Chris’s Stage 2 Lynch Syndrome Colon Cancer Story

- Name: Chris T.
- Diagnosis: Colon cancer
- Age at DX: 31
- Staging: 2
- 1st Symptoms:
- Family history led to early colonoscopy
- In hindsight: lower abdominal pain when sneezing, choppy bowel movements
- Treatment:
- Surgery
- Colectomy (total removal of colon)
- Surgery
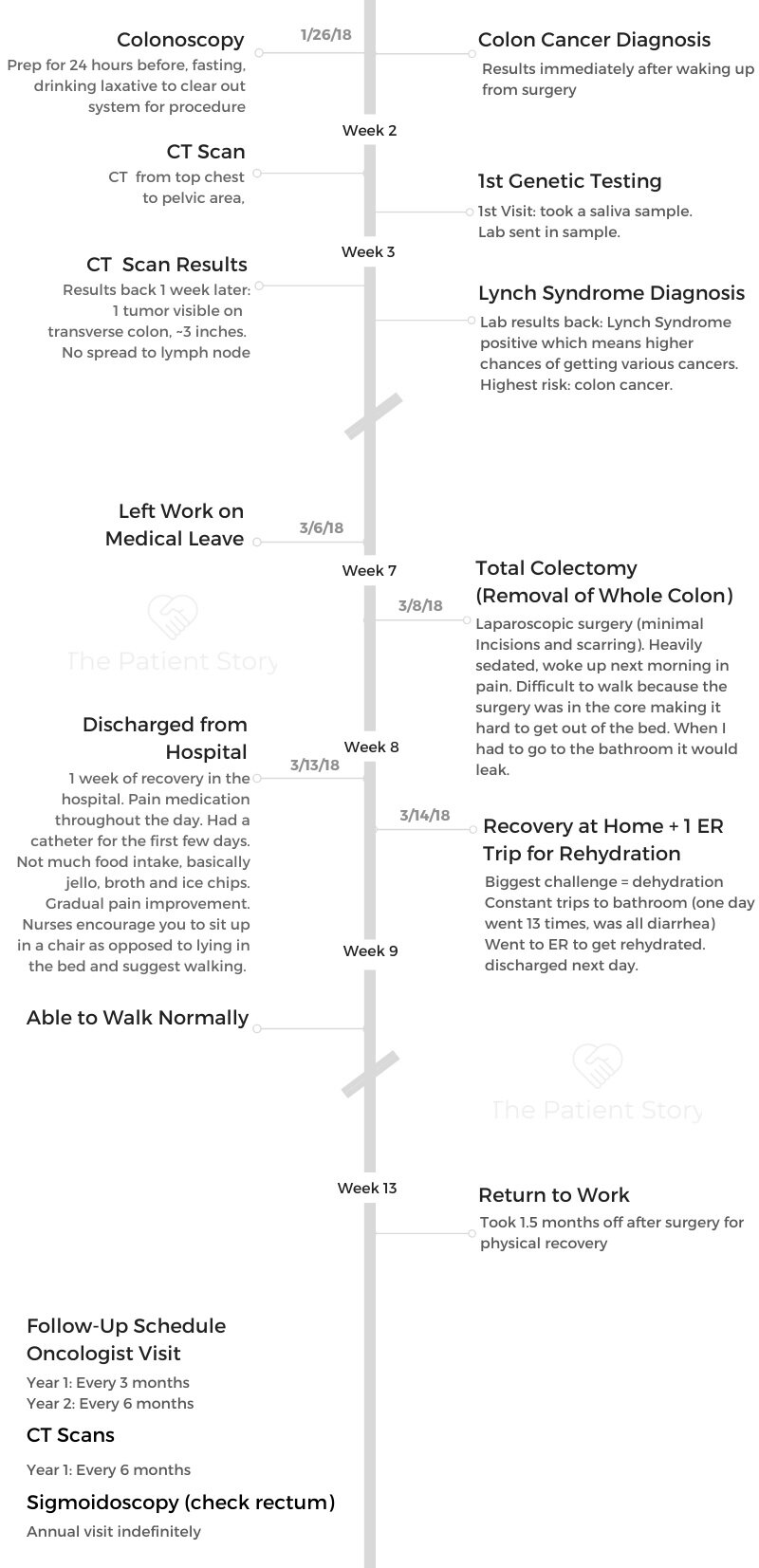
- Colonoscopy and Diagnosis
- How did you know something was wrong?
- When did you get the colonoscopy before your diagnosis?
- In hindsight, were there any red flags, symptoms, etc.?
- How long had you experienced those symptoms?
- How old were you when you got the colonoscopy?
- What is the prep for the colonoscopy procedure?
- What’s a colonoscopy like?
