JJ’s Stage 4 Colorectal Cancer Story
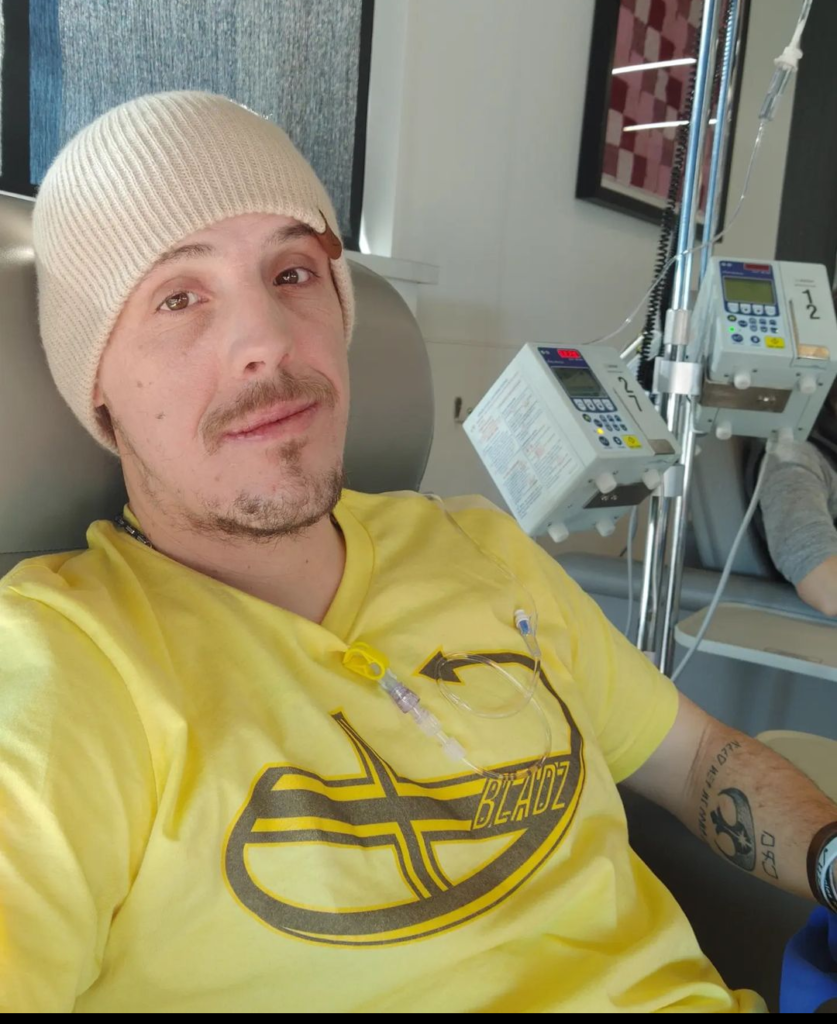
Despite no known family history of cancer, JJ was diagnosed with colorectal cancer at only 27 years old.
After brushing off abdominal pain for months, JJ went to the doctor, which led to an emergency CT scan and colonoscopy.
JJ found out his cancer was caused by Lynch syndrome, an inherited disorder that increases the risk of getting cancer. The doctors tried 5 different chemotherapy regiments, but they were all unsuccessful.
Finally, JJ joined a clinical trial that has kept his cancer from spreading further, beating the 25% odds of surviving past 5 years after diagnosis.
JJ shares the reality of being on lifelong chemotherapy, finding support in Man Up to Cancer, starting his advocacy journey, and the importance of listening to your body.
I’m beating the odds every single day I’m alive.
JJ S.
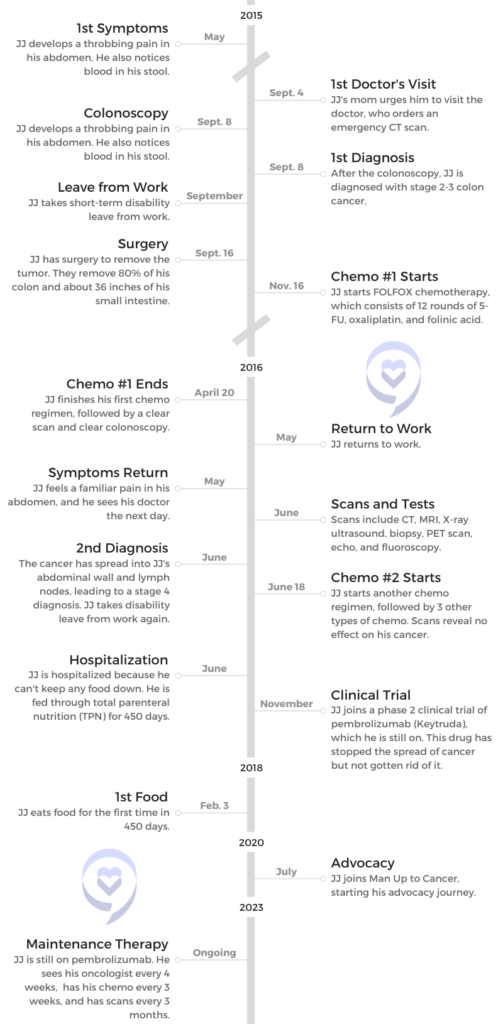
- Name: JJ S.
