Keith’s Stage 4 Colorectal Cancer Story
Shortly after gallbladder removal, Keith developed what felt like gallbladder pain. His wife encouraged him to go to the ER where he received a CT scan that revealed a mass in his colon. After removing the mass and some lymph nodes, a biopsy showed Keith had stage 4 colorectal cancer.
As a husband and a father of two boys, Keith discusses the impact his diagnosis has had on his outlook and life and how he stopped working to prioritize time spent with his sons.
Now on his third line of treatment, Keith discusses cancer support groups, chemotherapy, treatment side effects, mental health, how he is considering a double lung transplant, the importance of being a patient advocate, and his advice for others on their own cancer journeys.

Don’t give up hope, number one. Absolutely educate yourself on your disease and be an advocate for yourself along with your care team.
Keith H.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Colorectal Cancer Symptoms
- Diagnosis & Treatment
- Mental Health
- Metastasis
- How long after your diagnosis did you learn your cancer metastasized?
- How did you react to your cancer recurrence?
- What treatment did you opt for with your recurrence?
- Not knowing where the recurrence was at first, was chemotherapy the right choice?
- What chemo were you on post-recurrence?
- Did you experience side effects on this chemo?
- Staying on a curative path
- What cancer treatment are you on currently?
- How long will you be on your current treatment?
- Reflections
Colorectal Cancer Symptoms
Tell us about yourself
I’m Keith. I’m 43 years old. My hobby is that I love to be outside kayaking, hiking, and walking. I’m a Corvette enthusiast who’s working on my car and hanging out with my dogs. Those are usually the 2 that hang out with me while my kids are at school and one might poke his head in. He’s a very large Great Dane. My wife, kids, and I like to travel. We like to do a lot of international travel and domestic as well.



When did your symptoms first occur?
Early in the year 2021, I had my gallbladder removed. Then in May, I started to have abdominal pain again, very similar to when I had gallbladder issues.
I was coaching Little League baseball the night of May 4th, 2021. As the night progressed, the abdominal pain continued to get a little worse, so much so that my wife forced me to the hospital in the middle of the night.

Getting emergency surgery
I went to the emergency room, and they did a quick CT scan and found a mass in my colon. They did a couple of other tests like blood work and stuff, and they said that they were going to be prepping me for emergency surgery because they wanted to get that mass out.
As they did more digging and research, they also found several lymph nodes that were impacted as well as 4 lesions on my liver at that time. So that’s a whirlwind of how we got started.
I went through that emergency surgery that night and was in the hospital for about 11 days. A couple of days after my surgery, I became septic so I had a lot of issues health-wise. We weren’t sure how that was going to play out, but I was actually able to make it out of the hospital the day before my wedding anniversary, which was nice. I started chemo shortly thereafter.
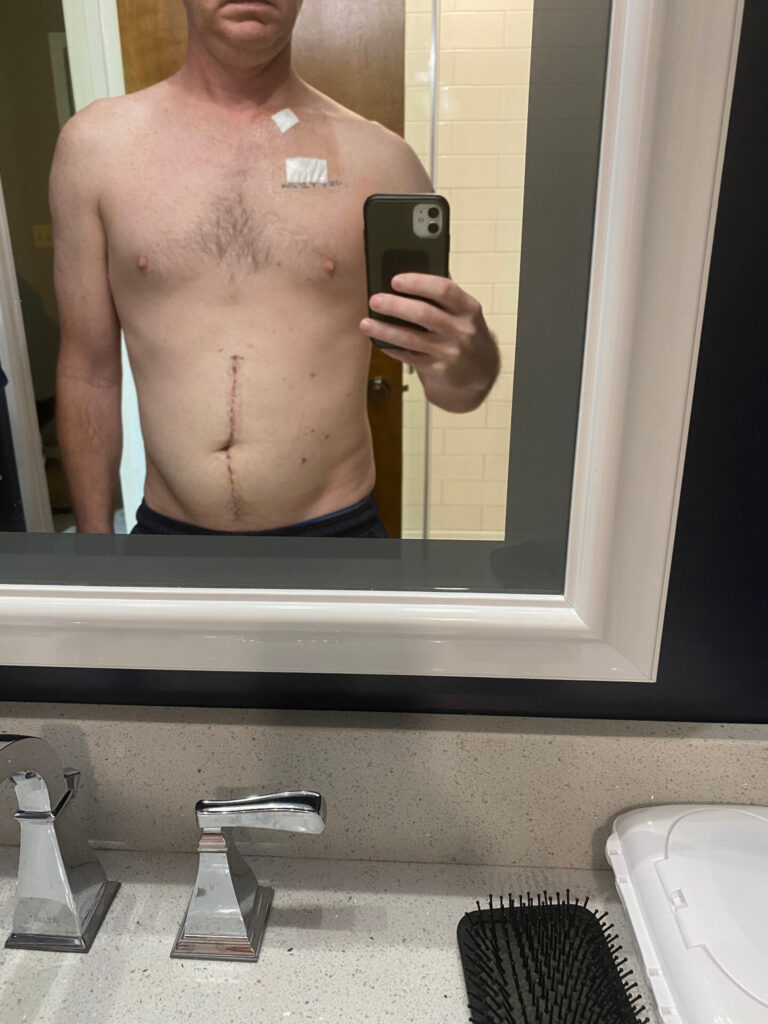
I went to the emergency room, and they did a quick CT scan and found a mass in my colon.
Did you have other symptoms besides abdominal pain?
No, nothing. Even what would have been 6 months before that, I did a triathlon. No issues. I’m not necessarily saying I’m the most healthy person in the world, but I definitely didn’t consider myself unhealthy by any stretch of the imagination.



