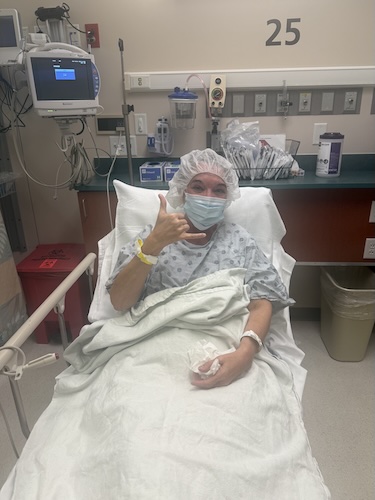
Stage 4 Colon Cancer, Faith, and Family: Kristie’s Story of Redefining Life
Kristie went in for a routine screening colonoscopy she’d scheduled on her husband’s birthday, a date she now remembers for both celebration and shock. She went in for her first colonoscopy only after her OB-GYN insisted a second time, following a missed referral during the pandemic. Waking from anesthesia, she heard the words no one wants to hear: the doctor had found cancer in her sigmoid colon, later staged as stage 4 colon cancer when they found spots in her liver. Her surgeon spoke plainly about metastatic disease and palliative care, but also emphasized that treatments and outcomes are changing quickly and that her attitude and support system would matter.
Interviewed by: Keshia Rice
Edited by: Chris Sanchez
Before her colorectal cancer diagnosis, Kristie was an active high school English teacher, department chair, Ph.D. student, and devoted member of her church and community. She was athletic, too; she ran 5Ks, hiked and went camping with her husband, and spent weekends traveling to watch one son pitch college baseball and the other teach and coach. Looking back, she realizes that chronic constipation and pencil-thin stools were possible warning signs of colon cancer, but she attributed them to lifelong constipation and perimenopause. Now she uses her platform to urge others to “pay attention to your poop” and to keep up with colonoscopy screening.

Kristie’s experience has included multiple rounds of chemotherapy, radiation, a colon resection with temporary ileostomy, liver ablations, and a planned liver resection. Chemo has brought cumulative side effects like diarrhea, neuropathy, cold sensitivity, severe skin reactions, and deep fatigue that she describes as akin to trying to walk against ocean waves. But she also talks about the infusion nurses who treat her with deep compassion, friends who drive her to chemo so her husband can keep working, and sons who quietly carry their own fear while trying to let her rest.
Over time, Kristie C. has shifted from seeing herself primarily as a full-time teacher to embracing a new identity as a writer and researcher who lives with chronic illness. Her faith, family, and love of nature shape how she uses whatever time she has: investing in relationships, advocating for public education and more just health care, and speaking honestly so others feel less alone.
Watch Kristie’s video or read her interview transcript below to know more about her story:
- Kristie’s first colonoscopy at age 51 led to an unexpected stage 4 colorectal cancer diagnosis on her husband’s birthday, reshaping how she thinks about time, work, and legacy
- Her experience with multiple treatment regimens has been physically and emotionally intense, but she emphasizes that, “There is beauty to be found… There is hope, and there are lessons to be learned.”
- Kristie shifted from being a constantly producing teacher to a writer and researcher, focusing on presence, purpose, and connection
- Her story highlights how serious illness is as mental as it is physical; it demands feeling hard emotions without staying stuck in despair, and choosing where to place hope each day
- Kristie’s marriage, faith, and friendships have deepened as she and her husband both live with cancer diagnoses, learning to let others help, protect space for caregivers, and hold on to joy alongside uncertainty
- Name: Kristie C.
- Diagnosis:
- Colon Cancer
- Age at Diagnosis:
- 51
- Staging:
- Stage 4
- Symptoms:
- pencil-thin stools
- constipation (had always been chronic and she attributed to perimenopause)
- Treatments:
- Chemotherapy, including adjuvant chemotherapy
- Radiation therapy
- Ablation therapy: liver ablation
- Surgeries: colectomy, temporary ileostomy, ileostomy reversal, liver resection (scheduled)
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- My name is Kristie
- I was diagnosed with colon cancer on my husband’s birthday
- My life before my colon cancer diagnosis
- Teaching, faith, and identity as an educator
- Subtle colon cancer symptoms and "Pay attention to your poop"
- Sharing a cancer diagnosis on my husband's birthday, and his own cancer experiences
- Marriage, caregiving, and being in the "C-Word Club" together
- Hearing “stage 4 metastatic” for the first time
- Telling our adult sons about stage 4 colon cancer
- What chemotherapy and radiation really felt like
- My original diagnosis vs. recurrence and living with chronic cancer
- Living with stage 4: hope, faith, and not choosing despair
- Redefining my identity after cancer as a writer, researcher, and outdoor person with chronic illness
- My message to newly diagnosed cancer patients and caregivers
My name is Kristie
I am from South Carolina, and I was diagnosed with stage 4 colorectal cancer. My cancer is technically colon cancer, but it is in the sigmoid part of my colon, which is so low that they go back and forth as to how they treat it, whether it is just straight colon or rectal, but it is technically colon cancer.
