Stage 4 Bowel Cancer to No Evidence of Disease: Nina’s Honest Experience
When Nina first began noticing changes in her body, she never imagined they would lead to a stage 4 bowel cancer experience. A busy mom of three in Leeds, Yorkshire, England, and a longtime hairdresser, Nina had always seen herself as “the healthy one.” She was active, into Pilates, and focused on holistic wellness. For years, her digestive issues were labeled as irritable bowel syndrome (IBS), even as her discomfort escalated and new symptoms appeared, including skin flare-ups and blood and mucus in her stool. In the middle of the COVID lockdown, she pushed through the pain, assuming it was just another rough patch.
Interviewed by: Carly Knowlton
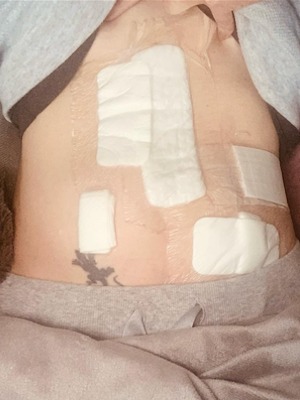
Everything changed around Mother’s Day 2021, when severe, localized pain and dark stool led to an urgent trip to the accident and emergency (A&E) department. Imaging revealed a mass in her bowel that had spread to her ovaries and suspicious spots elsewhere, leading to a stage 4 bowel cancer diagnosis. Nina underwent major surgery to remove part of her bowel, both ovaries, and a section of her bladder. She was placed on chemotherapy as “mop-up” treatment, but the treatment regimen hit her hard. She lost a significant amount of weight, needed total parenteral nutrition (TPN) and fluids, and scans then showed new liver spots. One doctor told her the liver disease was inoperable and brought up palliative care.

Nina refused to accept that as the end of her stage 4 bowel cancer story. Anchored by her three children and her belief that it wasn’t her time, she focused on everything within her control — nutrition, movement, supplements, prayer, and making keepsakes for her kids in case she couldn’t be there in the future. Her oncologist adjusted her chemotherapy schedule, and follow-up scans showed the liver lesions shrinking. Surgery later revealed those lesions had turned into dead tissue, with no active cancer remaining, leading to a discussion of having no evidence of disease that felt surreal and almost too fragile to celebrate.
Today, Nina’s experience is about more than clear scans. She talks openly about the anxiety, hypervigilance, and survivor’s guilt that followed treatment, including becoming more of a hermit, fearing certain foods and products, and feeling like she has to make every moment count as a parent. Meditation, Pilates, daily movement, and making her own skincare have become part of her ongoing healing. Nina’s stage 4 bowel cancer experience may be uniquely her own, but her message is universal: hold on to hope, listen to your gut, and remember that you are not a number.
Watch Nina’s video or read the edited transcript below to find out more about her experience:
- Early symptoms of bowel cancer can be mistaken for IBS, so persistent red flags like blood and mucus in stool or severe new pain should be taken seriously and re-evaluated
- A “no” from one clinician, including talk of palliative care only, doesn’t have to be the end of the story, seek a second opinion
- Asking questions and revisiting treatment options can sometimes open new paths
- Nina describes a meaningful transformation from constantly rushing and “pushing herself” to slowing down, honoring her limits, and prioritizing peace, presence, and time with her children
- Survivorship brings complex emotions, including anxiety and survivor’s guilt; getting support, sharing honestly, and finding a community of people who understand can make that phase more manageable
- Every person and every cancer experience is different; you are not a statistic, and there is value in focusing on hopeful stories as well as medical care.
- Name: Nina H.
