Strength in Family & Advocacy: Chrystal’s Story of Stage 3C Cervical Cancer with PALB2 Mutation
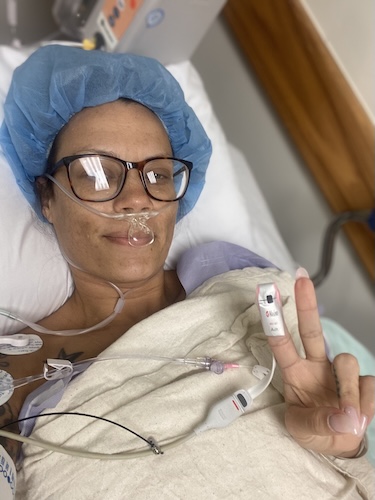
Chrystal, a nurse and devoted mom of three, found out that she had stage 3C cervical cancer in March 2025. She had felt a deep pull towards healthcare after losing her mom to breast cancer when she was only a little older than Chrystal is now. Determined never to feel helpless again, she pursued nursing, focusing on geriatrics and long-term care.
Interviewed by: Taylor Scheib
Edited by: Chris Sanchez
Chrystal’s symptoms crept in gradually, including pain during intimacy, abnormal bleeding, irregular periods, extreme exhaustion, and swelling in her groin. She attributed some of these symptoms to other issues, like shingles. But when she discovered a lump under her arm, it spurred her to see her gynecologist. After a series of tests, including a cold knife cone biopsy, Chrystal received the life-changing diagnosis of cervical cancer (squamous cell carcinoma of the cervix, stage 3C, with PALB2 mutation). (Editor’s Note: Squamous cell carcinomas of the cervix are the most common type of cervical cancer. A PALB2 mutation is a mutation of a special cancer-preventing gene that causes it to stop working.)

Chrystal found that mental health was key in her stage 3C cervical cancer experience. She was mentally exhausted trying to deal with the long waiting periods for test results. She found solace in her family, especially her husband, a fellow cancer survivor, who provided not just emotional support but practical advice about chemotherapy. Chrystal also opened up to her daughter, sharing every detail of her diagnosis and treatment. She did this to arm her daughter with information and to encourage her, too, just in case she would have a similar experience in the future. By being so transparent, she sparked an honest dialogue about women’s health.
Caregiver support was equally crucial. Chrystal recognised how deeply her experiences affected her husband and friends. She encourages others to check in on their caregivers, acknowledging that their stress often goes unnoticed.
Education became both Chrystal’s coping mechanism and mission. She actively searched for information about stage 3C cervical cancer and treatments to fill gaps in online resources. Now, she connects with other cervical cancer survivors to offer them guidance and hope. She’s even co-planning a cervical cancer retreat to foster community and support among survivors.
Chrystal now undergoes regular MRIs, mammograms, and follow-ups every six months. She’s also passionate about long-term care advocacy and remains committed to her family. Watch her video and find out more about:
- How her medical background shaped her stage 3C cervical cancer experience.
- Why caregiver support is as important as patient care.
- The frank, open, and empowering conversations Chrystal and her daughter had.
- How she took her experience forward into advocacy for cervical cancer awareness.
- The unexpected mental health challenges Chrystal faced beyond her treatment.
Scroll down to read the transcript of Chrystal’s interview.
- Name: Chrystal M.
- Age at Diagnosis:
- 41
- Diagnosis:
- Cervical Cancer (Squamous Cell Carcinoma) with Pelvic Lymph Invasion
- Stage:
- Stage 3C
- Mutation:
- PALB2
- Symptoms:
- Pain during intimacy
- Irregular menstrual periods
- Abnormal bleeding, sometimes heavy
- Severe exhaustion
- Pain in left leg and groin area (deep vein thrombosis)
- Lump in left armpit
- Treatments:
- Surgery: installation of inferior vena cava filter
- Radiation therapy: brachytherapy
- Chemotherapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Hello, I'm Chrystal
- How I knew something was wrong
- The doctor I went to first
- Researching my symptoms
- The moment when everything changed
- How I found my care team
- My treatment plan
- When the reality of my diagnosis hit me
- My husband was able to relate to what I was going through
- I had side effects from my treatment
- I had to do high-dose rate brachytherapy
- I had more testing done
- My cancer spread
- What have been the most challenging parts of my diagnosis
- Where I’m at now with my diagnosis
- What my monitoring is like
- I wanted to be open with my daughter
- What I want others to know
Hello, I’m Chrystal
I’m 41 years old. I was diagnosed with stage 3C cervical cancer in March 2025.
