Empowering Men with Cancer | Cancer Friends
Featuring Trevor Maxwell

The Patient Story’s series “Cancer Friends” features Andrew and Esther Schorr. They co-founded PatientPower.info, a resource for other cancer patients and caregivers to help them through their diagnosis and treatment.
Watch other “Cancer Friends” episodes on our video channel here!
This segment focuses on Trevor Maxwell, the founder of Man Up to Cancer. After being diagnosed with colon cancer, Trevor went to a dark place. Support from his family led him to seeking help. Trevor noticed how few men were engaging in online support groups, so he created Man Up to Cancer.
Trevor shares his journey, how he started a group for men to be vulnerable and how the experience has changed him. He also details how cancer has given him a more present and grateful mindset.
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.

Introduction to Trevor Maxwell
Andrew Schorr, The Patient Story: Hello, It’s Andrew Schorr with another edition of our Cancer Friends series. I’m in San Diego, but joining us from Cape Elizabeth, Maine, is my friend Trevor Maxwell. Trevor, thanks for joining us.
Trevor Maxwell: Pleasure’s all mine, Andrew. So great to see you. Thanks for having me.
Andrew, TPS: It’s great to see you. Trevor, I’m really delighted that we can tell your story, which has been quite a journey.
You have really been a pioneer in giving voice to men like you and me, living with cancer, and saying that it may be a little different or that men maybe didn’t speak up so much. Maybe we were keeping a lot inside. I’m sure you’ve seen it all, but it started with you. We should also mention that you have a new book. What’s the name of the book?
Trevor: The book is called “Open Heart, Warrior Spirit: A Man’s Guide to Living With Cancer.” I am excited to get it out to the world.
Andrew, TPS: It is coming out to the world now in December 2022, and people can get it through Amazon, etc. The book is just an example of where you’ve come. Let’s back up. You’ve been a newspaper reporter in Portland in New England. You’ve been in public relations. [You have a] wife of many years now, and you’ve been together 30 years, married 20. You had 2 little girls.
1st Symptoms
Andrew, TPS: What happened? You had a cancer diagnosis. Tell us how this happened.
Trevor: In the spring or late winter — this would have been right around January [or] February 2018 — I started to just get super, super fatigued. As I look back on it, I know that I was getting more and more fatigued throughout 2017, but I was 40 years old [and] working full-time as a public relations and freelance writer. My wife was working full-time as a teacher, and our daughters were 12 and 10 at the time.
As I started to get more and more tired, I just chalked it up to midlife fatigue. I had had some bouts of depression [and] anxiety prior to cancer, so I just said, “Well, this is mental health.” We were just kind of cruising through life.
The biggest things I identified mostly as [were] being a husband, dad, also a writer, and someone who enjoyed writing about others and putting the spotlight on other people.
Then this fatigue just kept creeping more and more. I’d walk up the stairs, and my heart is just kind of pounding out of my chest. I was 41 and I had not seen my primary care doctor in several years. I wasn’t doing check-ins at that point or annual physicals because I didn’t really feel like I had a need to.
I did finally call my primary care [physician], and she said, “We need to do some blood work. [We’ve] got to figure this out.” [They] did some blood work. [It] turned out I was super anemic [and] hardly had any iron in my blood. She said, “We need to get you a colonoscopy. Have you noticed any bleeding anywhere?” I had not.

Colon Cancer Diagnosis
Trevor: I went in for a colonoscopy. Even at that time, between my primary care doctor and the gastroenterologist, no one was thinking [it was] cancer. I had looked it up, like, “What are the causes of blood loss?” You know, a couple of things. Cancer, of course, is on there, but it certainly was not on the radar.
March 22, 2018, I went in for a colonoscopy and had the procedure. Afterwards, the nurse took my wife and I and said, “You need to see the doctor.” I went into the doctor’s office, and he said, “I’m sorry to tell you this, but you have a pretty large mass in your ascending colon.”

