The White Ribbon Project Stories
Chris Draft:
The Team Player
Story 3 of The White Ribbon Project Stories
Chris Draft left if all out on the field when he was playing for the NFL.
“I’ve had asthma attacks. I was in the hospital about six, seven times while I was playing in the league.”
Different teams, same mantra: Don’t take anything or anyone for granted, not while he played, but especially off the field.
He cherished every moment with the love of his life, Keasha Rutledge.

“Intelligent, strong, fierce woman, that just lit up a room when she walked into it,” describes Chris. “She actually graduated a year early from high school, attended Clemson University, graduated with a degree in electrical engineering.”
Keasha was passionate about her education, dance, and also about her health. While training for a 10k race, Chris says Keasha started to feel shortness of breath.
Keasha would get antibiotics and then undergo a chest X-ray before the couple was devastated by the news.
“That was lung cancer. Went to a biopsy right out two days after Christmas,” Chris says. “We found out the most important fact about lung cancer at that moment, and that is… anyone with lungs can get lung cancer now.”
Chris admits he wouldn’t have believed someone with no smoking history and so young could get lung cancer.

“37 years old and amazing shape. Never smoked. If she is not right in front of me and somebody told me that I would probably be like, ‘Oh, that’s kind of crazy. What are you saying to me?’ Because all of the messaging historically was just about the connection with smoking.”
11 months later, Chris and Keasha got married. Instead of gifts, they asked people to support their vision of building awareness that anyone with lungs can get lung cancer.




“She came to me and she said, ‘What if we don’t get presents? What if we ask our family and friends just to donate to the foundation?’ And literally, that’s the point where we started our Team Draft initiative that is changing the face of lung cancer,” Chris says.
So our wedding day was two commitments, you know, one to the lung cancer community and the other one to each other.
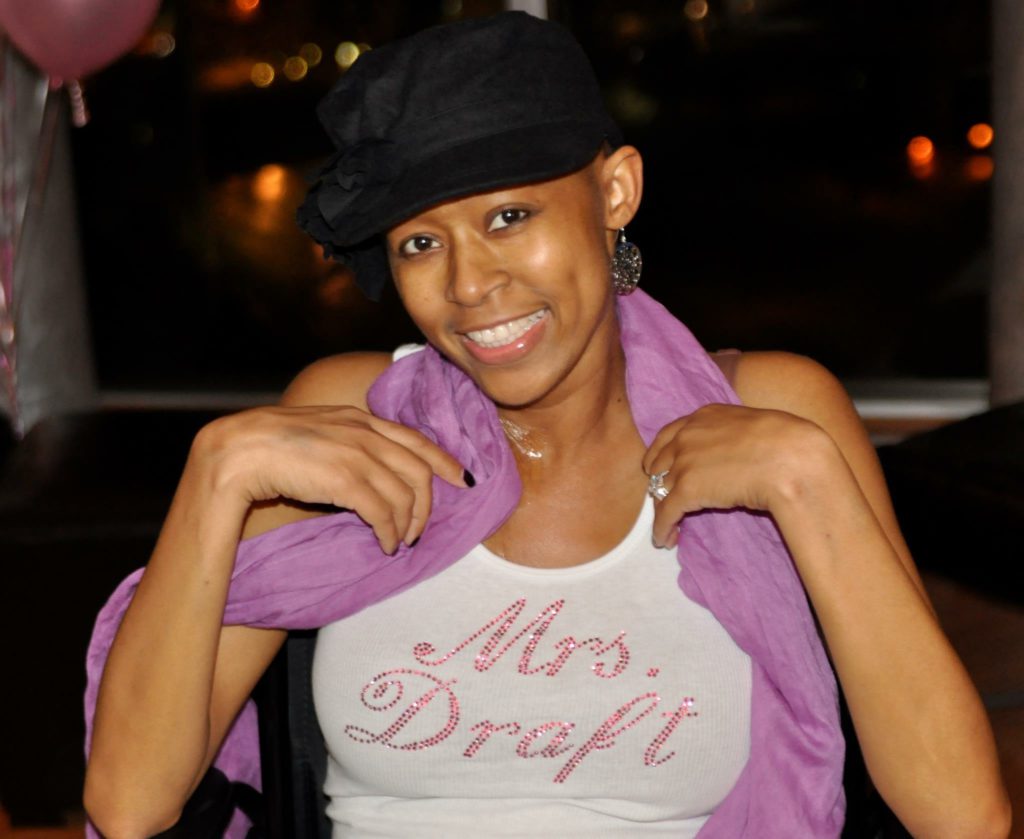
One month later, Keasha passed away. From that time on, Chris has dedicated his time and energy to the mission of spreading a message he believes can help save countless lives.
Anyone with lungs can get lung cancer.
And it has been a huge goal in lung cancer, which is the deadliest cancer in the U.S., killing the most men and women in the country each year, according to the Centers for Disease Control.
A decade later, Chris reflects on his tireless lung cancer advocacy. For him, the definition of winning is crystal clear in this space:
Shifting away the focus from the narrative of the smoking stigma in lung cancer to growing more advocacy and love within the lung cancer community, itself.
“The honesty to just acknowledge that getting people to stop smoking was not anything done out of malice to create some type of stigma. But it was about actually loving people enough to say, we need to get them to stop smoking.”
Beyond that, Chris hopes to refocus lung cancer awareness away from the sole focus of smoking histories to survivorship, and most importantly, to lead all of these efforts with love.
“It starts with caring about the people because if we want to educate, then the lung cancer community has to be bigger than just the people that have lung cancer so that someone can know that anyone can get it before they actually get it right, so that they can support research before it actually happens to them,” he says.
I’m saying all that matters is if we love our people, then the answers will be simple. Stop trying to complicate it, and that’s where The White Ribbon Project starts.

