Thriving with Multiple Myeloma: Bispecific Treatment Options
Multiple myeloma patient advocate Kenny Capps speaks with multiple myeloma expert Dr. Carl Ola Landgren of the University of Miami Sylvester Comprehensive Cancer Center as he shares actionable insights on the latest treatments, effective side effect management, and innovative therapies. Gain the knowledge you need to thrive with multiple myeloma and take charge of your journey.
Learn about treatments like CAR T-cell therapy and bispecific antibodies. Discover effective strategies for managing treatment side effects to improve your quality of life. Get expert tips for living well and staying active while managing multiple myeloma. Understand how to tailor your treatment journey with the latest medical advancements and expert advice.
Edited by: Katrina Villareal
- Introduction
- What Does Relapsed/Refractory Mean in Multiple Myeloma?
- What Percentage of Multiple Myeloma Patients Experience Relapse or Become Refractory to Initial Therapy?
- Does Traditional Chemotherapy Still Play a Role in the Relapsed/Refractory Setting?
- Bispecific Antibodies vs. CAR T-cell Therapy
- Are There Specific Patients Populations More Likely to Benefit from Bispecific Antibody Therapy?
- Common Side Effects: Bispecific Antibodies and CAR T-cell Therapy
- Clinical Research and Development
- What Should Patients Consider When Deciding on Bispecific Clinical Trial Participation?
- What Makes a Cancer Center Comprehensive?
- Overcoming Barriers to Patient Engagement
- Finding More Information About the Latest Relapsed/Refractory Treatment Options
- Conclusion
Introduction
Tiffany Drummond: I’m a patient advocate with over 20 years of experience in cancer research. My journey as a caregiver began when my mother was diagnosed with endometrial cancer in 2014. I quickly realized the challenges of finding resources, support, and shared experiences, and I’m committed to helping others avoid similar difficulties, no matter the condition.
At The Patient Story, we create programs to help you figure out what comes next. Think of us as your go-to guide for navigating not only the cancer journey but your overall health journey. From diagnosis to treatment, we’ve got you covered with real-life patient stories and educational programming with subject matter experts. I’m here to help you and your loved ones best communicate with your healthcare team as you go from diagnosis through treatment and survivorship.

We want to thank our promotional partners for their support. Because of you, our programming reaches the audience who needs it. I hope you all find this program helpful, but please keep in mind that the information provided is not a substitute for medical advice.
We have two amazing guests that I want to introduce as we talk about the latest treatment options for multiple myeloma. Dr. Carl Ola Landgren is a hematologist and oncologist, professor of medicine, and division chief of myeloma in the Department of Medicine. He is the director of the Sylvester Myeloma Institute at the Sylvester Comprehensive Cancer Center and co-leader of the Translational and Clinical Oncology Program at the University of Miami. We are so happy to have you, Dr. Landgren. Thank you so much for taking the time to be with us. Our moderator will be Kenny Capps, a multiple myeloma survivor and thriver.


Kenny Capps: Thanks, Tiffany, I’m honored to be your moderator. I’m the executive director of Cancer Active, a nonprofit organization dedicated to empowering those affected by cancer to live active and fulfilling lives. I’ve been on my journey with multiple myeloma since 2014. I understand many of the challenges that patients must navigate.
I was diagnosed relatively young at the age of 42 and have lots of bone involvement, spinal compression, fractures, and lesions. I’ve undergone infusions and a bone marrow transplant. I’ve lost count of how many bone marrow biopsies I’ve had. In 2023, I relapsed, changed therapies, and added radiation treatment to the list of things I’ve never done before.
I did all this while raising three kids, training 30 to 70 miles a week, running 1,200 miles across the state of North Carolina, and experiencing all the celebrations and heartbreaks that come with life, regardless of whether you’re treating cancer or not. I’ve had many experiences and a lot of education as an athlete, a coach, an attorney, and a father, and 10 years ago, I combined all of those experiences to become a patient advocate and a Cancer Active leader.

We’re fortunate to have one of the leading voices in multiple myeloma research and treatment with us. Dr. Landgren is not only a pioneer in advancing care for this disease but also deeply committed to translating cutting-edge science into real, human-centered solutions for patients like you and me. His work has helped reshape how we understand and treat multiple myeloma, giving us more options and more hope than ever before.
This conversation is all about you. We’ll explore the latest in multiple myeloma treatment and emerging research, and, most importantly, answer your questions in a way that makes this topic understandable and actionable. It’s my privilege to introduce our distinguished guest, Dr. Carl Ola Lindgren.
Dr. Carl Ola Landgren: Thank you very much for having me. It’s a great pleasure and a great honor.

What Does Relapsed/Refractory Mean in Multiple Myeloma?
Kenny: Our audience is pretty savvy, but for those unfamiliar with the term relapsed or refractory in the multiple myeloma setting, could you break down what that means?
Dr. Landgren: Relapsed and refractory refers to the multiple myeloma disease becoming active again. Someone who is newly diagnosed would typically receive combination therapy with or without transplant and with continued therapy, which we also call maintenance therapy. Over time, unfortunately, the majority of patients will have the disease become active again and this is because we do not have an established cure for the disease.
In 2025 and onwards, many patients can live for 10 to 20-plus years and there will be patients who will not have their lifespans shortened, which is what the field is going for. For the most part, the disease will be managed as a chronic disease as we try to develop definitive cures.

