Danielle’s Stage 2 Classical Hodgkin’s Lymphoma Story
Danielle was diagnosed with stage 2 Hodgkin’s lymphoma at 25 years old. Read her in-depth story about tests and biopsies, undergoing ABVD chemo and freezing her eggs to preserve fertility options.

- Name: Danielle D.
- Age when diagnosed: 25
- Diagnosis:
- Hodgkin’s lymphoma
- Stage 2
- 1st Symptoms:
- Growing lump on right side of neck (swollen lymph node)
- Tests & Biopsies:
- CT scan
- Needle biopsy
- Excisional biopsy
- PET scans
- Pulmonary function test (lungs)
- Blood work before every treatment
- Treatment:
- ABVD Chemotherapy Regimen
- 3 cycles
- Each cycle = 1 month, biweekly
- Total of 6 infusions
- 3 cycles
- ABVD Chemotherapy Regimen
- Fertility Preservation:
- Decided to freeze eggs before chemotherapy
- 2-week process
- Daily hormone shots
- Daily blood work
- Egg retrieval procedure (26 eggs)
- Decided to freeze eggs before chemotherapy
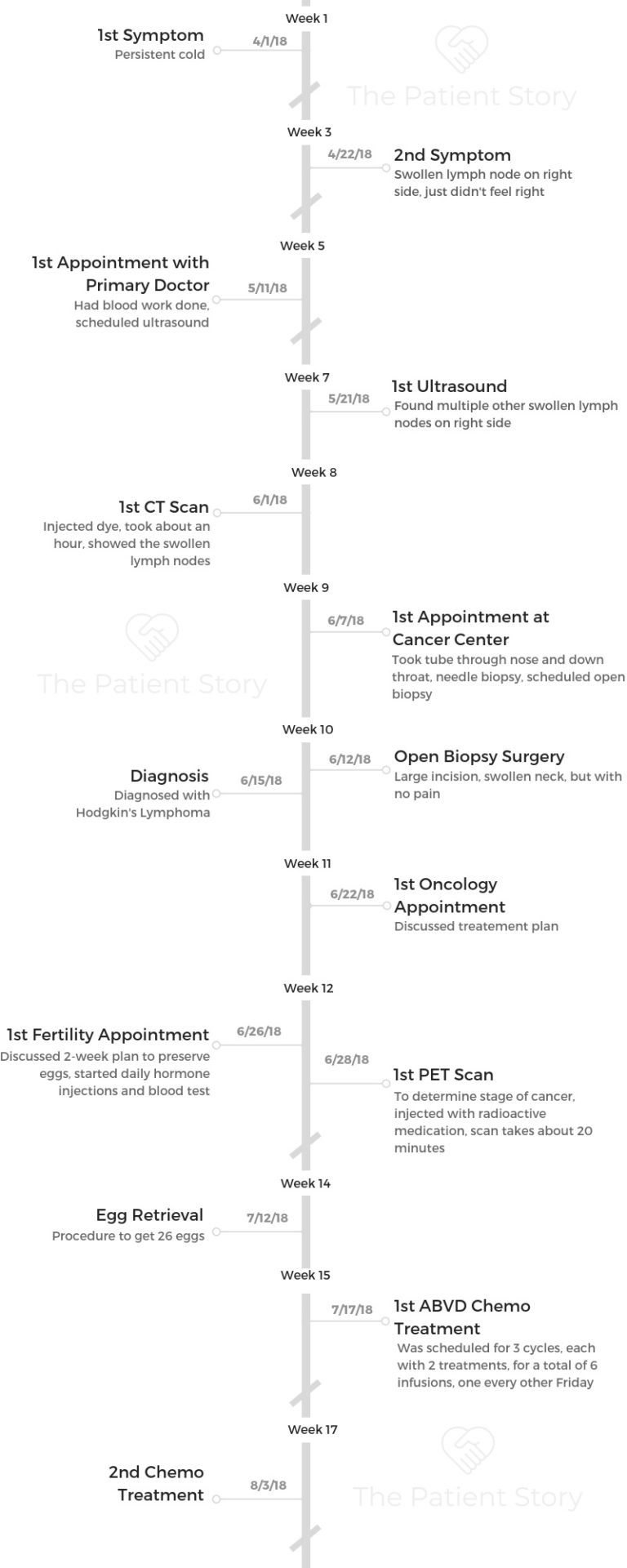
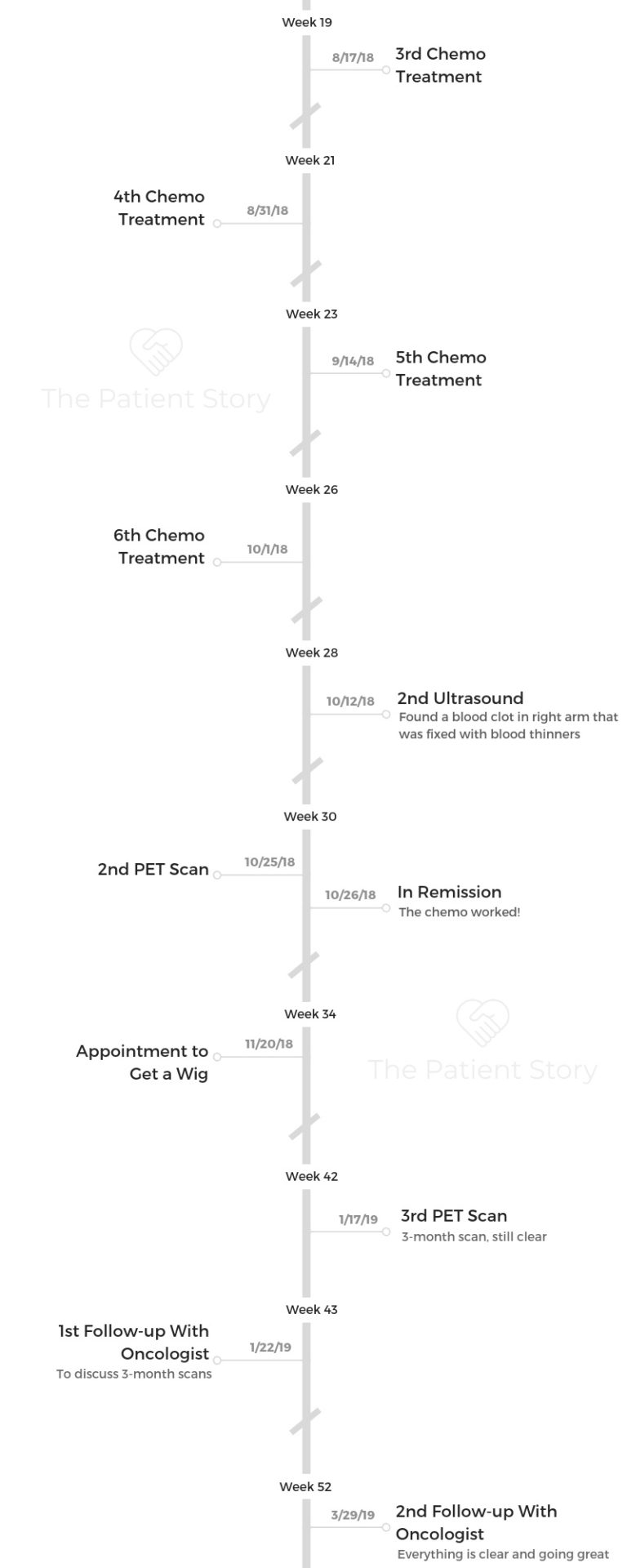
- 1st Symptoms & Tests
- What were the first symptoms?
- What made you go to the doctor?
- Describe the ultrasound
- How long did it take to get ultrasound results?
- Describe the CT scan
- How long did it take to get the CT scan results?
- Describe your meeting with the ENT doctor
- What’s the needle biopsy like?
- What was the excisional biopsy like?
- How long did it take to get the excisional biopsy results?
- Treatment Decisions
- How did you process the cancer diagnosis?
- How did you break the news to your loved ones?
- How did you decide where to get treatment?
- Did you get a second opinion?
