Amanda’s Extraovarian Primary Peritoneal Carcinoma Story
Amanda, a resident of Seattle, Washington, shares her harrowing journey with cancer, which began with her family’s history of the disease. In 1999, her mother’s diagnosis of endometrial uterine cancer marked the start of a series of cancer battles within her family. Despite initial success in treatment, subsequent diagnoses among family members, including her older brother’s colon cancer, prompted concern. Initially hesitant to undergo testing, Amanda eventually faced her own health scare, experiencing symptoms like fatigue and changes in bowel habits.
In 2017, Amanda received a shocking diagnosis of metastatic cancer of an unknown primary source. Despite challenges in pinpointing the primary tumor, Amanda underwent surgery and radiation treatment. However, her journey took a new turn in 2022 when she experienced pelvic pressure and underwent surgery for what was ultimately diagnosed as extraovarian primary peritoneal carcinoma (EOPPC).
Facing uncertainty, Amanda opted for chemotherapy and immunotherapy, navigating side effects and advocating for her preferred treatment options. Today, Amanda is in remission and emphasizes the importance of self-advocacy, finding a supportive medical team, and cherishing life’s moments amidst the challenges of cancer treatment.

- Name: Amanda W.
- 1st Diagnosis (DX):
- Metastatic cancer of an unknown primary source
- 2nd Diagnosis (DX):
- Extraovarian Primary Peritoneal Carcinoma (EOPPC)
- Symptoms:
- Swollen lymph node in groin
- Pressure and pain in pelvis
- Treatment:
- Surgery
- Radiation
- Immunotherapy
- Keytruda
- Chemotherapy
- Carboplatin, taxol, and paxil
Always listen to yourself and push for the things that you feel in your heart you want.
Amanda W.
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Symptoms
Tell us about yourself
My name is Amanda and I live in Seattle, Washington. My cancer journey has been very long. I’m going to have to take you all the way back to 1999, because it didn’t really begin with me. It began with my mom, and in 1999, I was 19 years old, and a freshman in college.

She was diagnosed with stage 2 colon cancer.
I received a phone call from my mom one day and she said, “Mandy, I have cancer.” My heart sank, because back then, cancer still felt like an ultimate death sentence. She was diagnosed with endometrial uterine cancer. She had radiation, was fine, and we went about our merry way thinking that was a one and done thing.
Three years later, my older brother was 26 at the time, and started getting really sick. He was a captain in the Army and was supposed to be in the pinnacle of health and fitness. He lost 30 pounds overnight and started going through a slew of tests. The last one was a colonoscopy on September 2nd. I remember the day clearly. He was diagnosed with stage 2 colon cancer.
We were floored because he was 26. Back then, we thought colon cancer was an old person’s cancer. My mom went to her oncologist and started talking to him about it and he put two and two together. I have a younger brother and an older brother. He said, “You need to get your other two children checked out.” My mom said, “Honey, we need to get you and Nick,” my younger brother, “colonoscopies.” I said, “No, there’s no way I’m going to go get a colonoscopy.” I put it off. I was 22 at the time when she approached me about this, so I put it off for two years, to the point where I started noticing newer symptoms.
What were your initial symptoms?
It was about September of 2004. I had just gone back to school, so I was finishing my college degree. I chopped them up to working full time and going back to school. It was massive fatigue. I wanted to sleep all the time when I came home from school or work. My bowel habits changed. I had this really chalky complexion. It felt like I was not absorbing all the nutrients that my body was taking in.
My gut started to say, okay, I think I need to go in and get this colonoscopy. That led me to make an appointment. It was two days after Christmas in December of 2004. I went in for my colonoscopy. When I came to, I remember my doctor talking to the nurse and saying, “You need to go get her mom and bring her back to my office.” I was like, oh my gosh, how can this be happening? I knew something was wrong.
I didn’t have full blown cancer yet, but I had a very large colon polyp that was weeks away from turning into cancer. There was no way to absolutely tell, but it was within weeks to a few months. I had to have part of my colon in my rectum removed. That’s a whole story in and of itself, because I almost died from that surgery.
Receiving genetic testing
It was because of that we realized we needed to be tested for any kind of genetic abnormality, which led my mom to get tested. Back then, there were insurance laws that led my brother and I to not want to get tested, because if it came back as anything, we could potentially not get health insurance.