If there is reappearance of rising levels of proteins in the blood, if other clinical suspicions are going on that would trigger additional radiological assessments, like PETs, PET/CTs, or MRIs, or if we do bone marrow biopsies and see that there is more disease, then that would be consistent with the disease becoming active again.
When we do clinical trials, we have rule books for what is what. We have a rule book for what’s called a partial response, what’s a complete response, what MRD negativity is, and we also have rules for what progressive disease is and how to capture that. If you don’t have a common language, we cannot compare the results across different trials, so that’s very important. We worked on that as a community for over 20 years.
In the setting of those rules, a relapsed/refractory disease refers to a situation when a patient has rising levels of markers by these definitions we have, either while being on a given therapy or if it happens within 60 days after stopping therapy, then that would also count as a relapsed/refractory state.
We looked at drugs that had a good benefit, were not too toxic for the patient, had no other contraindications, and tried to see how we can partner them with other drugs than we did the previous time we gave them.
Dr. Landgren
Kenny: About refractory, does that mean that they are unable to continue along that line of treatment?
Dr. Landgren: The word refractory carries probably more focus on things that are not true, which is that you cannot go back and use that treatment. In reality, what it means is that right now, it is not the optimal therapy to use going forward. You can revisit and use that drug in the future, maybe in combination with other drugs at a later time point as what we very frequently do. We recycle the drugs.
An example could be you use a proteasome inhibitor, an IMiD (immunomodulatory drugs), and a steroid with a CD38-targeted antibody as a combination therapy and you give that for a certain number of cycles. You may collect stem cells, give more cycles, do a transplant or not, and go to a maintenance therapy. You may have an IMiD at a lower dose with the CD38-targeted antibody and eventually, you may step down to a single drug IMiD.
Many years later, there’s a reappearance of protein in the blood. Could you go back and use a proteasome inhibitor? Yes, you can. Could you go back and use the CD38-targeted antibody? Yes, you can. Is it the best thing to use that same IMiD at the same dose level? Probably not because the disease was able to grow through that. What about increasing the dose? Probably not the best option right now, so maybe switch to another IMiD or some other drug. Then you can overcome this reappearance or relapse and get many more years with the same benefit. You get rid of the disease and keep the disease from becoming active.

If the disease comes back again, could you not ask the same question? Could you go back to those same drugs, including the first IMiD? I would think yes. You could think about using the same drugs over and over again, but there are so many new drugs coming to the field. Many times, we are going to new mechanisms of action as the next step forward.
At some point, when we have used all the different mechanisms of action, we will go back, recycle, and use them in different combinations. We looked at drugs that had a good benefit, were not too toxic for the patient, had no other contraindications, and tried to see how we can partner them with other drugs than we did the previous time we gave them.

Kenny: When you’re saying that, what I think about is lenalidomide, bortezomib, and dexamethasone, and then a maintenance therapy after a bone marrow transplant, but a patient might stop responding to 5 or 10 mg of lenalidomide at some point in the future. You’re saying that they could switch over, so maybe pomalidomide at some point as a substitute, but that doesn’t discount the possibility that lenalidomide might be a solution for them in the future.
Dr. Landgren: That’s exactly right. If you look at how these drugs were developed, they were developed for certain indications. You mentioned pomalidomide as the next move and that’s the example I gave between the lines. I didn’t mention the drugs, but you filled in the blanks and the drugs you gave were probably the drugs that, for the most part, would fit with the example I gave.
We do not have an established cure, so if you look at the population databases that are currently available, unfortunately, the majority of patients will have the disease become active again at some point.
Dr. Landgren
Pomalidomide was developed in 2006 and was given to a patient that lenalidomide failed and that’s how the FDA approval was granted. It’s a logical thing to do. What hasn’t been done in a trial is to go back and revisit lenalidomide at a later time point. Why is that? Once the drugs are approved, they are commercially available and we can prescribe them.
It addresses an important topic of the so-called real-world evidence and that’s where people like me come into play. I have been a doctor for 29 years. I’ve treated probably thousands of patients and used all the FDA-approved drugs. I’ve worked on very many clinical trials, phase 1 and phase 2 studies, and also some of the phase 3 trials. I have a lot of experience with these drugs.
When people like me use the drugs every day in our clinics, we learn how to use them in a recycled manner for patients who have the disease coming back. Sometimes we document and many times, we talk about it. When I’m at meetings, many colleagues who may see fewer patients could come up and get the advice. We try to share our experiences with each other and that’s how we help each other as a community.