- Age at Diagnosis:
- 38
- Diagnosis:
- Bowel Cancer
- Staging:
- Stage 4 (Metastatic)
- Symptoms:
- Longstanding IBS-like symptoms
- Skin flare-ups
- Blood and mucus in stool
- Dark stool
- Treatments:
- Surgeries: bowel surgery, removal of both ovaries, partial bladder resection, liver surgery with removal of two liver sections
- Chemotherapy
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Meet Nina: An Active Mom, Hairdresser, Pilates Lover
- First Red Flags Before Diagnosis
- Trip to A&E and Getting the Stage 4 Bowel Cancer Diagnosis
- First Chemotherapy Plan and Sudden Liver Metastases
- Refusing to Accept Palliative-Only Care
- Adjusting Chemotherapy Regimen and Shrinking the Liver Tumors
- Life Before Cancer: Extremely Active and “Didn’t Fit the Box”
- Telling the Kids and Parenting Through Chemo
- Side Effects of Chemotherapy
- Anxiety, Hypervigilance, and Becoming More of a Hermit
- Finding a New Mental Balance and Avoiding Doom-Scrolling
- Hearing “No Evidence of Disease”
- Major Surgeries and Surgical Menopause
- Recovery and How Long It Took to Feel Like Herself
- What Survivorship Feels Like Now
- Being “The Strong One” and Finding Community
- Making Keepsakes for Her Kids
- Meditation, Movement, and Lifestyle Changes After Cancer
- Advice to Others
- Final Reflections and Listening to Your Gut
Meet Nina: An Active Mom, Hairdresser, Pilates Lover
I’m Nina. I live in Leeds in England. I was diagnosed with stage 4 bowel cancer in 2021.
I have three kids, so they take up a lot of my time. I’m very passionate about my family time and all those kinds of things. I’m very into my Pilates and holistic side of things. I am a hairdresser by trade as well, so that’s what I did before. I’m back doing that part-time.
First Red Flags Before Diagnosis
I suffered with IBS for years, or what they thought was IBS. It was during the COVID lockdown where things progressively got worse, to the point where the discomfort was becoming more and more. I was having skin flare-ups and everything. Then I started having blood and mucus in my stools.
I contacted the doctors and they were like, “Come in.” It was lockdown, so it was difficult to get an appointment. I got in for some tests, but I never asked what they were testing me for or what tests they were doing. When the results came back and everything was fine, they were just very much like, “Oh, it’s just IBS. Maybe cut out certain foods and see yourself what things are bothering you,” so not much help at that point.
Then things got a little bit better. I started cutting stuff out of my diet. I did the York Test to find out what I was allergic to and what I might be intolerant to, and I cut a load of stuff out of my diet. That was in the summer of 2020, mid-lockdown. By Christmas, things did get worse.
I woke up the day before Mother’s Day 2021 in severe pain, but I got myself through the day. I thought, “It’s just a bad spout; ignore it.” But the following morning, I was very concerned, because my stool was dark. The pain was horrendous. It was down one side.
Trip to A&E and Getting the Stage 4 Bowel Cancer Diagnosis
We thought it was best to phone 111 and see what they recommended. They told us to go to A&E, and that’s where it all started. While I was in, I thought I’d be out later on and that it’s fine and it’ll be nothing.
They scanned me and everything, and the doctors came to see me and they were like, “We think it’s a twisted ovary or something like that. We’re going to keep you overnight and do a few more tests in the morning.” That was fine. The following morning is when the doctors came to see me and said, “We’ve had a better look at your scan and you’ve got a mass on your bowel that’s spread. It looks like it’s gone to your ovaries, and you’ve got two other spots that we’re concerned about,” one on your liver and one in my chest.
They said, “We think it’s cancer and we need to get looking now and get you in.” Basically, they kept me in while they did all the other tests to see what everything was. It was confirmed that what was in the bowel was cancer, and they were certain that it had gone to my ovaries. The scans on my liver and chest all came back clear at that time.
They sent me in for an operation six weeks later. I went in for my operation. They removed part of my bowel. Luckily, they were able to put it back together and I didn’t have to have a bag. Then they took both ovaries just to make sure. While they were in, they did notice something on my bladder, so they had to take a little bit of my bladder too. But they felt like they did quite a good mop-up job and thought that was it.
First Chemotherapy Plan and Sudden Liver Metastases
They decided to put me on six sessions of chemo, three weeks apart, as a bit of a mop-up just in case. But that didn’t go to plan. I fell ill on the chemo, to a point where again I ended up being taken in. I’d lost a lot of weight, and they thought I had an obstruction.
They scanned me for that and had to keep me in. I was put on TPN and fluids because I couldn’t eat or drink. The scan revealed that I had two spots on my liver.