What did doctors say about your minimal symptoms?
I was told that 41 was very young to be diagnosed with this. They mentioned that they’re seeing more and more of this in younger patients being diagnosed very late stage. Some of the traditional symptoms are rectal bleeding and abdominal discomfort. But for me, I really didn’t have any of that, other than the gallbladder pain that came back.
I thought it was strange because you shouldn’t have pain in an organ that was removed. I thought initially it was maybe some type of surgery complication that turned out to not be a surgery complication at all. It was a whole other issue.
I was told that 41 was very young to be diagnosed with this. They mentioned that they’re seeing more and more of this in younger patients being diagnosed very late stage.
Diagnosis & Treatment
What was your official diagnosis?
I was diagnosed with stage 4 colorectal cancer.
How did you react to your cancer diagnosis?
It was tough. I went to the hospital during COVID times, so nobody else could come with me. I went by myself. I was in the emergency room by myself and had to make a call to my wife that they found a mass. Even at that point, I still really didn’t comprehend or grasp what the situation was. I was thinking, okay, they found something, they got to get it out and then I can go home and move on with life. That wasn’t the case.
It was very shocking initially and I was almost numb. It wasn’t until after the surgery when I started to recover in the hospital that my situation and the diagnosis became real.
The more doctors that I spoke to while I was in the hospital didn’t necessarily paint a real great picture of the survivability, how long I would be around, and all those things. Luckily, I have a great oncologist I met several weeks after all that, which helped put things into perspective a little bit, and while obviously still serious, there’s at least hope.



I still really didn’t comprehend or grasp what the situation was. I was thinking, okay, they found something, they got to get it out and then I can go home and move on with life. That wasn’t the case.
What cancer treatment options were you given?
After surgery recovery, I met with my oncologist about 4 weeks after my initial diagnosis and surgery. We walked through traditional first-line chemotherapy FOLFOX, which is a pretty aggressive first-line treatment and pretty standard care for most of these patients. We did add Avastin into the mix as well to hit it harder, which is probably the best way to describe it.

We talked through side effects and what to expect over these 6 months. The intent was curative intent and to get me to a position where I could be surgical in regards to the liver situation.
Undergoing liver surgery and chemo
We went through 4 months of FOLFOX before I was able to have my liver surgery. They did a liver resection in October of 2021 and took out about 30% of my liver. The good news is most of the lesions that were in the liver were necrotic. Chemotherapy, knock on wood, had done its job, and then I recovered from that surgery.
They did ask me to complete 4 additional rounds of clean-up chemo just to make sure there wasn’t anything lingering out there that didn’t show up on scans. I left the hospital in October extremely excited. You get this diagnosis 4 months before and it’s a pretty dark picture, and to be told that we got it all? In my mind, I beat it and we’re moving on with life. We can go back to normal.
About 2 months after that, a follow-up CT scan showed numerous spots in my lungs. It had hid for a little while and then metastasized further into the lungs which we’re still working on treating today.
About 2 months after that, a follow-up CT scan showed numerous spots in my lungs. It had hid for a little while and then metastasized further into the lungs which we’re still working on treating today.
Describe your side effects from chemotherapy