- Describe the hospital you went to
- Any advice on choosing the right treatment center?
- Any advice before going into treatment?
- Being a self-advocate as a patient
- Chemotherapy
- What was your treatment plan?
- Describe the ABVD chemotherapy regimen
- Describe the chemotherapy process
- What were the chemo side effects?
- Tips on how to deal with side effects
- How did you decide not to get a port or PICC line?
- Your veins eventually became an issue
- Any advice on whether to get a port or PICC line?
- Post-Treatment Scans
- Hair Loss
- Emotions, Support & Care
- What were the hardest parts mentally and emotionally?
- What helped you through that stress the most?
- Talk about being young with cancer
- How did you approach dating during treatment?
- You want to help others now who’ve just been diagnosed
- Why was it important to find a cancer community?
- Were you able to ask people for support?
- How important was it to have caregivers?
- Work & Finances
- Fertility & Egg Freezing
- Survivorship
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Being diagnosed with cancer is definitely a scary thought, and it’s a very scary process. You don’t really know what you’re in for, but you do have a lot of people there for you.
Just stay strong. I think the attitude of it all through the whole process definitely helps a lot. Truly feel your feelings while going through everything; don’t hold anything in.
The positivity really does help, and it makes a huge difference through the whole treatment process.
Danielle D.
1st Symptoms & Tests
What were the first symptoms?