At this point, when the guy came to see me when I was in — again, it was COVID, so we didn’t have many people that were allowed to come in — the doctor came to see me and asked if my husband could come the next day to discuss the results. So you kind of know that there’s something.
The next day, he came and the doctor told us they’d seen these two spots that, in his eyes, weren’t operable. He basically just said that he’d get the palliative care team to come and see me.
Refusing to Accept Palliative-Only Care
From that point on, it was like, “Right, I’m not taking that as an answer. I’ve got three kids. I don’t think it’s my time. I’m a healthy eater. I’m going to up my game. I looked into every bit of food that I could possibly think of that would help me heal my body and fight the cancer.”
That was my aim: to get out of the hospital and just crack on with that. I was busy making things for the kids while I was in the hospital so they had something of mine. You sit there and think about things you might say to your kids at different stages of life. I was preparing myself for things to write down, to be able to give them if I wasn’t around. I’d probably say that was the darkest point of my journey, really.
After, when I did get out, when I put a bit of weight back on and was allowed back out, they were ready to decide whether to do the chemo again. They decided that my oncologist, who didn’t see me in hospital because it was somebody else, still thought the chemo was working. But he did change how he was administering it.
Adjusting Chemotherapy Regimen and Shrinking the Liver Tumors
Rather than just going in and having the drip and then having tablets for a week, I’d go in every two weeks for a drip and then I’d come home with another little drip on. Then we’d see how I went halfway through and scan me.
The liver bits had actually shrunk, so he was happy with that. They kept me on for the rest of the program, and they were hoping that if they’d shrunk enough, they’d be able to operate. At the end of it in the October, they left me for a few months just to heal, and then they scanned me and they were right — the lesions had shrunk and they were happy to operate. There didn’t seem to be any more spread anywhere else.
It was February 22nd when they decided to remove the bits from my liver. They were very shocked by what they found when they tested it. It was all dead tissue. There was no active cancer there. It had completely died. They were basically like, “Whatever you’re doing, keep on doing it.”
That’s what I’ve been doing since and all my scans have been clear. I’ve been very lucky. I do put it down to what they did, and I put it down to my diet and all my praying and crying. I did say at the very beginning, it wasn’t my time. It will be five years next year, but it does feel like it was only last week. I don’t think it will ever fully go.
Life Before Cancer: Extremely Active and “Didn’t Fit the Box”
I was a busy mum of three. I worked in hairdressing full-time. Because it happened after lockdown but before things were fully back to normal, I was a busy mum with three kids. I trained. I did silly winning competitions, like the mud races and all that. I loved all that. I weight trained. I was very active and very healthy but probably pushed myself a little bit too much.
It was a bit of a shock because I was a healthy eater, I trained, I worked out, and I was very active. I had three kids, so I was constantly running around after them. It was a shock because I didn’t put myself in that bracket. I think that’s what the doctors didn’t do at first. They thought, “She’s healthy. She eats well. She trains.” I never went on about being tired because I’m a mum of three. I’m always going to be tired.
I was a very active person. I was always quite a positive person beforehand, but I do think I took life a little bit for granted. One of the positives that has come out of this is it has made me look at life a bit better and slow down and appreciate the little things.
Telling the Kids and Parenting Through Chemo
We didn’t want to name it because I’d had some problems for years. We didn’t tell them it was anything. We didn’t say cancer. We didn’t want them to hear that word and be scared, so we kept it quiet. After my operation, I lived with my parents for six weeks while I healed, but the kids could come and see me. We tried to keep everything as normal as we could.
When chemo started and I fell poorly, I think it was because I was hiding it. Every time I felt bad, I didn’t want them to see me like that, so I was dealing with it on my own. Trying to feed myself and all that was hard. When palliative care came into it, we had to tell them the truth.
They’re quite strong characters, so they never asked us the worst. You don’t want them to ever go, “Are you going to die?” They didn’t ask that. I think that’s because my husband and I are quite positive people. We don’t look for the negative. We always look for that little silver lining, and I think that helped.