At the time, I couldn’t tell you much about where the colon was or what it did. He said, “You have a mass. It’s about 9 or 10 centimeters, [about] 4 inches plus. We’re going to need to refer you to a surgical oncologist, and we’re sending off tissue samples for pathology.”
He didn’t say the word, but I’m hearing all this stuff like “oncologist.” I’m just like, “Are you saying that I have cancer?” He looks at me and says, “Until the tests come back, I can’t tell you 100%, but I’m 99% certain that you have colon cancer.”
When I use the phrase “life asteroid,” that’s really what it was. You’re just going along through your life and then this asteroid comes and just blows everything up. That was the day everything changed for us.
Processing the Diagnosis
Andrew, TPS: Wow. So there you are. You have 2 little kids. Your wife. You’ve been healthy. You mentioned you had some bouts of depression and anxiety before. Did this send you into a tailspin?
Trevor: Yeah, absolutely. The first period after a diagnosis, you really are in a physiological shock state. I remember the first week, [I was] reaching out to people, calling people, and [saying] “I have cancer. We’re going to do what we need to do.” But it was kind of dreamlike. It was very surreal.
Then after that, I was thrust into this very unfamiliar chute. You’re down the chute into this cancer land. You need to have surgery. You’ve got to talk about chemo. You’re trying to learn all the stuff.
It’s just so overwhelming and scary. We have little kids. I had no frame of reference that this was going to happen in my life, so it was crushing. Then my mental health really started to go to some very dark places.
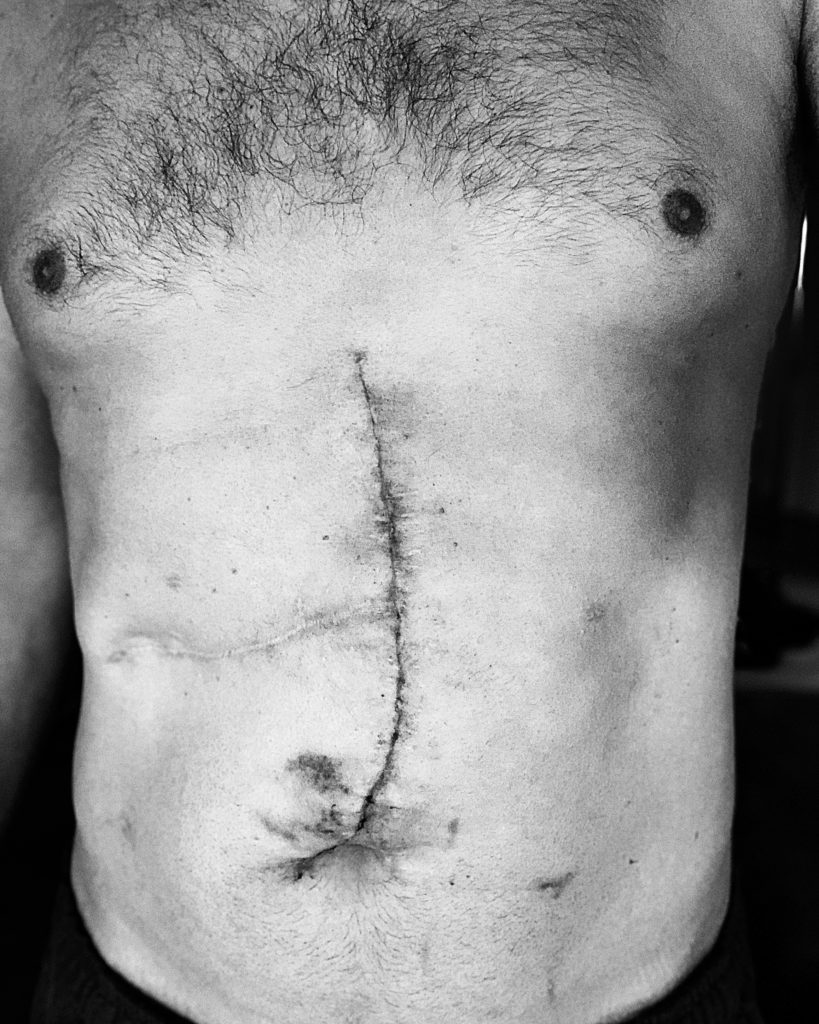
During 2018, I had colon surgery [and] started on chemo. We thought I was stage 3 early on, but right away, we did a scan after chemo. It showed a lesion in my liver, a metastatic tumor, and they could see that it was there prior to [chemo]. They just didn’t see it on the first scan.
There I was, a stage 4 metastatic cancer patient. In terms of survival, when you’re looking at colorectal cancer, if your stage is 1 through 3, you’re looking at 70+% survival, depending on your stage.
It’s a very good prognosis if you get it early. But once it spreads to other organs — often the liver, lungs, and other places — then the 5-year overall survival rate goes down to less than 15%.
Mental Health Problems
Andrew, TPS: Tell us how you reacted.
Trevor: Just crippling anxiety and depression. Very clinical. I thought I was going to have to go into an inpatient hospital for my mental health, not even my cancer. I had the first surgery, chemotherapy, and then I went for my first liver resection in the fall of 2018.
I was just at my lowest point. I was in a very dark place. I was checked out, isolated, couldn’t make a phone call, [and] couldn’t even talk to people about it. I just thought, “I’m going to die. I’m going to leave my kids behind. I’m a failure.”