I am a mom to three beautiful children. I am a nurse who is passionate about geriatrics and long-term care. I’ve worked mostly in the nursing home, and it’s definitely my life’s work. My father and I have been to several baseball games this year. That was my treat to myself during treatment. We love to go out, be outside in the sunshine, experience different things, and we just like to do things outside.
I did not start in the medical profession; I started in my parents’ business. They owned a flooring business. I became a mom. And then my mother was diagnosed with breast cancer; she passed away at 43, she lost that battle, and I did not know how to help her. I felt useless and helpless, and I was very worried. My father called me and was trying to kind of explain things, and he’s not medical either, and so I just felt this calling. My spirit just felt pulled to medicine. And I never wanted to be in the dark again.
How I knew something was wrong
My first red flag was something that kind of incrementally increased over about three years. That was pain during intimacy. At first, it was just kind of positional, and then it kind of led to some bleeding. And then it got to being almost full menstrual blood, and so that was very concerning, aside from the fact that it was very painful. I began to have irregular periods where I might have a full period every two weeks and then may go, say, six weeks without one. My hormones were just all over the place. I was exhausted. I’m a nurse, so I understand, we all have those things that wear us out, but I was more exhausted than usual. I also began to have pain in my left groin area, almost like where your lymph node is, it began to get very swollen and painful, but at the time, I wrote it off because of shingles. I actually experienced shingles every so often, so I thought maybe it was something to do with that.
And it wasn’t until I experienced or felt a knot in my left armpit one morning in the shower. It was a Friday morning, and I remember going to work and then casually mentioning it to a coworker, and she was like, You should probably get that checked.
The doctor I went to first
I had been seen by a gynecologist here locally; he is a great, fabulous guy. I had an abnormal PAP about three years ago. He wanted to do a colposcopy, so we did that. Then he scheduled another LEEP procedure about a year later. And I said, no, absolutely not. I just could not even think about confirming that appointment, it made me nauseous. So fast forward to, I’ve not gone to any appointments for about a year and a half. And that’s when I went to a gynecologist to talk to them about the lump under my arm. And that’s when she said, We need to do a pap smear.
I don’t even have a PCP, okay. To this day, I still don’t. I’ve had cancer, but I don’t have a regular routine doctor that I go see and get meds from. So she was talking to me both as a PCP, as a woman, and as the gynecologist that was like, hey, we really need to check this out. So she said, why didn’t you have the procedure, why didn’t you want to have the colposcopy? And she got to the root of it, which was my fear because it’s painful. I have an immediate reaction to epinephrine, which is commonly used to control the bleeding. It makes me feel like I’m going to have an absolute heart attack. All of it is bad for me. And she said, well, why don’t we do this? I’ll do a regular little PAP smear in the office, no pain, no problem, which I agreed to. And then she said, I’m going to see what the results are, and if they’re abnormal, like we suspect that they might be, I will schedule you for a cold knife cone biopsy in the O.R., that way you can be put under general anesthesia, you won’t feel a thing.
Researching my symptoms
I had no idea what was going on with my body at the time, so I’m on the Google machine trying to search for my symptoms. And whenever I went to social media, because that’s where I tend to get a lot of information these days, nobody really had a lot of information about what I needed. So I honestly just sat and waited, I waited for the scan appointment, I waited for the results. I waited, and I was in MyChart all the time.
The results came back, they were cervical dysplasia or cervical intraepithelial neoplasia (CIN) 3, which is the high-grade abnormal cells. And she said, I want to get you in for the cold knife cone biopsy to take the biopsy under general anesthesia. I’m going to call the O.R. and see when we can get you booked. I went into the O.R. two days later. and then just kind of casually clicked into place, and I was able to get seen pretty quickly.
The moment when everything changed
It took me nine days to get my biopsy results; that was a really long time. I checked MyChart every hour, both at work and at home. I called the lab and said, Hey, I had a biopsy done nine days ago, and within an hour, they sent me the results, but I was at work when I read the report, and I was numb immediately, like, Okay, well, we’ll just deal with that whenever we get home. My husband was running some errands.