My mom was tested and she came back positive for what is called Lynch syndrome, and the rest of the journey unfolds from there. It wasn’t until 2017 that I was genetically tested and tested positive for Lynch syndrome. There are a lot of things that happened before that. One being, after my experience with the colon polyp, a year later my mom was diagnosed with colon cancer. A year after that, my maternal grandfather was diagnosed with colon cancer, and then my cousin was diagnosed with stomach cancer, and unfortunately passed away within 9 months. I did develop a skin cancer, squamous cell.
All of this happened within an 8 or 10 year period. Then we had a little bit of a gap in time.

I was genetically tested and tested positive for Lynch syndrome.
»MORE: Genetic Testing For Cancer
Years later, new symptoms arose
In 2017, I developed a lump in my lymph node in my left groin. It popped out overnight. It was small but concerning. I was coming off of a season of doing triathlons and races. I climbed Mount Whitney, which is the tallest mountain in the lower 48. I was at the epitome of health at that point. My first thought wasn’t, this is potentially cancer. It was, I have some kind of infection. I did go to the doctor and said, “This is really concerning.”
At the time, I had bacterial vaginosis as well. They chalked it up to that. I said, “Well, this is my family’s history. I would be much more comfortable if we could schedule a biopsy.” They said, “We don’t think you need that,” but my gut was like, I want a biopsy. Something was screaming inside of me to get a biopsy, but they put me on antibiotics and it went away.
Six months later, the lump came back with a vengeance and I lost a lot of weight. I went into the same clinic, but saw a different doctor, and I said, “I want to get this biopsied. This is very concerning.” I did have bacterial vaginosis again, but I knew enough about my body to know that something was wrong. She said, “I agree with you.” She was an awesome doctor. I never felt like I had to push for anything with her. If I said I wanted something, she said, “No problem, we’ll do it.”
First Diagnosis
What did biopsy results show?
I went and got this biopsied on St. Patrick’s Day. I was working at a restaurant at the time, and I was heading out the door to go to work when I got a phone call from her. She said, “I got your test results back, and it is cancer.” The blood drained from me. My immediate thought was, it must be lymphoma. Then I just started spiraling.

My final diagnosis was metastatic cancer of an unknown primary, which is very rare.
She continued, “The actual diagnosis is called metastatic cancer of an unknown primary source.” She gave me the cell type and it was the squamous cell. Then I had to undergo a bunch of other testing to figure out where this was coming from because they ruled out lymphoma. They started ruling out everything.
Then she got me into an oncologist at Moores Cancer Institute down in San Diego, because that’s where I was living at the time. They did know there was a secondary tumor, but they could not find a primary tumor. My final diagnosis was metastatic cancer of an unknown primary, which is very rare. That was 2017, and from there, I had surgery to remove it.
How did you process your cancer diagnosis?
I didn’t process that very well. I went into shock and was extremely numb. My whole family lived in Seattle at the time, and I lived in San Diego, so I was alone. People started coming down to help me go to appointments but it was really, really scary.
After talking to the oncologist, there were two main cancers that he thought it could be. One was vulvar cancer and the other was anal cancer. Not that any cancer is glamorous by any means, but these were two cancers where I was like, how am I going to get through this? I knew I could get through other sorts of cancers, but these two specific cancers, because there’s so much stigma attached to them, it all was devastating. Then I was like, you know what? I’m just going to take it one step at a time. I need to collect information.
Describe your experience with your medical care team
From the time of diagnosis to the point of being in surgery was about a month. I was diagnosed on March 17th and then I was in surgery on April 17th. I had colonoscopies, CT scans, PET scans, and a bunch of other procedures to rule out everything. I saw 5 different oncologists. Ultimately, I settled with a gynecological oncologist, who I adore to this day.


We believed it was more than likely some kind of gynecological cancer that was the primary source. I have been incredibly lucky with having an amazing support team. I know that people have horror stories. I feel like I’ve been in the medical world for so long that I have a pretty good gauge around who I can and cannot work with. That’s not to say that everybody I’ve worked with has had the best bedside manner, but my core team has always been phenomenal.
I didn’t get a second opinion because it was such a weird diagnosis and because my whole diagnosis process involved 5 different oncologists, I felt like I was thoroughly being taken care of. There were so many different eyes on my pathology report that I felt well cared for. My oncologist had an incredible reputation, so I felt really lucky. I do highly recommend people get a second opinion if they feel like something in their gut is telling them something’s off.