I was diagnosed with colon cancer on my husband’s birthday
I was diagnosed on July 12th, 2023, and I remember the date because it was my husband’s 58th birthday.
I had recently visited my OB-GYN. I saw her at 50. She told me I needed to have a colonoscopy, and I said, “Yeah, it is time.” I had watched my husband go through one at 50 and did not think anything about it, but it was not long after we had just started going back, opening up after COVID, and so I did not get a call from them. So when I went back at 51, she said, “Did you not get a colonoscopy?” And I said, “No, they never called me.” And she said, “No, no, we are going to take care of this right away,” and she had her nurse call an office in town, and they got me in within a couple of weeks.
When the nurse called, she said, “We have an opening on July 12th,” and I was hesitant. My husband happened to be there, and I said, “It’s your birthday.” And he was like, “No, no, no. Go get it done. Get it done in the morning, and then we will go do something fun for the rest of the day for my birthday.” And I said okay but it was my very first colonoscopy ever.
I woke up from the medicine, and the doctor said, “We found cancer.” That was the first thing he said. I was really silly about it. I was like, “How much is this going to disrupt my life?” And he said, “Oh, this is definitely going to disrupt your life.” He said, “I have already tattooed it and biopsied it, or I have taken some to be sent for a biopsy. I referred you to a surgeon. You should get a call from them within a couple of days.” So it was obviously big enough for him to tell that it was going to be a problem.
My life before my colon cancer diagnosis
I was one of those people. Some people would call me an overachiever. I was definitely one of those people who felt like a moment could not be wasted in a day. I was busy all the time. I taught secondary English. Most of the time, 11th graders. I would have a couple of 10th graders, and I would have a couple of seniors, but the majority were 11th grade. I was the department chair.
I was working on my PhD, which I did finish. So I was teaching during the day. I was writing a couple hours at least once a week, sometimes twice a week for my classes, conducting action research, very much active in church and community, and with friends, and so there was hardly ever a day when I just came home. I have two grown sons. They are now 27 and 22. When I was diagnosed — well, my younger one is still in college. He is working on a graduate degree, but my younger son was playing college baseball. My older son teaches. He teaches high school as well, high school social studies, and coaches football and baseball. So we were traveling to see my younger son play, and we were going to see my older son’s teams play. We were just very active. I did not slow down at all.
Teaching, faith, and identity as an educator
It is an immense factor in my identity. I would say, first and foremost, my identity is as a follower of Jesus, but then second, I am a wife and mom, third, an English teacher, and every one of those other identities has been shaped by my role as a teacher, my husband as a teacher, my older son as a teacher. We are a family of educators.
I have advocated at the state and national level for public education, for the National Writing Project, and for National Board Certified Teachers. I am a National Board Certified Teacher. I do not know how to look at the world outside of being a teacher. In fact, I was talking about children and my need to protect children. I said, I am a Christian, a mom, and a teacher. My entire existence is focused on protecting and educating children. The high school where I teach — or I did teach — was the high school my husband graduated from and both of my sons graduated from, and my husband taught in the same school district. I used to tell people it would be really hard to find somebody more invested in our local school system than me. Both of my sons played sports there. My husband did too. He coached. Our worlds center on school activity.
Subtle colon cancer symptoms and “Pay attention to your poop”
I tell everybody there were no signs, none that I would have been aware of recognizing. I did battle constipation. However, I have battled constipation most of my life. It was nothing new, and I was reaching the age of perimenopause, and I knew that that was also a time when digestive issues go along with perimenopause, and so I thought constipation was just part of my life. I had no idea that it could have been indicating colon cancer.
Later on, I found out that smaller, they call it pencil-sized stools, are an indication of colon cancer, I guess because the tumor takes up part of your colon and makes the stool smaller. When I look back, I can say, ‘well, yeah, I did notice some of that,’ but I was not aware that that was an indication of colon cancer. So when I was first diagnosed, I was just absolutely blindsided because I had no idea how to look for it. I had no hereditary expectations of it. Nobody in my family had ever been diagnosed with colon cancer. I was clueless. Maybe, had I been aware a little more of the idea of a pencil-sized stool, I might have been alerted. But I also was so busy and, as I said, had hit a point in my life of perimenopause, I probably would have attributed it to something else.
I have also tried to make it one of my goals when March comes around, and Colon Cancer Awareness Month, I try to make sure people know to get their colonoscopies. But I have adopted this hashtag on my Instagram. Whenever I talk about my colon cancer, I do hashtag “pay attention to your poop,” because I did not know that there was even the idea that there was a pencil-sized stool. So I really want to make people aware of this. It is gross, and people do not like to talk about it, but we need to pay attention to our poop.