- Diagnosis (DX):
- Colorectal cancer
- Stage 2-3
- Stage 4
- Colorectal cancer
- 1st Symptoms:
- Throbbing abdominal pain
- Blood in stool
- Age at DX: 27
- Tests for DX:
- CT scan
- Colonoscopy
- Treatment:
- Surgery to remove tumor
- FOLFOX chemotherapy
- Fluorouracil (5-FU)
- Oxaliplatin
- Folinic acid
- Pembrolizumab (Keytruda)
- Infusions every 3 weeks
This article has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Pre-Diagnosis
Introduction to JJ
I’m JJ Singleton. I’m from a small town in western North Carolina. I usually just say I’m from near Asheville because everybody’s heard of Asheville. Nobody’s heard of Canton, North Carolina, which is a town of about 3,000 people. [I] grew up in a community of about 1,000 people, so [a] very small town, country oriented.
I was a huge sports person. [I] grew up playing basketball, football, ran track, [and] played college football for 2 years before too many concussions made me quit.
Other than that, the only really good thing about me [is] I’m a huge nerd, like “Harry Potter,” “Lord of the Rings,” [and] “Star Wars.” I’m very unashamed [and] just admit that I love all of that, and it’s one of the joys of my life.
Then [with] “Star Wars,” I became a huge fan of it after I got sick. I associate falling in love with it as something that helped save my life. [It] allowed me to escape the whole cancer thing.
[I] even got a tattoo of [the] phrase, “Never tell me the odds.” One of the authors actually even put my Instagram name in a book for “Star Wars.” It’s been a huge part of my life the last few years.
1st symptoms
It was around 2015, a little bit before that. After I got hurt playing football — that was like 2008 — I just let myself go. I started eating a lot, quit working out (I lived in a gym while I was playing and athletic), [and] drank way too much in college.
At the beginning of 2015, I was at 315 pounds, and I decided to get healthy again. I started going to CrossFit with one of my old football coaches, eating healthy, and started losing weight.
Around Memorial Day of that year is the first time I felt a throbbing in my abdomen. Me, typical stubborn male, [thought] I pulled a muscle because I was doing Tuesday workouts, getting ready for a competition in August.
All summer, I associated it [as being] a pulled muscle or my stomach was adjusting to a totally new diet with actually eating healthy. Through that summer, the pain would come and go. It would get worse. I was starting to have issues using the bathroom.

I did the competition on August 1st. After that, my body crashed. I couldn’t eat, I couldn’t drink without becoming violently sick to my stomach, and I was losing about 5 pounds a week at that time because I just wasn’t able to eat. I was dehydrated every day.
I would lay in bed and look at my symptoms, and the bottom was always colon cancer or cancer. I was just like, “That can’t can’t be me.”
Then my mom made me go to the doctor, and by that point, I could put my shirt up against my stomach and you could see the tumor throb through the skin. As soon as the doctor looked at that, he was like, “You got to go get a scan right now.” That’s kind of where it all started.
The Diagnosis
How much time passed between your symptoms starting and going to the doctor?
It was from Memorial Day, so May to September 4th, because September 4th is when I went to the doctor and went through the scan.
They said there was a mass, and then as soon as he said that back in the doctor’s office, all the dots connected from the last few months of what I was dealing with. Before I even had to go get a colonoscopy a few days later, because it was Labor Day weekend, I knew it was cancer.

What was that feeling?
It was just a feeling that it all made sense. Why I was going to bed at 7:00 when I was dead tired, [and] why I was having so much pain and not using the bathroom and losing weight. Just everything that I’d been going through that I had come up with some excuse for in my head.
I grew up in a culture where we didn’t go to the doctor. I’ve been to the doctor to get sports physicals and then when I broke a finger in middle school. Other than that, I never really went to the doctor for anything because it just wasn’t something we did.
When [my mom] made me or told me I was going to the doctor, I knew I looked bad. I knew it must be really bad to get told that I was having to go the next day.
What happened after going to the doctor?
It was a whirlwind because, like I said, that was on the Friday of Labor Day weekend. By the time that day ended, I’d already had this colonoscopy scheduled for the Tuesday when everybody started back to work after Labor Day.
I got to drink the prep on Labor Day there. Usually that’s one of these weekends I look forward to in the year the most because it’s the opening weekend of college football. Months before it, [I already] took a long weekend that weekend.
Most people go to the lake or the beach. I sit in my living room and drink beer and watch college football all day. I didn’t watch one single game [because] I was in so much pain. I’d already told my family and people that I knew what it was.
