The Reality of Platinum Resistance: Alicia’s Ovarian Cancer Story Framed by a Medical Expert
Alicia’s stage 3C ovarian cancer experience began during what should have been a season of joy. She had a thriving hairstyling career and a roller derby community, and had recently gotten married. Around the time of her wedding and honeymoon, her period stopped for a year and then returned as nearly two years of daily bleeding, sometimes so heavy she had to use adult diapers that she had to change every five minutes.
Edited by: Katrina Villareal
She also developed high blood pressure, a persistent cough, bloating, and lower back pain, but a normal Pap smear and the timing of midlife led her to assume that it was perimenopause.
To help place Alicia’s experience in medical context, we spoke with Dr. Ursula Matulonis, chief of the Division of Gynecologic Oncology at Dana-Farber Cancer Institute in Boston. According to Dr. Matulonis, Alicia’s experience is unfortunately not unusual. She explains that most high-grade serous ovarian cancers present at stage 3 or 4, often starting in the fallopian tube and spreading silently through the abdomen.

It took a full year before Alicia found a specialist. She tearfully asks herself now, “Why didn’t I think it was cancer?” The specialist initially suspected endometriosis after seeing uterine polyps. A procedure to remove them gave her just 24 hours before the bleeding resumed. Multiple emergency visits followed, and the biopsy came back as precancerous, not cancer. Everything changed when her doctor reviewed her scans and told her, “You have cancer. You have two cancers,” then arranged for her to be admitted that day for emergency surgery the next morning. Alicia was diagnosed with stage 3C ovarian cancer and stage 1 uterine cancer.
During surgery, Alicia’s team found what the surgeon called a “hot mess”: an enlarged, inflamed, partly decaying uterus and large ovarian cysts that required an open incision and a total hysterectomy. After a week and a half in the hospital, she returned home to recover, then had a port placed and started chemotherapy. At first, her stage 3C ovarian cancer experience seemed to turn a corner. Her tumors shrank, her numbers looked good, and she rang the bell at her last infusion. Within two weeks, however, the cancer was back —- and further testing showed that her disease was platinum-resistant.
Losing so much time to appointments meant she eventually lost her job and her insurance, forcing her to search for a center that could treat her through a charity program. She found that at Moffitt Cancer Center in Florida, where a leading OB-GYN oncologist reviewed her records, retested her samples, and explained that her cancer is rare, hormone-based, and not genetic, making treatments more limited and clinical trials harder to access, especially as a dual cancer patient with a new metastatic mass in her vaginal cuff. Even as the focus shifts to keeping the cancer stable and planning radiation, Alicia leans on her Buddhist faith and her wife for support.
Dr. Matulonis underscores how crucial it is to understand tumor histology and genetics such as BRCA status and markers like HER2 and folate receptor alpha (FRα) used to guide treatment decisions. She describes a rapidly evolving landscape of drugs and clinical trials and emphasizes that hope rests not in false promises, but in accurate information, shared decision-making, and matching the right option to the right patient at the right time.
Watch the video and read the interview transcripts below to know more:
- Heavy, persistent bleeding was attributed to perimenopause despite a normal Pap smear, highlighting how gynecologic cancers can be masked by common midlife symptoms.
- It took a year, multiple hospital visits, and a “precancerous” biopsy before she learned she had two cancers and needed emergency surgery the next day.
- After surgery and chemotherapy that initially appeared successful, the cancer returned within weeks as platinum-resistant disease, limiting treatment and clinical trial options.
- Transferring to a specialized cancer center provided access to financial assistance, additional treatment options, and clearer guidance about her diagnosis.
- Persistent or worsening symptoms deserve continued attention, even when early tests are normal or labeled “precancerous.”
- Finding emotional or spiritual grounding, such as Alicia’s Buddhist practice, can help patients navigate repeated setbacks and uncertainty.
- Dr. Ursula Matulonis emphasizes that alongside resilience, evolving science and individualized care offer meaningful pathways forward for many patients facing ovarian cancer.
- Name: Alicia N.