I really didn’t have any symptoms except for the one lymph node on my right side that was just getting bigger and bigger as time went on. It just wasn’t going down.
What made you go to the doctor?
I noticed that the lymph node wasn’t going down. It was just getting bigger, and it was only on one side. As soon as I started to feel other ones lower down my neck, it just didn’t seem right.
The day I ended up going to see my primary doctor, I just went in there and told her that I had this little lymph node and it wasn’t going down. She wanted to get blood work, and then I went out to get ultrasound done. In the ultrasound, that’s when we found several smaller lymph nodes.
Describe the ultrasound
It was the same exact day that I had gone and seen my primary doctor when I got the ultrasound.
I felt like my doctor had known that something was going on but wasn’t really quite telling me. I just felt scared in a way. Worried.
When had I gone for the ultrasound, I just felt like they were just subtle and nice. The one lady who had done it was very sweet, but you could tell she was really finding a ton of things on the right side just because she was taking a lot more time on that side than the left side.
The whole time I just kept thinking, “What if this is something very serious?” I just didn’t know what it could have been. It was almost like an ultrasound for a baby, but it was on my neck.

How long did it take to get ultrasound results?
It took about a week. My mom had been calling the doctors and saying, “What’s going on? What’s going on?” to push those results.
It was very hard because I knew, especially with my mom freaking out, something wasn’t right. I just don’t know why it took them so long to find out these results.
I was just in a panicked stress about if they had known something and were trying to come up with some plan, but it was taking longer than what it should have.
I was angry, upset, worried. My stress and anxiety were going up.
Describe the CT scan
After the ultrasound, he really didn’t quite give me any result except for the fact that I had a lot lymph nodes, and they wanted to then go through the CT scan.
So I went through the CT scan, which also showed lots of smaller lymph nodes.
I was actually very nervous during the CT scan. I didn’t know. Once again, just going through all of this not knowing what’s going on, just knowing there’s something not right.
When I found out I needed to get an IV, I was just so nervous because I didn’t expect that. I was terrified of needles, so I was a wreck the whole time trying to figure this out and what was going on.
The nurses were great. They were so sweet, but I was just all stressed and worked up. I laid down, and they pushed the medication through. I was in this machine where they scanned my entire neck. That also showed all of the swollen lymph nodes.
It probably took about an hour to get me all done. I was just going with it, but also being so nervous. I just didn’t understand. I didn’t even really know what a CT scan was.
It was painless, except when they injected the dye. It was an interesting process, the way that it makes you feel.
They tell you, “Okay, you’re gonna feel like you’re going to have to go to the bathroom. You’re going to have to pee.” That’s exactly what it felt like. It’s a weird feeling. I just didn’t know what to expect.
How long did it take to get the CT scan results?
It really didn’t take long for me to know that I had an appointment with a doctor at Wilmot Cancer Institute, because I had seen it on my chart before I was even told by my doctor.
Once again, I knew that they had figured that something was going on, but they didn’t want to say that yet. I think they were just trying to wait for all the testing and everything to really confirm that this may be what we’re looking for.
»MORE: Dealing with scanxiety and waiting for results
Describe your meeting with the ENT doctor
I went there with my mom. Just seeing the word “cancer” in the place that I was going to, I was like, “Wow, there’s the chance that I could have cancer.”
I even got a new patient folder with all this information on it, like how there’s support groups for cancer patients and all this. I still didn’t know that I was probably going to be told later on that, “Yeah, here you have cancer.”
There were just so many doctors and nurses around. I still had no idea what was going on. They were doing a lot of testing. They had to put a tube down my nose, into my mouth, taking a look basically at everything in my neck.
Then they told me, “Okay, we’re most likely looking at lymphoma. But what we’re going to do is a needle biopsy, and that will rule out any type of infection.”
They went through with that, and it came back right then and there that there was no infection.
What’s the needle biopsy like?
The needle biopsy really wasn’t bad at all, but of course the fear and panic of a needle going into your neck is a little scary, so I had the nurses holding my hands and everybody there for me. It really wasn’t that bad at all.
They took a needle to my neck, and then they were able to take some of the lymph node out just to get a sample to it, to look through and see if there was any type of infection. The doctor had told me right then and there they would know if it had an infection or not.
What was the excisional biopsy like?
After that, they told me, “We’re definitely looking at lymphoma, and we do want to have you have an open biopsy surgery done.”
That was within a few days. I had to prepare for it. They gave me all the papers. All of a sudden, I’m signing all these papers for my first surgery, and that’s when I knew, “Okay, I’ve got cancer. Now they just need to find out what type.”
When I went to the hospital with my mom, we made it very early in the morning. I couldn’t eat or drink or anything.
Once I got in there, I looked up at the screen and saw that there were numbers. Really, you’re a patient there, and you’re just a number. It was all this new experience. I’ve never had surgery in my life.