[I was] going through that and just feeling like, “How could I have cancer at 27 years old?” Then that Tuesday happened. It was [the] colonoscopy, meet with the surgeon the next day, and within a few days I was in the hospital for surgery.
My colon was about 95% blocked.
They said I was the youngest person that they had seen in a long time, just because we’re such a small area. They were like, “We don’t know why you’re so young with this massive tumor.” Then they’re like, “You should have come in months ago, as soon as you felt the pain.”
I was like, “Well, now I know that, but back then I wasn’t thinking I ever needed a doctor.”


Then they were like, “This has probably been growing in your colon for years to get to this big.”
I was just in disbelief. I was just finally getting my life healthy.
Did you feel pain or anything before Memorial Day?
No, because the way it grew and the position it was, as soon as it got to that certain size is when I felt it. It was in there and growing. It kind of grew horizontally through the colon. Then it just started growing.
It was slow growing until a certain point, and then it just started growing exponentially. As soon as it got big enough to where it started obstructing and pushing through the colon into the small intestines is when I started feeling the pain.
How did you process the diagnosis?
Very badly at first. I was in disbelief. I went numb. Even when I was going to tell my grandparents and my dad and stuff, I was just kind of like, “Okay, yeah, this is it, and I don’t know what’s going to go on.”
Then as the days went by, I went into that kind of sports mindset I’ve had my whole life, like, “Okay, this is what they’re telling me. I’m going to do surgery, recover, 12 rounds of chemo, and then hopefully you’ll be done.” I had a game plan.
I was just like, “I’m going to put my head down, put the blinders on, get through it, and then get my life back.” [That] was like the game plan for me then. I know looking back now that probably wasn’t the healthiest thing, because I was like, “I could shoulder it all. I don’t need help.”
My family was there to help me, to take me to chemo, and be there at the hospital, but I was like, “I’m going to get through it. This is going to be a very small chapter in my life, and I’m going to go back to being who I am.”
»MORE: Patients share how they processed a cancer diagnosis
Treatment
Surgery and genetic testing
After I had the surgery, I ended up being in the hospital for 16 days because my body did not like to heal right. They had to go back in for a second surgery to make sure there was no leakage because I had bile that was just building up in my abdomen.
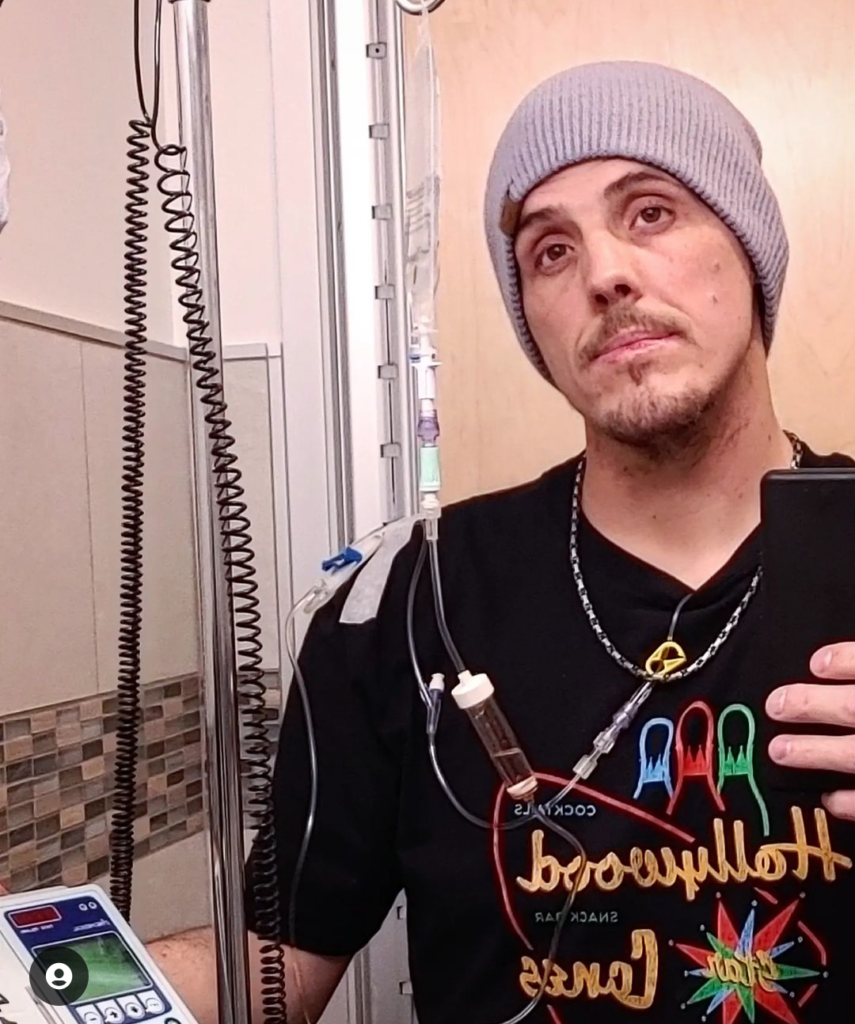
That was the first sign that my body did not like surgeries and hospitals, because I’ve been in there way too much. After that, they were like, “You are so young. We want you to go to Duke just to see why you have this cancer.” There was no real family history of it.
