Dr. Kenneth Biehl
Radiation Oncologist
Dr. Kenneth Biehl is a radiation oncologist who specializes in radiation therapy for cancer patients. In this interview with The Patient Story, Dr. Biehl talks about what radiation therapy is, possible radiation side effects, and patients’ and caregivers’ frequently asked questions.
I love that I can help people through this process of learning what’s going to happen to them and their body and things that they can do to overcome the cancer.
Dr. Kenneth Biehl
- Name: Dr. Kenneth Biehl
- Role: Oncologist
- Specialty: Radiation therapy
- Experience: 10+ years
- Salinas Valley Memorial Hospital, Comprehensive Cancer Center (current)
- Key messages to patients & caregivers:
- Radiation treatment is a quick procedure, largely painless in the moment
- One of the most common questions from patients is what are the radiation side effects? His answers: depends heavily on what cancer and where in your body.
- Radiation therapy is often given to help people with side effects, not just to help destroy the cancer
- Clinic takes many precautions to protect other parts of the body from radiation exposure
- Says most patients who don’t have physically intense jobs are able to work through radiation treatment
- Radiation Therapy Treatment
- In layman’s terms, what is radiation therapy treatment?
- Does radiation therapy hurt? What does radiation therapy feel like?
- What are the side effects of radiation therapy?
- What are some examples of side effects for different cancers?
- There are different ways of giving radiation treatment
- You specialize in “External Beam Radiation Treatment.” What is that?
- How do you protect other organs during the radiation treatment?
- How do you protect the patient from radiation exposure to healthy parts of the body?
- Can patients bring family or friends to the radiation therapy treatment?
- Is there risk of a patient exposing those around them to radiation after their treatment?
- Relationship with Patients
- How many patients do you see in your clinic?
- What are the differences between the experience at a mid-level size clinic like yours compared to smaller and bigger clinics?
- What can a patient expect during the radiation treatment process?
- The first radiation therapy session is actually a simulation
- How often do patients typically see you?
- What are the most common cancer patient questions about radiation?
- Can patients work through their radiation therapy treatment?
Radiation Therapy Treatment
In layman’s terms, what is radiation therapy treatment?
Radiation treatments are high-energy photons, so similar to the light from the sun, but it’s a lot higher energy than from the sun. It passes through the whole body. As it passes through the body, it causes breaks in the DNA of cells, both cancer cells and normal cells.
The way the radiation works is the cancer cells are unable to repair themselves, unable to repair that DNA damage whereas the normal cells are able to repair themselves. So you’re able to kill cancer cells while preserving normal cells.
Does radiation therapy hurt? What does radiation therapy feel like?
Radiation therapy is very similar to getting any other X-ray. If you’ve had an X-ray, that’s how radiation feels.
During the treatment you don’t ever feel anything. The treatments are very brief. They only take a minute or two to give the treatment.
In some rare cases where you’re getting very high doses of radiation, it can take up to 10 to 12 minutes or so. During the radiation treatment you don’t feel anything at all.
Generally, if you have a longer course of radiation where you’re getting radiation treatment over five to eight weeks or something like that, then the radiation treatment side effects will begin usually in the third or fourth week of treatment.
What are the side effects of radiation therapy?
It really depends on where the radiation treatment is given. If you have radiation treatment given for breast cancer or prostate cancer, those are in totally different positions on the body. The breast cancer’s often close to the surface of the skin so you’re much more likely to have some skin side effects. Those are usually just little darkening of the skin first then a little pinkness in the skin.
What are some examples of side effects for different cancers?
The side effects of radiation treatment for the breast are generally: if you have a left-sided breast cancer, the heart and the lungs sit right behind it. If it’s on the right side then the heart’s usually out of the field and we don’t have any side effects with the heart. Those side effects are long term. It’s not anything that you’d feel during the radiation.
What you start to notice during maybe the third or fourth week of treatment is a little fatigue and also some changes in your skin. A little redness or pinkness in the skin, a little darkening of the skin.