What was your treatment plant?
The treatment plan was up in the air because this is a rare cancer. Ultimately, there were talks of me doing chemotherapy and radiation, but we settled on surgery and radiation. I was pretty adamant that I did not want to do chemotherapy. I had a very strong opinion about not doing it, primarily because there was no primary tumor and they got all of the cancer out.
I did settle on radiation. I felt like radiation was the lesser of both evils, but after going through radiation, my opinion about it completely changed. I don’t think that there’s a lesser of either one. They’re both horrible and they both come with horrible side effects. At the same time, they save so many lives. It was a hard decision to make because I’m very holistic. When I laid out all of the pieces, it was a no brainer. I did 6 weeks of radiation, 5 days a week, and then surgery.
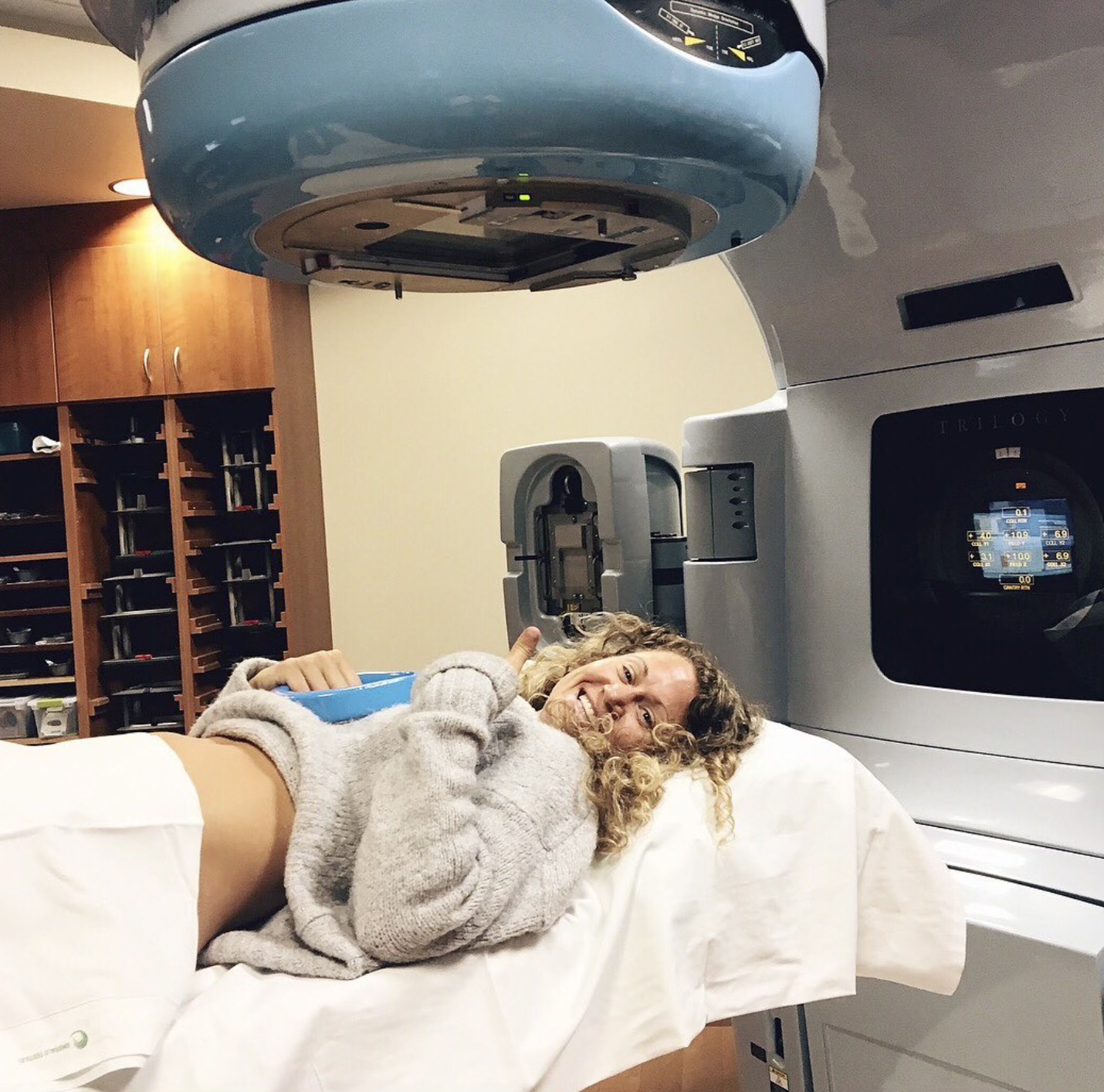
Second Diagnosis
Second cancer symptoms
That brings me to my latest cancer diagnosis. That was in 2017, and a year after I finished radiation, my mom was diagnosed with colon cancer again. Then 6 months later, she was diagnosed with bladder cancer. She’s had 4 cancers 4 times. Then we had a bit of a gap, and in that time, my bonus dad passed away from liver cancer. Then, in August of 2022, I started feeling fullness in my pelvis.