By accepting help and getting out there and saying that I couldn’t do this on my own, I started to get better. All of a sudden, I was meeting people that were helping me. I wasn’t alone.
Just all this crushing emotional burden came down on me because I had always viewed myself as a very capable, strong person who was there for his wife and kids. Now I was facing this life-threatening illness with really a terminal diagnosis and I didn’t know how to handle it.
My first instinct was to just leave. I wanted to just go into the woods and say, “I don’t want to be a burden.” That’s a theme that comes up a lot in managing cancer. We don’t want to be burdens to our family. Sometimes when you get a diagnosis like this, that’s how you feel. That first stretch was a very tough place to be.
Finding Purpose Again
Andrew, TPS: Somewhere along the line, Trevor, you found purpose to dig yourself out of the hole. Tell us about that and what you noticed about yourself as a guy and then how it could relate to others.
Trevor: I’m really, really lucky because I have a wife and kids and family and friends who [are supportive]. I told them, “I don’t want to burden you anymore. I just want to leave.” My wife is like, “Hell, no, you’re not leaving. We’re going to love you through this and you’re going to get better.”
I say I’m lucky because a lot of men that I know don’t have that support system. When they want to run away, they just run away. My family was like, “Whatever we need to do to get through this, we’ll do.” My wife really gave me that tough love conversation.
One night [I was] talking to my wife. It’s around Christmas 2018. [I] just had my liver surgery. I had drain tubes. I was a mess. She was just encouraging me to somehow get out of this mental health pit.
I said, “I just can’t get over the idea of the kids remembering me as sick, being on the couch, being on the bed.” She said, “I’m not afraid they’re going to remember you as sick. I’m afraid they’re going to remember you as sad.”
In the book, I say this is [the] kind of conversation that puts you on a different path. I call that my Shawshank moment. Get busy living or get busy dying. Because I knew at that point I’m not a sad person. I never was.
It was just that cancer had taken me into a very depressed and anxious place. I couldn’t snap my fingers and just crawl out of that pit at that moment. But I heard what she said and it kind of cracked me open to the place where I could be like, “All right, I can’t do this by myself. I need to get help.”

That was the turning point. I started asking for help everywhere. I went to the Dempsey Center here in Maine. I got individual counseling [and] group counseling. I started reaching out to groups online, especially COLONTOWN and the Colon Club.
By accepting help and getting out there and saying I couldn’t do this on my own, I started to get better. All of a sudden, I was meeting people that were helping me. I wasn’t alone. I realized that so many people are going through this challenge. So many people with kids and people at my age and even earlier.

That was really the turning point that started leading me towards my purpose. How I finally really got revved up about my purpose was as my mental health got better, I started seeing what I call the 3-to-1 rule in cancer land.
In all these cancer support communities, whether it be the Dempsey Center or COLONTOWN or places online, usually it’s at least 3 women to 1 man. Women are much more comfortable in general accessing these supports that are out there, networking, being out there, having conversations with other patients, getting second opinions, [and] all this stuff.
Where are the men at in these support spaces? Is it possible that I’m one of the only few men who is getting crushed by this and needs help? I knew there were other guys out there struggling like me and who could use the benefits of these support places.
Maybe these places, for whatever reason, just weren’t connecting with the men. There were barriers. Men needed the help, but they’re not accessing it. That was the issue. I was looking for a place to give back and I was coming out of this mental health pit.
That really was the genesis of the Man Up to Cancer movement and mission. [It] was to say, “Let’s build something specifically for men who are out there struggling.”
By supporting them, we can also support their partners, spouses, families, and communities. [In] Man Up to Cancer, we inspire men to avoid isolation during the journey. In doing that, we also help everyone around them. That’s the background.