Sometimes patients after surgery on their breast, there’ll be a little inflammation still in the breast. The breast will look a little larger. They’ll notice as time goes on, the breast gets smaller. Some of that can be attributed to the radiation. Some of that is decreased inflammation in the breast.
Those are the sort of side effects that you can develop. That redness in some rare cases can progress to a little peeling in the skin or sometimes even a little blistering in the skin in a more severe side effect.
With prostate cancer, the prostate is deep within the pelvis so there aren’t really any skin side effects. But the prostate sits right between the bladder and the rectum so you can have side effects in both the bladder and the rectum.
In the rectum you can have some diarrhea, some urgency with your bowel movements. With the bladder you can have some urgency with your bladder, feeling like you have to get to the bathroom right away. Sometimes you can have some burning with urination.
Most of those side effects of radiation are gone within a month or two with the radiation finishing up. Some are gone very quickly after radiation treatment.
If you then take that and you say I’m going to give radiation treatment to the brain, then you have a totally different set of side effects. Or if you’re treating the neck it’s a different set of side effects, or the arm or a leg or something like that. The side effects are very dependent on where the radiation treatment is given.
There are different ways of giving radiation treatment
That’s mostly what I do here. Particularly with what I used to do with the female gynecological malignancies, we’d give internal radiation treatments with something called brachytherapy.
You actually place a radioactive source within the body either in the vagina or the uterus. You place it there, you leave it there for a certain amount of time and then you remove it.
So you can be a little more precise with the radiation because you put it right where you want it and then you remove it. Rather than having it pass through the whole body.
You still run into the same idea where you have to plan out where to give the radiation and see what the normal organs are around it and try to lower the dose of those areas.
In some ways, you can be much more specific with radiation treatment in those cases with the internal treatments. There are a number of different places that do that, that sort of treatment. There are a number of different types of cancer you can treat with those.
You specialize in “External Beam Radiation Treatment.” What is that?
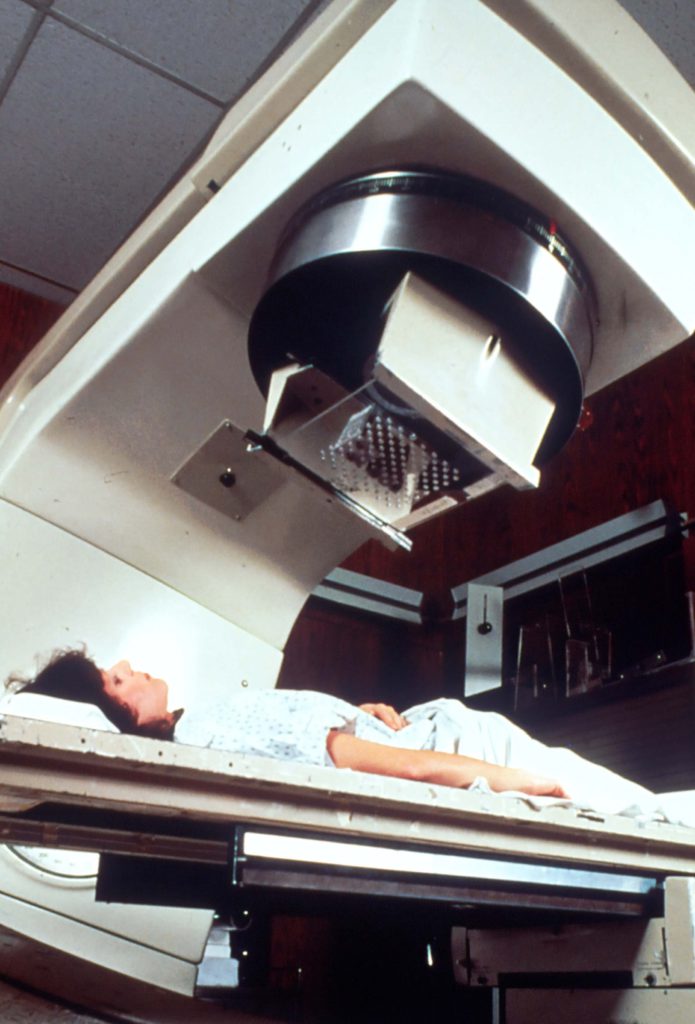
External beam radiation treatment is where it’s much like an x-ray machine. It shoots out of the end of a machine and it passes through the body and then comes out the other side of the body. That’s what I specialize in.