- Age at Diagnosis:
- 42
- Diagnoses:
- Ovarian Cancer
- Uterine Cancer
- Staging:
- Stage 3C (ovarian cancer); stage 1 (uterine cancer)
- Symptoms:
- No menstrual cycle for one year, followed by almost two years of daily bleeding
- Large blood clots
- High blood pressure
- Random cough
- Bloating
- Treatments:
- Surgery: total hysterectomy
- Chemotherapy
- Radiation therapy (planned)


Thank you to Corcept Therapeutics for their support of our independent patient education program. The Patient Story retains full editorial control over all content.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
- Alicia’s ovarian cancer and uterine cancer story
- Life before cancer and personal background
- Early symptoms around the time of my wedding and honeymoon
- Perimenopause assumptions and worrying symptoms
- Honeymoon bleeding crisis and search for a specialist
- Not considering cancer at first
- Emotional reflection on delayed suspicion
- Delay in finding a specialist and ongoing bleeding
- Polyp removal, ER visits, and precancerous results
- Emergency diagnosis of two cancers
- Ursula Matulonis, MD explains ovarian cancer in detail
- Alicia's Radical hysterectomy and recovery
- Dr. Matulonis explains diagnosis, staging, and upfront treatment strategy
- How Alicia learned about platinum resistance and impact on her work
- Dr. Matulonis on platinum sensitivity, platinum resistance, and reuse of platinum
- What are Antibody-drug conjugates and folate receptor alpha
- Alicia on a new metastasis, her faith, and hope for the future
- "Office Hours" with Dr. Matulonis: Side Effects, Scans, and Smarter Treatment Decisions
- Managing side effects, neuropathy, and bevacizumab risks
- Cure, remission, and long‑term planning
- Clinical trials, immunotherapy, and research progress
- Communicating scan results and tailoring treatment
- Role of specialists, community oncologists, and virtual care
- Balancing efficacy, toxicity, and patient priorities
- Hope, information, and shared decision‑making
- More Ovarian Cancer Stories
I thought I was perimenopausal because I was going a year without a cycle. Then all of a sudden, I had a cycle for almost two years straight.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient
Alicia’s ovarian cancer and uterine cancer story
Life before cancer and personal background
Hi, my name is Alicia, and I have stage 3C ovarian cancer and stage 1 uterine cancer.
I was a hairstylist before all of this. I was also on a roller derby team. I was active. I love animals. I have two dogs and two cats. I grew up on a farm. I have a beautiful wife, and we’ve been married for three years. I was also an Army brat, so that was a big thing because I moved all over the place. I had a Japanese grandmother, so I have my Japanese background.

Early symptoms around the time of my wedding and honeymoon
I had just met my wife. I was into my career and had started having an awesome clientele. I was on a roller derby team, getting active, about to start bouting, and everything. Then I met my wife, and we ended up getting married. That’s when my symptoms were the heaviest, when the wedding happened.
I thought I was perimenopausal because I was going a year without a cycle. Then all of a sudden, I had a cycle for almost two years straight, every day, not even 24 hours of being free of it. Then I started having more symptoms added on to that.
What concerned me was that during my honeymoon, I graduated to adult diapers and was going through those every five minutes.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient

Perimenopause assumptions and worrying symptoms
I thought it was due to perimenopause. The symptoms that came along with it got me worried because, all of a sudden, I had high blood pressure, which I had never had. I had this random cough. The only time I had a cough like that was when I used to get a bronchial cough during the winter, so I thought it was something similar. Then I started getting bloated and had lower back pain. The lower back pain I thought was due to work, because I stood all day long behind a chair.
I had my Pap smear done, and it came back normal. Around that time, I was questioning it. What concerned me was that during my honeymoon, I graduated to adult diapers and was going through those every five minutes. My wife was like, “Something’s not right. We have to get you checked.”
Honeymoon bleeding crisis and search for a specialist
We went to Siesta Key for the week. During that week, it was good — no bleeding. Then all of a sudden, on the last day, it kicked up. I had to get adult diapers plus overnight pads. It was not looking good. The clots were coming in handfuls, which was what was concerning. I started having pain as well, but I thought it was normal period cramps.
For the rest of the day, we couldn’t do anything. The good thing was that we were leaving the next day. I was concerned because I was like, “Okay, what’s going on?” That’s when I started Googling our local area for specialists, because I knew I needed to have somebody more than just a regular doctor.
Thinking back to before I was diagnosed, I asked myself, ‘Why didn’t I think it was cancer?’
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient
Not considering cancer at first
I just thought it was a hormonal issue. Cancer never crossed my mind. I thought it was probably severe menopause, something of that nature. The weird thing was that I wasn’t getting tired like you would think I would be, because of how much I was bleeding. It was the clotting that was causing me to worry, because I never had that problem. I never put two and two together — the symptoms I was having, along with the bleeding.
Emotional reflection on delayed suspicion
I never thought I would tear up, because I’ve shared it so many times. But thinking back to before I was diagnosed, I asked myself, “Why didn’t I think it was cancer?” You think you get over it after telling your story multiple times, but you never do.