Sharing a cancer diagnosis on my husband’s birthday, and his own cancer experiences
I have tried to make a conscious effort not to bring it up on social media on his birthday. I want it to still be his birthday, you know, but we are aware of it, and we make jokes about it between the two of us. I am very open on social media about my battle with cancer, but on his birthday, it is all about him. I try to make sure that he gets the spotlight and not, oh, yeah, this is my diagnosis anniversary. It is there. It is real. I am not ashamed of it or anything, but I do not want to take away from him.
He is also a prostate cancer survivor. He was diagnosed with prostate cancer in the spring, right before I was diagnosed. He had had his prostate removed the month before I was diagnosed, and in his prostate cancer journey, you know, the different MRIs and PET scans and things that we do, they found a meningioma in his brain, and so he had to have that removed. That was benign, though, but he had that removed the week before Thanksgiving, as I was in the middle of my first few rounds of chemo. So we have had our encounters with cancer.
Marriage, caregiving, and being in the “C-Word Club” together
It is absolutely huge. I tell everybody there is no way I do not think I would have done as well as I have done had he not been supportive. When major events like this happen, it does one of two things to a couple: it either brings them closer or it separates them. While he was with me in childbirth and stuff, prostate cancer meant that he came home from his prostate surgery with a catheter, and all the gross things that happened with colon cancer — when I had my colon resection, I had a temporary ileostomy.
He has seen me in a lot of really yucky situations, where my poop was hanging out of my stomach in a bag, and now, after the colon resection, I battle what is called LARS, low anterior resection syndrome, which means that I do not have a lot of wait time to go to the bathroom. He has been nothing but supportive and has seen me in lots of really gross situations, and I am so grateful that it has brought us closer, that it has made us a stronger team, and it has really made us understand that we do not want to go through life without each other.
We have seen each other in new lights and in some gross situations, but at the same time, it has really put the focus on our friendship, our partnership, our companionship, and our dependence on each other. I always thought I was quite the independent person, and cancer will not let you be too independent, especially when you are recovering from surgeries and have things like ileostomies. So it has made me appreciate him as someone I can depend on.
Hearing “stage 4 metastatic” for the first time
I want to tell you that when I met with the surgeon the first time — and he was wonderful to me — but the first time I met him and sat in his office, he was the one who had to deliver the news that I had already seen, which was stage 4. I had already seen the CT scan results because we get those online on MyChart, and I can read them, which I am very grateful for. The CT report showed everything was clear except for my liver; there were spots in my liver. So I knew that it was in my liver.
But when I sat in the office with him across from me, with my husband beside me, and he said, “It is stage 4 metastatic cancer. We do not talk about cures in stage 4. We will talk about palliative care,” he unloaded on me first and foremost, from the very beginning, before he said anything else, the worst case scenario. I did not understand that that was what he was doing at first.
My association with palliative care was when my father-in-law died when he was placed in a palliative section of the hospital, and they just gave him pain medicines as he died. So that was my first image of what he meant by palliative care. I started crying, and he said, “I know this is upsetting. I would be worried about you if you were not upset about this.”
Then he gave me the worst case scenario first, but then he sort of framed it for me —“Now that I have given you the worst case scenario, let me walk you back.” He said, “First of all, be very careful of what you read on the internet. A study that was current even just five years ago is out of date now. There are so many new treatments being created every single year. So the numbers from five years ago do not hold anymore. Secondly, even if we are not able to cure it, there are lots of treatments. It does not mean that you will die within two years. That may be what the numbers say right now, but we have lots of options.”
He said, “You clearly have a good support system,” with my husband being there. “What happens from here on out depends on your attitude and the approach you take. There are lots of supports available to you. If you keep a positive outlook, if you do what you are told in terms of taking care of yourself, still trying to eat and exercise, it does not have to be an immediate death sentence.” But he scared me pretty good to begin with.
Immediately, I thought about things like, I do not want to die in my 50s. My mother, who had some chronic illnesses — never cancer, but some chronic illnesses — died in her 60s, and I thought, “I am not even going to make it as long as my mom did.” Then my next thought was, “I am not going to get to be a grandma. I am not going to know what that feels like,” because I want to enjoy being a grandma. I immediately started thinking about all the things I was not going to get to do, and that upset me tremendously. I did a lot of crying. I did a lot of questioning, like, why? How did this happen?
I was so concerned about my health before I found out I had cancer. I am going to grab a Kleenex because my nose is running, and that is part of chemo stuff. Literally less than two months — it was probably closer to a month — before I was diagnosed, at the end of May, six weeks before I was diagnosed, I ran a 5K. I ran 5Ks probably three or four times a year, competitively. I would run for practice at least a mile, two, or three times a week, probably a 5K at least once a week. I used to be an active member of a cardio kickboxing group. It closed as a result of COVID, but I did yoga twice a week. I was in great shape. I was really particular about what I ate. My husband and I hiked all the time. That was our favorite thing.