- Describe how you learned the diagnosis
- What questions did you have?
- Tests and Scans
- What appointments did you have to schedule before the surgery?
- There was a lot of waiting for scheduling appointments and for test results
- Any tips on how to manage the stress of constantly waiting?
- What is a CT scan like?
- How did you do genetic testing?
- What is Lynch syndrome?
- How did you decide where to go for treatment?
- Treatment Decisions
- What was the recommended treatment for your colon cancer?
- Deciding whether to remove the entire colon
- How did the surgeon describe the odds of you having to have a colostomy bag?
- Would your decision have been different if you needed a colostomy bag after the colectomy?
- People will always give their advice — even unsolicited
- How did you handle unwanted advice from well-meaning people?
- Finding your cancer community is important
- You decided to remove the entire colon (colectomy)
- Was it helpful to have your wife at appointments?
- Colon Removal Surgery (Total Colectomy)
- What do you remember about the surgery and recovery?
- What was the impact to your life after removing your colon?
- The results of the colectomy were successful
- How was dealing with food and bowel movements?
- How did they know when to discharge you from the hospital?
- Was there anything you wish you had known before the surgery?
- Any questions you suggest other patients keep in mind?
- Post-Surgery Recovery
- Mental and Emotional Impacts of Cancer
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Stay strong and positive. Don’t focus on any negatives within the situation. Just focus on each step of how you can get better, and try to handle those as soon as you possibly can.
Chris T.

Colonoscopy and Diagnosis
How did you know something was wrong?
Unfortunately, cancer has been a part of my family history. Not me, per se, but my dad had cancer. Some other people: my grandma and a couple aunts. My dad got cancer in his early 40s, so I was always told to just go get checked out.
I just went in for that routine colonoscopy, and once they were done, they basically told me I had colon cancer and they didn’t know the stage or anything. At that point, I didn’t have scans.
When did you get the colonoscopy before your diagnosis?
I got a colonoscopy that January, and our daughter was born in May. I initially was going to wait until the following January to do it, but I decided to accelerate it just because she would be 1 [year old]. That was a blessing to have that pushed up instead of waiting another year.
Just speaking with my doctor and telling her my family history and me wanting to get a colonoscopy, she encouraged me to go. Prior to the colonoscopy, I had got some blood work done.
I had low iron, which my doctor found out. Then after I explained my family history, she sent me in, even though I was going in anyway. That’s where it all started.
In hindsight, were there any red flags, symptoms, etc.?
Regarding symptoms, initially, I didn’t really feel any symptoms. After finding out that I had colon cancer, in hindsight, I was able to pinpoint certain symptoms — certain things you attribute to things like age.
There were things I brought up to the doctor’s a couple years ago, like when I sneezed, I’d get a pain in my lower abdomen. I was like, “That’s odd.” I went in for that, and they didn’t really know what it was.
Also, not to be too specific, but when I had bowel movements, they would be choppy instead of just one whole piece or cylinder.
In hindsight, [it] was that way because it’s a tumor, chopping the bowels as they went down, and the tumor would cause that excess gas. When I was sneezing, [there was] that pain.
Also, for whatever reason, I would be full for hours after eating one orange. That’s because of how acidic the oranges are. Those were some symptoms that I realized after the fact.
How long had you experienced those symptoms?
I don’t remember exactly how long, but I know that the sneezing pain situation happened at least a couple of years, but it was happening [more] frequently [closer] to the date I got tested. It happened once a month, or something like that. A couple years before, every few months or so.
That would happen more frequently closer to the colonoscopy, and then I don’t really necessarily remember the date of when my bowel started seeming choppy or I felt full from the acidity for eating certain foods.
How old were you when you got the colonoscopy?
31. That was the first one I’d ever gotten. From what I understand, it used to be in [your] 50s when you’re supposed to go, but they pushed it up just because people are getting it more frequently now at a younger age. I think the average or the recommendation now is mid-40s or late 40s. That’s for people who don’t have history. Late 40s, early 50s is what I understood.
When I went in, everyone was confused why I was going in, because initially when I was describing what was happening, they were just like, “Oh, you don’t have any blood in your stool, or you don’t have any of the common symptoms. Why are you here?”
Then I’d fill them in, and they understood it [was] because of my family history.
What is the prep for the colonoscopy procedure?
At first I was nervous just because I’ve never had anything like that done.
You have to fast for a certain amount of time prior to the colonoscopy, and you have to drink this liquid that clears out your colon so they can get a clear view of everything.
Then you have to take a couple of pills as well. I don’t remember the specific name of the medicine.
The worst part — or the challenging part of the prep — is drinking gallons of this liquid that they make you drink to clear out your bowel. It doesn’t taste the best, and you have to frequently use a bathroom to clean out your system, for about 24 hours.