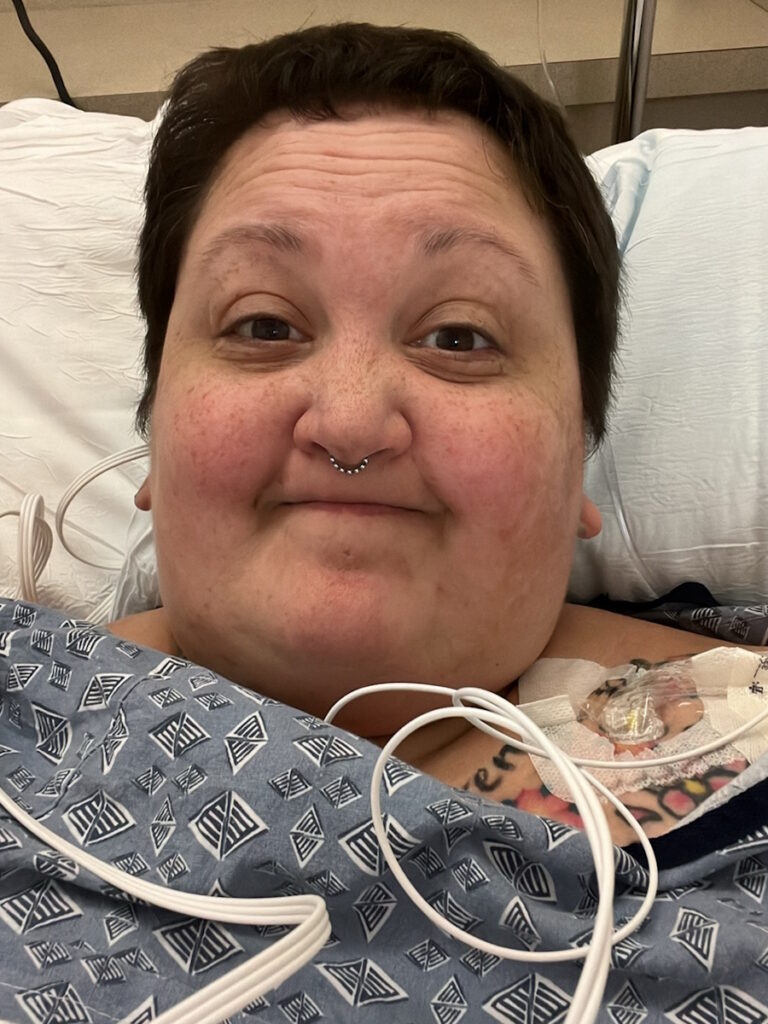
Delay in finding a specialist and ongoing bleeding
It took me a year to find a specialist. I don’t know why it took me so long. In my head, after that day, it was to see if it would go any longer, to see how the rest of the week would go — and it ended up being how the rest of the year would go — because I wanted to make sure I had something to tell the doctors.
At that time, I stopped doing roller derby. I just went to work and went home. After that year, I ended up finding a specialist. When I did, it was weird because they first thought I had endometriosis. I had a regular cycle all my life, so I never had endometriosis. They did a pelvic exam and saw polyps in my uterus, and that’s where it came up as being questionable for endometriosis.
On the day of my appointment, I went in to get my results to find out that I had two cancers and that I was getting admitted to the hospital to have emergency surgery the next day.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient

Polyp removal, ER visits, and precancerous results
They did a procedure to remove the polyps, which was supposed to stop the bleeding. I got 24 hours of no bleeding. After that, they said, “Okay, go to the hospital.” I probably had three to four hospital visits before I got an oncology referral.
The results from the biopsy of the polyps came back precancerous. It didn’t even come back as cancer. The hospital visits and finally seeing my doctor took about a month.
Emergency diagnosis of two cancers
When I saw her, she looked at my scans and said, “Yeah, you have cancer.” I was like, “What?” She said, “You have two cancers at that.” I was like, “Oh my gosh. Are you serious?”
She said, “Yeah, you have two cancers. It will take your insurance two weeks to approve the surgery, so I’m going to fit you into my schedule for tomorrow for emergency surgery. I’m going to admit you today so we can do the emergency surgery, because you need this taken out.”
I didn’t have time to process, because everything went so fast. On the day of my appointment, I went in to get my results to find out that I had two cancers and that I was getting admitted to the hospital to have emergency surgery the next day.
Alicia’s story continues below.
Ursula Matulonis, MD explains ovarian cancer in detail
Professional role and path into oncology
I’m Ursula Matulonis. My official title is chief of the Division of Gynecologic Oncology at the Dana-Farber Cancer Institute in Boston, Massachusetts.
I became interested in oncology when I rotated on an oncology ward while in medical school. I saw and understood the seriousness of oncologic diagnoses, which is what drew me into oncology.
Initially, I wanted to be a bone marrow transplant physician and take care of folks with acute leukemia. But when I started my fellowship at Dana-Farber, I had an eye‑opening experience with the world of solid tumors. At that time, there were very few individuals seeing patients with gynecologic cancers, so I moved, developed our program, and eventually joined the division at Dana‑Farber. It’s been a career‑long interest in oncology and, since fellowship, in gynecologic cancers.

I saw and understood the seriousness of oncologic diagnoses, which is what drew me into oncology.