I went to Duke. They got me genetically tested. I have Lynch syndrome, which is the reason I got cancer so young. The reason we didn’t know anything about it is because we had such a sketchy family history in parts.
My dad’s side of the family didn’t go to the doctors at all. My grandma had some brothers that died early. Then on my mom’s side, my grandma didn’t really know much of her family history just because back then they moved, and there were no records of it. Somewhere down the line it came through, and it just decided to pop up with [me].
Before 15 [or] 20 years ago, if anybody in the family died, they weren’t getting [any] autopsy or anything done. They were just putting them in the coffin, burying them, and that was it.
I had no idea. Genetics has come so far.

Did you know about colorectal cancer?
Not at all. The only thing I’d ever really heard about it is older people got it, and all the TV sitcoms and stuff when people would make fun of people, [like] “I have to go get a colonoscopy.” That’s all my whole knowledge of it was before this.
Did you research or ask questions?
I asked questions. At that time, my mom was coming out to the doctors and stuff with me, so she would ask a lot of the questions. I realized quickly after a while in the doctors’ offices, I would just go numb. I’m like, “Tell me what I’m doing, and then y’all can talk about the questions.” I would research.
I never liked talking about my bowel movements or what was going on with my colon or anything like that. I’ve realized a lot of people are like that. That’s been one of the things, too, about breaking the stigma against colorectal cancer. You hear people all the time [who] have no issues talking about leukemia or breast cancer, but people don’t want to ask you about your bowel movements.
Having trouble asking for support
My family has always been supportive. They were like, “You can talk to us about anything.” Still, it’s like they didn’t really understand it because they’ve never been through it.
At that time, I had no idea there were so many organizations and support [options] out there. Like I said, I had the blinders on. I wasn’t going to ask for help. I was just like, “I’m doing this.” My ignorance led me not to search for message boards and organizations at that time. [I] tried to shoulder it all myself.
Starting chemotherapy
After I got out — I got out around the beginning of October — they were like, “Take 6 weeks to heal.” That’s when I went to do the genetic testing. Then my oncologist in Asheville was really good friends with my one in Duke, so they kind of worked together as a team.
[They] allowed me to do all my treatments 30 minutes away in Asheville instead of 5 hours away in Durham. They came up with a plan. They thought they had all the cancer out from the surgery.
Let’s just go through the 12 rounds of FOLFOX, which is the normal first line of defense of colon cancer. We started that in November of 2015. I was not ready for chemo. You go through the whole education of like, “Okay, this is what chemo can do to you. This is what it’s going to feel like.”
It’s all made by people who’ve never had it. I was like, “Okay, it’s going to feel like a bad hangover. I went through 5, almost 6 years of college. I know what that feels like.” [I] was totally wrong. [I] went in there that first time, and it knocked me for a loop. I was not expecting that kind of feeling.
Drugs in your chemotherapy regimen
The FOLFOX was the 5-FU, oxaliplatin, and [fluorouracil]. I can’t pronounce some of the drugs’ names. Oxaliplatin was the hard, harsh drug of that cocktail.
What side effects did you have?
I had horrible nausea there. Within 30 minutes of getting the drugs in there, I could start feeling my stomach do flips. [I] had diarrhea constantly [and] had no appetite. I had to force myself to eat a little bit or drink.
Then with FOLFOX, it has a cold sensitivity. You can’t drink anything cold other than lukewarm temperatures, which I hated. It was a chore to drink room-temperature water for 3 or 4 days. I’ve had horrible mouth sores since the very beginning.
My whole family, we’ve always had fever blisters and sores on our mouth, so bad genetics to begin with. Then you had chemo and the anxiety and stress that that brings. That was one of the things that has impacted me to this day.
It started by just having [what] almost felt like fever blisters on my lips. Then as the days went by, I would feel sores on the gumlines, and then my tongue would lose all its taste buds and feel raw. Then I would feel like I have strep throat with sores down my throat.

I couldn’t eat anything other than soft foods. I’d been so used to that with eating after my surgery. I was so sick of it, and it was harder to get the proteins and the nutrients you needed to help your body recover. It just started a long journey of really not enjoying eating.
»MORE: Cancer patients share their treatment side effects
What helped with side effects?
They gave me some medicine to help with the neuropathy, and it kinda seemed to help a little bit. I still have neuropathy to this day. The nausea medicine [helped]. I started taking the pre-nausea meds the night before and kept [taking] it every 6 and 8 hours through 3 days, even if I wasn’t sick at the beginning, just to stay ahead of it.
Then I started doing the edibles to help with the nausea. That was one of the few things that allowed me to be hungry and help with the nausea, because I was losing weight at first. Those were really the things that kind of helped.