What’s a colonoscopy like?
They check your medical information and confirm it’s you. I go in the back and change and lie in the bed. It’s not too intense when you’re sitting there.
A part of my preparation process was then to use anesthesia. The nurses come back, and they check my blood work and then administer the process of anesthesia. I go in the back and eventually come out and just wake up with some of the results. It was fairly quick.
Describe how you learned the diagnosis
It was a curt situation. The doctor came in. I was like, ‘Hey, so how’d everything look?’ [I was] in these happy spirits. He was like, ‘Well, not really good. You have cancer.’
Our jaws dropped. There wasn’t really too much bedside manner with it. They weren’t mean about it, but it wasn’t too much bedside manner. I know different doctors are different, but that was my experience. I wouldn’t want anyone to be discouraged because of that.
At that point, we started asking about next steps, and that day there was nothing we could do. We went home and then just scheduled everything as soon as possible.
»MORE: Patients share how they processed a cancer diagnosis
What questions did you have?
- How bad is it?
- Can you tell the stage?
- What did you see?
- Does it look like it went here or there?
He gave it a generic description of the size. At that point, he told me it doesn’t look like stage 4. Worst case is stage 3, but we can’t confirm that, so you’ll get scans and do all the other testing.
That’s all the information I was able to get, but it was still just uncertain.
Tests and Scans
What appointments did you have to schedule before the surgery?
First it was the CT scan to see how big the tumor was and genetic testing, to pinpoint why it happened, if there was a reason why it happened, and then the next steps to take for the surgery.
We scheduled a scan as quickly as possible at the nearest Kaiser that had the first opening for CT scans. We didn’t want to wait a couple of weeks. I think we scheduled something for a couple days later.
There was a lot of waiting for scheduling appointments and for test results
The worst part about that initial process — besides or excluding finding out I had cancer — was waiting a while to get the results for the CT scan, because that will take about the week. You’re just sitting, waiting there and trying to just figure it out. You’re wondering about the severity of a situation and basically prepping yourself.
It seemed like it was a common thing for them. Unfortunately, they just need the information, and then it’s like, “Okay, my job’s done here. Go to the next step.” I understand, but you don’t feel that way from our perspective as patients and caregivers.

Any tips on how to manage the stress of constantly waiting?
I’m just a really positive person and optimistic. That’s how I was raised. But obviously, there’s challenges. You’ve just got to look at the bright side of everything.
There’s a reason I went in early. I’m glad I caught it early. This could be happening years from now. I don’t know how bad it would be, but I’m just happy that I was addressing it. Just trying to put a positive spin on everything.
My wife was really helpful as well. She was really strong in that situation. While she was pregnant, she was very helpful. It was also challenging for her. Within that waiting period, we just focused on everything positive. Moving forward and beating it as soon as possible.
I try to apply that to everything in general, though. There’s always pros and cons to situations. There’s people, there’s kids who find out news about cancer and everything. Just having a proper perspective of it. Not feeling sorry for myself.
What is a CT scan like?
I’m not sure how many of them did, but they did from the top of my chest down to my pelvic area, basically my upper thigh. They didn’t see anything anywhere else besides the one tumor that was on my transverse colon, which I think is the lower right part if you’re looking down at your stomach.
I forget how big. I think it was around 3 inches or so. They [hadn’t spread to lymph nodes], so they were able to find that it was just the one large tumor.
How did you do genetic testing?
After they did CT scan, I went to see the genetic counselor. It was all a process of just rescheduling these different appointments, but just trying to get in to see me as soon as possible.
With the genetic counselor, I went back several times. I think they took a spit sample, and then they had to send it in. Then when they got that back, I went back to hear the results.
»MORE: Read our interview with a genetic counselor
What is Lynch syndrome?
We figured out that I had Lynch syndrome. You have a higher chance of getting certain types of cancer. The main cancer that I had a higher chance of getting was colon cancer. I think they said there was a 50 to 80% chance that I would get it.
Then all the other cancers are smaller percentages. If someone has a 2% chance of rectal cancer, I have an 8% chance of rectal cancer, and so on for other types of cancers.
Everything else was on the smaller end, like in the single digit percentage, meaning a higher risk for the colon cancer was the only one that was that 50 to 80% range due to the Lynch syndrome.
How did you decide where to go for treatment?
I was meeting a surgeon at the local Kaiser I go to. Depending on the type of surgery that I wanted to get done, depending on the experts, he wasn’t the best, but I was initially just going to have him move the ascending colon.
Treatment Decisions
What was the recommended treatment for your colon cancer?
It’s either removing a portion or removing the whole thing.