Dr. Ursula Matulonis, Gynecologic Oncologist
How common is ovarian cancer and what makes it unique
It depends on how you consider rare because there are specific definitions, but there are about 21,000 cases of ovarian cancer in the United States per year. That number has been dropping, likely for several reasons: individuals pulling back on the use of hormone replacement therapy and better identification of individuals at higher risk of developing ovarian cancer, such as germline BRCA1 or BRCA2 mutation carriers who can undergo risk‑reducing surgery. That annual number now seems to have stabilized to around 20,000 to 21,000 cases.
There are many unique aspects of epithelial ovarian cancer. We used to think of it as coming from the surface of the ovary, but in a substantial number of cases, it probably comes from the fallopian tube, specifically the fimbria. In serous tubal intraepithelial carcinoma (STIC), a tiny cancer starts in the fallopian tube, and because the ovary is a neighboring organ, the cancer cells spread to the ovary and disseminate easily through the abdominal cavity. As a result, most patients with high‑grade serous ovarian cancer, which is the most common histology, present with stage 3 or 4 disease, meaning the cancer can extend from the pelvis all the way to the upper abdomen or even outside the abdomen into areas like the chest or supraclavicular lymph nodes.
When someone comes in with a new diagnosis of ovarian cancer, we take into account the stage of the cancer, the histology, and whether or not that patient can undergo upfront cytoreductive surgery.
Dr. Ursula Matulonis, Gynecologic Oncologist
The molecular aspects are also unique. High‑grade serous cancers often have homologous recombination deficiency (HRD), an abnormality in DNA repair that makes them particularly sensitive to platinum drugs. Tumors with a BRCA mutation — whether inherited (germline) or only in the tumor (somatic) — are especially sensitive to platinum. On the other hand, to date, high‑grade serous ovarian cancer has shown low sensitivity to immunotherapy, in part because it tends to have a low tumor mutational burden and is immunologically “cold,” so checkpoint inhibitors have had limited activity.
It’s also important to remember that other histologies — such as low‑grade serous, clear cell, low‑grade endometrioid, high‑grade endometrioid, mucinous tumors, and carcinosarcomas — have distinct biologies and genetic makeups. For example, low‑grade serous ovarian cancer can be very sensitive to hormonal therapies, especially aromatase inhibitors, while clear cell and mucinous tumors tend to be less sensitive to platinum.
Alicia’s Radical hysterectomy and recovery
I was scheduled for a full hysterectomy. She was trying to do it laparoscopically, but she couldn’t because my uterus was so enlarged and inflamed. She said I had a hot mess in there for her, so they had to make an old-school incision. Part of my uterus was decaying. My left ovary was 6 to 7 centimeters big, and my right ovary was 10 centimeters. The cyst on the ovaries was 10 centimeters. She had to scoop out as much cancer as she could.
After that, I stayed in the hospital for a week and a half to recover because they wanted to make sure that everything was okay. At that time, I was processing it a little bit more, and then it was, “Okay, after you get out of surgery, you will meet your oncologist in your town.” I was 45 minutes to an hour away from home, and they found an oncologist in my town to do treatment. After that surgery, I had to get my port surgery, which was about six weeks after my recovery. I started treatment the day after I got my port.
Treatment was going well… Everything was looking good... After a week or two, the cancer was back… They found out I was platinum-resistant.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient
First-line chemotherapy and initial response
The first chemo was doing well. I had rare side effects. I always have to have the rarest, I guess — go big or go home. I was tired, had a lot of bone pain, and a lot of neuropathy. I lost my hair, but other than that, I was fine. Treatment was going well, and everything was starting to shrink. My numbers were good. Everything was looking good.
When we got to my last treatment, they were like, “Okay, you can ring the bell if you want to, because your numbers are down to normal and everything is looking good.” I rang the bell. After a week or two, the cancer was back. When they looked at it and redid the genetic testing, that’s when they found out I was platinum-resistant.

Dr. Matulonis explains diagnosis, staging, and upfront treatment strategy
When someone comes in with a new diagnosis of ovarian cancer, we take into account the stage of the cancer, the histology, and whether or not that patient can undergo upfront cytoreductive surgery (CRS). If a patient is not feeling well, has a lot of ascites (fluid in the abdomen), fluid around the lungs, or other factors that make upfront surgery unsafe, we start with a biopsy and then use neoadjuvant chemotherapy — chemotherapy first. Typically, that means three cycles of chemotherapy, then reevaluation and surgery if feasible, followed by additional chemotherapy to complete about six total cycles.
When added to chemotherapy, bevacizumab can enhance responsiveness and sometimes keep cancer in remission longer, but it has its own side effects.
Dr. Ursula Matulonis, Gynecologic Oncologist
For high‑grade cancers like high‑grade serous, clear cell, high‑grade endometrioid tumors, and carcinosarcomas, the backbone chemotherapy is carboplatin and paclitaxel. Standard of care remains carboplatin plus paclitaxel. Aromatase inhibitors are being tested as frontline therapy for low‑grade serous ovarian cancer, which asks whether hormonal therapy might replace upfront chemotherapy in that subtype, but this is not the current standard of care.
