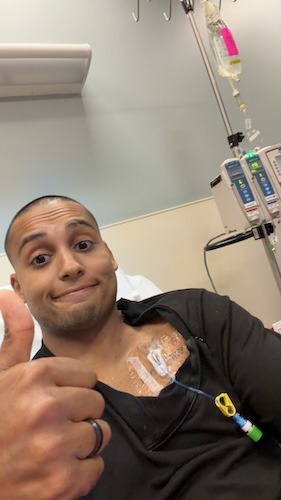
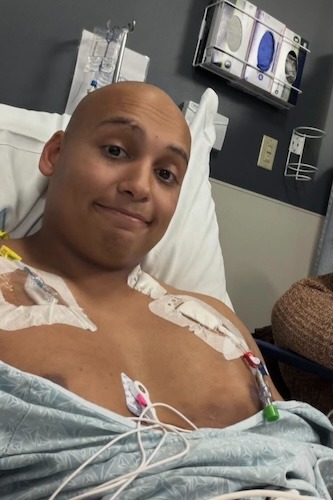
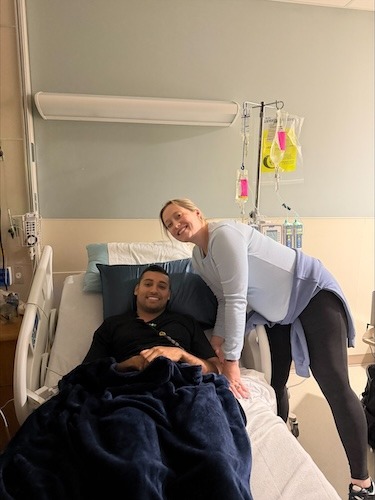
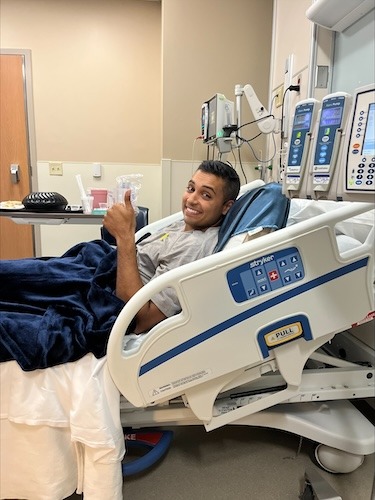
James Faced Recurrent Hodgkin Lymphoma While Becoming a Dad
Hodgkin lymphoma and a stem cell transplant aren’t what most people expect to face in their early 20s — let alone Hodgkin lymphoma twice — but that’s exactly what happened to James. He was first diagnosed with stage 2 Hodgkin lymphoma at 22, during his senior year of college at the University at Buffalo. He struggled with weeks of night sweats and intense itching, and his younger brother spotted a tennis ball-sized lump on his neck. Within weeks, James was fast-tracked to Roswell Park Comprehensive Cancer Center, where he started ABVD chemotherapy, determined to finish his finals, graduate on time, and hold onto a sense of normalcy even as his hair fell out and his social life became a blur.
Interviewed by: Nikki Murphy
Edited by: Chris Sanchez
James reached remission after six months of treatment for Hodgkin lymphoma, but life after being declared cancer-free was far more complicated than he expected. He describes feeling like a “shell” of himself in college and then struggling to reenter everyday life. To cope, he numbed himself with alcohol and distanced himself from people while “scanxiety” and fear of recurrence quietly grew in the background. Over time, he stopped drinking, went back to graduate school for his MBA, and built a career in sales that had him traveling across the country. He also met his future wife, and they now have a newborn son.

Seven years later, subtle but familiar warning signs appeared again: a small lump, swollen lymph nodes, and the same relentless itching. Initially, his blood work was clean, and doctors thought it was an infection or mono, but scans and a biopsy confirmed that his Hodgkin lymphoma had returned, likely due to reawakened dormant cancer cells. The timing was devastating: his wife was around 29 to 30 weeks pregnant when they learned he would need intensive chemotherapy and an autologous stem cell transplant, necessitating prolonged hospital stays and a long recovery.