He comes home, and he is still unpacking the vehicle, you know, unloading the groceries, and I gave him a hug. And when I squeezed him, I pulled him to me, and I was looking behind him, so he’s facing over my shoulder, and I’m facing over his, and I said, I can’t look at you when I say these words, but I have cancer. And he lost it, he was just like, Chrystal, I don’t know what I’ll do without you. And so we hugged and cried and hugged and cried for about two days, not even wanting to leave each other to go to work or to go to this or that. We stayed together for about two days there. And then we started to pray, and I actually got anointed at church not too long after that by one of the church elders. And I’m not here to tell you that it did or didn’t work, but I certainly felt support from the community. My friends started to come out of the woodwork, old colleagues that I had not talked to in years, and routinely check on me today.
How I found my care team
I asked my doctor what her recommendation was. She was part of a network, and I went to a university hospital, which turned out to be a great thing for me, the patient, because they inundated me with resources. They have somebody to help you with everything, and then they have lots of educational materials, which I really found helpful. They made me a whole binder of phone numbers and different materials that I would need during my treatment, so that’s kind of what led me to where I ended up going. It just seemed like every time I talked to another doctor, I would mention it to somebody, and they’d say, “Oh, he’s great.”
“Doctor so-and-so is wonderful, you’ve got the best doctor.” I just felt really comfortable. I’ve worked in healthcare, so you kind of know, this doctor is very personable, their bedside manner is wonderful, they’ve answered all of my questions, and they’ve treated me well. And so I have zero complaints about any of the people who provided my care.
My treatment plan
I had a complication, and the doctor who had to see me for the complication was new to me. I was new to her, and she had a heart-to-heart conversation with me. One evening, late one night, she stayed late to take my case, and she said, “If it comes back that the cancer is in more than one place, we’re not going to do a hysterectomy because I don’t want to get in there.” Because my first question is, how soon can we get it out? Can we go in there and just remove all of it? I’m done with my uterus anyway, just go ahead and do a hysterectomy, I’m fine with that. And she said, “Actually, if we get in there, the tumor can be adhered to your bladder, it could be adhered to your kidneys, you could come out of there with a new appliance, like a colostomy or something like that. She said, I don’t want to go in there and stir it up. So what we’re going to do is 28 days of external radiation, 6 to 7 chemotherapy appointments, and then, for brachytherapy or high-dose radiation treatments at the end of therapy.
When the reality of my diagnosis hit me
I was in the office with another nurse, and he was going over my patient’s instructions for external radiation. And that’s when I started to realize how serious this was. He mentioned the side effects, and he was talking about the team and the fact that the team included so many people. But the one that got me was the nuclear physicist, that’s when I realized I had cancer, that’s when it hit me. Because I’m such a strong personality, I’m so used to controlling the outcome of as many things in my life as possible. I try really hard to steer things in the direction that I want them to go. This was something that I could not do with this; I could not will it out of my body, I could not go take a medication, and it would immediately be gone. There’s not like this definitive, okay, you have it today and you don’t tomorrow kind of line, which is what I was trying to get to. I think that’s what I really needed.
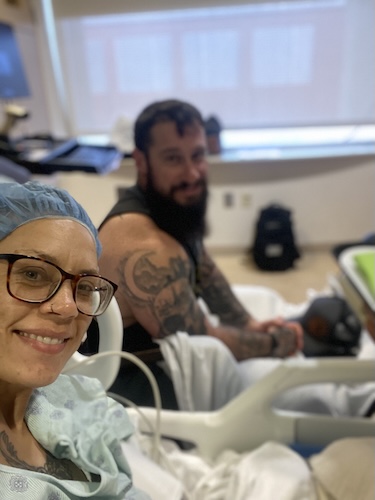
My husband was able to relate to what I was going through
My husband is also a cancer survivor. He had testicular cancer when we first met, so he had a lot of advice as far as chemo because he did chemotherapy. And so we were talking about things. One of the concerns that I had and maybe someone else too, was that chemo immediately makes you feel like a horrible person, like it immediately just makes you feel so sick. And he said he pictured it in his mind, something like lethal injection or something with an immediate, horrible, terrifying response. And he said, “But it’s not like that. You won’t feel bad for several days, and then you just kind of treat the symptoms.” And so that really helped me understand at least that part of it. My biggest chore was trying to educate myself more on the external radiation, so the nurses gave me as much information as they could. But then I went to the internet to try to see functionally out here, in the world, what are we doing? What kind of groceries are we buying? What kind of activities are we doing? Do I need to sleep extra or is it really not that bad?