I knew I was in good hands with the nurses and the doctors there. I got all ready, they put the IV in, and then they did a very good job of explaining everything.
I was just glad my mom was there. As soon as they pushed me down to the operating room, I could feel myself going out of it.
The next minute I know, I’m waking up. I didn’t feel any pain or anything, so I was like, “Oh wow, it’s done.”
I grabbed the mirror that the nurse had given me to look at my neck. I could see it was very swollen, and there was the huge incision. I just can’t believe that that had just happened.
I really am very surprised with how much I never felt any pain or anything. I was just extremely tired and a little out of it, but other than that, I really didn’t have any pain.
How long did it take to get the excisional biopsy results?
After the surgery, I think it was about 2 days. I got the call, and they told me they were gonna call me with the results.
I was waiting and waiting, and then I finally got the call. He had told me right then and there it was Hodgkin’s lymphoma.
Treatment Decisions
How did you process the cancer diagnosis?
I just remember I went home and I did all my research. I was looking it up. I didn’t really quite know about lymphoma or what types. I just felt like all of a sudden I was educating myself on all of these types of lymphomas and which one I could possibly have.
I got the call while I was at work. I had already told a lot of my coworkers. They saw everything that I was going through with testing and everything, so it wasn’t a shock to anybody.
It wasn’t even a shock to me once I got that call from the doctor. He told me I had Hodgkin’s lymphoma.
He said, ‘Danielle, I hope I’ve prepared you enough for this.’
I said, ‘Yeah, you really did. You prepared me. I’m just ready to do whatever I have to do to get rid of it.’
I really wasn’t aware of what I was going into, but I just knew, “Okay, stay strong. You’re gonna get through this. I have amazing friends and family who are gonna be there for me.”
»MORE: Patients share how they processed a cancer diagnosis
How did you break the news to your loved ones?
I texted some of my friends. My coworkers, I feel, just knew. I told them, “This is what we’re looking at.” They knew it was lymphoma, so I just mentioned, “Yep, it’s Hodgkin lymphoma.”
With my parents, I called them both up and told them it is Hodgkin’s lymphoma. Because I feel like the testing took so long with all of that and we were very prepared on what we were going to be told, I think the actual results weren’t a shock at all to anybody.
It was getting that it’s confirmed, and now it’s time to get treatment done.
»MORE: Breaking the news of a diagnosis to loved ones

How did you decide where to get treatment?
I was just placed right over at the cancer center by the doctors, and I’ve always heard really good things about it. I know a lot of people, some family friends, who have gone there.
I really liked how all the doctors and nurses treated me there. I was really happy that I was placed there.
Did you get a second opinion?
I never really did get a second opinion just because I figured that I was in a good place, and we had caught it early. I figured they knew what they were talking about.
They already know of a really good plan for Hodgkin’s lymphoma treatments and what has cured past patients. If it was a different type of maybe a more difficult type of cancer, I think I would have done more looking around to make sure. I think it was very straightforward, so I was like, “Okay, I’m ready.”
Describe the hospital you went to
I was at a large hospital. I’ve always been a person that likes to be around more people. I was happy to see that I wasn’t the only one there, even though I was the youngest that was there.
I knew that there were other people around me. Even in the pods, getting treatment, it was nice to always be around people. I did really enjoy the large hospital.
I think that it was hard to see and look around. I was the only young cancer patient. I probably saw one other person who was my age there one time.
A lot of the time, it was all older people. I felt a little lost and thought, “How did this happen?” But there were really no negative things about this place. I really did love it a lot.
Any advice on choosing the right treatment center?
I think that looking around and seeing the employees and the nurses and doctors there, being positive, and always wanting to cheer you up, that’s a huge thing. That makes a huge difference.
I think, too, go to a place where there are a lot of organizations and groups to help out. They always had massage therapists there. They were always looking out just to help out cancer patients specifically with stress and anxiety. There were so many groups just right there. That’s what I loved about that place.
Any advice before going into treatment?
I know that with my treatment plan, it was always known that I was gonna do 3 cycles, or 6 treatments, of ABVD chemo, but then they were also trying to get me to do radiation.
I’m glad that I chose not to do radiation. When they do come up with a plan, just know what’s best for you and your body.
Just know your options.
Being a self-advocate as a patient
When I was being told my options, I just thought, “Okay, well, you’re telling me that there is radiation that I could do, but also that it could increase my chances of getting breast cancer because it would have been too close to my breast at such a young age.”
That wouldn’t have been right. So why add that on if I know that chemo can just help me out?
Maybe also have a plan, but just take it step by step. You don’t always have to go with the whole plan. Just take it day by day, step by step.
If chemo does it, then why go and try to add more to it if you don’t need to?