Through grueling high-dose chemo, isolation, neuropathy, fatigue, and the emotional toll of being immunocompromised while preparing for fatherhood, James kept getting out of bed each day, walking the halls, and writing down one thing he was grateful for. About two to two and a half weeks after his stem cell transplant, he was declared no evidence of disease (NED) and cleared to be in the delivery room to meet his son. He calls this experience “phenomenal” and is one of the images that kept him going during the hardest nights in the hospital. Today, he is rebuilding life in Buffalo with his wife and baby, navigating isolation, and working from home. He redefines survivorship as giving back to others through events like Ride for Roswell and Light the Night.
Watch James’ video or browse the edited transcript of his interview below. You’ll learn more about his story:
- Early Hodgkin lymphoma symptoms like night sweats, intense itching, and a noticeable neck lump should never be ignored, especially when they persist or worsen.
- Community connections and specialized cancer care at centers like Roswell Park can accelerate diagnosis and treatment, helping patients move quickly from fear to a clear plan.
- A universal truth in cancer care is that recovery is not only physical; mental health support, including therapy and naming depression or anxiety, can be essential to healing.
- James’ experience shows that life after a stem cell transplant involves lasting changes like isolation, fatigue, and neuropathy, but also new purpose, including fatherhood and advocacy.
- He focused on small daily wins and practicing gratitude, even on the hardest days. This helped him keep moving, both literally and emotionally, through intensive chemo and stem cell transplant recovery.
- Name: James B.
- Age at Diagnosis:
- 22; recurrence, 29
- Diagnosis:
- Relapsed Hodgkin Lymphoma
- Staging:
- Stage 2 (initial diagnosis)
- Symptoms:
- Night sweats
- Itching
- Persistent lump in the neck
- Treatments:
- Chemotherapy: ABVD, ICE, and BEAM
- Autologous stem cell transplant
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Introduction and first diagnosis
- My first symptoms during college
- The path to my first cancer diagnosis
- How quickly my symptoms escalated
- When the word “cancer” entered the conversation
- Fast-tracked care and community connections
- Hearing the first diagnosis and college impact
- My ABVD chemo regimen and finishing college on time
- Social life, drinking, and being a shell of myself
- Remission and the seven years between
- My second diagnosis and recurrence
- Intensive treatment: ICE, BEAM, and stem cell transplant
- The birth of my son and the timing of my recovery
- Recovering from a stem cell transplant with my newborn child
- Isolation, immunity, and my new routines
- Survivorship, scanxiety, and giving back
- Encouraging other men to seek help
- My message of hope
Introduction and first diagnosis
My Hodgkin lymphoma diagnosis and where I live
My name is James. I was diagnosed for the first time in 2018. I have had cancer twice. The first time I was diagnosed in 2018, it was the end of my senior year of college at UB with Hodgkin lymphoma. It was stage 2 at that point. I went through chemo, came out the other end, and recovered. Fast forward seven years, and it came back in September 2025. This time, the treatment was a lot more intense, but it was the same diagnosis.
Who I am beyond cancer
So I do sales and have been in sales for a couple of years now. I work from home, which has been very flexible with having a newborn. I recently became a dad about ten weeks ago. My son was born on December 2nd, so just a couple of weeks after I finished my last treatment of chemo and my stem cell transplant. I was in the hospital with my wife, holding my newborn. So things went pretty quickly. Outside of all this, I enjoy golfing and supporting the Buffalo Bills and Buffalo Sabres, because I am from Buffalo, New York. There is not much to do here other than support sports, as there is always snow outside.