With it being lockdown, they never saw me in the hospital. They never saw me poorly in a hospital bed with tubes or anything like that, so I think that helped them. I have a good team around me. The family is great.
Side Effects of Chemotherapy
I think I did two or three the first time around, and then they changed it. It was either six or eight the second time around. I think it was six. My husband thinks it was eight. I can’t quite remember. I didn’t lose my hair, and again, I think that helped with the kids because my youngest one doesn’t think I had chemo. He’s like, “You didn’t lose your hair, Mummy.” I was like, “Mummy did.”
The sickness and the tiredness got worse with each round. But I think because I had such a healthy diet, I was always in the mindset of, after every chemo, I need to heal myself for the next one. I juiced. I did everything I possibly could so that the chemo would have another good go at doing what it needed to do.
I never want to feel like that again. I dealt with it, and I do feel like I dealt with it well, but I’d never want to go back there. I had this weird cold thing. I couldn’t touch certain things. I couldn’t touch knives and forks. I don’t know what the name of that is. I couldn’t drink anything below my body temperature; otherwise it would feel like it was locking my throat. Apart from those side effects, I was quite lucky.
Anxiety, Hypervigilance, and Becoming More of a Hermit
I’ve become a little bit of a hermit. I do lock myself away a bit because a lot of things do scare me now. I felt like I was so healthy beforehand and I would not have expected anything like that, so I don’t socialize as much as I used to.
I’m too scared to drink, even though I didn’t drink before. Going out and being in that social environment, I get quite anxious. Same with the kids: whatever they eat, whatever they drink, I’m very conscious. I make all my own skincare range because I’m too scared to put anything on my skin that I don’t know what’s in it, so I have become a little bit of a nervous wreck.
Each year, I have gotten better, and every time I get a clear result, it gets a little bit easier. I’m working a bit more now, so that’s helping. But I think getting over the mental side has been the hardest. The physical side, I’m more or less back to the way I was, but the mental side is taking a bit longer. I meditate. I also don’t read or look up things too much now. I’ve cut that down a bit and just try to be a bit more present.
Finding a New Mental Balance and Avoiding Doom-Scrolling
I know I’m healthy. I’m doing everything right and just stick to the positives. We’re in a world where you can overlook stuff. The more you look up stuff, the more you see the negative than the positive.
Doing something like this is trying to put that positive out there. I’ve got a positive story. I had a positive outcome, to say how stage 4 bowel cancer had gone so many places. I’m lucky to be where I am, because we did have a neighbor who was also diagnosed at the same time as me who didn’t get through it, so it does make you count your lucky stars a little bit that I’m still here.
As much as I lock myself away, I’ve been given that chance to live again. I drive the kids potty because I want to make every second count, every memory count, and they’re like, “I just want to be a teenager.”
What I’ve found on this journey is that when you’re in the treatment and your surgeries, you’re fighting the fight. Then when you’re finished and the doctors go, “Yep, fine, see you in a year,” you feel very much left and quite vulnerable. Any little twinge or anything, I feel like I have to phone them and go, “Just please check it. Just make sure that it’s nothing.” They are understanding of that. They know that they told me I was fine before, so I don’t always take their word for it. But again, that is getting better.
Hearing “No Evidence of Disease”
I was with my mum. She came with me to the meeting to see the oncologist, for him to say, “There’s no evidence of disease and we’re just going to put you on monthly checkups.” That was it.
I didn’t want to celebrate it. I didn’t know what to do because we walked out of the meeting, and then my mum looked at me and went, “Are you happy? Are you happy?” I went, “Yeah, but I don’t feel like I can enjoy it. I feel like if I laugh in its face, it might come back,” so it was a bit of a surreal moment.
I didn’t want to go out and start screaming, “It’s gone! I’m free from it,” because there’s always that what if. I always have to mentally have it there and prepare myself to hear those words again, so I didn’t feel like I could just jump for joy.
Major Surgeries and Surgical Menopause
They removed part of my lower bowel, both my ovaries, and a section of my bladder where there seemed to be some disease. That was the first surgery. They did all that and “had a good rummage,” they said, and looked at everything else. They didn’t see it anywhere else, just those things.