The reason they recommend removing the whole thing is because having Lynch syndrome, the chance of getting colon cancer again is increased.
Deciding whether to remove the entire colon
I’ll start with the pros of not taking the whole colon. The pros of that were basically, I could guarantee that I wouldn’t have a colostomy bag. The surgery was quicker; the recovery was faster. I didn’t know how my body would react to taking the whole colon.
They described removing partial colon as an easy procedure, easy surgery. I looked at it as well [that] I still have some of that to help my body process [and keep] the same functions that it’s supposed to have.
The uncertainties of removing the whole thing and not trusting certain information I find on the internet and just not sure about how I was going to be able to navigate through life.
That thought process was stressful and intense, because although people tell you that things are going to be okay, you don’t know how your body’s going to react to not having a colon and then substituting that and using your small intestines to function as the colon would.
The initial questions were:
- Am I going to have a bag (ostomy), and if I do, that’s not the worst thing in the world, but how am I going to move through life?
- Am I going to be able to go to Disneyland?
- Am I going to be randomly on a jog and have to go to the bathroom urgently or at park or wherever, whatever I’m doing?
All those things played a factor, and I basically consulted with our friend who’s an oncologist. I talked to her, and friends and family helped as well.
The main issue was having a colostomy bag. After I got over that, I was able to move forward easier with choosing to remove the whole colon.
The doctor saying that I did not need a colostomy bag really helped me with that as well. They didn’t do anything to my rectum, because the colon connects to the rectum, so that that’s still intact. He’s like, “If something else happens, we’re able to still work with you to not have a colostomy bag.”
Just thinking about the big picture and everything helped me ultimately decide that having a colostomy bag wasn’t the end of the world. Just being healthy is the most important. That’s what helped me move forward with it.
Just mirroring off of that, on the other end of removing the whole thing. The main reason for me doing it was because of having those genetic testing, having Lynch syndrome, the odds of it coming back being significantly high for me.
How did the surgeon describe the odds of you having to have a colostomy bag?
He just mentioned that surgery in general doesn’t require that, the way the surgery is done and how they’re able to fix things back together. Basically, it’s not required for a lot of people.
Every situation is different for people. There’s people who have Crohn’s disease or other types of things on why they need to have their colon removed. Some people might have to have the surgery and have a bag temporarily, depending on the surgery or depending on how your body needs to recover.
He pretty much guaranteed I wouldn’t need one and if I needed one, it would be temporary while I was in the hospital. They would just go back and patch me up, and I’ll be good going forward.
Would your decision have been different if you needed a colostomy bag after the colectomy?
I would have been leaning toward not removing the whole thing, but I honestly can’t say what I would have decided. I was being pushed towards removing the whole thing regardless, just because ultimately it was the best thing to do.
Sitting from where I’m sitting and knowing how I felt then, I feel that it would have been more difficult to decide.
People will always give their advice — even unsolicited
To be honest, it could be a little irritating and stressful dealing with certain people, because a lot of people think they’re doctors and have the best answers when they’re not. I have people giving me information, trying to go directly against my surgeon, who [specializes] in colonoscopies and colon surgeries.
Everybody’s giving their 2 cents, which could throw you off or derail you from what you shouldn’t be doing or what is in your best interest, even though they have your best interest at heart.
It doesn’t really align sometimes with what you’re thinking, because everybody just gets panicky and starts throwing out recommendations or worst-case scenarios like, “Oh, I know someone who doesn’t have a colon, and this is how their life is, or whatever perspective they have on it.” That part was difficult.
How did you handle unwanted advice from well-meaning people?
Eventually, after that point, I would still talk with people, but I filtered it out. I just started doing my own research. My wife and I did research. We just prioritized opinions, even though everyone’s opinion matters.
We prioritized my friend who’s an oncologist who works with cancer, obviously, all the time and every day, and my specialist surgeon and the certain doctors that we trust. We just had it prioritized that way.
I also find this platform amazing. I searched hashtags on Instagram and was able to find a few helpful people to give their perspective, their story of their situation regarding having a colon removed or life without a colon, how they handle things, and what their experience was. That was really helpful.
Finding your cancer community is important
I think this site is awesome for that. That’s what actually helps a lot on me making a decision. Ultimately, obviously, it was my own decision, but it was helpful hearing success stories of people who actually went through it.
Looking up things on the internet can be unhelpful, just from a broader angle. You might read something that doesn’t even apply to you. People have surgeries for different reasons. The reason you’re having a surgery might not [be the same]. You might not have the same reaction to someone else.
I always suggest the internet’s helpful, but then just be aware of not looking at the negative stories and thinking that that can be your worst-case scenario. Filtering that out and knowing what source is credible and how it applies to you.