»MORE: How to be a self-advocate as a patient
Chemotherapy
What was your treatment plan?
I was told that I was going to have to do 3 cycles. Each would be 2 treatments of ABVD chemo. Those are the 4 drugs that I would have to be given. A chemo treatment one day would be about probably 4 hours.
Describe the ABVD chemotherapy regimen
There were 6 infusions total. For every cycle, it’s 2 treatments, so there was 1A, 1B, 2A, 2B, 3A, 3B. I made my chemo treatment days on Fridays, and it would be every 2 weeks.
I would get one treatment on Friday, and then the next Friday it would be a free day. Then Friday after that, I would get my next treatment.
So you’d do 1A and then 2 weeks later 1B. Then again it would start 2A, then 2 weeks later 2B.
Describe the chemotherapy process
I’d first go and get blood work. After that, I would get assigned a pod and just sit there in the chair. They would put the IV in.
They’d give some medications, like the steroids and all of that, to help a little bit. I did ask for anxiety meds because I was getting so worked up and worried.
Then they started off with the first 2 medications, one each at a time. They would have to sit there and have to push the medication through the IV slowly.
They had a little timer, and at first it was okay. In the first one, it was just like, “Well, what is all this?” I was learning it all myself, taking it all in.
Then the last 2 medications were through the bag, which they would just drip into the IV. As time went on through treatments, it got to me more and more with nausea and all my emotions.
Each treatment got harder as time went on, but I always had support systems there. I was always allowed 2 people at a time.
What were the chemo side effects?
Burned skin
During the treatment I was okay, and then the next day I would wake up and feel a little out of it, a little strange. My face would almost look like I had just gotten this sunburn. It was weird. It made my skin very red, and then I would be okay.
Fatigue
By the second day, which would be a Sunday, I would just sleep for about 16 hours. Mondays are my days off from work, so it was nice that Mondays I was able to just take it all in and just relax.
Nausea
As the week went on, it was more nausea. Dealing with a lot of that. Sometimes I’d feel a little dizzy.
Jaw pain
I would try to eat as much as I can, but I would start to experience jaw pain. That first week after treatment, I was really experiencing all the symptoms.
Then week 2 would come around, and all of a sudden, I was back to myself a week later, just to go and get treatment again in 4 days.
I just know that with the jaw pain, that was scary. I actually ended up calling my oncologist about that. That I really didn’t know what to do. I just rode it out.
Constipation
Constipation was actually my worst symptom during chemo.
I had never experienced that before chemo. The doctors had told me about what medication to get before I start treatment, which I did. I went out and got those, but nothing was working.
It took me a very long time to find out what I could do, but that had me in bed for a while because it became very painful.
MiraLAX was the one that I ended up finding out on my own that would be the best that would work. Friends and family were the ones who had recommended I get that, which is very easy to purchase. I was able to grab that and just start that, which ended up helping a lot.
Halfway through my treatments, I no longer had to deal with that anymore. I got better with that, but that was after I was trying all of these other things that my doctors were telling me about, medication-wise.
Tips on how to deal with side effects
Right off the bat, when you’re told that you need to start treatment, ask about anything that could help with any type of symptoms that you may get or may experience. Just get any advice that you can from them.
Also, try to talk to your family and friends about it, because they may tell you things that the doctors may not tell you. Some of the symptoms could be taken care of by doing other things besides medications.
How did you decide not to get a port or PICC line?
Weirdly, a port was never talked about. When I was doing my research on Hodgkin’s lymphoma, I had seen that a lot of people were getting this port or a PICC line.
I was wondering why that was never brought up, but I was almost like, “I don’t want to bring that up because I don’t want to have that if I can try to do everything through an IV.” That’s what I wanted to do, so I just went with it.
»MORE: Read patient PICC line experiences
Your veins eventually became an issue
After some time during the end of my treatments, my veins were getting a little destroyed. It was about 2 infusions that I had left where it was very hard for the nurses to find a really good vein, even the nurses trying to just simply take blood.
It was very hard, and as time went on, after my last treatment, I ended up getting a blood clot in my right arm.
If I needed 6 more treatments, I would have probably needed to get a port. I think because we had caught it so soon, they were able to avoid the port and just use an IV.
Any advice on whether to get a port or PICC line?
I would only get a port if I really needed to go through maybe 12 or more treatments.
When it was getting really bad to find a vein, I did keep thinking, “Oh no. What if I do need more treatments? I’m going to probably need to go to get a port.” It never got to that point, thank goodness.
I was glad that I did just go through the IV process. They were able to eventually always get a good vein. With good nurses, they were always to find something.
Post-Treatment Scans
How many PET scans did you undergo in all?
After my excisional biopsy, they did a PET scan to find out exactly the staging of the lymphoma.