We would hike and tent camp. Literally, the summer before, within a couple of weeks before I was diagnosed, when we would go see my younger son play in summer ball in North Carolina, we would tent camp. We would find a national forest or a campground close to the ball field, and we would bring our tent, and we would tent camp and then get up and hike, go get something good to eat, and then go see my son play ball. That was how we intended to spend all summer long. So I was wrestling with this: you have done so much to take care of your health, and it did not stop colon cancer.
Then I went on a thing of, well, where is this coming from? It is not hereditary — some people’s are, but mine was not. When they did the tests, they determined that it was not hereditary. It was environmental. So I went through this whole thing about processed foods. My area of research is adolescent literacy in the outdoor classroom, so I am quite the advocate for environmental concern and protection. I went through this thing like, these are environmental conditions that we have brought in, and so then I get angry. I went through a whole lot of trying to find what gave me this, despite trying to take care of myself, and I struggled a lot with questions of why and how this happened to me.
Telling our adult sons about stage 4 colon cancer
My husband and I, we have — I do not know if you call it a policy — we have just agreed that no matter what happens, whatever news we get medically, we do not do anything until we talk in person to Jordan and Joel, our sons. They hear first directly from us. My younger son happened to be playing ball in Virginia when I got this news. My older son, I came home and had him come to the house, and I told him, sitting on the couch.
My older son is the one who stuffs his emotions. So he listened really quietly and just said, “Yeah, okay,” and did not let me know how he was feeling at all. When we told my younger son, when we went to see him play ball in Virginia, the first night, we were like, we are not going to tell him before he throws. He is a pitcher, because I did not want this on his mind to affect his performance when he was on the mound. He came in — he is a relief pitcher, a left-handed relief pitcher — he came in for just two innings. After the game, we were cheering him on, had a really good two innings, and he said, “Coach said because I did not do but two innings, I am probably going to be in the bullpen again tomorrow night.” So we went, well, we cannot tell him now. He played an away game the next night.
So we went to see the away game, and it started raining. He had a really rough outing that time, but we had to tell him because we were going back home and, like I said, I was not going to tell anybody else — I was not even going to tell my dad — until I had told him. So we had to tell him after the game, before he got on the bus to go back, and it was awful. I hated telling them because I wished we had had more time to talk it through, but I said, “Joel, I have to tell you what the test results said.” We tried to reassure him. It was like, “It is okay. I am probably going to start chemo. We want you to stay and keep playing. There is no reason for you to have to come home because your dad will take me to treatments.” It was in the summer, so we were out of school. I was like, “You keep doing you. We want you to focus on your future,” which I realize now that was really how we felt, but that was impossible for him.
The summer leagues only go through the end of July anyway, so we only had a couple of weeks left, and when he came home before he went back to school, he was like, “Mom, you know I could not think of anything else. It was on my mind,” and I was like, “I know, but there was nothing you could do.”
Later on, when the chemo got really rough, and they were planning for the colon resection surgery, he would talk to my husband on the phone without me, and my husband would tell me later. He would say things like, “Do I need to come home?” My husband said that he would tell him, “I will let you know when it is time to come home. If I thought she was in that bad of shape, I would have told you to transfer to a school down here. But she would be so upset if you gave up baseball to come back home.” So what we ended up doing was, when he played his college games, my husband would — we had a Jeep Wrangler and a Subaru Outback — whichever vehicle we took, he would clear out the back and lay blankets and pillows down, and I would lay in the back until our son came in to pitch, and he would text me, “He is in the pen.” Then I would get out, go sit in the stadium, watch him throw, and then I would go back to the car. We made it work.
I am going to tell you one other quick story. After my colon resection — that was on January 29th, 2024 — they ran more tests. They do CT scans and things like that to see if the surgery worked. When I went back to my oncologist, he told me, he said, “You look clear now.” He said, “Come here,” and he pulled me up to the screen. I have to say this about all of my oncologists and surgeons: they have been wonderful about this. Whenever they pull up the records on the screen, they would have me come sit beside them, and they would show me exactly what they saw. He said, “I want you to look,” and he had changed my diagnosis from palliative to curative.
Now we are back at palliative because it has recurred in my liver — that is another story — but when he told me that, when he showed me that he moved it to curative, my friend Vicky, who takes me to several treatments — I have been so blessed with friends who have taken me to treatment: Vicky, Evelyn, and Sherry. They have taken me to my chemo treatments so my husband can continue to work during the chemo treatments. That way, he saves up his days so that he can be there with me in surgeries. His current employers have been wonderful about letting him get comp time so that he can be with me during the surgeries, but for regular everyday chemo, my friends would take me.