I had side effects from my treatment
Initially it wasn’t terrible. I was a little tired, but again, that was one of my primary symptoms going in, so I wasn’t new to doing things in life exhausted, I was used to that. But the nausea did not set in after my first chemo for about 3 or 4 days. They had given me a drug that covers you for nausea for about 72 hours. She said, “You normally won’t feel nauseous for 3 to 4 days.” And about day 4 to 5 routinely, I would start to feel bad. The cumulative effect of all of the treatments together, though, you start with the external radiation, you’re doing that every day, that makes you tired. It’s pretty stressful to make sure that your bladder is the same amount full at the same time every single day, and that means you can’t go tinkle. That means you’re a cough or sneeze away from disaster, to be honest. They make you drink tons of water whenever you’re nauseous, and sometimes that didn’t go well. But as far as the fatigue, I would say at about two weeks, that’s when I had to quit my job, two weeks after I started radiation and one week after I started chemotherapy. Then with the chemo, we ended up just doing five treatments because when I was scheduled for the sixth chemotherapy, they actually put me in for the HDR, and he didn’t want me to do chemo and HDR at the same time, so I just did my high dose radiation on a Tuesday and Thursday of two different weeks.
I had to do high-dose rate brachytherapy
With the HDR, I showed up at the hospital at about six in the morning. I had not had anything to eat since 6 p.m. the day before, nothing to drink since noon the day before. They take me in, put an IV. They go over a ton of consents, you meet with anesthesia, the doctor, the O.R. nurses, they take you back into surgery, they put you to sleep, and then they place this device with a little tube coming out of it. You are lying flat when you wake up in recovery. The nurses are quick to manage your pain. They gave me something, and then they attached me to a PCA, which is a patient-controlled analgesic, so that I didn’t have to ask for pain medication. I just had a little button to give myself medication whenever I needed it. That was very, very helpful not to have the anxiety of like, is this going to hurt? After you come out of surgery, you go into recovery. My family met me in the recovery room, and I waited for about an hour while they planned my scans and all that good stuff. Then they took me into the radiation therapy room, where they placed radioactive seeds on my cervix to be circulated in and out for about ten minutes.
They played some music while I did this; it was not painful at all. I would say the most uncomfortable part, it’s not even super painful, but it was just pressure and uncomfortable, was whenever they removed it, but the doctor was very good. He warned me before he touched me. He warned me before he did anything and what it was going to cause. This is going to cause pressure; you’re going to feel a little bit of pain here, hit your pain pump, those kinds of things. All I had to do after that, and they would literally wheel me down the hall back to my room. I would use the restroom, and as soon as I could void my bladder, they would let me go, and I just did that four times. The biggest thing with that was just making sure that I followed the diet regulations or recommendations. They wanted me to stay clear of liquids only after 6 p.m. the day before, which is a nightmare because I eat late, so I felt like I was starving by the next day when I got out.
I had more testing done
The doctor did the initial cold knife cone biopsy. It was positive at 19 out of 20 margins. So the cancer had spread beyond just this little sample that they took. So then she took me in. I had some hemorrhaging going on, and they had to take me into the O.R. to stop it. She also did another biopsy then because she wanted to get the rest of it. So she went in and took out another big chunk, and there was less of the cassettes. I don’t remember how many, but there was less cancer in that tumor, thankfully. They scheduled me for my Pet scan, and while I was waiting for the Pet scan.
My cancer spread
The pathology came back on the tumor, which said it was PALB2 positive, which is hereditary. My mother, who passed away from breast cancer, and her mother, who passed away from breast cancer, were also PALB2 positive.
They did the genetic testing, and then they also found that there was extensive lymphoma with lymphovascular invasion in my tissue, on my cervix. We go to a PET scan, and they shoot you with a radioactive tracer in an IV. Other than that, it’s painless. And then they scan your body, and you get results a few days later.
I went to this appointment by myself, and the doctor read my results with the radiologist, and she said, “It spread to your pelvic lymph nodes, you have stage three cancer.” And my brain just said no, I’m too young for that. My brain said, No, no, no, you got something wrong, there’s no way it could be stage three.