What Percentage of Multiple Myeloma Patients Experience Relapse or Become Refractory to Initial Therapy?
Kenny: Given the evolving landscape of myeloma treatment, what are the current estimates for the percentage of patients who experience relapse or become refractory to initial therapy? How do factors, such as patient age, disease stage, and genetic risk profile, influence these rates?
Dr. Landgren: We do not have an established cure, so if you look at the population databases that are currently available, unfortunately, the majority of patients will have the disease become active again at some point. There’s a small group of patients whose disease doesn’t come back and that’s an important piece to point out that the disease is curable.
The problem is that the disease is very different from patient to patient. We call it genomically heterogeneous, which means it’s not the same disease in every patient. When we profile the disease, we can see that if we perform whole genome sequencing, the average patient has a few thousand mutations and you can also see alterations in the immune system. With a disease that is so different from patient to patient, it’s not surprising that when you give the same therapy to everyone, the outcome would be different and that’s why we say there are different prognoses.
As the treatment gets better and better, more and more patients could benefit from the therapies, so there will be fewer patients who will have the disease return sooner.
Dr. Landgren
People have talked about high risk or standard risk in this very setting. The concept of high-risk disease is a moving target. If you have a weaker treatment and you treat 1,000 patients, more patients will not benefit from that treatment because the disease biology could be stronger than the therapy over time and it will come back sooner.
As the treatment gets better and better, more and more patients could benefit from the therapies, so there will be fewer patients who will have the disease return sooner. For that reason, the so-called high-risk group is shrinking and it’s always in the light of how you treat. Ultimately, with the best available therapy, there is no high-risk disease and we could envision a scenario of a cure.
The rate of relapse is in the light of how we treat, but we still don’t have a definitive cure, so statistically, the majority of patients will have their disease coming back. What’s different at this time compared to 10 or 20 years ago is the duration of the benefit of therapy is drastically different.
The disease will probably come back for the majority of patients, so we are trying to develop curative strategies that are definitively curative.
Dr. Landgren
When I was in fellowship 25 years ago, the time from diagnosis to a patient passing away from the disease could be only one or two years. I have many patients who are 20 years out and doing great, and many of those patients will not die due to myeloma. We will all die at some point, but many people will probably die with myeloma not from myeloma, which is a huge change.
Kenny: Yeah, and that’s a phrase I hear more and more, which is good to hear.
Dr. Landgren: If we can keep the disease away and people can have a good quality of life and no shortening of lifespan, that’s a huge deliverable. For many patients, we’re already at that point, but there may have to be changes in treatment. The disease will probably come back for the majority of patients, so we are trying to develop curative strategies that are definitively curative.

Does Traditional Chemotherapy Still Play a Role in the Relapsed/Refractory Setting?
Kenny: You mentioned quality of life and that’s impacted by the progression of the disease, side effects from treatment, or the psychosocial challenges that patients have to deal with day-to-day that negatively impact how they feel and what their life is. As you mentioned, the treatments over the past decades have changed dramatically. In the context of relapsed/refractory multiple myeloma, does traditional chemotherapy still have a role to play in the world of IMiDs, CD38 treatment, bone marrow transplants, and CAR T-cell therapy?
Dr. Landgren: We don’t want to stop using drugs that we know work until we have a definitive cure. You want to keep all the different options. We want to have all the doors open. But the order and the priority of the different therapies will probably continue to change.
When I was in fellowship, the therapies were very, very inferior. The overall survival was one to two years. The remission rates were in the single digits. These days, if I treat, I would achieve remission rates of 90 to 95-plus percent. I have MRD negativity rates in my newly diagnosed patients of over 70%.
Will that mean that chemotherapies will go away? I don’t think so. Not until we have a cure. Potentially, the role for these therapies will shift that they will be options if patients have later line relapses.
Dr. Landgren
For the majority of my patients, I don’t use any chemotherapy. For many years, we have also explored harvesting the stem cells and holding them, so you could also not go for a transplant. Transplant is chemotherapy. In the United States, it’s called transplant, but in Europe, it’s called high-dose chemotherapy and it is chemotherapy because it’s melphalan chemotherapy. The stem cells are not part of the treatment. They’re a way to recover from the chemotherapy.
There will be a shift away from chemotherapy as we see more and more immunotherapies coming. The CD38-targeted antibodies are coming at full speed, but there are also new antibodies with new targets coming. In 2024, the FDA approved CAR T-cell therapy for the first relapse.
Will that mean that chemotherapies will go away? I don’t think so. Not until we have a cure. Potentially, the role for these therapies will shift that they will be options if patients have later line relapses. If you have immunotherapies upfront and if there is recurrence, there are more immunotherapies. If there is a recurrence again, there are more immunotherapies. Eventually, maybe the chemotherapies will be part of it.
There will be patients who will be outliers from this principle. Chemotherapy drugs are the most tumor-sensitive drugs. Some patients to whom we give immunotherapies don’t do as well. Those patients are a minority, but there are patients like that, so it’s good to have options.

