, “No, I’m all right. I don’t need therapy. I just need to make sure you’re good.”
He had not cried in front of me, dealing with this, the entire time. I was like, “I don’t know if you cry at home, but at some point, you have to face the fact that I have cancer.”
‘We’re beating this. I’m not dying on you or leaving you here with the kids. We’re going to get through this.’ That was my affirmation to myself. I needed that for me.
I think it came down to he was having a hard time with me not being the person that I was. I couldn’t do a lot of the cooking and the cleaning, things like that. It wasn’t that he was like, “Oh, she’s lazy.” It was hard for him to come to grips with.
Because the communication wasn’t strong, he was internalizing everything. It made it even harder and frustrating for me and for him.

I never blame cancer to say, ‘Oh, it ruined my life and my relationship.’ It made things hard, and you never know how other people are going to deal with it.
It was easier for me to stay positive because I was going through it. I think it was harder for him to see me going through something like that because I was military. I’ve always been strong-willed, doing what I need to do to get things done. For him to see me helpless in some way, I think it bothered him.
Those are the things people don’t tell you about. Your relationships could suffer. Not saying it’s going to go the way mine did, but you’re going to have to find something else that you guys can lean on that makes you happy because the old you is not there, that’s for sure. You’re not your normal self.
»MORE: 3 Things To Remember If Your Spouse Is Diagnosed With Cancer
Cancer impact on your life perspective
Your whole life changes. It’s not just, “I had cancer, and now it’s over.” I wish it was like that, but it continues to rear its ugly head in my life.
The biggest part of that is just knowing you have to tell yourself that you want to live. That this is still better than what it could have been.
Yes, my whole life changed. Everything was flipped upside down, but I’m also here. I still get to socialize with my family. I still get to see my kids. I still get to raise my kids. I still get to just have a life.
I won’t tell anybody that every day is a good day, because it’s not. That would be a complete lie. Some days are really hard emotionally, dealing with anxiety.
Some days it’s just hard. Some days I just want to lay in the bed, and I just have to really push myself to keep going.
My faith keeps me strong as well. Trying to maintain and keep my mind off of it, glass half full instead of half empty.
Things could be much worse for all of us. Everybody who is now a survivor, everyone who is in remission, or even all of us who go through treatment still — you’re still here.
We have to play off of that. We’re still here. Things could be worse. We’re still here, so we have to be positive.
Remain positive. Remain strong. Fight it. Don’t let it get the best of you. Fight it with every inch and ounce of being. Fight it. Don’t lay down. Don’t let it take your happiness, your joy. You’ve got to fight.


Inspired by Lauren’s story?
Share your story, too!
Acute Lymphoblastic Leukemia (ALL) Stories
Lauren M., T-Cell Acute Lymphoblastic Leukemia (T-ALL)
Symptoms: High fever, trouble breathing while lying flat, bad cough, headaches
Treatments: Chemotherapy, radiation, lumbar puncture
Christine M., Acute Lymphoblastic Leukemia (ALL)
Symptoms: Enlarged lymph nodes, pain in abdomen, nausea
Treatments: Chemotherapy, bone marrow transplant
Lauren J., Acute Lymphoblastic Leukemia (ALL)
Symptoms: Extreme fatigue, easily bruised
Treatments: Chemo pills, chemotherapy, spinal taps, total body radiation, bone marrow transplant
Renata R., B-Cell Acute Lymphoblastic Leukemia, Philadelphia chromosome-positive (Ph+ALL)
Symptoms: Fatigue, shortness of breath, nausea, fevers, night sweats
Treatments: Immunotherapy, chemotherapy, TKI, stem cell transplant (tentative)





Leave a Reply