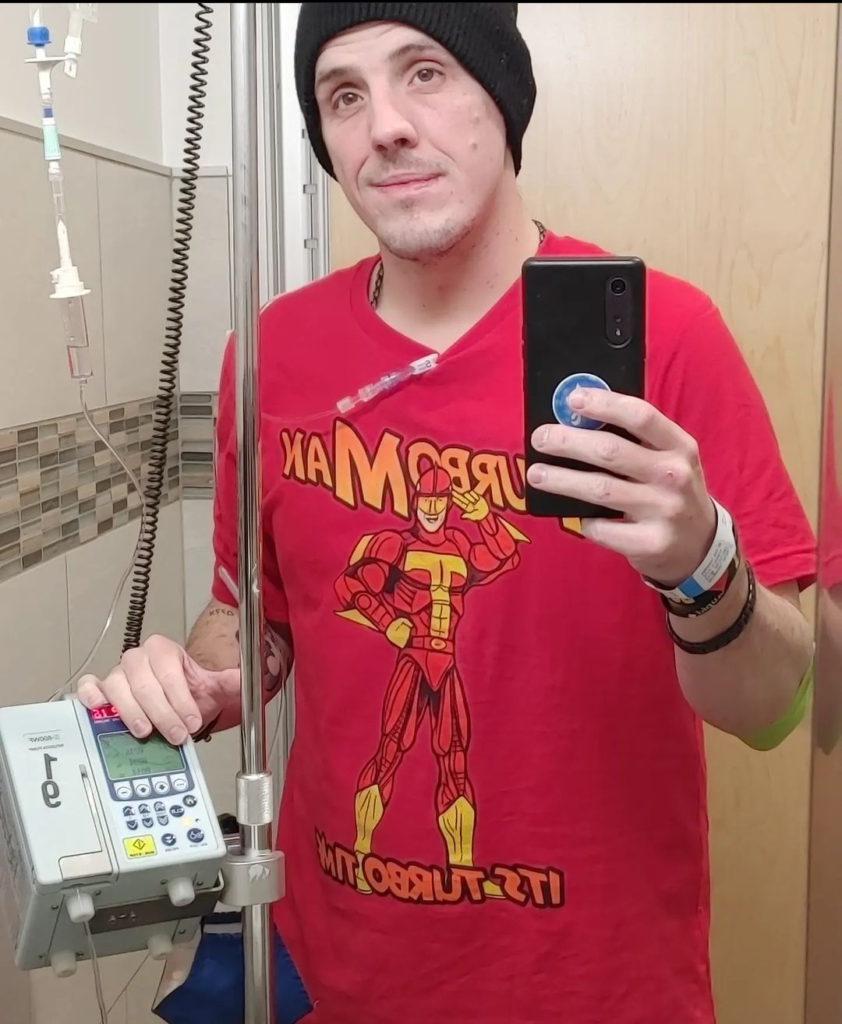
Relapse and Clinical Trial
Relapse
[Chemo] was 6 months, 12 rounds of that. I finished around mid-April of 2016, and my scan was good right after that. I had a colonoscopy a couple of weeks later. It was clean, so I took a little vacation. [I] started back to work at the beginning of May.
About 2 weeks later — so it was about 6 weeks from the last chemo — I woke up [and] felt the throbbing in my abdomen again. This time I was at the doctor’s at like 6:30, waiting on [my surgeon] to pull in because I was like, “I’m not waiting again.”
That kind of started the next couple of weeks of every kind of scan, biopsy, [and] a trip to Duke. We learned that the cancer came back, but it wasn’t my colon this time. It spread to my abdominal wall and lymph nodes throughout my body.

What stages were your diagnoses?
[The first diagnosis] was stage 2, borderline stage 3, because it spread through the colon, but it hadn’t spread into any lymph nodes. It hadn’t spread into my small intestines. It was just on the outside.
They took around 80% of my colon and about 36 inches of my small intestine out just because that’s where the tumor had grown through. But I just had stage 2 then, and then it came back as terminal stage 4.
What was going through your head with your second diagnosis?
On the way to the doctor’s office, I tried to convince myself it’s scar tissue. I had such a major surgery. They cut me twice. Scar tissue built up and popped. I’ve heard that happen in people. I tried to convince myself that, but by the time I got to the doctor and I could feel the throbbing, it was so similar. It brought back all the memories of the summer before.
I was just like, “I know this is back. I know.” At that point, my mindset was like, “Another 6 months of chemo.” Then I went to the doctor’s and the scans, and it wasn’t until I went to Duke around the second week of June when I realized and they told me.
They’re like, “All right, there’s no cure for this now. You have this for life because of the way the tumor came back.” It’s not in a solid organ in the tumor. It wasn’t a solid tumor. It’s like a non-solid area of liquified tumor masses that we could not remove at this time.