I was really busy at the time. I’m an artist, and I flip furniture for a living, so I was fully engrossed in that. Then I moved into the spot I’m currently in. I had all this stuff going on, plus the grief of losing my stepdad, but I had this dull new pressure in my pelvis. I was keeping tabs on that. It was around my birthday, September 6th, that it started feeling stronger and stronger.
It started to feel like I was being pushed open from the inside of my pelvis. I called my oncologist that I started seeing for maintenance and follow up and said, “I feel like I need to come in and see you. Something feels off.” I went in, saw him, he gave me a physical exam, and he said he did feel something in there. He got me orders for a CT scan.
Receiving surgery to determine the problem
In mid-October, I got a CT scan and there was a grapefruit-sized mass in my pelvis. A good portion of it was cystic, but there was a small portion at the very base that was solid. I just knew it was cancer. It went from sort of painful to excruciatingly painful within 2 weeks. I had a trip to Disneyland with my family in October and it was horribly uncomfortable.


I lost a lot of weight. Right before I went on that trip, I had to go to the ER because I hadn’t had any bowel movements for 5 days. The mass was wrapping around my colon. He got me scheduled for surgery, and at that point I just wanted it out, so I didn’t care. It was like being ripped apart from the inside out and it was growing really fast.
I went in on November 17th and I didn’t know they were going in laparoscopically. There were all these different things that could have potentially happened in this surgery. I went in very blind, not knowing what I was going to wake up to. My doctor, who’s my surgeon and oncologist said, “We’re going to go in laparoscopically but I don’t know what we’re going to find when we get in there. We may have to cut you open. I don’t know if anything is affecting your colon, so there’s a small chance that you could wake up and you could have an ileostomy or colostomy bag.”
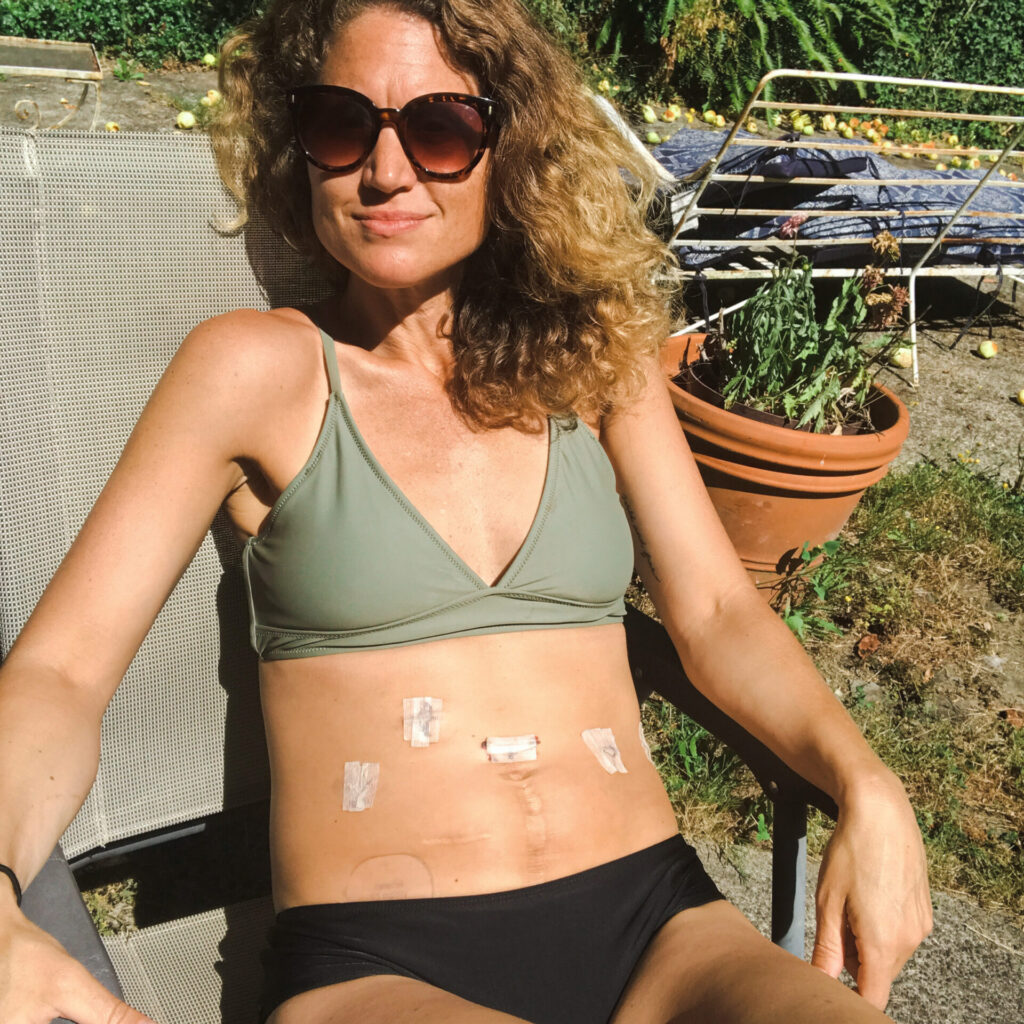
“We’re going to go in laparoscopically but I don’t know what we’re going to find when we get in there.”
Amanda’s surgeon
It was really nerve wracking going into this surgery. My previous colon polyp was right down there too, so I had to have part of my rectum and my colon removed when I was 24. I’m like, this is either colon cancer or endometrial cancer. When I woke up, the first thing I did was reach my hand down to my belly. I felt the tape, but I didn’t feel any bags. I had to have a temporary ileostomy bag when I was 24 because I developed peritonitis from that surgery, and that’s why I almost died. That’s a whole other story, but I knew what to expect. I was like, thank God I don’t have that because I didn’t want to have to go through that again.
What was your second cancer diagnosis?
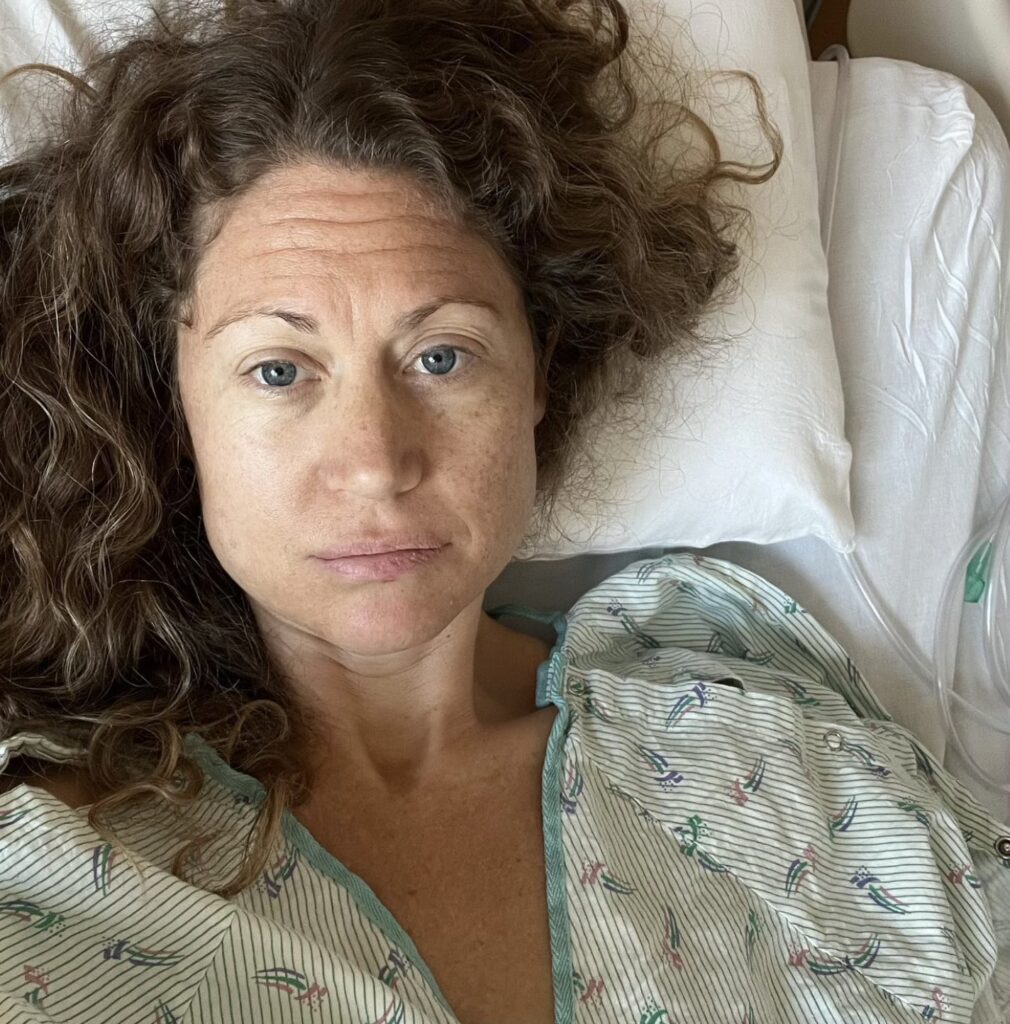
My official diagnosis came back as extra ovarian primary peritoneal carcinoma.