They did put me into surgical menopause with that. That’s probably been another battle in itself, just getting over the surgical menopause. I thought it was going to be moods and hot sweats. I wasn’t expecting the joint problems, brain fog, and all that, because my brain does not work like it used to either. That’s another thing, but I won’t put that down to the chemo; I’ll put that down to my hormones.
The second surgery was just my liver. They took two sections of my liver, but at the same time found scar tissue that had caused the bowel obstruction. They did all that at the same time. It was a good six weeks, maybe a bit longer with the second. I don’t know why, but physically, it took a lot longer. Six weeks until I felt more like myself.
Recovery and How Long It Took to Feel Like Herself
I don’t think you realize how much you use your core. The taking of the organs didn’t seem to bother me. Everything worked fine. I was lucky because I didn’t have to have a bag, so I think that was a big help.
I heal pretty well. I do bounce back pretty quickly. The first surgery, I was six weeks and straight into chemo, so we never really knew what was causing problems — whether it was the chemo, still getting over the surgery, or going through the menopause. A lot of things at that point were masked.
The second surgery, again because it was the same kind of surgery, it was another six weeks until I could physically do the basics. I was just happy to be here, to be honest. I just took my time. I’ve got an army of people around me, so I just took my time and didn’t push myself, because they all know what I’m like. I can try and jump in too soon, hence my mum keeping me for six weeks every time.
What Survivorship Feels Like Now
It’s a strange one because you don’t want to take anything for granted. You want to live your life to the full, but at the same time, you’re scared. You’re scared of hearing those words ever again. Then you get the guilt. There’s a bit of guilt there, going, “I shouldn’t be scared. I should be going for it.”
Then there’s this survivor’s guilt. The amount of people who I knew that didn’t make it through, you do question, “Why me? Am I not doing enough? Am I not living my life? Are they going to think I’m not living my life to the fullest?” It’s a strange one. People think you should be jumping up in the air and celebrating it, but you’re just scared to hear those words again.
From the beginning, when we found out it was stage 4 bowel cancer, it was, “I’m not going to be here for my kids.” You sit and plan all the things that you might say through each milestone of their life. You never forget that feeling, and you don’t ever want to feel that feeling. So surviving it, you do want to make the most of life, but it’s hard. It’s hard.
Being “The Strong One” and Finding Community
I have a very good unit, and I am the positive person everyone comes to. They’re like, “You’re not the one who’s supposed to break. You’re the one who’s supposed to hold everyone together.” As a family, we all saw it as: if anyone’s going to get through it, it’s Nina. She doesn’t go without a fight. That’s kind of how it was.
Survivorship is one of those things you don’t understand unless you’ve had those words. I was very open on my Instagram about my story and what I was going through, just in case it reached anybody else that was fighting. I have met some lovely people and made some close friends who are either going through it now or went through it at the same time as me.
You have that little community where you’ve got a little secret wink of, “I know how you’re feeling,” kind of thing — and you need that. As much as your family love and care for you, they don’t quite understand. There needs to be support for them as well, because they don’t quite understand that being scared of what’s coming, especially when you think that that is it.
It feels like it’s just a matter of weeks or months or something. I can’t even explain that feeling. I’m not saying it’s any easier when you haven’t got kids, but when you have kids, you think you’re never going to see them do certain things in their life. You have kids because you want to see all that.
Making Keepsakes for Her Kids
I made some little knitted mice. I think one of my sisters must have bought me a kit. I made one for each of my kids. I think I did some for my mum as well. When I was in the hospital the second time round, when I was poorly in between my chemo, I made them all little bookmarks — something that I’d made and touched so they could have something.
I wanted them to have something that would remind them of me if I wasn’t there. I just wanted them to have something that I’d made. I’m not very good at knitting. They’ve still got them.
Meditation, Movement, and Lifestyle Changes After Cancer
I meditate. I’ve got better at it because I was not very good at it at first. I have a very busy head. I do lymph drainage, a body tap. I have a trampoline in my back garden that I bounce on every day.
I do Pilates. I don’t lift weights like I used to. I don’t put my body under that much stress because I believe stress was a big cause of my cancer. I do meditation, Pilates, moving my body in general without pushing myself, and walking. We have a dog now. Once I knew that I was okay, just being outside in the fresh air has helped.