My first symptoms during college
Early Hodgkin lymphoma symptoms in college
I started waking up in the middle of the night, having sweats, a little drenched. I kind of just brushed it off as maybe I was battling an illness or something. Then it started getting to a point where I was experiencing itching on my legs and my arms, really aggressively. I was starting to have scars, and I thought, “This is probably not normal.” I stayed pretty healthy, and I worked out; I kept myself in shape. But my younger brother noticed a huge lump on my neck. I always thought it was maybe just an inflamed muscle or something I pulled. I never honestly really looked into it too much, but when I finally looked at it, it had grown to probably the size of a tennis ball. That is when I knew that it was not normal, and I had to get that checked out.
The path to my first cancer diagnosis
The first thing I did was go to my primary doctor. I showed them the lump and said, “Hey, I’m not sure really what this is.” They looked at it and said, “We recommend that you do a scan.” I think it was a CT scan first, and then it ended up being a PET scan, and then an overall biopsy at the end. After the first scan, they told me, “We recommend you go to Roswell Park,” which is our cancer hospital in Buffalo, New York, to get this checked out. Things moved pretty quickly. Within a couple of weeks, I was at Roswell for an appointment with the lymphoma team. From there, just based on the sheer size of my neck and how it looked, they immediately ordered a biopsy, which is when they figured out that the tumor was cancerous.
How quickly my symptoms escalated
From the time of the night sweats to the diagnosis, it was about two weeks, so it moved pretty quickly. I think the sheer size of the lump definitely scared my primary doctor to the point where I was getting an appointment with Roswell within a couple of days.
That lump had not just grown over two weeks, though. I looked back at pictures because I was curious: how in the world did I not see this? In all the pictures, there was something there. I just never noticed it. It was the craziest thing. I do not know how I never noticed it or how I was never aware of it, but it had always been there. I just never focused on it until my brother called it out. Then it became very apparent that it was not normal.
When the word “cancer” entered the conversation
When I was recommended to Roswell, deep down, I started to get some fear about whether this was cancer or not. If you are at your primary doctor and they are not able to give you an answer on something, and they are directing you to a cancer doctor, that is usually when fear starts to creep in, and you get a bad feeling about it. That is when I thought, “Oh, this is not good,” because I had gone to my primary for other things, and usually they had an answer. When they do not have an answer, and they are directing you to someone like a cancer doctor who might have an answer, it is never a good feeling.
It was about two weeks of blood work and scans before the full diagnosis. They did blood work first, then a CT scan and a PET scan. I think all of that happened within a week. Based on the scans, they scheduled a biopsy for the following week, and then I had my follow-up with my doctor a day or two later, where they essentially told me, “This is cancer, and we need to get you started on treatment right away.”
Fast-tracked care and community connections
I am very lucky. We have a lot of connections in the community, which is great. One of my neighbors works at Roswell, and I was living at home at that time while still in college. My parents immediately called them, and they were able to get me in really quickly, because I know at times it can be drawn out. I was very fortunate.
Hearing the first diagnosis and college impact
How I processed a Hodgkin lymphoma diagnosis at 22
It is tough when you are 22 years old and in college. You have finals going on, and all your buddies are talking about going out to the bars and living a normal life. You are sitting in the waiting room, and the doctor is telling you, “You have Hodgkin lymphoma, stage 2, and we have to get a port in your chest and start chemo for the next six months. This is your plan; this is the layout.” Every plan you have just goes out the window.
As a senior in college, you are trying to think about your career: what am I going to do after college? Where am I going to work? Next thing you know, it is, “Okay, how am I going to survive and get through this so that I can have a career and have a life after this?” It was depressing and really tough. But I tried to be positive each day.
When you are in a hospital, you see people in much worse situations. I tried to have some gratitude that at least there is a cure for my situation, versus some people who have terminal cancer. I tried to consider myself the lucky one, that my body just had to go through a little pain for six months, and then I could come back on the other side stronger and ready to attack life again.