Man Up to Cancer
Andrew, TPS: January 2020, you launch Man Up to Cancer, not quite 2 years after you were diagnosed. How did you start?
Trevor: I knew the idea was going to be Man Up to Cancer because we want to take back that phrase. To me, “man up” means bringing your toughness, because you’re going to need every bit of your toughness to get through cancer — but also being willing to accept help, having the bravery and courage to accept help along the way, and then give it when you can.

I said, “I’m going to do something called Man Up to Cancer, but I don’t exactly know what it’s going to be yet.” I knew I wanted to have a group, and I knew I wanted to do a podcast and have a website with resources. I actually started putting up a Facebook group and I developed the framework.
Everything about Man Up to Cancer uses the wolf and the wolf pack theme. The whole idea behind that was we need to be wolves for one another going through cancer. Wolf packs are very social. If there’s a sick or injured wolf, the pack is going to take care of that wolf.
They’re not going to just abandon them. If that wolf dies, they have a ceremony. They remember that wolf. I thought, “As men going through cancer, why aren’t we together like this? We need a pack.” I had fun with it. I just started putting wolf stuff everywhere and being like, “Hey, be part of the cancer Wolfpack.”
Then one really important thing happened. Anyone can have an idea like this, but you need people to buy in and help spread it. My buddy Joe Bullock from Durham, North Carolina, was that first follower who came in and was like, “This is exactly what I’m looking for. Can I help you build this and spread the word?”
I was like, “Yeah, come on board.” To this day, Joe has been the lead administrator of the Facebook group. We have the private Facebook group for Man Up to Cancer, the Howling Place, which is for male patients, survivors, caregivers, any type of cancer, any age, any background, [and] anywhere in the world.
We have about 2,000 men in that group now. Joe has been critical to building that up and really facilitating the community piece of it so that I could do the podcast, the website, fundraising, all these other components of Man Up to Cancer, and writing the book.
The two of us have worked really well to grow the community and to facilitate it. Then I’ve also been able to do these other pieces along the way. It started with the Facebook group. Then I started the podcast. I’ve done 68 episodes. [I’m] on a little break right now.
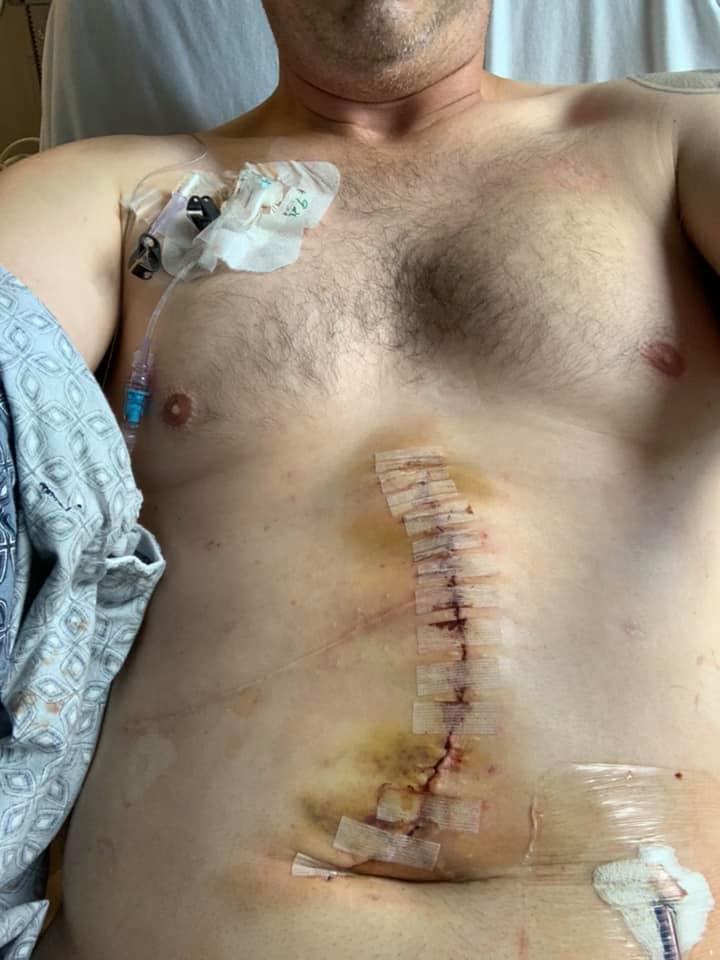
Of course, all through this, though, I’m going through cancer. I still have active cancer. I’ve now had 5 major surgeries. I’ve gone through a bunch of chemo, so I haven’t really had a break from the physical treatments of cancer.
My mental health has been a lot better. I still have my days, of course, where I have ups and downs. I throw a pity party occasionally, but I just don’t dwell there like I did.