They’re like, “You’re going to be on chemo for life.” That’s when they were like, “You got to battle.” The odds were about 25% to make it 5 years. I was numb, went back to the hotel in Durham, and just kind of just sat in the shower because at that point, the tumor was growing.
It was causing me severe back pain. My life at that point was pretty much laying on a heating pad, taking pain medicines, taking hot showers, and trying to get a couple hours of where I wasn’t in extreme pain.
I was numb to the world. [I] couldn’t talk to people, couldn’t text even. I was getting messages. My mom was there [for the diagnosis]. I was like, “You tell people. Let them put it out there.” I couldn’t even pick up my phone to answer.
»MORE: Breaking the news of a diagnosis to loved ones
Getting through feeling numb
It took me a long time. Actually, it took me many years because after I got that, I was like, “Okay, I’m just going to go to treatment.” Through the next about 6 months until around November of 2016, it was just solid bad news.
I would do a couple of rounds of that chemo, [get a] scan, [and it] wasn’t working. It was growing. I was in more pain. Same thing. By October, I literally wasn’t leaving my house except to go to doctor appointments. I was all day on the heating pad because my back was in so much pain.
[I was] going through about a bottle of 100 pain pills in a week, and that wasn’t even taking the edge off. It allowed me maybe a couple of hours of sleep at night. I was hopeless, and then it got really bad. The cancer grew into my stomach where it empties into my intestines and closed it completely off.

I went to the hospital because everything I was eating was sitting in my stomach until I threw it up. I spent almost a month in the hospital. Everything kind of happened really quick around then.
Right before that happened, I made the decision to apply for a clinical trial because all the FDA-approved chemos didn’t work, and it was either hospice and dying or try this clinical trial. That was my only 2 options.
They were like, “This is your last chance. If this doesn’t work, you’re too far gone. You will either be dead by the time we realize it didn’t work, or you’re going to die.” I was like, “Okay, we’ll go for it.”
[I] realized how crazy clinical trials could be. The only thing I ever heard about was on TV and thinking I’m a lab experiment, which [is] totally wrong. [I] realized I have complete control of it, but realizing that I’m doing a drug that they don’t know the side effects for. I’m in there, filling out hundreds of pages of possible side effects, and I give my consent to all of them. [It] was a waking up moment.
The clinical trial
It was a phase 2 trial. They knew it worked. It was a drug. It was pembrolizumab, or Keytruda, which was the drug, and it worked in other cancers. The type of cancer that worked is where it’s mutated in the microsatellite, to get really technical.
I was accepted into it, but it was a stage 2 trial, so I had to go and fill out everything. Before I could get my first infusion of it is when I got rushed to the hospital, where I couldn’t eat anything. The pain was so extreme, and I was losing weight again. I lost about 60 pounds in 2 months from everything.
They put me in the hospital, and they’re like, “All right, we got to push back your treatment because we got to figure out some way.” They tried a feeding tube, and it just kind of balled up in my intestines, so they had to take all that out.
It ended up they had to put drainage tubes into my stomach and my intestines to drain the bile and just the digestive fluids. I got fed through stuff called TPN and ended up being on that for 450 days. I went 450 days where I did not eat solid food. I didn’t eat anything. I got 15-hour infusions of that every single month.

Being on treatment for life
When that started in the hospital, they were like, okay. Then I started the clinical trial while I was in the hospital, and I’m still on that drug. It worked. I’m part of the very weird small percentage where it worked just enough to keep the cancer from spreading, but not like it does the 99% of people where it either cures it, [or] takes the cancer away. That’s why I’m on it for life or until it quits working.
It’s an infusion. I go there every 3 weeks right now to get infusions. Since that time, I’ve had spots pop up, where I’ll get drugs added to take them away, just depending on what pops up and what doesn’t. That’s my baseline because the mass of non-solid tumor in my abdomen, that’s what the immunotherapy is keeping from spreading again.
Processing the choice between hospice or a clinical trial
For me, it was a quick decision because I was like, “I don’t want to die right now.” At that point, I was still like, “I could still be doing this and fight.” At that point, all I wanted to do is live to the age of 30. If I could get another year and a half, I’ll be okay, so If this clinical trial can do that…
In my head, I was like, “I can deal with the pain and the life I’m living right now at least another year.” I wasn’t even doing it for me. It was for friends [and] family, just so I could be there a little longer. That was my mindset of why I just automatically said, “Yeah, let’s do the clinical trial. I wasn’t wanting to go to the hospice and die in 2016 yet.
Did the clinical trial make you feel better?
Over the course of the next year, it was weird because the year I was on TPN, I had a pain pump, too, because the pain got so extreme. I couldn’t do anything. Over that 14 months, it shrank it enough to where it’s not the constant horrible pain.
I still feel pain in my back, in my abdomen, every single day, but it’s something I can live with. [I can] still get up and go on a walk or go sit and watch a movie and be okay with it. When I think about it, it’s still there, and some days are worse than others.
Finding Support
What helped you?