My ABVD chemo regimen and finishing college on time
My treatment was the ABVD regimen. It was chemo every other week, so essentially twice a month for six months — twelve treatments total. Each treatment lasted anywhere from four to five hours. The chemo was a drip with four different kinds of drugs being dripped into your system.
At first, I did not have a port, so it was going through my veins. I do not recommend that, because it was excruciating. Eventually, I did get a port because I could not keep doing that.
I still went to class. I would do chemo, then rest up for a couple of days. The first couple of rounds of treatment were not as bad for me. I was able to do my finals, graduate on time, and walk across the stage, which was great. I did it a couple of days after treatment and was not feeling great; my hair was falling out. But I still made it a priority to walk across the stage. It was something I wanted to do and something to be proud of. It was definitely tough.
Social life, drinking, and being a shell of myself
Looking back, I do feel like I missed out on parts of the college experience. At that time, I was drinking a lot. I do not drink anymore; I am four years sober and have been sober for a while now. I would still go out, which I would not recommend. I would go out every once in a while and feel like s*** most of the time. I would not feel great.
My social life still existed, but mentally, I was never present. I was physically in places, but I was never actually there. I was a shell of myself. I was in pain a lot, with a lot of joint pain. I was constantly exhausted. I would sleep for days at times. I did not have an appetite. I tried my best to get out and be a part of life, but I just never felt the same.
Remission and the seven years between
Hearing “remission” and post-treatment depression
Hearing “remission” after six months of treatment was huge. When you are in that battle for six months, you start to accept that maybe this is your life moving forward. It becomes the same cycle: you start to feel better after chemo, and then you are back in there again.
When I heard “remission,” I was just so thankful, because you always fear that your scans will not be clean. I was grateful and happy, but at the same time, I did not know how to live life. I struggled coming out of being cancer-free. I did not acclimate back into normal life well at all. I was abusing a lot of alcohol to numb myself, just being transparent. It was one of the things that made me feel okay and safe. I distanced myself from a lot of people. People do not talk about it much, but you can get really depressed after treatment. There is a lot of fear and anxiety that comes from being cancer-free, because you still have to go back for scans, and there is always the fear of recurrence.
Eventually, over time, I distanced myself from alcohol and was able to start building a life back up for myself. I went back to grad school and got my MBA. I got into a career I love that lets me travel across the United States. I met my now wife, and we now have a beautiful son together. I was able to get married. A lot of great things happened from getting past this. Obviously, it came back, but those things are still great, even though I had to fight it again.
My second diagnosis and recurrence
Signs and symptoms of Hodgkin lymphoma recurrence
Before the recurrence, I was traveling a lot for work. Sometimes I get sick from being on planes. After one trip, I came back home and was not feeling good. Being seven years clean, I did not think it was cancer. I thought I had just caught something on the plane. But it lasted for a couple of months, to the point where I started to get a little lump, and my lymph nodes were swollen. They were not as big as last time, but they were swollen and noticeable in my neck, which definitely alarmed me. Then I started to get that itching again that I had when I was first diagnosed. That really alarmed me.
I went to Roswell. They did some blood work, and my blood work came back clean, which was a relief. They put me on some antibiotics, but nothing really helped. I still had the lump on my neck and was still not feeling good. They eventually said it was mono. They did a scan. Apparently, something I was not aware of then, mono can at times cause dormant cancer cells to reawaken. If your treatment did not work right away, sometimes you have very tiny dormant cells that just exist. Apparently, the mono reawakened those cells. When they did a scan, they saw that. They did a biopsy and confirmed that my cancer had indeed returned.
The emotional impact of a second cancer diagnosis during my wife’s pregnancy
My wife and I had just gone on our babymoon. We went out to Colorado and then to Vegas. We were traveling before the baby came. It was really tough. My wife was pregnant, sitting across from me, and I was in the room while the doctor told us the cancer had returned.