I eat extremely healthily. I eat more of a vegan diet, but I just think as long as you’re eating good food, not processed, stick to that. I do supplements, but I think in general it’s just reading your body. If I’m tired, what can I do to help my body? Meditation has been great for my head because that is one thing I do struggle with.
Everything I use on my body, I make, like my own creams and stuff. My kids aren’t the biggest fans; they’re getting used to it. Pilates and meditation have been the main thing for me right now.
Advice to Others
I think all cancers kind of come to the same thing. You’ve just got to hold on to hope, no matter what the diagnosis is. We are not a number. Everyone’s unique. I always say: don’t Google.
Look for the positive stories. I was never one to go and look at negative stories. There are some great books out there. “Radical Remission” was one of the books that I read that was just a game changer for me, because it had so many positive stories and outcomes in it.
You’re not saying you look for the negative, but the negative stuff comes up pretty easily, so don’t look for that. What I tell the people that have contacted me is: everyone’s journey is different. I’m not saying the younger ones or the older ones are any different, but don’t put yourself in any kind of box.
I just had hope. I told my oncologist, I’m here till I’m 96, so I’m not that easy to get rid of. You do have to take it into your own hands a little bit. The doctors can do what they can do, but don’t just leave it to them. There are so many things that you can do for yourself, whether it’s healthy eating, meditating, or moving.
Moving is a big one. Don’t just crumble, as much as it’s so hard. Speak. Tell people how you feel. Even if you think they don’t want to hear it or they’re too scared to hear it, it’s better out than in. If you can’t speak to the loved ones about it, there are people out there that will talk to you. Macmillan is amazing.
You’re not alone, because it is a very lonely place. It is a very, very, very lonely place. That’s what I told my father-in-law, actually. He was diagnosed this year. He’s a big guy, very proud. I just remember holding his hand and saying, “You’re not alone.” I said to my husband, “I want him to know that he’s not alone, because as much as you put a brave face on, it was a very dark and lonely place, especially when you feel that people don’t understand.” You’re not alone.
Let’s have hope and just find your little community to talk to.
Final Reflections and Listening to Your Gut
It’s tricky because, like I said, we aren’t a textbook, so everyone’s different. As I’ve said to anybody who’s spoken to me about what I did or things I might have taken, you’ve got to find your own path. You can take advice from everybody, but don’t do anything that doesn’t feel right.
I always went with my gut. If something in my gut took me in that direction, I would follow that. But if people were advising all sorts and I had a doubt, I wouldn’t go down that route. Tune into yourself and figure out what’s right for you.
Do what you can do for yourself and not just leave it to the doctors, because the doctors can only do what they can do. They are amazing. I had some amazing people at the hospital. I’ll never forget their faces and their names. But at the same time, I did take control of it myself for certain things. Everyone’s journey is different.

Inspired by Nina's story?
Share your story, too!
More Metastatic Colorectal Cancer Stories
Raquel A., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Frequent bowel movements, pin-thin stools, mild red blood in stool
Treatment: Chemotherapy
Steve S., Colorectal Cancer, Stage 4 (Metastatic)
Symptoms: Blood in stool, changes in bowel habits, feeling gassy and bloated
Treatments: Surgery, chemotherapy, monoclonal antibody, liver transplant
Jessica T., Colon Cancer, BRAF+, Stage 4 (Metastatic)
Symptoms: Severe stomach cramps, diarrhea, vomiting, anemia (discovered later)
Treatments: Surgery (hemicolectomy), chemotherapy
Jennifer T., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Weight loss, coughing, vomiting, sciatica pain, fatigue
Treatments: Surgeries (colectomy, lung wedge resection on both lungs), chemotherapy, immunotherapy
Kasey S., Colon Cancer, Stage 4 (Metastatic)
Symptoms: Extreme abdominal cramping, mucus in stool, rectal bleeding, black stool, fatigue, weight fluctuations, skin issues (guttate psoriasis)
Treatments: Surgeries (colectomy & salpingectomy), chemotherapy