We sort of had to grow organically and slowly, which is good. That’s the way a community like this should grow. A piece of that has just been because I’ve been in the trenches with the treatments I’ve been going through, so I’ve needed and I’ve really wanted Man Up to Cancer to just kind of slowly grow.
We’re not about numbers. Yes, we want to help the guys out there who need it, but to me it’s about the quality of the relationships and the quality of the people who come into the group.
We have a lot of other leaders now in the group who are ambassadors for Man Up to Cancer. It’s not just me out here saying a message. We have a pretty large group of ambassadors who believe in this mission of not isolating and who are out there talking about it.

Stuffing Emotion Down
Andrew, TPS: What is it, Trevor, about men, where without your organization, we tend to stuff it? I’ve been that way. I’ve been living with leukemia for 26 years. Little kids, duties as a father, a breadwinner, just try to push on and not talk about it much.
Trevor: Absolutely. A couple of things come to mind. Number one — and I talk about this a lot in the book — is cultural conditioning. We are conditioned as men in America and in many other cultures to when a challenge comes along in life, that we’re supposed to be able to fix it or solve it, that we are supposed to be strong and tough, and that we can handle our business.
For a lot of things, that rugged individualism is a positive. But with cancer, it’s not.
Men who isolate going through cancer have worse problems with mental health, anxiety, depression, all that stuff, and more substance abuse. They are more apt to have broken relationships, and they have worse medical outcomes. There’s real consequences here.
To your question, I think a lot of men just have that instinct that is like, “Well, this is a problem. [I’m] not going to burden others. I just need to focus on somehow I’m going to fix this on my own, and I shouldn’t need help.” That is a killer. That’s a killer. If you think like that going into cancer, it’s going to be a really tough road.
Then number two is the environment. [In] these support communities, a lot of men were trying to meet men where they are. A lot of men don’t feel comfortable going into a co-ed environment or an environment where it’s 75% women, 25% men, and being vulnerable with sharing about the struggles they’re going through.
That is meeting men where they’re at. It’s 2022. We’d love it if everything could be coed and not have genders assigned to it, but that’s not the reality on the ground. The reality on the ground is that many men just don’t feel comfortable. They don’t want to be perceived as weak. They don’t want to be seen in those groups as struggling.

This is the environment piece of it, because I think we have these stereotypes around men. People are like, “You can create whatever group you want, but the men aren’t going to be willing to share. They’re not going to be vulnerable.”
I’ll tell you what, you give them a platform and have it be just guys and the sharing is just like [boom]. I think some of it is, some of these men hadn’t had a support environment that they felt comfortable in.

Man Up to Cancer gives them a place to start being more vulnerable, sharing some of the struggle, [and] sharing what it’s really like to go through this cancer without those feelings of feeling shameful or that they’re going to be judged.
We put up the walls and started inviting people to do that, and some of our role models started sharing their vulnerabilities and how bad it sucks to go through cancer. All of a sudden, all these men just started opening up.
We’ll have people every week that’ll be like, “I haven’t really shared about this. I’ve been going through cancer for a couple of years, and I haven’t shared about this part of it, but man, I’m really struggling with X.”
Other guys will come in and be like, “Yeah, man, I’ve been struggling with that, too. You’re not alone in that.” That is the heart of what happens in the group — that kind of just bonding and open sharing [with] no judgment [and] all love.
Group for All Cancers
Andrew, TPS: One of the things I wanted to ask you about is “cancer land.” You used that term earlier. So much in cancer land has been driven by treatment and specific diseases.
Trevor: Correct.
Andrew, TPS: Your organization is talking to men no matter what cancer [they have]. It seems like that was maybe a real gap not just for men, but across cancer land. [It was] not so much about treatment, but about being a man with cancer.