You decided to remove the entire colon (colectomy)
I also decided to remove my whole colon, which is called a colectomy. I did that because I didn’t want to increase the risk of getting colon cancer again with having Lynch syndrome. That’s the highest-percentage place that my cancer can come back.
I didn’t want to regret not removing the whole thing and seeing however many years it comes back for whatever reason and comes back more aggressive. In my situation it wasn’t aggressive; it was a slow-growing tumor.
Just talking with a close friend who’s an oncologist, she told me that. I thought it was the right approach, and I wouldn’t want to regret that down the road if I get cancer again, which I don’t think I will.
If I did, I wouldn’t want it to be because I didn’t remove my colon, because I didn’t want to go to the bathroom a few more times a day.
That’s what I decided, but I had the option to decide that down to the minute before my surgery was going to take place.
The surgeon said it’s the same thing for me. I’m going to go in there, and I don’t need to get any different tool for the surgery.
You literally have up until before you’re sedated and under to decide. I was in the back, and I was pretty confident on deciding that I wanted to remove the whole colon.

Was it helpful to have your wife at appointments?
Yeah, it was very helpful to have her there. She took notes while I was engaged with the doctor, and she actually stayed in the hospital with me pretty much every night, while she was pregnant, while I was recovering.
Regarding the prep, it’s very helpful to have someone go with me, field questions, and ask additional questions. In the moment, you might have a list of questions. You can get caught up in the conversation and forget to ask something, but that other person being there will be able to help with that.
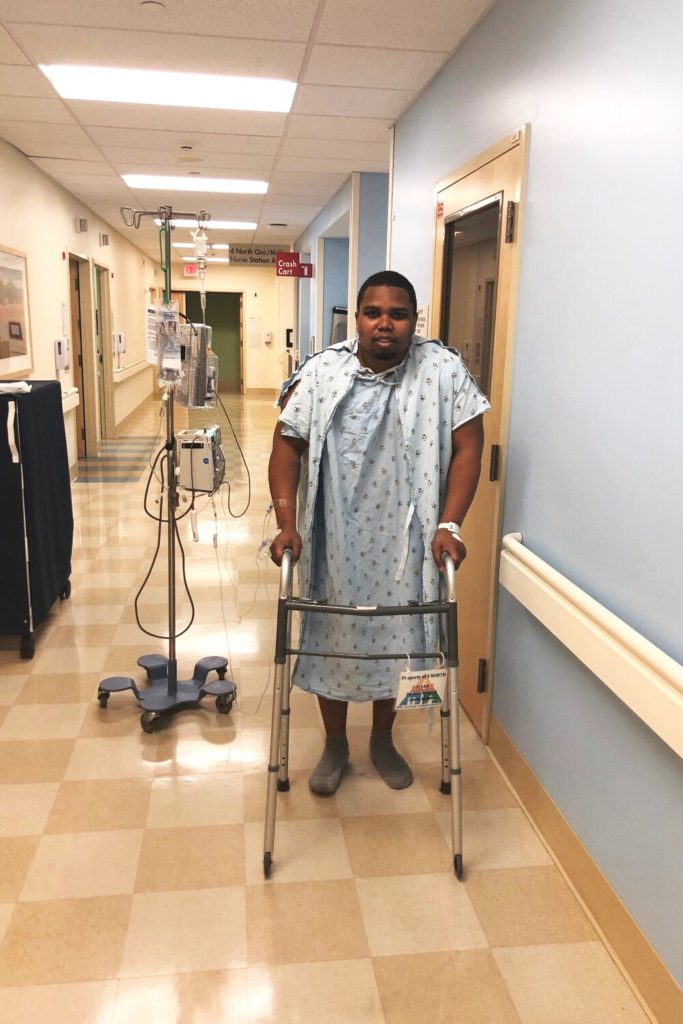
Colon Removal Surgery (Total Colectomy)
What do you remember about the surgery and recovery?
I don’t remember how long the surgery was. I know that the recovery was challenging. I was in the hospital for about a week. I was heavily sedated, and I woke up that next morning. I was in pain.
It was very difficult to walk because the surgery was in your stomach, in your core, so it was hard to get out of the bed. When I had to go to the bathroom, it would kind of leak out, like a green liquid. I needed help to go to the bathroom.
I had pain medication throughout the day. I also had a catheter for the first few days. I couldn’t eat much, basically jello, broth, and ice chips. There were days I didn’t want to eat anything.