So my friend Vicky was there. My husband met us there. After that meeting, I came out and told them first. We got in the car, and I called Joel first in West Virginia and told him that they had moved it to curative, and I could hear him crying, and I am going to cry thinking about it. Then we got home, and I waited for my older son to come in from work and got him in the living room, and told him that it had been moved to curative. He said, “Good,” and he went to the bathroom, and I heard him break down. As I said, he is the one who stuffs his feelings.
That day, it was clear to me how much effect it had had on them when it was like they could finally relax. They handled it pretty well in front of me, but when I was able to give them the good news, that was when it really became clear to me the effect it had had on them. Honestly, my older son moved home. At first, he moved home to stay. He never said outright that it was because I was in chemo, but for the first year of my chemo and surgeries, he lived at home. That next summer, after I had had the surgery and it looked much better, he moved back out. As I said, he will not say it out loud, and the other one says it to my husband, not to me. I think they do not want to upset me either.
What chemotherapy and radiation really felt like
I despise chemo. I am on a chemo break right now because I am scheduled for a liver resection on December 23rd. Today, the day that I am recording this, would have been my next chemo treatment, and I am so grateful that I am not in that infusion center. Let me say, my infusion nurses have been nothing but good to me. They are so compassionate and caring.
I only had five days of radiation. They did radiation right before my colon resection because they said that would improve my chances of not having a recurrence, but because I had radiation, that is what required me to have the ileostomy. They said it did so much damage that they did not want me to try to pass stool through that damaged area. That is why they had to do the temporary ileostomy, and I am very fortunate and grateful that my ileostomy was able to be reversed.
As far as chemotherapy, I have been through three series now. The first one: seven treatments, seven treatments of this drug combo, and I had an eighth treatment before my colon resection without one of the drugs because they needed to stop that earlier than regular chemo before I had the surgery. What the pump means is — this series, I would go on a Tuesday and get probably five hours’ worth of infusion in my port, and then they connect me to a pump. Then I wear the pump home for two days, for 48 hours, and then I go back on a Thursday, and they disconnect the pump.
In my experience, chemo side effects are cumulative. The first couple of times that I had chemo treatment, it was not horrible. I got a little sick to my stomach. I did have diarrhea. One of the side effects of every chemo version I have had has been diarrhea. I have to run to the bathroom, but at that point, to begin with, it was before I had my colon resection, so it was manageable. In the first two series, I had to go to the hospital a couple of different times. They discovered through all the scans that I have diverticulosis, and the first time I had that one chemo drug, it irritated that, and it turned into diverticulitis, which caused fever. One of the things they tell chemo patients is that the minute you get to 100.4, you have to go to the emergency room immediately. That is where we discovered the diverticulitis, which was painful and caused a fever. A couple of times, I have gotten dehydrated, especially with the ileostomy.
The side effects are rough, no lie. I did not have much neuropathy at first. The worst of the first set was diarrhea and nausea, and dehydration. While I had the ileostomy, I went through my second series. They called it adjuvant chemo. They were hoping just to prevent recurrence, and it has worked for the colon — praise God, I have not had any recurrence in the colon. It did not prevent recurrence in my liver. For the adjuvant chemo, they moved me to another chemo drug. That has some really yucky side effects.
I now have neuropathy. My feet, especially — I have some in my fingertips but mostly in my feet — which is numbing and painful at times. I have really sensitive feet. This new chemo drug also causes cold sensitivity. You cannot drink cold drinks. It literally sends electric shock waves in your mouth when you go to drink something. I will never forget the first time I felt it in my fingertips. I thought I was putting sour cream on a baked potato or something, and we had the squeezable sour cream. I picked it up and dropped it and screamed; it was like electric shock waves through my fingertips. It is just massive cold sensitivity.
Of course, I have lost some of my hair. I have not lost all of it, thank goodness, and I am very appreciative of that. I can try to rock a pixie cut. With the new chemo drug, the cold sensitivity got so bad that we tried to do oral chemo. I forgot what it was called, but I tried the pill because I had read on several support groups online that people did not experience the side effects with the oral chemo as they did with the infusion chemo.
So I tried that. Well, then I had what they call hand-foot syndrome, and I got to the point, after a few weeks of oral chemo, where I could barely walk. I would go see my son play baseball. I would stay in the car, and then my husband would drive me to the front and help me walk to the seat. My feet were in such pain and so tender, and they were peeling, the skin was peeling, that it was just horrible. It was just painful, and the skin on my hands was peeling. So then the doctor said, “Okay, we need to stop this for a while,” and so we went on watch and wait until it showed back up in my liver.
I have had two liver ablations, where they have gone in and done lasers to try to cut those out. After the second one, when it showed up again, my new oncologist — my prior oncologist moved away — said, “We are going to have to go back on chemo.” This time, I was on the first combo I tried again, but instead of one drug, they did another. Again, the worst parts of that have been the diarrhea, but the new drug caused what they call “chemo rash.” That has been on my face and neck, but they cheer when you get the chemo rash because that is an indication that the chemo is working, and it has.