It felt like I need my mom. It was an immediate. And I don’t have many of those moments because I’ve been grown with kids for a long time, and I’ve not had my mother for 17 years, but that was a moment where I just needed a woman older than me who knew more than me. Who knew that it was going to be okay to just wrap me up and hold me, that’s what I needed. There was a nurse there that day, and I don’t know how she knew, she didn’t say anything, she just walked up to me in her cute periwinkle colored scrubs, and she squeezed me as hard as she could, so much so that I left makeup on shirt, and I needed that. And I told her, I said, you have no idea how much that was needed, I needed that so much. But it was just like a gut punch, like, this is wrong, something’s wrong. Where’s my mom? She’ll know, like, tell mom to figure this out because this is all wrong.
What have been the most challenging parts of my diagnosis
My biggest concern was how am I going to be able to function? My husband has to work, I’m supposed to be working. We have a young child in the house, and then I found out that I had a grandson on the way, and I was just like, I don’t have time for this. And then I thought, okay, we’ll just chip away at it, and then by the end of the summer, you’ll be done with it.
Because I found a lump under my arm first, I went into my mammogram hyperventilating because I thought that my cervical cancer was a metastasis of breast cancer. I thought that it started up here, and so I went in for a diagnostic mammogram, and that just happened to be the day that I was hemorrhaging, so I was having a complication. I was bleeding down my legs and I mean with a full diaper pad on. It was so much like I said, they took me into the O.R. and that was a whole thing. But yeah, I nearly bled to death, and I thought, I have breast cancer, and this is the end. And then my brain started thinking of all the things that if I were going to die, that I would do or not do, and I started to do those things. I said, if you want to own a library, go buy those books, and I started hoarding books. And then I decided that if I wanted to go watch baseball, I was going to go watch baseball because I didn’t know when I’d be able to.
I thought I was really, truly not going to make it. I thought, well, you better make the most of the time you have, sweetheart, because it’s almost the end. And so whenever I found out that my mammogram was negative, I was in shock. I thought, well, as much as I was in denial about the cancer itself, I can’t believe how hard it is for me to accept a negative mammogram. But it really was. I was very worried at first. The doctor actually ended up doing an ultrasound of the lump under my arm, and she said it’s nothing, it was because I had recently lost some weight.
Where I’m at now with my diagnosis
I am trying to fill my plate again, so I have started working with some cervical cancer warriors, survivors. I message several girls routinely, one of the people that I’ve met on the internet has volunteered to co-host a cervical cancer retreat of sorts in her state of Oregon next year, and she’s actively in treatment right now, she’s still finishing that up. Whenever she’s done with that, we’re going to hit the gas and move forward on getting together with other ladies, just because it’s a lonely disease, it’s lonely to be treated for this disease. We want to have some camaraderie and meet with other girls and just discuss and vent and cry and hug and have lifelong friendships from it, so we’ve got that coming up. And then I have become much more vocal on social media as of late, and I’m working with several organizations to try to change some things in long term care. That field is a passion of mine, and those residents mean more to me than life itself, so I am serving that community actively, and I have some job opportunities that have come along the way or come up as a result of that. I’m very excited about the future. focusing on my family, making it the healthiest it can be. Cancer is hard on your family. Trying to catch up with my husband and compare notes after the fact. He was very worried. It affected him in subconscious ways and more obvious ways, and speaking with him afterward, I did not realize how unwell he was. He just would not bother me at the time, or he thought that it would be a burden to me to discuss it. And generally speaking, most of the men in my life were pretty quiet about things like that, so we don’t discuss feelings.
It’s weird whenever you’re worried about how your disease is going to affect someone else. And then whenever you see it happen, you feel responsible in a way, but then you also realize that’s what life is, that’s what my husband signed up for, that’s what I signed up for, so we just got through it. I’m so happy to be on the mend. I’m so happy to feel well. I feel better than I have in years.
What my monitoring is like
I do have a negative MRI, which is why I say no evidence of disease. Every six months, I have a follow-up with someone. It will either be with the high-risk breast clinic that I see, so they picked me up, and they want me to be. I have an MRI every six months and then the mammogram, the traditional mammogram. And then the doctor wants me to come in about every six months, the gynecologist, to have a pap smear, be seen, and do some labs. I’m doing something every six months.
I wanted to be open with my daughter
I felt compelled to tell somebody. My mother was very private about her struggle with breast cancer, and there was a lot that I did not know, that I still don’t know, even with my nurse brain trying to fill in the blanks of what she must have been going through. I shared every intricate detail with my daughter so that if, heaven forbid, she ever were to find herself in a situation where she needed that information, she would know that it’s survivable. She would know that the treatment is so advanced. I tried to include my daughter in that as best I could so that she could understand without scaring her. So I tried to put it into 16-17-year-old girl terms. And that opened a dialogue for her and me to discuss women’s health differently. Which is hard for parents, you know, the reproductive system. And you don’t want to talk to your daughter about her reproductive system, necessarily, but in this case, I felt like knowledge was power.