Instead of an easier regimen of treatment, though the last one was tough, this new treatment plan was very intense. To hear that, knowing we had a baby coming, knowing that I would be spending nights at the hospital instead of just going in for day treatments, and facing a stem cell transplant on top of that, it was tough. It was extremely disappointing to hear. I was filled with a ton of fear, and we did not really know what to do at that moment. It was a really dark moment for us as a family.
She was about 29 or 30 weeks pregnant at that point. She was getting close.
Intensive treatment: ICE, BEAM, and stem cell transplant
My ICE chemo, BEAM chemo, and transplant timeline
The plan was ICE chemo and then BEAM chemo with a stem cell transplant. I would start with ICE chemo. ICE chemo meant three to four days in the hospital, where I would get treatment around the clock. Then I would have two to two and a half weeks to recover, and then I would be back again at the hospital overnight getting the same chemo.
After the second round of ICE chemo, if my scans came back clean, I could proceed to the next phase, which was BEAM chemo. If they did not, I would have to do ICE chemo one more time. Thankfully, after two cycles of ICE chemo, I was good and moved on to BEAM chemo.
I already had a port in my chest and still do, but for BEAM chemo, they needed to put another port in with thicker tubes and wires sticking out. Before I even did BEAM chemo, they harvested my stem cells. They put me on medications that allowed my stem cells to move into my bloodstream. I spent two days having my stem cells harvested. I would go into a clinic at Roswell from about 7 a.m. to 1 p.m., be hooked up to a machine, and they would harvest and freeze the cells. After they harvested enough, I was admitted to Roswell for seven straight days of chemo.
That was the BEAM chemo. I did not fully realize while I was going through it — and I am happy I was not — but the regimen itself is very intense. It completely wipes your system and your bone marrow clean. At the conclusion of that chemo, they reinfuse your stem cells that were frozen back into your body through a drip.
This was a lot different from just going in every other week for a couple of hours. This meant putting the rest of my life on hold. I could not work. I had to have a caregiver after this. My wife, who was pregnant with our child, was driving me to all my appointments. I had to go every day. I was on a ton of meds. The stem cell transplant is no joke. I was in good shape, but going through that, I had complications. I had to go back to the hospital because I started to have a fever. I had to spend a couple of days there getting blood transfusions and platelet transfusions. I had to get multiple of those. It was very tough on the body and mentally, too.
Balancing treatment and preparing for fatherhood
Managing all of that while preparing for a child was challenging. Every day, I tried to be positive. I would try to find one thing to be grateful for each day.
There were a lot of long nights at the hospital, and you can get into a dark place when you are by yourself with your thoughts and things are not going well. You are losing your hair, your eyebrows are gone, your eyelashes are gone, and your skin looks dead. I was just trying to stay positive each day. I would get out of bed every day and try to walk for miles around in a circle on the unit, or on the treadmill in the hospital wing. I tried to do some workouts. I tried to always eat. I tried to really talk to the nurses and get to know them.
There is no perfect way to handle going through something like this, but I think having a positive mindset is extremely important, especially when your physical body is going through so much. You have to be strong mentally, or it is really easy to give up.
The birth of my son and the timing of my recovery
Being in the delivery room after my transplant
My wife gave birth after they declared me NED this time. It was about two to two and a half weeks after my stem cell transplant that she gave birth. I was able to be in the room for that, which was a phenomenal experience.
Our team of doctors did an amazing job getting all my treatments scheduled. I was very lucky that I did not have to do a third treatment of ICE. If I had, I would not have been able to be in the room for the delivery of our child. It worked out. I got my stem cell transplant, and I had to recover, but I was cleared by the doctors to be in the delivery room and at the hospital. At the end of the day, it was amazing because that was one of the things that was keeping me going throughout all my treatments. I had a picture of our baby from when he was in my wife’s womb, and I had it on the nightstand. I would look at that every night, and it definitely helped get me through everything.