After I was done with all 6 of my treatments, they wanted to do a PET scan to make sure that the chemo had worked, which it did.
Once I was told I was in remission, they wanted to schedule a PET scan for about a month or 2 out. When they had realized that we had 2 clear PET scans after treatment, they did not want to any more. I had a total of 3 PET scans.
Describe the PET scan
The first one that I had gone through was a learning experience for me for sure. I had no idea what I was getting into, but you go in there and they inject you with the radioactive substance through an IV.
They check your blood levels again with just a prick to the finger. You do have to drink this liquid, which lights up all of your organs.
After that, you have to wait an hour. Once the hour passes, you go into the scan. You lie down. They strap you in a little bit. If you are claustrophobic like me, they have medication options for you if you want.
I just kept my eyes closed and just went through it. You slide in and out of the machine through the whole process.
Sometimes they’ll play music for you if that helps, and it takes about 15 or 20 minutes. They take a few pictures. Then after that, they’ll come out and unstrap you, and you’re all set to go.
How long did it take to get the PET scan results?
It would take about 2 to 3 days after usually for the results to be returned back to me.
What’s “scanxiety?”
Scanxiety is a real thing. I really experienced that a lot every time. Especially as time went on, it just got worse. Even after treatment, it brought up memories of when I was in there before, when I had the cancer in me. So scanxiety is definitely a thing.
I think it’s all built up before you go into a scan. You have all of this anxiety. You just pray that it’s gone, or you pray that the chemo’s working.
Or what if it’s just gotten worse? It’s all these things in your mind that are just running through your mind, and you’re just sitting there questioning everything.
A lot of my experiences from treatment and chemo [were] being brought up, and then you just sit there thinking, “How could this be?” A lot of questions are just raising the anxiety of it all.
How did you get through the scanxiety?
I really tried to just stay focused, be strong, think positive and just pray that the chemo worked. If you still have cancer in you, you’ve just got to keep the fight going.
Hair Loss
When did you start to lose your hair?
I started to lose my hair exactly a week after my first treatment. I had so much hair, so I was like, “All right, as long as I can’t really notice right now, I’m just going to go with it.”
When I was brushing my hair a week after my first treatment, I could tell it’s actually really happening. I always told myself I’d deal with it when it starts to happen. Now it’s actually happening, so I broke down a little bit.
I couldn’t believe it was actually happening. It was reality. Then every time I was in the shower, it was just hair everywhere. It was constantly on my hands.
Describe the hair loss
For a very long time, my hair held out. It was thinning and thinning and thinning. It got to the point where I just decided, “Well, you still can’t tell too much.” Nobody else could tell, so I just went with it.
Then time went on where the top of my head was getting a little bit thinner and balder, very flat looking. I always would wear a hat. Eventually, as time went on, the hat wasn’t even working. I really didn’t have any strands of hair left.
My friends and family were telling me I needed to look into a wig. It took me a very long time to come to the realization I’m gonna need to get a wig.
I started to do my research. It wasn’t until I actually finished treatment, around the holidays coming up. I was just like, “Okay, I do need to get a wig. A hat is not working anymore. I really have no more hair.”

I eventually did buy a wig, and I still wear it to this day. Still trying to get through all of that, and as my hair grows, I can feel myself growing as a person again and getting not back to where I was, but getting back to life and just trying to stay strong through it all.
»MORE: Dealing with hair loss during cancer treatment
Did you shave your head?
I never shaved my head. I didn’t really want to. I think that was very hard for me. I was like, “Well, I can just go with it a little bit and see how long I can carry this out for without having to shave my head or without getting a wig or without having to wear hats.”
I was in denial that I was losing my hair. Then it got to the point even my coworkers were like, “Yeah, I think you should do something. You should look into something.”
What killed me also was that here you are told, “You’re in remission. You’re cancer free.” And then you’re still looking at yourself in the mirror like, “Wow, I still don’t have my hair, though, and that’s a huge thing for me.”
You’re in remission and you’re cancer-free, but I’m still looking in the mirror seeing everything I’ve gone through and the loss of my hair.
I finished treatment October. It was about a month later when I ended up really working up the courage just to go get a wig. I’ve been wearing it ever since November.
Any advice on how to find the right wig?
I would recommend going somewhere, if you can, in person to get a wig. I was able to find somebody in the area that I live, and she was great. I tried on many different ones while I was there.
As soon as she put this one on, it was like my exact hair. It was the style I get, the color I get when I go to a hairdresser. It’s great to be there in person and actually try them on, if you can.
Any problems with wearing the wig?
I never found any problems with the wig, just trying to keep it stylish and smooth. I do find it a little tricky, though. I used to love hugging people, and now it’s like, “Watch the hair. Be careful of the hair.”