The White Ribbon Project is a grassroots campaign started by Heidi Nafman-Onda, a lung cancer patient advocate, and her husband, Pierre Onda, a former primary care physician.
They, along with so many others, felt a lack of support and an unwillingness to represent their lung cancer stories, so they began to build actual wooden white ribbons and sending them to anyone impacted by lung cancer to understand:
This ribbon is for you. For all of us.




“We’re going to walk with you. We’re going to make sure we get people around you to keep supporting you because we know that cancer is not just a physical thing, but it’s a mental and emotional thing,” Chris shares.
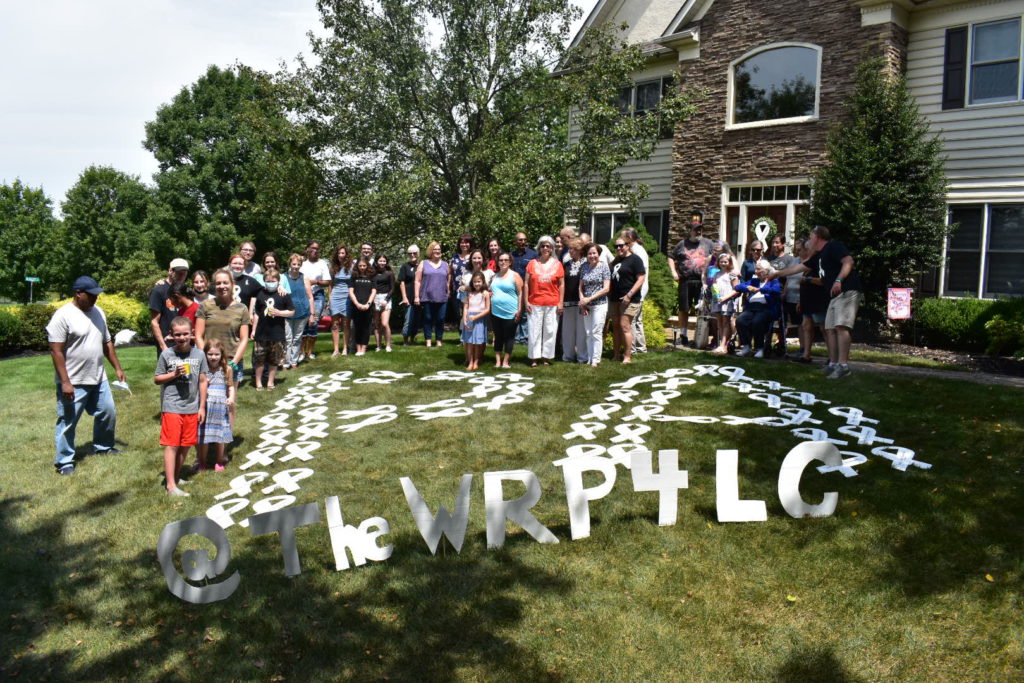
“That’s why even with these ribbons, as we’re giving them out all over the country, we’re challenging people to tell their particular story about what’s going on so they can help somebody that’s in a similar situation. It’s not just to tell your story, just to tell it, but to relate to people so that they can see themselves within that disease.”
When Chris looks at this work, he’s driven by a greater purpose. It starts with the lung cancer community but embraces so much more, including partnerships across other health communities who are also fighting for the same thing: A better future.
“We are touching more than just the lung cancer community to make sure that there’s access for early detection, for screening. Research is going to biomarker testing that’s going towards targeted therapy. That’s the future of cancer care. That’s not just about lung cancer. So as we make it more people more aware of biomarker testing that goes across all cancers, that’s an education that is critical research.”
This former pro football player says his new team, The White Ribbon Project, has had an amazing season this last year. With more ribbon builds and support all across the country and the world.
This former pro football player says his new team, The White Ribbon Project, has had an amazing season this last year. With more ribbon builds and support all across the country and the world.
But it’s a new season, and there’s a lot more work ahead.