We can also add bevacizumab to carboplatin and paclitaxel. Bevacizumab is a monoclonal antibody that targets vascular endothelial growth factor (VEGF). When added to chemotherapy, bevacizumab can enhance responsiveness and sometimes keep cancer in remission longer, but it has its own side effects, such as hypertension, potential kidney damage, wound‑healing problems, and voice changes. It does not appear to improve overall survival but can prolong the time the cancer stays in remission.
Molecular testing and PARP inhibitors
Alongside starting chemotherapy, I order molecular tests so we understand the tumor while we’re treating it. I typically do next‑generation sequencing (NGS) on the tumor to understand the genetic changes, and I also order homologous recombination deficiency (HRD) testing. HRD testing helps predict how sensitive the cancer will be to platinum and to PARP inhibitors.
There are two main HRD states: HRD (homologous recombination deficient), where PARP inhibitors can be considered, and HRP (homologous recombination proficient), where DNA repair is relatively normal, and PARP inhibitors used as maintenance is currently not allowed under FDA guidelines. In the setting of a BRCA mutation, PARP inhibitors can have a significant positive impact on outcomes and are an important part of maintenance strategies.
I also routinely order HER2 testing and folate receptor alpha (FOLR1) testing by pathology. This is important because if a patient goes into remission and then relapses — particularly with a short remission — we may use these markers to choose antibody-drug conjugates (ADCs) or other targeted therapies in the recurrent setting.
Even in platinum‑resistant settings, after some time off, reusing platinum can sometimes be effective, as several trials have shown improved responses when platinum is reintroduced after a break.
Dr. Ursula Matulonis, Gynecologic Oncologist
How Alicia learned about platinum resistance and impact on her work
He told me that it’s the type of cancer I had in my body. Sometimes it happens to patients where it resists, and we can no longer use that treatment on the cancer because it will not work anymore.
I had been working, but I ended up having to stop. I was losing so much time because of my appointments that I couldn’t work the hours to keep my insurance, so I lost my insurance. I had to find another center to work with me, because the center I was at did not have a charity program, so I couldn’t do a payment plan or anything like that.
Dr. Matulonis on platinum sensitivity, platinum resistance, and reuse of platinum
As treatment progresses, the concepts of platinum‑sensitive and platinum‑resistant recurrence become important. The platinum‑free interval is the time from the last dose of platinum (like carboplatin) to the first documented recurrence, whether that’s a rising CA‑125 or symptomatic disease, like ascites or bowel obstruction.
Broadly, platinum‑sensitive recurrence means a longer interval off platinum (classically more than six months) and is typically treated by reusing platinum. Platinum‑resistant recurrence refers to recurrence within about six months of the last platinum dose, and platinum‑refractory means the cancer grows while the patient is still on platinum. In platinum‑refractory disease, I do not reuse platinum; we need a different strategy.
That said, even in platinum‑resistant settings, after some time off, reusing platinum can sometimes be effective, as several trials have shown improved responses when platinum is reintroduced after a break.
I still had hope. I knew I was in the right place because everybody talks so highly of Moffitt.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient
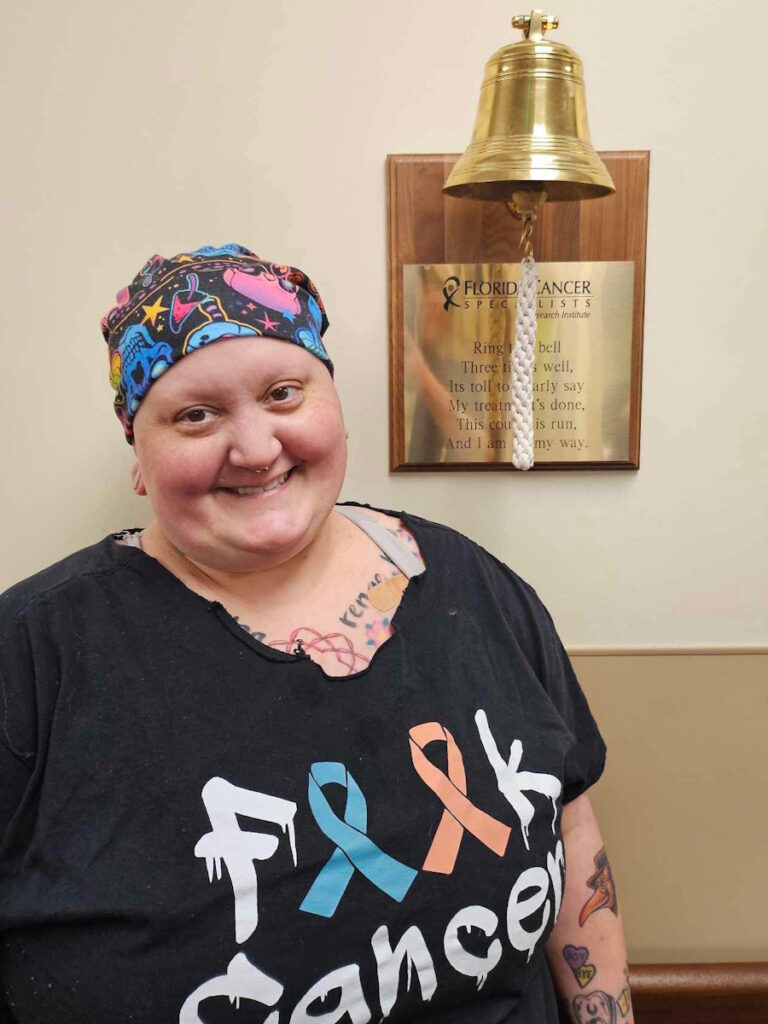
Transferring to Moffitt allowed Alicia to regain hope
I found one of the best cancer centers in Florida: Moffitt Cancer Center. They picked me up. I was able to transfer to them. I asked my main oncologist, “Can you transfer me?” and they did. I was able to get a charity program with them, and I got a new oncologist there. That’s when she went through my records and explained again about the platinum resistance and introduced a new chemotherapy regimen to me.