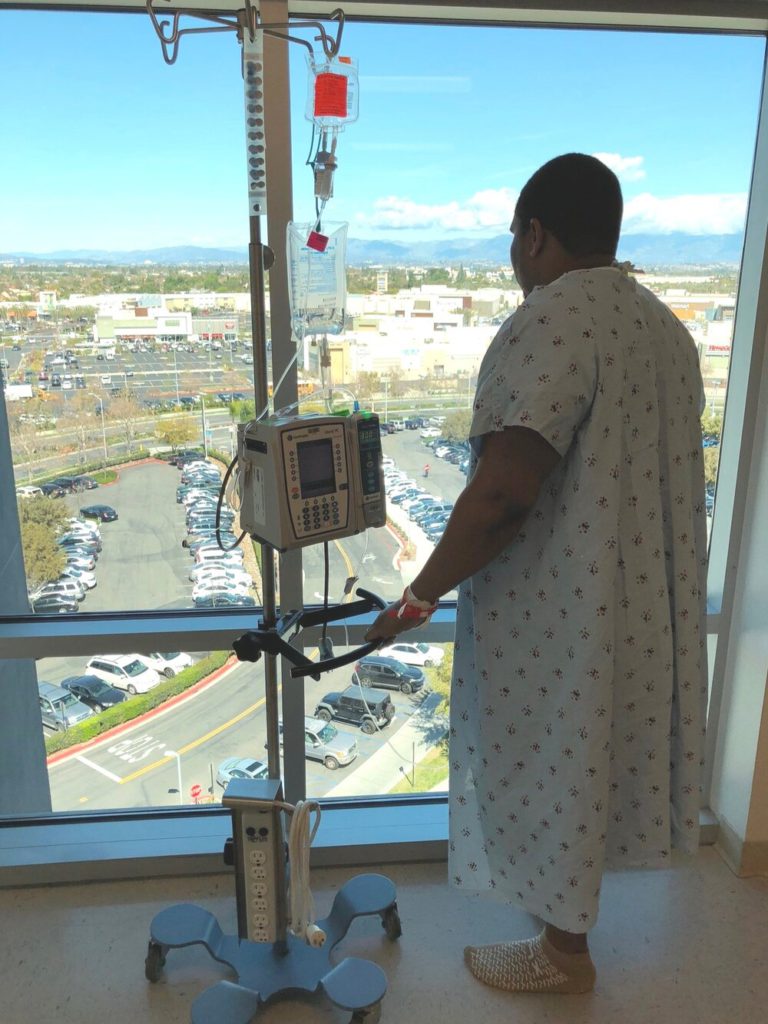
Then you start to get better, and they encourage you to sit up in a chair as opposed to laying in the bed. They encourage you to walk around the hospital. We’ll walk around with the little thing that holds your IV, the pole. That gradually got better.
What was the impact to your life after removing your colon?
One doctor told me you can have a bowel movement about 10 times a day, they’re going to be this way or that way, and the recovery can take this amount of time.
The main difference they describe is just how often you go to the bathroom. In my case, I’m basically going about the same as I did prior to my surgery, regarding bowel movements.
There’s also days that it’s worse. Depending on certain things you eat, it might come out differently, but you’re able to eat whatever you want, and that didn’t change.
The results of the colectomy were successful
What they described to me from best to worst case scenario, I’m more on the best-case scenario, which has been such a blessing. I’m very grateful for that.
With that being said, I’m extremely happy that I chose that option. Initially, going through the recovery, this was a little frustrating and painful and just dealing with all that, questioning your decision. As you heal and get better, it was all okay in the end.
How was dealing with food and bowel movements?
They slowly integrate solid foods, but I felt that when I did, I wasn’t really ready for that. I didn’t really have an appetite for it, but they eventually started implementing solid foods.
I’d still take my time and maintain a liquid diet, which was just water, jello, puddings, and stuff like that.
How did they know when to discharge you from the hospital?
They made sure I was hydrated enough [and] took the catheter out to see how I reacted to that. How I was feeling overall was the main thing.
Was there anything you wish you had known before the surgery?
They were pretty good about informing me on everything prior to the surgery. They didn’t leave anything out. It was nice having them do the laparoscopic surgery, where it wasn’t too invasive. That was helpful knowing that in advance, and we were pretty well informed.
We had several doctor visits and asked thousands of questions, but they were very helpful. The nurse practitioners [and] everyone were helpful within that process.
We did extensive research on our end, so by the end of that, we felt like we took a course on it as well. I think I had all the information I needed going into it. It was just the uncertainty of how my body would react to the surgery.
Any questions you suggest other patients keep in mind?
I would suggest if you’re uncomfortable about the colostomy bag, ask about how the procedure is done. I also asked about the scarring and how that would look.
I would recommend asking about just the recovery process. Make sure you’re giving them your full medical history and let them know everything related to your body so they can give you the best-case scenario.
Post-Surgery Recovery
How was recovery at home?
Once I was discharged, it was challenging at home. They gave me the medicine I needed, but I would walk around and try to get through the pain.