I talked a little bit before about some of the quality assurance measures that we do. Things we do to help localize the tumor. We put sometimes little marks on people’s skin. Those can either be a little tattoo or be less permanent marks we put on the skin.
With those marks it’s just quality assurance. It helps us line up initially for where we’re going to give the radiation treatment. But then we almost always do an X-ray as well so we can see internally where we’re treating with the radiation treatment before we get started with the radiation.
How do you protect other organs during the radiation treatment?
For example, with the heart, particularly for a breast cancer patient with left-sided tumors, here in my clinic we do something called a deep-inspiratory breath hold where we have the patient take a deep breath, they hold it, and we give the radiation treatment while they’re holding their breath.
What that does is inflates the lung so that pushes the heart both further away from the skin and further down in the chest. That pushes the heart out of the way of the radiation treatment. By doing that, we can really decrease the dose of radiation to the heart. It’s one way we’ve been able to really make improvements.
We do other things that are similar to that with prostate cancer. There are some gels we can put in to help push the rectum further away from where we’re treating.
We’re also with our radiation treatment machine, we’re really good at shielding different parts of the body and helping prevent too much radiation from getting to those other areas in the body.
How do you protect the patient from radiation exposure to healthy parts of the body?
We do that planning scan so we map things out and we make sure that we’re treating the tumor or the tumor bed, and that we’re not treating other areas. Within the machine there are some lead shields that we use called “leaves” in the machine head. They prevent the radiation from going to areas in the patient that we don’t want to. We also sometimes use different sorts of shields on the body surface but most of the time we don’t do that.
For the workers, there’s some lead and other types of shielding between them and the machine. We also wear a badge here in the clinic for the workers to make sure we aren’t giving radiation. The room and the building is made so there’s almost no radiation treatment escaping the building. The shielding around the room where we give the radiation treatment doesn’t allow that.
Can patients bring family or friends to the radiation therapy treatment?
The answer to that is always no. They can’t come in for the radiation treatment because we want to protect them.
Is there risk of a patient exposing those around them to radiation after their treatment?
For the types of radiation treatment that I’ve explained, the answer to that is no. The radiation goes through your body, it passes through you, as soon as the machine is turned off or that seed is taken out of your body, there’s no more radiation.
Sometimes we give radiation in either a pill form or some sort of liquid form. The most common reason for doing that is probably thyroid cancer. In those cases you do have to avoid being around people for a certain amount of time. Depending on the dose that you get, that can vary a little bit.
Same thing with some internal seeds that we leave in for things like prostate cancer. Sometimes you can’t hold a baby on your lap or something like that if you have a permanent in-dwelling seed that emits radiation treatment.
Relationship with Patients
How many patients do you see in your clinic?
On a daily basis here in Salinas I probably have 30-35 patients getting their treatments. Those patients are usually in intervals of every 15 minutes or so. We treat most of the working day here.
What are the differences between the experience at a mid-level size clinic like yours compared to smaller and bigger clinics?
Some places, in a smaller community, they don’t treat nearly as many patients. They treat maybe half the day, just the morning. Other places that I’ve worked out, large academic centers, we had 14 different machines and they were all treating 35 patients a day on those machines so it can be really busy.
The difference here is that I’m a generalist for radiation treatment. I treat every site. I love that, I really love treating all the different sites. Before when I was working at an academic center I would just specialize in certain types of cancer and my specialty used to be female gynecologic malignancies. I still treat female gynecologic malignancies but I don’t specialize in that anymore.
What can a patient expect during the radiation treatment process?
I try and have my patients come see me before they start any of their other treatments. Often times they’ll be having surgery or chemotherapy before they’re getting ready to do the radiation treatment.. They do that or sometimes we save that until after the radiation treatment, as well.