I tell everybody, and it is such a cliché, but chemo is a literal and a metaphorical toxic relationship. It is literally putting toxins in your body to kill the cancer, but you have to be grateful for the toxicity because it is killing the cancer. It is the definition of a toxic relationship. I watch my face break out and flake; then it dries out. If my face looks shiny right now, it is because I am constantly putting Aquaphor or baby oil on it to counter the dryness that comes from the new drug. Here is the funny part about it: my hair is coming out because of the regimen, but the new drug is turning my face into werewolf world because my eyebrows are not normally black (they are normally brown), and my cosmetologist said I look like Bert and Ernie. She trims up the eyebrows, but the eyelashes, boy, they are on point. They are just thick. I am getting little hairs all over my face like I never had before in my life.
It is just such an emotional roller coaster: you are throwing up one minute, you are pooping another, your hair is falling out, but it is growing on your face, and there is the fatigue. That is the word they use, but I say it is more like weakness. I told somebody it feels like what it feels like when you are in the ocean, and you are trying to walk against the waves, and you are having to push so much harder on your legs. That is what chemo fatigue feels like. My friends have learned. I am like, this is chemo week. I am in the house this weekend. Then, on my off week, I start feeling stronger, and I can go do things again.
It is a whirlwind, a storm of symptoms and emotions and ups and downs mentally and physically. People told me over and over again, all my nurses and doctors said, the cancer battle is as much mental as it is physical. It is. You have to learn to accept when you cannot do things and then take advantage of the moments you can, and you must learn to deal with the uncertainty. Anyway, I would not wish chemo on anybody except for the fact that it kills the cancer. Now, because of the chemo, I can have a liver resection, but I never thought I would say, “Please cut on me.” I would rather you cut on me than go through another chemo treatment.
My original diagnosis vs. recurrence and living with chronic cancer
I think the original diagnosis was worse, and I will tell you why, but my reaction to the relapse is a different one. The original diagnosis threw such a curve in my life. My husband would probably say a U-turn. It was so unexpected. It derailed my expectations for my life in such a way. I honestly thought I was going to be back at work after a semester.
I remember the first time insurance people started telling me to apply for disability. I thought, “They think I am going to die.” I planned to go get chemo, get surgery, and be back. I struggled for months with that initial diagnosis before I came to be at peace with the idea that I may never go back to work full-time, that I am going to have to fulfill my destiny differently, and it is not going to be full-time teaching anymore. So I wrapped my mind around, well, you have always wanted to write. Here is your chance to write. You can write from the bed. So that is what I have tried to embrace. I have tried to embrace a new academic purpose in my life.
The relapse has a different reckoning. When I went back on chemo this third time and we started the Signatera test, those are the blood tests that indicate whether, even if the scans show clear, there is still cancer in your blood somewhere, that it is still there, that there are cells they just cannot see yet — my Signatera, ever since the first one I have had, has been positive. That means I am not rid of the cancer, regardless of what the scans show. Then I saw the numbers increase. So I had to reckon with, “Okay, what am I going to do with this time that I have, and how am I going to negotiate having a chronic illness?”
It goes from thinking you are going to be cured to dealing with chronic illness and dealing with how you navigate life that way. Then I had to confront the idea: Am I okay with chemo for the rest of my life? Because that is where it was leaning. Probably less than two months ago, my oncologist said I would most likely be on chemo for the rest of my life. I might qualify for a liver transplant, which was a whole other scary option, because that is a huge major surgery. That is when I started thinking about second opinions.
I have been blessed with wonderful insurance, and that is truly a blessing. My insurance has a medical nurse and a mental health nurse who call me once a month, and I have fully taken advantage of that service. They have been so helpful and supportive in helping me talk through my thoughts on what is happening. My medical nurse asked me if I had thought about a second opinion, and I said I had not before now, but I am now. I need to see if there are other options out there. She said, “If they are in network, we cover it,” and I was like, “This is wonderful news.”
So I started doing some research and reached out to MD Anderson in Houston, and I was amazed at how quickly they responded. They were like, “Yes, come here, let us see what we can do.” When I met with my oncologist there, she said that I had received excellent care, which I knew I had. I have received nothing but top-notch care, excellent doctors. She said, “I am not sure that there will be other options,” and she was honest with me at the beginning, too. “But let us do some really high-powered tests and see what we can find.”
When I got the first results from those high-powered tests, they showed some things in my abdomen and lungs. My immediate reaction was, “It has spread even further,” and I really had a breakdown moment then. I went through that again: “I do not want to die in my 50s,” and I thought, if it has spread, it is going to go quickly. Then, when I talked to my oncologist again, she relieved me of those fears. She said, “No, that is not cancer there,” and when I met with my surgeon, he said the same thing. “The spots in your lungs are most likely scars.” I have had COVID three times. They could be scars from COVID or from some type of lung infection as a child or something. She said their machines were just so powerful that they were going to pick up any abnormality, but those are not cancer. I was so relieved.