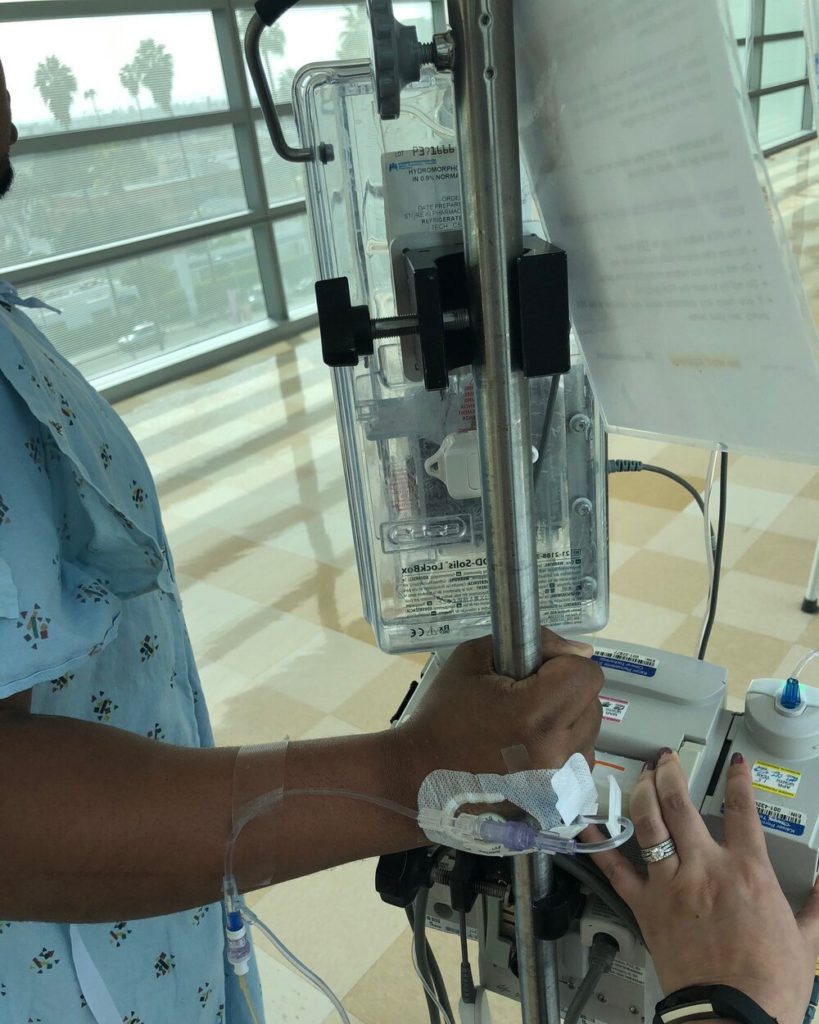
The biggest challenge that I had was dehydration, because once I was able to go to the bathroom, [I went] more often. One day I went 13 times or something, and it was all like diarrhea. I was extremely dehydrated and had to go back to the ER to get rehydrated. I think I stayed in the hospital for a day or so maybe.
I just had a catheter. I had just learned to go to the bathroom. Initially, it wasn’t a lot. The more I ate, obviously, the more frequently I would go, but initially it wasn’t too often.
After that I was getting back into the normal swing of things. It was very painful but every day was progressing in the right direction.
A couple weeks after the surgery, I was able to go on walks. They weren’t quick walks, but I was able to go out and do stuff.
Every week from there was going in the right direction. I think 3 weeks after the surgery, I was actually walking a couple miles a day or something.

What were the next steps after surgery?
They told me to monitor my bowels and hydration. I know I had to go back to get my stitches or staples removed from the surgery. I think that was a few weeks after the surgery. It wasn’t painful; it was like a pinch when they took it out. It wasn’t bad at all.
How was the healing process after the surgery (total colectomy)?
I don’t want anyone to be discouraged from that, because that was a small part of the journey. In that process, second guessing why [we] removed the whole colon and if it would have been less excruciating pain if I didn’t and all that stuff, but those were just small moments within that.
Gradually, every day you got better. Initially, it was very painful. I don’t want to lie, but after about a week or so, it was fine. I got back pretty quickly.
You had to stop work for about a month and a half
Initially, it was tough getting through the surgery recovery, but then after that, it was nice pulling my strength back up, going on walks, eating more normal food, and doing more normal things from prior to the surgery.
When I went back to work, I was pretty much 100%. It’s nothing physical, where I have to do manual labor. It’s at a desk, so it wasn’t as difficult to come back. I wanted to make sure I was 100% and take advantage of the leave they provided.
Any guidance on how much time to take off work?