Of all the chemo that I’ve been on, that first-line treatment was pretty rough. FOLFOX is not for the faint of heart. I had a lot of fatigue and nausea. At one point, I did have a blood clot that they deemed Avastin probably caused. That was a little scary. I had a blood clot that started in my leg and moved into my lungs. We were able to work through that and get that resolved.
Mental Health
The physical and mental toll of cancer

I did seek out some professional help from a therapist’s standpoint, and that helped me tremendously.
I looked at it as 2 things. There’s the physical piece – there’s a lot of medications and vitamin supplements and things like that I was taking to help. But I think the first year of this was more challenging on the mental side if I’m being honest. It was pretty dark for a while because the first thing most people do is grab their cell phone and computer and start searching for your disease and they want to learn more about it.
The prognosis for stage 4 colon cancer patients is not really great. I’ve got 2 young boys and my wife, we have a great family. To think about losing all that in a very short window is very humbling. I went through a pretty dark depression phase where I lost hope. This was before treatment really started and things started to actually show some progress.
»MORE: Cancer and Mental Health
I did seek out some professional help from a therapist’s standpoint, and that helped me tremendously. Not only to be able to take the feelings that I’m having at different points throughout the day or the week or whatever and work through and process those but to get me centered and present instead of sheltering away.
Breaking the stigma of men expressing their emotions
I think that the traditional model of men don’t cry, keep your feelings in, walk it off, and rub some dirt on it is just culture. My wife and I had a lot of conversations about depression and the diagnosis. It’s great to be able to talk to friends and family, but there’s a note that a professional can bring to those conversations that friends and family can’t.



Friends and family will tell you, “You got this, you’re going to be okay, we’re going to get through all those things,” and it’s all with good intentions. But the professional side will actually take you through how to deal with the dark stuff, how to work through those feelings, how to deal with anxiety, and how to deal with depression so you can actually enjoy life instead of just living secluded and isolated.
I did find a couple of groups shortly after my diagnosis that really helped me with peer-to-peer, patient-to-patient, sharing stories, hope, avoiding isolation, and being able to talk to people who truly understood what I was going through.
Talking to children about a cancer diagnosis
Honestly, as a father, that was the hardest conversation I’ve ever had. My wife and I talked a lot about this before and what approach we wanted to take. At the time, 2.5 years ago, they would have been 9 and 11. You think 9 and 11-year-olds are pretty young, but kids are smart, especially with technology at their fingertips. They’re able to find the answers if you don’t provide them, so we made the decision that we were going to be age-appropriate, open, and honest with my diagnosis, my condition, and how life is going to look for a while.
»MORE: How to Talk to Kids About Cancer
I look back on that and I’m really glad we made that decision because I’ve met other folks that are going through similar things that chose a different option. Every family is different and everybody’s decision on how they include their family in these conversations is something very personal. But I’ve also seen a lot of family and friends be torn apart simply because they felt things were hidden from them.
We made the decision that we were going to be age-appropriate, open, and honest with my diagnosis, my condition, and how life is going to look for a while.

I wanted that to be the voice, I wanted them to feel like they’re a part of this story and what we’re going through, and not dismissed. Even 2.5 years into this, I still double down and think that was the right decision for us.
Having a support system
As for my parents and in-laws, we needed a lot of help right in the beginning. This was right at the beginning of summer break when all this happened. My kids are extremely active in sports and activities. Being out of the mix for a while, recovering from surgery, we needed a lot of help shuttling kids here and there and just dealing with life. It doesn’t stop just because somebody gets sick.
We were able to have a lot of conversations and tough conversations, but at the same time, as family does, there’s a lot of hope, positivity, and support that comes with those conversations.

Metastasis
Blood work is pretty traditional and then we also used ctDNA testing to monitor residual disease and that’s actually what gave us the smoke alarm…It posted positive.
How long after your diagnosis did you learn your cancer metastasized?