I had a moment of confronting that my death may be far more imminent than I had pretended before. I faced a moment then, and my husband was so positive. He was like, “You do not know that yet. Do not buy trouble before you know.” I did, though. I honestly thought at that point that I needed to give specifics of the funeral I wanted. Honestly, before I had my colon resection, my husband and I did go visit an attorney and have all the paperwork drawn up for wills and living wills, and powers of attorney, and those kinds of things, because it made it real. I had to confront the reality of what may happen, and that is not pleasant at all.
The good news is that when my oncologist called me, she said she had presented the scans to the tumor board, and an amazing surgeon has agreed to do a liver resection. They actually think that I may not have to have chemo afterwards. So I am holding on. I am holding on to faith that that is what is going to happen. As I said, my liver resection is on December 23rd. But now, because I have been through these ups and downs, it is never out of my mind that this is what we are going to try now. I am not banking ever on it being over. I am praying hard that I will not have to do chemo again, and my oncologist is certain that we have lots of options later on if it recurs again.
The idea of recurrence is always there now. I will die, whenever that is — when I die, I will die expecting a recurrence. It is part of my life now.
Living with stage 4: hope, faith, and not choosing despair
I have to hold on to my faith. I have to believe that God will turn this into something good. He already has, and He will continue to turn what is yucky in human terms into something beautiful. I have seen it happen. I have seen it happen multiple times. It does not change the reality that death is close, but the fact that death is close has made me reckon with how I want to spend the time that I have.
I had a friend ask me, “How can you be so hopeful? How are you holding on to your faith?” I am like, “What is my alternative? If my alternative is despair, do I want to spend the time I have left in despair? No.” I do not want to spend a moment in despair. It has really made clear to me that, if before my diagnosis I was conscious of making every moment count, it was in a different way of making every moment count. I was very driven by this idea that I had to produce. I had to produce professionally. I had to produce in terms of service. I had to be working toward something good.
It is the same now, but it is a different good. It is not necessarily a production that is valued in the professional world. It is: how am I going to make every moment count for when I am gone, that I will have left a positive legacy, that I will have invested in the people that I love, that I will have invested in what I want to say to the world in terms of my writing, and what I want to leave for others?
It has made me hyper-aware of my privilege. I can stay at home and focus on my health and doing what I want to for the rest of my life because I was a public school teacher who built up retirement funds and has really good insurance. It has made me hyper-aware of that, and so I am driven to shout about the injustices that exist in our health care system, that people who do not have the insurance that I have are trying to work and have chemo. Some people lose their homes because they cannot afford treatments and have to choose between medicine and essential elements of life. As I said, this has made me hyper-aware of my privilege, so I feel like God is telling me, “You need to use this time to advocate for others. You need to use this time to raise awareness and to show others that there can be hope in a desperate situation.”
It all comes down to, I have to choose how I am going to spend whatever time I am given, and I do not want to spend it in despair. So where do I find my hope? I find my hope in God. I find my hope in the love of my family. I find my hope in spending time in the beauty that is nature, finding healing in nature, and sharing literature, because that is why I became an English teacher: to share stories. That is why I was interested in this. Our lives are composed of stories, and I want my story to be a good one, one of hope.
It has made me far more dependent. I mean, I did daily devotions before I was diagnosed, but my conversations with God are so much more real now, and I thought I understood what depending on God was when it came to my children growing up, when I could not protect them anymore. It has just intensified now. I have seen marriages break up. I have seen people get angry at God, but for me, if God and my family are what matter most, I want to use this time to draw closer to them, and they are what bring me happiness.
Redefining my identity after cancer as a writer, researcher, and outdoor person with chronic illness
Part of me takes pride now in calling myself a writer/researcher. That is what I call myself now, not necessarily a teacher. I am teaching one class adjunct at a local college, and I love that, but my body is not going to allow me to be a full-time teacher anymore. So I am trying to embrace it, and I take some pride in saying that I am a writer and researcher.
But gosh, my friends in my PhD program are headed to Las Vegas this week to the Literacy Research Association conference, and I am not going with them. That still sticks in my craw. That is not completely out of the picture in the future, but sometimes I get a little anxious, thinking that I am losing ground professionally. And then I have to readjust. I have to readjust.
Last spring, May of 2025, the school where I taught had a large AVID program. AVID is a particular program to help students get college-ready, and every year I taught a group of AVID students English 101 and 102. These are early college students who graduate with an associate’s degree with their high school diploma. The AVID director would invite me to a graduation celebration of those AVID students.