But with the radiation treatment they’ll visit with me, we’ll do a planning treatment scan. With that scan, I can map out where the radiation treatment is going to be given to. I can map out the areas we’re trying to avoid treating. We come up with a plan, there are different ways of doing that. There are a bunch of really technical names for that called IMRT or inverse planning for radiation treatments, intensity modulated radiation treatments, and we also do stereotactic radiation treatments here.
We go through the plan which can take anywhere from a day if it’s a very simple plan or it can take up to a week or even longer depending on how complex the plan is for planning.
They come in on the first day of treatment. During that week we’re also doing some quality assurance testing and we do some of that as well when the patient first comes in. So that first day of treatment usually takes a little bit longer, maybe a half an hour as opposed to fifteen minutes for all the other treatments.
Everyday is the same. Radiation treatment takes about a minute or two to give. You come in, you feel the same after the treatment as you do before the treatment with some very… there are some cases where you can have a little bit of nausea perhaps after the treatment, about an hour or so after treatment but that’s pretty rare and only has to do with treatments for the stomach.

The first radiation therapy session is actually a simulation
It’s not a treatment, it’s a simulation where we map out where the tumor is or where the tumor was if they’ve already had surgery, where the tumor can sometimes spread to or is most likely to spread to.
I also map out where the normal tissues are so we can direct the radiation treatment and point it at the area where we want to treat and we can avoid treating those other normal organs, as best as we can. We usually do a really good job of that.
How often do patients typically see you?
I meet with them initially. When they start the radiation treatment I see them at least once a week.
If they start to have any problems or any side effects of radiation I see them more often than that, as often as they need to during their treatment.
After they’re done, between myself and the medical oncologist and surgeons, we have a set schedule for when we’re going to see the patients.
That really depends on what type of cancer they have. What the likelihood of that cancer coming back is.
What are the most common cancer patient questions about radiation?
The most common questions that I get from patients are what are the side effects going to be?
And it’s really hard to answer that question without knowing what type of cancer you have and where that cancer is in the body, and what other organs are going to be next to it.
I think that’s a great question and a question that every patient needs to ask their physician.
The other questions are how well is the treatment going to work? How good is it? We don’t give radiation treatment unless we think the benefits are going to far outweigh the risks of the radiation treatment. That depends on what type of cancer you have, what stage the cancer is at, what the reason for giving the radiation treatment is. A lot of my patients will ask me what are the chances of curing the cancer. Depending on what type of cancer that is I can give an answer.
A lot of times I give radiation treatment to help with symptoms as opposed to helping to cure the cancer.We treat some patients who we’re trying to help them feel better if they have metastasis into their bone or into their brain, we give radiation treatment to help prevent the pain or the other things that are going on from the cancer. Those are probably the most common questions I get.
Unfortunately, it’s not like a certain type of chemotherapy where you already know what the side effects of that chemotherapy are going to be. It really just depends on where the radiation treatment’s given. That’s what determines what the side effects are going to be.
Can patients work through their radiation therapy treatment?
I have a lot of patients who are office workers. They generally can work straight through the radiation treatment.
I have some patients who work out in the fields, as well. In some cases I’ll tell patients to stop working but it’s not really the radiation treatment itself that makes it so they can’t work, it just depends on what they’re doing and how physical their work is.
Ask An Oncologist
Dr. Christopher Weight, M.D.
Role: Center Director Urologic Oncology
Focus: Urological oncology, including kidney, prostate, bladder cancers
Provider: Cleveland Clinic
…
Doug Blayney, MD
Oncologist: Specializing in breast cancer | HER2, Estrogen+, Triple Negative, Lumpectomy vs. Mastectomy
Experience: 30+ years
Institution: Stanford Medical
…
Dr. Kenneth Biehl, M.D.
Role: Radiation oncologist
Focus: Specializing in radiation therapy treatment for all cancers | Brachytherapy, External Beam Radiation Treatment, IMRT
Provider: Salinas Valley Memorial Health
…
James Berenson, MD
Oncologist: Specializing in myeloma and other blood and bone disorders
Experience: 35+ years
Institution: Berenson Cancer Center
…








Leave a Reply