About 2 months. It would have been January or February 2022 till March or April that I didn’t have residual disease and nothing showed up on the scans. Then we started using a couple of different tools to monitor my disease. Blood work is pretty traditional and then we also used ctDNA testing to monitor residual disease and that’s actually what gave us the smoke alarm. It was a test called Signatera, which is a molecular test for ctDNA. It posted positive.
How did you react to your cancer recurrence?
It sparked a flurry of emotions and feelings that it’s back. Because of that positive test, my medical team ordered scans and so forth. At first, nothing showed up, so we were at this weird place where we knew something was there. We know something’s brewing, but we just can’t see it and we don’t know where it is.

What treatment did you opt for with your recurrence?
I’m really lucky in regard to the medical team that I have. My oncologist and I walked through different options. We could do nothing and wait to see what pops up and deal with it then. Or, what is not very common, is my oncologist actually offered me to go ahead and start back on treatment again knowing that something’s there, it’s going to show up, we just don’t know when. While chemotherapy is not fun, we opted to go ahead and start treatment to be as aggressive as we possibly could. About a month after that, they did a follow-up CT and then found 14 spots on both sides of my lungs.


Not knowing where the recurrence was at first, was chemotherapy the right choice?
I think if anything, it bought me time to process and plan with my team what approach we wanted to take. The treatment that I started then would have been the treatment that I would have started if we waited regardless. I know there’s no real way of knowing, but in my heart, I believe it probably saved it from popping up in other places as well. While 14 spots in your lungs are not great, it could have been worse. I think that some of those tools that we’ve used put us in a position to get ahead of it to try to treat it the best we could.

What chemo were you on post-recurrence?
I know there’s no real way of knowing, but in my heart, I believe it probably saved it from popping up in other places as well.
My second line treatment was called XELIRI, which is Xeloda Irinotecan, and then we kept Avastin in the mix as well. I was on that cocktail for about a year and a half.
»MORE: Chemotherapy FAQs & Patient Stories


Did you experience side effects on this chemo?
There were side effects, so still some fatigue and some nausea, but the ability to bounce back was so much faster. When I was on my first-line treatment with Folfox, after that infusion, I would be out of commission for 4 or 5 days in a row and miserable. The worst flu possible is the best way to describe it.

Then when I moved to the second-line treatment, the day after infusion was pretty rough. Then you started to come out of it pretty quickly and that cycle was every 3 weeks. I actually got an extra week of good feeling into that mix too. While again, no chemo is great, it definitely was good from a quality-of-life perspective.
Staying on a curative path
We had that tougher conversation around curative intent versus palliative care, and I’m still on a curative path. I’m not ready to succumb to this is going to be my life forever. I know that seems kind of silly at times, but I think for me mentally, I need to know that curative is still a path.

I’ve also learned I have to accept stability as positive.
Hearing that was obviously frustrating, it was discouraging. But I feel like we were in the right place to get started when we did. As I said, that cocktail worked for about a year and a half.
What we started to see, and this was just a couple of months ago was that some of those numbers like my Signatera test started to increase, but my scans still showed stability. Again, maybe I’m an oddball, but we’re in this weird situation where we know the chemo that I’m on wasn’t reducing anymore, but it was keeping things stable. I’ve also learned I have to accept stability as positive.
But we had that conversation around if this drug is no longer shrinking but is holding it stable, is it best to stay on this until it stops working altogether or do we want to go ahead and fast forward a little bit and jump on third-line treatment? The path that we’ve always taken is the most aggressive path and the best probable outcome. We made the decision to go ahead and jump ship and start third-line treatment, which started about a month and a half ago.
What cancer treatment are you on currently?
The third line for me is Vectibix, which is an EGFR inhibitor along with Irinotecan. So one of the old drugs and one of the new drugs and that’s where this lovely rash comes from, is from the Vectibix.
How long will you be on your current treatment?
The good news is that I have found options post this line of treatment. Exiting standard of care, there are a couple of clinical trials that I’ve already looked into and tentatively been approved for.