I was kind of in and out, but I do remember every time a nurse came in, I asked, “Is it cancer? What cancer is it?” She said, “Your doctor will be in and talk to you in the morning.” He came in around 6 or 7 a.m. and confirmed that most of it was cystic, but there was a small portion down in the base that was cancerous.
It was the same cell type as before, the squamous cell. I had to wait for pathology reports to come back to confirm all of this, but he did mention in that initial meeting that the next course of treatment would most likely be a mix of chemotherapy and radiation. That was in the back of my mind.
Three weeks later, my brother went with me to get the pathology report back. Initially, I was diagnosed with endometrial carcinoma. Later, after they sent it off to another specialist, my official diagnosis came back as extra ovarian primary peritoneal carcinoma. I think of it as ovarian cancer and peritoneal cancer.
What was your next course of treatment?
When I went to see my oncologist, my biggest concern was, I had really long, beautiful curly hair. I was like, I really don’t want to lose my hair. I know a lot of people are not going to understand this, but I feel very strongly about not wanting to do chemotherapy. He said, “I could put you on one where, most likely, you won’t lose your hair.” I said, okay, I’ll do that.
»MORE: Hair Loss and Regrowth After Chemotherapy
We were originally going to see if we could go the radiation route. It turns out, I couldn’t do radiation because too much of my previous area that was radiated before would be covered, and it was too dangerous. I had to go the chemotherapy route.
My brother and I went back to him in early January of 2023. He presented all of the options for me. One of the options was that I could do a mix of carboplatin and I think doxil and I wouldn’t lose my hair. Then he presented a mix of carboplatin, taxol, and paxil with Keytruda immunotherapy.
There were so many studies coming out showing incredible things were happening with this immunotherapy, but I would lose my hair. He said, “There are studies showing that Keytruda is bringing the recurrence rate down to next to nothing.” It was a no-brainer for me, especially having Lynch syndrome and knowing that I had such a high chance of recurrence rates and a laundry list of cancers that I can get. Two weeks later, I was at my first chemo appointment.
Side Effects
Was this second cancer diagnosis connected to your first diagnosis?

I don’t think this was connected to my first diagnosis when I was 24, but he does think this is the primary tumor to the diagnosis in 2017. My other oncologist was very clear that it’s not an if, it’s a when. The original tumor will pop out at some point. It was a relief when it finally did, because I’ve been walking on eggshells.
July of 2020, I had a scare. I had a pelvic ultrasound done, which was part of my regular screening. The tech was acting really weird and asked me weird questions. I was like, just come out and say you found something. It turned out to be nothing, but that was the last straw, because since I was 24 years old, I’ve been told that I need to have a hysterectomy. I wanted to have kids, and so I didn’t. I said by my 40th birthday, I’ll make the decision.
This was the final straw. I called my oncologist and said, “I don’t want to wait anymore. I’m tired of having scares. I want the hysterectomy.” I had a total hysterectomy in July of 2020 to prevent this from happening. Ironically, I was still diagnosed with extra ovarian primary peritoneal cancer.
Did you have any side effects from chemotherapy?