This past May, I was invited, and that was my last group. That was my last group of students to graduate from the school where I taught. The kids that are at the high school where I taught now, the kids that are there now, I do not know them. I did not teach any of them, and that hurts my feelings when I think about it. Then I have to readjust my thoughts: you are not teaching that group of students anymore. You are reaching a different group of students now, and you are reaching a different audience. You have a different purpose now.
My husband has said that I might not have pursued this part of my career had cancer not happened. I would have held on to those high school students so long. He was like, “This is giving you a chance to see what else you can do,” and that is what I have to think of it as.
My identity as an outdoors person — sometimes I wonder if others will view me as a fraud because, as I said, my research is adolescent literacy in the outdoor classroom, and I can still do small lessons outdoors. But the person who used to hike 7 to 10 miles and then come back to a tent, I cannot do that anymore because I have to be close to a bathroom. I can do short walks, and I try to as often as I can, but I really miss that part of my identity. I always have to be conscious of where the bathroom is and whether I have taken Lomotil so that I can go out in the woods.
That part of my identity, I am struggling with losing that part, and I have to reshape it. I cannot run right now, one, because of chemo, and two, because of neuropathy. So I am like, well, when I can start training again, when I have the energy to start training again, maybe I can start doing race walking instead of running. Then I see, well, this is okay. You can be an example, a spokesperson for what it means to be outdoors with a chronic illness. As I said, it is constantly readjusting my thinking.
My message to newly diagnosed cancer patients and caregivers
First message is for caretakers: caretakers have to be taken care of, too. I have seen my husband. We have recently had to help his mother move into assisted living as she is getting older, so he is taking care of an elderly parent and me, and he has worn thin, just frazzled. He needs time where he can relax, where he can do what he wants to do. Sometimes that means away from all humans. Sometimes he needs to be by himself, and sometimes asking him, “What would you like to do?” is even too much for him. He is just like, “No, you just decide and let me chill.” So I definitely want to say caretakers need to be taken care of, too.
In terms of being diagnosed, it is okay to feel what you feel. It is okay to feel it and acknowledge it. One of the things I try to do is say, “Okay, this is fear that I am feeling right now,” or, “This is jealousy that I am feeling right now.” It is okay to feel what you feel. Know that people are not going to understand unless they have been through it. They are not going to understand. Some of them will want to understand. Some of them will be afraid and step back.
Some people will say things that are hurtful and they do not intend to be hurtful, and it is okay to say, “That was hurtful” — even if you do not say it in front of them — to acknowledge it again, to say, “that hurt my feelings.” Process your feelings. Acknowledge them, and when you are feeling down, say, “It is okay to feel down now,” but know that it is not good to stay there. It is not good to stay down.
There is hope. We can keep going. Our lives may not look the same, but there is beauty there, too. There is beauty in learning what your body can do, even as it is battling chemo side effects. There is beauty in learning that you are more than what your face says. The women’s issues — losing hair and things like that — I have really had to reckon with my vanity, and that is what it is. It is vanity. Beauty truly is more than what is on your face.
The friendships that last while you are battling cancer are the real friendships. Those are the ones with the people who truly care about you, and those are the ones worth holding on to. Those are the ones that will see you through it, whether it is the friendship with my husband and my friends that carry me to treatments, the ones who pray with me, or the ones who send me sweet messages. Those are what carry me through.
it is okay to feel down, but try your best not to stay there. Try to change your thinking to see where the beauty is. What is the message God is sending you? What is there to see that you did not understand before? Maybe think of it as a new quest, a new challenge in life. As an English teacher, I used to say, “This is a plot twist in my story. Where is this going to take me, and what new things am I going to discover?”
It does not mean that you are not going to be in pain, both physical and emotional, but again, what is there to learn from the pain? What is there to see in the pain? How does that make you more sympathetic to others’ pain? Where is this journey going to take me now? I have learned things about teaching from my experience as a patient. So there is beauty to be found. There is hope, and there are lessons to be learned.

Inspired by Kristie's story?
Share your story, too!
More Metastatic Colon Cancer Stories
Raquel A., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Frequent bowel movements, pin-thin stools, mild red blood in stool
Treatment: Chemotherapy
Steve S., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Blood in stool, changes in bowel habits, feeling gassy and bloated
Treatments: Surgery, chemotherapy, monoclonal antibody, liver transplant
Jessica T., Colon Cancer, BRAF+, Stage 4 (Metastatic)
Symptoms: Severe stomach cramps, diarrhea, vomiting, anemia (discovered later)
Treatments: Surgery (hemicolectomy), chemotherapy
Jennifer T., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Weight loss, coughing, vomiting, sciatica pain, fatigue
Treatments: Surgeries (colectomy, lung wedge resection on both lungs), chemotherapy, immunotherapy
Kasey S., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Extreme abdominal cramping, mucus in stool, rectal bleeding, black stool, fatigue, weight fluctuations, skin issues (guttate psoriasis)
Treatments: Surgeries (colectomy & salpingectomy), chemotherapy