Bispecific Antibodies vs. CAR T-cell Therapy
Kenny: Could you discuss further the differences between bispecific antibodies and CAR T-cell therapy?
Dr. Landgren: A bispecific antibody is exactly what the name tells you: it’s bi, so it’s two, and it’s specific, so it’s specific in the sense that it goes for myeloma and it’s linked towards immune cells, T cells. The way these antibodies are engineered is they have two heads. One head binds to a protein on the surface of the myeloma cells and the other head binds to a surface marker on the T cell. On the T cell, the marker is CD3. For the myeloma cells, there are currently two approved antibodies that have two different targets: BCMA (B-cell maturation agent) and GPRC5D.
A bispecific antibody is exactly what the name tells you… One head binds to a protein on the surface of the myeloma cells and the other head binds to a surface marker on the T cell.
Dr. Landgren
There are three bispecific antibodies approved for multiple myeloma. All of these antibodies bind to CD3. They bring the T cells to the antibody, so they hold on to the T cell, and when they grab the myeloma cell with the other marker, the myeloma cell is now neighbors with a T cell and the T cell will then do its job of killing the myeloma cell. That’s how bispecific antibodies work.
CAR T cells is an acronym for chimeric antigen receptor T cells. T cells circulate in the blood and you can take them out from the blood of a person. They are not stem cells. They’re not the type of cells you would collect for a transplant. These are circulating immune T cells. You can take them out and send them to an approved facility. They will do a transduction of these T cells, which means they are being exposed to a genomic vector that will change the DNA in these cells. They will insert certain information that contains instructions for these T cells to do things that they normally wouldn’t do, which is to develop an antenna on their surface and that is what the receptor is. They are the same T cells plus the instruction that says to make this receptor on their surface. Other than that, they do the same job they normally would do. You feed them with glucose and nutrients and keep them warm.
In a way, bispecific antibodies and CAR T cells do the same thing. They take advantage of T cells.
Dr. Landgren
In the current development setting, about four to six weeks later, you give the CAR T cells to the patient. When they reenter the body, they will be let in because the body will recognize them as their own T cells. When they come in, they are now programmed with receptor-like antennae on the surface to bind to something that fits, which is the BCMA protein. When they bind to it, same as the bispecific antibodies, now a T cell is neighbor to a myeloma cell and when it sees the myeloma cell, it will kill it.
In a way, bispecific antibodies and CAR T cells do the same thing. They take advantage of T cells. In one setting, you keep the T cells in the body and give a matchmaker, which is the antibody. In the other example, you take out the T cells, modify them, and give them back.

There are other ways of doing it. You can have donors give blood where you can make something called allogeneic CAR T cells, which is a mass-produced CAR T cell that comes from a pool of donors, and you give that to multiple patients. The idea here is that you can give them immediately because there is no need to harvest them, manufacture them, and give them back. You have donor-derived T cells. Unfortunately, there are none yet approved for myeloma.
There are also other technologies where you can insert mRNA-made T cells and bispecific antibodies. Similar to how the COVID vaccines were developed, you can use mRNA infusions to synthesize these types of products within the body. That has not yet happened in humans, but there are a lot of animal models. We’ll see how these mRNA-based technologies will speed up the development of immunotherapies. This is going to be very, very exciting.
The jury is still out on the right sequence, whether you should do CAR T-cell therapy first and then at a later time point, bispecific antibodies or vice versa.
Dr. Landgren
Are There Specific Patients Populations More Likely to Benefit from Bispecific Antibody Therapy?
Kenny: Are there specific patient populations that are most likely to benefit from bispecific antibody therapy?
Dr. Landgren: Currently, there is no head-to-head randomized study that has compared patients given a bispecific antibody and patients given CAR T-cell therapy. All the studies have compared CAR T-cell therapy with older combination therapies or bispecific antibodies compared with older combination therapies.
What we do know is if a patient has an activation of the disease or there is a relapse, the majority of patients have a slower evolution of the disease. The disease usually shows up as increasing protein markers in a blood test and it can go on for many weeks or even months before you start making decisions to change the therapy, so you have some time to make treatment decisions.
But for some patients, the disease becomes active in a short timeframe, so you cannot wait to collect the T cells, send them for manufacturing, keep the disease under control with bridge therapy, and then give back the CAR T cells. In their case, a bispecific antibody is the better option.

If you have patients where the disease is moving more slowly, you have two options. You could argue which is better and I would say different experts would have different opinions. In my experience, different patients will have different opinions.
The jury is still out on the right sequence, whether you should do CAR T-cell therapy first and then at a later time point, bispecific antibodies or vice versa. There are so many details when it comes to this and we don’t have the data to fully answer.
If you started with a bispecific antibody, could you do CAR T-cell therapy in the future?
Dr. Landgren
If you treat someone with CAR T-cell therapy, on average, it would last for many years. But if a patient, God forbid, has a shorter benefit, let’s say 6 or 12 months, going right to a bispecific antibody with the same target usually doesn’t work because the time in between is too tight. But if you go to another therapy with another target with another mechanism of action, could you revisit that same target using a bispecific? I would say the answer is yes for the most part. It comes back to recycling drugs or targets.
If you started with a bispecific antibody, could you do CAR T-cell therapy in the future? Yes, with the same target, but if you do them back to back, that may not be optimal. If the cells build up some form of resistance to the same mechanism of action, you want to distract the cells by doing something else to bring down the disease. If you get good mileage out of that and need to switch again, that could be the time to go back to the same target.