“So what does success look like? It looks like all of the cancer centers realizing that everyone who walks in there, it matters. We want them to all get ribbons. But really, the ribbon is just a reflection of saying that you matter.
“We recognize the trauma of this diagnosis. We’re going to stand with you. We recognize that you probably don’t know anything about cancer. So we’re going to help you work through all these words and all this trauma of just being overwhelmed by a diagnosis.”
Keasha may not be here, but her fight and what she stood for is very much alive. That love for others has lived on through Chris for these past 10 years.




And now, also through The White Ribbon Project.
This ribbon says you are not alone and you’ve got people fighting for you. We are out here together. We’re on the same team.
→Back to The White Ribbon Project Stories





Inspired by Chris's story?
Share your story, too!
More non-small cell lung cancer (NSCLC) stories
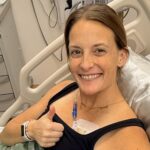
Michelle W., Non-Small Cell Lung Cancer, EGFR+, Stage 2B
Symptoms: None; discovered by chance during a check-up for persistent head and neck pain
Treatments: Surgery (lung resection), chemotherapy (upcoming), targeted therapy (upcoming)
Kelsey D., Non-Small Cell Lung Cancer, EGFR+, ALK+, Stage 4 (Metastatic)
Symptoms: Severe back pain, falling due to collapsed spinal vertebrae
Treatments: Radiation therapy, targeted therapy (tyrosine kinase inhibitor, osimertinib), surgery (spinal fusion surgery), chemotherapy (through a clinical trial)
Megan F., Non-Small Cell Lung Cancer, ALK+, Stage 4 (Metastatic)
Symptoms: Chest pain, anxiety, shortness of breath, arm pain and swelling, back pain
Treatment: Targeted therapy (lorlatinib)
Roxanne C., Non-Small Cell Lung Cancer (NSCLC), Stage 3
Symptoms: None; incidental finding
Treatments: Surgery (lobectomy), chemotherapy (cisplatin), radiation therapy, targeted therapy (tyrosine kinase inhibitor/TKI)
Natalie B., Non-Small Cell Lung Cancer, Stage 4 (Metastatic)
Symptoms: Extreme fatigue, severe cough
Treatments: Chemotherapy, immunotherapy, clinical trials, radiation therapy, surgery (double lung transplant)