Recovering from a stem cell transplant with my newborn child
Physical and emotional side effects after my transplant
The recovery was tough. There are a lot of side effects I never realized I could go through at a young age. I sometimes have neuropathy in my hands, which causes me to drop things. I was making my wife a bagel a couple of days ago, and I just dropped it and could not explain why. I have dropped iced coffees. I have heard that it is a common side effect that can go away, but early on, it was mostly fatigue. I did not want to get out of bed. Some days, I would just lie in bed, and it hurt to get out of bed.
Sleeping was hard. I could not sleep. I had nightmares and night terrors. I would wake up thinking I was at the hospital because you get woken up every couple of hours for blood work. It was tough. You also cannot see anyone. With a stem cell transplant, you have to isolate yourself because you do not have an immune system. It wipes out every vaccine you have had since you were a child. I was essentially just living within our walls unless I was going to the hospital for checkups. That is tough.
On the newborn part, that keeps you busy. It is one of the greatest feelings ever to be a dad, especially after getting through what I went through. Having my wife’s support throughout all of it is incredible. She was pregnant and my caregiver, which is insane to even think about. It should be the other way around. Unfortunately, these were the cards we were dealt. I had an amazing support system.
Today, I am about 91 days out from my stem cell transplant. My hair is starting to come back in, which is great. I am starting to feel better. But it is something I will have to live with for the rest of my life. I will have to make choices about things I eat, things I put in my body, and take my health a lot more seriously. It does not just go away once you are cancer-free. This is something you live with for the rest of your life.
Tips for recovering after a stem cell transplant
I would say, try to get up each day and do something for your body. It is really easy to get into a mindset where you are just going to rest. Rest is good, do not get me wrong, but you can get into a mindset where you do not get out of bed, and that becomes the norm. I have seen with myself that pushing yourself each day helps, whether it is walking up the stairs a couple of times, walking outside and getting some fresh air, or walking the dog. Just try to get on your feet and get out there. It is tough to just sit in bed and be in pain all the time. My recommendation would be to stay active.
The other thing is to try to find one thing to be grateful for every day. I think that is the most important part: your mindset. I would write down in my notes what I was grateful for each day. That would give me some strength to get out of bed, and from there, I would attack the day. Gratitude is a big part of it.
Isolation, immunity, and my new routines
Living in isolation after my transplant
The biggest challenge for me has been isolation. I do sales for a living, so before my diagnosis, I was hopping on planes and going out to meet customers. Now I am working from home every day, which is phenomenal for spending time with my son and my wife, but I cannot really go out and do the things I used to do. I cannot go to dinners or see people as I used to. I have to be really cognizant of my health and wear a mask whenever I am out and about. These are my new ways of life, at least for the foreseeable future.
You have to stay busy because every day feels like you are living the same day, and that gets taxing after a while.
What isolation means day-to-day
In terms of what isolation means, I actually built a gym in my basement because I will not be able to really be around anyone for a while, so I have been working out there. Isolation is essential until my counts — my blood counts and my system — stabilize. I cannot get vaccines until six months out. Usually, around that point, which will be around May, I should be able to start returning to a new normalcy. When I travel, I will still have to wear a mask, but I will be able to go out more.
For now, I can pick my spots. If I go grocery shopping, I can wear a mask, or if the store is empty, I can keep my distance from people and really make sure I wash my hands and do not touch my face. Truth be told, I do not really have an immune system this early on; it is still developing. If I get anything, what might be a common cold for someone else could be something that lands me in the emergency room. That is the last thing I want to happen at this stage.
On the lighter side, I have a newborn, so I can stay in and help out as much as possible. That is the excuse. It is the newborn and me; we are in the bubble together. The newborn is getting all his vaccines before me, which is pretty insane. My wife loves having a reason to keep visitors away. She has a nice excuse. She has been really happy about that because if that was not the case, I know family would be trying to come over, and it would be a zoo. It is nice to have this time for our family to focus on us and not have to deal with all the chaos that comes with having a newborn.