Until it stops working. I love being the oddball. All the spots in my lungs are very small and they’re all under a centimeter. So for me to get into any clinical trials, I don’t qualify because they’re not big enough to biopsy. I’m in that weird situation of, you almost want it to grow to be able to qualify for trials and things like that. But mentally, I just can’t accept that. I’m just going to continue to beat it down until I can’t beat it down anymore, so it’s indefinite right now.
The good news is that I have found options post this line of treatment. Exiting standard of care, there are a couple of clinical trials that I’ve already looked into and tentatively been approved for. It’s a pretty aggressive opportunity that’s being tested in an NCI center close to me, it’s a double lung transplant for metastatic cancer patients. That tumor board has already approved me, but I have to exhaust the traditional standard of care, which is the current treatment that I’m on now.
Reflections
There are plenty more options out there as long as you’re willing to do the research and find them and go wherever it takes to get whatever that treatment may be.
The importance of being a patient advocate
I don’t want to take anything away from my team because they are great, but at the same time, there’s a realization that you’re not their only patient. They’re not going to invest 40 hours a week looking into different options for you.

I’ve learned a lot through a couple of advocacy groups that I’m a part of that have really helped me understand the value of second opinions. For me, second, third, fourth, fifth, sixth, and seventh opinions. I’ve traveled quite a bit to get a better understanding of options that are out there and things that are at different cancer centers I can’t get locally. That has helped me open up some doors and continue to build that hope strategy around, there’s something else after this instead of just saying, this is the last standard of care line. This is it.
There are plenty more options out there as long as you’re willing to do the research and find them and go wherever it takes to get whatever that treatment may be.
Doing your own research to understand your options
I think a big misunderstanding, and it is not the fault of your local oncologists and teams, I think it’s just how the systems are built. You have to be a component of your care and you have to be an advocate of your care. That also comes with education. I had this misunderstanding that I would just go to my oncologist and they would take care of everything and they would prescribe, “Here’s what you need to do to get rid of X, Y, and Z,” and then things would be great.
I can’t stress enough, exhaust your options in regard to opinions. There are never too many opinions and too many places to visit to get ideas.

There are limitations to every cancer center that’s out there. Some specialize in the cancer you have and some don’t. For me, knowing that I’m not going to get a list of trials that are across the United States for me to look into. They provide some that they’re familiar with, but ultimately, a lot of that research lies on the patient along with opinions. I can’t stress enough, exhaust your options in regard to opinions. There are never too many opinions and too many places to visit to get ideas.
How often are your scans?
Because I’m still on active treatment, I see my local team every 2 weeks and we complete scans every 3 months. My next scan will probably be at the end of September. That’ll be the first true telltale sign of how this new line is actually working. My hope is it can get me to a point where surgery would be an option from a lung standpoint, but it’s got to do some good work.



I will say that the positive is that, I just had my third, but after 2 rounds of this, one of the tumor markers in my blood is the second lowest it’s ever been. I’m hoping that correlates in September to good news on a scan, but we’ll see when we get there.
Do you experience scanxiety?

Let yourself be surprised when there’s good news and actually enjoy that.
It was a lot worse in the beginning than it is now, but don’t get me wrong, there’s still scanxiety. I think My Chart is a blessing and a curse at times because you have access to those scans as soon as they’re available. Sometimes I see them before my oncologist. When it’s a good scan, that’s great, because then you can high 5 and move on about the day. It’s when it’s not that the panic sets in – do I need to call, when are they going to see it, what’s our next step?
»MORE: Coping With Scanxiety: Advice From Cancer Patients
How I’ve learned to deal with it is you just have to accept it. That sounds really weird, but you have to accept the situation you’re in. You’re going to get good news and you’re going to get bad news, and more than likely, you’re going to get bad news more than good news. With that mindset, you’re not expecting to go in and everything’s going to be great and the scans are going to be clear.
Don’t set yourself up for something that’s not realistic. It helps a ton. Let yourself be surprised when there’s good news and actually enjoy that. When it’s not, learning how to process that, going back to see a professional that can help with tools and tips and tricks to work through some of those things has helped me post-scan to be able to control some of those things.
Do you still work?
I stopped working after my diagnosis. We were lucky enough to be in a situation where I could step away from work and we could live our lives as normally as we had. I know that is not the situation for a lot of folks, so I don’t take that lightly.
What it has allowed me to do is spend my time how I want to spend it and prioritize my time differently than I did in the past. I think with a lot of folks, work is always this big rock that you always have to spend time on. Then, you get home and you got kid’s activities and all these different things. It just consumes the day. With me not having to work, I’ve been able to spend time with my kids that I never would have had the ability to do.