All that help [from Man Up to Cancer] happened a few years later. That started about 2 years ago in 2020. From the time I started the clinical trial and went through that 14 months, that was the darkest time.
I was laying in bed about 22 hours a day. This life was not living. [I] had dealt with a lot of suicidal thoughts [and] came very close to committing it and not being here. Luckily, there were a few people I would talk to online because I was on my phone or in bed all day.
That helped, but I was still stubborn, like, “What do I matter? Why would anybody want to listen to me, a person from a town of 3,000 people? What experience do I have to help people?”

I was just so deep in my own head and knocking my self-worth down and not believing anything good could come from it until about 2020, when I started having people and started kind of opening up.
Then Joe Bullock, who’s the lead administrator of Man Up to Cancer with Trevor [Maxwell], asked me to join the group. I’d joined groups earlier, and I would leave within a week because it was just so much about this drug and this treatment and this. I was like, “I hear that all the time anyways. I don’t want to be in a group with it.”
That group changed my life. I started [and] became comfortable talking to people. Through that group and Joe and Trevor, they got me to apply to an ambassadorship with Fight CRC, which I got. I was an ambassador there, and now I’m part of another organization called the Colon Club and Colon Cancer Coalition.
It’s kind of snowballed really quickly over the last 2 years to where I’ve got to do amazing things, [like] go on travel that I’ve always wanted to do. It’s crazy how just saying yes to one thing and joining one group kind of snowballed into changing my whole life.
Man Up to Cancer
Man Up to Cancer is just a group. There’s a website, a podcast, and then a private Facebook group where you have to be a man and you’ve got to be dealing with cancer or be a caregiver to somebody with cancer. It’s just a place you can go there and be yourself.
There’s so much stigma and everything to a man, like we’re supposed to shoulder everything. We’re not supposed to show emotions. Especially from the culture that I grew up in, that Southern Appalachian person, you’ve got to be tough. You’ve got to be the leader. Everybody, rely on yourself.

You can just go in there, and you can be sad, be angry, be happy. It’s a free place to share the very dark humor that cancer patients have and not be judged for it, because other people don’t get it. You can talk about stuff that has nothing to do with cancer in there.
It was just kind of like a group of friends that I had that actually understood what I was going through and then showed me that I wasn’t alone and there were people and groups that accepted people out there.
How did being open to support help you?
It’s helped me so much, between the groups, then admitting that I needed to go to therapy, and becoming an advocate for men getting professional help and therapy and then being in the groups and opening up.
It’s made a total difference in my life because now I have a reason on these bad days — like tomorrow, when I’m feeling horrible from yesterday’s chemo and I don’t want to get out of bed, I can roll over and check my phone. If I’m in a down place, I can message somebody, and they’ll understand.
Then I can be that person on the weeks in between chemos, where people can see what I’ve been through. That was a big thing, too, because a lot of people started following me the last year. They see me, and they’re like, “How can I ever become as open and okay with all this as you are?”
Then I tell them, “I went through 5 years of this, where I was the exact opposite of what I am now.” Helping people get to that point a lot quicker than I did is a big thing.
Going to therapy
I started that before I joined any group. I realized that the thoughts I was having in my head about not wanting to live terrified me enough to where I needed help, just because I didn’t want to put that burden on other people of walking through the door and seeing something that I did.
It just scared me enough to realize that I needed it, and be damned what anybody else that still has that stigma said about it. People tell me I’m strong, tough all the time, but the toughest thing or the bravest thing I ever did was admit to myself I needed help and I couldn’t do it alone.
I still deal with it every day, but it’s made me realize that mental health is not a start and end point. It is a very fluid kind of process. I can go through days or a week where I’m feeling horrible, and then you go through [it and] you talk. The next day, you might feel a little better. That’s okay. You don’t have to make improvements every single day.
Reflections
How are you doing now?
Actually, I just had my 3-month scans last week. [I] got the results 2 days before Christmas. Everything’s stable. The main tumor’s stable. I have spots that pop up. I have a couple of nodules in my lungs and some stuff that are too small to do anything about right now, so we just add those to the watch list.
As of right now, I’m going to keep the same treatment I’m on for another 3 to 4 months until my next scan. It’s working. Still working. I just completed my 126th round of chemo immunotherapy treatments. We’re happy.
The side effects suck, but they allow me to be alive, and I have them every 3 weeks. I usually get about 2 weeks of — I don’t say feel good because I never feel really good anymore — feeling okay enough to allow me to get out and do what I need to do. I can travel if I need to.
Finding comfort in “Star Wars”
It was during that 14 months of not eating. It was around February of 2017. There was a snowstorm here, [and it] knocked out the cable. I had nothing to watch. In the middle of the night, all I could hear was that TPN pump going.
My uncle, who I lived in their basement apartment at the time, had recorded the 6 “Star Wars” movies. I’d watched bits and pieces of it, but I’d always been more “Harry Potter” and “Lord of the Rings.” I was like, “I’m going to watch it.”