I still had hope. I knew I was in the right place because everybody talks so highly of Moffitt. I knew they were going to help me find something to take care of my cancer. I was like, “Okay, let’s do everything we can, because I want to get back to at least a normal life.”
Trusting a new oncologist and treatment options
I was leery, but her nurse practitioner told me that she was one of the top OB-GYN oncologists in the center, and she was also in charge of trials. Going to a new place and a new doctor, you’re always going to be kind of leery, because you have to explain everything all over again, tell them about side effects that you experienced, and things like that. But she gave me the option to either continue with the chemo or not if I didn’t want to, or I could have gone to another place.
I had options regardless, and she listened to everything I was saying. I put it in her hands because she knows what she’s doing. I asked, “What’s the best thing that you can do for me?” She took my samples again to see what would actually work and what wouldn’t work, and that’s when the new drug came into play.
My cancer is rare. It’s hormone-based and not genetic… I have to be careful not to run through my options… There are not a lot of them out there for the type I have.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient
What are Antibody-drug conjugates and folate receptor alpha
Antibody-drug conjugates (ADCs) are an important class of newer therapies. These drugs combine an antibody that targets a surface protein on the cancer cell with a potent chemotherapy payload attached to it. Two key targets we focus on are HER2 and folate receptor alpha (FOLR1).
For FOLR1, one ADC is approved for platinum‑resistant ovarian cancer in patients whose tumors have at least 75% of cells staining strongly positive for folate receptor alpha. In a pivotal trial, this FOLR1‑targeted ADC, compared with standard chemotherapy, showed the first survival benefit in the platinum‑resistant setting — improving both progression‑free survival and overall survival. That represents a major step forward.
Not all tumors meet that high FOLR1 threshold, so other ADCs are being developed that can work at lower levels of expression or target different proteins, such as HER2 or CD6. Some ADCs are more biomarker‑agnostic, which means they don’t require a very high level of the target to show activity.
When planning treatment, we think about which ADC makes sense based on markers and prior lines of therapy. For example, the FOLR1 ADC approval is written for up to three prior lines of treatment with high FOLR1 expression, because beyond that, responses declined in early studies. In contrast, some HER2‑targeted ADC trials in gynecologic cancers did not limit the number of prior lines and still saw activity across a broad range of prior treatments.
Weekly paclitaxel plus bevacizumab is one of our most active regimens in the platinum‑resistant setting and can keep cancer in remission for months.
Dr. Ursula Matulonis, Gynecologic Oncologist
Alicia on a new metastasis, her faith, and hope for the future
Becoming platinum resistant again and having limited options
When I got there, this was far into my year of dealing with all of this. I’ve been at Moffitt for a year now. By August 2026, it will be three years of dealing with this. I actually became resistant to another drug as well, because it did not work. It worked in the beginning, but towards the end, it was not showing improvement. A new drug was the only thing that was showing to keep me stable.
At this point, I had already gone through two types of chemo regimens that are the strongest for ovarian cancer. For me to be resistant to both is one of the rare cases. Once again, she was able to explain more of why my cancer behaves the way it does. My cancer is rare. It’s hormone-based and not genetic. When it comes to hormone-based ovarian cancer, it’s harder to find treatments, and when I do have treatments, they’re very minimal. It’s one of those things where I have to be careful not to run through my options. At the same time, she has been keeping track of trials, but there are not a lot of them out there for the type I have.
New metastatic mass and barriers to clinical trials
I found out that I have a metastatic mass that appeared, so that makes it a little bit harder. I also found out that because I’m a dual cancer patient, it’s harder to find a trial that will accept me for ovarian cancer. Even though my uterine cancer is not there or not popping up, they only want patients with one cancer.