It’s never been itchy or anything, but sometimes it does get in the way. With the spring and summer coming up, I am hoping to not wear it so much because I feel like it will get very warm, and it’s not going to be something I’m going to want on my head all the time.
Emotions, Support & Care
What were the hardest parts mentally and emotionally?
I feel like the chemo treatment itself was very mentally draining for me, having to go over there every 2 weeks knowing for the week I’m not going to feel well.
I’m going to be sleeping for 16+ hours, and I’m not going to be able to do the things with my friends that I normally would do on the weekends. I think just receiving the infusion and the treatments was probably the hardest.
What helped you through that stress the most?
I think what helped me move forward is just knowing that I have such a great support system and that this isn’t forever.
This is only going to be a few months of my life, and then I’ll be back to doing things that I love to do. I have the rest of my life to live, so just focusing on the now and just getting through what I’m going through right now.
Talk about being young with cancer
I was 25 when I was diagnosed with Hodgkin’s lymphoma. In a way, it has set me back a little bit, especially with dating or just wanting to enjoy certain things in life or just go out with friends. For that little time period, I felt like that was all taken away for a little bit.
It really made me grow up a lot and realize life can be taken at any moment, or things can happen at any moment where you have to really just focus on you and getting better.
I don’t know. I feel like in a way, it was something that held me back a little bit, but now it’s becoming something positive where I feel like I can help other people.
How did you approach dating during treatment?
While I was going through treatment, I just knew that I needed to focus on myself, and so that’s why I really couldn’t focus on dating.
I didn’t really want to bring anybody into all of this, and I don’t even know how I could have really dated when I was going through treatment.
That really hurt me a lot because I am young. I’m getting to that point where I do want to be with somebody. Even now after cancer, a lot of my friends and everybody know what I’ve gone through. There are guys out there who do want to date me, but are they actually aware of everything I’m going through right now?
I’m still not fully okay with everything, so it’s been a little bit of a struggle in trying to open up again and try to be okay, focus on that and not this.
I feel like I’m healing myself first, and then once I feel like I’m ready again to date and do other things again, then I’ll be good.
Time is definitely a pressure. I feel like right now, this is my time to be out and to date and socialize. For those few months where I was basically sleeping 16 hours and going through treatment and not really myself, that took up some of my time.
Now I feel like I’m having this anxiety of, “Oh my gosh, I need to make up for that time.” But I know that I need to focus on healing myself first.
You want to help others now who’ve just been diagnosed
I do feel like this has become something positive. I notice in the past few months, too, I’ve just been much happier. I’ve been able to get back to the gym. Seeing that there are all these other cancer survivors or cancer fighters out there on social media that are my age, a little older or a little younger, just helps.
I feel like I can actually make something positive out of this and help those people, because I know that’s what I needed when I was going through treatment.
It’s always good to see people who are being strong in that same situation that you’re going through.
Why was it important to find a cancer community?
It’s always good to find other people who are going through that exact same thing, going through chemo. Your friends and family are there for you. They’re always there for you; they’re going to be there for you.
It’s always good to vent to them, but I think it hurt them and it hurt me that they don’t really understand what it was like to actually receive chemo and to have those symptoms.
You don’t really understand until you’re actually going through it. I didn’t understand either before I started going through treatment.
It was good to see and connect with other people who understood exactly the symptoms and everything that I was talking about. Losing your hair — nobody will understand until it actually does start to happen to you.

Were you able to ask people for support?
I felt like I was able to ask for support, but also I feel like I was a zombie through treatment and I was just trying to get through it.
It wasn’t until afterwards that I realized I needed it more than ever, the support and comfort. During treatment I was just focused on, “Okay, just get it done. Get through it. You got this.”
But then it wasn’t until after that I had the most crazy breakdowns, and that’s when I started to feel everything.
I was so happy that I was told I was in remission, but after that, I was just like, “Okay, what now?” Now I don’t go to my oncologist every 2 weeks; I don’t have to go through chemo.
That became my life, and now it’s all of a sudden like, ‘Okay, you’re good, you’re done.’
Then I was just having that fear of what if it comes back? Everybody else around me was just so happy, and I was happy, too. But I still had that inside me, where I was like, “What if?” And having to deal with my hair.
»MORE: What kind of support cancer patients say helped the most
How important was it to have caregivers?
I found it very important to have caregivers. I would spend the weekends at my mom’s, that weekend that I would get treatment, just so that she could cook for me or just check on me to make sure that I was still breathing after 16+ hours of sleep. Just somebody to be there for me.
I was living with my one of my friends. She was very supportive, too. She would come in and check on me and be there for me, but I just knew that I needed to go home on the weekends to my mom’s when I would get treatment.
Work & Finances
Were you able to work through chemotherapy?