Common Side Effects: Bispecific Antibodies and CAR T-cell Therapy
Kenny: For patients treated with bispecific antibodies, could you discuss the most common side effects and how they are managed?
Dr. Landgren: Compared to bone marrow transplants, CAR T-cell therapy is way less toxic, so the patient experience is much easier. I’ve seen patients who were transplanted years ago and got CAR T-cell therapy and they said this was not even comparable. My oldest patient who turned 87 years old underwent CAR T-cell therapy when he was 86. We would not transplant an 86-year-old, but you could give CAR T cells. I have also treated patients in that age category with bispecific antibodies. I have many patients who have done that and they do extremely well. On average, both CAR T-cell therapy and bispecific antibodies are very, very well-tolerated overall, but everything has some form of side effect. If there is no side effect, usually there is no effect, unfortunately.
On average, both CAR T-cell therapy and bispecific antibodies are very, very well-tolerated overall, but everything has some form of side effect.
Dr. Landgren
When you give a CAR T cell product, you would expect to see cytokine release syndrome (CRS), which means the immune system gets triggered by this immunotherapy and releases substances that the immune system uses to communicate with different immune cells and other surrounding cells. These are the cytokines and chemokines. When they get released, it leads to an immune reaction. It’s a ramped-up version of a person getting sick from an infection or inflammation. Patients get a fever, they don’t feel well, and they could have organs responding to it, like blood pressure going down and things like that.
There are two approved CAR T cell products. When you give cilta-cel, CRS usually takes about a week to kick in. Presumably, that’s the time it takes for the CAR T cell product to amplify, expand, and become fully active. But if you look at the alternative protocol ide-cel, usually the same phenomenon with CRS happens sooner, around the next day. The time windows are different for these different products for reasons we don’t completely understand.

The duration of CRS is usually one to a few days. If the patient has a fever, we can treat it with acetaminophen or we can also give steroids. If it’s a little bit stronger, we would give IL-6 (interleukin-6) receptor inhibitors. There’s a drug called tocilizumab that we use quite frequently and usually, that takes the edge off it. We may have to give IV fluids if the blood pressure goes down a little bit.
Unfortunately, some patients get a little bit sicker and we may have to give them additional drugs. But for the most part, CRS is very manageable and the majority of patients don’t have severe side effects. When this has leveled off, the patient would leave the hospital if the patient was admitted.
Many institutions, including ours in Miami, can administer CAR T-cell therapy outpatient. We have the patient come in, give the CAR T cells, and have the patient stay in close proximity to our institution. If the patient were to develop CRS, we would treat it along the lines of what I said. We may have to admit the patient after a week for one, two, or three nights, and then we can discharge them.
For a few weeks, we would do labs once a week to make sure blood counts are stable and then we would do them once a month and eventually, every three months. We would keep the patient on prophylactic medications with antivirals and antibiotics. We usually give IVIG infusion, which means that we supplement immunoglobulin G levels to keep the patient free from infections. Over time, all these things will be taken off. The average patient could be off therapy for many years and do blood tests every three months.
For the most part, CRS is very manageable and the majority of patients don’t have severe side effects.
Dr. Landgren
For bispecific antibodies, you see the same CRS phenomenon. If you look at the registrational trials that led to the approval of these drugs, the rates are quite high with over 70 or up to 80 percent of patients developing CRS. Most of them are less intense. They are also along the lines of what I said, like fever and drops in blood pressure.
Nevertheless, the FDA has put in the USPI (United States Prescribing Information) saying that the first few doses should be done inpatient to monitor and see if the patient develops CRS, which the majority of patients do if you follow the standard trajectory of the standard recommendations.
Our group at the University of Miami has used premedication with a single dose of IL-6 receptor inhibitors. We give one dose one hour before the very first dose of a bispecific antibody. We presented this at ASH 2024 in San Diego, showing that you can decrease that rate of CRS to 10% and they virtually are always the lowest grade.
This is a huge step forward and sets the stage for thinking about doing this outpatient. If you can premedicate and avoid 9 in 10 patients from having any side effects or if the patient has CRS symptoms and you could guide them on the phone to come in for monitoring or do some intervention overnight, that’s a huge improvement. Premedications should be part of the next step and we are working on that with other groups. I hope in 2025 that these therapies could also be given outpatient.
It’s very important for physicians who treat patients with bispecific antibodies to keep an eye on immunoglobulin G levels and use proper antibiotic and antiviral medications, so patients don’t run into opportunistic infections
Dr. Landgren
An important side effect profile for bispecific antibodies is infection. I have seen this firsthand because I’ve been involved with drug development for a very long time. When I worked in Miami, I was the chief of the Memorial Sloan Kettering myeloma program for many years, so we were involved a lot in these early developments. We don’t want to develop great drugs that hold the myeloma away and allow patients to have a good quality of life but have other problems arising, such as infections.
It’s very important for physicians who treat patients with bispecific antibodies to keep an eye on immunoglobulin G levels and use proper antibiotic and antiviral medications, so patients don’t run into opportunistic infections, which could be very dangerous. This is very important to emphasize. We can premedicate the immediate side effects, but the doctors need to stay on top of it. Patients also need to know that if they develop an infection, they should always alert their doctor.

Clinical Research and Development
Kenny: When it comes to discussing clinical trials and patient support, what do you see as the most promising areas of investigation in terms of bispecific antibody development?
Dr. Landgren: We will see more and more trials with bispecific antibodies that will be used in combinations. At ASH 2024, we saw combinations of two bispecific antibodies: BCMA-CD3 and GPRC5D-CD3. This is the REDIRECT trial, which has been discussed at prior meetings. There were more patients this time and you see very high rates of response. You also see BCMA-CD3 partnered with lenalidomide or carfilzomib, a proteasome inhibitor, in the MagnetisMM-20 study. There are many other studies as well.