Trevor: Yeah, you nailed it. That, from day 1, has been built into the recipe. We are not a treatment group. We have more than 20 types of cancer represented in our group.
From the beginning, I didn’t want [it] to be a treatment group because there’s tons of those. I wanted to be the emotional support, like the guys lodge. You’ve had a day of being out in the woods, and now you just kick back in the lodge and [socialize].

We talk about cancer. We vent about it. We share about it. It, of course, is a central theme in our group and what connects us as that shared experience and challenge. But we’re just a social group at the heart of it. We talk about our pets, cars, and favorite drinks. It’s the social isolation, too, that is not being addressed by some of these other groups.
There are great groups for treatment out there. What we can do is act as a bridge. Let’s say someone comes in, and they have colorectal cancer. We’re not going to sit there talking about all the treatments at all.
We’ll say, “Hey, come here for your emotional support and your brotherhood, but if you want to learn about your treatment options, go connect with these people at COLONTOWN, Fight CRC, Colorectal Cancer Alliance, or all these groups that are out there that do these different things. If you want to learn about advocacy, here’s the places where you can go.”
We find that most of our core members, people who are really into it will go to these different groups based on their cancer type to talk about those treatment options and then they’ll come to The Howling Place to get the emotional support, joke around and all that stuff.
I’m really proud of that because I don’t know of any pan-cancer groups for men that cross. We have guys with all these different types of cancer. Because of the shared experience and hearing these words, “You have cancer,” we have so much that binds us together emotionally.
»MORE: Hear from colon cancer patients and survivors
Positive Changes for Members
Andrew, TPS: You’ve seen people change. We’re going to talk about how you’ve changed, but you’ve had these thousands of men who participate. Tell me a couple stories about the guy who was all bottled up who maybe isn’t now. Can you think of some stories?
Trevor: I think of Mike Reilly. Mike is a young colorectal cancer survivor, diagnosed at 31, with a wife. He lives near Buffalo. His story is really inspiring in that he was told, “You only have a couple of months to live. Wrap up your affairs. There’s nothing we can do for you.”
Then through COLONTOWN, he was able to find out that’s not necessarily true. I’m going to go over here to this other hospital, and they gave him a different plan. Now he has the HAI pump, and he’s been NED, no evidence of disease, for a year and a half.
Huge difference in his treatment plan, but that leads into then our movement with Man Up to Cancer. Then I saw him in COLONTOWN. I connected with him. We kind of became friends. He came into Man Up to Cancer, and then I saw him change as a leader.
He had been someone who didn’t talk. He was one of those guys who was in isolation. He wasn’t really talking about it. He wasn’t a leader at that point. He was someone who was struggling emotionally. Then through the friendships in Man Up to Cancer and through that empowerment, he has really established himself as this voice for men’s health and getting screened. [He’s] also in the group encouraging people to avoid isolation.
He’s just out there doing his thing. He’s covered with tattoos. Handsome young guy, covered in tattoos. He hauls cars for a living.