Next thing I know, I watched all 6 in a row. I looked back after I got done, and I was like, “That was the first 12-14-hour block where I wasn’t in my head so much and just thinking about what I’m dealing with.”
That started where I watched all the movies, all the cartoon TV shows, and then I found out there were books. There’s hundreds of them, so I just started reading those. I would post a picture years ago of whatever book I was reading while I was getting a chemo treatment.
One of the authors, Claudia Gray — she’s my favorite “Star Wars” author — is seeing that. [She] started following me on Instagram. Fast-forward to last year, January, she had just released a new book I was going to buy, and I get an email or a DM being like, “What’s your address? I’m going to send you a signed copy of my new book.”
That’s all I thought it was — late Christmas gift, just appreciation. I get it and I open it, and it’s like, “Turn to page 18 for a surprise.” I read it, and at first I thought the droid’s name — [because it’s] spelled out like not how I spell my Instagram name, it took me a minute — I’m like, “That sounds very familiar.”
The next sentence has it exactly how I write it on my Instagram, and it made me proud. [It] took my breath away. I can look up on their official Wikipedia stuff on the internet, and it has it there. It was amazing and just something that I tell everybody about.
Chemo routine
I got, “Never tell me the odds,” tattooed on my arm just a few weeks ago. People notice I do those pre-chemo thoughts. That is the last thing or first thing on my mind right before I open the door to go into chemo every morning.
But before that, I have the same routine every single chemo treatment. I go and get my Starbucks coffee. I get to the cancer center about an hour early, I sit in my car and drink it, and I read whatever “Star Wars” book I’m reading at that time.
That just allows me 30-45 minutes of not thinking about what’s coming up next. Then I get done, close it, and the first thing that pops to my mind is what I talk about. Then I go get chemo.
Beating the 5-year odds
I did. I passed that a little over a year or about a year and a half ago. I’m beating the odds every single day I’m alive.
Advice for patients and caregivers
First thing is don’t isolate. Isolation can cause mental health issues, but it also will affect your physical [body] and the way to heal. That’s a big thing in Man Up to Cancer. You don’t want men to isolate because it actually dramatically decreases your chance to recover or to do as good on chemo.
That is my big thing. Everybody knows that cancer is physical. You see the chemo effects and the physical effects. But for me, the mental part of it is something I was not expecting [and] did not have any knowledge about. It’s what threw me for more loops than anything.
The fact that I can help people understand that it is going to be a physical battle. The mental part of it is going to throw you for a loop. You’re going to get depressed, feel alone, no matter if you’re in a group of 1,000 people.
Cancer’s so individualized that everybody feels alone at some point, and just know that you’re not. There’s so many people and groups that you can find your little niche in it, and don’t be afraid to ask for help.
Listening to your body
Anything that feels off, anything that feels similar to what you’ve felt before, I’d say go directly back to the doctor. I’ve known a lot of people who’ve had horrible experiences with doctors not believing them.
Demand a second opinion. Go to a second, third, fourth doctor. You know your body, and 99% of doctors have never been through cancer. They could do the medical side. You could read about it in textbooks, but they don’t know the feelings that we know. If you feel anything or if you see one symptom, it’s always better to be safe than sorry.

Inspired by JJ’s story?
Share your story, too!
More Colorectal Cancer Stories
Ken S., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Frequent loose bowel movements, intermittent rectal bleeding, fever and chills, rapid and significant weight loss
Treatments: Surgeries (total colectomy, liver resection), ablation therapy (liver and lung ablations), chemotherapy (FOLFOX, capecitabine, fluorouracil), monoclonal antibody (panitumumab)
Carrie H., Colon Cancer (Signet Ring Cell Carcinoma of the Colon), Stage 4 (Metastatic)
Symptoms: Persistent upset stomach, significant bloating
Treatments: Surgeries (colon resection, oophorectomy, hysterectomy, laparoscopic tumor resection, liver resection, kidney resection), chemotherapy, radiation therapy
Nathan G., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Persistent heartburn, feeling full after eating, severe abdominal pain
Treatments: Surgeries (colectomy, cytoreductive surgery, lymphanadectomy), chemotherapy (FOLFOX, HIPEC or hyperthermic intraperitoneal chemotherapy)
Mariana T., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Bloating, anemia, appearance of blood in stool
Treatments: Surgeries (bowel resection, oophorectomy, salpingectomy), chemotherapy (oxaliplatin, fluorouracil, FOLFOX), immunotherapy (bevacizumab)
Helen D., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Pelvic pressure and pain, burning with urination, bloating, constipation for a short period, low energy or fatigue, discomfort sitting, night sweats
Treatments: Chemotherapy (FOLFOX, FOLFIRI, hepatic artery infusion pump therapy), targeted therapy (panitumumab), surgeries (liver resection and ablations, colon resection, full hysterectomy)







Leave a Reply