What I’m talking about are combinations of bispecific antibodies and other drugs. Eventually, that’s probably what these drugs will fit in with the best. What we will learn, hopefully very fast, is which are the better options to partner them with, the optimal dosing schedules, and the optimal duration of therapy. Can you step down the dose? Can you give it less often? Can you even stop some of these therapies over time?
I don’t have the evidence to prove this, so don’t take this 100% for sure, but based on my looking at data, I project that patients who have been treated with bispecific antibodies, if they have been successfully treated for an extended period or for whatever defined window of time, they may be able to go off therapy.
The missing piece that we are trying to develop is a blood-based MRD test. If you could give treatment and prove that there is no detectable disease, if you could reliably check every three months and make sure there is no disease, many patients could potentially be off therapy for extended periods. It’s an important piece that’s currently missing and we are working on that together with other groups to move that forward.

What Should Patients Consider When Deciding on Bispecific Clinical Trial Participation?
Kenny: For patients who might be considering a clinical trial involving bispecific antibodies, what factors should they consider when making the decision?
Dr. Landgren: The field is moving forward so fast. At this time, bispecific antibodies are only FDA-approved for patients who have failed four or more prior lines. We see from all these trials that they seem to work very well for patients who had their first, second, or third relapse, but that’s only available in trials at the current time.
Getting a second opinion is very well-invested time.
Dr. Landgren
I mentioned combinations with IMiDs and proteasome inhibitors, but there are other drugs as well. I mentioned two bispecific antibodies, but you also have naked antibodies like daratumumab being combined with bispecific antibodies.
If someone is looking for a trial in the space of one to three prior lines, you have to determine what’s available, where you live, what’s feasible to do, what are the different options, what are the dosing schedules, and what are the safety profiles. The side effects always should be looked at in combination with efficacy. It’s a balance between the two. Look at what’s available and make wise decisions. If you’re not sure, go for a second opinion. Getting a second opinion is very well-invested time.
What Makes a Cancer Center Comprehensive?
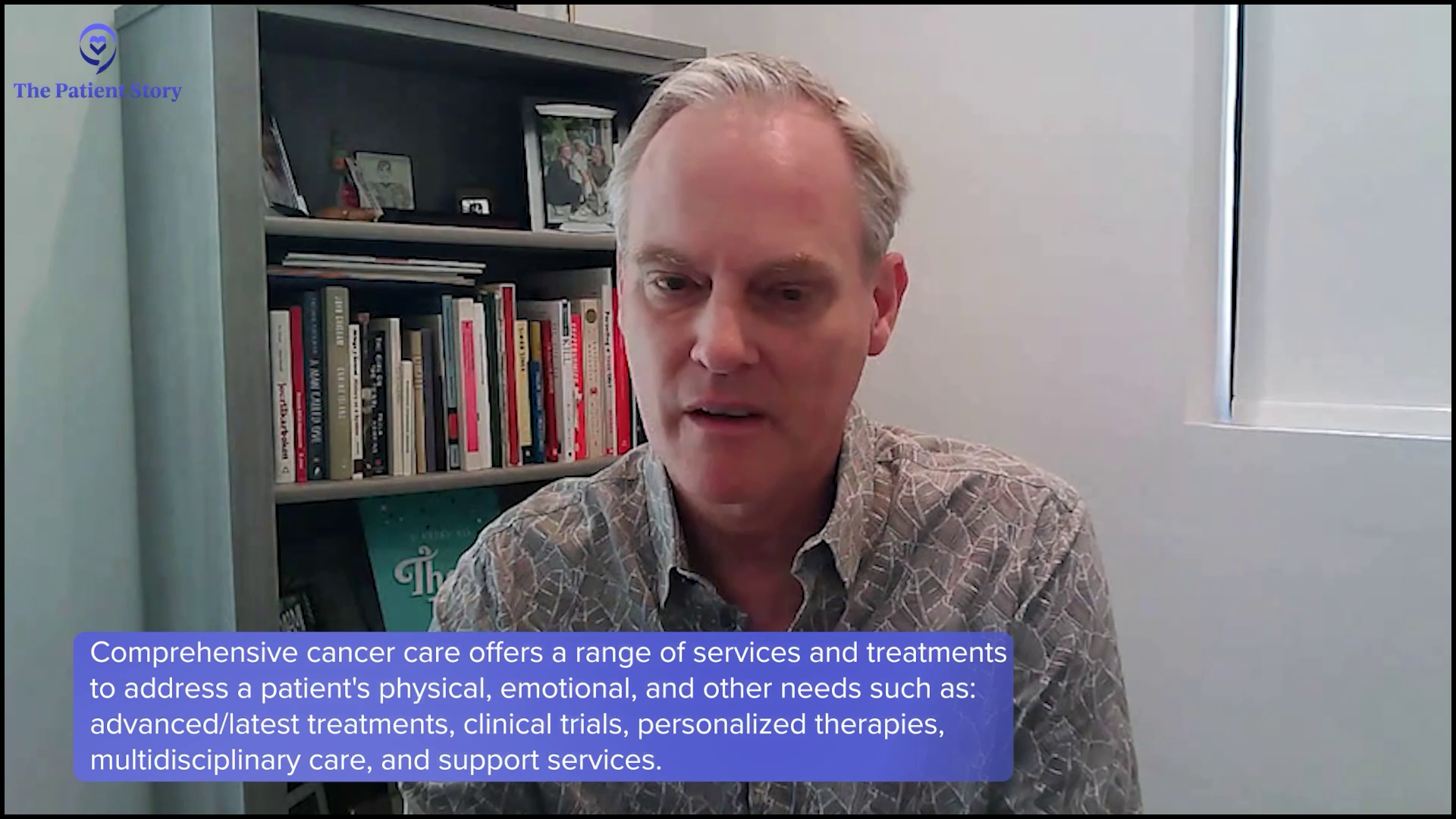
Kenny: Could you tell us more about the oncology social work service at the Sylvester Comprehensive Cancer Center? What makes it truly comprehensive?
Dr. Landgren: We have a very strong team for multiple myeloma. We have doctors, nurse practitioners, nurses, pharmacists, social workers, patient coordinators, navigators, and researchers. We have a very, very comprehensive program.
Many times, patients ask about the cost and implications of the drugs due to insurance. People are changing from one insurance to another or someone is switching to Medicare and wants to know how that works. We have people dedicated to our program. If I get asked this, which I very frequently do, I will always involve my social worker and finance people to help guide the patient. As a doctor, I don’t have access to all this information, but I have a very strong team that will always help me.
If they come to us for help, we want to make sure that we can give every patient the same high level of knowledge, experience, and care that they deserve.
Dr. Landgren
Overcoming Barriers to Patient Engagement
Kenny: One of the challenges is getting some patients to the clinic because I have a feeling that some of them feel like it’s overwhelming. It’s beyond them either because of the cost or the amount of effort on their part to understand. There’s a base layer of knowledge and there’s a language that they have to learn to speak. Sometimes I have a feeling that the patients feel like they don’t belong in this world. How do you navigate that with a patient? Sometimes you have limited time yourself to engage with them. You can’t solve all the problems, like psychosocial issues, mental wellness issues, diet and nutrition issues, and so forth. All of those things are not where you are, but they’re still your patient.