With chemotherapy, I had no idea what to expect. You can read and read but everybody’s bodies are so different. I went into that first chemotherapy session extremely nervous. I was trying to preserve my hair, so I did cold capping but it didn’t work.
The nurses would give insight into what to expect over the course of the following days. They said, “You probably won’t sleep or you’ll be up at 3 a.m. painting your bathroom.” I slept fine that night, but the next day, I had so much energy. I thought, if this is what it’s like, I’m fine. This is great. I can do this. Then I went to lunch with my family. We were walking down that beach and all of a sudden my legs felt like tree trunks. I said, “Mom, I have to go home. I feel like I can’t walk anymore.”
I went home and laid on the couch and proceeded to fall into the most excruciating pain I’ve ever felt in my life. It was like all my bones were crushing. I had a splitting headache. I did call my doctor, because after three days of feeling this way, I said, if this is how I’m going to feel, I’m not doing this anymore. I cannot do five more of these.
Did anything help with the chemo side effects?
I’m very active on social media. I was putting it out there in my stories, and people kept writing back to me and they’re like, “Are you on Claritin?” I said, “Nobody told me to be on Claritin,” and I did start taking that. It was a night and day difference. Check with your doctor first, but Claritin was the missing piece for me. I had bone pain but it was not as excruciating.
The first chemotherapy is very shocking, but then you start to develop your rhythm. After 5 days, I started feeling better and better. Week two, I felt pretty good. Week three, I felt great. You find your groove.
Asking for help during cancer treatment
Everybody wants to help but you have to tell people exactly what you need, and you can’t be afraid of telling people what you need.

I had so many people asking what I needed, and it was wonderful, but also very hard for me to respond to everybody. I thought, we do wedding registries and birth registries. I’m putting together a friggin cancer registry, because why not? I don’t have kids, I’m not married, but if people want to help, I’m going to lay out exactly what I need. I put together a document, I put it on my website, and I shared it on all my socials. Direct links to an Amazon wish list and my Venmo were on there.
I had a friend who started a meal train for me. I put my dietary restrictions and everything I needed. Everybody wants to help but you have to tell people exactly what you need, and you can’t be afraid of telling people what you need. Some other things I really loved were heating pads. I got inundated with pajama sets, socks, and slippers, which was really nice.
A lot of people lose their sense of taste and I still had mine for the most part. I wanted fruit all the time and popsicles. I ate so much watermelon. I did Liquid I.V.s and hydration stuff. I invested in new water bottles. I used to hate ice cold water, and now I live for it. A lot of things change physically in your body. I wanted ice cold things all the time.
Immunotherapy
Do you have any side effects from Keytruda?
I get pretty bad rashes on my face that look like acne. I get it all over my face and my chest. Every immunotherapy is different. I always say it’s like Russian roulette because I never know what I’m going to get afterwards. Over the summer, my whole body, head to toe was covered in this horrible rash after one session. That never happened again.
It’s much easier than chemotherapy. I’m growing my hair back now and there’s not those kinds of side effects. One of the ways that it really affects me is fatigue and my breathing. It can affect your lungs. I have to take a lot more deep, longer breaths. I get winded faster.
I’m currently seeing a neurologist because there’s some things going on neurologically right now. He doesn’t know that it’s necessarily from Keytruda, but we’re crossing all our t’s and dotting our i’s right now. I will say that it’s chemo brain.
One of the major side effects is it affects your thyroid. I already had Hashimoto’s so it is really affecting my thyroid, which could be contributing to a lot of fatigue. We’re constantly having to adjust my thyroid medication which is a bummer because there’s so many side effects that come with low thyroid that are hard. It’s also a wonderful alternative for people and it’s helping. It’s giving so many people additional years when they normally wouldn’t have them.
»MORE: Keytruda Side Effects
Describe the process of receiving Keytruda
You go in and it’s a 4-hour day because I have to get labs. I meet with my doctor, and then the actual treatment itself is only 30 minutes. It’s way different than chemotherapy, which was like a full day at the hospital.

I get it every 3 weeks and. I have a port here. I named her Natalie Portman. I do pretty much everything from my port. Occasionally, if I’m just doing a blood draw, I’ll do it from my arm. If you’re on the fence about whether or not to get a port, it’s not the prettiest thing, but it is such a life saver. The poke here is so much better than the poke in your arms. I have rolling veins and I have a hard time getting access through my veins, so this has been a lifesaver.