With this new mass that popped up, the next step is radiation therapy for my vaginal cuff. The good thing is I’m still stage 3, but now it’s metastatic. (According to the National Cancer Institute, cancer that spreads from where it started to a distant part of the body is called metastatic cancer. For many types of cancer, it is also called stage 4 cancer. The process by which cancer cells spread to other parts of the body is called metastasis.)
My advice is not to give in to negativity, which is the hardest thing, and to be as strong as you can, even when you feel that you’re not.
Alicia N., Stage 3C Ovarian Cancer and Stage 1 Uterine Cancer Patient
Coping, faith, and Buddhist perspective
It’s tough because you feel that there’s an end or that things are starting to clear, and then something new pops up. Because I’m Buddhist, we look at it as an obstacle to overcome and not to let it take over. Our saying is “turn poison into medicine,” so you’re taking your suffering, which is poison, and you’re turning it into happiness and better results.
I have that to help keep me sane through all this, because if not, I don’t know where I would be. My wife is my rock for sure.
Advice to others and mental health
My advice is not to give in to negativity, which is the hardest thing, and to be as strong as you can, even when you feel that you’re not. This takes you to a whole other mental level, whether you have mental health issues or not. Know that you can live a long life, but you have to have the right mindset for it and want to live.
Ovarian Cancer Resources
“Office Hours” with Dr. Matulonis: Side Effects, Scans, and Smarter Treatment Decisions
In the remainder of our conversation, Dr. Matulonis kindly expands on the science and strategy behind ovarian cancer care, from managing side effects and understanding platinum resistance to evaluating clinical trials and long-term planning.
Managing side effects, neuropathy, and bevacizumab risks
One of the most significant chronic side effects in ovarian cancer treatment is peripheral neuropathy, which is numbness and tingling in the fingertips and toes, often from taxanes, like paclitaxel. Sometimes neuropathy improves after initial chemotherapy, but it can also be long‑lasting. When reusing paclitaxel, even weekly, I check carefully that neuropathy is not worsening to the point of affecting function.
For bevacizumab, we must consider medical comorbidities. Patients with underlying heart disease, low left‑ventricular ejection fraction, or chronic kidney disease (CKD) may be at higher risk for cardiac or renal complications. Bevacizumab can worsen blood pressure and kidney function, and can impair wound healing. It is contraindicated in the setting of an active small bowel obstruction, because earlier trials showed cases of bowel perforation in platinum‑resistant ovarian cancer patients with obstruction.
Weekly paclitaxel plus bevacizumab is one of our most active regimens in the platinum‑resistant setting and can keep cancer in remission for months, but it requires weekly visits, causes hair loss and neuropathy, and adds bevacizumab‑related toxicities. These practical and quality‑of‑life issues are part of every treatment discussion.
Cure, remission, and long‑term planning
When starting upfront carboplatin‑paclitaxel chemotherapy, the purpose we write on the consent form is curative. Patients can be cured of ovarian cancer, especially those with BRCA mutations or other high‑risk mutations that confer enhanced sensitivity to platinum. Unfortunately, a majority of patients do develop recurrent disease later.
In recurrence, there are more choices. We look at histology, the number of prior lines, HRD/BRCA status, HER2 and FOLR1 expression, and other genetic alterations, such as cyclin E1 amplification or KRAS mutations, especially in low‑grade serous cancers. We also consider prior toxicities and what the patient is willing and able to tolerate in terms of logistics and quality of life.
The science and clinical trials are hugely important for discovering new vulnerabilities and new treatments.
Dr. Ursula Matulonis, Gynecologic Oncologist
Clinical trials, immunotherapy, and research progress
Clinical trials are a critical part of progress, but they are not for everyone and should never be forced. I present all reasonable options, including trials, but it’s ultimately the patient’s decision.
As of now, immunotherapy with checkpoint inhibitors has had limited benefit in most ovarian cancers because of low tumor mutational burden and the immunologically cold nature of high‑grade serous disease. However, newer immunotherapy approaches are under study, including bispecific antibodies that target two proteins at once, CAR T‑cell and CAR NK (natural killer) cell therapies, and combinations of weekly paclitaxel with experimental immunotherapies.
Antibody-drug conjugates are also being tested earlier in the disease course, including as maintenance after platinum‑sensitive recurrence and, in some trials, in frontline settings alongside or following carboplatin-paclitaxel. Research into DNA repair pathways continues as we look for new ways to target homologous recombination defects beyond PARP inhibitors.
We are making progress, but there is still a long way to go. The science and clinical trials are hugely important for discovering new vulnerabilities and new treatments.
Communicating scan results and tailoring treatment
Delivering scan results, especially bad news, never gets easier. I always have to prepare myself before walking into the room, because patients often look at my expression to gauge what the scans show. With electronic medical records, scan results are now released directly to patients by law, so many patients have already read them before we talk. They may not interpret all the details, but they usually know if something is good or bad.