Then at the end of the day, he’s posting about, “Hey, make sure if you’re struggling, reach out to us or see a counselor.” I love role models like that who are complex. We can’t put them in a box. You can be a guy’s guy and a tough guy and all these things, but you can also take care of your mental health. Especially during cancer, taking care of your mental health [and] emotional health is part of how you get through this.
As you know, finding male role models in cancer land in all these support groups and everyone else is difficult. To have men who are willing to put themselves out there in public to speak, to write about it, to share — every time a guy does that, some other guy is out there being like, “Oh man, thank goodness I’m not the only one feeling these things.”
Personal Changes from Man Up to Cancer
Andrew, TPS: Trevor, I want to ask about how this has changed you. We should mention you’ve gone through 5 surgeries. I think you may have a 6th one coming up. You’re going through all the treatment stuff, and thank God, now you’re here. You’re going into your 6th year. Is that right?
Trevor: I will be at my 5-year mark in March of 2023. I’m 4.5 years right now, coming up on 5 years real quick.
Andrew, TPS: How has this changed you?
Trevor: It’s a great question. I don’t spend a lot of time thinking too much about my own evolution because I’m living it day to day. When I step back, I guess I could say that for me, doing Man Up to Cancer, I have more support now than I’ve ever had.
I have this Wolfpack. I have these guys that if I’m having a rough day, I can go online and get all this love and support, which is huge for me. I’m just so grateful for that. I’m grateful for the men in the Wolfpack and others that I’ve met through this Man Up to Cancer journey who support me and my family.
That’s number one. The second thing I really wanted to do was get redemption. I felt when I checked out from my family and when I was going through all that depression and anxiety, I let them down. I know they don’t look at it that way and I don’t either.
I don’t look back and get upset with myself for the way I was, because I needed to go through that dark place to do the work that I do now. I wouldn’t have this purpose without going through that hell. I’m thankful for it now.
As I started to get out of it and improve my mental health, I wanted to show my daughters especially that life is going to knock you down. Life is going to get you to your knees, whether it’s cancer or something else. You don’t have a choice. That’s what’s going to happen. But you do have a choice on how you respond to that.
I wanted to show them that life knocked me down, but that I could get up, and I could do something with that pain. That I could make some change in the world that’s positive, that’s loving, and that’s helpful so that no matter how long I live — because my prognosis is still not good.
If I have another year or 2, or whether I get through this and live another 40, that I can on that day, whenever that is, say, “You know what? I got up and did something to give them that example,” so that when the hard times come in their life, they can look to me as a role model, too, and say, “Look what Dad did.”

How You View Every Day Now
Andrew, TPS: Trevor, there’s uncertainty in all our lives, and there certainly is uncertainty in yours with advanced colon cancer. The 6th surgery [is] coming up, but happily, the book [is] coming out. How do you view every day now as you are propelled by Man Up to Cancer?
Trevor: Again, I have my normal ups and downs, and I have my appropriate emotions for what I’m facing — going through a life-threatening illness when you have a family like this. Our girls are 17 and 15 now. I’m so grateful to be here with them. I guess what I’m saying is it’s not all sunshine and rainbows.
It’s hard. It’s really hard, and we can’t ignore that. At the same time, I think my heart and my spirit and my mind have all kind of evolved to live with this and to accept it. If I progress and pass away soon, of course that’s never going to be okay. It’s all going to be grief for the people left behind.
What I want everyone to know and feel hopefully is that the joy of having me in their lives outweighs the sadness of having to say goodbye to me. For me personally, I have adopted a very present mindset. I am very in the here and now, and I am grateful for every day.
I’m grateful for all the blessings we have in our lives, and I feel like I’m on bonus time. There were plenty of times in the past 5 years that I did not think that I would be here in 2022, so I’m very grateful for that. I’m grateful to just keep doing what I’m doing, first and foremost with my family, Sarah and the girls, and how wonderful our family is.
Sage is applying for colleges, and I’m teaching Elsie how to drive now. I already taught Sage how to drive. These are things that every dad wants to do. These [are] milestones. Every time that something like this happens, I just give myself that smile and be like, “Look how amazing this is.”
It’s a very present, grateful mindset. Again, that’s not all the time. You can’t live with that kind of mindset all the time. I’ll get pissed off. I’ll get sad. I’ll get upset. But for the most part, I’m much more present and grateful than I was. I’ve always been a grateful person, but now it’s even more so.
I’m out walking the dog and just wondering at nature and being here. You think those big thoughts and big feelings when you’re living stage 4. I’m grateful for that. All these silver linings, which there are many, I didn’t see early on in cancer.
I would have said, “Don’t even talk to me about the gifts of cancer.” But now that I’m almost 5 years in, I’m definitely accepting of them. I think I’m in a good place. I think I’m doing the best that I can. I think our family is doing the best that we can with a really tough situation.
Doing Man Up to Cancer and being able to have those relationships and being able to bring something positive in some lives out there in cancer land, outside of my family, is something that I’m most proud of, and it’s an honor and a privilege to do it.

Conclusion
Andrew, TPS: Just as you say you’ve received gifts, though, with Man Up to Cancer, you’ve given us a gift. I want to thank you as a guy living with cancer, and I know I speak for many, Trevor.
We all have our journeys. You’ve had your own personal journey. The fact that you have found purpose and then reached out to all of us. Thank you, my friend. I really appreciate it.
Trevor: Thank you, Andrew.

Inspired by Trevor’s story?
Share your story, too!








Leave a Reply