I did work through treatment. I know that I wanted to work. I was given that option where I could take the disability leave. My work was amazing with that, but I was like, “No, I don’t want to not work.”
I want to work. I want to be able to get up and try to live life still normally as much as I can. If I can get up and go to work, I want to do that. They were so great about that.
There were days that I wouldn’t go to work or I would have to leave early because I didn’t feel well, but I know that I wanted to work and try to make life still very normal, as much as possible.
I work at a pediatrics office. I work at the front, so it was a little scary thinking that here I do work in a pediatrics office and that there’s a lot of sickness going on, but it was nice because I didn’t have to work with the patients face to face.
My work was allowing me to do more paperwork, phone calls, a lot of that, away from patients so that I wouldn’t get sick.
»MORE: Working during cancer treatment
Financial toxicity: paying for cancer treatment
I’m still paying medical bills, and my insurance covered a ton of it. Thank goodness for insurance, but I’m still trying to pay medical bills to this day.
That’s why I still wanted to work, because I wanted to make that full amount instead of a certain percentage that I would only get if I took the disability. I knew that I needed to do that.
I still had rent to pay for and electric bills — like bills are still on top of the medical bills — so I need to still work. I felt like if I was doing that, I was going to be okay.
Any advice or tips on the financial aspect?
Hopefully, wherever you are getting treatment, there are people who can help you out with fundraisers. I wish that I had done some type of more fundraising when I was going through treatment to help these bills, but it was hard for me to do because my mind was just so focused on other things.
Luckily, I had my parents there, who have helped me out anyway, and I still am very thankful for my insurance. They did help a lot. When I did the egg freezing, I was able to go through organizations.
So just look for fundraisers and donations and anything like that around your area. Hopefully they can help out in some way.
Fertility & Egg Freezing
How did you approach the issue of fertility preservation?
The day of my first appointment with my oncologist, she had brought up this to-do list before I start treatment. On there was the issue of fertility, and she said with my cancer and the treatment that I’m going through, I would only have a 4% chance of infertility. I didn’t even want to take that chance, because I’d make it very clear in my future I want to have a lot of kids, and I want to have a family.
I didn’t really want to take any percentage, so she gave me all the information. I went right over to fertility center, and they were able to help me.
It was a very quick process, a 2-week process, with blood work every day. Then it was lot of hormonal shots that I had to give myself. That was a whole process itself, and that was before I even started treatment.
I had to go through all that, and they were able to retrieve 26 eggs to freeze. It’s just good to know that I have those in case I get a second type of cancer before I’m able to have kids, because I’m so young.
»MORE: Fertility preservation and cancer treatment
Any tips to anyone else considering freezing their eggs?
If you go to a fertility center that has the exact same organizations that will help pay, I would definitely go for it if you can get help with the costs.
I knew that I was very lucky that I had people who were helping out with the cost, so I was going with it. I was able to do it, and I did feel much better.
You most likely don’t need to do it, but I just didn’t want to put any percentage of infertility in my mind while I’m trying to go through treatment. I just knew, “Okay, this is the time. I’m going to do it.” I was lucky to have a lot of help with the cost.
»MORE: Read a patient’s detailed IVF journal

Survivorship
Any last advice in general?
Being diagnosed with cancer is definitely a scary thought, and it’s a very scary process. You don’t really know what you’re in for, but you do have a lot of people there for you. Just stay strong.
I think the attitude of it all through the whole process definitely helps a lot. Truly feel your feelings while going through everything; don’t hold anything in. Just know the positivity really does help, and it makes a huge difference through the whole treatment process.
Survivorship can be something you have to learn and figure out
As soon as you finish treatment, you’re not just done. There are so many things that you have to go through even after that.
I think a lot of people who haven’t gone through cancer don’t realize that. Even though this is amazing that person is in remission or they’re cancer-free, they’re still going through so much, and they still need that support.

Inspired by Danielle’s story?
Share your story, too!
Classical Hodgkin’s Lymphoma Stories
Jessica H., Hodgkin’s Lymphoma, Stage 2
Symptom: Recurring red lump on the leg (painful, swollen, hot to touch)
Treatment: Chemotherapy
Riley G., Hodgkin’s Lymphoma, Stage 4
Symptoms: • Severe back pain, night sweats, difficulty breathing after alcohol consumption, low energy, intense itching
Treatment: Chemotherapy (ABVD)
Amanda P., Hodgkin’s Lymphoma, Stage 4
Symptoms: Intense itching (no rash), bruising from scratching, fever, swollen lymph node near the hip, severe fatigue, back pain, pallor
Treatments: Chemotherapy (A+AVD), Neulasta
Brescia D., Hodgkin’s Lymphoma
Symptom: Swelling in the side of her neck
Treatment: Chemotherapy: 6 rounds of ABVD









Leave a Reply