I thought that was enough [time off]. I don’t want to take too much time because I need to take time later in the year for paternity leave, so that motivated me to not take too much tine as well. I personally think a month and a half was enough for me.
»MORE: Working during cancer treatment
What’s the follow-up plan?
Every 6 months would be the routine for that initially, then moved to every year. I’ll still see my oncologist every 3 months. I met with my oncologist 3 months after my surgery, then I saw her every 3 months, except this year it’s every 6 months.
Every year I’ll have to have a sigmoidoscopy (check rectum) to see if anything came about, if there’s anything cancerous there. It’s every year ongoing because that’s the closest thing to the colon, the highest thing to getting cancer, so they’re going to check that every year.
Describe the follow-up appointments
The appointments consist of blood work and the scans. Not every appointment has a scan, but it does have blood work. They test you and see how you’re feeling if the blood work seems fine. There’s a couple urine tests as well through the visits, but they’re general checkups.
Mental and Emotional Impacts of Cancer
How has cancer impacted you?
Just perspective. I’ve always had a good perspective on everything. An example is when my mom unfortunately passed away from gastric cancer. When she was in her hospital bed, she was telling me there’s kids who have cancer.
At least I’m 50-something and always had that positive spin on things where you can’t feel sorry for yourself. Although this did help with perspective, I’ve always had a good understanding of things could be worse.
It helped me try to spread this information and help people as much as possible, be a positive example of someone who can get through the situation successfully. Just wanting to spread that as much as I can.
Physically, I feel fine. When I was first done with surgery and started to work out again, I was hesitant to do anything core-related. I got over that and was able to do so.
I just try not to push it with certain things. It’s just me, depending on the day, being cautious, but I’m pretty much able to do everything I could before physically.
You still think about cancer sometimes
There’s times when you feel something, especially after the surgery. Little twinges where the surgery were — is that something related to the cancer or to the surgery?
There are times I don’t think I have it, but I might think that feels different. I am just more aware of smaller things that aren’t a big deal in my body. I’m not necessarily afraid of them. I’m just like, “Well, I had a scan this month and blood work this month. Everything was fine.” The consistent checkups help me with the anxiety.
Knowing I had a CT scan last October and an oncology appointment this year — if something feels different, it’s comforting knowing I had those appointments.

What helped you mentally heal?
Family. My wife was very helpful. Knowing I had a daughter on the way a few months after my surgery definitely helped me be in the right spirits, focus, and try to get back as soon as I possibly could.
Talking to people. Not anyone who’s negative or had a negative outlook on things. Community. Family. A good support system with family and friends was really helpful. I had people visiting me throughout the process while I was recovering, so that helped a lot.
Message to those hearing your story
I would say to stay strong and positive. Don’t focus on any negatives within the situation. Just focus on each step of how you can get better, and try to handle those as soon as you possibly can.
Regardless of the results that you hear from the doctor, just know you have a chance, and you’ll be able to beat whatever situation you’re going through.
Don’t be afraid to do the proper procedures and surgeries to give you the best possible outcome for surviving and beating it down the road. I know my situation was tough to decide whether to get rid of the whole colon or partial.
Just do whatever’s best for your overall health, even if it means potentially having to change your day-to-day life. I think that will be the right thing to do.

Inspired by Chris’s story?
Share your story, too!
Colon Cancer Stories
Nathan G., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Persistent heartburn, feeling full after eating, severe abdominal pain
Treatments: Surgeries (colectomy, cytoreductive surgery, lymphanadectomy), chemotherapy (FOLFOX, HIPEC or hyperthermic intraperitoneal chemotherapy)
Mariana T., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Bloating, anemia, appearance of blood in stool
Treatments: Surgeries (bowel resection, oophorectomy, salpingectomy), chemotherapy (oxaliplatin, fluorouracil, FOLFOX), immunotherapy (bevacizumab)
Helen D., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Pelvic pressure and pain, burning with urination, bloating, constipation for a short period, low energy or fatigue, discomfort sitting, night sweats
Treatments: Chemotherapy (FOLFOX, FOLFIRI, hepatic artery infusion pump therapy), targeted therapy (panitumumab), surgeries (liver resection and ablations, colon resection, full hysterectomy)
Jim S., Colon Cancer, Stage 4 (Metastatic)
Symptom: Back pain, especially when sleeping for long periods
Treatments: Surgery (partial colectomy), chemotherapy (FOLFIRINOX, bevacizumab, oxaliplatin, irinotecan)
Meagan M., Colon Cancer, Stage 3C
Symptom: Appearance of blood in stool
Treatments: Surgery (partial colectomy), chemotherapy (FOLFOX)








Leave a Reply