One of the things that I’m most grateful for is the last 2 summers, our kids would go to some type of camp or care when I was working. But since I’ve been home, we didn’t have to do that. I was able to stay with the boys both summers and they coined the term Summer of Dad. What they would do is they would take a plain old calendar, and just start filling it with all these activities that they would want to do throughout the summer break. My job was to find ways to get all those things to happen over the course of 65 days or 80 days or whatever it is.
It has been so much fun and so rewarding to spend that time with my kids. My phone’s not ringing. I don’t have to worry about email. I don’t have to worry about the grind of a traditional job. I’m able to spend my time how I want.
Which cancer support groups do you recommend?

I would be remiss if I didn’t mention a couple of groups that helped me tremendously through this diagnosis. One of those is colon cancer-specific. It’s a group called ColonTown, a nonprofit organization that focuses on patient and caregiver-led support, education, and being able to, share stories and speak to people who are going through things that you’re actually going through.
The other group would be Man Up To Cancer. This is an all-cancer type group, but specifically for men. We touched a little bit earlier on that stigma of male mental health, isolation, and those types of things. That group is phenomenal at helping solve that gap and really providing support and help for men specifically to not isolate during these times and how critical it is to not do that.

As a cancer patient being able to find the people who are going through this with you, it’s amazing. The connections you can make with people, whether it be online or in-person, that are going through things. It’s almost a bond that’s stronger than any relationship I’ve had with people I’ve known for years. I don’t know if it’s a trauma response or what it is, but it’s interesting to be able to surround yourself with like-minded people in similar situations. You just feel that weight gets taken off your shoulders to some extent when you can share and know that people get it.
What advice do you have for others on a cancer journey?

Don’t give up hope, number one. Absolutely educate yourself on your disease and be an advocate for yourself along with your care team. Be a part of those conversations. Don’t just let those conversations be done to you and take your life back.
To say I’m not scared of death is an extreme understatement. I’m actually terrified of that, but can’t control when that’s going to happen. It’s all in science’s hands at this point. What I don’t want to do if I get to that point, is look back and say I’ve wasted the last year, 2 years, 3 years, whatever that is, worrying and not living my life. That will be my biggest regret as a father, a husband, and just as a human.
Everybody has a stopwatch above their head, and some might be shorter than others, but I’m going to maximize every day I can and I’m going to do whatever I can to enjoy it, whether that be enjoying my own hobbies or spending time with my friends and family. I’m not going to let it take that part of my life away.
More Colorectal Cancer Stories
Kristie C., Colon Cancer, Stage 4 (Metastatic)
Symptoms: None per se that she noticed; she experienced constipation and passed narrow stool, but had been experiencing constipation most of her life, and thought that these digestive issues could also have resulted from perimenopause
Treatments: Chemotherapy (including adjuvant chemotherapy), radiation therapy, ablation therapy (liver ablation), surgeries (colectomy, temporary ileostomy, ileostomy reversal, scheduled liver resection)
Briana H., Colorectal Cancer, Stage 3
Symptoms: Periods of constipation initially lasting one week and then extending to two weeks, nausea, pain in lower left abdomen, lack of appetite, vomiting and inability to keep fluids down
Treatments: Surgeries (colon resection, tumor removal, colostomy placement, colostomy reversal), chemotherapy
Kailee O., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Sensitive stomach sometimes leading to vomiting after eating, bleeding during bowel movements, persistent fatigue, back pain, abdominal pain, anemia, significant symptom flare-up during second pregnancy
Treatments: Surgery (colectomy), chemotherapy, targeted therapy
Starr S., Colon Cancer, Stage 4 (Metastatic)
Symptom: Abdominal pain
Treatments: Chemotherapy, surgeries (colectomy, hepatectomy, lymphadenectomy), targeted therapy
Jackson L., BRAF Mutation Colon Cancer, Stage 4
Symptoms: Severe stomach pain, fatigue, lack of motivation, anemia, blood in stool, thinning stool
Treatments: Surgeries (emergency bowel obstruction surgery with temporary colostomy, possibility of HIPEC in 2026), chemotherapy, immunotherapy
Heather C., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Severe bloating, indigestion, vomiting, rectal bleeding
Treatments: Chemotherapy, surgery (liver transplant, upcoming)