Dr. Landgren: I serve as the chief of the program, so I’ve thought about these things a lot and how we can scale this up and give the ultimate quality for every patient. How can we treat every patient and provide VIP medical care and support?
The way I try to build our program is to build multidiscipline cells of professionals. Every doctor works with a nurse practitioner, a nurse, and a patient coordinator. That’s the backbone of the little group that we have. We have been growing quite fast with an increase in patients of over 20% every year. If the patient volume goes up, when the group gets too busy, then we hire another doctor, nurse, nurse practitioner, and patient coordinator.
At this point, we have close to 10 of those cells. The right size for our program is somewhere between 15 and 20, but right now, 10 is a good number. We will probably hire another one or two and keep on going as our needs grow because there are a lot of patients who need our help. We don’t wish anyone to have myeloma, but if they come to us for help, we want to make sure that we can give every patient the same high level of knowledge, experience, and care that they deserve, and we are very committed to doing that.
Our program is very active when it comes to different patient organizations… I work with anyone who reaches out to us and I always dedicate my time and attention.
Dr. Landgren
On top of that, we have pharmacists, dietitians, finance, and social workers who support all these groups. The model we have is to build a very small group of experts that hold everything together, where everyone knows the patient and the patient knows them. You don’t call a 1-800 number; you call directly or send a message and we will respond usually within an hour if you send a message through our portal. We will be very, very responsive.
We also organize patient seminars. We have programs where patients can volunteer if they want to be part of that. They can talk to other patients. Some patients like that, some patients don’t, but we have that as an option. Our program is very active when it comes to different patient organizations. I’m very inclusive as a person. I welcome all the different organizations and I’ve done so for a long, long time.
I work with the Multiple Myeloma Research Foundation, the International Myeloma Foundation, the HealthTree Foundation, The Leukemia & Lymphoma Society, and The Patient Story. I work with anyone who reaches out to us and I always dedicate my time and attention. If they have in-person meetings or virtual meetings, we always try to help. That’s how we want to share our expertise and our knowledge to help the community.
Finding More Information About the Latest Relapsed/Refractory Treatment Options
Kenny: What advice would you give to patients and caregivers who are seeking more information about the latest treatment options for relapsed/refractory myeloma?
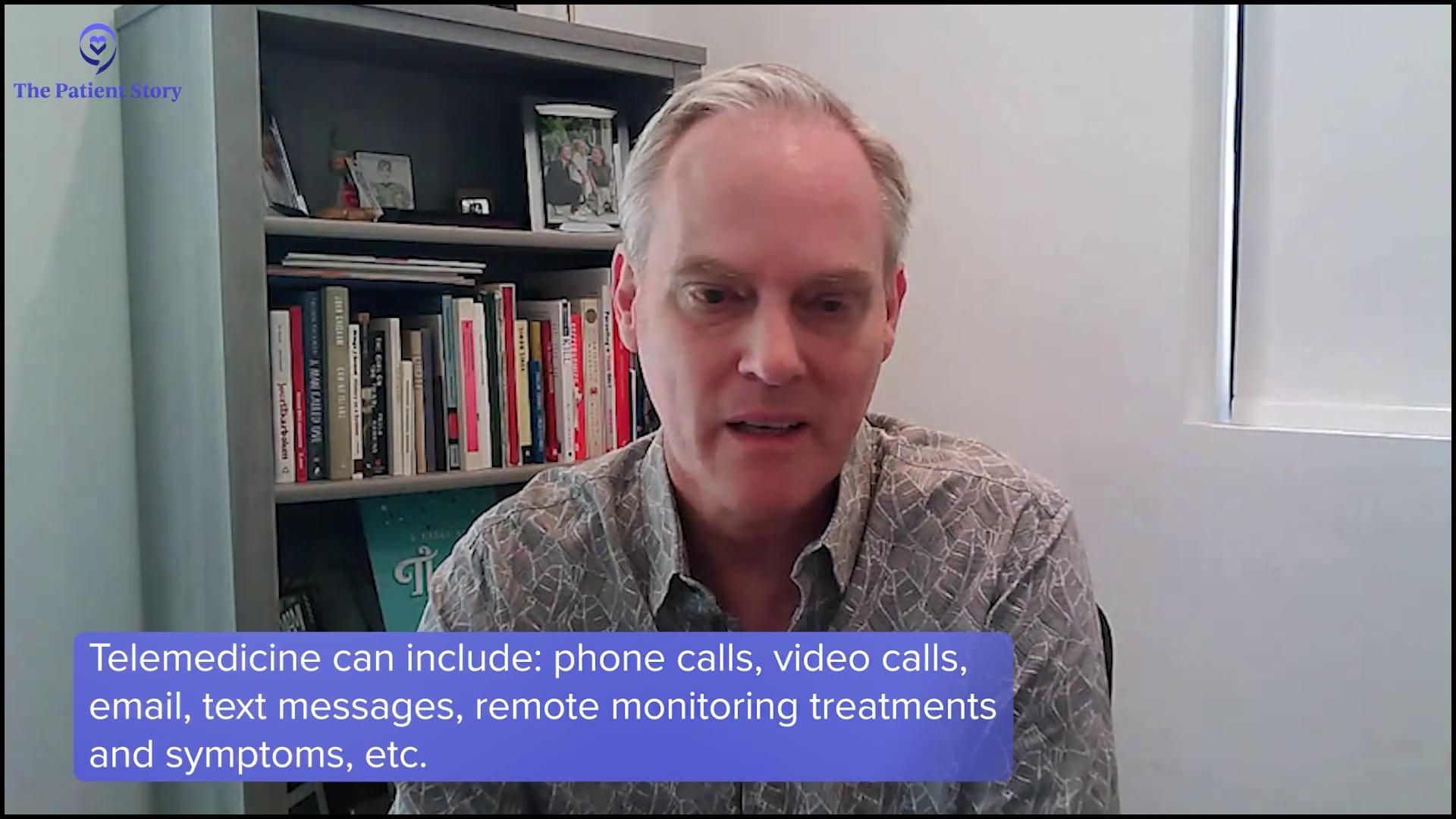
Dr. Landgren: If you have a doctor who you trust and things are going well, work with that doctor and follow that doctor’s recommendations. If you want to have a second opinion, it’s very easy these days to get one. You can travel or if you’re within the States, for the most part, telemedicine visits are available and it’s very important to be able to continue that.
After COVID, I know that there have been some discussions about whether telemedicine should remain or not. All the patient organizations should band together and make sure politicians will never be able to change that because that is going to create barriers for patient access.
If you live in a big city, you have access. If you live in a smaller town, you don’t have access if you have to travel long distances, if you are older, or if you’re frail. Telemedicine breaks down all these barriers. In my opinion, the number one priority for all patient organizations is to make sure that no politician will ever change that because that’s going to cause a lot of patient suffering. In the end, it’s going to take people’s lives and have a lot of negative impact.