They go through my port and it’s pretty easy. You’re usually in the chair for about an hour, because sometimes the pharmacy takes a while to get you the medication. I drive myself and I get them in the mornings, and then I come home.
It gives me a bit of a stomach ache. I want to stay inside and be close to the bathroom. Other times, I’ll go out to my workshop and work. I don’t make a lot of plans with people after treatment. Every session is a little bit different. I just gauge it off of how I feel.
How did you get the generic version of Keytruda?
I have therapy every 3 weeks, so I have one more year of Keytruda. The social worker in the hospital ended up going straight to the company, and they gave me the treatment. It’s income based. I wasn’t working very much and I’m still not working a tremendous amount.
People don’t understand that there are so many tools you can access through your hospital social worker. People think I can’t get this, so I’m just out of luck. Talk to your social worker at your hospital. There’s usually always something that can be done, or at least they can try to do something. My social worker went directly to the company that makes [Keytruda], and I get it now.
Reflections
Reaching cancer remission
I am in full remission now. I was supposed to do 6 rounds of Keytruda, the generic version, with my chemotherapy, but my insurance kept denying it. I only did 2 rounds of it with chemotherapy. I’m doing 2 additional years of immunotherapy now, as much as my body can tolerate. I had my first scan right after I finished my 6 rounds of chemotherapy and everything looked great.
I had a couple scans because I thought I was feeling similar pressure, but it’s post-surgical changes and not abnormalities. All my organs settle differently now. If I am not having regular bowel movements, it’ll start to feel like pressure in there. I have to be really on top of my digestive track. Everything has been really good so far. I seem to be tolerating immunotherapy pretty well.
»MORE: Learn More About Cancer Remission
Do you have any advice for someone on a journey with cancer?
Always listen to yourself and push for the things that you feel in your heart you want.
Make sure that your team really listens to you because they’re your team for the long haul. Just because you are going through cancer doesn’t mean that once you go through treatment and if you go into remission, then it’s done. You’re with them for the long haul. You want to be very comfortable with them.
Always listen to yourself and push for the things that you feel in your heart you want.
My team knows that I like to do a mix of holistic and Western medicine. I’m grateful for both. One of my oncologists said the most amazing things to me. He said, “There’s great things about Western medicine and there’s great things about holistic medicine. They work symbiotically together.” I loved that he said that because I felt heard. Find somebody that makes you feel heard and try to live your life. It’s the scariest thing you’ll probably ever go through, but you have to keep finding life in the little moments throughout your day.
More Ovarian Cancer Stories
Alicia N., Ovarian Cancer, Stage 3C; Uterine Cancer, Stage 1
Symptoms: No menstrual cycle for one year followed by almost two years of daily bleeding, large blood clots, high blood pressure, random cough, bloating, lower back pain
Treatments: Surgery (total hysterectomy), chemotherapy, radiation therapy (planned)
…
Melanie E., High-Grade Serous Ovarian Cancer, Stage 4 (Metastatic), BRCA1+
Symptoms: Cough, stabbing pain in right rib area, bloating, frequent urination, moodiness, fatigue
Treatments: Surgery (debulking surgery including full hysterectomy), chemotherapy, immunotherapy
…
Amber C., High-Grade Serous Ovarian Cancer, Stage 4B
Symptoms: bowel irregularities (urgency, alternating constipation & diarrhea), night sweats, unintended weight loss, irregular periods, fatigue, pain while sitting or going to the bathroom, blood in stool
Treatments: Surgeries (debulking surgery, radical hysterectomy, oophorectomy, ileostomy placement, preventive double mastectomy with breast reconstruction), chemotherapy, targeted therapy (PARP inhibitor)
…
Courtney H., High-Grade Serous Ovarian Cancer, Stage 3C, BRCA1+
Symptoms: Noticeable body changes, fatigue and frequent napping, random abdominal pain, severe constipation, loss of appetite, weight loss
Treatments: Chemotherapy (carboplatin & paclitaxel), PARP inhibitor (olaparib), surgery (interval debulking, thoracoscopic thymectomy)
…
Gigi D., High-Grade Serous Carcinoma, Stage 1A, HER2+, PR+, ER-
Symptoms: Hiccup-like sensations behind the sternum, gastrointestinal issues, spotting
Treatment: Chemotherapy (carboplatin & paclitaxel)
…








Leave a Reply