Survivorship, scanxiety, and giving back
What survivorship means to me
Survivorship for me is about giving back. It has always been my belief that when you get something or are able to get through something in life, you are supposed to give it away. I hope that the experience I had — the pain I went through and being able to come out on the other side — can offer hope and inspiration to someone new who might be going through this and is not sure what to expect. It is a lot to take on mentally when you are told you have cancer. If my message and story can help inspire someone and give them some hope and strength to get through this, then I hope they carry their story and message on to someone else. That is how a fellowship and community are built: people sharing their experience, strength, and hope, and inspiring others that they, too, can get through this.
Without that, it is just a dark place if you do not have folks on the other side sharing their stories and giving you hope. Survivorship is always about giving back. I am active in the Ride for Roswell, which is a cancer bike ride we do every year. That is something I am a part of. This year, they are doing a Light the Night event for lymphoma awareness, and I am going to be the speaker for that event. These are all things I am very excited about. I think it is important to give back when you can, and thankfully, I made it through on the other side, where I am in a position to do that.
Scanxiety and mental health support
There is definitely a lot of anxiety, and I am talking to a therapist about it. I think it is important to take care of your mental health. It is not a weakness to admit that you need to talk to someone and seek help.
I would recommend that anyone going through something like this consider therapy. I would be shocked if someone did not have PTSD or anxiety after hardcore chemo and seeing the impact and effects it has on your body. I am working through the anxiety, but I have a good support system and a lot of loving people in my corner. I think with time that can ease a bit, and I can become more comfortable in public and get my confidence back.
Encouraging other men to seek help
Advice for men on mental health and therapy
Mental health affects everyone, whether you are a man or a woman. It does not just affect you; it affects all the people around you. It is really important to recognize that and get help if you need it. There is no shame in getting help for mental health. I can promise you that if you get help, it improves other aspects of your life: your relationships with your family, your kids, your spouse, and your work relationships.
If you are struggling, get help. It took me a while to get to this point. I was always against seeing a therapist, but after seeing the impact therapy had on people close to me, I was willing and open to give it a shot. I have seen benefits from it so far. It is a good tool to have in your toolkit when it comes to recovery. Making sure you get help, being honest, and being open about what you are going through, and not being afraid to share your experience and encourage others to be open too — that is important.
My message of hope
How to stay hopeful through cancer treatment and recovery
My message of hope would be: do not give up. There are going to be really bad days in treatment and even in recovery, but hold on to the small good things every day. It could be waking up and feeling a little less sore, being able to stomach some food that you could not during treatment, being able to go for a walk, being able to work out a little bit, or being able to enjoy your favorite food again. Try to hold on to the little things people take for granted every day. When you are going through treatment, a lot of that gets taken from you.
It is important to celebrate small wins and not get too far ahead of yourself. It is a day-by-day process. If you take it day by day, celebrate small wins, and make the most out of s** situations when they come along, it puts you in a favorable position to conquer this.
At the end, I do not think there is anything more I need to add. That is my story.

Inspired by James's story?
Share your story, too!
More Hodgkin Lymphoma Stories
Jessica H., Hodgkin’s Lymphoma, Stage 2
Symptom: Recurring red lump on the leg (painful, swollen, hot to touch)
Treatment: Chemotherapy
Riley G., Hodgkin’s Lymphoma, Stage 4
Symptoms: • Severe back pain, night sweats, difficulty breathing after alcohol consumption, low energy, intense itching
Treatment: Chemotherapy (ABVD)
Amanda P., Hodgkin’s Lymphoma, Stage 4
Symptoms: Intense itching (no rash), bruising from scratching, fever, swollen lymph node near the hip, severe fatigue, back pain, pallor
Treatments: Chemotherapy (A+AVD), Neulasta
Brescia D., Hodgkin's Lymphoma
Symptom: Swelling in the side of her neck
Treatment: Chemotherapy: 6 rounds of ABVD