Conclusion
Kenny: I love it. Thank you, Dr. Landgren, for taking the time to speak to The Patient Story.
Dr. Landgren: Thank you very much for having me. It was a great pleasure.
Tiffany: What an engaging conversation. Thank you again, Kenny and Dr. Landgren, for taking the time to dive deep into the latest treatment options for relapsed/refractory multiple myeloma patients. If you are a patient advocate, patient, or caregiver, consider being a voice leader in your community or with The Patient Story.
It’s important to be empowered so that you and your caregivers can make informed decisions about your care and that includes being educated about the latest treatment options. Until next time, I’m Tiffany Johnson signing off and on behalf of The Patient Story, thank you for watching.
Relapsed/Refractory Multiple Myeloma Patient Stories
Dr. Yvonne D., Relapsed/Refractory Multiple Myeloma
Symptoms: Severe hip pain, trouble walking due to a broken pelvis, extreme fatigue, bone pains
Treatments: Chemotherapy, stem cell transplant, radiation therapy, surgeries, CAR T-cell therapy
Michele J., Relapsed/Refractory Multiple Myeloma
Symptoms: Fatigue, anemia, persistent lower back pain, sharp leg pain during movement
Treatments: Surgery, chemotherapy, stem cell transplant
Theresa T., Relapsed/Refractory Multiple Myeloma, IgG kappa Light Chain
Symptom: Extreme pain in right hip
Treatments: Chemotherapy, CAR T-cell therapy, stem cell transplant, radiation
Laura E., Multiple Myeloma, IgG kappa
Symptom: Increasing back pain
Treatments: Chemotherapy, stem cell transplant, bispecific antibodies
Donna K., Refractory Multiple Myeloma
Symptom: None; found through blood tests
Treatments: Total Therapy Four, carfilzomib + pomalidomide, daratumumab + lenalidomide, CAR T-cell therapy, selinexor-carfilzomib