And so that’s how you turn something into a benefit. That’s how you make it better. I can tell you that external radiation really wasn’t that bad; I didn’t get any burns. I can tell you my story, and you can hear my voice and see that I’m okay, so that you have hope that you can get through it, too. The nature of 80% of the messages that I read and respond to are ladies who are saying, “Hey, I just got diagnosed,” or, “I saw your video about external radiation.” And it helps so much, and I don’t say that to compliment myself, I’m just sharing what happened to me. And in no special way or format, I’m just telling people that I have it, too. And that by itself, I think, has helped so many people, like, hey, this is not a gross, ugly thing. Not just horrible people have it, and it’s not taboo. Several of us are struggling with this, and this is how we took care of it. So I’ve met some lifelong friends from this, and even people who are not in this country. I have made friends who live in Canada and the UK and different places all around the world, just because we have this thing in common.
What I want others to know
Put one foot in front of the other and just keep going. There will be days when, if you think about it, you will talk yourself out of it, or you will make yourself believe that you cannot do it. But just put a foot in front of the other, and you will eventually be finished with the treatment. That was my biggest thing. I just thought, oh my gosh, that seems like a terribly long time, if you will just put a foot in front of the other.
Check on your caregivers whenever you have the bandwidth, whenever you can, check on your caregivers. It’s important. Those people are stressed out, too. They’re not actively being treated, necessarily, but they’re right there with you in the trenches. And they sometimes need to decompress, too.

Inspired by Chrystal's story?
Share your story, too!
More Cervical Cancer Stories
Willow B., Pelvic Cancer, Grade 1, Stage 2.5
Symptoms: Persistent fever-like chills, scratchy throat, fatigue, post-orgasm pain, heavy bleeding, severe cramping
Treatments: Surgery (radical hysterectomy), radiation, chemotherapy, hormone replacement therapy (HRT)
...
Samantha R., Adenocarcinoma Cervical Cancer, Early Stage
Symptoms: Irregular bleeding, pain
Treatments: Surgery (radical hysterectomy, pelvic exenteration), chemotherapy, immunotherapy, radiation therapy, hormone replacement therapy, hyperbaric oxygen therapy
...
Amanda L., Cervical Cancer, Stage 3
Symptoms: Heavy periods, abnormal bleeding, large blood clots, severe cramping, severe abdominal pain, pain radiating down the left leg, loss of mobility in the left leg, loss of appetite, fatigue
Treatments: Chemotherapy, radiation therapy (external beam radiation therapy & brachytherapy)
...
Mila L., Squamous Cell Cervical Cancer, Stage 1B1
Symptoms: Abnormal lump in cervix area, bleeding after sex
Treatments: Chemotherapy (cisplatin), radiation, adjuvant chemotherapy (carboplatin & paclitaxel
...
McKenzie E., Cervical Cancer, Stage 3C2
Symptoms: Severe abdominal & back cramping, persistent & extreme pain, heavy discharge & bleeding
Treatments: Radiation, chemotherapy (cisplatin), brachytherapy, immunotherapy (Keytruda)
...
Marissa N., Squamous Cell Cervical Cancer, Stage 3B
Symptom: Excessive and prolonged vaginal bleeding
Treatments: Chemotherapy (cisplatin), radiation, brachytherapy
...
Leanne B., Cervical Cancer, Stage 4
Symptoms: Fatigue, irregular periods, pain after sex
Treatments: Radiotherapy, brachytherapy, chemotherapy (carboplatin & paclitaxel)/p>
...
Kristine M., Adenocarcinoma Cervical Cancer, Stage 2B
Symptom: Tumor found during postpartum pap smear
Treatments: Colposcopy with endocervical curettage, cone biopsy, total abdominal radical open hysterectomy with lymph node removal
...
Kate R., Squamous Cell Carcinoma of Unknown Primary Origin, Stage 3C
Symptoms: Intermittent spotting during or after sex, unpredictable menstrual cycle, abdominal pain particularly under the rib cage
Treatments: Chemotherapy (cisplatin & paclitaxel), immunotherapy (Keytruda), surgery (total abdominal hysterectomy with bilateral salpingo-oophorectomy & omentectomy)
...