I review the scans myself, pull up the images, and, with the patient’s permission, turn the screen around to show exactly what is happening and compare current and prior scans. Sometimes imaging underestimates tumor burden, especially when cancer spreads as a thin layer over intestinal surfaces that CT cannot easily see. Symptoms — such as early satiety, nausea, vomiting, or gastrointestinal issues — can reveal more than the scan alone.
We integrate imaging, symptoms, tumor markers like CA‑125, and patient preferences to decide whether to change treatment, continue and re‑scan later, or shift focus to symptom control. We also consider clinical trial options, travel distance, and whether virtual visits are feasible, especially for patients who live far from Boston.
My job is to come up with treatment plans that address the molecular aspects of the cancer, avoid worsening preexisting side effects, and respect the patient’s wishes and life circumstances.
Dr. Ursula Matulonis, Gynecologic Oncologist
Role of specialists, community oncologists, and virtual care
General oncologists take care of many different cancers, which makes it difficult to keep up with the details of each tumor type, the newest research, and targeted therapies. There is a huge amount of information — press releases, abstracts, papers — and even subspecialists cannot attend every meeting. That’s why working with a specialist in gynecologic oncology is important when possible, especially for complex cases or when considering novel therapies.
Telemedicine has helped. I hold licenses in multiple states, including Massachusetts, Maine, and Rhode Island, so I can see patients virtually and advise them or their local oncologists on options, including clinical trials. Whether a patient wants to travel several hours for a trial is their choice; my role is to present accurate information and realistic expectations.
Balancing efficacy, toxicity, and patient priorities
My job is to come up with treatment plans that address the molecular aspects of the cancer, avoid worsening preexisting side effects, and respect the patient’s wishes and life circumstances. It is exciting to see medications that can relieve a small bowel obstruction from platinum‑resistant disease, reduce pain, and improve quality of life.
For any given patient, we think across classes of drugs:
- Chemotherapy (platinum and non‑platinum)
- Bevacizumab (with careful attention to contraindications)
- Antibody-drug conjugates (HER2, FOLR1, others)
- Hormonal therapies for estrogen receptor-positive tumors (especially low‑grade serous)
- Targeted agents for specific mutations (e.g., KRAS, cyclin E1 amplification)
- Immunotherapy or bispecific antibodies in trials
We ask: What is the goal — cure, long remission, or symptom control? What side effects are acceptable? How far can the patient travel? Are they interested in a clinical trial? There are many options now, which are very different from five to 10 years ago, but the art is matching the right option to the right patient at the right time.
Patients should be offered options, never pressured, and supported whether they choose standard care, a clinical trial, or a more comfort‑focused approach.
Dr. Ursula Matulonis, Gynecologic Oncologist
Hope, information, and shared decision‑making
Hope is always important. I understand that if someone is not feeling well, it can be hard to feel hopeful, but doing some research, understanding their cancer, and having open conversations about new therapies can help. Clinical trials of immunotherapies, ADCs, DNA repair-targeting drugs, and other approaches are ongoing and may expand options further.
Scientists are discovering new vulnerabilities in ovarian cancer, especially in DNA repair pathways, while clinical researchers test how best to use new and existing drugs. Patients should be offered options, never pressured, and supported whether they choose standard care, a clinical trial, or a more comfort‑focused approach.

Inspired by Alicia's story?
Share your story, too!

Thank you to Corcept Therapeutics for their support of our independent patient education program. The Patient Story retains full editorial control over all content.
This interview has been edited for clarity and length. This is not medical advice. Please consult with your healthcare provider to make informed treatment decisions.
The views and opinions expressed in this interview do not necessarily reflect those of The Patient Story.
More Ovarian Cancer Stories
Randalynn V., High-Grade Serous Carcinoma, Stage 1C
Symptoms: Pulling sensation when emptying bladder; abdominal pain
Treatments: Chemotherapy (carboplatin & paclitaxel), surgery
...
Shirley P., High-Grade Serous Carcinoma, Stage 3C, BRCA1+
Symptoms: Pulling sensation when emptying bladder; abdominal pain
Treatments: Chemotherapy (carboplatin & paclitaxel), de-bulking surgery, PARP inhibitors
...
Suzann B., High-Grade Serous Carcinoma, Stage 3C, BRCA1+
Symptoms: Inability to urinate
Treatments: Chemotherapy, de-bulking surgery, total hysterectomy
...
Susan R., High-Grade Serous Ovarian Cancer, Stage 4
Symptoms: Pulling sensation when emptying bladder, abdominal pain
Treatments: Chemotherapy (carboplatin & paclitaxel), surgery
...
Sara I., High-Grade Serous & Clear Cell Carcinoma, Stage 3A
Symptoms: Random sharp pains, unrelated scan showed ovarian cyst
Treatments: Debulking surgery, chemotherapy (carboplatin & paclitaxel), PARP inhibitors (clinical trial)
...




